Published online Jan 15, 2023. doi: 10.4251/wjgo.v15.i1.55
Peer-review started: September 20, 2022
First decision: October 14, 2022
Revised: October 28, 2022
Accepted: December 6, 2022
Article in press: December 6, 2022
Published online: January 15, 2023
Processing time: 111 Days and 16.8 Hours
In recent years, immune checkpoint inhibitors (ICIs) have made significant breakthroughs in the treatment of various tumors, greatly improving clinical efficacy. As the fifth most common antitumor treatment strategy for patients with solid tumors after surgery, chemotherapy, radiotherapy and targeted therapy, the therapeutic response to ICIs largely depends on the number and spatial distribution of effector T cells that can effectively identify and kill tumor cells, features that are also important when distinguishing malignant tumors from “cold tumors” or “hot tumors”. At present, only a small proportion of colorectal cancer (CRC) patients with deficient mismatch repair (dMMR) or who are microsatellite instability-high (MSI-H) can benefit from ICI treatments because these patients have the characteristics of a “hot tumor”, with a high tumor mutational burden (TMB) and massive immune cell infiltration, making the tumor more easily recognized by the immune system. In contrast, a majority of CRC patients with proficient MMR (pMMR) or who are microsatellite stable (MSS) have a low TMB, lack immune cell infiltration, and have almost no response to immune monotherapy; thus, these tumors are “cold”. The greatest challenge today is how to improve the immunotherapy response of “cold tumor” patients. With the development of clinical research, immunotherapies combined with other treatment strategies (such as targeted therapy, chemotherapy, and radiotherapy) have now become potentially effective clinical strategies and research hotspots. Therefore, the question of how to promote the transformation of “cold tumors” to “hot tumors” and break through the bottleneck of immunotherapy for cold tumors in CRC patients urgently requires consideration. Only by developing an in-depth understanding of the immunotherapy mechanisms of cold CRCs can we screen out the immunotherapy-dominant groups and explore the most suitable treatment options for individuals to improve therapeutic efficacy.
Core Tip: This review focuses on the potential mechanism of immunotherapy ineffectiveness in colorectal cancer patients with “cold tumors”, how to increase the infiltration of effector T cells at tumor sites by combination therapy strategies, how to transform “cold tumors” into “hot tumors” to expand the number of people benefiting from immunotherapy, and make recommendations on how to screen out immune-dominant populations in the future.
- Citation: Li DD, Tang YL, Wang X. Challenges and exploration for immunotherapies targeting cold colorectal cancer. World J Gastrointest Oncol 2023; 15(1): 55-68
- URL: https://www.wjgnet.com/1948-5204/full/v15/i1/55.htm
- DOI: https://dx.doi.org/10.4251/wjgo.v15.i1.55
As one of the most common gastrointestinal malignancies, colorectal cancer (CRC) ranks third in incidence and second in tumor-related mortality among common malignant tumors in the world[1]. With the in-depth exploration of the pathogenesis of CRC, immune checkpoint inhibitors (ICIs) have gradually entered the field as an antitumor treatment for CRC. Current tumor immunotherapy strategies include oncolytic virus (OV) therapy, monoclonal antibodies, ICIs, cytokine therapy, tumor vaccines, and adoptive cell therapy[2,3], and these strategies are characterized by the enhancement of innate and adaptive immunity to clear tumor cells, with the aim of inducing a durable and effective antitumor immune response. Regardless of whether the tumor type is classified as deficient mismatch repair (dMMR) or microsatellite instability-high (MSI-H) or proficient MMR (pMMR) or microsatellite stable (MSS), the antitumor effects of ICIs ultimately rely on CD8+ T cells and tumor-infiltrating lymphocytes, which have been confirmed in numerous studies to be important features that distinguish malignancies from “cold tumors” or “hot tumors”[4]. In a phase 2 clinical trial comparing the efficacy of dMMR or pMMR CRC with pembrolizumab immunomonotherapy, the median progression-free survival (mPFS) was 5 mo and 2 mo in patients with dMMR and pMMR, respectively. In addition, the objective response rate (ORR) was 40% for dMMR CRC, and there was no response for patients with pMMR CRC[5]. It can be concluded that patients with pMMR/MSS CRC who exhibit traits of “cold tumors” do not benefit from programmed cell death protein 1 (PD-1) inhibitor therapy[6,7]. The results of a meta-analysis by Li et al[8] also confirmed this conclusion. However, dMMR patients make up the vast majority of all CRC patients as accounting for 95%[9]. At present, the exploration of the reasons for the poor efficacy of immunotherapy in dMMR CRC patients and whether its efficacy can be improved has become a hot issue worldwide.
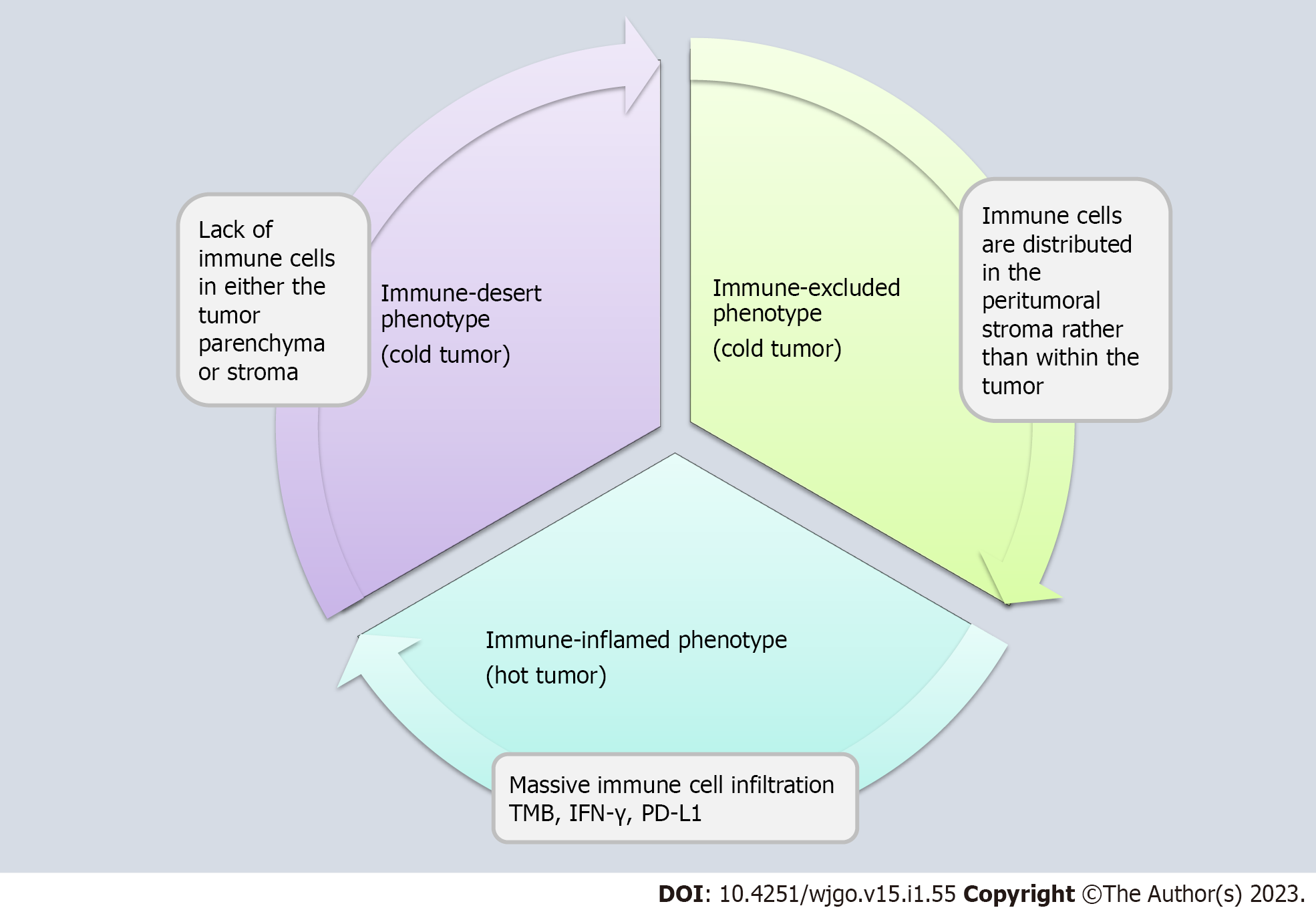
In 2017, Chen and Mellman[6] pointed out that tumors can be divided into three immune phenotypes, the immune-inflamed, the immune-excluded and the immune-desert phenotypes, which are based on PD-1 ligand (PD-L1) expression, the total number of immune cells, and their spatial distribution in the tumor microenvironment (Figure 1). High levels of immunocyte infiltration, a high tumor mutational burden (TMB), and high interferon-γ (IFN-γ) signal transduction and PD-L1 expression are the characteristics that define immunoinflammatory tumors and are also key to the success of antitumor immunotherapy[10,11]. The immune-inflamed phenotype is characterized by a large number of immune cells in the tumor parenchyma, also known as a “hot tumor”, which is often sensitive to ICIs[12]. In contrast, although there are a large number of immune cells in the immune-excluded phenotype, the immune cells are mainly distributed in the stroma around the tumor rather than within the tumor. Tumors of this phenotype are less responsive to immunotherapy. The immune-desert phenotype is characterized by a lack of immune cells in both the parenchyma and stroma of the tumor; such tumors rarely respond to immunotherapy[6]. The immune-excluded and the immune-desert phenotypes also have a low TMB and low expression of histocompatibility complex class I (MHC I); these tumors are called “cold tumors”[11,13]. Studies have shown that poor sensitivity to immune checkpoint suppression monotherapy in patients with “cold tumors” is associated with congenital immune deficiency or the suppression of innate antitumor immunity[6,14]. It can be concluded that the most effective way to increase the response of “cold tumors” to immunotherapy is to eliminate barriers to tumor immunosuppression and immune escape mechanisms, thereby establishing or maintaining an adaptive immune response.
For effector T cells to exert antitumor immunity, a complete immune cycle process, in which many factors that can influence T cell priming and homing to the tumor site, including a lack of tumor antigens, a defect in antigen-presenting cells (APCs), a lack of T-cell activation and defects in homing to the tumor bed, is required. All of these processes can lead to a T cell-inflamed phenotype and antitumor immunity failure[14]. Therefore, an in-depth understanding of the various mechanisms of T cell infiltration impairment and how immunocombination therapy strategies affect the immune system’s anti-tumor ability is critical for understanding the transformation of “cold tumors” into “hot tumors” and may help to clarify which step of the antitumor immune response is not working; thus, the mechanism of action can be used to develop individualized treatment regimens.
