Published online Sep 27, 2021. doi: 10.4240/wjgs.v13.i9.1095
Peer-review started: March 17, 2021
First decision: May 4, 2021
Revised: May 15, 2021
Accepted: August 20, 2021
Article in press: August 20, 2021
Published online: September 27, 2021
Processing time: 185 Days and 2.1 Hours
Synchronous colonic cancer incidence is uncommon, and awareness about this rare condition is improved recently. However, in the presence of acute colonic obstruction, investigation and management of synchronous colonic cancer can be difficult and challenging.
A patient presented with acute colonic obstruction with impending rupture and complete examination of this patient revealed the presence of three colonic can
The presence of multiple colonic cancers must be ruled out in order to plan the best management. We present the case with a review of literature and discuss the management of the case.
Core Tip: Synchronous colorectal cancer is not unusual. More than two colon cancers may be encountered occasionally. Consequently, the colon has to be fully evaluated before definitive surgery. However, in emergency situations such as obstructive cancer, investigation and management may become very challenging. We present and discuss about a case with three colon cancers at the same time, of which two were completely occlusive, rendering the management even more difficult.
- Citation: Bergeron E, Maniere T, Do XV, Bensoussan M, De Broux E. Three colonic cancers, two sites of complete occlusion, one patient: A case report. World J Gastrointest Surg 2021; 13(9): 1095-1101
- URL: https://www.wjgnet.com/1948-9366/full/v13/i9/1095.htm
- DOI: https://dx.doi.org/10.4240/wjgs.v13.i9.1095
Colorectal cancer (CRC) is the third most commonly diagnosed malignancy and the fourth leading cause of cancer death in the world[1]. The frequency of synchronous CRC (sCRC) may reach 20% in patients with familial adenomatous polyposis, hereditary non-polyposis colorectal cancer, chronic ulcerative colitis[2] and serrated polyposis syndrome[3]. In patients without these risk factors, prevalence of sCRC is estimated to be 3.5%[4], while the current improved awareness increased these estimates from 5% up to 8.4%[5-7].
Reports on the occurrence of triple or more sCRC range from 0.1% to 0.7%[8-13], and up to 1.6% in a recent review[7]. This review described a series of 1005 patients, of whom seven patients (0.7%) had four CRC and one patient (0.1%) had 5 CRC[7]. In another case, up to seven CRC in the same patient have been reported[14]. The importance of preoperative endoscopic examination of the entire colon to rule out polyps or secondary cancers is well established. However, in emergency situations such as obstruction, perforation or ischemic disease, management may become particularly challenging[1,15,16].
We report a patient who presented with acute and severe obstruction of the sigmoid colon due to a cancer, which was managed initially with a loop colostomy. The patient was subsequently discovered to have two more cancers on the right side, one of which was also completely occluding the caecum. The case and its management are discu
A 77-year-old patient presented at the emergency room on February 13th, 2019, with an overly distended abdomen.
The patient was vomiting fecaloid material for the last 24 h. He passed no stools or gas in the last three days.
The patient reported rectal bleeding for almost one year. He never had colonoscopy.
The patient is a diabetic male with obesity (Body mass index = 35). There is no personal or familial history of polyposis or inflammatory bowel disease. There was no colonic cancer in the family of the patient.
Upon arrival, vital signs were within the normal limits. The patient was afebrile. The abdomen was very tense but without signs of peritonitis. There was no mass on rectal exam.
Hemoglobin, white cell count, liver and renal function tests were within normal limits. Carcinoembryonic antigen (CEA) was 2.3 µg/L; (Normal: 0-4.9 µg/L). Colonoscopy was well tolerated. An obstructive cancer of the proximal sigmoid colon was confirmed. Two other cancers were found on the right side: one at the caecum and another one at the mid part of the ascending colon. No polyposis was found.
