Published online Sep 26, 2022. doi: 10.4330/wjc.v14.i9.514
Peer-review started: July 16, 2022
First decision: August 4, 2022
Revised: August 11, 2022
Accepted: August 30, 2022
Article in press: August 30, 2022
Published online: September 26, 2022
Processing time: 65 Days and 6.8 Hours
Intra-atrial right coronary artery (RCA) is a rare and generally asymptomatic anomaly of development of the coronary arteries. This malformation could pot
We report the case of a 54-year-old man with atypical chest pain who underwent multi-detector computed tomography angiography (MDCTA). The exam revealed no significant coronary artery stenoses; however, an intra-atrial course of mid RCA was evident. Medical therapy was administered, and the patient was discharged to home without undergoing a conventional angiography. Previously reported autoptic and clinical cases were retrieved from the PubMed literature database to compare the clinicopathological features of this case.
MDCTA depicted the abnormal course of the coronary artery in this patient as an intra-atrial course of the mid RCA. Finding this abnormality was crucial to avoid an inadvertent injury during interventional or surgical procedures.
Core Tip: We present a rare case of an intra-atrial course of the mid right coronary artery (commonly referred to as right coronary artery) detected by multi-detector computed tomography angiography (MDCTA). We performed a systematic review of the few cases in the literature. Since this anomaly could potentially expose the patient to catastrophic outcome in case of injury during interventional or surgical procedures, its recognition via MDCTA is crucial before such interventions.
- Citation: Barbiero G, Maiolino G, Argiolas A, Testolin L, De Conti G. Intra-atrial course of right coronary artery: A case report. World J Cardiol 2022; 14(9): 514-521
- URL: https://www.wjgnet.com/1949-8462/full/v14/i9/514.htm
- DOI: https://dx.doi.org/10.4330/wjc.v14.i9.514
Intra-atrial or intra-cavitary course of the right coronary artery (RCA) is defined as a segment of the RCA that courses through the right atrial (RA) chamber[1,2]. It is a relatively rare vascular anomaly, with a reported incidence of 0.09%-0.1%[1,2].
Historically, this anomaly of development was most often identified by accident, during coronary surgery or autopsy, due to its benign outcome; however, in the era of multi-detector computed tomography angiography (MDCTA), it is now detected more frequently, and its incidence rate has risen to 1.8%[1]. From a radiological point of view, it was defined as a segment of RCA entirely surrounded by intra-atrial contrast in all phases of the cardiac cycle, unlike the myocardial bridge, in which a segment of the coronary artery appears as entirely surrounded by myocardial muscle[1,2]. Its recog
Herein, we report the case of a patient with an anomalous course of the RCA through the RA which was identified using MDCTA. Furthermore, to the best of our knowledge, we provide, for the first time, a discussion based on a review of all cases of intra-atrial course of RCA in the literature. The review was conducted according to the guidelines of the Declaration of Helsinki and approved by the Ethics Committee of the University of Padua.
A 54-year-old Caucasian male with moderate cardiovascular risk factors (i.e., obesity, hyperlipidemia, and hypertension) presented to the cardiologic clinic with atypical angina presenting without dyspnea.
The patient reported that the symptoms had started 2 h before presentation, describing atypical chest pain without dyspnea.
The past history of the patient was unremarkable.
The patient denied any personal history relevant to atypical angina, dyspnea, or other cardiovascular symptoms and any family history of cardiovascular disease.
On physical examination, the significant vital signs were as follows: body mass index of 28.7 kg/m2; heart rate at regular pulse of 80 beats per min; and blood pressure of 163/92 mmHg. Dyspnea, heart murmurs, and other signs of heart failure were absent.
Levels of myocardial injury enzymes (i.e., troponin T and creatine kinase) were normal. Electrocardiography demonstrated a sinus rhythm of 77 beats per min and absence of ST depression with minimal alterations in lateral repolarization.
