Published online Aug 26, 2015. doi: 10.4331/wjbc.v6.i3.71
Peer-review started: January 30, 2015
First decision: March 6, 2015
Revised: March 30, 2015
Accepted: June 15, 2015
Article in press: June 16, 2015
Published online: August 26, 2015
Processing time: 208 Days and 17.5 Hours
The lack of newly developed antibiotics, together with the increase in multi-resistance of relevant pathogenic bacteria in the last decades, represents an alarming signal for human health care worldwide. The number of severely infected persons increases not only in developing but also in highly industrialized countries. This relates in first line to the most severe form of a bacterial infection, sepsis and the septic shock syndrome, with high mortality on critical care units. No particular anti-sepsis drug is available, and the therapy with conventional antibiotics more and more fails to provide a survival benefit. Due to the fact that the pharmaceutical industry has withdrawn to a high degree from the development of anti-infectious agents, a huge challenge for health care is approaching in the 21st century. In this article, these problems are outlined and possible alternatives are presented which may be helpful to solve the problem.
Core tip: The dramatic increase in multiresistance of relevant pathogenic bacteria can be assumed to be one of the main global health care problems of the 21st century. At the same time, the development of new antibiotics decreases considerably from which a significant lack in the health supply for combating infections can be scheduled. In this paper, alternative strategies are discussed which are focused mainly on the development and application of antimicrobial peptides. These can easily be synthesized in high amounts under moderate costs, have usually a high therapeutic index, and do not have a tendency for resistance emergence. Recent developments are presented from which it may be deduced that the most serious form of a bacterial infection, sepsis and septic shock, may be treatable in near future.
- Citation: Brandenburg K, Schürholz T. Lack of new antiinfective agents: Passing into the pre-antibiotic age? World J Biol Chem 2015; 6(3): 71-77
- URL: https://www.wjgnet.com/1949-8454/full/v6/i3/71.htm
- DOI: https://dx.doi.org/10.4331/wjbc.v6.i3.71
The assessment of infections has changed completely in the last 30 years. Up to the 1980’s it was believed that all bacterial infections were controllable with antibiotics: “It’s time to close the book of infectious diseases”[1]. But already at the end of the 1990’s, the general view changed: “Bacterial infections are a worldwide threatening of human health, in developed states they are the third frequent, in countries of the Third World “even the most frequent cause of death”[2].
These new assessments can be summarized in the statement: “Bacterial infections are the largest health care challenges of the 21st century”.
The reasons for this paradigm change are complex. One of the main reasons is certainly the drastic increase in bacterial resistance: The occurrence of bacterial drug resistance, which is - among others - caused by wrong antibiotic medication and the excessive use of antibiotics in animal husbandry, represents an increasing threatening for human health. This situation is communicated also more and more in the media, for example in a contribution by the well-renowned British BBC[3]. The uncontrolled emission of antibiotics in mass animal husbandry, leading to a contamination of the soils and the water, represents a selection pressure on bacteria from the environment such as Staphylococcus aureus (S. aureus) and Pseudomonas aeruginosa (P. aeruginosa) with subsequent increase in resistance. As examples for the increase in resistance, it should be stated that more than 90% of the S. aureus strains are resistant to all penicillins and other related antibiotics, and many, i.e., around 30% nowadays with increasing tendency, are resistant even to the newer methycillin-related drugs (MRSA). Further relevant resistant germs with high infection potential are beside MRSA, vancomycin-resistant Enterococci, fluorquinon-resistant P. aeruginosa, and ESBL (extended spectrum beta-lactamase)-resistant Escherichia coli and Klebsiella pneumonia. Infections induced by multiresistant strains frequently lead to heavy infections, for example to wound, urinary, and respiratory infections which finally may lead to the life-threatening sepsis syndrome with multi-organ failure.
