Published online Mar 16, 2013. doi: 10.4253/wjge.v5.i3.117
Revised: December 25, 2012
Accepted: January 23, 2013
Published online: March 16, 2013
Processing time: 183 Days and 23.1 Hours
AIM: To evaluate the clinical usefulness of single-balloon endoscopy (SBE) in patients in whom a colonoscope was technically difficult to insert previously.
METHODS: The study group comprised 15 patients (8 men and 7 women) who underwent SBE for colonoscopy (30 sessions). The number of SBE sessions was 1 in 7 patients, 2 in 5 patients, 3 in 1 patient, 4 in 1 patient, and 6 in 1 patient. In all patients, total colonoscopy was previously unsuccessful. The reasons for difficulty in scope passage were an elongated colon in 6 patients, severe intestinal adhesions after open surgery in 4, an elongated colon and severe intestinal adhesions in 2, a left inguinal hernia in 2, and multiple diverticulosis of the sigmoid colon in 1. Three endoscopists were responsible for SBE. The technique for inserting SBE in the colon was basically similar to that in the small intestine. The effectiveness of SBE was assessed on the basis of the success rate of total colonoscopy and the presence or absence of complications. We also evaluated the diagnostic and treatment outcomes of colonoscopic examinations with SBE.
RESULTS: Total colonoscopy was successfully accomplished in all sessions. The mean insertion time to the cecum was 22.9 ± 8.9 min (range 9 to 40). Abnormalities were found during 21 sessions of SBE. The most common abnormality was colorectal polyps (20 sessions), followed by radiation colitis (3 sessions) and diverticular disease of the colon (3 sessions). Colorectal polyps were resected endoscopically in 15 sessions. A total of 42 polyps were resected endoscopically, using snare polypectomy in 32 lesions, hot biopsy in 7 lesions, and endoscopic mucosal resection in 3 lesions. Fifty-six colorectal polyps were newly diagnosed on colonoscopic examination with SBE. Histopathologically, these lesions included 2 intramucosal cancers, 42 tubular adenomas, and 2 tubulovillous adenomas. The mean examination time was 48.2 ± 20.0 min (range 25 to 90). Colonoscopic examination or endoscopic treatment with SBE was not associated with any serious complications.
CONCLUSION: SBE is a useful and safe procedure in patients in whom a colonoscope is technically difficult to insert.
- Citation: Kobayashi K, Mukae M, Ogawa T, Yokoyama K, Sada M, Koizumi W. Clinical usefulness of single-balloon endoscopy in patients with previously incomplete colonoscopy. World J Gastrointest Endosc 2013; 5(3): 117-121
- URL: https://www.wjgnet.com/1948-5190/full/v5/i3/117.htm
- DOI: https://dx.doi.org/10.4253/wjge.v5.i3.117
Colonoscopy is playing an increasingly important part in the diagnosis and treatment of colorectal diseases. Its diagnostic role has been enhanced by the development of improved imaging techniques such as magnifying endoscopy and narrow band imaging. Therapeutically, progress in resection techniques such as endoscopic mucosal resection and endoscopic submucosal dissection has contributed to the widespread application of colonoscopic therapy. The availability of improved devices such as variable stiffness and small-caliber colonoscopes allows instruments optimally suited for individual patients to be selected[1,2]. Despite recent progress, however, the passage of a colonoscope is often difficult in subjects who have an elongated colon or severe adhesions.
Balloon endoscopy was originally developed to facilitate insertion of an endoscope deep into the small intestine. First, double-balloon endoscopy (DBE) was developed by Yamamoto et al[3]. Subsequently, single-balloon endoscopy (SBE) was developed and applied clinically[4-6]. A balloon at the tip of a sliding tube or an overtube is inflated to grip the intestine, and both the scope and the sliding tube are simultaneously withdrawn, thus shortening the intestine. By repeating these maneuvers, the endoscope can be inserted more deeply into the small intestine.
We performed colonoscopy by SBE in patients in whom a conventional colonoscope was technically difficult to insert because of an elongated colon or severe adhesions and retrospectively evaluated the clinical usefulness of this procedure.