This immunophenotype causes a poor immune response because more effector T cells cannot home from the tumor matrix to the inside of the tumor[15]. The underlying premise for the exertion of antitumor immune effects by effector T cells involves their migration to the tumor site, where their arrival involves multiple steps, as follows: immune cells first reach the blood vessels of tumor tissue through peripheral blood circulation and then penetrate tumor blood vessels to reach tumor tissue[16,17]. Chemokines, an important class of cytokines that affect the occurrence, development and angiogenesis of tumor cells, bind to chemokine receptors on the surface of effector T cells and play a key role in coordinating the transport of immune cells to the tumor core. The transport of immune cells into the tumor core occurs through endothelial adhesion and migration under the guidance of chemokines. Previous studies have shown that a variety of chemokines positive for various ligands can be involved in the recruitment of tumor T cells, including CC-chemokine ligand 4 (CCL4), CCL5, CXC-chemokine ligand 9 (CXCL9), CXCL10 and CXCL16, and that the lack or insufficiency of these chemokines can lead to the absence of immune cells in the tumor core[18-20]. For example, CXCL9 and CXCL10 participate in the recruitment of effector T lymphocytes in the human body mainly by binding to their corresponding receptors, and their expression levels determine the number of effector T lymphocytes infiltrating the tumor core. In the absence of CXCL9 and CXCL10 expression, effector T lymphocytes are not recruited into the tumor[20]. In human ovarian cancer cells, methylation of the CXCL9/10 genetic locus can result in immune evasion, and similar results were confirmed in a related study on colon cancer[21]. CCL5 is a typical cytokine secreted by normal T cells with chemotactic activity, and its increased expression can promote the transport of effector T cells into tumor cells[22]. This chemokine acts synergistically with IFN-γ-induced chemokines to establish an immuno-thermal phenotype, and studies have concluded that the cooperation between CCL5 and CXCL9 elucidates an important mechanism of tumor rejection to the T cell response[23]. However, certain chemokines such as CXCL1, CXCL2, and CXCL3 exert their effect by recruiting subsets of immunosuppressive T cells, such as myeloid-derived suppressor cells (MDSCs), to the tumor site, while CXCL12 mediates effector T lymphocytes into the tumor stroma, thus excluding them from recruitment into tumor cells[24].
The recruitment of effector T lymphocytes to tumors depends not only on the role of chemokines positive for various ligands but also on function of the vascular system and tumor matrix as a physical barrier. Structural and functional abnormalities in the tumor vasculature promote tumor growth and metastasis as well as immunosuppression[25]. An insufficient number of pericyclic cells or loose vascular basement membrane connections in tumor tissue that cover endothelial cells increases the permeability of tumor blood vessels, thereby promoting tumor metastasis[26,27]. As tumor cells continue to grow, the increased supply of nutrients and oxygen enhance the expression of vascular endothelial growth factor (VEGF) and basic fibroblast growth factor (bFGF), which promote the production of tumor cell blood vessels and create a hypoxic and acidic environment[28-30]. Hypoxia recruits immunosuppressive cells to the tumor immune microenvironment (TME) and can inhibit the function of immune effector T cells[31]. The neovascular endothelial cells can interfere with the function of T cells by altering the expression of receptors and their ligands, thereby causing immunosuppression[32]. In contrast to hematologic tumors, the matrix barrier is the last barrier affecting immune cells entering solid tumor tissue. When the tumor matrix is activated and fibrosis occurs, the antitumor treatment effect is inversely proportional to the activation and fibrosis of the matrix; that is, the lower the activation and fibrosis of the tumor matrix are, the better the antitumor effect[33]. Stromal cells in the TME can be divided into infiltrating immune cells, angiogenic vascular cells, cancer-associated fibroblasts (CAFs) and cancer-associated adipocytes[34]. CAFs account for a large proportion of the TME. The fibrous structure induced by CAFs can affect the delivery of immune drugs to tumor tissues and reduce antitumor immune efficacy[33]. It can be concluded that the state of chemokines in the immune microenvironment and the presence of specific vascular factors or stromal barriers are key factors affecting the inability of immune cells to nest inside of immune-repelling tumors.
The main feature of the immune-desert tumor phenotype is the absence of a perinucleoplasm or intratumoral immune cell infiltration[35]; therefore, any infiltration of immune cells is mainly an initiation error (i.e., insufficient antigen release, insufficient antigen presentation, and T cell initiation and activation disorders) in the anticancer immune response[15]. For these “cold tumors” to be transformed into “hot tumors”, characterized by a large amount of immune cell infiltration into the tumor tissues, the immune escape mechanism mainly involves immune initiation and the transfer of immune cells to tumor cells.
Newly emerging or overexpressed antigens in tumor tissue are collectively referred to as tumor antigens, which can be divided into tumor-specific antigens (TSAs) and tumor-associated antigens (TAAs) according to tumor specificity[36]. TSAs, produced during tumor mutations as neoantigens, are specific to tumor cells or are present only in certain tumor cells and are not expressed in normal cells[37]. Neoantigens have stronger immunogenicity and higher specificity than TAAs, making them a target for immune responses[38]. TMB is an index used to evaluate the number of gene mutations in tumor cells. The higher the gene mutation frequency of the tumor cells, the more tumor antigens are carried on the cell surface[39]. Some current evidence suggests that tumors with a higher mutation load can improve immunotherapy efficacy by modulating the degree of infiltration of immune cells to influence the immune properties of the TME[40]. Therefore, the lack of neoantigen production and a low TMB are the reasons for the lack of antigen release.
After tumor antigens are recognized, they must be processed by antigen-presenting cells (APCs) to initiate an immune response. As the most powerful APCs, dendritic cells (DCs) function to process antigen information and play a key role in the immune response[41]. DCs can be highly expressive MHC molecules, which bind to their captured tumor antigens and present them to T cells in the form of peptide-MHC molecular complexes, resulting in the activation of effector T cell responses to cancer-specific antigens. Therefore, the absence of DCs plays a key role in tumor immune evasion and immunotherapy failure[42]. However, the response of T cells is regulated by a series of co-suppressive or co-stimulatory signals; for example, the B7 molecule is the most important co-stimulatory molecule of T lymphocytes, superceding CD80 and CD86, which bind to the co-stimulatory protein CD28 to induce T cell activation and proliferation; however when it binds to cytotoxic T lymphocyte-associated antigen 4 (CTLA-4), immune responses are downregulated[43].
In solid tumors, vascular system abnormalities lead to restriction of the process of immune cell infiltration into the tumor, while vascular system normalization can improve the immunosuppressive microenvironment and facilitate immunotherapy drug delivery[44]. Targeting growth factors such as VEGF to inhibit the pathological angiogenesis of cancer has become a recognized therapeutic strategy[45]. VEGF and epidermal growth factor receptor (EGFR) are common therapeutic targets in CRC. Studies[46,47] have shown that immunotherapy and EGFR antagonists, VEGF antagonists and mitogen-activated protein kinase antagonists are utilized in the treatment of malignant tumors, which can bring new options and hope for patients with pMMR/MSS CRC.
The results of a series of clinical studies on immune-targeted combination therapies have shown that the efficacy of immunotherapy in CRC patients has made a breakthrough[48]. The mechanism by which immune-targeted combination therapy can enable patients with MSS bowel cancer to achieve immune efficacy (i.e., VEGF inhibition can restore tumor blood vessels to normal, increase the efficient initiation and activation of T cell responses, and recombine the typical immunosuppressive tumor microenvironment, thus indicating a synergistic effect between tumor immunotherapy and antivascular therapy)[49]. Regulatory T cells (Tregs) in the TME can inhibit effector T cells by either direct contact pathways or by secreting inhibitory cytokines, where targeted inhibitors can induce the proliferation of CD8 T cells in lymph nodes or suppress this pathway by infiltrating into tumor tissue, thereby improving the body’s anti-immune response[50]. Targeted inhibitors can improve transcriptional activity, increase the expression of anticancer genes and reduce the proliferation of tumor cells by inhibiting the elimination of acetyl groups[51]. It can be concluded that the application of anti-angiogenic targeted therapy combined with immunotherapy in MSS CRC patients is theoretically supported. A Japanese phase Ib REGONIVO study[48] conducted in recent years used nivolumab (a PD-1 inhibitor) plus regorafenib for CRC as the first treatment strategy. The results showed an ORR of 33.3%, a median progression-free survival (PFS) duration of 7.9 mo (95%CI 2.0, NE) and a 1-year overall survival (OS) rate of 68.0% in MSS CRC patients, which highlighted the benefits of immunotherapy for patients with cold CRC. The study further found that the median PFS of patients with PD-L1 combined positive score (CPS) > 1 was significantly better than that of patients with CPS ≤ 1 (6 mo vs not reached, P < 0.05). However, several studies, such as the North American Phase II study (NCT04126733), the Chinese population REGOTORI study[52] and the French Phase II REGOMUNE trial[53], all adopted a combination of immune and targeted dual therapy strategies, and although the results showed some efficacy, they were not as significant as those seen in the Japanese population.
Although chemotherapy drugs may kill immune cells that fight the tumor immune response, there is growing evidence that chemotherapy can activate the body’s immune response through multiple mechanisms. In addition to directly killing tumor cells, chemotherapy drugs stimulate the immune system by enhancing immunogenicity and increasing T cell infiltration, which converts “cold tumors” into “hot tumors”[54,55]. Chemotherapy drugs can enhance the recognition and presentation of DCs, activate cytotoxic T lymphocytes to attack tumors, and stimulate the release of interleukin-2 (IL-2), IL-4, and IFN-γ, causing an antitumor immune response[56,57]. Most chemotherapy regimens use a multidrug combination approach; however, the improvement in drug resistance remains nonsignificant[58]. Other studies have found that the use of PD-L1 inhibitors can reduce the incidence of chemotherapy drug resistance, mainly because chemotherapeutic drugs can lead to drug resistance by inducing the expression of PD-L1[55]. However, ICIs (such as CTLA-4 or PD-1/PD-L1) cannot directly kill tumor cells and must rely on the host immune system to enhance antitumor activity. In conclusion, chemotherapy combined with ICIs can improve the immunogenicity of CRC subtypes, help improve immune drug efficacy, and inhibit chemotherapy drug resistance. In recent years, the combination of chemotherapy and immunotherapy has attracted the attention of most clinicians and researchers and has been explored in multiple clinical trials. For example, in a phase 2 clinical study (NCT03374254) using chemotherapy to treat immunocompromised patients with non-MSI-H or pMMR advanced CRC, pembrolizumab combined with chemotherapy was used in both the first and second lines of treatment[59]. A phase 2 clinical study (METIMMOX study) evaluating the efficacy of the FLOX regimen plus nivolumab in the first-line treatment of MSS metastatic CRC (mCRC) validated the possibility of changing tumor immunogenicity and inducing a response to ICIs in this patient group[60]. Based on the publication of the results of this combination therapy strategy, we expect that the ongoing studies will lead to lasting outcomes for patients who have cold CRC. At present, a series of studies have been carried out to explore the effect of chemotherapy combined with antitumor immunotherapy, which has broad application prospects based on the relevant results. The question of how to achieve the optimum combination effect and the optimum timing and drug dose for combination therapies is still a hot topic for further exploration in future research.