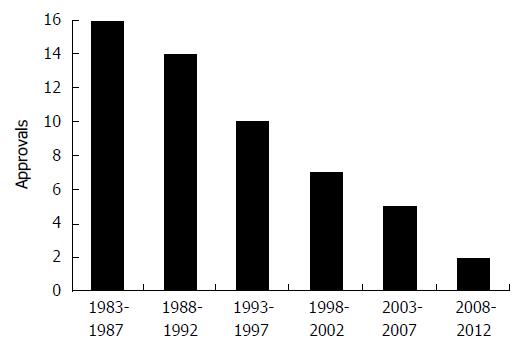
More than 100000 patients suffer annually from MRSA infections in Germany, with a mortality rate of up to 10% by sepsis or pneumonia (“Deutsche-Sepsisgesellschaft”)[4]. Very important germs with high infection and mortality potential are also the MDR (multi-drug resistant). Mycobacterium tuberculosis strains (MDRMt). These are in particular in Eastern Europa a huge threatening of human health, which does not lead to short-time infections as described above but to a long-term infirmity of infected people with a high death-rate. For these bacteria, in contrast to those described above, even the bioactive compounds from their cell wall have not been characterized so far. Another reason for the paradigm change mentioned above is that in the last decades pharmaceutical companies have brought to market only two new classes of antibiotics, which moreover have only effects against particular bacteria. This situation is expressed by the statement: “We are facing a huge crisis worldwide not having an antibiotics pipeline”. (Dr. Janet Woodcock, Director of CDER at FDA)[5]. The lack in the development of new antibiotics is illustrated in Figure 1 showing a dramatic decrease of newly approved compounds.
There is no evidence that this situation will change. In the pipeline of the pharmaceutical industry no broad-band developments are reported. This fact leads to ironic or even sarcastic formulations from experts such as the following: Who Will Mourn the Passing of the Pharmaceutical Industry[7]?
Details of “Medicines in Development” against a variety of bacterial and viral infections, mostly by small Biotech companies, is found in the 2013 report[8].
The failure of the pharmaceutical industry to develop new antibiotics has of course a rational background: The development of anti-infective drugs is a very laborious, long-lasting, and expensive procedure, and is frequently “crowned” by failure[9]: Thus, for example, the development of an effective anti-sepsis medicament (see below) has been described as “Money graveyard” for pharmaceutical companies, because in more than 20 clinical phases III there was no survival benefit for patients, but the companies had invested overall some billion $. Thus, drug development is targeted to fulfill primarily the promise of the return of investment rather than creating new anti-infective drugs.
Bacterial infections may give rise to a variety of different diseases, from harmless local infections affording no treatment over more severe local infections such as skin and skin-related infections up to the most severe form, the sepsis. In contrast to other infections such as respiratory or urogenital tract diseases, sepsis is a systemic disease, i.e., it is spreading over the blood stream. For this, no particular drug is available since the withdrawal of Drotrecogin-α (recombinant protein C, Xigris®) in October 2012, which anyway was only suitable for a small number of patients. The numbers known from the USA may give a hint regarding the high relevance of the septic syndrome in health care, when compared with the data from other diseases: annual death cases United States: Sepsis 215000; Myocardial Infarction 193000, Lung cancer 153000.
