Published online Oct 15, 2016. doi: 10.4251/wjgo.v8.i10.751
Peer-review started: April 3, 2016
First decision: May 17, 2016
Revised: June 8, 2016
Accepted: August 15, 2016
Article in press: August 17, 2016
Published online: October 15, 2016
Processing time: 185 Days and 13.5 Hours
Irreversible electroporation (IRE) is a non-thermal ablation technique used especially in locally advanced pancreatic carcinomas that are considered surgically unresectable. We present the first case of acute superior mesenteric artery (SMA) occlusion secondary to pancreatic IRE procedure that has not been reported before in the literature. A 66-year-old man underwent neoadjuvant chemoradiotherapy for locally advanced pancreatic ductal adenocarcinoma. IRE procedure was applied to the patient during laparotomy under general anesthesia. After finishing the procedure, an acute intestinal ischemia was detected. A conventional vascular angiography was performed and a metallic stent was successfully placed to the SMA and blood flow was maintained. It is important to be careful in such cases of tumor involvement of SMA when evaluating for IRE procedure of pancreatic tumor.
Core tip: Irreversible electroporation (IRE) is a non-thermal ablation technique is a hope for patients who have unresectable locally advanced pancreatic carcinomas; especially, when any vascular surgical approach is impossible because of the tumor involvement. We encountered superior mesenteric artery occlusion after IRE procedure for locally advanced pancreatic cancer. We suggest that treating physicians should keep in mind that kind of mortal vascular complications of IRE. Stent placement via angiography could be the lifesaving treatment choice for vascular occlusions due to IRE procedure.
- Citation: Ekici Y, Tezcaner T, Aydın HO, Boyvat F, Moray G. Arterial complication of irreversible electroporation procedure for locally advanced pancreatic cancer. World J Gastrointest Oncol 2016; 8(10): 751-756
- URL: https://www.wjgnet.com/1948-5204/full/v8/i10/751.htm
- DOI: https://dx.doi.org/10.4251/wjgo.v8.i10.751
The majority of the pancreatic adenocarcinomas are diagnosed at an advanced stage, with resectable tumors being identified in only 10%-20% of the cases at the time of first admission[1]. Involvement of the celiac trunk, superior mesenteric artery or portal vein without distant metastasis is observed in 40% of cases with stage 3 disease[2,3]. For these patients, a 5-year survival rate of 6.8% has been reported following surgical resection[4]. These patients are now classified as locally advanced stage pancreatic cancer (LAPC), and their survival rates are reportedly better compared to patients with distant metastasis. The probability of surgical resection following neoadjuvant treatment is higher in these patients[5]. Nowadays, different ablation techniques are being studied in combination with neoadjuvant treatment[6]. Some thermal ablation techniques such as radiofrequency ablation (RFA), cryoablation and microwave ablation have been developed and defined for tumor ablation. Thermal ablation methods are reported to cause necrosis during treatment for LAPC through thermal injury in the peripancreatic fatty tissue, main vascular structures, pancreatic tissue, duodenum and biliary tract[7]. These morbid complications are limitations of these techniques for pancreatic tumors.
Irreversible electroporation (IRE) creates pores in cell membrane by transmitting short electrical currents at high voltage[8]. As a result, the phospholipid membrane of the cell is permanently damaged, and the apoptosis and necrosis complex is observed due to the impairment of cellular homeostasis. Since IRE is not a thermal ablation technique, it is assumed that it is affected to a lesser extent from the vascular flow surrounding the tissue[9]. No decrease in ablation energy is observed, due to the effect on the main vascular blood flow. Also, due to the shorter duration of treatment, a larger affected tissue volume, and a lower pain response, this technique is considered to be superior to other ablation techniques[10]. Previous studies demonstrated that IRE use in the treatment of locally advanced pancreatic cancer was safe, since it resulted in no harm to the peripancreatic tissues and did not affect the superior mesenteric artery, porta hepatis and biliary tract[11]. Metallic stent removal is recommended prior to the use of IRE in cases where a metallic stent is applied in the biliary tract for biliary obstruction. It is believed that the presence of a metallic stent in the field of electrical flow within the duodenum may result in damage to the adjacent structures [12].
