Published online Aug 27, 2025. doi: 10.4240/wjgs.v17.i8.106499
Revised: April 24, 2025
Accepted: June 23, 2025
Published online: August 27, 2025
Processing time: 146 Days and 4.1 Hours
Recently, intestinal stenting combined with laparoscopic surgery has received increasing attention as a treatment option for acute intestinal obstruction. How
To assess the efficacy and safety of combining intestinal stenting with laparoscopic surgery for the management of acute intestinal obstruction.
Clinical data from 74 patients with colorectal cancer and acute intestinal obstruction, who were admitted to the emergency department of the authors’ hospital between October 2023 and November 2024, were collected and analyzed. Patients were divided into two groups based on the surgical intervention: A control group (emergency open surgery, n = 37) and a study group (intestinal stent implantation combined with laparoscopic surgery, n = 37). Observation indicators included stent placement rate, obstruction relief rate, and stent-related complications.
Intestinal stent placement was 100% successful in the study group, all of whom experienced relief from obstruction while exhibiting a significantly lower rate of ostomy creation and a higher rate of primary anastomosis than in the control group, as well as less intraoperative blood loss, shorter time to flatus, and shorter hospital stay. The complication rate was 5.41% (2/37; bleeding and re-obstruction), with no statistically significant difference between the two groups in terms of operative duration or perioperative mortality. The overall complication rates were 5.41% (2/37) and 21.62% (8/37) in the intervention and control groups, respectively. Tumor recurrence and overall survival rates were 2.70% and 97.30% in the study group and 13.51% and 91.89% in the control group, respectively.
Intestinal stenting relieved acute obstructions, reduced the number of emergency surgeries, and supported laparoscopic procedures while improving primary anastomosis rates, minimizing ostomy occurrence, surgical trauma, and complications, and accelerating recovery.
Core Tip: To assess the efficacy and safety of combining intestinal stenting with laparoscopic surgery for the management of acute intestinal obstruction. We concluded that intestinal stenting relieved acute obstructions, reduced the number of emergency surgeries, and supported laparoscopic procedures while improving primary anastomosis rates, minimizing the occurrence of ostomies, surgical trauma, and complications, and facilitating a faster recovery.
- Citation: He YN, Zhao TT. Efficacy and safety of combining intestinal stenting with laparoscopic surgery in colorectal cancer patients with acute intestinal obstruction. World J Gastrointest Surg 2025; 17(8): 106499
- URL: https://www.wjgnet.com/1948-9366/full/v17/i8/106499.htm
- DOI: https://dx.doi.org/10.4240/wjgs.v17.i8.106499
Acute intestinal obstruction is a common form of intestinal blockage characterized by a rapid onset, complex symptoms, and various causes, with epidemiological data showing an incidence rate of up to 30%[1,2]. Intestinal obstruction accounts for 15% of the population with an acute abdomen[3]. The growth of colorectal tumors in the intestinal lumen is the main cause of intestinal lumen narrowing[4]. Severe abdominal pain, vomiting, bloating, and bowel dysfunction are the typical symptoms of acute bowel obstruction[5]. Currently, surgery is the primary treatment for acute intestinal obstruction[6]. However, surgical interventions are often associated with severe complications, with mortality rates exceeding 5%-15%[7]. Emergency surgery often affects patients’ quality of life and mental health.
Laparoscopic surgery for rectal cancer has recently gained popularity worldwide. Numerous clinical studies, including randomized trials, have shown that this approach is feasible and safe and provides favorable short-term benefits and oncological outcomes similar to those of open surgery[8]. Metal stents are widely used to treat patients with colorectal cancer and acute intestinal obstruction[9]. Intestinal stenting effectively widens narrowed intestinal passages, alleviates blockages, assists bowel decompression, and decreases bowel wall swelling and edema[10]. A meta-analysis reported that while emergency surgeries had a higher clinical success rate (99% vs 52.5%), the stent group had a higher initial anasto
Nevertheless, the existing evidence remains fragmented, with insufficient data on long-term oncological safety and a lack of standardized protocols. This study explored the combined effectiveness and safety of intestinal stent implantation and laparoscopic surgery in improving the outcomes of patients with colorectal cancer with acute intestinal obstruction. By examining this approach, we aim to provide a valuable reference for clinical practice and deepen our understanding of its potential benefits in this patient population.
Clinical data from 74 patients diagnosed with colorectal cancer who had acute intestinal obstruction and were admitted to the Nanchong Central Hospital between October 2023 and November 2024 and followed up for at least 12 months were retrospectively collected and analyzed. The patients were divided into two groups based on the surgical intervention: A control group (emergency open surgery, n = 37) and a study group (intestinal stent implantation and laparoscopic surgery, n = 37).