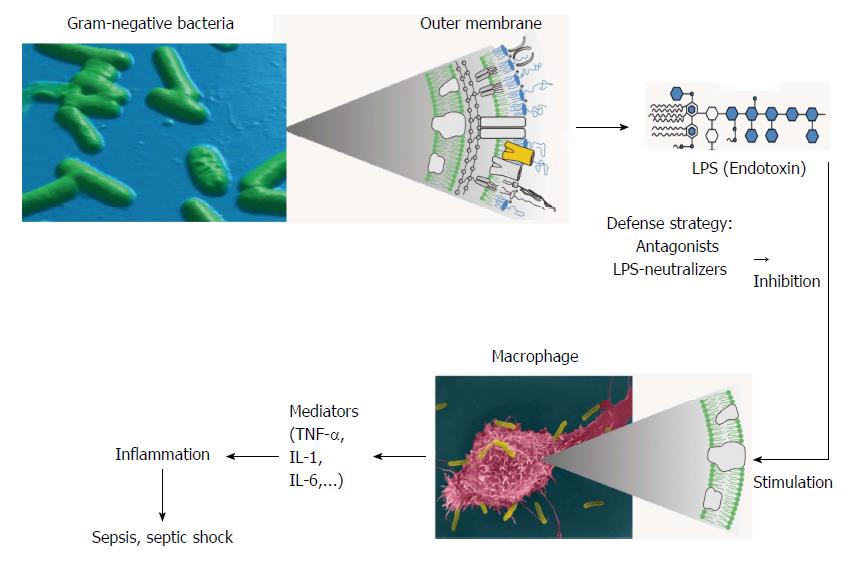
In selected video presentations, the dramatic kind of occurrence and frequency of sepsis are presented most impressive[10,11]. It is well known that septic shock may occur for patients, whose bodies are weakened due to other traumata (heavy burns, accidents, surgery, etc.), who have a priori a weak immune system, or who are infected due to unfortunate reasons (even an inaccurate treatment of a tooth may lead to sepsis because bacteria from the mouth may infiltrate the bloodstream). It is important to note that not the bacteria and their toxins, but rather the overshooting reaction of the body to these stimuli is responsible for the induction of the sepsis syndrome. Whereas the presence of the inflammation-inducing bacterial “pathogenicity factors” (PFs) such as endotoxin [lipopolysaccharide (LPS)] for Gram-negative and lipoprotein (LP) from Gram-positive source at low concentrations is beneficial for the immune system in particular in the early childhood, the negative consequences at high concentrations lead to the well-known cytokine storm (Figure 2)[12].
The lack in progress in the fight against sepsis has not changed during the last decades, however, the occurrence of drug-resistant strains has severely worsened the situation. Whereas for the drug-susceptible bacteria an elaborate therapy by applying suitable antibiotics and “adjunctive” and “volume replacement” procedures in critical care units may lead to some therapeutic success, bacteria such as MRSA and ESBL - resistant strains from Escherichia coli and Klebsiella pneumonia cannot be treated adequately. Even if the immune system is potent enough to combat the bacterial invasion, the release of the bacterial toxins LPS and LP from the cell envelopes of bacteria induces the immunity to go haywire. These toxins react with cells of the immune system in a heavy way by producing so-called cytokines (mediators), which leads to a self-poisoning of the body. As shown in Figure 2, the liberation of LPS - which may take place by the action of the immune system or only by cell division of the bacteria - from the bacterial outer membrane is responsible for the heavy inflammation reaction by interacting with cell receptors, as shown here on macrophages (for LPS: Toll-like receptor 4, for LP: Toll-like receptor 2), with subsequent cell signaling.
In Figure 2 also possible intervention strategies are depicted, like antibacterial drugs, LPS neutralizers, and protein antagonists such as antibodies (see below).
Even if suitable antibiotics would be available, this frequently does not necessarily improve the health of the patients, but in contrary may worsen their state, because due to bacterial killing the bacterial toxins are now released from the bacterial cell envelopes with a severe increase in the inflammation reaction. “There are more and more results from animal models and from clinical studies that the antibiotic-induced release of biologically active LPS leads to a worsening of the critical state of septic patients”[13].
A detailed characterization of the terms and symptoms, which may occur in humans due to a systemic inflammation is given in the Table 1.
| Term | Definition |
| Endotoxemia | Occurrence of Lipopolysaccharide (Endotoxin) in Blood |
| Bacteremia | Occurrence of living bacteria in blood |
| SIRS | Generalized hyperinflammatory reaction with different causes, Infections, Burns, Traumata |
| Sepsis | SIRS induced by an infection |
| Severe Sepsis | Sepsis with organ dysfunction |
| Septic Shock | Sepsis with shock |
Regarding all previous efforts for the development of anti-septic compounds, the corresponding experimental therapies have failed to improve the clinical outcome of severe sepsis and septic shock, and sometimes even increased mortality. The targets of current and past anti-septic strategies can be divided into five categories[9]: (1) Cell-signaling; (2) Coagulation pathway; (3) Endotoxin; (4) Immunomodulation; and (5) Specific mediators.