Studies conducted in various centers around the world have reported the short and long term protocol of IRE to be effective in the treatment of LAPD. In these studies no important morbid complication was reported like SMA occlusion. However, in this case report, we draw attention to a previously unpublished complication of IRE in LAPC.
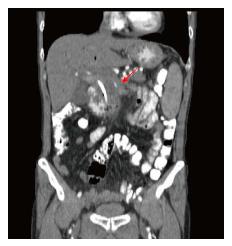
A 66-year-old man with locally advanced pancreatic head adenocarcinoma diagnosed by fine-needle aspiration biopsy 6 mo ago was admitted to our institution. Tumor markers were measured, with CA 19-9 = 4801 IU/mL and CA 125 = 161 IU/mL. After diagnosis, a plastic stent was placed in ductus choledocus with ERCP. Immediately afterwards, chemoradiation was administered to the patients [5 cycles of chemotherapy consisting of Folfox + 5-FU + Oxaliplatin every 14 d, for 28 d RTA (28 fractions 50, 4 gray IMRT received)]. After admission to our hospital, computerized tomography (CT) examination was performed to the patient, and a malignant mass of 45 mm in diameter was observed at the pancreatic head level (Figure 1). It was noted that the tumor had surrounded the superior mesenteric artery 360 degrees, the affected segment of SMA was 40 mm. The tumor had apparently reduced the SMA diameter by 3 mm (Figure 1). Main pancreatic duct was markedly dilated, and the diameter was measured as approximately 7 mm. There was no metastasis and the tumor was stable after neoadjuvant chemotherapy.
The patient was referred to our hospital with a diagnosis of LAPC. Irreversible electroporation for pancreatic tumor and simultaneous gastrojejunostomy was planned. The abdomen was opened with a median incision above the umbilicus and abdominal exploration was performed. During the exploration, no distant metastases were identified anywhere in the abdomen. Intraoperative liver ultrasonography was used to detect possible metastasis to liver. The patient was under general anesthesia, surgery was performed in the supine position. The gastro-colic omentum was opened to reach and expose the pancreatic tumor. Electroporation was performed in accordance with the procedural instructions.
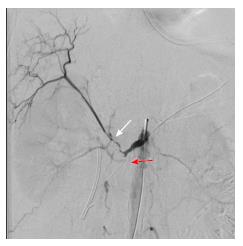
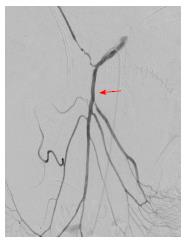
IRE was performed using the Nanoknife System (Angiodynamics, Lanthan), as described in the previous manuscript on IRE for the pancreas. High definition intraoperative ultrasound imaging was used in all cases, which is required to demonstrate non-traumatic precise needle placement and also for continuous ablation assessment during IRE. In sum, 3 monopolar probes with 2-cm spacing will deliver an electroporation defect of approximately 3.5 cm axial, 2.5 cm anterior-posterior, and 2.5 cm cranial-caudal. This electroporation procedure is achieved through a maximum of 1.5 cm exposure, 1500 V/cm, and 100 s wavelength. The procedure was performed in 45 min. After IRE procedure a gastrojejunostomy completed. After completing gastrojejunostomy anastomosis, a color change was concurrently observed in the small intestine. Based on a suspicion of SMA occlusion, arterial pulse was checked in the small bowel mesentery. No pulse was obtained in this area. The abdomen of the patient was closed, and he was taken to the angiography unit because SMA occlusion developed in the tumor surrounded segment. In angiography images, it was observed that a short segment after the origin of SMA, right hepatic artery was arising. Even after 1 cm distal to right hepatic artery origin there was no blood flow in the SMA (Figure 2). First of all, occluded segment was dilated with a 3 mm balloon. After dilatation a 4 mm and 3 cm length metallic stent was placed to this dilated segment (Figure 3). There were no complications in the postoperative follow-up. The patient was discharged without any complication the sixth day postoperatively.