The study group comprised 15 patients (8 men and 7 women) who underwent SBE for colonoscopy (30 sessions) in our hospital from July 2007 through June 2012. The number of SBE sessions was 1 in 7 patients, 2 in 5 patients, 3 in 1 patient, 4 in 1 patient, and 6 in 1 patient. The mean age at examination was 65.7 ± 8.7 years (range 38 to 81). Seven patients concurrently had cardiovascular diseases such as arrhythmias and hypertension, 1 had diabetes mellitus, and 1 had a history of cerebral infarction. Six patients had a history of open surgery (total hysterectomy in 5 and cholecystectomy in 2). Two patients who had undergone total hysterectomy had received radiotherapy to treat uterine cancer.
Total colonoscopy was technically difficult to perform in all patients. In 5 patients, total colonoscopy was unable to be performed by their previous physicians. In the other 10 patients, total colonoscopy was not successfully accomplished at the previous examination in our hospital. In 9 of these patients, the first author of this paper, who has more than 20 years of experience in colonoscopy, was charge of the previous examinations. The deepest part of the colon reached on previous unsuccessful colonoscopic examinations was the sigmoid colon in 7 patients, followed by the transverse colon in 3, the descending colon in 2, and the ascending colon in 2. The details were unknown for 1 patient in whom colonoscopy was performed by a previous physician. The mean time from starting scope insertion to the unsuccessful discontinuation of examination was 30.7 ± 6.4 min (range 19 to 38 min) in 10 patients for whom the details were provided by their previous physicians; the details of examination were unavailable for 5 patients. The reasons for difficulty in scope passage were an elongated colon in 6 patients (40%), severe intestinal adhesions after open surgery in 4 (27%), an elongated colon and severe intestinal adhesions in 2 (13%), a left inguinal hernia in 2 (13%), and multiple diverticulosis of the sigmoid colon in 1 (7%).
Among 30 sessions of SBE, the objective was follow-up after endoscopic resection of colorectal polyps in 21 sessions (70%), endoscopic resection of colorectal polyps in 5 sessions, confirmation of colorectal polyps suspected on barium enema examination in 3 sessions, and screening for colorectal disease in 1 session. Three endoscopists were responsible for SBE. The first author was in charge of 26 sessions (87%). Twenty-three sessions (77%) were performed on an outpatient basis, and 7 sessions (23%) were performed after hospitalization.
As premedication, antispasmodic drugs such as scopolamine butylbromide (10 mg) were administered before 24 sessions (80%). Sedatives and analgesic agents were concurrently used in 28 sessions (93%), including 14 sessions in which multiple drugs were used. The used drugs were diazepam in 25 sessions, pethidine hydrochloride in 15, propofol in 2, and midazolam in 1.
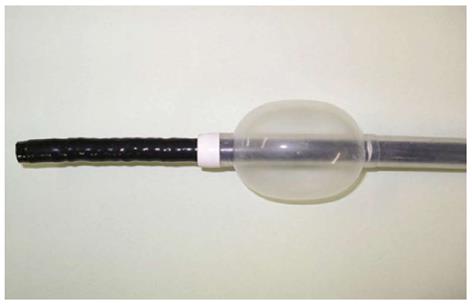
SBE was performed with an enteroscope with an effective length of 2000 mm, an outer diameter of 9.2 mm, and a forceps channel diameter of 2.8 mm, allowing the use of conventional endoscopic devices (Figure 1). The SBE system consisted of a dedicated sliding tube with a silicone balloon attached to its tip. Single-balloon colonoscopy was performed by the two-operator technique under fluoroscopic guidance. The basic insertion procedure was similar to that of conventional enteroscopy. The balloon attached to the sliding tube was inflated to grip the intestine, and both the scope and the sliding tube were withdrawn in tandem to shorten the intestine. By repeating these steps, the endoscope was inserted deeper into the intestine[4-6]. To insert the endoscope into the large intestine, the abdomen was compressed manually or body position was changed as required. During colonoscopic examination with SBE, air was insufflated 25 times, and carbon dioxide was insufflated 5 times at the discretion of the endoscopist in charge.
The primary variable used to evaluate SBE was the success rate of total colonoscopy, which was defined as insertion of the endoscope into the cecum. Secondary variables were the presence or absence of complications related to colonoscopy with SBE. We also evaluated the diagnostic and treatment outcomes of colonoscopic examinations with SBE.