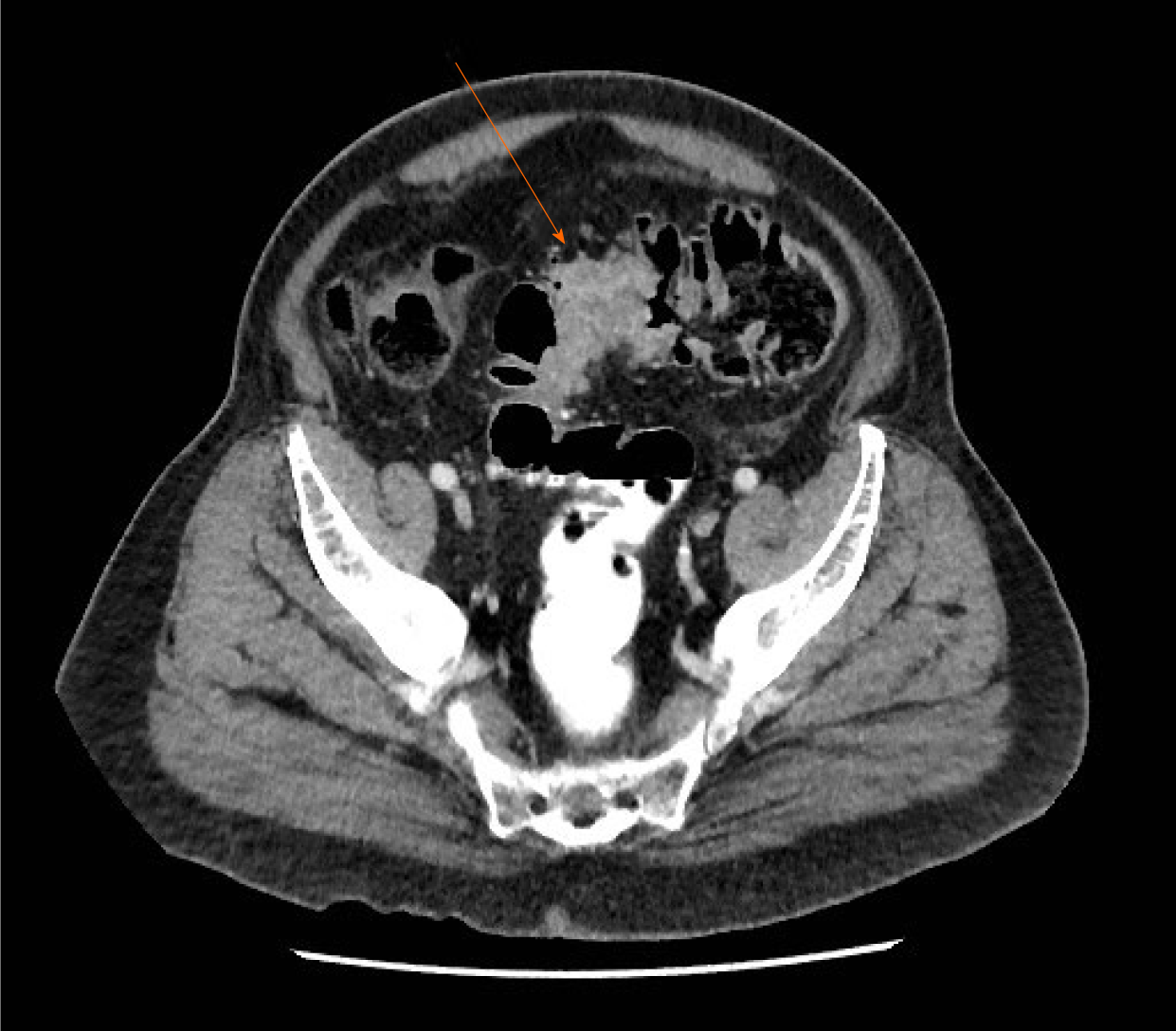
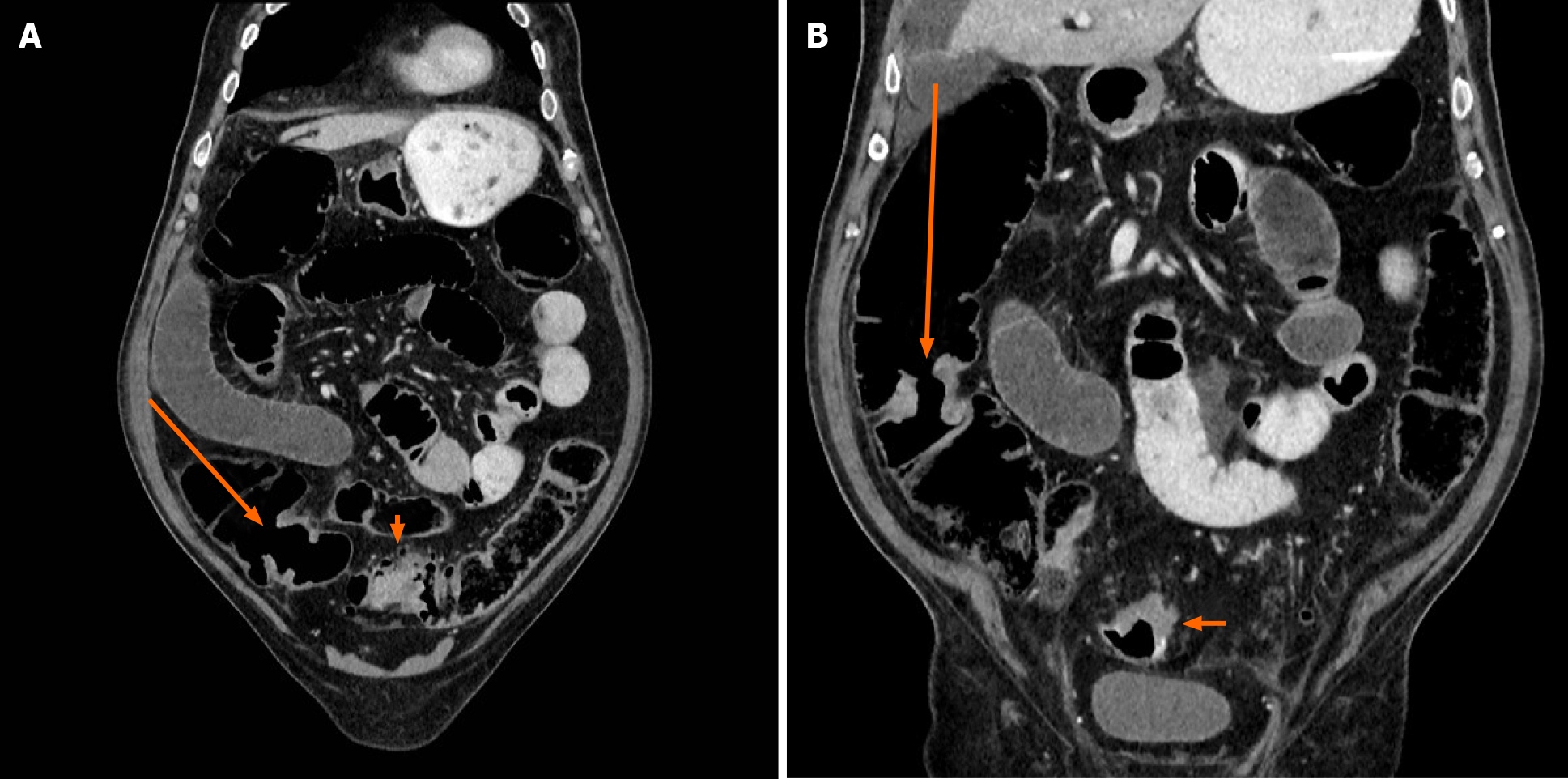
Computed tomography (CT)-scan showed significant dilatation of the small bowel loops and colon, secondary to a neoplastic sigmoid lesion (Figure 1). Some free fluid was also seen. There was no evidence of metastatic disease. Retrospectively, caecal (Figure 2A) and middle right colonic tumors (Figure 2B) could be identified on CT-scan but were difficult to diagnose prospectively in an emergency setting without associated acute bowel caliber change.
Three colonic cancers. Occlusive cancers at the ileocaecal valve and at sigmoid colon. Final pathology report identified three adenocarcinomas. The sigmoid cancer was a pT4 adenocarcinoma, invading the surrounding tissues. Incidentally, there was a con
The patient was initially hydrated. A nasogastric tube was installed, which evacuated brownish material. The patient was brought to the operating room during the evening and a left-sided loop colostomy was carried out. The colostomy was fashioned through a small left paramedian incision directly over the junction of the descending and sigmoid colon.