From the analysis of published data it can be deduced that seven agents yielded at least some improvement in clinical trials: a high-dose corticosteroid, two anti-endo-toxin therapies, a human recombinant IL-1 receptor antagonist, an intensive insulin therapy, an intravenous immunoglobulin, and a recombinant activated protein C10.
High dose corticosteroids, have been used until 1989. At the beginning, the compounds actually showed some survival benefit, but further analyses revealed that the survival rate in patients with septic shock was even lowered[14]. IL-1 receptor antagonists were used until 1997 and again showed a survival benefit at first, which could not be confirmed in follow-up trials. The same applies to monoclonal anti-TNFα antibodies (afemilomab, Abbott), which showed some positive effects, but no overall increase in survival. The use of anti-IFNγ antibodies (INNO-202, Innogenetics) showed some benefit in monkeys (reported in 2003), but for unknown reasons was not further pursued through clinical studies. Intensive insulin therapy (IIT) is not recommended at this time because the first encouraging results could not be transferred to other ICU-populations. Furthermore, the application of IIT resulted in significant harm to patients by severe hypoglycemia.
Details of the numerous attempts for combating sepsis and the reasons of failure are described by Fink and Shaw Warren[15].
The common problem of the strategies mentioned above is that all concepts (with the exception of compounds that are targeting the bacteria’s endotoxins) do only tackle some aspects of severe sepsis rather than addressing the body’s whole inflammatory state, triggered by bacteria or rather bacterial PFs. Accordingly, these strategies had been - at best - only be partially successful.
An alternative approach relates to immunomodulation mediated by short peptides to bolster host immunity, rather than reacting directly with bacteria or their PFs. Representative compounds are defensins, cathelicidins, dermicines and derivatives thereof, which are able to stimulate the expression of cytokines and chemokines. Some data indicate that these peptides may modulate the inflammatory cascade by targeting multiple inflammatory mediators, which may lead, among others, to an alteration of cell membrane function connected with the inhibition of TLR4 signaling induced by LPS. However, no data are available that would indicate their clinical usefulness in sepsis.
The latest failed clinical trials concern two in preclinical investigations very promising compounds, talactoferrin, a recombinant lactoferrin produced by Agennix, and the LPS-antagonist Eritoran by EISAI corporation. Both compounds did not succeed in phase III studies, an explanation may be with the former compound that talactoferrin is focused mainly on Gram-negative bacteria, but may not have enough potential to neutralize endotoxins (see, e.g.[16]), and with the latter that LPS-antagonists of course cannot act against Gram-positive bacteria and their toxins.
Presently, only two anti-septic compounds are under development. The approach by Medinox (United States) is in phase I/II and exploits the compound NOX100 (Irish Pharm. Healthcare Assoc., 2010), which is believed to neutralize excessive NO produced during inflammation. Again, only one side-aspect of bacterial sepsis is addressed, and accordingly, it is unlikely that the compound will be broadly efficacious and of benefit for sepsis patients. Similar applies to compound cyto-FAB (anti-TNF, AstraZeneca), which has entered clinical phase II trials (Irish Pharm. Healthcare Assoc., 2010). The current therapeutic situation is best described by the following statement: “Mostly old therapeutic concepts in a ‘new design’ are currently pursued, although it has been reported that 395 medicines and vaccines are under clinical evaluation, with 88 of them denoted as antibiotics/antibacterials”[8]. As can be concluded from the above, an efficacious and safe anti-septic drug is yet to be developed.
At the beginning of the 1990’s, more and more investigators focused on the design and synthesis of antimicrobial peptides (AMP) in the fight against bacteria and their toxins, mainly based on the use of endogenous (body-own) AMPs such as cathelicidins, defensins, and dermicins. Up to now, these activities have not led to a newly approved drug, except for daptomycin, a lipopeptide which acts only against Gram-positive bacteria. The reasons for the inefficacy are manifold: AMPs are efficacious mucosal factors, but naturally never exposed to the systemic environment, rendering them inherently toxic at concentrations required to bind the bacteria and their toxins when used systemically. A second point is the fact that the bacterial surface structures, which are the first line of attack for the AMPs, show so many variations that not a single compound is able to act as broad-band drug. Nearly all of these approaches were directed against bacteria.