Radiation therapy is an effective antitumor method for the palliative treatment of most patients with local or solitary metastatic tumor lesions, as well as extensive, advanced metastatic lesions. Radiotherapy can induce the body’s antitumor immune response, and its synergistic effect with ICIs can enhance the ability of the body’s immune system to recognize and eradicate tumor cells[61]. Some studies have shown that radiotherapy can transform immunologically “cold tumors” into “hot tumors” to a certain extent and increase the number of immune-beneficial populations[62]. With the advent of the era of immunotherapy, the immunostimulatory and immunosuppressive effects of radiation therapy have also been given increasing attention. Studies have confirmed that the combination of radiation therapy and ICIs can significantly enhance the regressive changes in tumor tissue. A meta-analysis of ICIs with or without radiotherapy in patients with melanoma showed that radiation therapy plus ICIs improved PFS without serious adverse effects[63]. Irreparable damage to DNA is one of the main mechanisms by which radiation therapy kills tumor cells and is also the key to radiation therapy-induced immune regulation. Radiation therapy can induce abscopal effects and reverse resistance to immunotherapy[64]. Radiotherapy also induces immunogenic cell death (ICD) of tumor cells by upregulating the release of damage-associated molecular patterns (DAMPs)[65]. When radiotherapy rays act on tumor cells, they can enhance their expression of MHC I molecules and improve their antigen presentation capacity[66]. In addition, radiotherapy can induce the secretion of chemokines, such as CXCL9 and CXCL10, and the release of pro-inflammatory cytokines, such as IL-2, tumor necrosis factor and type I interferons (IFN-α or IFN-β), recruit T cells and promote the infiltration of DCs and effector T cells into irradiated tumors, thereby regulating the immune state of the TME[66-69]. Radiotherapy also induces ICD and increases the release of TAAs by upregulating the release of DAMPs[70]. It follows that radiotherapy can promote the effect of immunotherapy drugs by altering changes in the TME. In turn, immunotherapy promotes the effects of radiation therapy by targeting and modulating various T cell populations.
Studies have confirmed that dual immunotherapy can obtain significant clinical efficacy, mainly due to the synergistic effect of the combination of anti-PD-1 and anti-CTLA-4 to increase the infiltration of effector T cells, which can play a role in overcoming the congenital tolerance of immune monotherapy in patients with cold CRC[71]. In a systematic review and meta-analysis by He et al[72], it was found that the combination of PD-1 and CTLA-4 inhibitors had the highest efficacy. CTLA-4 and PD-1 are both immune checkpoint proteins on T cells but play different roles in the immune response. Anti-CTLA-4 has the effect of expanding T cells in lymphoid organs and tumor tissues, while PD-1 is associated with ligand binding and overcomes the immunosuppressive antitumor effector T cells in the tumor bed[73]. CTLA-4 is highly expressed in Tregs, and many studies have shown that anti-CTLA-4 monoclonal antibody (mAb) can induce Treg depletion at tumor sites and normalize the TME[74]. A large phase II clinical study (CCTG CO.26) reported at the ASCO GI meeting in 2019 used a PD-L1 mAb combined with a CTLA-4 mAb to treat patients with advanced refractory CRC (98% of whom were pMMR/MSS). The study results showed that the mOS of the dual immunotherapy group reached 6.6 mo, and further exploration showed that MSS CRC patients with a TMB of 28 or more had the greatest OS benefit (HR, 0.34)[75]. Other studies have shown that dual immunotherapy does not significantly aggravate toxic side effects compared with immune monotherapy[76]. Some studies have shown that neoadjuvant immunotherapy can activate more effector T cells that kill tumor cells and induce a stronger tumor-specific T cell response[77]. A clinical study using neoadjuvant combination immunotherapy (NICHE study) showed that 27% of patients with pMMR achieved a pathological response, and 3 patients achieved a major pathological response, which brought hope for the application of dual immunotherapy to neoadjuvant therapy for MSS CRC[78]. Dual immunotherapy exhibits the characteristics of the complementary mechanisms, has long-lasting efficacy (in contrast to immune monotherapy), and therapeutic toxicity that is controllable; thus, it is expected to reverse the resistance of MSS CRC patients to ICIs. Although this study achieved the primary endpoint, the improvement in OS was not significant, so the conclusion that dual immunotherapy is efficacious has not been widely accepted, and the combination of dual ICIs in future clinical practice still needs more exploration.
As a class of viruses that can lyse tumor cells, OVs destroy tumor cells by selective replication and expansion in tumor cells, releasing TAAs and tumor-associated neutrophils. In this way, OVs induce the ICD of tumor cells while activating and promoting T cells to infiltrate the tumor site to improve the tumor microenvironment; thus, “cold tumors” can be effectively immunoactivated and transformed into “hot tumors”[3,79-81]. However, OVs alone have difficulty maintaining a long-term immune response and are prone to immune resistance. If OVs are used in combination with ICIs, they can not only reduce the immune tolerance of tumor cells but also significantly improve the antitumor efficacy, as demonstrated in the early stages of therapeutic safety studies. It has been shown in patients with advanced melanoma treated with the combination of talimogene laherparepvec and pembrolizumab that OVs can induce elevated PD-L1 expression at tumor sites as well as a significant increase T cell infiltration to improve the tumor microenvironment[82]. Therefore, it can be understood from these research results that OVs combined with ICIs are not only dependent on the degree of infiltration of immune cells but can also improve the infiltration of effector T cells in tumor tissues, successfully reversing the nonimmune inflammatory microenvironment in “cold tumors”.
There is increasing evidence that the gut microbiome affects the host’s innate and adaptive immune responses, providing a basis for a new class of antitumor agents that combine immunotherapy and gut microbiome therapy[83-86]. Both gut microbes and their metabolites can transform the immune microenvironment by inducing the release of proinflammatory cytokines and increasing the recruitment of T cells to the tumor site. The combination of gut microbes and immunosuppressants can reduce immune resistance. Pathogen-associated molecular patterns of gut microbes are recognized by Toll-like receptors and activate DCs to initiate adaptive immune responses, thereby alleviating immunosuppressive drug resistance and exerting antitumor effects[87]. The gut microbiome, modulated in specific ways, can improve the efficacy of immunotherapy while also alleviating immune-related adverse events caused by immunosuppressive drugs[88]. These findings suggest that Bifidobacterium may alleviate immunotherapy-associated colitis by altering the composition of the gut microbiota[89]. Microbial metabolites, such as the short-chain fatty acids produced by intestinal microorganisms after fermentation, which can induce the production of CD4 T cells and IL-22 to protect intestinal integrity from foreign microorganisms and maintain intestinal homeostasis, can also participate in the body’s immune regulation[90,91]. Gopalakrishnan et al[84] confirmed that the antitumor immune response is affected by the number and type of intestinal microorganisms in the gut microbiota. Specifically, the higher the diversity of gut microbes is, the longer the ORR and survival period of immunotherapy[92]. The gut microbiome of patients with CRC is less diverse and less sensitive to antigen stimulation, so it may be difficult to generate an immune response, which explains why the vast majority of CRC patients have “cold tumors”[93]. As a newer class of antitumor agents, gut microbes play an important role in antitumor immunotherapy, but their mechanisms of immune regulation are complex and are affected by factors such as body weight, age, diet, ethnicity, and living environment[94]. These individual differences have brought great challenges to the development of gut microbial antitumor immunotherapy.
Tumor vaccines have been used in a variety of tumor treatments and activate the body’s immune response, amplifying the antitumor immune response, and can induce durable antitumor immunity[95]. Tumor vaccines are divided into targeted antigen vaccines, autologous tumor cell vaccines, and DCs vaccines[96]. The first cancer vaccine approved by the United States of America Food and Drug Administration, Sipuleucel-T, was found to significantly improve the prognosis of patients with hormone refractory prostate cancer[97]. MAGE-A and NY-ESO-1, TAAs with strong antigenicity and specificity in the cancer testis antigen family, are highly expressed in a variety of tumor tissues, including CRC, and are expressed at low levels in normal tissues[98,99]. Therefore, they can be specifically recognized by the body’s immune system and exert antitumor effects. MAGE-A and NY-ESO-1 can induce a robust T cell antitumor response, and their related antibodies can be used as alternative biomarkers in vaccine therapy research[100,101]. At present, research on tumor vaccines based on MAGE-A4 and NY-ESO-1 has been carried out successively, and the results show that these vaccines have broad application prospects[101,102]. However, it is difficult to achieve high immune response rates with a single cancer vaccine alone, as has been confirmed in several clinical trials in patients with CRC[103-105]. Given that vaccination stimulates the body’s immune system to exert an effective antitumor response, the combination of ICIs and vaccines may lead to better outcomes for cold CRC patients.
Studies have demonstrated that either chemotherapy or targeted combination immunization can improve the antitumor immune response in patients with cold CRC. A series of studies have been carried out in the clinic based on the characteristics of chemotherapy drugs that can release tumor antigens, and targeted drugs that can regulate the immune microenvironment to explore whether the addition of immunotherapy will further improve the immune response of patients[51,54,55]. A phase 2 clinical study, AtezoTRIBE, which used FOLFOXIRI plus bevacizumab with or without atezolizumab for the first-line treatment of unresectable advanced CRC, showed that the addition of atezolizumab not only did not significantly increase the incidence of adverse reactions but also prolonged the PFS of patients with mCRC[106]. Another phase 2 clinical study, BACCI, compared the efficacy of capecitabine plus bevacizumab with or without atezolizumab[107]. The results showed that the combined atezolizumab group did not have significantly improved PFS or OS, but the ORR increased from 4.35% to 8.54%. The MODUL study used fluoropyrimidine plus bevacizumab with or without atezolizumab as first-line therapy and as maintenance therapy after stabilization, but the results showed that the addition of immunotherapy to maintenance therapy did not improve the prognosis of patients with advanced MSS CRC[108]. Neoadjuvant chemoradiotherapy (NCRT) is a standard treatment model for locally advanced rectal cancer. The addition of immunotherapy based on NCRT has been shown in a number of studies to promote the treatment response. For example, in a clinical study conducted in Japan on the use of immunoconsolidation therapy after neoadjuvant radiotherapy (NCT02948348), MSS CRC patients achieved a 29.7% pathological complete response (pCR) rate[109]. A phase 2 clinical study (ANAVA) in Italy used sequential immunotherapy after NCRT, and a pCR rate of 21.8% was observed in patients with MSS CRC[110]. Additional trials are ongoing to test the NCRT strategy with checkpoint inhibitors (NCT04083365 and NCT03994835).
