Published online Apr 16, 2011. doi: 10.4253/wjge.v3.i4.71
Revised: February 23, 2011
Accepted: March 2, 2011
Published online: April 16, 2011
AIM: To evaluate the association of Helicobacter pylori (H.pylori)-related chronic gastritis stage with upper gastrointestinal symptoms and gastroesophageal reflux disease (GERD).
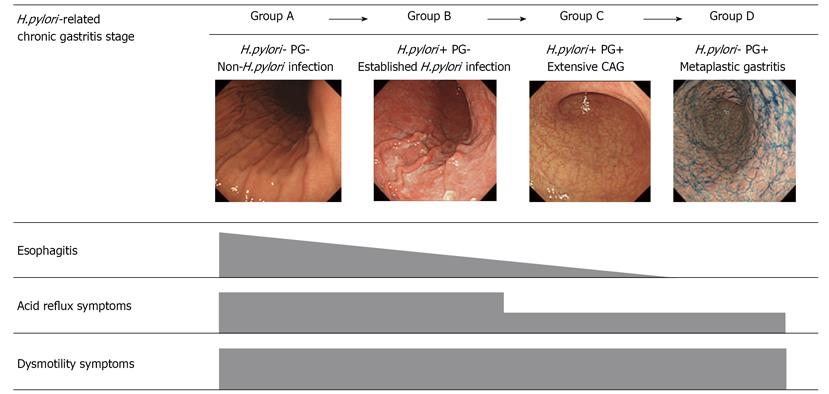
METHODS: Subjects underwent upper gastrointestinal endoscopy, a questionnaire using a frequency scale for symptoms of GERD (FSSG), and measurements of serum H.pylori-antibody and pepsinogen (PG) levels. They were classified into the following 4 groups in terms of H.pylori-related chronic gastritis stage: Group A (n = 219), H.pylori(-)PG(-); Group B (n = 310), H.pylori(+)PG(-); Group C (n = 279), H.pylori(+)PG(+); and Group D (n = 17), H.pylori(-)PG(+).
RESULTS: Reflux esophagitis occurred in 30.6% of Group A, 14.5% of Group B, 6.8% of Group C, and 0% of Group D (P < 0.001). Scores for acid reflux symptoms decreased significantly with chronic gastritis stage (from Group A to D) (P < 0.05), while scores for dysmotility symptoms did not differ significantly. The prevalence of non-erosive reflux disease (NERD) did not differ among groups. However, in subjects with GERD, the prevalence of NERD tended to increase with chronic gastritis stage (P = 0.081).
CONCLUSION: Acid reflux symptoms and the prevalence of reflux esophagitis can be assessed by measuring both serum H.pylori-antibody and PG levels.
-
Citation: Enomoto S, Oka M, Ohata H, Mukoubayashi C, Watanabe M, Moribata K, Muraki Y, Shingaki N, Deguchi H, Ueda K, Inoue I, Maekita T, Iguchi M, Yanaoka K, Tamai H, Fujishiro M, Mohara O, Ichinose M. Assessment of gastroesophageal reflux disease by serodiagnosis of
Helicobacter pylori -related chronic gastritis stage. World J Gastrointest Endosc 2011; 3(4): 71-77 - URL: https://www.wjgnet.com/1948-5190/full/v3/i4/71.htm
- DOI: https://dx.doi.org/10.4253/wjge.v3.i4.71
Gastroesophageal reflux disease (GERD) includes not only reflux esophagitis (RE) confirmed by upper gastrointestinal endoscopy, but also non-erosive reflux disease (NERD) characterized only by subjective symptoms, such as heartburn without RE. The Montreal definition was presented as the worldwide consensus on GERD in 2006[1] and is based mostly on subjective symptoms: “GERD is a condition that develops when the reflux of stomach contents causes troublesome symptoms and/or complications”. According to this definition, GERD is further classified into esophageal syndrome and extraesophageal syndrome, and a wide variety of symptoms are present. Thus, closer examination of subjective symptoms is required in differentiating GERD from other organic digestive tract diseases.