The patient underwent MDCTA (Aquilion ONE; Toshiba Medical Systems, Otawara, Japan) using the following scan parameters: prospective protocol; gantry rotation time of 350 ms; 512 × 512 matrix; slice thickness of 0.5 mm with 0.25 mm increments using kernel FC03; automatic exposure control (SURE bExposure 3D; Toshiba Medical Systems) (SD 110 for contrast-enhanced images); and iterative reconstruction.
An intravenous contrast (60 mL Iomeron® 400 mg iodine/mL; Bracco Imaging Italy s.r.l., Milan, Italy) was administrated at 5 mL/s flow. Heart rate was set between 50 and 60 beats per min with intravenous administration of metoprolol. The data were transferred to an external workstation (Vitrea2 FX version 6.3; Vital Images, Plymouth, MN, United States) providing multiplanar reformation (commonly referred to as MPR) and volume rendering technique (commonly referred to as VRT).
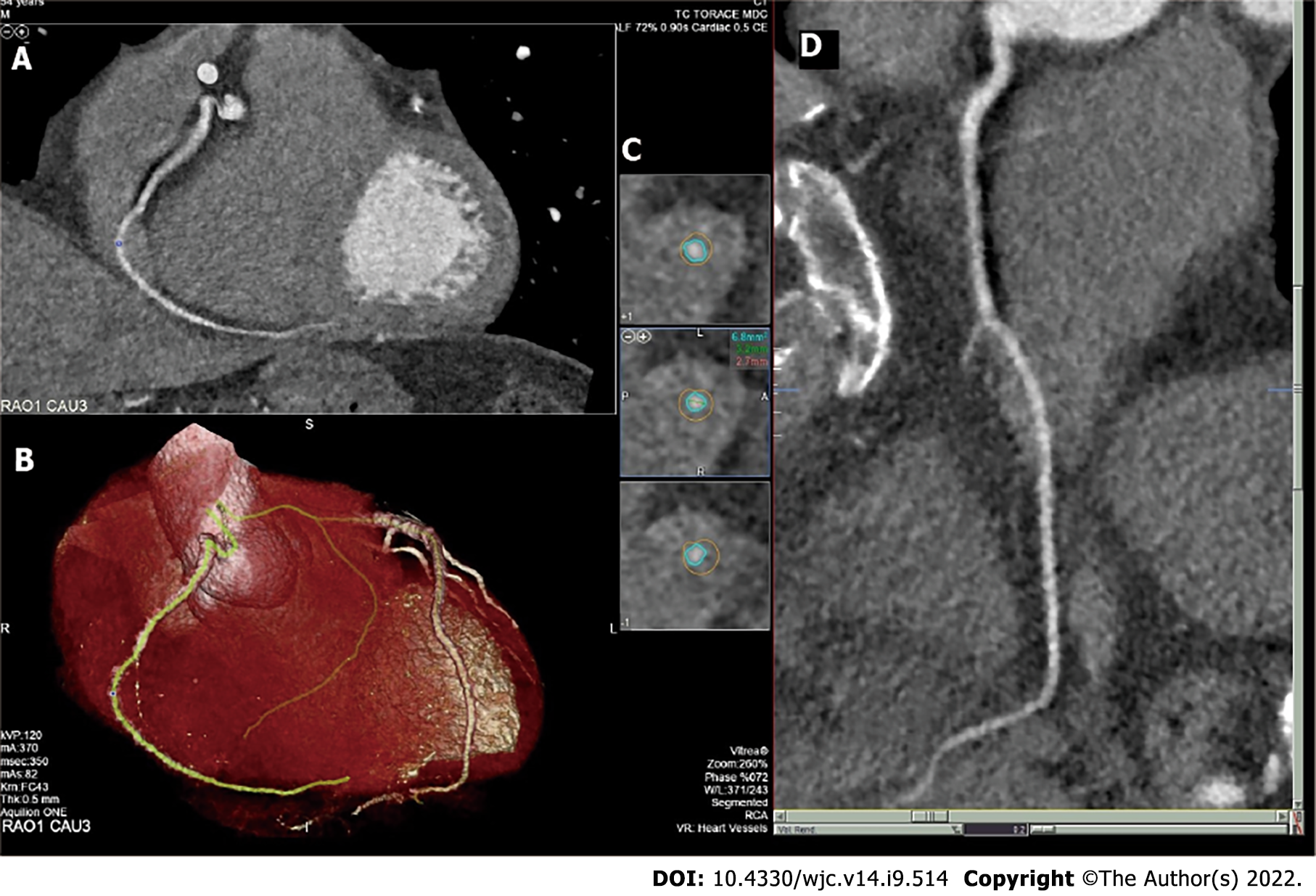
From the scans, mild coronary calcification (Agatston calcium score of 34) of the left anterior descending (LAD) coronary artery, without significant stenoses (> 70%) of all segments, was detected. Additionally, an abnormal course of the mid RCA was identified. As demonstrated by axial images and CT multiplanar reconstruction, the origin and the proximal tract of the RCA were normal, with an epicardial course in the right atrio-ventricular groove; however, the artery penetrated the anterior RA wall and then exhibited an intracavitary course of 25 mm (Figure 1). After the exit from RA, the RCA passed normally in the atrio-ventricular groove and then continued normally at the level of the diaphragmatic crux.
Considering the patient's medical history along with the MDCTA imaging findings, the final diagnosis was an intra-atrial course of the mid RCA without significant coronary atherosclerosis.
The patient responded well to standard medical therapy (i.e., rosuvastatin, administered at 5 mg per day) and was discharged home on postoperative day 2 without having to undergo a conventional angiography study.
At the last follow-up (5 mo postoperatively), the patient was still alive.
RCA anomalies are rare and abnormal courses of the RCA are even more rare, with an incidence of 0.1%[2]. In the literature, an intra-atrial course of the RCA was reported only in 9 autoptic cases[3,4] and in about 80 clinical cases[1,2,5-26] (Table 1). Most clinical cases were case reports, but a few case series were reported[1,2,5,9,10,16,21].
