Published online Dec 27, 2015. doi: 10.4240/wjgs.v7.i12.394
Peer-review started: April 30, 2015
First decision: August 4, 2015
Revised: September 17, 2015
Accepted: October 16, 2015
Article in press: October 19, 2015
Published online: December 27, 2015
Processing time: 239 Days and 12.5 Hours
A 53-year-old man with multiple medical conditions presented to the emergency department with complaints of vomiting, anorexia and diffuse colicky abdominal pain for 3 d. A computed tomography scan of the abdomen and pelvis showed radiographic findings consistent with Rigler triad seen in small proportion of patients with small bowel obstruction secondary to gallstone impaction. In addition there was a gastric outlet obstruction, consistent with Bouveret’s syndrome. The patient underwent an exploratory laparotomy and enterotomy with multiple stones extracted. The patient had an uneventful post-surgical clinical course and was discharged home.
Core tip: Gallstone ileus is an uncommon cause of small bowel obstruction. The classic finding of Rigler triad is often seen. Bouveret’s syndrome is a subset of gallstone ileus, and usually presents with gastric outlet obstruction as opposed to small bowel obstruction. We present a case where there were multiple stones, each causing obstruction in different locations. Clinicians need to be aware of the possibility of multiple stones when deciding treatment options.
- Citation: Gaduputi V, Tariq H, Rahnemai-Azar AA, Dev A, Farkas DT. Gallstone ileus with multiple stones: Where Rigler triad meets Bouveret’s syndrome. World J Gastrointest Surg 2015; 7(12): 394-397
- URL: https://www.wjgnet.com/1948-9366/full/v7/i12/394.htm
- DOI: https://dx.doi.org/10.4240/wjgs.v7.i12.394
Bouveret’s syndrome is an uncommon form of gallstone ileus, caused by a gall stone which has migrated into the duodenal bulb from a bilioduodenal fistula comprising only 1%-3% of all cases. It is a rare cause of gastric outlet obstruction. The gallstone usually obstructs the distal part of the small intestine where the lumen is narrowest. It rarely obstructs the duodenum. Bouveret’s syndrome presents as a distinct variety of gallstone ileus because of how proximal the obstruction is[1,2]. It is known to occur more commonly in elderly women due to the increased incidence of gallstone disease and can cause significant mortality in patients with multiple medical comorbidities. The pathophysiology of this syndrome stems from the increase in gallbladder intraluminal pressure due to obstruction which in turn leads to local ischemia and necrosis. This enables the gall stone to penetrate the wall of the gallbladder and enter into the intestines[3].
A 53-year-old man with multiple medical conditions including diabetes mellitus type 2, hypertension and end stage renal disease on renal replacement therapy, presented to the emergency department with vomiting, anorexia and diffuse colicky abdominal pain for 3 d. He denied having ever smoked, consumed alcohol or used illicit drugs. In the emergency department he was afebrile and hemodynamically stable. His abdomen was distended, soft, non-tender with no rigidity, but with hypoactive bowel sounds. Laboratory results revealed an elevated white blood cell count of 20 k/uL, serum bicarbonate of 32 mEq/L, serum chloride of 88 mEq/L, serum blood urea nitrogen 36 mg/dL, creatinine 6.4 mg/dL, serum lipase of 38 and normal liver function tests.
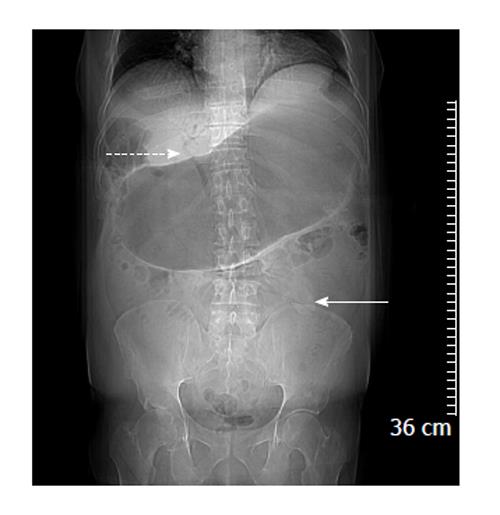
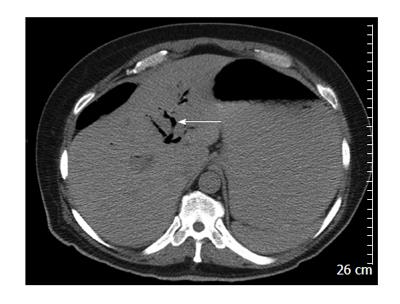
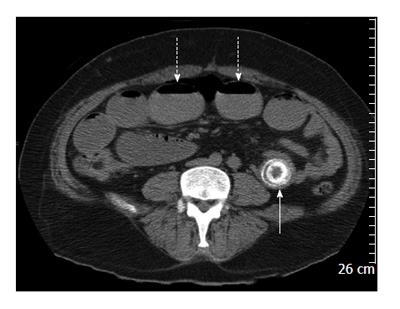
A computed tomography (CT) scan of abdomen and pelvis showed findings consistent with Rigler triad seen in gallstone ileus: (1) Signs of small bowel obstruction; (2) pneumobilia; and (3) ectopic gallstone. Both the pneumobilia and ectopic gallstone are seen in the scout (Figure 1), with the pneumobilia more clearly seen in the axial cuts (Figure 2). The small bowel obstruction as well as the large stone in the left lower quadrant with a transition point in the bowel caliber are seen on lower abdominal cuts (Figure 3). What was unusual in this case was the extent of gastric outlet obstruction in comparison to the small bowel distention. On closer inspection a smaller stone fragment was noted in the duodenum (Figure 4), leading to a secondary Bouveret’s syndrome.