Questionnaires are effective in ascertaining the subjective symptoms of GERD patients. Many GERD-specific questionnaires have been developed[2], including the questionnaire for the diagnosis of reflux diseases[3], which is the most widely used of these questionnaires around the world. In Japan, Kusano et al developed the frequency scale for symptoms of GERD (FSSG)[4], a scale that has been used for early diagnosis and therapy assessment. Of the 12 FSSG questions, 7 questions deal with acid reflux symptoms, and the remaining 5 questions deal with gastrointestinal dysmotility symptoms, allowing GERD to be assessed by symptom group[5]. Assessing upper gastrointestinal symptoms by broadly dividing them into two groups is not only useful for planning treatment strategy for GERD[6], but it is also important for objectively analyzing the disease state.
By measuring two serum parameters, the Helicobacter pylori (H.pylori) antibody (Ab) titer and the serum pepsinogen (PG) level as a screening test for extensive chronic atrophic gastritis (CAG)[7], we have graded H.pylori-related chronic gastritis into four stages from A to D: Group A, H.pylori-negative/PG-negative; Group B, H.pylori-positive/PG-negative; Group C, H.pylori-positive/PG-positive; and Group D, H.pylori-negative/PG-positive. Group A included H.pylori non-infected healthy subjects. Group B showed established H.pylori infection, but without CAG. Group C had CAG. Group D had severe intestinal metaplasia due to progression of CAG, but H.pylori had been spontaneously eliminated, representing so-called metaplastic gastritis. CAG advances from Ato B to C, and then to D. We have documented that the incidence of gastric cancer gradually increases with chronic gastritis progression[8,9,10]. This has enabled screening of high-risk patients for gastric cancer based on serodiagnosis. An inverse relationship has been reported between CAG and RE onset[11], and many studies have found that the incidence of H.pylori infection is lower in Japanese RE patients than in healthy individuals (control group)[12-14]. A study found that NERD is closely related to H.pylori infection and progression in gastric mucosal atrophy[15]. Moreover, one study found a negative correlation between GERD and the anti-H.pylori-Ab positive rate[16], while another study documented that H.pylori infection was unrelated to GERD and was neither an exacerbating factor nor a preventive factor[17]. To the best of our knowledge, no studies have used GERD-specific questionnaires to quantify acid reflux and gastrointestinal dysmotility symptoms and to closely examine the relationships between H.pylori-related chronic gastritis progression and upper gastrointestinal symptoms.
In routine clinical care, performing endoscopy on all patients complaining of upper gastrointestinal symptoms is difficult, and some supplementary parameters would be useful to gather more information to make the diagnosis of GERD. The aim of this study was to examine the relationship of H.pylori and PG status with GERD.
In Japan, health checkup programs are performed to identify selected diseases (e.g., gastric cancer) in their early stages of development. Both symptom-free subjects and subjects showing specific symptoms took part in upper gastrointestinal endoscopic examinations at our institution. Between January 2006 and March 2008, a total of 1165 factory workers (1147 males, 18 females) ranging in age from 40 to 70 years who underwent upper gastrointestinal endoscopy and completed the FSSG questionnaire were enrolled. In addition, all enrolled subjects underwent serological testing and their H.pylori-Ab titers and serum PG levels were measured. Subjects who had a previous history of surgical resection of the stomach, H.pylori eradication, or those who had been prescribed a proton pump inhibitor (PPI), which might affect gastrointestinal function, were excluded from the study. Furthermore, subjects with and without H.pylori infection were selected for the study using serum-specific antibody titers as described in the following section. Thus, 825 subjects (812 males, 13 females) were eligible for this study. The ethics committee of Wakayama Medical University approved the study protocols.
H.pylori-Ab titers were measured using an enzyme-linked immunosorbent assay (ELISA) (MBL, Nagoya, Japan)[18]. In the present study, H.pylori-Ab titers ≥ 50 U/mL were taken to be H.pylori-positive, and < 30 U/mL indicated H.pylori-negative. H.pylori-Ab titers ≥ 30 but < 50 U/mL were considered unclassifiable, and subjects showing titers within this range were excluded from H.pylori infection assessment. The sensitivity and specificity of the ELISA test used in this study were 93.5% and 92.5%, respectively[18]. Serum PG levels were measured by radioimmunoassay (Dainabot, Tokyo, Japan)[19]. PG, a measure of gastric atrophy, was considered positive for values of PG I ≤ 70 μg/L with a PG I/II ratio of ≤ 3[20,21]. These criteria offer a sensitivity of 70.5% and a specificity of 97% for the diagnosis of extensive CAG, using pathological diagnosis as the gold standard[20]. Subjects for whom both H.pylori infection and PG level could be determined were divided into the following four groups in terms of H.pylori-related chronic gastritis stage: Group A, H.pylori-negative/PG-negative; Group B, H.pylori-positive/PG-negative; Group C, H.pylori-positive/PG-positive; and Group D, H.pylori-negative/PG-positive[8].