The inclusion criteria are patients diagnosed with colorectal cancer with acute intestinal obstruction; abdominal computed tomography revealing irregular thickening of the bowel wall, proximal lumen dilation, and abnormal gas; inability to pass through the narrowed segment via laparoscopy; presence of ≥ 3 symptoms (abdominal pain, vomiting, and/or abdominal distension); and complete clinical data. The exclusion criteria were as follows: Presence of psychiatric disorder(s), severe cardiovascular or cerebrovascular disease, intestinal obstruction with perforation, high-risk factors for undergoing endoscopy, and unwillingness to provide written informed consent.
This study was approved by the ethics committee of the authors’ Nanchong Central Hospital.
Control group: Patients in this group underwent emergency laparotomy. Preoperatively, a thorough examination was performed to assess whether the tumor had invaded surrounding organs. The choice of surgical approach, anesthesia method, and patient positioning was based on the individual patient’s condition. For patients without invasion of surrounding organs, tumor resection was performed along with colostomy. In cases where the tumor was non-resectable, a double-barrel colostomy was established.
Study group: Patients in the study group underwent intestinal stenting combined with laparoscopic surgery. Initially, intravenous anesthesia was administered, and a colonoscope was inserted through the anal canal to reach the distal end of the intestinal obstruction. Subsequently, a super-slippery and stiff guidewire was placed through the working channel, and a contrast catheter was advanced through the narrowed segment of the intestine using the guidewire. Based on computed tomography evaluation of stricture length, a 26 mm × 80/100 mm self-expanding metallic stent was selected for placement. The stent was released under endoscopic visualization, and its position and expansion were monitored. The procedure was performed once satisfactory deployment was confirmed. Postoperatively, the patients’ vital signs were monitored, and upright abdominal radiographs were obtained to further assess the stent position and expansion, as well as to confirm the absence of perforation. Laparoscopic colorectal resection was performed 10-14 days after stent placement with appropriate preoperative assessment. Patients were placed in the Trendelenburg position and underwent tracheal intubation under general anesthesia. The operation ports were selected based on the tumor location, pneu
The study assessed the success rate of stent placement, the rate of obstruction relief, and stent-related complications, including re-obstruction, bleeding, dislocation, and perforation in the study group[12]. Basic surgical metrics were compared between the two groups[13], including the ostomy rate, primary anastomosis rate, operative time, intraoperative blood loss, time to flatus, length of postoperative hospital stay, and perioperative mortality rate. The overall complication rates were recorded for both groups, including gastrointestinal bleeding, wound infection, pulmonary infection, anastomotic leakage, and postoperative intestinal obstruction[14]. Complication rates were calculated as follows: (Number of gastrointestinal bleeding, wound infections, pulmonary infections, anastomotic leakages, and postoperative intestinal obstructions)/total number of patients × 100. Patients were followed up for 12 months to record tumor recurrence and overall survival rates for both groups.
All statistical analyses were performed using SPSS version 26.0 (IBM Corp., Armonk, NY, United States). Continuous data were expressed as mean ± SD and were analyzed using independent sample t-tests or paired t-tests. Categorical variables are expressed as counts (percentages) and analyzed using Pearson’s χ2 test, Yates’ correction for continuity, or Fisher’s exact test. Differences with P < 0.05 were considered to be statistically significant.
No statistically significant differences were noted between the two groups in terms of age, weight, duration of illness, platelet count, red and white blood cell counts, sex, smoking status, alcohol consumption, exercise habits, ethnicity, pathological staging, lymphatic metastasis, differentiation, degree of intestinal obstruction, primary tumor characteristics, or histological type (P > 0.05), indicating comparability between the two groups. The data are summarized in Table 1.
