Published online Oct 27, 2013. doi: 10.4240/wjgs.v5.i10.282
Revised: September 10, 2013
Accepted: October 15, 2013
Published online: October 27, 2013
Processing time: 94 Days and 18.1 Hours
Bezoars are usually confined to the stomach which is seen in individuals with psychiatric illness like trichotillomania, trichophagia and gastric dysmotility. Long standing bezoars may extend into the small intestine leading to a condition known as Rapunzel syndrome. Diagnosis can be established by endoscopy, ultrasonography and computed tomography scan. Treatment includes improvement of general condition and removal of bezoar by laparoscopic approach or laparotomy. Psychiatric consultation is necessary to treat and prevent relapse. We report a case of Rapunzel syndrome in a 16-year-old girl with trichotillomania. She presented with history of epigastric mass for three months and recent onset of pain abdomen, vomiting and early satiety. Skiagram of abdomen was showing distended stomach and endoscopy revealed trichobezoar. At laparotomy, stomach was distended with trichobezoar and there were multiple small intestinal intussusceptions. Gastrotomy and manual reduction of intussusceptions with the removal of trichobezoar with its tail was done. Patient recovered completely after the procedure.
Core tip: Rapunzel syndrome is a rare condition which occurs in younger age group with trichotillomania and trichophagia. When trichobezoar is diagnosed further work up has to be carried out to rule out the presence of its tail extending into the small intestine causing complications such as intestinal obstruction, bleeding, malnutrition and perforation. We report a case where multiple intussusceptions were present which is rare. Though gastrotomy with enterotomy is advised to remove bezoar, we were able to remove the entire length of intestinal tail through gastrotomy itself and there was no need for enterotomy to remove the intestinal part of bezoar.
- Citation: Prasanna BK, Sasikumar K, Gurunandan U, Sreenath GS, Kate V. Rapunzel syndrome: A rare presentation with multiple small intestinal intussusceptions. World J Gastrointest Surg 2013; 5(10): 282-284
- URL: https://www.wjgnet.com/1948-9366/full/v5/i10/282.htm
- DOI: https://dx.doi.org/10.4240/wjgs.v5.i10.282
Trichobezoar is a condition where in swallowed hair starts accumulating in the stomach over a period of time to form a concretion which presents later with features of malnutrition and intestinal obstruction. These patients will usually have psychiatric conditions such as trichotillomania and trichophagia. When the bezoar extends into the small intestine it is called as Rapunzel syndrome which was first reported in 1968 by Vaughan et al[1]. It can even present with complications like intestinal obstruction, perforation and peritonitis. Here we present a rare case of Rapunzel syndrome with multiple small intestinal intussusceptions in an adolescent girl.
A 16-year-old girl presented with history of mass in epigastric region for three months duration, abdominal pain for one month and vomiting for three days. The patient had delayed developmental milestones and poor performance at school. There was history of pulling and swallowing hair for three years for which tonsuring was done one year earlier. The patient had received psychiatric treatment for these complaints.
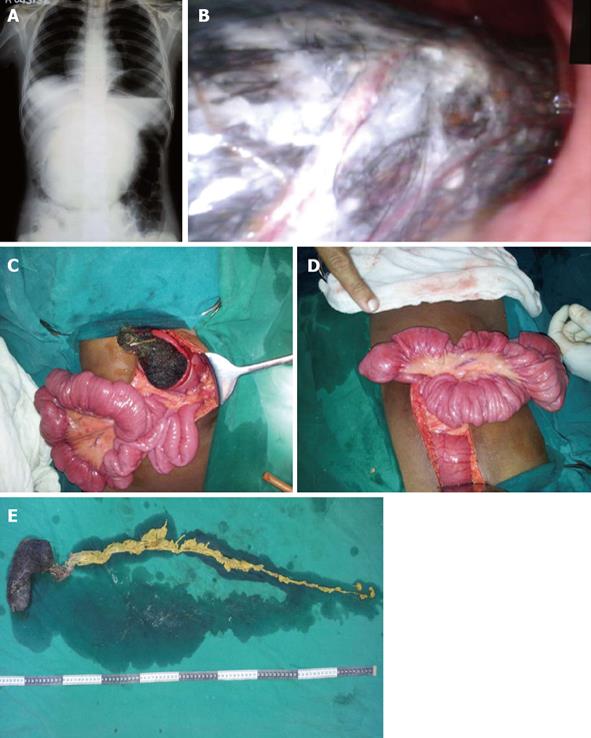
On examination, the patient was conscious, cooperative, pale and haemodynamically stable. Abdominal examination revealed a firm epigastric mass measuring 15 cm × 10 cm. Laboratory investigations revealed hemoglobin of 7.8 g/dL, serum total protein of 4.5 g/dL and serum albumin of 2.5 g/dL. Ultrasound examination of the abdomen was normal. Skiagram of the abdomen showed grossly distended stomach (Figure 1). Upper gastrointestinal endoscopy revealed presence of trichobezoar (Figure 1). The patient was given one packed cell transfusion to correct anemia and was posted for elective laparotomy.