We have chosen another approach: Our rational was to engineer simpler, smaller synthetic polypeptides, which are essentially non-toxic, but still capable of binding PFs. Originally based on comprehensive biophysical studies of natural occurring antimicrobial proteins (e.g., cyclic peptides from anti-Limulus factor, shortened peptide variants from human lactoferrin, porcine NK-lysine, human granulysin), we have developed a new class of synthetic polypeptides (lead compound: Aspidasept®), which possess potent antibacterial activities. These were originally scheduled to bind to and neutralize the lipid A part of Gram-negative LPS, but in the meantime could be shown also to neutralize Gram-positive lipopeptides/proteins[17-19] (a neutralization of peptidoglycan and lipoteichoic acid could also be observed, but it can be highly doubted that these are relevant PFs, as still proposed[20]).
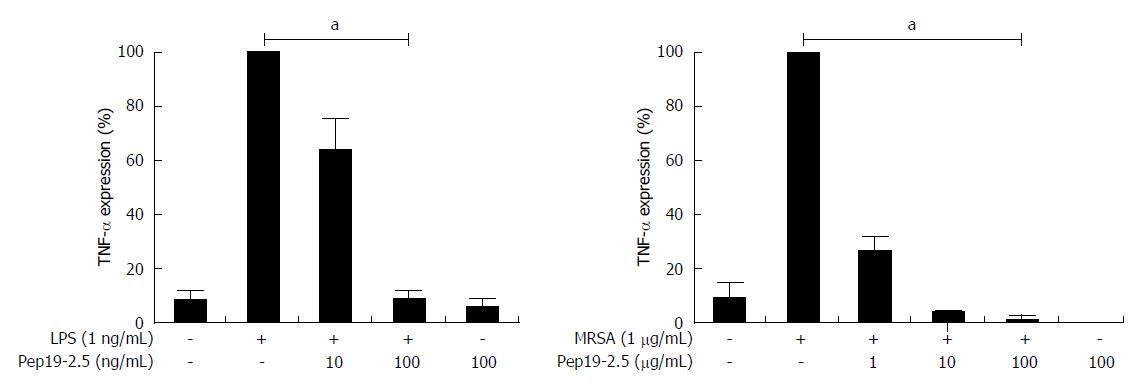
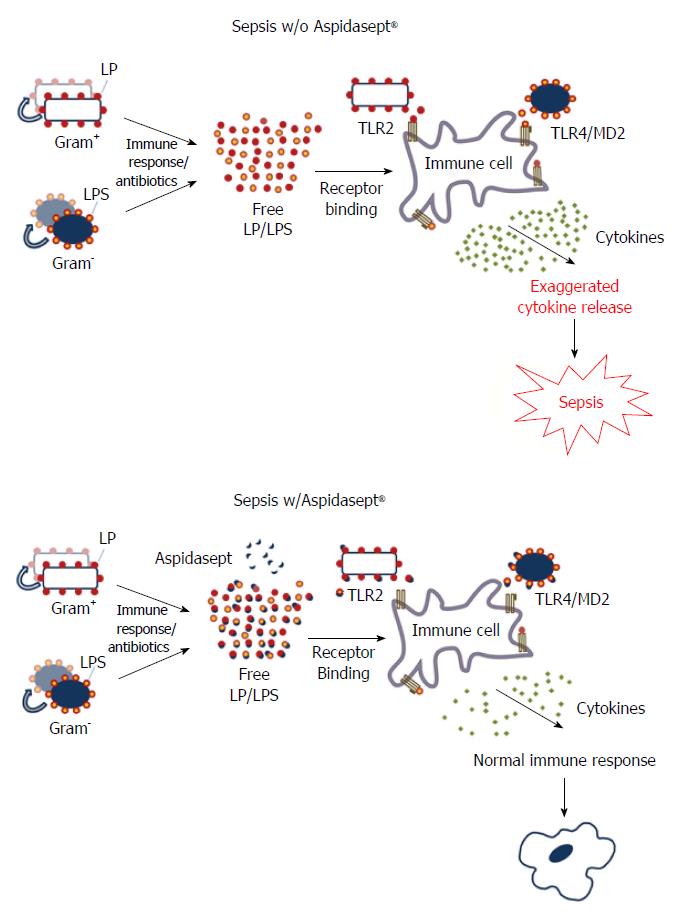
The neutralization of the PFs from nearly all bacteria prevents the over-shooting inflammation reactions induced by these during sepsis. A variety of in vitro, in vivo and ex vivo data is indicative of high inflammation-decreasing activity and efficient protection (e.g., strong weakening of infections, increased survival). As example for the inhibition of the inflammation reaction, in Figure 3 data from an ex vivo model of the human lung are presented. A schematic view on the processes taking place in human blood in the absence (up) and presence (down) of Aspidasept® are shown in Figure 4.