| Factors | Study group (n = 37) | Control group (n = 37) | P value |
| Age | 50.67 ± 11.49 | 51.16 ± 10.58 | 0.869 |
| Body weight (kg) | 76.19 ± 8.48 | 75.02 ± 8.16 | 0.546 |
| BMI (kg/m2) | 26.13 ± 4.38 | 27.05 ± 5.15 | 0.369 |
| Disease course (weeks) | 3.13 ± 0.57 | 3.23 ± 0.52 | 0.653 |
| Platelet (× 109/L) | 228.17 ± 50.21 | 220.48 ± 57.07 | 0.682 |
| Erythrocyte (× 109/L) | 4.69 ± 0.67 | 4.75 ± 0.59 | 0.637 |
| Leukocyte (× 109/L) | 8.12 ± 1.19 | 7.91 ± 1.32 | 0.474 |
| Sex | 0.661 | ||
| Male | 27 (72.97) | 31 (77.50) | |
| Female | 10 (27.03) | 9 (22.50) | |
| Smoking | 0.768 | ||
| Yes | 25 (67.57) | 29 (72.50) | |
| No | 12 (32.43) | 11 (27.50) | |
| Alcohol consumption | 0.488 | ||
| Yes | 29 (78.38) | 30 (75.00) | |
| No | 8 (21.62) | 10 (25.00) | |
| Exercise habit | 0.717 | ||
| Yes | 4 (10.81) | 3 (7.50) | |
| No | 33 (89.19) | 37 (92.50) | |
| Ethnicity | 0.506 | ||
| Han | 35 (94.59) | 37 (92.50) | |
| Minority | 2 (5.41) | 3 (7.50) | |
| Pathological stage | 0.612 | ||
| Stage I-II | 17 (45.95) | 22 (55.00) | |
| Stage III-IV | 20 (54.05) | 18 (45.00) | |
| Lymphatic metastasis | 0.527 | ||
| Yes | 12 (32.43) | 11 (27.50) | |
| No | 25 (67.57) | 29 (72.50) | |
| Intestinal obstruction degree | 0.848 | ||
| Complete | 24 (64.86) | 27 (67.50) | |
| Incomplete | 13 (35.14) | 13 (32.50) | |
| Primary tumor | 0.879 | ||
| Colon cancer | 15 (40.54) | 18 (45.00) | |
| Rectal cancer | 22 (59.46) | 22 (55.00) | |
| Histological type | 0.974 | ||
| Adenocarcinoma | 14 (37.84) | 15 (37.50) | |
| Mucinous carcinoma | 13 (35.14) | 14 (35.00) | |
| Undifferentiated carcinoma | 10 (27.02) | 9 (22.50) | |
| Differentiation degree | 0.875 | ||
| Well-differentiated | 20 (54.05) | 19 (51.35) | |
| Moderately differentiated | 8 (21.62) | 8 (21.62) | |
| Poorly differentiated | 9 (24.33) | 10 (27.03) | |
All 37 patients in the study group (100%) successfully underwent intestinal stent placement. All patients with successful stent placement achieved clinical relief, with a 100% rate of obstruction relief. After stenting, one patient experienced bleeding, which improved with conservative treatment, and another patient developed re-obstruction on postoperative day 4, which resolved with enema treatment. No instances of stent dislocation or perforation were observed, and the stent-related complication rate was 5.41% (2/37).
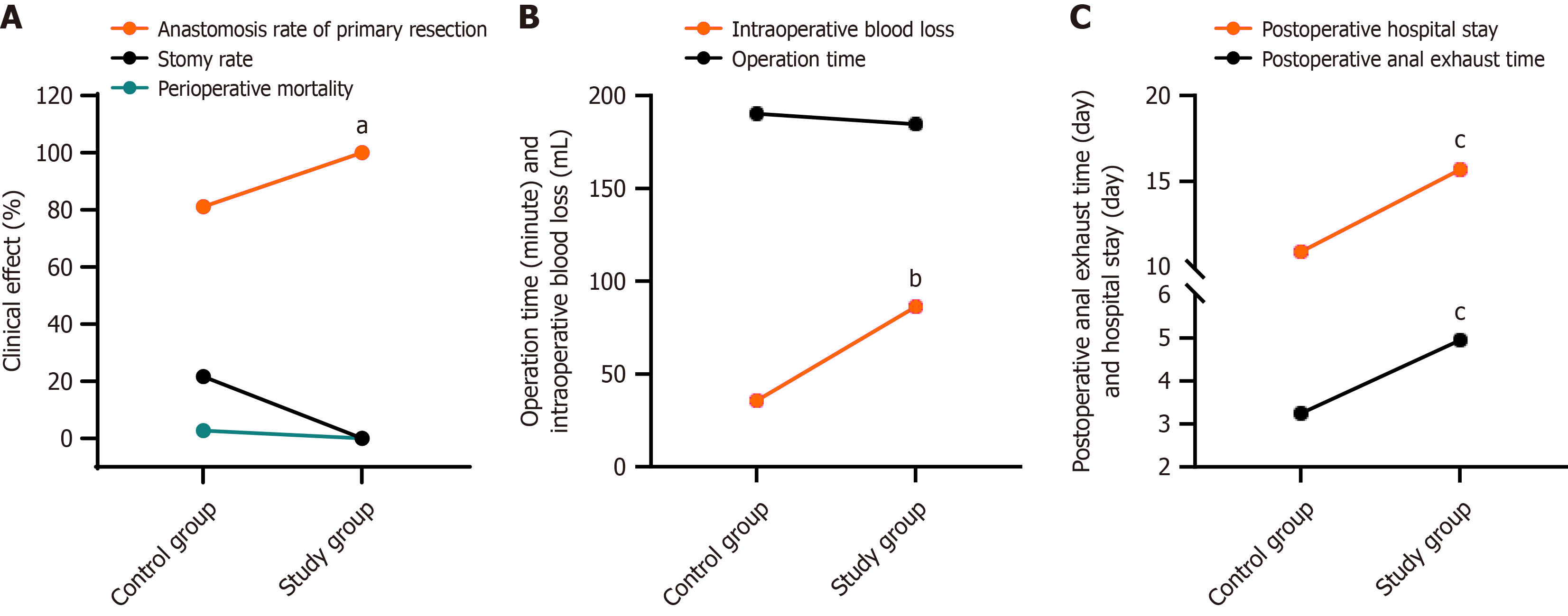
The ostomy rate in the intervention group was significantly lower than in the control group (0.00% vs 21.62%), whereas the primary anastomosis rate was significantly higher in the intervention group (100.00% vs 81.08%) (P < 0.05). However, there was no significant difference in the perioperative mortality rates between the two groups (0.00% vs 2.70%; P > 0.05) (Figure 1A).