Nearly 30% to 40% of patients with pancreatic adenocarcinoma have a locally advanced disease with stage III at the time of diagnosis and half of the tumors involved celiac axis and SMA. Autopsy studies have demonstrated that 30% of the patients with pancreatic cancer are in locally advanced stage with no distant metastasis[13]. Chemoradiotherapy used in the conventional treatment of such patients is of limited efficacy. In the past, hepaticojejunostomy or gastrojejunostomy were commonly used in the palliative surgical treatment of patients with LAPC. IRE is a new hope for the patients’ with LAPC in locally control of pancreatic cancer with survival benefits. We perform IRE for LAPC invaded or encapsulated superior mesenteric artery in the absence of distant metastasis. We perform 3 to 5 per annually IRE since 2013 in our institution.
In the classical surgical approach, pancreaticoduodenectomy (PD) is preferred in resectable pancreatic carcinomas. Although acute occlusion or thrombosis in the hepatic artery, portal vein, SMA or celiac artery are rarely observed following this operation, they are still considered as the most significant causes of mortality. Gaujoux et al[14] preoperatively evaluated 545 patients who underwent PD, by arterial reconstruction, examining SMA and celiac artery stenosis with CT, and detecting hemodynamically significant stenosis is 27 (5%) of the patients. On the other hand, five patients died due to undetectable stenosis and ischemic complications. Stent placement and bypass procedures were preoperatively performed in those patients, with an effort being made to prevent postoperative ischemic complications. Overall, the rate of complications was reported as 2.6%. It was observed that 36% of these complications were ischemic complications associated with undetectable stenosis[14]. Other studies in the literature recommend the application of CT, angiography or intraoperative Doppler ultrasonography, and clamping the gastroduodenal artery for the diagnosis of SMA occlusion[15]. Median arcuate ligament compression, atherosclerotic stenosis or fibromuscular dysplasia and tumor involvement of SMA might be the cause of acute occlusion of SMA in patients with pancreatic cancer[16]. Recommended treatment modalities in acute SMA occlusion include thrombectomy, revascularization with side-to-side or end-to-side anastomosis, and stent application by angiography[17]. While SMA occlusion is rarely observed during PD, acute SMA occlusion has never been previously reported in the literature in patients who underwent IRE. The impaired blood supply in the jejunal segments, which was noticed intraoperatively in our case presented here, enables the detection of SMA occlusion. Since access to the occluded segment in our case would be easier by vascular angiography, stent placement was preferred for treatment choice. Accessing the SMA surgically, on the other hand, was not possible because of tumor involvement. Therefore, by using angiography, diagnosis and treatment were both performed at the same time.
Owing to the imaging techniques used today, LAPC can be diagnosed preoperatively. Endoscopically applied biliary and/or duodenal stents provide a chance for palliative treatment by eliminating the risk of surgical morbidity for the patient[18]. Currently defined thermal ablation techniques are known to be inefficient for adequate ablation of tumor cells adjacent to vascular structures due to the heat sink effect. IRE provides non-thermal ablation in tumor cells through the short electrical currents with high amplitude. Therefore, it can be applied in LAPC without being affected from the flow in portal vein, celiac artery, biliary tract or SMA. However, IRE modulates vascular smooth muscle cells to apoptosis; but it has been demonstrated that elastin and collagen in particular, which are present in vascular structures, have been affected from this ablation technique[19]. After IRE blood flow is intact and vascular smooth muscle cells repopulate in a short time period[19]. The method’s efficacy was demonstrated in studies performed on large tumor areas, where its application was associated with shorter times and lesser complications. Folfirinox or gemcitabine based chemotherapy is used for approximately 4 mo in the first line treatment of LAPC, and its efficacy is approved by the National Comprehensive Network Guideline[20].