| Ref. | Patients, n | Type | Sex | Age in yr | Risk factors | Symptoms | Imaging | Segment of RCA | Intra-atrial course length in mm | Stenosis, % | Outcome |
| Kolodziej et al[3], 1994 | 3 | Autoptic series | UNK | UNK | UNK | UNK | Postmortem examination | Mid | 15; 20; 30 | No | Mortem |
| Rosamond et al[14], 2007 | 1 | Case report | M | 54 | NR | Palpitation, atrial fibrillation | MDCTA 64 | Distal | 35 | No | No atrial fibrillation |
| Scheffel et al[11], 2007 | 1 | Case report | F | 77 | Hypertension, hyperlipidemia, family history | Atypical chest pain | MDCTA | Mid | 55 | No | NR |
| Zalamea et al[5], 2009 | 2 | Series | F; F | 70; 54 | Atrial fibrillation; Smoker | Dyspnea on exertionChest pain, nausea, diaphoresis | MDCTA | Mid-distal; Mid-distal | 40-50; 55 | No; No | No ablation; NR |
| Andrade et al[6], 2010 | 1 | Case report | M | 46 | Strong family history | No | MDCTA | Mid | 25 | No | NR |
| Lee et al[8], 2010 | 1 | Case report | F | 57 | Hypertension, hyperlipidemia | Atypical chest pain | MDCTA | Mid | 38 | No | Discharged |
| Renapurkar et al[12], 2010 | 1 | Case report | F | 49 | Family history | Atypical chest pain | MDCTA 64 DS | Mid | 10 | No | NR |
| Chou et al[19], 2011 | 1 | Case report | M | 56 | Diabetes, hypertension | Chest tightness | MDCTA | PL | NS | No | Symptoms persistence |
| Christopher and Duraikannu[7], 2011 | 1 | Case report | F | 48 | No | Chest pain, dyspnea, palpitation | MDCTA | Mid | 15 | No | NR |
| Bansal et al[10], 2011 | 2 | Series | NS | NS | NS | NS | MDCTA | Segment 3; Segment 2 | 13.2; 15.6 | NS | NS |
| Zeina[17], 2011 | 1 | Case report | M | 59 | Multiple | Chest pain | MDCTA 64 | Distal | 40 | No | NR |
| Waniewska et al[24], 2012 | 1 | Case report | F | 62 | NR | Atrial flutter, atrial fibrillation, fainting, hypotension | MDCTA | Distal | 50 | No | RFA |
| Opolski et al[9], 2014 | 14 | Series | M:F = 2:12 | 54 (mean) | Diabetes, hypertension, hyperlipidemia, smoker, family history | Atypical chest pain, stable angina pectoris, syncope, dyspnea, palpitations, arrhythmia | MDCTA | Segment 3 (47%); Segment 2 (40%); Segment 1 and 4 (13%) | 29 (mean) | No | Conservative approach |
| Bunkiewicz et al[13], 2015 | 1 | Case report | F | 78 | Hypertension, previous acute coronary syndrome | Not specific chest pain, low tolerance of physical effort, dry cough | MDCTA | Mid | 20 | No | UNK |