No statistical difference was observed in the mean ± SD operative duration between the study group (190.25 ± 18.61 minutes) and control group (184.62 ± 19.33 minutes) (P > 0.05). Mean intraoperative blood loss in the study group was 35.75 ± 11.24 mL, which was significantly less than that in the control group (86.34 ± 30.19 mL). The mean time to postoperative flatus was shorter in the study group (3.25 ± 0.42 hours) than that in the control group (4.95 ± 0.57 hours), and the length of hospital stay was 10.91 ± 1.25 days, shorter than that in the control group (15.69 ± 2.46 days). These differences were statistically significant (P < 0.001) (Figure 1B and C).
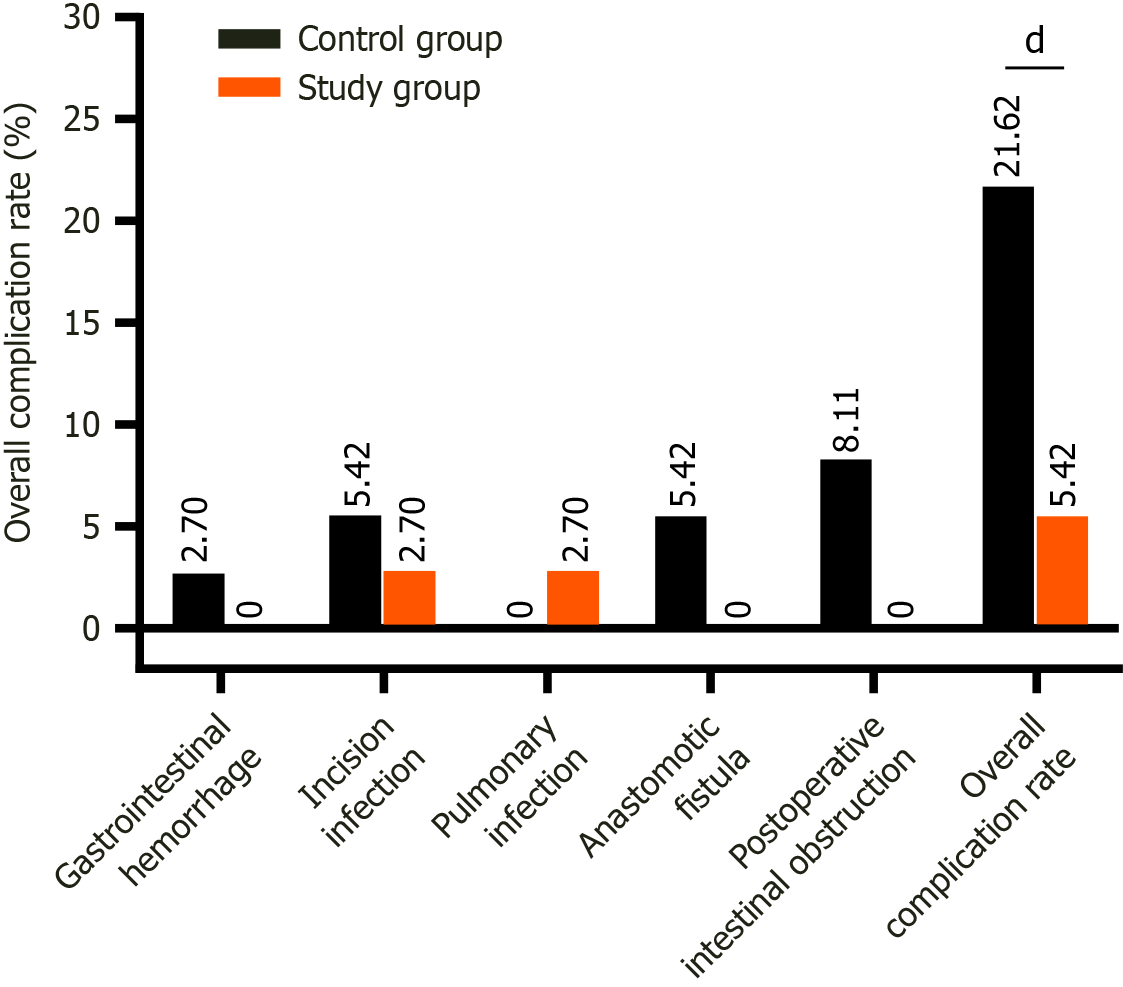
The overall complication rates in the study and control groups were 5.42% (2/37) and 21.62% (8/37), respectively (P < 0.05) (Figure 2).