On exploration, the stomach was distended and there were multiple intussusceptions in the jejunum and proximal ileum (Figure 1). The tail of bezoar was palpable throughout the jejunum and proximal ileum. Intussusceptions were manually reduced and gastrotomy along the body of the stomach parallel to greater curvature for a length of 10 cm was carried out. The trichobezoar made of bile stained foul smelling hair and cotton thread was removed along with the tail part (Figure 1). Gastrotomy was closed in two layers. Post operative period was uneventful and she was discharged with psychiatric counseling. At the follow-up examination two weeks following surgery, the patient was found to be free of abdominal symptoms and there was an improvement in her hemoglobin and serum total proteins when compared to the preoperative levels.
The term “bezoar” is derived from the Persian word “Padzahr” which means antidote[2]. There are various types of bezoar including trichobezoar (hair), phytobezoar (vegetable material), lactobezoar (milk products), pharmacobezoar and bezoars of honey comb, and cotton fibers. This condition is common in teenage girls with trichotillomania and trichophagia and patients with gastric motility problem. Debakey and Oschner suggested that the slippery nature of hair and its entrapment within gastric folds could be the reason for bezoar formation[3]. Over a period of time, hair gets matted with each other and with other indigestible materials like cotton fibers and vegetable matter to assume the shape of the stomach. Sometimes its tail may extend into the small intestine.
Bezoars can present with mass in the abdomen, abdominal pain, nausea, vomiting, weakness, weight loss, constipation, diarrhea and malnutrition[4]. In the present case, the patient had mass per abdomen associated with pain and vomiting. Rarely it may present with complications like intestinal obstruction, bleeding, perforation and obstructive jaundice, pancreatitis and appendicitis[5]. Intestinal obstruction can be the direct effect of the bezoar or secondary to intussusception. The clinician must consider the possibility of Rapunzel syndrome when patient with trichobezoar presents with features of intestinal obstruction[5]. The diagnosis can be made out by ultrasound, computerized tomography, barium meal and endoscopy.
Endoscopic retrieval of gastric trichobezoar is less invasive and cost effective than surgical removal[6]. But it is successful in only few patients and there are instances of respiratory arrest due to airway obstruction while attempting to remove trichobezoar[7]. When Rapunzel syndrome is suspected endoscopic retrieval should not be tried. Large gastric bezoars can be removed with laparoscopic approach safely but at the rate of prolonged operative time[8]. There are instances where Rapunzel syndrome has been managed laparoscopically[9].
In the present case, although the bezoar was extending into the small bowel as a lead point causing multiple intussusceptions, the patient did not have classical features of intestinal obstruction except for non bilious vomiting.
In cases with the bezoar extending into the intestine, usually enterotomy is advised to remove the bezoar. But in the present case the complete trichobezoar could be delivered out through a gastrotomy after reducing the intussusceptions at multiple levels in jejunum and ileum. It is a potentially life threatening condition where early diagnosis, surgical intervention has its role. Unless psychiatric counseling and follow up is done, this condition can recur[10].
P- Reviewers Jenke AC, Konishi T, Namikawa T, Pogorelic Z S- Editor Qi Y L- Editor A E- Editor Lu YJ
| 1. | Vaughan ED, Sawyers JL, Scott HW. The Rapunzel syndrome. An unusual complication of intestinal bezoar. Surgery. 1968;63:339-343. [PubMed] |
| 2. | Williams RS. The fascinating history of bezoars. Med J Aust. 1986;145:613-614. [PubMed] |
| 3. | Debakey M, and Oschner A. Bezoars and concretions: A comprehensive review of the literature with analysis of 303 collected cases and a presentation of 8 additional cases. Surgery. 1938;4:934-963. |
| 4. | Harikumar R, Kumar S, Kumar B, Balakrishnan V. Rapunzel syndrome: a case report and review of literature. Trop Gastroenterol. 2007;28:37-38. [PubMed] |
| 5. | Godart B, Wangermez M, Doucet C, Faure JP, Beauchant M. [Rapunzel syndrome associated with small bowel intussusception, acute pancreatitis and bile duct dilatation]. Gastroenterol Clin Biol. 2006;30:1324-1325. [PubMed] |
| 6. | Konuma H, Fu K, Morimoto T, Shimizu T, Izumi Y, Shiyanagi S, Urao M, Miyazaki A, Watanabe S. Endoscopic retrieval of a gastric trichobezoar. World J Gastrointest Endosc. 2011;3:20-22. [PubMed] |
| 7. | Esmaili MR, Abbasi HR, Baradaranfar MH. Respiratory arrest due to airway obstruction following endoscopic removal of Trichobezoar. J Pak Med Assoc. 2011;61:700-701. [PubMed] |
| 8. | Dorn HF, Gillick JL, Stringel G. Laparoscopic intragastric removal of giant trichobezoar. JSLS. 2010;14:259-262. [PubMed] |
| 9. | Hernández-Peredo-Rezk G, Escárcega-Fujigaki P, Campillo-Ojeda ZV, Sánchez-Martínez ME, Rodríguez-Santibáñez MA, Angel-Aguilar AD, Rodríguez-Gutiérrez C. Trichobezoar can be treated laparoscopically. J Laparoendosc Adv Surg Tech A. 2009;19:111-113. [PubMed] |
| 10. | Salaam K, Carr J, Grewal H, Sholevar E, Baron D. Untreated trichotillomania and trichophagia: surgical emergency in a teenage girl. Psychosomatics. 2005;46:362-366. [PubMed] |