During the postoperative period, the colostomy was functional and allowed the stools to evacuate. The size of the abdomen significantly reduced. This window permi
The patient was planned for a total colectomy with ileorectal anastomosis, nine days after the first intervention. Meanwhile, there was recurrence of abdominal distension and the discharge from colostomy had become minimal. The intervention was done through a midline incision. It was technically difficult owing to the distended small bowel, secondary to an evident occlusion from the tumor of the caecum. The intestinal wall was diffusely thickened demonstrating a process originating for many weeks. There was no evidence of peritoneal metastases. A subtotal colectomy was carried out keeping as much distal sigmoid as possible to allow a side-to-side ileosigmoid anasto
One week later, postoperative course became complicated with an anastomotic leak that was treated with reoperation, drainage and proximal ileostomy. The patient had a further complicated course with abdominal abscesses, pneumonia, and enterocutaneous fistula originating from small bowel proximal to the ileostomy. This latter was treated with bowel rest and parenteral nutrition.
Hospital stay was for almost six months. Before discharge, the patient was reoperated after ensuring that the ileocolonic anastomosis was free of leakage and permeable. A short resection of the small bowel was done at the site of fistula and the ileostomy was closed. Postoperative period was uneventful. Because of the complicated postoperative course and the delay at discharge from the surgery, adjuvant chemotherapy was not planned.
One year later, there was no clinical or radiologic evidence of recurrent or metastatic disease. CEA was 5.8 µg/L (Normal: 0-4.9 µg/L). Endoscopic examination of the remaining 30 cm of the rectum and colon showed no lesion. An incisional hernia was repaired. Two years later, the patient is still functioning well and in good condition. However, CEA was found to be increased to 17.1 µg/L (Normal: 0-4.9 µg/L) subsequently, but no recurrent disease could be demonstrated with thoracoabdominal CT scan and positron emission tomography-CT. However, favourable clinical evolution notwithstanding, locoregional recurrence remains of concern.
CRC is the second and third most common malignancy in males and females, respe
Occurrence of three or more colon cancers at the same time in an individual is an unusual situation[7-13,15,18,19] but such incidence has been reported to be up to 1.6%[7]. Reports of the occurrence of two or more sCRC up to 12%[20] emphasize the mandatory investigation of the entire colon to rule out synchronous tumors and plan proper management[21].
The more challenging cases occur in patients presenting with a surgical emergency. Fifteen to 30% of sCRC cases present as an emergency occlusive situation[1,22,23]. The sigmoid colon is the most common location of CRC obstruction; 75% of the tumours are located distal to the splenic flexure[21].
In the present case, initial management was dictated by the overly distended abdomen in the patient in bad condition. Facing an occlusive sigmoid cancer while unaware of the concurrent occlusive caecal cancer, the possible management options at this time were proximal colostomy, Hartmann’s procedure or total colectomy[1]. However, the last two options take longer time and may be technically challenging, because of intestinal distension as well as potentially threatening procedures for the patient[1].
The colostomy allowed the patient to be stabilized and medically evaluated for subsequent procedure. Impending rupture of the colon and presence of stools contra
It is important to completely visualize the proximal colon through the colostomy, as well as the distal part of the large bowel through the rectum. Colonic stenting as a bridge to definitive surgery[24-26] was not considered in this situation due to potential impending rupture and immediate unavailability of this modality. Moreover, stent of an obstructing cancer is yet to be recommended as a standard treatment, and colo
If the obstructing lesion of the caecum had been identified initially, a total colectomy with or without ileostomy could have been carried out. However, due to the bad condition of the patient, such a procedure would have been technically difficult and potentially risky. A simple ileostomy would have left in place a close loop obstruction of the colon with a remaining risk of rupture. The proper management would have probably been damage control procedure with laparotomy, loop colostomy and ileostomy, leaving an open abdomen, stabilizing the medical condition, allowing the intestine to decompress, and proceeding with total or subtotal colectomy and ileocolonic anastomosis. Whatever the contemplated intervention, either of the options was associated with major concerns.