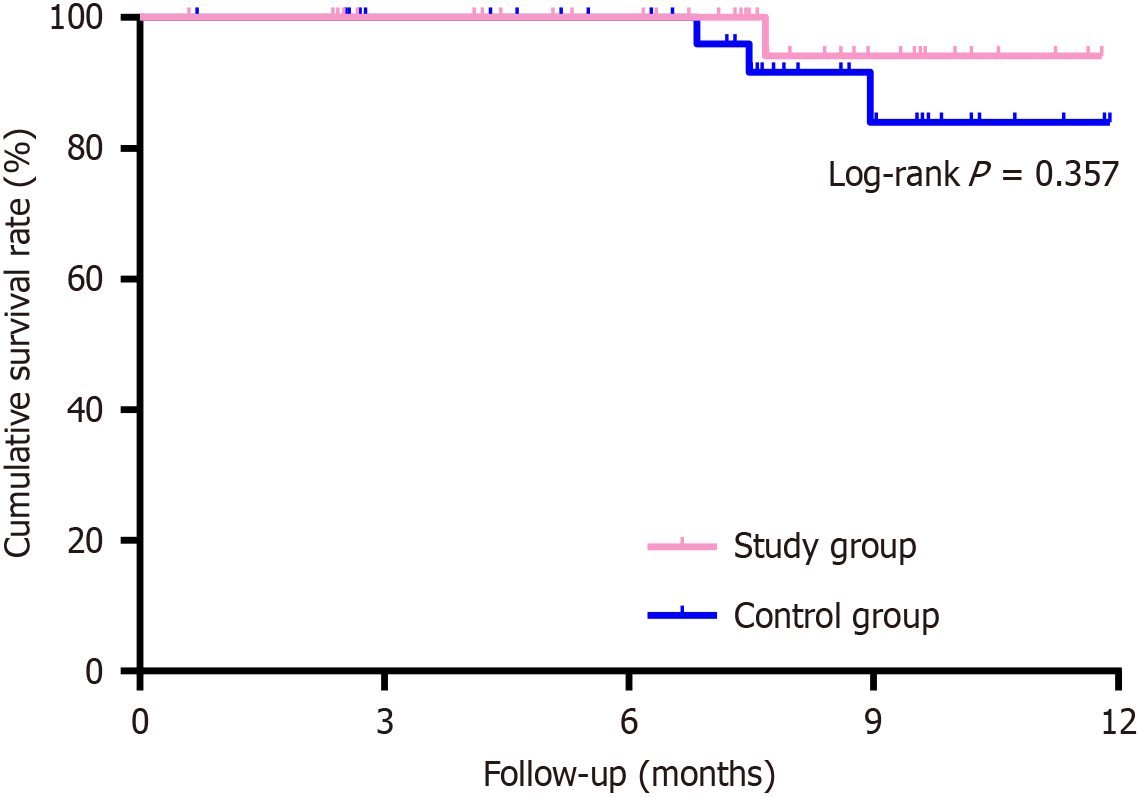
At the 12-month follow-up, one patient had a recurrence in the study group, corresponding to a recurrence rate of 2.70% and an overall survival rate of 97.30% (36/37). The 12-month cumulative survival rate was 97.30%. In the control group, five patients experienced recurrence, corresponding to a recurrence rate of 13.51% and an overall survival rate of 91.89% (34/37), with a 12-month cumulative survival rate of 84.58%. No statistically significant differences were observed in tumor recurrence and overall survival rates between the two groups (P > 0.05). The results are summarized in Table 2, and the 12-month cumulative survival rates for both groups are represented in Figure 3.