In a study by Martin et al[21], 54 patients who underwent IRE were compared with 85 patients who were admitted for standard chemotherapy. At the end of the study, no significant differences were found in overall survival and progression-free survival between patients who underwent systemic chemotherapy for 4 mo and who underwent IRE treatment[21]. The overall survival results of the IRE applied to 200 patients revealed no significant differences with patients receiving chemoradiotherapy and it was recommended that chemoradiotherapy, is used along with IRE as part of a triple treatment protocol. In this multicenter study, minor complications were observed among those 200 patients, but no case of acute vascular occlusion was encountered[22]. Other studies with large series demonstrated that application of IRE was safe and efficient around vascular structures[23].
Unexpected complications are being reported as clinical studies are continuing. Following application of this technique, various complications have been reported secondary to electrical transmission, especially in patients with metallic biliary stents or enteric stents[12].
In the review of the literature, we did not encounter any study on SMA occlusion following IRE application, as was the case with our patient presented herein. A recent systematic review reported an IRE-related complication rate of 13%, with an IRE-related mortality of 2%[24]. Martin et al[22], in a recent study with a population of 200 patients suffering from LAPC treated with IRE, showed an overall rate of adverse events of 37% (74 patients with 149 overall complications) and a mortality rate of 2%. The most common complications (including both percutaneous and open techniques) described after the use of IRE on pancreas are pancreatitis, pneumothorax, hematoma, abdominal pain, bile leakage, pancreatic leakage, duodenal leakage, duodenal ulcer, deep vein thrombosis/pulmonary embolism and superior mesenteric venous occlusion.
In healthy individuals average diameter of SMA was reported between 7.3 and 5.9 mm[24]. The measured diameter of SMA in this case with CT scan was 3 mm. The tumor involved the artery and decreased its diameter nearly 50%. After the IRE procedure edema may developed around the ablation area or at the wall of the artery may especially cause an SMA occlusion. SMA occlusion and intestinal ischemia was noticed earlier in the present case, since IRE was applied simultaneously with open surgery, and this condition was treated by an angiographically applied vascular stent before necrosis developed in the jejunal segments. It is more important to be careful in percutaneous IRE procedures for LAPC because it is difficult to diagnose intestinal ischemia such a short time period.
The anatomy of the hepatic artery varies substantially. Reported rate of replaced right hepatic artery from SMA ranges from 5% to 25%[25]. A variant artery is an important risk factor when the surgeon unaware of this anomaly. It is possible to progress the thrombosis to the stump of right hepatic artery in such cases. This is another possible fatal complication of SMA occlusion when hepatic artery arises from SMA. The liver and gut will become necrotic within a few hours.
Recently, percutaneous IRE application has been tried and its results in terms of overall survival were observed to be positive[26]. Placement of probes could be both percutaneous and surgical; it depends on localization of the lesion and experience of the team. One should pay attention to acute vascular occlusions that might develop in such cases. It is also necessary to bear in mind that acute vascular occlusions might develop during percutaneous or surgical IRE application in LAPC.
IRE expands the scope of treatment of lesions that is near to major vascular/biliary/urinary structures. Because of this adjacency, these lesions are not suitable for local ablative therapies and could only be try to treat with some forms of external beam radiation therapy. In order to prevent injury of these major structures by displacement of electrodes, there is a need for general anesthesia (deep paralysis)[23]. The only contraindication of IRE is patients with pacemakers or with cardiac arrhythmias[27]. IRE is mostly applied for locally advanced tumors invaded to adjacent structures. As in our case, if there is a severe vascular invasion is decreasing the diameter more than 50%, a coated vascular stent could be placed to the narrowed segment before applying IRE.