This study was approved by the Institutional Ethics Committees of Kitasato University School of Medicine. Before performing colonoscopy with SBE, we provided all patients with a detailed explanation of the objectives and methods of examination, possible complications, and the possibility to select other procedures, such as barium enema. The decision to undergo colonoscopy with SBE was in accordance with the free will of each patient. Written informed consent for examination was obtained from all subjects. Continuous data are expressed as means ± SD.
Total colonoscopy was successfully performed by SBE in all sessions. The mean time required to reach the cecum was 22.9 ± 8.9 min (range 9 to 40 min).
The main complication associated with SBE was mild redness of the colorectal mucosa in some patients, caused by insertion of the sliding tube and pressure applied by the balloon. However, there were no serious complications associated with colonoscopic examination with SBE.
Abnormal findings were found during 21 (70%) sessions of SBE. The most common abnormality was colorectal polyps (20 sessions), followed by radiation colitis (3 sessions) and diverticular disease of the colon (3 sessions). Finally, 56 colorectal polyps were newly diagnosed on colonoscopy with SBE. Colorectal polyps were resected endoscopically in 15 sessions. A total of 42 polyps were resected endoscopically, using snare polypectomy in 32 lesions, hot biopsy in 7 lesions, and endoscopic mucosal resection in 3 lesions. The 14 other polyps underwent biopsy with histopathological evaluation. The final histopathological diagnoses were intramucosal cancer in 2 lesions, tubular adenoma in 42, tubulovillous adenoma in 2, hyperplastic polyp in 8, and inflammatory polyp in 2. There were no complications associated with endoscopic resection or biopsy of the colorectal polyps. The mean examination time was 48.2 ± 20.0 min (range 25 to 90 min).
Colonoscopy is essential for the diagnosis and treatment of colorectal disease. In particular, the indication range of colonoscopic treatment has been broadened owing to improved techniques for the endoscopic resection of colorectal tumors, endoscopic hemostasis, and endoscopic balloon dilatation of intestinal stenosis. As for colonoscopic devices, image quality as well as insertability has improved considerably. However, total colonoscopy is still technically difficult to perform in about 10% to 15% of subjects[7-10]. Even though our hospital specializes in gastrointestinal endoscopy, we still encounter patients in whom total colonoscopy is technically difficult to perform. Excluding follow-up examinations after colorectal surgery or other procedures, we performed 3140 sessions of colonoscopy during the year of 2011. A conventional colonoscope could not be inserted to the cecum in 32 sessions (1.0%). In many patients with difficulty in scope insertion, barium enema examination was performed to evaluate sites of the colon that could not be assessed on endoscopy. Factors related to technical difficulty in colonoscope insertion have been reported to include advanced age, female sex, a low body mass index, an elongated colon or adhesions, multiple diverticula, and inadequate bowel preparation[7-11]. In our series, the main factors that precluded colonoscope passage during SBE were an elongated colon and severe adhesions.
Patients in whom colonoscope insertion is expected to be technically difficult, especially those who are sensitive to discomfort and pain associated with colonoscopy, should receive adequate doses of analgesics and sedatives before examination. Manual compression of the abdomen by an assistant and the use of an overtube may facilitate scope passage in patients in whom insertion is difficult because of an elongated colon[11]. In such patients, a variable stiffness colonoscope or a colonoscope with a long effective length should be used. Lichtenstein et al[12] reported that the use of a small-caliber, push-type enteroscope with an effective length of greater than 2000 mm allowed total colonoscopy to be performed in about half of all patients in whom scope passage was difficult. If colonoscopy is performed in patients with severe adhesions in the colon after open surgery, a small-caliber colonoscope should be used. At present, very small-caliber colonoscopes with an outer diameter of 10 mm or less are commercially available. We previously reported that the use of a colonoscope with an outer diameter of 9.2 mm and an effective length of 1600 mm (CF-PQ260L®, Olympus Co., Tokyo, Japan) allowed total colonoscopy to be performed in the majority of patients in whom scope insertion was precluded by an elongated colon and adhesions[13]. Preliminary studies have suggested that the use of a guide-wire-directed endoscope or a spiral overtube can facilitate colonoscope insertion when difficulty is encountered[14,15].