| Group | Control group (n = 37) | Study group (n = 37) | P value |
| Tumor recurrence rate | 5 (13.51) | 1 (2.70) | 0.097 |
| Overall survival rate | 34 (91.89) | 36 (97.30) | 0.317 |
Acute intestinal obstruction is a clinical condition characterized by a rapid onset and progression that requires immediate intervention to relieve the obstruction, prevent further deterioration, and improve patient prognosis[15]. Surgical intervention is currently considered the best option for colorectal cancer complicated by acute intestinal obstruction. The common surgical approaches include stenting and emergency surgery. Although emergency surgery is widely used in clinical practice, it is associated with significant trauma, high risk, and numerous complications, often necessitating secondary surgery to restore intestinal patency[16]. This has led to the development of safer and more effective therapies. Stenting was initially used for vascular and biliary diseases and has gained popularity due to its minimally invasive nature and short operative duration.
Results of the current study indicate that, although the surgical durations for both groups were similar (study group, 190.25 ± 18.61 minutes vs control group, 184.62 ± 19.33 minutes; P > 0.05), the primary anastomosis rate in the study group was significantly higher than that in the control group (100.00% vs 81.08%; P < 0.05). This finding suggests that the combination of stenting and laparoscopic surgery offers a significant advantage for improving tumor resection rates[17]. Stent placement effectively relieves intestinal obstruction, enhances blood flow, and improves the surrounding tissues, thereby facilitating better conditions for future surgeries. Studies have shown that stenting achieves a primary anastomosis success rate of > 83.1%[18,19].
The results of this study demonstrated that the mean length of hospital stay was statistically shorter in the study group (10.91 ± 1.25 days) compared to the control group (15.69 ± 2.46 days) (P < 0.001). This is consistent with the results of previous studies, which reported a 20%-30% reduction in hospital stay in the study group[14,20].
The results of this study further showed that the incidence of complications in the intervention group was significantly lower than that in the control group (5.42% vs 21.62%), a statistically significant difference (P < 0.05). The intestinal stent implantation rate was 100%. This may be because the procedure enhanced bowel patency and blood flow, thereby reducing the incidence of postoperative complications. This finding is consistent with those of previous studies[21-23].
In addition, the results of this study showed that during the follow-up period, only one patient in the study group relapsed, corresponding to a recurrence rate of 2.70%. In contrast, five patients in the control group relapsed, resulting in a recurrence rate of 13.51%. The difference between the two groups was statistically significant. In terms of overall survival, the study group exhibited a survival rate of 97.30% (36/37) compared to 91.89% (34/37) in the control group. Although the differences in tumor recurrence and overall survival rates did not reach statistical significance (P > 0.05), the lower recurrence rate in the study group and the 12-month cumulative survival rates of 97.30% and 84.58% reflected a notable difference in survival, suggesting clinical relevance despite the lack of statistical significance[21,24-26].
Despite the numerous advantages of stenting, it is crucial to adhere strictly to surgical indications in clinical practice. Appropriate surgical methods should be selected based on the severity and location of the strictures to ensure treatment safety and efficacy. Therefore, future research should further explore the application of stenting in different types of colorectal cancer complicated by acute intestinal obstruction and establish more systematic evaluation criteria to guide clinical practice.
This study has certain limitations. First, this was a single-center retrospective design, which may have limited the generalizability of the results to larger populations. Second, confounding factors (e.g., complications and previous treatment) may have affected the results. The sample size was relatively small; therefore, the reliability of the results must be further verified in larger, multicenter, prospective, and randomized controlled studies.
The results of this study demonstrate that combining stent implantation with laparoscopic surgery in patients with acute intestinal obstruction can achieve benefits, including a higher primary anastomosis rate, reduced intraoperative blood loss, a shorter hospital stay, and fewer complications. Large-sample, multicenter, prospective, randomized controlled studies should be conducted to confirm the results of this study.