In conclusion, we present a new and fatal complication of IRE procedure for LAPC. In our patient, the diameter of SMA was decreased over 50% when compared with a healthy individuals SMA. We think that both arterial narrowing and IRE depend tissue edema are affective factors for acute SMA occlusion. However, it might also be speculated that the monopolar probes itself caused direct SMA injury or induced, e.g., a small hematoma in the vicinity of the SMA, resulting in occlusion of the already narrowed vessel.
A 66-year-old man presented with locally advanced pancreatic head adenocarcinoma.
Chronic inflammation, desmoids reaction around the tumor.
Tumor markers were measured, with CA 19-9 = 4801 IU/mL and CA 125 = 161 IU/mL.
Computerized tomography examination revealed a malignant mass of 45 mm in diameter was observed at the pancreatic head level and the tumor had surrounded the superior mesenteric artery 360 degrees.
The patient received systemic chemotherapy following irreversible electroporation.
This case is a unique case of superior mesenteric artery occlusion as a complication of irreversible electroporation.
Irreversible electroporation creates pores in cell membrane by transmitting short electrical currents at high voltage. As a result, the phospholipid membrane of the cell is permanently damaged, and the apoptosis and necrosis complex is observed due to the impairment of cellular homeostasis.
While a general clinical decision making algorithm would not be appropriate and each clinical situation needs to be individualized. As in this case, if there is a severe vascular invasion is decreasing the diameter more than 50%, a coated vascular stent could be placed to the narrowed segment before applying irreversible electroporation.
The manuscript by Ekici et al describes a case of arterial complication following irreversible electroporation (IRE) for locally advanced pancreatic cancer. IRE is one of the new methods for local therapy of non-metastatic but locally advanced pancreatic cancers. The present case report is both timely and important, highlighting a potential adverse event using this technique.
Manuscript source: Invited manuscript
Specialty type: Gastroenterology and hepatology
Country of origin: Turkey
Peer-review report classification
Grade A (Excellent): 0
Grade B (Very good): B, B
Grade C (Good): 0
Grade D (Fair): 0
Grade E (Poor): 0
P- Reviewer: Kleeff J, Minaga K S- Editor: Gong ZM L- Editor: A E- Editor: Lu YJ
| 1. | American Cancer Society. Cancer Facts & Figures 2011. Atlanta: American Cancer Society 2011; . |
| 2. | Arnoletti JP, Frolov A, Eloubeidi M, Keene K, Posey J, Wood T, Greeno E, Jhala N, Varadarajulu S, Russo S. A phase I study evaluating the role of the anti-epidermal growth factor receptor (EGFR) antibody cetuximab as a radiosensitizer with chemoradiation for locally advanced pancreatic cancer. Cancer Chemother Pharmacol. 2011;67:891-897. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 22] [Cited by in RCA: 26] [Article Influence: 1.9] [Reference Citation Analysis (0)] |
| 3. | Callery MP, Chang KJ, Fishman EK, Talamonti MS, William Traverso L, Linehan DC. Pretreatment assessment of resectable and borderline resectable pancreatic cancer: expert consensus statement. Ann Surg Oncol. 2009;16:1727-1733. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 717] [Cited by in RCA: 618] [Article Influence: 38.6] [Reference Citation Analysis (0)] |
| 4. | Bilimoria KY, Bentrem DJ, Merkow RP, Tomlinson JS, Stewart AK, Ko CY, Talamonti MS. Application of the pancreatic adenocarcinoma staging system to pancreatic neuroendocrine tumors. J Am Coll Surg. 2007;205:558-563. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 89] [Cited by in RCA: 88] [Article Influence: 4.9] [Reference Citation Analysis (0)] |