| Buckley et al[16], 2017 | 17 | Series | NS | NS | NS | NS | MDCTA | NS | NS | NS | NS |
| Krishnan et al[4], 2017 | 6 | Autoptic series | M | 69 (mean) | NS | UNK | Postmortem examination | Type I: Mid; Type II: Mid; Type III: Anterior branch | Type I: 22 (mean); Type II: 36; Type III: UNK | No | Mortem |
| Ganga et al[20], 2019 | 1 | Case report | M | 45 | NR | Atypical chest pain | MDCTA | Mid | 45 | No | NR |
| Bouhuijzen et al[18], 2019 | 1 | Case report | F | 64 | NR | Atypical chest pain | MDCTA | NS | 40 | No | |
| Hossain et al[2], 2019 | 7 | Series | M:F = 71.4:28.6 | 67.3(mean) | Chest pain (25%), shortness of breath (33%) | Pre-TAVR | MDCTA | NS | 33.4 (mean) | No | No coronary intervention |
| Mahmoud et al[22], 2020 | 1 | Case report | F | 61 | NS | Chest pain | MDCTA | Mid | 39 | NS | NR |
| Junco-Vicente et al[21], 2020 | 3 | Series | 1M; 2F | NS | NS | Chest pain | MDCTA | Mid | 27.7 (mean) | No | UNK |
| Marrone et al[26], 2020 | 1 | Case report | F | 48 | Aortic valve disease | NR | MDCTA | Distal | 49 | No | NR |
| Ganga et al[1], 2021 | 21 | Series | M:F = 1.3:1 | 53.7 (mean) | NR | NR | MDCTA | Mid (16/21); Distal (5/21) | 14.85 (mean) | No | NR |
| Frey et al[23], 2022 | 1 | Case report | M | 55 | Hypertension, hypercholesterolemia, smoker, obesity | Atypical angina, dyspnea | MDCTA | Mid (posterior) | 40 | No | Conservative approach |
| Borges et al[25], 2022 | 1 | Case report | M | 66 | NS | Palpitation, tachycardia, dyspnea | MDCTA | Mid | 30 | No | NR |
| Barbiero et al | 1 | Case report | M | 54 | Hypertension, hyperlipidemia, smoker | Atypical chest pain | MDCTA | Mid | 25 | No | Medical treatment |
An intra-atrial course of RCA was first described in 1975 by McAlpine[27]. The prevalence of this variant was initially reported to be between 0.09% and 0.1%[5-7], but these rates probably represented underestimations because the conventional angiographic luminographic 2D assessment may not be able to recognize this abnormal variant. The most recent studies – involving cases that are being diagnosed by the new advanced imaging techniques – have reported a prevalence of 1.3%[2] and 1.8%[4]; certainly, the increasing use of MDCTA of the coronary arteries will lead to an even greater increase in identification of this anomaly[8].