RE was diagnosed by upper gastrointestinal endoscopy. According to the Los Angeles classification system[22], Grades A through D indicate erosive esophagitis. In the present study, only patients with erosive esophagitis were diagnosed with RE, and subjects with Grade M (minimal change)[23]or Grade N were not diagnosed with RE. Hiatal hernia was diagnosed endoscopically when the distance between the crural impression and the gastroesophageal junction was 2 cm or more.
Using the FSSG questionnaire, subjective symptoms of GERD were quantified, and total, acid reflux, and gastrointestinal dysmotility scores were calculated. GERD was defined as a total score ≥ 8, which is the recommended cut-off FSSG value for GERD[4]. Furthermore, NERD was defined as total score ≥ 8 without endoscopic erosive esophagitis.
All data analyses were performed using SPSS version 11.0 software (SPSS, Chicago, IL, USA). Pair-wise differences in the FSSG score were analyzed using the unpaired Student’s t-test, and overall differences in age and FSSG score were analyzed using the Kruskal-Wallis test. Pair-wise and overall differences in categorical variables were analyzed by Fisher’s exact test. All tests were 2-sided, and values of P < 0.05 were considered significant. Data are expressed as means ± standard deviation.
As mentioned above, of the 1165 subjects in whom H.pylori-Ab titers and serum PG levels were measured, those meeting the exclusion criteria were removed. Most of the remaining 825 subjects were men (98.4%) and drinkers (74.9%). Reflecting the high incidence of H.pylori infection among middle-aged and elderly individuals in Japan, the incidence of H.pylori infection was high (71.4%). With regard to RE, Grade D (the most severe LA grade) was not seen in any subjects, and Grades A and B (mild grades) accounted for 94.6% of cases.
The analysis was conducted between H.pylori-positive (n = 589) and H.pylori-negative (n = 236) subjects and between PG-positive (n = 296) and PG-negative (n = 529) subjects (Table 1). The prevalence of RE was significantly higher for PG- and H.pylori-negative subjects than for their positive counterparts (P < 0.001). The acid reflux score was significantly higher for PG-negative subjects than for PG-positive subjects (P < 0.05), but no significant difference existed between H.pylori-positive and -negative subjects. No significant differences in gastrointestinal dysmotility scores between H.pylori-positive and -negative subjects or between PG-positive and -negative subjects were present. The prevalence of GERD patients with total FSSG scores ≥ 8 tended to be high for PG-negative subjects (P = 0.076), but no significant difference existed between H.pylori-positive and -negative subjects. While no significant difference in the prevalence of NERD patients was evident between H.pylori-positive and -negative subjects or between PG-positive and -negative subjects, the prevalence of NERD among GERD patients was significantly higher for H.pylori-positive subjects (P = 0.027).