| 5. | Gillen S, Schuster T, Meyer Zum Büschenfelde C, Friess H, Kleeff J. Preoperative/neoadjuvant therapy in pancreatic cancer: a systematic review and metaanalysis of response and resection percentages. PLoS Med. 2010;7:e1000267. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 1243] [Cited by in RCA: 1170] [Article Influence: 78.0] [Reference Citation Analysis (1)] |
| 6. | Li J, Chen X, Yang H, Wang X, Yuan D, Zeng Y, Wen T, Yan L, Li B. Tumour cryoablation combined with palliative bypass surgery in the treatment of unresectable pancreatic cancer: a retrospective study of 142 patients. Postgrad Med J. 2011;87:89-95. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 17] [Cited by in RCA: 20] [Article Influence: 1.3] [Reference Citation Analysis (0)] |
| 7. | Pezzilli R, Serra C, Ricci C, Casadei R, Monari F, D’Ambra M, Minni F. Radiofrequency ablation for advanced ductal pancreatic carcinoma: is this approach beneficial for our patients? A systematic review. Pancreas. 2011;40:163-165. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 23] [Cited by in RCA: 24] [Article Influence: 1.7] [Reference Citation Analysis (0)] |
| 8. | Al-Sakere B, André F, Bernat C, Connault E, Opolon P, Davalos RV, Rubinsky B, Mir LM. Tumor ablation with irreversible electroporation. PLoS One. 2007;2:e1135. [PubMed] |
| 9. | Lee EW, Thai S, Kee ST. Irreversible electroporation: a novel image-guided cancer therapy. Gut Liver. 2010;4 Suppl 1:S99-S104. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 106] [Cited by in RCA: 105] [Article Influence: 7.0] [Reference Citation Analysis (0)] |
| 10. | Narayanan G, Hosein PJ, Arora G, Barbery KJ, Froud T, Livingstone AS, Franceschi D, Rocha Lima CM, Yrizarry J. Percutaneous irreversible electroporation for downstaging and control of unresectable pancreatic adenocarcinoma. J Vasc Interv Radiol. 2012;23:1613-1621. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 151] [Cited by in RCA: 163] [Article Influence: 13.6] [Reference Citation Analysis (0)] |
| 11. | Månsson C, Nilsson A, Karlson BM. Severe complications with irreversible electroporation of the pancreas in the presence of a metallic stent: a warning of a procedure that never should be performed. Acta Radiol Short Rep. 2014;3:2047981614556409. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 13] [Cited by in RCA: 21] [Article Influence: 1.9] [Reference Citation Analysis (0)] |
| 12. | Iacobuzio-Donahue CA, Fu B, Yachida S, Luo M, Abe H, Henderson CM, Vilardell F, Wang Z, Keller JW, Banerjee P. DPC4 gene status of the primary carcinoma correlates with patterns of failure in patients with pancreatic cancer. J Clin Oncol. 2009;27:1806-1813. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 770] [Cited by in RCA: 853] [Article Influence: 53.3] [Reference Citation Analysis (0)] |
| 13. | Gaujoux S, Sauvanet A, Vullierme MP, Cortes A, Dokmak S, Sibert A, Vilgrain V, Belghiti J. Ischemic complications after pancreaticoduodenectomy: incidence, prevention, and management. Ann Surg. 2009;249:111-117. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 130] [Cited by in RCA: 130] [Article Influence: 8.1] [Reference Citation Analysis (0)] |
| 14. | Machado MA, Herman P, Montagnini AL, Costa ML, Nishinari K, Wolosker N, Machado MC. A new test to avoid arterial complications during pancreaticoduodenectomy. Hepatogastroenterology. 2004;51:1671-1673. [PubMed] |
| 15. | Fortner JG, Watson RC. Median arcuate ligament obstruction of celiac axis and pancreatic cancer. Ann Surg. 1981;194:698-700. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 29] [Cited by in RCA: 34] [Article Influence: 0.8] [Reference Citation Analysis (0)] |