During colonoscope insertion, the scope may bend or form large loops in patients with an elongated colon. The presence of bowel adhesions can restrict mobility of the colon and cause sharp bends, which preclude scope passage. Excessive force to promote passage can injure the intestine. We performed colonoscopic examination by SBE in patients with a history of difficulty in scope insertion even by experienced endoscopists. A balloon attached to a sliding tube was inflated to grip and shorten the intestine, thereby preventing overextension of the intestine during the procedure and facilitating passage of the endoscope through regions with adhesion. Because the outer diameter of the SBE was only 9.2 mm, pushing the scope and distension of the intestine caused only mild discomfort to patients. Subsequent shortening of the intestinal tract with a sliding tube was also easily accomplished. In our study, SBE permitted total colonoscopy in all patients with a history of difficulty in colonoscope insertion. There were no serious complications associated with colonoscope insertion or endoscopic treatment. Eight patients (53%) underwent repeated examinations, and total colonoscopy was successfully accomplished at all sessions, confirming that SBE is consistently effective. During SBE, the mean time required for scope insertion into the cecum was 22.9 min. This prolonged insertion time was attributed to the extra time required for insertion of a sliding tube and shortening of the intestine.
Balloon endoscopy has previously been reported to be useful for colonoscopy in patients with a history of difficulty in colonoscope insertion[16-23]. Most studies used a DBE, but two studies conducted in the United State and Holland reported the results of SBE[22,23]. Keswani[22] randomly assigned 30 patients with a history of difficulty in colonoscope insertion to undergo SBE or conventional colonoscopy. The success rate of total colonoscopy was significantly higher in the SBE group (93%) than in the conventional colonoscopy group (50%), with no examination-related complications. Teshima et al[23] reported that total colonoscopy was successfully accomplished in 22 (96%) of 23 sessions of SBE performed in 22 patients with a history of difficulty in colonoscope insertion. In contrast to DBE, SBE does not require a balloon attached to the tip of the scope. Consequently, intestinal gripping strength might be lower with SBE than with DBE. However, our results suggest that SBE with only one balloon attached to the sliding tube was able to adequately shorten the large intestine, allowing total colonoscopy to be successfully accomplished.
Because SBE does not require attachment of a balloon to the scope tip, the preparation time is shorter and insertion of the scope is easier than with DBE. One study reported that the single-balloon technique performed with a DBE, in which a balloon was attached only to the overtube, facilitated scope insertion in patients in whom a colonoscope had been technically difficult to insert[17]. DBE with a short effective length of 1520 mm are now available and have been reported to be useful[21].
In addition to diagnostic procedures such as biopsy, SBE allowed colorectal polyps to be endoscopically resected with no problems or complications. In contrast to a standard colonoscope, the opening of the forceps channel of SBE is located in the 8 o’clock direction. The field of vision is thus similar to that during upper gastrointestinal endoscopy. Because the scope is long, twisting maneuvers applied by the operator are sometimes not transmitted to the scope tip, making it difficult to accurately position endoscopic devices relative to target lesions. Because the forceps channel diameter was 2.8 mm, which is smaller than that of a standard colonoscope, it was difficult to aspirate intestinal juice and air after the insertion of endoscopic devices. Many lesions located at curvatures of the large intestine or on the proximal sides of folds were difficult to view endoscopically. When the intestine was shortened with the use of a sliding tube, the region surrounding lesions was straightened, facilitating lesion inspection as well as endoscopic therapy.
Our results showed that SBE facilitated total colonoscopy in patients in whom scope passage was difficult, confirming that SBE is useful and safe in Japanese subjects. However, this was a retrospective study in a small number of patients, and 1 endoscopist with many years of experience in colonoscopy performed most of the examinations. To clarify whether the technical ability of the operator affects the performance of SBE, prospective studies performed by endoscopists with different levels of experience are needed.
Colonoscopy is playing an increasingly important part in the diagnosis and treatment of colorectal diseases. Therapeutically, progress in resection techniques such as endoscopic mucosal resection and endoscopic submucosal dissection has contributed to the widespread application of colonoscopic therapy. Despite recent progress, however, the passage of a colonoscope is often difficult in subjects who have an elongated colon or severe adhesions.
Colonoscopy’s diagnostic role has been enhanced by the development of improved imaging techniques such as magnifying endoscopy and narrow band imaging. Therapeutically, progress in resection techniques such as endoscopic mucosal resection and endoscopic submucosal dissection has contributed to the widespread application of colonoscopic therapy.