Therefore, the benefits of multiple combination therapies are still controversial, and the balance between immune benefits and adverse reactions is controversial and requires further research and verification. However, we expect that additional clinical studies can allow these patients to achieve higher pathological response rates.
As a very complex and dynamic ecosystem, the TME is the site for tumor cell survival and proliferation and contains many different kinds of cell populations, including tumor cells, immune cells, and supporting cells (e.g., fibroblasts, stromal cells, and endothelial cells)[111,112]. The TME can be divided into an immune cell-based microenvironment and a non-immune microenvironment dominated by fibroblasts[113]. Similar to many tumors, the TME plays an integral role in immunotherapy in CRC patients, and immunotherapy responses vary due to differences in the TME[114]. One study based on genomics analysis showed that CRC patients can be divided into different immune subtypes, and through the analysis of molecular phenotypes, the immune status of the tumor microenvironment can be determined, and the degree of TMB in CRC patients can be predicted[115]. Several existing studies have shown that biomarkers such as MSI-H, TMB and the gut microbiome can be used as predictors of immunotherapy prognosis[116-118]. The new study found that the PORE/polymerase delta 1 catalytic subunit (POLD1) mutation present in patients with MSS CRC is associated with TMB and MSI status and that CRC containing this mutation can exhibit immunoinflammatory characteristics. CRC is a highly heterogeneous tumor, and accurate immunomolecular typing can reveal the differences between subtypes, which may help to screen out the immunotherapy-dominant populations. This strategy will increase the accuracy of the biomarkers as prognostic indicators and will allow the development of an individualized hierarchical diagnosis and treatment strategy for MSS CRC patients that maximizes patient benefits[119,120]. POLE/POLD1 mutations can lead to activation of the TME, which elicits an immune response to the tumor. He et al[121] and Chen et al[122] found that POLAR/POLD1 can be used as a molecular marker for predicting the efficacy of ICIs in CRC patients.
With developments in the understanding of tumor biology and tumor immune tolerance mechanisms, the existing research results suggest that a combination immunotherapy strategy for cold CRC will allow a good immune response in some patients; however there has been no major breakthrough, and maintaining a long-term antitumor immune response is still the main challenge. It is necessary to further explore the best combination of treatments to expand the populations benefiting from immunotherapy and to find new biomarkers to accurately screen sensitive populations, which can promote the development of future precision biomarkers and precision therapies.
The authors are highly grateful to anonymous reviewers for their helpful suggestions and valuable comments.
Provenance and peer review: Invited article; Externally peer reviewed.
Peer-review model: Single blind
Specialty type: Oncology
Country/Territory of origin: China
Peer-review report’s scientific quality classification
Grade A (Excellent): 0
Grade B (Very good): B, B
Grade C (Good): 0
Grade D (Fair): 0
Grade E (Poor): 0
P-Reviewer: Hashimoto K, Japan; Win TT, Malaysia S-Editor: Chen YL L-Editor: A P-Editor: Chen YL
| 1. | Sung H, Ferlay J, Siegel RL, Laversanne M, Soerjomataram I, Jemal A, Bray F. Global Cancer Statistics 2020: GLOBOCAN Estimates of Incidence and Mortality Worldwide for 36 Cancers in 185 Countries. CA Cancer J Clin. 2021;71:209-249. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 75126] [Cited by in RCA: 64542] [Article Influence: 16135.5] [Reference Citation Analysis (176)] |
| 2. | Weiden J, Tel J, Figdor CG. Synthetic immune niches for cancer immunotherapy. Nat Rev Immunol. 2018;18:212-219. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 105] [Cited by in RCA: 124] [Article Influence: 15.5] [Reference Citation Analysis (0)] |
| 3. | Russell SJ, Barber GN. Oncolytic Viruses as Antigen-Agnostic Cancer Vaccines. Cancer Cell. 2018;33:599-605. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 141] [Cited by in RCA: 183] [Article Influence: 26.1] [Reference Citation Analysis (0)] |
| 4. | Ghiringhelli F, Fumet JD. Is There a Place for Immunotherapy for Metastatic Microsatellite Stable Colorectal Cancer? Front Immunol. 2019;10:1816. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 43] [Cited by in RCA: 56] [Article Influence: 9.3] [Reference Citation Analysis (0)] |
| 5. | Le DT, Uram JN, Wang H, Bartlett BR, Kemberling H, Eyring AD, Skora AD, Luber BS, Azad NS, Laheru D, Biedrzycki B, Donehower RC, Zaheer A, Fisher GA, Crocenzi TS, Lee JJ, Duffy SM, Goldberg RM, de la Chapelle A, Koshiji M, Bhaijee F, Huebner T, Hruban RH, Wood LD, Cuka N, Pardoll DM, Papadopoulos N, Kinzler KW, Zhou S, Cornish TC, Taube JM, Anders RA, Eshleman JR, Vogelstein B, Diaz LA Jr. PD-1 Blockade in Tumors with Mismatch-Repair Deficiency. N Engl J Med. 2015;372:2509-2520. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 6096] [Cited by in RCA: 7233] [Article Influence: 723.3] [Reference Citation Analysis (0)] |
| 6. | Chen DS, Mellman I. Elements of cancer immunity and the cancer-immune set point. Nature. 2017;541:321-330. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 2373] [Cited by in RCA: 3597] [Article Influence: 449.6] [Reference Citation Analysis (0)] |
| 7. | Lizardo DY, Kuang C, Hao S, Yu J, Huang Y, Zhang L. Immunotherapy efficacy on mismatch repair-deficient colorectal cancer: From bench to bedside. Biochim Biophys Acta Rev Cancer. 2020;1874:188447. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 79] [Cited by in RCA: 135] [Article Influence: 27.0] [Reference Citation Analysis (0)] |
| 8. | Li Y, Du Y, Xue C, Wu P, Du N, Zhu G, Xu H, Zhu Z. Efficacy and safety of anti-PD-1/PD-L1 therapy in the treatment of advanced colorectal cancer: a meta-analysis. BMC Gastroenterol. 2022;22:431. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 29] [Cited by in RCA: 16] [Article Influence: 5.3] [Reference Citation Analysis (0)] |
| 9. | Akin Telli T, Bregni G, Vanhooren M, Saude Conde R, Hendlisz A, Sclafani F. Regorafenib in combination with immune checkpoint inhibitors for mismatch repair proficient (pMMR)/microsatellite stable (MSS) colorectal cancer. Cancer Treat Rev. 2022;110:102460. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1] [Cited by in RCA: 22] [Article Influence: 7.3] [Reference Citation Analysis (0)] |
| 10. | Goodman AM, Sokol ES, Frampton GM, Lippman SM, Kurzrock R. Microsatellite-Stable Tumors with High Mutational Burden Benefit from Immunotherapy. Cancer Immunol Res. 2019;7:1570-1573. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 98] [Cited by in RCA: 213] [Article Influence: 35.5] [Reference Citation Analysis (0)] |
| 11. | Hegde PS, Karanikas V, Evers S. The Where, the When, and the How of Immune Monitoring for Cancer Immunotherapies in the Era of Checkpoint Inhibition. Clin Cancer Res. 2016;22:1865-1874. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 462] [Cited by in RCA: 684] [Article Influence: 76.0] [Reference Citation Analysis (0)] |
| 12. | Galon J, Bruni D. Approaches to treat immune hot, altered and cold tumours with combination immunotherapies. Nat Rev Drug Discov. 2019;18:197-218. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1151] [Cited by in RCA: 2213] [Article Influence: 368.8] [Reference Citation Analysis (0)] |
| 13. | Hegde PS, Chen DS. Top 10 Challenges in Cancer Immunotherapy. Immunity. 2020;52:17-35. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 567] [Cited by in RCA: 1322] [Article Influence: 264.4] [Reference Citation Analysis (0)] |
| 14. | Bonaventura P, Shekarian T, Alcazer V, Valladeau-Guilemond J, Valsesia-Wittmann S, Amigorena S, Caux C, Depil S. Cold Tumors: A Therapeutic Challenge for Immunotherapy. Front Immunol. 2019;10:168. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 423] [Cited by in RCA: 807] [Article Influence: 134.5] [Reference Citation Analysis (0)] |
| 15. | Chen DS, Mellman I. Oncology meets immunology: the cancer-immunity cycle. Immunity. 2013;39:1-10. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 3297] [Cited by in RCA: 4762] [Article Influence: 396.8] [Reference Citation Analysis (1)] |
| 16. | Kershaw MH, Westwood JA, Parker LL, Wang G, Eshhar Z, Mavroukakis SA, White DE, Wunderlich JR, Canevari S, Rogers-Freezer L, Chen CC, Yang JC, Rosenberg SA, Hwu P. A phase I study on adoptive immunotherapy using gene-modified T cells for ovarian cancer. Clin Cancer Res. 2006;12:6106-6115. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 1006] [Cited by in RCA: 967] [Article Influence: 50.9] [Reference Citation Analysis (0)] |
| 17. | Hyun YM, Sumagin R, Sarangi PP, Lomakina E, Overstreet MG, Baker CM, Fowell DJ, Waugh RE, Sarelius IH, Kim M. Uropod elongation is a common final step in leukocyte extravasation through inflamed vessels. J Exp Med. 2012;209:1349-1362. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 91] [Cited by in RCA: 112] [Article Influence: 8.6] [Reference Citation Analysis (0)] |
| 18. | van der Woude LL, Gorris MAJ, Halilovic A, Figdor CG, de Vries IJM. Migrating into the Tumor: a Roadmap for T Cells. Trends Cancer. 2017;3:797-808. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 144] [Cited by in RCA: 220] [Article Influence: 27.5] [Reference Citation Analysis (0)] |
| 19. | Maimela NR, Liu S, Zhang Y. Fates of CD8+ T cells in Tumor Microenvironment. Comput Struct Biotechnol J. 2019;17:1-13. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 341] [Cited by in RCA: 319] [Article Influence: 45.6] [Reference Citation Analysis (0)] |