Reportedly, the segments of the RCA most frequently involving an intra-atrial course were segments 3 (47%) and 2 (40%)[9], with mean length ranging from 14 mm to 53 mm[9]. In our perusal of the literature, the most frequent intra-atrial segment of the RCA reported was the mid segment (Table 1), with a length of intra-atrial RCA ranging from 13.2 mm[10] to 55 mm[5]. Rarely, the intra-atrial course of the RCA involved segments 1 and 4 (13%)[9] or has lengths shorter (as low as 13 mm) or longer (up to 55 mm)[10-12].
In our review of the literature, most cases were female, and the patient’s ages ranged from 45 years[20] to 78 years[13]. In none of the cases was there presence of significant coronary artery stenoses nor were mild atherosclerotic plaques indicated[9]. A possible explanation could be the absence of mechanical stress on the segment of the coronary artery when it coursed intra-atrially or intra-myocardially rather than in the epicardial fat, although this conclusion is not definitive[9].
Association between the intra-cavitary course of the RCA and other coronary anomalies have been described, such as with the intramuscular course of the LAD coronary artery or with the anomalous origin of the left circumflex (commonly known as LCX) coronary artery from the right aortic sinus[9]. Patients with intra-cavitary course of the RCA were usually asymptomatic, and its discovery was incidentally encountered during an MDCTA coronary study conducted for other reasons (i.e., atypical chest pain, chest tightness, dyspnea, palpitation, atrial flutter or fibrillation, arrhythmia, fainting, hypotension, or syncope) (Table 1).
An intracavitary course of the RCA has a higher probability of iatrogenic damage than myocardial bridging because of the risk of direct injury at the abnormal vessel segment during surgical manipulation or endoatrial procedures (i.e., ablation, catheterization, or electrode implantation). Therefore, although it is usually considered an asymptomatic variant, its early recognition is crucial to avoid vessel catastrophic lesions during such procedures[2].
MDCTA is a less invasive and less user-dependent method than conventional angiography and can accurately depict the coronary vasculature and its variants of origin, termination, or course[2]. The recognition of an intra-atrial course of the RCA by MDCTA could facilitate avoidance of potential hazards during surgical and/or interventional procedures.
Provenance and peer review: Unsolicited article; Externally peer reviewed.
Peer-review model: Single blind
Specialty type: Cardiac and cardiovascular systems
Country/Territory of origin: Italy
Peer-review report’s scientific quality classification
Grade A (Excellent): 0
Grade B (Very good): B
Grade C (Good): C
Grade D (Fair): 0
Grade E (Poor): 0
P-Reviewer: Hakimi T, Afghanistan; Pan SL, China S-Editor: Wu YXJ L-Editor: A P-Editor: Wu YXJ
| 1. | Ganga KP, Ojha V, Goyal A, Deepti S, Kumar S. Intra-atrial right coronary artery on dual-source CT: prevalence and characteristics. Diagn Interv Radiol. 2021;27:595-598. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 2] [Cited by in RCA: 3] [Article Influence: 0.8] [Reference Citation Analysis (0)] |
| 2. | Hossain R, Chelala L, Amin SB, Bergquist PJ, Vairavamurthy J, Jeudy J, White CS. Intracavitary Coronary Artery: An Unusual Coronary Anomaly. J Thorac Imaging. 2019;34:W121-W124. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 2] [Cited by in RCA: 2] [Article Influence: 0.3] [Reference Citation Analysis (0)] |
| 3. | Kolodziej AW, Lobo FV, Walley VM. Intra-atrial course of the right coronary artery and its branches. Can J Cardiol. 1994;10:263-267. [PubMed] |