The results showed that single-balloon endoscopy (SBE) facilitated total colonoscopy in patients in whom scope passage was difficult, confirming that SBE is useful and safe in Japanese subjects. However, this was a retrospective study in a small number of patients, and 1 endoscopist with many years of experience in colonoscopy performed most of the examinations.
The manuscript describes an interesting technique in the diagnosis and treatment of colorectal diseases. It is an excellent article on single balloon endoscopy.
P- Reviewers Efthymiou A, Bolke E, Mudawi HMY, Iijima H, Gonzalez-Granado L S- Editor Song XX L- Editor A E- Editor Zhang DN
| 1. | Brooker JC, Saunders BP, Shah SG, Williams CB. A new variable stiffness colonoscope makes colonoscopy easier: a randomised controlled trial. Gut. 2000;46:801-805. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 80] [Cited by in RCA: 73] [Article Influence: 2.9] [Reference Citation Analysis (0)] |
| 2. | Horiuchi A, Nakayama Y, Kajiyama M, Fujii H, Tanaka N. Usefulness of a small-caliber, variable-stiffness colonoscope as a backup in patients with difficult or incomplete colonoscopy. Am J Gastroenterol. 2004;99:1936-1940. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 31] [Cited by in RCA: 33] [Article Influence: 1.6] [Reference Citation Analysis (0)] |
| 3. | Yamamoto H, Yano T, Kita H, Sunada K, Ido K, Sugano K. New system of double-balloon enteroscopy for diagnosis and treatment of small intestinal disorders. Gastroenterology. 2003;125:1556; author reply 1556-1557. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 1] [Reference Citation Analysis (0)] |
| 4. | Kobayashi K, Katsumata T, Saigenji K. Clinical usefulness of single-balloon enteroscopy for the diagnosis and treatment of small-intestinal diseases. New Challenges in Gastrointestinal Endoscopy. Tokyo: Springer 2008; 243-250. |
| 5. | Kawamura T, Yasuda K, Tanaka K, Uno K, Ueda M, Sanada K, Nakajima M. Clinical evaluation of a newly developed single-balloon enteroscope. Gastrointest Endosc. 2008;68:1112-1116. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 107] [Cited by in RCA: 110] [Article Influence: 6.5] [Reference Citation Analysis (0)] |
| 6. | Tsujikawa T, Saitoh Y, Andoh A, Imaeda H, Hata K, Minematsu H, Senoh K, Hayafuji K, Ogawa A, Nakahara T. Novel single-balloon enteroscopy for diagnosis and treatment of the small intestine: preliminary experiences. Endoscopy. 2008;40:11-15. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 215] [Cited by in RCA: 209] [Article Influence: 12.3] [Reference Citation Analysis (0)] |
| 7. | Shah HA, Paszat LF, Saskin R, Stukel TA, Rabeneck L. Factors associated with incomplete colonoscopy: a population-based study. Gastroenterology. 2007;132:2297-2303. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 238] [Cited by in RCA: 267] [Article Influence: 14.8] [Reference Citation Analysis (0)] |
| 8. | Loffeld RJ, van der Putten AB. The completion rate of colonoscopy in normal daily practice: factors associated with failure. Digestion. 2009;80:267-270. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 29] [Cited by in RCA: 26] [Article Influence: 1.7] [Reference Citation Analysis (0)] |
| 9. | Anderson JC, Gonzalez JD, Messina CR, Pollack BJ. Factors that predict incomplete colonoscopy: thinner is not always better. Am J Gastroenterol. 2000;95:2784-2787. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 141] [Cited by in RCA: 151] [Article Influence: 6.0] [Reference Citation Analysis (0)] |
| 10. | Aslinia F, Uradomo L, Steele A, Greenwald BD, Raufman JP. Quality assessment of colonoscopic cecal intubation: an analysis of 6 years of continuous practice at a university hospital. Am J Gastroenterol. 2006;101:721-731. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 116] [Cited by in RCA: 135] [Article Influence: 7.1] [Reference Citation Analysis (0)] |
| 11. | Rex DK, Chen SC, Overhiser AJ. Colonoscopy technique in consecutive patients referred for prior incomplete colonoscopy. Clin Gastroenterol Hepatol. 2007;5:879-883. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 70] [Cited by in RCA: 74] [Article Influence: 4.1] [Reference Citation Analysis (0)] |