Aspidasept’s scheduled therapeutic concentrations in sepsis patients are far below the concentrations at which side effects (“no observed adverse effect level”, NOAEL) do occur. In fact, experiments in rats by a CRO (contract research organization) which have been conducted in accordance to ICH guideline M3, revealed that at a concentration of 0.5 mg/kg per day with infusions for 14 d no toxic effects were found. Therefore, this concentration is within the NOAEL. At 3.2 mg/kg per day, slight toxic effect occurred, indicating that this belongs to the MTD (maximum tolerated dose). Both concentrations are more than 200-fold higher than the scheduled concentration in septic patients. Therefore, these data provide for the first time the opportunity to develop an equally safe and efficacious medication against sepsis.
It cannot be expected that in the next decades new effective broad-band antibiotics will enter the market. Since the increase in multi-resistance and the demographic development - with a growing proportion of elder people - will continue, a huge burden to the health care system can be supposed. Therefore, to solve the urgent problems concomitant with lack of new medicaments and increasing resistance, new approaches must be developed. The presented data of antimicrobial peptides with high efficiency to neutralize the bacterial toxins may be one chance for the future. Whether this development will be the only promising approach, is unclear. However, one of the main arguments for the development of AMP is the rather simple and cheap synthesis up to very large scales (kg). In upcoming clinical trials it should turn out whether the highly successful preclinical data in vitro, in vivo, and ex vivo can be confirmed successfully also for septic patients as significant decrease in lethality. This would be the first therapeutical approach with antimicrobial peptides in clinical practice. A success would be also insofar important, since development of resistance against these AMPs is less probable.
P- Reviewer: Hu QH, Wang P S- Editor: Tian YL L- Editor: A E- Editor: Wang CH
| 1. | World Health Organization. WHO Report on Global Surveillance of Epidemic-prone Infectious Diseases - Introduction. Available from: http://www.who.int/csr/resources/publications/introduction/en/. |
| 2. | Hughes JM. Policy and Politics in Nursing and Health Care (eBook). Mason DJ, Leavitt JK, Chaffee MW, editors. 6th ed. USA: Elsevier Health Sciences 2014; . |
| 3. | British Broadcasting Corporation. Antibiotics resistance ‘as big a risk as terrorism’ - medical chief. [accessed 2013 March 11]. Available from: http://www.bbc.com/news/health-21737844. |
| 4. | Prevention and control of MRSA (bilingual). Available from: http://www.krankenhaushygiene.de/Nutzerdaten/File/empfehlungen/2010_rki_mrsa.pdf. |
| 5. | Woodcock J. Re-Entering Antibacterial Drug Development Summit. 2015 Nov 16-18; Hilton Back Bay Boston, Boston, MA. Available from: http://www.healthtech.com/Antibacterial-Drug-Development/. |
| 6. | Boucher HW, Talbot GH, Benjamin DK, Bradley J, Guidos RJ, Jones RN, Murray BE, Bonomo RA, Gilbert D. 10 x ‘20 Progress--development of new drugs active against gram-negative bacilli: an update from the Infectious Diseases Society of America. Clin Infect Dis. 2013;56:1685-1694. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 559] [Cited by in RCA: 529] [Article Influence: 44.1] [Reference Citation Analysis (0)] |