| 4. | Krishnan B, Cross C, Dykoski R, Benditt DG, Mbai M, McFalls E, Li JM, Bertog S, Tholakanahalli VN. Intra-Atrial Right Coronary Artery and its Ablation Implications. JACC Clin Electrophysiol. 2017;3:1037-1045. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 4] [Cited by in RCA: 4] [Article Influence: 0.5] [Reference Citation Analysis (0)] |
| 5. | Zalamea RM, Entrikin DW, Wannenburg T, Carr JJ. Anomalous intracavitary right coronary artery shown by cardiac CT: a potential hazard to be aware of before various interventions. J Cardiovasc Comput Tomogr. 2009;3:57-61. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 12] [Cited by in RCA: 10] [Article Influence: 0.6] [Reference Citation Analysis (0)] |
| 6. | Andrade JG, Heilbron BG, Leipsic JA. Intracavitary right coronary artery. Can J Cardiol. 2010;26:211-212. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 10] [Cited by in RCA: 10] [Article Influence: 0.7] [Reference Citation Analysis (0)] |
| 7. | Christopher J, Duraikannu C. Case report: Intra-atrial course of right coronary artery: Evaluation by dual-source CT. Indian J Radiol Imaging. 2011;21:57-59. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 6] [Cited by in RCA: 7] [Article Influence: 0.5] [Reference Citation Analysis (0)] |
| 8. | Lee YS, Bastarrika G, Schoepf UJ. Intra-atrial course of the right coronary artery demonstrated at computed tomography coronary angiography. J Thorac Imaging. 2010;25:W115-W117. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 3] [Cited by in RCA: 4] [Article Influence: 0.3] [Reference Citation Analysis (0)] |
| 9. | Opolski MP, Pregowski J, Kruk M, Staruch AD, Witkowski A, Demkow M, Hryniewiecki T, Michalek P, Ruzyllo W, Kepka C. The prevalence and characteristics of intra-atrial right coronary artery anomaly in 9,284 patients referred for coronary computed tomography angiography. Eur J Radiol. 2014;83:1129-1134. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 7] [Cited by in RCA: 7] [Article Influence: 0.6] [Reference Citation Analysis (0)] |
| 10. | Bansal A, D'souza MM, Tripathi RP. Intracavitary course of right coronary artery. Indian J Radiol Imaging. 2011;21:238-239. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 1] [Cited by in RCA: 1] [Article Influence: 0.1] [Reference Citation Analysis (0)] |
| 11. | Scheffel H, Vetter W, Alkadhi H. Intra-atrial course of the right coronary artery: a previously missed anomaly. Eur Heart J. 2007;28:1919. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 7] [Cited by in RCA: 7] [Article Influence: 0.4] [Reference Citation Analysis (0)] |
| 12. | Renapurkar R, Desai MY, Curtin RJ. Intracavitary course of the right coronary artery: an increasingly recognized anomaly by coronary computed tomography angiography. J Thorac Imaging. 2010;25:W77-W78. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 5] [Cited by in RCA: 6] [Article Influence: 0.4] [Reference Citation Analysis (0)] |
| 13. | Bunkiewicz L, Niklas AA, Juszkat R, Niklas K, Tykarski A. Intra-atrial course of the right coronary artery: an uncommon anomaly diagnosed by coronary computed tomography angiography. Kardiol Pol. 2015;73:61. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1] [Cited by in RCA: 1] [Article Influence: 0.1] [Reference Citation Analysis (0)] |
| 14. | Rosamond T, Wetzel LH, Lakkireddy D, Ferrell R, Tadros P. IntraCameral right coronary artery: detection by 64 slice coronary computed tomographic angiography and implications for radiofrequency ablation of atrial dysrhythmias. Pacing Clin Electrophysiol. 2007;30:1571-1574. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 10] [Cited by in RCA: 10] [Article Influence: 0.6] [Reference Citation Analysis (0)] |
| 15. | Bansal A, D'souza MM, Wardhan H, Tripathi RP. Intra-cavitary course of right coronary artery: what the cardiologists should be aware of! Indian Heart J. 2011;63:475-476. [PubMed] |