| 20. | Spranger S, Bao R, Gajewski TF. Melanoma-intrinsic β-catenin signalling prevents anti-tumour immunity. Nature. 2015;523:231-235. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1641] [Cited by in RCA: 2110] [Article Influence: 211.0] [Reference Citation Analysis (0)] |
| 21. | Peng D, Kryczek I, Nagarsheth N, Zhao L, Wei S, Wang W, Sun Y, Zhao E, Vatan L, Szeliga W, Kotarski J, Tarkowski R, Dou Y, Cho K, Hensley-Alford S, Munkarah A, Liu R, Zou W. Epigenetic silencing of TH1-type chemokines shapes tumour immunity and immunotherapy. Nature. 2015;527:249-253. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 662] [Cited by in RCA: 917] [Article Influence: 91.7] [Reference Citation Analysis (0)] |
| 22. | Topper MJ, Vaz M, Chiappinelli KB, DeStefano Shields CE, Niknafs N, Yen RC, Wenzel A, Hicks J, Ballew M, Stone M, Tran PT, Zahnow CA, Hellmann MD, Anagnostou V, Strissel PL, Strick R, Velculescu VE, Baylin SB. Epigenetic Therapy Ties MYC Depletion to Reversing Immune Evasion and Treating Lung Cancer. Cell. 2017;171:1284-1300.e21. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 230] [Cited by in RCA: 356] [Article Influence: 44.5] [Reference Citation Analysis (0)] |
| 23. | Dangaj D, Bruand M, Grimm AJ, Ronet C, Barras D, Duttagupta PA, Lanitis E, Duraiswamy J, Tanyi JL, Benencia F, Conejo-Garcia J, Ramay HR, Montone KT, Powell DJ Jr, Gimotty PA, Facciabene A, Jackson DG, Weber JS, Rodig SJ, Hodi SF, Kandalaft LE, Irving M, Zhang L, Foukas P, Rusakiewicz S, Delorenzi M, Coukos G. Cooperation between Constitutive and Inducible Chemokines Enables T Cell Engraftment and Immune Attack in Solid Tumors. Cancer Cell. 2019;35:885-900.e10. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 307] [Cited by in RCA: 551] [Article Influence: 91.8] [Reference Citation Analysis (0)] |
| 24. | Mortezaee K. CXCL12/CXCR4 axis in the microenvironment of solid tumors: A critical mediator of metastasis. Life Sci. 2020;249:117534. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 68] [Cited by in RCA: 117] [Article Influence: 23.4] [Reference Citation Analysis (0)] |
| 25. | Dirkx AE, Oude Egbrink MG, Kuijpers MJ, van der Niet ST, Heijnen VV, Bouma-ter Steege JC, Wagstaff J, Griffioen AW. Tumor angiogenesis modulates leukocyte-vessel wall interactions in vivo by reducing endothelial adhesion molecule expression. Cancer Res. 2003;63:2322-2329. [PubMed] |
| 26. | Zhao Y, Yu X, Li J. Manipulation of immune‒vascular crosstalk: new strategies towards cancer treatment. Acta Pharm Sin B. 2020;10:2018-2036. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 23] [Cited by in RCA: 50] [Article Influence: 10.0] [Reference Citation Analysis (0)] |
| 27. | Hashizume H, Baluk P, Morikawa S, McLean JW, Thurston G, Roberge S, Jain RK, McDonald DM. Openings between defective endothelial cells explain tumor vessel leakiness. Am J Pathol. 2000;156:1363-1380. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1179] [Cited by in RCA: 1170] [Article Influence: 46.8] [Reference Citation Analysis (0)] |
| 28. | Kuehlbach C, Hensler S, Mueller MM. Recapitulating the Angiogenic Switch in a Hydrogel-Based 3D In Vitro Tumor-Stroma Model. Bioengineering (Basel). 2021;8. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 2] [Cited by in RCA: 2] [Article Influence: 0.5] [Reference Citation Analysis (0)] |
| 29. | Fukumura D, Kloepper J, Amoozgar Z, Duda DG, Jain RK. Enhancing cancer immunotherapy using antiangiogenics: opportunities and challenges. Nat Rev Clin Oncol. 2018;15:325-340. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 745] [Cited by in RCA: 1392] [Article Influence: 198.9] [Reference Citation Analysis (0)] |
| 30. | Martin JD, Seano G, Jain RK. Normalizing Function of Tumor Vessels: Progress, Opportunities, and Challenges. Annu Rev Physiol. 2019;81:505-534. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 195] [Cited by in RCA: 351] [Article Influence: 70.2] [Reference Citation Analysis (0)] |
| 31. | Damgaci S, Ibrahim-Hashim A, Enriquez-Navas PM, Pilon-Thomas S, Guvenis A, Gillies RJ. Hypoxia and acidosis: immune suppressors and therapeutic targets. Immunology. 2018;154:354-362. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 129] [Cited by in RCA: 156] [Article Influence: 22.3] [Reference Citation Analysis (0)] |
| 32. | Huang Y, Yuan J, Righi E, Kamoun WS, Ancukiewicz M, Nezivar J, Santosuosso M, Martin JD, Martin MR, Vianello F, Leblanc P, Munn LL, Huang P, Duda DG, Fukumura D, Jain RK, Poznansky MC. Vascular normalizing doses of antiangiogenic treatment reprogram the immunosuppressive tumor microenvironment and enhance immunotherapy. Proc Natl Acad Sci U S A. 2012;109:17561-17566. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 613] [Cited by in RCA: 810] [Article Influence: 62.3] [Reference Citation Analysis (0)] |
| 33. | Valkenburg KC, de Groot AE, Pienta KJ. Targeting the tumour stroma to improve cancer therapy. Nat Rev Clin Oncol. 2018;15:366-381. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 475] [Cited by in RCA: 765] [Article Influence: 127.5] [Reference Citation Analysis (0)] |
| 34. | Egeblad M, Nakasone ES, Werb Z. Tumors as organs: complex tissues that interface with the entire organism. Dev Cell. 2010;18:884-901. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 987] [Cited by in RCA: 896] [Article Influence: 59.7] [Reference Citation Analysis (0)] |
| 35. | Kim JM, Chen DS. Immune escape to PD-L1/PD-1 blockade: seven steps to success (or failure). Ann Oncol. 2016;27:1492-1504. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 303] [Cited by in RCA: 478] [Article Influence: 53.1] [Reference Citation Analysis (0)] |
| 36. | Yarchoan M, Hopkins A, Jaffee EM. Tumor Mutational Burden and Response Rate to PD-1 Inhibition. N Engl J Med. 2017;377:2500-2501. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1693] [Cited by in RCA: 2417] [Article Influence: 302.1] [Reference Citation Analysis (0)] |
| 37. | Kelderman S, Kvistborg P. Tumor antigens in human cancer control. Biochim Biophys Acta. 2016;1865:83-89. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 11] [Cited by in RCA: 14] [Article Influence: 1.6] [Reference Citation Analysis (0)] |
| 38. | Havel JJ, Chowell D, Chan TA. The evolving landscape of biomarkers for checkpoint inhibitor immunotherapy. Nat Rev Cancer. 2019;19:133-150. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1246] [Cited by in RCA: 1683] [Article Influence: 280.5] [Reference Citation Analysis (0)] |
| 39. | Gubin MM, Artyomov MN, Mardis ER, Schreiber RD. Tumor neoantigens: building a framework for personalized cancer immunotherapy. J Clin Invest. 2015;125:3413-3421. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 379] [Cited by in RCA: 477] [Article Influence: 47.7] [Reference Citation Analysis (0)] |
| 40. | Mouw KW, Goldberg MS, Konstantinopoulos PA, D'Andrea AD. DNA Damage and Repair Biomarkers of Immunotherapy Response. Cancer Discov. 2017;7:675-693. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 492] [Cited by in RCA: 510] [Article Influence: 63.8] [Reference Citation Analysis (0)] |
| 41. | Santin AD, Hermonat PL, Ravaggi A, Chiriva-Internati M, Hiserodt JC, Pecorelli S, Parham GP. Effects of retinoic acid combined with irradiation on the expression of major histocompatibility complex molecules and adhesion/costimulation molecules ICAM-1 in human cervical cancer. Gynecol Oncol. 1998;70:195-201. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 11] [Cited by in RCA: 12] [Article Influence: 0.4] [Reference Citation Analysis (0)] |
| 42. | GeurtsvanKessel CH, Willart MA, van Rijt LS, Muskens F, Kool M, Baas C, Thielemans K, Bennett C, Clausen BE, Hoogsteden HC, Osterhaus AD, Rimmelzwaan GF, Lambrecht BN. Clearance of influenza virus from the lung depends on migratory langerin+CD11b- but not plasmacytoid dendritic cells. J Exp Med. 2008;205:1621-1634. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 369] [Cited by in RCA: 390] [Article Influence: 22.9] [Reference Citation Analysis (0)] |
| 43. | Schildberg FA, Klein SR, Freeman GJ, Sharpe AH. Coinhibitory Pathways in the B7-CD28 Ligand-Receptor Family. Immunity. 2016;44:955-972. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 343] [Cited by in RCA: 448] [Article Influence: 56.0] [Reference Citation Analysis (0)] |
| 44. | Clavreul A, Roger E, Pourbaghi-Masouleh M, Lemaire L, Tétaud C, Menei P. Development and characterization of sorafenib-loaded lipid nanocapsules for the treatment of glioblastoma. Drug Deliv. 2018;25:1756-1765. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 24] [Cited by in RCA: 44] [Article Influence: 7.3] [Reference Citation Analysis (0)] |
| 45. | Bertolini F, Marighetti P, Martin-Padura I, Mancuso P, Hu-Lowe DD, Shaked Y, D'Onofrio A. Anti-VEGF and beyond: shaping a new generation of anti-angiogenic therapies for cancer. Drug Discov Today. 2011;16:1052-1060. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 26] [Cited by in RCA: 31] [Article Influence: 2.2] [Reference Citation Analysis (0)] |
| 46. | Yang J, Yan J, Liu B. Targeting VEGF/VEGFR to Modulate Antitumor Immunity. Front Immunol. 2018;9:978. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 268] [Cited by in RCA: 445] [Article Influence: 63.6] [Reference Citation Analysis (0)] |
| 47. | MacDonald F, Zaiss DMW. The Immune System's Contribution to the Clinical Efficacy of EGFR Antagonist Treatment. Front Pharmacol. 2017;8:575. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 21] [Cited by in RCA: 31] [Article Influence: 3.9] [Reference Citation Analysis (0)] |