The complicated and prolonged postoperative course is unfortunate and beyond the scope of discussion. Consequently, the patient could not receive adjuvant chemo
This case emphasizes the importance to keep in mind, the possibility of additional colonic cancers that could be difficult to identify particularly in emergency and complicated situations. Reasonable efforts must be made to evaluate the entire colon in order to plan definitive management. A temporary colostomy in severe colonic obstruction allows the obstruction to resolve, the colon to be entirely evaluated, and the patient to be stabilized for definitive management. A total colectomy cannot be recommended straightaway[1] since a frequency of 3.5% for synchronous cancers[4] does not justify such an extensive procedure. Similarly, if a Hartmann’s procedure is done, investigation of the colon is mandatory before reoperation.
Considering this case and the review of literature, we can draw the following conclusions and recommendations: (1) Colon cancer has a high incidence, with a rate of sCRC between 3% and 12%, and thus represents a not so rare condition; (2) Obstructing colonic cancer is frequent at initial presentation and carries the same prevalence of sCRC; (3) A colostomy allows relieving obstruction of the colon and stabilization of a patient and gives access to the entire colon for investigation; (4) Every effort should be made to evaluate the entire colon and rectum before definitive treatment; and (5) The presence of two obstructing cancer at the same time remains a unique situation and management can be difficult.
Manuscript source: Unsolicited manuscript
Specialty type: Surgery
Country/Territory of origin: Canada
Peer-review report’s scientific quality classification
Grade A (Excellent): 0
Grade B (Very good): B
Grade C (Good): C
Grade D (Fair): 0
Grade E (Poor): 0
P-Reviewer: De Nardi P, Kim CW S-Editor: Wang JL L-Editor: A P-Editor: Wu RR
| 1. | Pisano M, Zorcolo L, Merli C, Cimbanassi S, Poiasina E, Ceresoli M, Agresta F, Allievi N, Bellanova G, Coccolini F, Coy C, Fugazzola P, Martinez CA, Montori G, Paolillo C, Penachim TJ, Pereira B, Reis T, Restivo A, Rezende-Neto J, Sartelli M, Valentino M, Abu-Zidan FM, Ashkenazi I, Bala M, Chiara O, De' Angelis N, Deidda S, De Simone B, Di Saverio S, Finotti E, Kenji I, Moore E, Wexner S, Biffl W, Coimbra R, Guttadauro A, Leppäniemi A, Maier R, Magnone S, Mefire AC, Peitzmann A, Sakakushev B, Sugrue M, Viale P, Weber D, Kashuk J, Fraga GP, Kluger I, Catena F, Ansaloni L. 2017 WSES guidelines on colon and rectal cancer emergencies: obstruction and perforation. World J Emerg Surg. 2018;13:36. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 244] [Cited by in RCA: 193] [Article Influence: 27.6] [Reference Citation Analysis (0)] |
| 2. | Gastrointestinal: synchronous and metachronous colorectal cancers. J Gastroenterol Hepatol. 2003;18:457. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 8] [Cited by in RCA: 6] [Article Influence: 0.3] [Reference Citation Analysis (0)] |
| 3. | Pyleris E, Koutsounas IS, Karantanos P. Three Colon Adenocarcinomas Arising in a Patient with Serrated Polyposis Syndrome: Case Report and Review of the Literature. Viszeralmedizin. 2014;30:136-139. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 2] [Cited by in RCA: 2] [Article Influence: 0.2] [Reference Citation Analysis (0)] |
| 4. | Lam AK, Chan SS, Leung M. Synchronous colorectal cancer: clinical, pathological and molecular implications. World J Gastroenterol. 2014;20:6815-6820. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in CrossRef: 118] [Cited by in RCA: 114] [Article Influence: 10.4] [Reference Citation Analysis (0)] |
| 5. | Bos ACRK, Matthijsen RA, van Erning FN, van Oijen MGH, Rutten HJT, Lemmens VEPP. Treatment and Outcome of Synchronous Colorectal Carcinomas: A Nationwide Study. Ann Surg Oncol. 2018;25:414-421. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 8] [Cited by in RCA: 13] [Article Influence: 1.6] [Reference Citation Analysis (0)] |