| 1. | Luo S, Wang Y. Value of Humanized Nursing under Emergency Green Channel on Gastrointestinal Function Recovery in Patients with Acute Intestinal Obstruction after Operation. Emerg Med Int. 2023;2023:2303766. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1] [Cited by in RCA: 2] [Article Influence: 1.0] [Reference Citation Analysis (0)] |
| 2. | Sato R, Oikawa M, Kakita T, Okada T, Abe T, Yazawa T, Tsuchiya H, Akazawa N, Yoshimachi S, Okano H, Ito K, Tsuchiya T. Impact of Sarcopenia on Postoperative Complications in Obstructive Colorectal Cancer Patients Who Received Stenting as a Bridge to Curative Surgery. J Anus Rectum Colon. 2022;6:40-51. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 1] [Cited by in RCA: 10] [Article Influence: 3.3] [Reference Citation Analysis (0)] |
| 3. | Zemour J, Coueffe X, Fagot H. Herniation of the broad ligament… And the other side? Int J Surg Case Rep. 2019;65:354-357. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 9] [Cited by in RCA: 12] [Article Influence: 2.0] [Reference Citation Analysis (0)] |
| 4. | Docsa T, Sipos A, Cox CS, Uray K. The Role of Inflammatory Mediators in the Development of Gastrointestinal Motility Disorders. Int J Mol Sci. 2022;23:6917. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 12] [Cited by in RCA: 19] [Article Influence: 6.3] [Reference Citation Analysis (0)] |
| 5. | Brodzisz A, Kuczyńska M, Zbroja M, Cyranka W, Cielecki C, Woźniak MM. Chronic Appendicitis-From Ambiguous Clinical Image to Inconclusive Imaging Studies. Diagnostics (Basel). 2022;12:818. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 4] [Reference Citation Analysis (0)] |
| 6. | Jackson P, Vigiola Cruz M. Intestinal Obstruction: Evaluation and Management. Am Fam Physician. 2018;98:362-367. [PubMed] |
| 7. | Listle H, Gutt C. [Conservative and surgical ileus treatment]. Chirurg. 2017;88:629-644. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 3] [Cited by in RCA: 4] [Article Influence: 0.5] [Reference Citation Analysis (0)] |
| 8. | Schnitzbauer V, Gerken M, Benz S, Völkel V, Draeger T, Fürst A, Klinkhammer-Schalke M. Laparoscopic and open surgery in rectal cancer patients in Germany: short and long-term results of a large 10-year population-based cohort. Surg Endosc. 2020;34:1132-1141. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 15] [Cited by in RCA: 33] [Article Influence: 5.5] [Reference Citation Analysis (0)] |
| 9. | Hu Y, Fan J, Xv Y, Hu Y, Ding Y, Jiang Z, Tao Q. Comparison of safety between self-expanding metal stents as a bridge to surgery and emergency surgery based on pathology: a meta-analysis. BMC Surg. 2020;20:255. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 3] [Cited by in RCA: 9] [Article Influence: 1.8] [Reference Citation Analysis (0)] |
| 10. | Aadam AA, Martin JA. Enteral stents in malignant bowel obstruction. Gastrointest Endosc Clin N Am. 2013;23:153-164. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 2] [Cited by in RCA: 3] [Article Influence: 0.3] [Reference Citation Analysis (0)] |
| 11. | Cirocchi R, Farinella E, Trastulli S, Desiderio J, Listorti C, Boselli C, Parisi A, Noya G, Sagar J. Safety and efficacy of endoscopic colonic stenting as a bridge to surgery in the management of intestinal obstruction due to left colon and rectal cancer: a systematic review and meta-analysis. Surg Oncol. 2013;22:14-21. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 162] [Cited by in RCA: 142] [Article Influence: 11.8] [Reference Citation Analysis (0)] |
| 12. | Yang L, Ma W, Wang M, Zhang R, Bi T, Zhou S. Efficacy of intestinal obstruction stent combined with laparoscopic surgery and neoadjuvant chemotherapy in patients with obstructive colorectal cancer. Oncol Lett. 2019;18:1931-1937. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 4] [Cited by in RCA: 7] [Article Influence: 1.2] [Reference Citation Analysis (0)] |
| 13. | Oh HH, Hong JY, Kim DH, Myung DS, Cho SB, Lee WS, Kim HS, Joo YE. Differences in clinical outcomes according to the time interval between the bridge to surgery stenting and surgery for left-sided malignant colorectal obstruction. World J Surg Oncol. 2022;20:178. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 8] [Cited by in RCA: 8] [Article Influence: 2.7] [Reference Citation Analysis (0)] |
| 14. | Sato K, Imaizumi K, Kasajima H, Kurushima M, Umehara M, Tsuruga Y, Yamana D, Sato A, Ichimura K, Isokawa M, Nakanishi K. Comparison of Short-term Outcomes of a Self-expandable Metallic Stent as a Bridge to Laparoscopic Surgery between Right- and Left-sided Obstructive Colorectal Cancers: A Retrospective Observational Study. J Anus Rectum Colon. 2022;6:239-248. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 1] [Reference Citation Analysis (0)] |