The patient underwent an exploratory laparotomy at which time distended proximal small bowel up to distal jejunum was seen. A large gallstone was noted here measuring 6 cm × 4 cm, while another gallstone was noted in proximal jejunum just beyond the duodeno-jejunal flexure measuring 2 cm × 2.5 cm. Enterotomy was performed and 2 gallstones were removed. No other lesion was identified in the small bowel. The gallbladder was palpated, but no definite stone was felt. The patient had an uneventful post-surgical clinical course.
Leon Bouveret first reported two cases of gastric outlet obstruction due to gallstones, in 1896 in the “Revue Medicale”[1,2]. Gallstone ileus is the cause in about 1%-4% of all cases with intestinal obstruction. Bouveret’s syndrome is a rare subset of gallstone ileus comprising of about 1%-3% of cases[2,3]. Bouveret’s syndrome is more prevalent in women with reported median age of presentation being 74 years. The gender difference in prevalence is explained by the higher incidence of gallstone disease in women, likely due to the cholestatic effects of estrogen[2]. The case we presented was unusual in regards to the gender and age of presentation.
The pathophysiology includes perforation of the wall of biliary system by a stone usually larger than 2.5 cm and subsequent passage into the bowel with impaction usually in the terminal ileum[4]. Around 1% of gall stone cases develop bilio-enteric fistulas including cholecystoduodenal (60%), cholecystocolic (17%), cholecystogastric (5%), choledochoduodenal (5%) fistulas[1]. Most common symptoms include vomiting (87%), abdominal pain (71%), hematemesis (15%), weight loss (14%), and anorexia (13%). Common signs may include abdominal tenderness (44%), dehydration (31%), abdominal distension (26%)[2]. Our case was unique as the patient had two stones, first in the distal duodenum causing gastric obstruction (Bouveret’s syndrome) and another larger stone in the left lower quadrant causing ileus of small bowel.
The Rigler triad consisting of small-bowel obstruction, pneumobilia and an ectopic gallstone is virtually pathognomonic for gallstone ileus. However, it is present on conventional radiographs in only about a third of gallstone ileus cases[5]. This triad of findings is more readily apparent on CT scans. CT scan also provides information about the presence of a fistula; the degree of inflammation in the surrounding tissue; the degree of bowel obstruction; the size, number and locations of the occluding gallstones. However, approximately 15% to 25% of gallstones are not able to be visualized on CT scans, as they are isoattenuating. Such stones can be visualized with magnetic resonance cholangiopancreatography[4,5].
The first successful endoscopic extraction was described in 1985 by Bedogni et al[6]. Endoscopy in tandem with extracorporeal shockwave lithotripsy[7] or endoscopic electrohydraulic lithotripsy[8] and percutaneous approaches should be considered before surgical options, as most patients with Bouveret’s syndrome make for poor surgical candidates[9]. Laser lithotripsy is also an alternative, non-invasive therapeutic option to surgical treatment in old or high-risk patients with Bouveret’s syndrome[10]. Indications for open surgery are stone size greater than 2.5 cm, residual stones in gall bladder, multiple stones in intestinal lumen, sepsis, perforation, stricture and failure of endoscopic approach[1]. In patients who require surgery, common options include enterolithotomy with or without intestinal resection and gastrostomy[11]. Cholecystectomy should be offered to prevent recurrences[12]. Our patient was not a candidate for endoscopic therapy due to the presence of multiple gallstones in separate locations.
In conclusion, gallstone ileus is an uncommon diagnosis and is usually identified by the Rigler triad seen on imaging. Bouveret’s syndrome is a rare subset of this that presents with gastric outlet obstruction. Clinicians should be aware of the possibility of multiple stones being present in the gastrointestinal tract, as is this is critical to choosing the right form of treatment.
A 53-year-old man with vomiting and abdominal pain for three days.
The clinical diagnosis was small bowel obstruction.
Other diagnoses included other types of gastrointestinal obstruction, as well as various causes of peritonitis.