| 7. | Projan SJ. Sepsis und antibiotika-induzierte Freisetzung von Endotoxinen. Available from: http://www.p-e-g.de/publikationen/ctj/0599/SEPSIS.PDF. |
| 8. | America’s Biopharmaceutical Research Companies. Biopharmaceutical Research Evolves Against Infectious Diseases with Nearly 400 Medicines and Vaccines in Testing. Available from: http://www.phrma.org/sites/default/files/pdf/MedsInDevInfectiousDiseases2013.pdf. |
| 9. | Seam N, Suffredini AF. Mechanisms of sepsis and insights from clinical trials. Drug Discov Today Dis Mech. 2007;4:83-93. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 15] [Cited by in RCA: 15] [Article Influence: 0.8] [Reference Citation Analysis (0)] |
| 10. | Sepsis Alliance. Introduction To Sepsis Alliance. Available from: https://www.youtube.com/watch?v=Sd5WPJ_U2TU. |
| 11. | Sepsis Alliance. Sepsis: EmergencyTM. Available from: https://www.youtube.com/watch?v=DnsQ4RlXsZY. |
| 12. | Alexander C, Rietschel ET. Bacterial lipopolysaccharides and innate immunity. J Endotoxin Res. 2001;7:167-202. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 129] [Cited by in RCA: 142] [Article Influence: 6.2] [Reference Citation Analysis (0)] |
| 13. | Heinemann M, Trautmann M. Sepsis und Antibiotika-induzierte Freisetzung von Endotoxinen. Konsequenzen für die Therapie? Chemotherapie. 1999;8:176-182. |
| 14. | Walmrath D, Grimminger F, Seeger W. [Severe sepsis--new therapeutic options]. Internist (Berl). 2001;42:1619-1620, 1623-1630. [PubMed] |
| 15. | Fink MP, Warren HS. Strategies to improve drug development for sepsis. Nat Rev Drug Discov. 2014;13:741-758. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 161] [Cited by in RCA: 193] [Article Influence: 17.5] [Reference Citation Analysis (0)] |
| 16. | Brandenburg K, Jürgens G, Müller M, Fukuoka S, Koch MH. Biophysical characterization of lipopolysaccharide and lipid A inactivation by lactoferrin. Biol Chem. 2001;382:1215-1225. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 89] [Cited by in RCA: 98] [Article Influence: 4.1] [Reference Citation Analysis (0)] |
| 17. | Gutsmann T, Razquin-Olazarán I, Kowalski I, Kaconis Y, Howe J, Bartels R, Hornef M, Schürholz T, Rössle M, Sanchez-Gómez S. New antiseptic peptides to protect against endotoxin-mediated shock. Antimicrob Agents Chemother. 2010;54:3817-3824. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 90] [Cited by in RCA: 101] [Article Influence: 6.7] [Reference Citation Analysis (0)] |
| 18. | Schürholz T, Heinbockel L, Martinez de Tejada G, Hornef M, Marx G, Brandenburg K. Neue Sepsistherapie am Horizont: Antiinflammatorische Peptide. DIVI. 2013;4:144-152. |
| 19. | Heinbockel L, Sánchez-Gómez S, Martinez de Tejada G, Dömming S, Brandenburg J, Kaconis Y, Hornef M, Dupont A, Marwitz S, Goldmann T. Preclinical investigations reveal the broad-spectrum neutralizing activity of peptide Pep19-2.5 on bacterial pathogenicity factors. Antimicrob Agents Chemother. 2013;57:1480-1487. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 64] [Cited by in RCA: 71] [Article Influence: 5.9] [Reference Citation Analysis (0)] |
| 20. | Reinhart K, Bauer M, Riedemann NC, Hartog CS. New approaches to sepsis: molecular diagnostics and biomarkers. Clin Microbiol Rev. 2012;25:609-634. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 324] [Cited by in RCA: 349] [Article Influence: 29.1] [Reference Citation Analysis (0)] |