| 12. | Lichtenstein GR, Park PD, Long WB, Ginsberg GG, Kochman ML. Use of a push enteroscope improves ability to perform total colonoscopy in previously unsuccessful attempts at colonoscopy in adult patients. Am J Gastroenterol. 1999;94:187-190. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 35] [Cited by in RCA: 34] [Article Influence: 1.3] [Reference Citation Analysis (0)] |
| 13. | Kobayashi K, Katou A, Mukae M, Ogawa T, Haruki S, Yokoyama K, Sada M, Koizumi W. Advantages and disadvantages of small-caliber endoscope with respect to insertion and examination. Endoscopia Digestiva. 2011;23:1103-1108. |
| 14. | Fritscher-Ravens A, Fox S, Swain CP, Milla P, Long G. CathCam guide wire-directed colonoscopy: first pilot study in patients with a previous incomplete colonoscopy. Endoscopy. 2006;38:209-213. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 19] [Cited by in RCA: 23] [Article Influence: 1.2] [Reference Citation Analysis (0)] |
| 15. | Schembre DB, Ross AS, Gluck MN, Brandabur JJ, McCormick SE, Lin OS. Spiral overtube-assisted colonoscopy after incomplete colonoscopy in the redundant colon. Gastrointest Endosc. 2011;73:515-519. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 29] [Cited by in RCA: 30] [Article Influence: 2.1] [Reference Citation Analysis (0)] |
| 16. | Pasha SF, Harrison ME, Das A, Corrado CM, Arnell KN, Leighton JA. Utility of double-balloon colonoscopy for completion of colon examination after incomplete colonoscopy with conventional colonoscope. Gastrointest Endosc. 2007;65:848-853. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 78] [Cited by in RCA: 78] [Article Influence: 4.3] [Reference Citation Analysis (0)] |
| 17. | May A, Nachbar L, Ell C. Push-and-pull enteroscopy using a single-balloon technique for difficult colonoscopy. Endoscopy. 2006;38:395-398. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 47] [Cited by in RCA: 46] [Article Influence: 2.4] [Reference Citation Analysis (0)] |
| 18. | Mönkemüller K, Knippig C, Rickes S, Fry LC, Schulze A, Malfertheiner P. Usefulness of the double-balloon enteroscope in colonoscopies performed in patients with previously failed colonoscopy. Scand J Gastroenterol. 2007;42:277-278. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 32] [Cited by in RCA: 33] [Article Influence: 1.8] [Reference Citation Analysis (0)] |
| 19. | Moreels TG, Macken EJ, Roth B, Van Outryve MJ, Pelckmans PA. Cecal intubation rate with the double-balloon endoscope after incomplete conventional colonoscopy: a study in 45 patients. J Gastroenterol Hepatol. 2010;25:80-83. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 35] [Cited by in RCA: 21] [Article Influence: 1.4] [Reference Citation Analysis (0)] |
| 20. | Kaltenbach T, Soetikno R, Friedland S. Use of a double balloon enteroscope facilitates caecal intubation after incomplete colonoscopy with a standard colonoscope. Dig Liver Dis. 2006;38:921-925. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 1] [Reference Citation Analysis (0)] |
| 21. | Gay G, Delvaux M. Double-balloon colonoscopy after failed conventional colonoscopy: a pilot series with a new instrument. Endoscopy. 2007;39:788-792. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 48] [Cited by in RCA: 51] [Article Influence: 2.8] [Reference Citation Analysis (0)] |
| 22. | Keswani RN. Single-balloon colonoscopy versus repeat standard colonoscopy for previous incomplete colonoscopy: a randomized, controlled trial. Gastrointest Endosc. 2011;73:507-512. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 34] [Cited by in RCA: 38] [Article Influence: 2.7] [Reference Citation Analysis (0)] |
| 23. | Teshima CW, Aktas H, Haringsma J, Kuipers EJ, Mensink PB. Single-balloon-assisted colonoscopy in patients with previously failed colonoscopy. Gastrointest Endosc. 2010;71:1319-1323. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 37] [Cited by in RCA: 38] [Article Influence: 2.5] [Reference Citation Analysis (0)] |