| 16. | Halazun KJ, Kotru A, Menon KV, Patel J, Prasad KR. Stenting of coeliac axis stenosis facilitates pancreatectomy. Eur J Surg Oncol. 2006;32:811-812. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 9] [Cited by in RCA: 11] [Article Influence: 0.6] [Reference Citation Analysis (0)] |
| 17. | Kneuertz PJ, Cunningham SC, Cameron JL, Torrez S, Tapazoglou N, Herman JM, Makary MA, Eckhauser F, Wang J, Hirose K. Palliative surgical management of patients with unresectable pancreatic adenocarcinoma: trends and lessons learned from a large, single institution experience. J Gastrointest Surg. 2011;15:1917-1927. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 72] [Cited by in RCA: 66] [Article Influence: 4.7] [Reference Citation Analysis (0)] |
| 18. | Maor E, Rubinsky B. Endovascular nonthermal irreversible electroporation: a finite element analysis. J Biomech Eng. 2010;132:031008. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 16] [Cited by in RCA: 19] [Article Influence: 1.3] [Reference Citation Analysis (0)] |
| 19. | Gourgou-Bourgade S, Bascoul-Mollevi C, Desseigne F, Ychou M, Bouché O, Guimbaud R, Bécouarn Y, Adenis A, Raoul JL, Boige V. Impact of FOLFIRINOX compared with gemcitabine on quality of life in patients with metastatic pancreatic cancer: results from the PRODIGE 4/ACCORD 11 randomized trial. J Clin Oncol. 2013;31:23-29. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 301] [Cited by in RCA: 341] [Article Influence: 26.2] [Reference Citation Analysis (0)] |
| 20. | Martin RC, McFarland K, Ellis S, Velanovich V. Irreversible electroporation in locally advanced pancreatic cancer: potential improved overall survival. Ann Surg Oncol. 2013;20 Suppl 3:S443-S449. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 184] [Cited by in RCA: 199] [Article Influence: 15.3] [Reference Citation Analysis (0)] |
| 21. | Martin RC, Kwon D, Chalikonda S, Sellers M, Kotz E, Scoggins C, McMasters KM, Watkins K. Treatment of 200 locally advanced (stage III) pancreatic adenocarcinoma patients with irreversible electroporation: safety and efficacy. Ann Surg. 2015;262:486-494; discussion 492-494. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 255] [Cited by in RCA: 294] [Article Influence: 29.4] [Reference Citation Analysis (0)] |
| 22. | Martin RC, Philips P, Ellis S, Hayes D, Bagla S. Irreversible electroporation of unresectable soft tissue tumors with vascular invasion: effective palliation. BMC Cancer. 2014;14:540. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 39] [Cited by in RCA: 41] [Article Influence: 3.7] [Reference Citation Analysis (0)] |
| 23. | Perko MJ. Duplex ultrasound for assessment of superior mesenteric artery blood flow. Eur J Vasc Endovasc Surg. 2001;21:106-117. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 83] [Cited by in RCA: 76] [Article Influence: 3.2] [Reference Citation Analysis (0)] |
| 24. | Sangam MR. Replaced right hepatic artery arising from superior mesenteric artery. Ind J Basic and App Med Resch. 2013;3:1-5. |
| 25. | Bagla S, Papadouris D. Percutaneous irreversible electroporation of surgically unresectable pancreatic cancer: a case report. J Vasc Interv Radiol. 2012;23:142-145. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 49] [Cited by in RCA: 52] [Article Influence: 4.0] [Reference Citation Analysis (0)] |
| 26. | Kingham TP, Karkar AM, D’Angelica MI, Allen PJ, DeMatteo RP, Getrajdman GI, Sofocleous CT, Solomon SB, Jarnagin WR, Fong Y. Ablation of perivascular hepatic malignant tumors with irreversible electroporation. J Am Coll Surg. 2012;215:379-387. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 185] [Cited by in RCA: 192] [Article Influence: 14.8] [Reference Citation Analysis (0)] |