| 16. | Buckley CM, Rosamond T, Hegde SR, Wetzel L. The intracavitary coronary artery: a rare anomaly with implications for invasive cardiac procedures – demonstration by coronary computed tomography angiography. J Am Coll Cardiol. 2017;69:1437. [RCA] [DOI] [Full Text] [Cited by in Crossref: 4] [Cited by in RCA: 4] [Article Influence: 0.5] [Reference Citation Analysis (0)] |
| 17. | Zeina AR. Anomalous intracavitary right coronary artery detected with cardiac computed tomography angiography: a rare but potentially lethal coronary anomaly. J Cardiovasc Med (Hagerstown). 2011;12:345-346. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 4] [Cited by in RCA: 4] [Article Influence: 0.3] [Reference Citation Analysis (0)] |
| 18. | Bouhuijzen LJ, Kardux JJ, Braam RL. Intracavitary course of right coronary artery. Neth Heart J. 2019;27:335-336. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 1] [Cited by in RCA: 1] [Article Influence: 0.2] [Reference Citation Analysis (0)] |
| 19. | Chou HP, Chen CK, Sheu MH, Wu MH. Anomaly of right coronary artery with intra-atrial course. Eur J Cardiothorac Surg. 2011;40:e67. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1] [Cited by in RCA: 1] [Article Influence: 0.1] [Reference Citation Analysis (0)] |
| 20. | Ganga KP, Ojha V, Shaw M, Kumar S. Intra-atrial course of the right coronary artery: depiction of a potentially hazardous entity on dual-source CT. BMJ Case Rep. 2019;12. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 3] [Cited by in RCA: 3] [Article Influence: 0.5] [Reference Citation Analysis (1)] |
| 21. | Junco-Vicente A, Martin-Fernandez M, Fidalgo-Argüelles A, Cigarran-Sexto H. Intra-atrial path of the right coronary artery: An infrequent and still unknown anomaly. Anatol J Cardiol. 2020;23:E15-E16. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 1] [Cited by in RCA: 1] [Article Influence: 0.2] [Reference Citation Analysis (1)] |
| 22. | Mahmoud O, Durr B, Alsaid A. Intra-Atrial Course of the Right Coronary Artery. Methodist Debakey Cardiovasc J. 2020;16:323. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 2] [Cited by in RCA: 2] [Article Influence: 0.4] [Reference Citation Analysis (0)] |
| 23. | Frey SM, Brantner P, Gehweiler J, Madaffari A, Zellweger MJ, Haaf P. 3D-printed visualization of a double right coronary artery with intra-atrial course. Int J Cardiovasc Imaging. 2022;38:709-710. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 1] [Cited by in RCA: 1] [Article Influence: 0.3] [Reference Citation Analysis (0)] |
| 24. | Waniewska J, Michałowska I, Oleksiuk T, Kwiatek P. Intra-atrial course of right coronary artery - case report. Pol J Radiol. 2012;77:58-59. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 2] [Cited by in RCA: 2] [Article Influence: 0.2] [Reference Citation Analysis (1)] |
| 25. | Borges SCDS, Carvalho CIR, Gonçalves METM, Baptista AIS, Moreira JI. Intracavitary Right Coronary Artery: An Incidental Finding with Potential Implications for Invasive Cardiac Procedures. Arq Bras Cardiol. 2022;118:1000-1001. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 1] [Cited by in RCA: 1] [Article Influence: 0.3] [Reference Citation Analysis (1)] |
| 26. | Marrone G, Crino F, Mamone G, Gentile G, Caruso S. Intracavitary right coronary artery. Eur Heart J Cardiovasc Imaging. 2020;21:935. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1] [Cited by in RCA: 1] [Article Influence: 0.2] [Reference Citation Analysis (1)] |
| 27. | McAlpine WA. Hearth and coronary arteries. Anatomical atlas for clinical diagnosis, radiological investigation and surgical treatment. New York: Springer-Verlag, 1975: 186-187. [RCA] [DOI] [Full Text] [Cited by in Crossref: 1] [Cited by in RCA: 1] [Article Influence: 0.0] [Reference Citation Analysis (1)] |