| 48. | Fukuoka S, Hara H, Takahashi N, Kojima T, Kawazoe A, Asayama M, Yoshii T, Kotani D, Tamura H, Mikamoto Y, Hirano N, Wakabayashi M, Nomura S, Sato A, Kuwata T, Togashi Y, Nishikawa H, Shitara K. Regorafenib Plus Nivolumab in Patients With Advanced Gastric or Colorectal Cancer: An Open-Label, Dose-Escalation, and Dose-Expansion Phase Ib Trial (REGONIVO, EPOC1603). J Clin Oncol. 2020;38:2053-2061. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 234] [Cited by in RCA: 531] [Article Influence: 106.2] [Reference Citation Analysis (0)] |
| 49. | Zhao Y, Boczkowski D, Nair SK, Gilboa E. Inhibition of invariant chain expression in dendritic cells presenting endogenous antigens stimulates CD4+ T-cell responses and tumor immunity. Blood. 2003;102:4137-4142. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 25] [Cited by in RCA: 28] [Article Influence: 1.3] [Reference Citation Analysis (0)] |
| 50. | Buchbinder E, Hodi FS. Cytotoxic T lymphocyte antigen-4 and immune checkpoint blockade. J Clin Invest. 2015;125:3377-3383. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 107] [Cited by in RCA: 132] [Article Influence: 13.2] [Reference Citation Analysis (0)] |
| 51. | Greer CB, Tanaka Y, Kim YJ, Xie P, Zhang MQ, Park IH, Kim TH. Histone Deacetylases Positively Regulate Transcription through the Elongation Machinery. Cell Rep. 2015;13:1444-1455. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 110] [Cited by in RCA: 125] [Article Influence: 12.5] [Reference Citation Analysis (0)] |
| 52. | Wang F, He MM, Yao YC, Wang ZQ, Jin Y, Wang FH, Qiu MZ, Lv ZD, Wang DS, Luo HY, Li YH, Zhang DS, Xu R. JS001 Combined With Regorafenib in Patients With Advanced Colorectal Cancer. May 12, 2020. [cited 3 November 2022]. Available from: http://clinicaltrials.gov/show/NCT03946917. |
| 53. | Cousin S, Cantarel C, Guegan JP, Gomez-Roca C, Metges JP, Adenis A, Pernot S, Bellera C, Kind M, Auzanneau C, Le Loarer F, Soubeyran I, Bessede A, Italiano A. Regorafenib-Avelumab Combination in Patients with Microsatellite Stable Colorectal Cancer (REGOMUNE): A Single-arm, Open-label, Phase II Trial. Clin Cancer Res. 2021;27:2139-2147. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 30] [Cited by in RCA: 93] [Article Influence: 23.3] [Reference Citation Analysis (0)] |
| 54. | Galluzzi L, Humeau J, Buqué A, Zitvogel L, Kroemer G. Immunostimulation with chemotherapy in the era of immune checkpoint inhibitors. Nat Rev Clin Oncol. 2020;17:725-741. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 285] [Cited by in RCA: 871] [Article Influence: 174.2] [Reference Citation Analysis (0)] |
| 55. | Haanen JBAG. Converting Cold into Hot Tumors by Combining Immunotherapies. Cell. 2017;170:1055-1056. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 147] [Cited by in RCA: 198] [Article Influence: 24.8] [Reference Citation Analysis (0)] |
| 56. | Wang Q, Ju X, Wang J, Fan Y, Ren M, Zhang H. Immunogenic cell death in anticancer chemotherapy and its impact on clinical studies. Cancer Lett. 2018;438:17-23. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 96] [Cited by in RCA: 189] [Article Influence: 27.0] [Reference Citation Analysis (0)] |
| 57. | Garg AD, Dudek-Peric AM, Romano E, Agostinis P. Immunogenic cell death. Int J Dev Biol. 2015;59:131-140. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 123] [Cited by in RCA: 177] [Article Influence: 19.7] [Reference Citation Analysis (0)] |
| 58. | Luqmani YA. Mechanisms of drug resistance in cancer chemotherapy. Med Princ Pract. 2005;14 Suppl 1:35-48. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 395] [Cited by in RCA: 442] [Article Influence: 22.1] [Reference Citation Analysis (0)] |
| 59. | Kim R, Chaves J, Kavan P, Fakih M, Kortmansky JS, Spencer K, Wong L, Tehfe M, Li JJ, Eyring AD, Mayo C, Chiorean EG. Safety and Efficacy of Pembrolizumab (MK-3475) Plus Binimetinib Alone or Pembrolizumab Plus Chemotherapy With or Without Binimetinib in Metastatic Colorectal Cancer (mCRC) Participants (MK-3475-651). Jun 21, 2022. [cited 3 November 2022]. Available from: http://clinicaltrials.gov/show/NCT03374254. |
| 60. | Anne H, Harme H, Kersten C. METIMMOX: Colorectal Cancer METastasis - Shaping Anti-tumor IMMunity by OXaliplatin (METIMMOX). Jan 1, 2022. [cited 3 November 2022]. Available from: http://clinicaltrials.gov/show/NCT03388190. |
| 61. | Simonelli M, Persico P, Perrino M, Zucali PA, Navarria P, Pessina F, Scorsetti M, Bello L, Santoro A. Checkpoint inhibitors as treatment for malignant gliomas: "A long way to the top". Cancer Treat Rev. 2018;69:121-131. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 27] [Cited by in RCA: 34] [Article Influence: 4.9] [Reference Citation Analysis (0)] |
| 62. | Demaria S, Coleman CN, Formenti SC. Radiotherapy: Changing the Game in Immunotherapy. Trends Cancer. 2016;2:286-294. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 198] [Cited by in RCA: 279] [Article Influence: 39.9] [Reference Citation Analysis (0)] |
| 63. | Yin G, Guo W, Huang Z, Chen X. Efficacy of radiotherapy combined with immune checkpoint inhibitors in patients with melanoma: a systemic review and meta-analysis. Melanoma Res. 2022;32:71-78. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 5] [Cited by in RCA: 11] [Article Influence: 3.7] [Reference Citation Analysis (0)] |
| 64. | Donlon NE, Power R, Hayes C, Reynolds JV, Lysaght J. Radiotherapy, immunotherapy, and the tumour microenvironment: Turning an immunosuppressive milieu into a therapeutic opportunity. Cancer Lett. 2021;502:84-96. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 33] [Cited by in RCA: 117] [Article Influence: 29.3] [Reference Citation Analysis (0)] |
| 65. | Herrera FG, Bourhis J, Coukos G. Radiotherapy combination opportunities leveraging immunity for the next oncology practice. CA Cancer J Clin. 2017;67:65-85. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 244] [Cited by in RCA: 364] [Article Influence: 45.5] [Reference Citation Analysis (0)] |
| 66. | Reits EA, Hodge JW, Herberts CA, Groothuis TA, Chakraborty M, Wansley EK, Camphausen K, Luiten RM, de Ru AH, Neijssen J, Griekspoor A, Mesman E, Verreck FA, Spits H, Schlom J, van Veelen P, Neefjes JJ. Radiation modulates the peptide repertoire, enhances MHC class I expression, and induces successful antitumor immunotherapy. J Exp Med. 2006;203:1259-1271. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 1089] [Cited by in RCA: 1360] [Article Influence: 71.6] [Reference Citation Analysis (0)] |
| 67. | Walle T, Martinez Monge R, Cerwenka A, Ajona D, Melero I, Lecanda F. Radiation effects on antitumor immune responses: current perspectives and challenges. Ther Adv Med Oncol. 2018;10:1758834017742575. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 115] [Cited by in RCA: 177] [Article Influence: 25.3] [Reference Citation Analysis (0)] |
| 68. | Bernier J. Immuno-oncology: Allying forces of radio- and immuno-therapy to enhance cancer cell killing. Crit Rev Oncol Hematol. 2016;108:97-108. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 18] [Cited by in RCA: 24] [Article Influence: 2.7] [Reference Citation Analysis (0)] |
| 69. | Chajon E, Castelli J, Marsiglia H, De Crevoisier R. The synergistic effect of radiotherapy and immunotherapy: A promising but not simple partnership. Crit Rev Oncol Hematol. 2017;111:124-132. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 73] [Cited by in RCA: 95] [Article Influence: 11.9] [Reference Citation Analysis (0)] |
| 70. | Golden EB, Apetoh L. Radiotherapy and immunogenic cell death. Semin Radiat Oncol. 2015;25:11-17. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 250] [Cited by in RCA: 344] [Article Influence: 34.4] [Reference Citation Analysis (0)] |
| 71. | Dudal S, Hinton H, Giusti AM, Bacac M, Muller M, Fauti T, Colombetti S, Heckel T, Giroud N, Klein C, Umaña P, Benincosa L, Bachl J, Singer T, Bray-French K. Application of a MABEL Approach for a T-Cell-Bispecific Monoclonal Antibody: CEA TCB. J Immunother. 2016;39:279-289. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 21] [Cited by in RCA: 29] [Article Influence: 3.6] [Reference Citation Analysis (0)] |
| 72. | He R, Zhao X, Liu J, Zhou Y, Zhang X, Cheng F. PD-1 and CTLA-4 inhibitors in combination vs. alone for the treatment of advanced melanoma: A systematic review and meta-analysis. Medicine (Baltimore). 2022;101:e30561. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 2] [Cited by in RCA: 3] [Article Influence: 1.0] [Reference Citation Analysis (0)] |
| 73. | Ribas A. Tumor immunotherapy directed at PD-1. N Engl J Med. 2012;366:2517-2519. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 480] [Cited by in RCA: 507] [Article Influence: 39.0] [Reference Citation Analysis (0)] |
| 74. | Arce Vargas F, Furness AJS, Litchfield K, Joshi K, Rosenthal R, Ghorani E, Solomon I, Lesko MH, Ruef N, Roddie C, Henry JY, Spain L, Ben Aissa A, Georgiou A, Wong YNS, Smith M, Strauss D, Hayes A, Nicol D, O'Brien T, Mårtensson L, Ljungars A, Teige I, Frendéus B; TRACERx Melanoma; TRACERx Renal; TRACERx Lung consortia, Pule M, Marafioti T, Gore M, Larkin J, Turajlic S, Swanton C, Peggs KS, Quezada SA. Fc Effector Function Contributes to the Activity of Human Anti-CTLA-4 Antibodies. Cancer Cell. 2018;33:649-663.e4. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 404] [Cited by in RCA: 457] [Article Influence: 65.3] [Reference Citation Analysis (0)] |
| 75. | Chen EX, Jonker DJ, Loree JM, Kennecke HF, Berry SR, Couture F, Ahmad CE, Goffin JR, Kavan P, Harb M, Colwell B, Samimi S, Samson B, Abbas T, Aucoin N, Aubin F, Koski SL, Wei AC, Magoski NM, Tu D, O'Callaghan CJ. Effect of Combined Immune Checkpoint Inhibition vs Best Supportive Care Alone in Patients With Advanced Colorectal Cancer: The Canadian Cancer Trials Group CO.26 Study. JAMA Oncol. 2020;6:831-838. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 209] [Cited by in RCA: 282] [Article Influence: 56.4] [Reference Citation Analysis (0)] |