| H.pylori infection | P value | Serum PG test | P value | |||
| - | + | - | + | |||
| n | 236 | 589 | 529 | 296 | ||
| FSSG | ||||||
| -total score (mean ± SD) | 3.58 ± 4.00 | 3.17 ± 3.90 | 0.175 | 3.45 ± 3.96 | 2.99 ± 3.87 | 0.104 |
| -acid reflux score (mean ± SD) | 1.78 ± 2.21 | 1.62 ± 2.32 | 0.350 | 1.79 ± 2.33 | 1.45 ± 2.20 | 0.038 |
| -dysmotility score (mean ± SD) | 1.80 ± 2.32 | 1.55 ± 1.99 | 0.127 | 1.66 ± 2.14 | 1.54 ± 2.02 | 0.432 |
| Erosive esophagitis (LA grade A-D) | 28.4%(67/236) | 10.7%(63/589) | 0.000 | 21.2%(112/529) | 6.1%(18/296) | 0.000 |
| FSSG total score ≥ 8 (= GERD) | 13.6%(32/236) | 11.7%(69/589) | 0.465 | 13.8%(73/529) | 9.5%(28/296) | 0.076 |
| FSSG total score ≥ 8 and non-erosive esophagitis (= NERD) | 8.1%(19/236) | 9.5%(56/589) | 0.510 | 9.8%(52/529) | 7.8%(23/296) | 0.377 |
| NERD/GERD | 59.4%(19/32) | 81.2%(56/69) | 0.027 | 71.2%(52/73) | 82.1%(23/28) | 0.317 |
The stage of H.pylori-related chronic gastritis was assessed in the 825 subjects (Table 2). With regard to background factors, significant differences were seen in age. The prevalence of RE showed significant decreases with the stage of the chronic gastritis (from Group A to D) (P < 0.001). Acid reflux scores showed a significant decrease with the chronic gastritis stage (P < 0.05). The gastrointestinal dysmotility score showed no significant differences between stages (P = 0.800). The ratios of GERD patients with total FSSG scores ≥ 8 showed no significant differences related to the chronic gastritis stage. No significant differences existed in the prevalence of NERD patients among Groups A, B, and C. However, the prevalence of NERD among GERD patients for Groups A, B, and C tended to increase with the chronic gastritis stage (P = 0.081).
| Stages of H.pylori-related chronic gastritis | Group A | Group B | Group C | Group D | Overall P value |
| H.pylori infection | - | + | + | - | |
| Serum PG test (extensive CAG) | - | - | + | + | |
| n | 219 | 310 | 279 | 17 | |
| Age (years: mean ± SD) | 55.23 ± 4.23 | 55.84 ± 4.0 | 56.79 ± 3.91 | 53.94 ± 5.01 | 0.001 |
| Sex (male/female) | 214/5 | 308/2 | 273/6 | 17/0 | 0.306 |
| Smokers | 44.29% | 35.16% | 41.58% | 41.18% | 0.164 |
| Drinkers | 75.34% | 75.48% | 74.19% | 70.59% | 0.939 |
| Serum PG I(ng/mL mean ± SD) | 59.82 ± 26.52 | 81.76 ± 48.16 | 36.59 ± 18.42 | 21.98 ± 15.99 | - |
| Serum PG II(ng/mL mean ± SD) | 10.80 ± 5.81 | 25.89 ± 18.42 | 20.70 ± 8.60 | 12.89 ± 4.84 | - |
| PG I/II | 5.70 ± 1.13 | 3.74 ± 1.31 | 1.76 ± 0.69 | 1.53 ± 0.95 | - |
| H.pylori Ig G Ab titer (U/mL mean ± SD) | 13.54 ± 5.26 | 475.31 ± 632.73 | 441.07 ± 50.94 | 16.71 ± 6.44 | - |
| FSSG | |||||
| -total score (mean ± SD) | 3.69 ± 4.01 | 3.33 ± 3.87 | 3.00 ± 3.94 | 2.88 ± 2.55 | 0.183 |
| -acid reflux score (mean ± SD) | 1.83 ± 2.26 | 1.77 ± 2.39 | 1.46 ± 2.25 | 1.29 ± 1.26 | 0.038 |
| -dysmotility score (mean ± SD) | 1.81 ± 2.37 | 1.56 ± 1.96 | 1.54 ± 2.03 | 1.59 ± 1.77 | 0.800 |
| Erosive esophagitis (LA grade A-D) | 30.6%(67/219 | 14.5%(45/310) | 6.5%(18/279) | 0%(0/17) | 0.000 |
| LA grade A/B/C/D | 45/18/4/0 | 30/13/2/0 | 11/6/1/0 | 0/0/0/0 | - |
| Hiatal hernia | 3.2%(7/219) | 5.8%(18/310) | 7.2%(20/279) | 5.9%(1/17) | 0.231 |
| FSSG total score ≥ 8 (=GERD) | 14.6%(32/219) | 13.2%(41/310) | 9.7%(28/279) | 0%(0/17) | 0.177 |
| FSSG total score ≥ 8 and non-erosive esophagitis (=NERD) | 8.7%(19/219) | 10.6%(33/310) | 8.2%(23/279) | 0%(0/17) | 0.496 |
| NERD/GERD | 59.4%(19/32) | 80.5%(33/41) | 82.1%(23/28) | - | 0.081 |
Previously, we have investigated the risk of gastric cancer based on H.pylori-related chronic gastritis stage as assessed by a combination of H.pylori-Ab titer and serum PG level[8]. The present results suggest that the disease states of GERD and NERD can also be assessed by evaluating the risk for RE and upper gastrointestinal symptoms accompanying gastric acid reflux and gastrointestinal dysmotility. As reported previously[11], the prevalence of RE was low for subjects with CAG. The FSSG was used to closely examine upper gastrointestinal symptoms, and acid reflux scores were low for the group in the advanced stages of H.pylori-related chronic gastritis, but no marked difference in gastrointestinal dysmotility scores was seen in relation to the chronic gastritis stage. The prevalence of NERD patients among GERD patients was lowest for Group A and highest for Group C, clarifying the relationship between NERD and the stage of H.pylori-related chronic astritis.