| 6. | Chin CC, Kuo YH, Chiang JM. Synchronous colorectal carcinoma: predisposing factors and characteristics. Colorectal Dis. 2019;21:432-440. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 10] [Cited by in RCA: 14] [Article Influence: 2.3] [Reference Citation Analysis (0)] |
| 7. | Kato T, Alonso S, Muto Y, Noda H, Miyakura Y, Suzuki K, Tsujinaka S, Saito M, Perucho M, Rikiyama T. Clinical characteristics of synchronous colorectal cancers in Japan. World J Surg Oncol. 2016;14:272. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 23] [Cited by in RCA: 13] [Article Influence: 1.4] [Reference Citation Analysis (0)] |
| 8. | Chen HS, Sheen-Chen SM. Synchronous and "early" metachronous colorectal adenocarcinoma: analysis of prognosis and current trends. Dis Colon Rectum. 2000;43:1093-1099. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 80] [Cited by in RCA: 71] [Article Influence: 2.8] [Reference Citation Analysis (0)] |
| 9. | Oya M, Takahashi S, Okuyama T, Yamaguchi M, Ueda Y. Synchronous colorectal carcinoma: clinico-pathological features and prognosis. Jpn J Clin Oncol. 2003;33:38-43. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 56] [Cited by in RCA: 63] [Article Influence: 2.9] [Reference Citation Analysis (0)] |
| 10. | Papadopoulos V, Michalopoulos A, Basdanis G, Papapolychroniadis K, Paramythiotis D, Fotiadis P, Berovalis P, Harlaftis N. Synchronous and metachronous colorectal carcinoma. Tech Coloproctol. 2004;8 Suppl 1:s97-s100. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 29] [Cited by in RCA: 33] [Article Influence: 1.7] [Reference Citation Analysis (0)] |
| 11. | Fukatsu H, Kato J, Nasu JI, Kawamoto H, Okada H, Yamamoto H, Sakaguchi K, Shiratori Y. Clinical characteristics of synchronous colorectal cancer are different according to tumour location. Dig Liver Dis. 2007;39:40-46. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 15] [Cited by in RCA: 16] [Article Influence: 0.9] [Reference Citation Analysis (0)] |
| 12. | Latournerie M, Jooste V, Cottet V, Lepage C, Faivre J, Bouvier AM. Epidemiology and prognosis of synchronous colorectal cancers. Br J Surg. 2008;95:1528-1533. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 53] [Cited by in RCA: 63] [Article Influence: 3.7] [Reference Citation Analysis (0)] |
| 13. | Bae JM, Cho NY, Kim TY, Kang GH. Clinicopathologic and molecular characteristics of synchronous colorectal cancers: heterogeneity of clinical outcome depending on microsatellite instability status of individual tumors. Dis Colon Rectum. 2012;55:181-190. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 18] [Cited by in RCA: 26] [Article Influence: 2.0] [Reference Citation Analysis (0)] |
| 14. | Kaibara N, Koga S, Jinnai D. Synchronous and metachronous malignancies of the colon and rectum in Japan with special reference to a coexisting early cancer. Cancer. 1984;54:1870-1874. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 4] [Reference Citation Analysis (0)] |
| 15. | Yeh CC, Hsi SC, Chuu CP, Kao YH. Synchronous triple carcinoma of the colon and rectum. World J Surg Oncol. 2013;11:66. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 6] [Cited by in RCA: 6] [Article Influence: 0.5] [Reference Citation Analysis (0)] |
| 16. | Park BS, Cho SH, Kim SJ, Kim TU, Kim DI, Son GM, Kim HS. Synchronous Quadruple Colon Cancer With Two Lesions Previously Obscured by Ischemic Colitis, Plus Bladder Cancer and Thymoma: A Case Report. Ann Coloproctol. 2021;37:S44-S47. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 2] [Cited by in RCA: 1] [Article Influence: 0.2] [Reference Citation Analysis (0)] |
| 17. | Mulder SA, Kranse R, Damhuis RA, de Wilt JH, Ouwendijk RJ, Kuipers EJ, van Leerdam ME. Prevalence and prognosis of synchronous colorectal cancer: a Dutch population-based study. Cancer Epidemiol. 2011;35:442-447. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 55] [Cited by in RCA: 60] [Article Influence: 4.3] [Reference Citation Analysis (0)] |