| 76. | Overman MJ, McDermott R, Leach JL, Lonardi S, Lenz HJ, Morse MA, Desai J, Hill A, Axelson M, Moss RA, Goldberg MV, Cao ZA, Ledeine JM, Maglinte GA, Kopetz S, André T. Nivolumab in patients with metastatic DNA mismatch repair-deficient or microsatellite instability-high colorectal cancer (CheckMate 142): an open-label, multicentre, phase 2 study. Lancet Oncol. 2017;18:1182-1191. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1775] [Cited by in RCA: 2082] [Article Influence: 260.3] [Reference Citation Analysis (0)] |
| 77. | Blank CU, Rozeman EA, Fanchi LF, Sikorska K, van de Wiel B, Kvistborg P, Krijgsman O, van den Braber M, Philips D, Broeks A, van Thienen JV, Mallo HA, Adriaansz S, Ter Meulen S, Pronk LM, Grijpink-Ongering LG, Bruining A, Gittelman RM, Warren S, van Tinteren H, Peeper DS, Haanen JBAG, van Akkooi ACJ, Schumacher TN. Neoadjuvant versus adjuvant ipilimumab plus nivolumab in macroscopic stage III melanoma. Nat Med. 2018;24:1655-1661. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 377] [Cited by in RCA: 635] [Article Influence: 90.7] [Reference Citation Analysis (0)] |
| 78. | Chalabi M, Fanchi LF, Dijkstra KK, Van den Berg JG, Aalbers AG, Sikorska K, Lopez-Yurda M, Grootscholten C, Beets GL, Snaebjornsson P, Maas M, Mertz M, Veninga V, Bounova G, Broeks A, Beets-Tan RG, de Wijkerslooth TR, van Lent AU, Marsman HA, Nuijten E, Kok NF, Kuiper M, Verbeek WH, Kok M, Van Leerdam ME, Schumacher TN, Voest EE, Haanen JB. Neoadjuvant immunotherapy leads to pathological responses in MMR-proficient and MMR-deficient early-stage colon cancers. Nat Med. 2020;26:566-576. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 341] [Cited by in RCA: 892] [Article Influence: 178.4] [Reference Citation Analysis (0)] |
| 79. | Malogolovkin A, Gasanov N, Egorov A, Weener M, Ivanov R, Karabelsky A. Combinatorial Approaches for Cancer Treatment Using Oncolytic Viruses: Projecting the Perspectives through Clinical Trials Outcomes. Viruses. 2021;13. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 30] [Cited by in RCA: 37] [Article Influence: 9.3] [Reference Citation Analysis (0)] |
| 80. | Russell L, Peng KW, Russell SJ, Diaz RM. Oncolytic Viruses: Priming Time for Cancer Immunotherapy. BioDrugs. 2019;33:485-501. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 62] [Cited by in RCA: 90] [Article Influence: 18.0] [Reference Citation Analysis (0)] |
| 81. | Bommareddy PK, Shettigar M, Kaufman HL. Integrating oncolytic viruses in combination cancer immunotherapy. Nat Rev Immunol. 2018;18:498-513. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 288] [Cited by in RCA: 469] [Article Influence: 67.0] [Reference Citation Analysis (16)] |
| 82. | Ribas A, Dummer R, Puzanov I, VanderWalde A, Andtbacka RHI, Michielin O, Olszanski AJ, Malvehy J, Cebon J, Fernandez E, Kirkwood JM, Gajewski TF, Chen L, Gorski KS, Anderson AA, Diede SJ, Lassman ME, Gansert J, Hodi FS, Long GV. Oncolytic Virotherapy Promotes Intratumoral T Cell Infiltration and Improves Anti-PD-1 Immunotherapy. Cell. 2017;170:1109-1119.e10. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 800] [Cited by in RCA: 1088] [Article Influence: 136.0] [Reference Citation Analysis (0)] |
| 83. | Matson V, Fessler J, Bao R, Chongsuwat T, Zha Y, Alegre ML, Luke JJ, Gajewski TF. The commensal microbiome is associated with anti-PD-1 efficacy in metastatic melanoma patients. Science. 2018;359:104-108. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1390] [Cited by in RCA: 2126] [Article Influence: 303.7] [Reference Citation Analysis (1)] |
| 84. | Gopalakrishnan V, Spencer CN, Nezi L, Reuben A, Andrews MC, Karpinets TV, Prieto PA, Vicente D, Hoffman K, Wei SC, Cogdill AP, Zhao L, Hudgens CW, Hutchinson DS, Manzo T, Petaccia de Macedo M, Cotechini T, Kumar T, Chen WS, Reddy SM, Szczepaniak Sloane R, Galloway-Pena J, Jiang H, Chen PL, Shpall EJ, Rezvani K, Alousi AM, Chemaly RF, Shelburne S, Vence LM, Okhuysen PC, Jensen VB, Swennes AG, McAllister F, Marcelo Riquelme Sanchez E, Zhang Y, Le Chatelier E, Zitvogel L, Pons N, Austin-Breneman JL, Haydu LE, Burton EM, Gardner JM, Sirmans E, Hu J, Lazar AJ, Tsujikawa T, Diab A, Tawbi H, Glitza IC, Hwu WJ, Patel SP, Woodman SE, Amaria RN, Davies MA, Gershenwald JE, Hwu P, Lee JE, Zhang J, Coussens LM, Cooper ZA, Futreal PA, Daniel CR, Ajami NJ, Petrosino JF, Tetzlaff MT, Sharma P, Allison JP, Jenq RR, Wargo JA. Gut microbiome modulates response to anti-PD-1 immunotherapy in melanoma patients. Science. 2018;359:97-103. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 2999] [Cited by in RCA: 3297] [Article Influence: 471.0] [Reference Citation Analysis (0)] |
| 85. | Routy B, Le Chatelier E, Derosa L, Duong CPM, Alou MT, Daillère R, Fluckiger A, Messaoudene M, Rauber C, Roberti MP, Fidelle M, Flament C, Poirier-Colame V, Opolon P, Klein C, Iribarren K, Mondragón L, Jacquelot N, Qu B, Ferrere G, Clémenson C, Mezquita L, Masip JR, Naltet C, Brosseau S, Kaderbhai C, Richard C, Rizvi H, Levenez F, Galleron N, Quinquis B, Pons N, Ryffel B, Minard-Colin V, Gonin P, Soria JC, Deutsch E, Loriot Y, Ghiringhelli F, Zalcman G, Goldwasser F, Escudier B, Hellmann MD, Eggermont A, Raoult D, Albiges L, Kroemer G, Zitvogel L. Gut microbiome influences efficacy of PD-1-based immunotherapy against epithelial tumors. Science. 2018;359:91-97. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 2493] [Cited by in RCA: 3791] [Article Influence: 473.9] [Reference Citation Analysis (0)] |
| 86. | Zhang CX, Wang HY, Chen TX. Interactions between Intestinal Microflora/Probiotics and the Immune System. Biomed Res Int. 2019;2019:6764919. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 63] [Cited by in RCA: 54] [Article Influence: 9.0] [Reference Citation Analysis (0)] |
| 87. | Zeng H, Umar S, Rust B, Lazarova D, Bordonaro M. Secondary Bile Acids and Short Chain Fatty Acids in the Colon: A Focus on Colonic Microbiome, Cell Proliferation, Inflammation, and Cancer. Int J Mol Sci. 2019;20. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 150] [Cited by in RCA: 321] [Article Influence: 53.5] [Reference Citation Analysis (0)] |
| 88. | Dubin K, Callahan MK, Ren B, Khanin R, Viale A, Ling L, No D, Gobourne A, Littmann E, Huttenhower C, Pamer EG, Wolchok JD. Intestinal microbiome analyses identify melanoma patients at risk for checkpoint-blockade-induced colitis. Nat Commun. 2016;7:10391. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 560] [Cited by in RCA: 769] [Article Influence: 85.4] [Reference Citation Analysis (0)] |
| 89. | Badgeley A, Anwar H, Modi K, Murphy P, Lakshmikuttyamma A. Effect of probiotics and gut microbiota on anti-cancer drugs: Mechanistic perspectives. Biochim Biophys Acta Rev Cancer. 2021;1875:188494. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 30] [Cited by in RCA: 124] [Article Influence: 24.8] [Reference Citation Analysis (0)] |
| 90. | McNabney SM, Henagan TM. Short Chain Fatty Acids in the Colon and Peripheral Tissues: A Focus on Butyrate, Colon Cancer, Obesity and Insulin Resistance. Nutrients. 2017;9. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 361] [Cited by in RCA: 347] [Article Influence: 43.4] [Reference Citation Analysis (0)] |
| 91. | Yang W, Yu T, Huang X, Bilotta AJ, Xu L, Lu Y, Sun J, Pan F, Zhou J, Zhang W, Yao S, Maynard CL, Singh N, Dann SM, Liu Z, Cong Y. Intestinal microbiota-derived short-chain fatty acids regulation of immune cell IL-22 production and gut immunity. Nat Commun. 2020;11:4457. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 415] [Cited by in RCA: 646] [Article Influence: 129.2] [Reference Citation Analysis (0)] |
| 92. | Hakozaki T, Richard C, Elkrief A, Hosomi Y, Benlaïfaoui M, Mimpen I, Terrisse S, Derosa L, Zitvogel L, Routy B, Okuma Y. The Gut Microbiome Associates with Immune Checkpoint Inhibition Outcomes in Patients with Advanced Non-Small Cell Lung Cancer. Cancer Immunol Res. 2020;8:1243-1250. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 72] [Cited by in RCA: 201] [Article Influence: 40.2] [Reference Citation Analysis (0)] |
| 93. | Ahn J, Sinha R, Pei Z, Dominianni C, Wu J, Shi J, Goedert JJ, Hayes RB, Yang L. Human gut microbiome and risk for colorectal cancer. J Natl Cancer Inst. 2013;105:1907-1911. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 566] [Cited by in RCA: 710] [Article Influence: 59.2] [Reference Citation Analysis (1)] |
| 94. | Cresci GA, Bawden E. Gut Microbiome: What We Do and Don't Know. Nutr Clin Pract. 2015;30:734-746. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 249] [Cited by in RCA: 269] [Article Influence: 26.9] [Reference Citation Analysis (1)] |
| 95. | Wong KK, Li WA, Mooney DJ, Dranoff G. Advances in Therapeutic Cancer Vaccines. Adv Immunol. 2016;130:191-249. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 72] [Cited by in RCA: 77] [Article Influence: 8.6] [Reference Citation Analysis (0)] |
| 96. | Butterfield LH. Cancer vaccines. BMJ. 2015;350:h988. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 168] [Cited by in RCA: 188] [Article Influence: 18.8] [Reference Citation Analysis (0)] |
| 97. | Higano CS, Schellhammer PF, Small EJ, Burch PA, Nemunaitis J, Yuh L, Provost N, Frohlich MW. Integrated data from 2 randomized, double-blind, placebo-controlled, phase 3 trials of active cellular immunotherapy with sipuleucel-T in advanced prostate cancer. Cancer. 2009;115:3670-3679. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 599] [Cited by in RCA: 593] [Article Influence: 37.1] [Reference Citation Analysis (0)] |