Lab values were significant for a raised white cell count, as well as a metabolic alkalosis seen in the electrolytes.
X-rays revealed a gastric outlet obstruction, and computed tomography scan showed small bowel obstruction as well, and the presence of multiple obstructing stones.
Pathology was consistent with a gallstone in the gastrointestinal tract.
Treatment for this patient was a laparotomy after fluid resuscitation, with an enterotomy and multiple stone removal.
Other reports discuss various treatments for gallstone ileus, depending on stone location and other factors.
Gallstone ileus refers to an ectopic location of a gallstone in the gastrointestinal tract; Rigler triad refers to the classic finding of pneumobilia, small bowel obstruction and ectopic gallstone; Bouveret’s syndrome refers to the subset of gallstone ileus where the stone causes a gastric outlet obstruction.
This case highlights the possibility of there being multiple stones causing obstruction in different areas, something which is important to be aware of when deciding which treatment option to use.
The authors describe a nice case of a patient with multiple obstructions caused by a gallstone including the special case of a gastric outlet obstruction.
P- Reviewer: Maiss J, Xu Z S- Editor: Ji FF L- Editor: A E- Editor: Liu SQ
| 1. | Kalwaniya DS, Arya SV, Guha S, Kuppuswamy M, Chaggar JG, Ralte L, Chejera R, Sharma A. A rare presentation of gastric outlet obstruction (GOO) - The Bouveret’s syndrome. Ann Med Surg (Lond). 2015;4:67-71. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 12] [Cited by in RCA: 10] [Article Influence: 1.0] [Reference Citation Analysis (0)] |
| 2. | Cappell MS, Davis M. Characterization of Bouveret’s syndrome: a comprehensive review of 128 cases. Am J Gastroenterol. 2006;101:2139-2146. [PubMed] |
| 3. | Baharith H, Khan K. Bouveret syndrome: when there are no options. Can J Gastroenterol Hepatol. 2015;29:17-18. [PubMed] |
| 4. | Pickhardt PJ, Bhalla S, Balfe DM. Acquired gastrointestinal fistulas: classification, etiologies, and imaging evaluation. Radiology. 2002;224:9-23. [PubMed] |
| 5. | Nickel F, Müller-Eschner MM, Chu J, von Tengg-Kobligk H, Müller-Stich BP. Bouveret‘s syndrome: presentation of two cases with review of the literature and development of a surgical treatment strategy. BMC Surg. 2013;13:33. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 31] [Cited by in RCA: 40] [Article Influence: 3.3] [Reference Citation Analysis (0)] |
| 6. | Bedogni G, Contini S, Meinero M, Pedrazzoli C, Piccinini GC. Pyloroduodenal obstruction due to a biliary stone (Bouveret's syndrome) managed by endoscopic extraction. Gastrointest Endosc. 1985;31:36-38. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 38] [Cited by in RCA: 37] [Article Influence: 0.9] [Reference Citation Analysis (1)] |
| 7. | Dumonceau JM, Delhaye M, Devière J, Baize M, Cremer M. Endoscopic treatment of gastric outlet obstruction caused by a gallstone (Bouveret’s syndrome) after extracorporeal shock-wave lithotripsy. Endoscopy. 1997;29:319-321. [PubMed] |
| 8. | Moriai T, Hasegawa T, Fuzita M, Kimura A, Tani T, Makino I. Successful removal of massive intragastric gallstones by endoscopic electrohydraulic lithotripsy and mechanical lithotripsy. Am J Gastroenterol. 1991;86:627-629. [PubMed] |
| 9. | Egawa N, Kamisawa T, Tu Y, Sakaki N, Tsuruta K, Okamoto A. The role of juxtapapillary duodenal diverticulum in the formation of gallbladder stones. Hepatogastroenterology. 1998;45:917-920. [PubMed] |
| 10. | Maiss J, Hochberger J, Hahn EG, Lederer R, Schneider HT, Muehldorfer S. Successful laserlithotripsy in Bouveret’s syndrome using a new frequency doubled doublepulse Nd: YAG laser (FREDDY). Scand J Gastroenterol. 2004;39:791-794. [PubMed] |
| 11. | Halabi WJ, Kang CY, Ketana N, Lafaro KJ, Nguyen VQ, Stamos MJ, Imagawa DK, Demirjian AN. Surgery for gallstone ileus: a nationwide comparison of trends and outcomes. Ann Surg. 2014;259:329-335. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 137] [Cited by in RCA: 159] [Article Influence: 14.5] [Reference Citation Analysis (0)] |
| 12. | Iancu C, Bodea R, Al Hajjar N, Todea-Iancu D, Bălă O, Acalovschi I. Bouveret syndrome associated with acute gangrenous cholecystitis. J Gastrointestin Liver Dis. 2008;17:87-90. [PubMed] |