| 18. | Jiang X, Xu C, Tang D, Wang D. Laparoscopic subtotal colectomy for synchronous triple colorectal cancer: A case report. Oncol Lett. 2016;12:1525-1528. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 5] [Cited by in RCA: 4] [Article Influence: 0.4] [Reference Citation Analysis (0)] |
| 19. | Bádon ES, Mokánszki A, Mónus A, András C, Damjanovich L, Méhes G. Quadruplicate Synchronous Adenocarcinoma of the Colon with Distant Metastases-Long-Term Molecular Follow-Up by KRAS and TP53 Mutational Profiling. Diagnostics (Basel). 2020;10. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 1] [Cited by in RCA: 1] [Article Influence: 0.2] [Reference Citation Analysis (0)] |
| 20. | Yang J, Peng JY, Chen W. Synchronous colorectal cancers: a review of clinical features, diagnosis, treatment, and prognosis. Dig Surg. 2011;28:379-385. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 31] [Cited by in RCA: 35] [Article Influence: 2.5] [Reference Citation Analysis (0)] |
| 21. | Frago R, Ramirez E, Millan M, Kreisler E, del Valle E, Biondo S. Current management of acute malignant large bowel obstruction: a systematic review. Am J Surg. 2014;207:127-138. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 122] [Cited by in RCA: 125] [Article Influence: 10.4] [Reference Citation Analysis (0)] |
| 22. | Barnett A, Cedar A, Siddiqui F, Herzig D, Fowlkes E, Thomas CR Jr. Colorectal cancer emergencies. J Gastrointest Cancer. 2013;44:132-142. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 30] [Cited by in RCA: 36] [Article Influence: 3.0] [Reference Citation Analysis (0)] |
| 23. | Ansaloni L, Andersson RE, Bazzoli F, Catena F, Cennamo V, Di Saverio S, Fuccio L, Jeekel H, Leppäniemi A, Moore E, Pinna AD, Pisano M, Repici A, Sugarbaker PH, Tuech JJ. Guidelenines in the management of obstructing cancer of the left colon: consensus conference of the world society of emergency surgery (WSES) and peritoneum and surgery (PnS) society. World J Emerg Surg. 2010;5:29. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 130] [Cited by in RCA: 98] [Article Influence: 6.5] [Reference Citation Analysis (0)] |
| 24. | Trompetas V. Emergency management of malignant acute left-sided colonic obstruction. Ann R Coll Surg Engl. 2008;90:181-186. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 67] [Cited by in RCA: 56] [Article Influence: 3.3] [Reference Citation Analysis (0)] |
| 25. | Costas-Chavarri A, Nandakumar G, Temin S, Lopes G, Cervantes A, Cruz Correa M, Engineer R, Hamashima C, Ho GF, Huitzil FD, Malekzadeh Moghani M, Sharara AI, Stern MC, Teh C, Vázquez Manjarrez SE, Verjee A, Yantiss R, Shah MA. Treatment of Patients With Early-Stage Colorectal Cancer: ASCO Resource-Stratified Guideline. J Glob Oncol. 2019;5:1-19. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 39] [Cited by in RCA: 59] [Article Influence: 9.8] [Reference Citation Analysis (0)] |
| 26. | van Hooft JE, van Halsema EE, Vanbiervliet G, Beets-Tan RG, DeWitt JM, Donnellan F, Dumonceau JM, Glynne-Jones RG, Hassan C, Jiménez-Perez J, Meisner S, Muthusamy VR, Parker MC, Regimbeau JM, Sabbagh C, Sagar J, Tanis PJ, Vandervoort J, Webster GJ, Manes G, Barthet MA, Repici A; European Society of Gastrointestinal Endoscopy. Self-expandable metal stents for obstructing colonic and extracolonic cancer: European Society of Gastrointestinal Endoscopy (ESGE) Clinical Guideline. Endoscopy. 2014;46:990-1053. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 262] [Cited by in RCA: 218] [Article Influence: 19.8] [Reference Citation Analysis (0)] |
| 27. | Flor N, Zanchetta E, Di Leo G, Mezzanzanica M, Greco M, Carrafiello G, Sardanelli F. Synchronous colorectal cancer using CT colonography vs. other means: a systematic review and meta-analysis. Abdom Radiol (NY). 2018;43:3241-3249. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 6] [Cited by in RCA: 13] [Article Influence: 1.9] [Reference Citation Analysis (0)] |