| 98. | Long YY, Wang Y, Huang QR, Zheng GS, Jiao SC. Measurement of serum antibodies against NY-ESO-1 by ELISA: A guide for the treatment of specific immunotherapy for patients with advanced colorectal cancer. Exp Ther Med. 2014;8:1279-1284. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 8] [Cited by in RCA: 12] [Article Influence: 1.1] [Reference Citation Analysis (0)] |
| 99. | Saito T, Wada H, Yamasaki M, Miyata H, Nishikawa H, Sato E, Kageyama S, Shiku H, Mori M, Doki Y. High expression of MAGE-A4 and MHC class I antigens in tumor cells and induction of MAGE-A4 immune responses are prognostic markers of CHP-MAGE-A4 cancer vaccine. Vaccine. 2014;32:5901-5907. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 44] [Cited by in RCA: 51] [Article Influence: 4.6] [Reference Citation Analysis (0)] |
| 100. | Van Der Bruggen P, Zhang Y, Chaux P, Stroobant V, Panichelli C, Schultz ES, Chapiro J, Van Den Eynde BJ, Brasseur F, Boon T. Tumor-specific shared antigenic peptides recognized by human T cells. Immunol Rev. 2002;188:51-64. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 291] [Cited by in RCA: 282] [Article Influence: 12.3] [Reference Citation Analysis (0)] |
| 101. | Scanlan MJ, Simpson AJ, Old LJ. The cancer/testis genes: review, standardization, and commentary. Cancer Immun. 2004;4:1. [PubMed] |
| 102. | Baumgaertner P, Costa Nunes C, Cachot A, Maby-El Hajjami H, Cagnon L, Braun M, Derré L, Rivals JP, Rimoldi D, Gnjatic S, Abed Maillard S, Marcos Mondéjar P, Protti MP, Romano E, Michielin O, Romero P, Speiser DE, Jandus C. Vaccination of stage III/IV melanoma patients with long NY-ESO-1 peptide and CpG-B elicits robust CD8(+) and CD4(+) T-cell responses with multiple specificities including a novel DR7-restricted epitope. Oncoimmunology. 2016;5:e1216290. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 38] [Cited by in RCA: 50] [Article Influence: 5.6] [Reference Citation Analysis (0)] |
| 103. | Schulze T, Kemmner W, Weitz J, Wernecke KD, Schirrmacher V, Schlag PM. Efficiency of adjuvant active specific immunization with Newcastle disease virus modified tumor cells in colorectal cancer patients following resection of liver metastases: results of a prospective randomized trial. Cancer Immunol Immunother. 2009;58:61-69. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 100] [Cited by in RCA: 96] [Article Influence: 6.0] [Reference Citation Analysis (0)] |
| 104. | Hazama S, Nakamura Y, Tanaka H, Hirakawa K, Tahara K, Shimizu R, Ozasa H, Etoh R, Sugiura F, Okuno K, Furuya T, Nishimura T, Sakata K, Yoshimatsu K, Takenouchi H, Tsunedomi R, Inoue Y, Kanekiyo S, Shindo Y, Suzuki N, Yoshino S, Shinozaki H, Kamiya A, Furukawa H, Yamanaka T, Fujita T, Kawakami Y, Oka M. A phase ΙI study of five peptides combination with oxaliplatin-based chemotherapy as a first-line therapy for advanced colorectal cancer (FXV study). J Transl Med. 2014;12:108. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 71] [Cited by in RCA: 69] [Article Influence: 6.3] [Reference Citation Analysis (0)] |
| 105. | Okuno K, Sugiura F, Inoue K, Sukegawa Y. Clinical trial of a 7-peptide cocktail vaccine with oral chemotherapy for patients with metastatic colorectal cancer. Anticancer Res. 2014;34:3045-3052. [PubMed] |
| 106. | Cremolini C, Rossini D, Antoniotti C, Pietrantonio F, Lonardi S, Salvatore L, Marmorino F, Borelli B, Ambrosini M, Barsotti G, Di Stefano B, Masi G, Boccaccino A, Tamberi S, Tamburini E, Frassineti L. G, Simionato F, Fontanini G, Boni L, Falcone A. FOLFOXIRI + Bev + Atezo vs FOLFOXIRI + Bev as First-line Treatment of Unresectable Metastatic Colorectal Cancer Patients (AtezoTRIBE). Aug 4, 2021. [cited 3 November 2022]. Available from: http://clinicaltrials.gov/show/NCT03721653. |
| 107. | Mettu NB, Twohy E, Ou FS, Halfdanarson TR, Lenz HJ, Breakstone R, Boland PM, Crysler O, Wu C, Grothey A, Nixon AB, Bolch E, Niedzwiecki D, Fruth B, Schweitzer B, Elsing A, Hurwitz H, Fakih MG, Bekaii-Saab T. Capecitabine and Bevacizumab With or Without Atezolizumab in Treating Patients With Refractory Metastatic Colorectal Cancer. Jan 10, 2022. [cited 3 November 2022]. Available from: http://clinicaltrials.gov/show/NCT02873195. |
| 108. | Tabernero J, Grothey A, Arnold D, de Gramont A, Ducreux M, O'Dwyer P, Tahiri A, Gilberg F, Irahara N, Schmoll HJ, Van Cutsem E. MODUL cohort 2: an adaptable, randomized, signal-seeking trial of fluoropyrimidine plus bevacizumab with or without atezolizumab maintenance therapy for BRAF(wt) metastatic colorectal cancer. ESMO Open. 2022;7:100559. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 2] [Cited by in RCA: 26] [Article Influence: 8.7] [Reference Citation Analysis (0)] |
| 109. | Yuki S, Bando H, Tsukada T, Inamori K, Komatsu Y, Homma S, Uemura M, Kato T, Kotani D, Fukuoka S, Nakamura N, Fukui M, Wakabayashi M, Kojima M, Sato A, Togashi Y, Nishikawa H, Ito M, Yoshino T. Study to Nivolumab Following Preoperative Chemoradiotherapy. Sep 16, 2021. [cited 3 November 2022]. Available from: http://clinicaltrials.gov/show/NCT02948348. |
| 110. | Salvatore L, Bensi M, Pietrantonio F, Boccaccino A, Barbara C, Auriemma A, Ratti M, Tamburini E, Bordonaro R, Clavarezza M, Avallone A, Bergamo F, Granetto C, Bustreo S, Di Fabio F, Smiroldo V, Corvari B, Tortora G. Immunotherapy In Locally Advanced Rectal Cancer (AVANA). Aug 4, 2022. [cited 3 November 2022]. Available from: http://clinicaltrials.gov/show/NCT03854799. |
| 111. | Zhang F, Guo J, Zhang Z, Qian Y, Wang G, Duan M, Zhao H, Yang Z, Jiang X. Mesenchymal stem cell-derived exosome: A tumor regulator and carrier for targeted tumor therapy. Cancer Lett. 2022;526:29-40. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 15] [Cited by in RCA: 85] [Article Influence: 21.3] [Reference Citation Analysis (0)] |
| 112. | Bejarano L, Jordāo MJC, Joyce JA. Therapeutic Targeting of the Tumor Microenvironment. Cancer Discov. 2021;11:933-959. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 151] [Cited by in RCA: 914] [Article Influence: 228.5] [Reference Citation Analysis (0)] |
| 113. | Xiao Y, Freeman GJ. The microsatellite instable subset of colorectal cancer is a particularly good candidate for checkpoint blockade immunotherapy. Cancer Discov. 2015;5:16-18. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 240] [Cited by in RCA: 286] [Article Influence: 28.6] [Reference Citation Analysis (0)] |
| 114. | Peddareddigari VG, Wang D, Dubois RN. The tumor microenvironment in colorectal carcinogenesis. Cancer Microenviron. 2010;3:149-166. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 147] [Cited by in RCA: 177] [Article Influence: 11.8] [Reference Citation Analysis (2)] |
| 115. | Liu C, Papukashvili D, Dong Y, Wang X, Hu X, Yang N, Cai J, Xie F, Rcheulishvili N, Wang PG. Identification of Tumor Antigens and Design of mRNA Vaccine for Colorectal Cancer Based on the Immune Subtype. Front Cell Dev Biol. 2021;9:783527. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 5] [Cited by in RCA: 15] [Article Influence: 5.0] [Reference Citation Analysis (0)] |
| 116. | Díaz-Gay M, Alexandrov LB. Unraveling the genomic landscape of colorectal cancer through mutational signatures. Adv Cancer Res. 2021;151:385-424. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 6] [Cited by in RCA: 19] [Article Influence: 4.8] [Reference Citation Analysis (0)] |
| 117. | Yarchoan M, Johnson BA 3rd, Lutz ER, Laheru DA, Jaffee EM. Targeting neoantigens to augment antitumour immunity. Nat Rev Cancer. 2017;17:209-222. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 524] [Cited by in RCA: 668] [Article Influence: 83.5] [Reference Citation Analysis (0)] |
| 118. | Yachida S, Mizutani S, Shiroma H, Shiba S, Nakajima T, Sakamoto T, Watanabe H, Masuda K, Nishimoto Y, Kubo M, Hosoda F, Rokutan H, Matsumoto M, Takamaru H, Yamada M, Matsuda T, Iwasaki M, Yamaji T, Yachida T, Soga T, Kurokawa K, Toyoda A, Ogura Y, Hayashi T, Hatakeyama M, Nakagama H, Saito Y, Fukuda S, Shibata T, Yamada T. Metagenomic and metabolomic analyses reveal distinct stage-specific phenotypes of the gut microbiota in colorectal cancer. Nat Med. 2019;25:968-976. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 404] [Cited by in RCA: 875] [Article Influence: 145.8] [Reference Citation Analysis (0)] |
| 119. | Rayner E, van Gool IC, Palles C, Kearsey SE, Bosse T, Tomlinson I, Church DN. A panoply of errors: polymerase proofreading domain mutations in cancer. Nat Rev Cancer. 2016;16:71-81. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 246] [Cited by in RCA: 278] [Article Influence: 30.9] [Reference Citation Analysis (0)] |
| 120. | Gong J, Wang C, Lee PP, Chu P, Fakih M. Response to PD-1 Blockade in Microsatellite Stable Metastatic Colorectal Cancer Harboring a POLE Mutation. J Natl Compr Canc Netw. 2017;15:142-147. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 140] [Cited by in RCA: 172] [Article Influence: 21.5] [Reference Citation Analysis (0)] |
| 121. | He J, Ouyang W, Zhao W, Shao L, Li B, Liu B, Wang D, Han-Zhang H, Zhang Z, Li W. Distinctive genomic characteristics in POLE/POLD1-mutant cancers can potentially predict beneficial clinical outcomes in patients who receive immune checkpoint inhibitor. Ann Transl Med. 2021;9:129. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 12] [Cited by in RCA: 26] [Article Influence: 6.5] [Reference Citation Analysis (0)] |
| 122. | Chen YX, Wang ZX, Yuan SQ, Jiang TJ, Huang YS, Xu RH, Wang F, Zhao Q. POLE/POLD1 mutation in non-exonuclease domain matters for predicting efficacy of immune-checkpoint-inhibitor therapy. Clin Transl Med. 2021;11:e524. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 7] [Reference Citation Analysis (0)] |