| 15. | Madyarov V, Kuzikeev M, Malgazhdarov M, Abzalbek Y, Zhapbarkulova G. Causes of adverse outcomes in acute intestinal obstruction. J Complement Integr Med. 2023;20:788-796. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 1] [Reference Citation Analysis (0)] |
| 16. | Lin W, Chok AY, Seow-En I, Tan EK. Stenting as bridge to surgery versus upfront emergency resection for non-metastatic left sided obstructing colorectal cancer: risk of peritoneal recurrence and long-term outcomes. Surg Endosc. 2024;38:2632-2640. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 3] [Reference Citation Analysis (0)] |
| 17. | Arezzo A, Passera R, Lo Secco G, Verra M, Bonino MA, Targarona E, Morino M. Stent as bridge to surgery for left-sided malignant colonic obstruction reduces adverse events and stoma rate compared with emergency surgery: results of a systematic review and meta-analysis of randomized controlled trials. Gastrointest Endosc. 2017;86:416-426. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 130] [Cited by in RCA: 150] [Article Influence: 18.8] [Reference Citation Analysis (0)] |
| 18. | Lara-Romero C, Vilches Á, Caunedo-Álvarez Á, Hergueta-Delgado P, Lavín-Castejón I, Andrade-Bellido R, Alcaín-Martínez G. Better recurrence-free survival after stent bridge to surgery compared to emergency surgery for obstructive left-sided colonic cancer in patients with stage III status of the American Joint Committee on Cancer (AJCC): a bicentric retrospective study. Int J Colorectal Dis. 2019;34:1241-1250. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 17] [Cited by in RCA: 26] [Article Influence: 4.3] [Reference Citation Analysis (0)] |
| 19. | Jain SR, Yaow CYL, Ng CH, Neo VSQ, Lim F, Foo FJ, Wong NW, Chong CS. Comparison of colonic stents, stomas and resection for obstructive left colon cancer: a meta-analysis. Tech Coloproctol. 2020;24:1121-1136. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 12] [Cited by in RCA: 19] [Article Influence: 3.8] [Reference Citation Analysis (0)] |
| 20. | Veld JV, Amelung FJ, Borstlap WAA, van Halsema EE, Consten ECJ, Siersema PD, Ter Borg F, van der Zaag ES, de Wilt JHW, Fockens P, Bemelman WA, van Hooft JE, Tanis PJ; Dutch Snapshot Research Group. Comparison of Decompressing Stoma vs Stent as a Bridge to Surgery for Left-Sided Obstructive Colon Cancer. JAMA Surg. 2020;155:206-215. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 34] [Cited by in RCA: 70] [Article Influence: 14.0] [Reference Citation Analysis (0)] |
| 21. | Gu JB, Yang H, Bao XB, Ma Z, Gu ZY. [Clinical curative effect of enteroscopic stent implantation combined with laparoscopy in patients with colorectal cancer and intestinal obstruction]. Zhonghua Yi Xue Za Zhi. 2024;104:2637-2641. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 1] [Reference Citation Analysis (0)] |
| 22. | Tan L, Liu ZL, Ran MN, Tang LH, Pu YJ, Liu YL, Ma Z, He Z, Xiao JW. Comparison of the prognosis of four different treatment strategies for acute left malignant colonic obstruction: a systematic review and network meta-analysis. World J Emerg Surg. 2021;16:11. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 6] [Cited by in RCA: 16] [Article Influence: 4.0] [Reference Citation Analysis (0)] |
| 23. | Arezzo A, Bini R, Lo Secco G, Verra M, Passera R. The role of stents in the management of colorectal complications: a systematic review. Surg Endosc. 2017;31:2720-2730. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 17] [Cited by in RCA: 11] [Article Influence: 1.4] [Reference Citation Analysis (0)] |
| 24. | Zeng K, Zhang F, Yang H, Zha X, Fang S. Laparoscopic versus open surgery in obstructive colorectal cancer patients following stents placement: a comprehensive meta-analysis of cohort studies. Surg Endosc. 2024;38:1740-1757. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 5] [Cited by in RCA: 3] [Article Influence: 3.0] [Reference Citation Analysis (0)] |
| 25. | Kanaka S, Yamada T, Matsuda A, Uehara K, Shinji S, Yokoyama Y, Takahashi G, Iwai T, Takeda K, Kuriyama S, Miyasaka T, Yoshida H. Short-term and three-year long-term outcomes of laparoscopic surgery versus open surgery for obstructive colorectal cancer following self-expandable metallic stent placement: a meta-analysis. Surg Endosc. 2024;38:5514-5527. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 2] [Reference Citation Analysis (0)] |
| 26. | Zhou XC, Ke FY, Dhamija G, Viroja RD, Huang CW. Application of metal stent implantation with endoscope and X-ray fluoroscopy combined laparoscopic surgery in the treatment of acute left hemicolon cancer obstruction. World J Surg Oncol. 2023;21:331. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1] [Cited by in RCA: 3] [Article Influence: 1.5] [Reference Citation Analysis (0)] |