Compared to Western countries, the number of GERD patients is lower in Japan, and the prevalence of NERD among GERD patients is higher[24]. Differences exist in the extent of CAG and in its associated reduction in gastric acid secretion that strongly correlate to H.pylori infection differences between Japan and Western countries[25], and the present study also showed that they most closely reflected the disease state of GERD in Japan. The prevalence of CagA+ H.pylori[26], which correlates pathologically to atrophic gastritis, is particularly high in Japan[27]. This is believed to contribute to differences in the relationship between GERD and H.pylori infection[28] in Japan and Western countries[29].
The present study also assessed the difference between H.pylori-positive and H.pylori-negative subjects and between PG-positive and PG-negative subjects. No significant differences existed in acid reflux and dysmotility scores between H.pylori-positive and H.pylori-negative subjects. Upper gastrointestinal symptom scores, particularly acid reflux scores, were significantly higher for PG-positive subjects than for PG-negative subjects. No significant differences existed in the prevalence of GERD patients with total FSSG scores ≥ 8 between H.pylori-positive and H.pylori-negative subjects, but the prevalence was greater for PG-negative subjects than for PG-positive subjects. GERD-related upper gastrointestinal symptoms are thus more closely influenced by extensive CAG than H.pylori infection. However, the finding that the incidence of endoscopy-diagnosed RE for H.pylori-negative subjects and PG-negative subjects was higher compared to their positive counterparts was very interesting. In other words, reduced acid secretion due to CAG has a great effect on the suppression of esophageal mucosal erosion, and, of the various subjective symptoms, acid reflux symptoms are suppressed because gastric acid secretion is markedly low. This might be the reason why the prevalence of NERD among GERD patients changes according to the H.pylori-related chronic gastritis groups.
The prevalence of NERD among subjects with total FSSG scores ≥ 8 was higher for H.pylori-positive subjects than for their negative counterparts. Groups A-D showed no marked differences in gastrointestinal dysmotility scores, and no marked differences were apparent between H.pylori-positive and H.pylori-negative subjects or between PG-positive and PG-negative subjects. These findings are extremely important when studying the disease state of GERD. In other words, in Groups C and D, where gastric mucosal atrophy is severely advanced, the symptoms and onset of NERD are influenced by gastrointestinal dysmotility rather than acid reflux, thus affecting therapy planning[6].
At present, the incidence of H.pylori infection is decreasing in Japan, and the number of patients with chronic atrophic gastritis or gastric cancer is expected to decrease in the future. However, the number of Group A subjects (H.pylori-negative and PG-negative) is likely to increase. Therefore, RE in Group A subjects who may experience both acid reflux and dysmotility symptoms must be managed. In Groups C and D, with a higher risk of gastric cancer[8,30], treatments are provided less frequently for RE, but because acid reflux symptoms are lacking, these subjects are less likely to visit a medical center on their own and undergo thorough testing, such as upper gastrointestinal endoscopy.
Instead of prospectively observing the onset rate of GERD over a long period of time, the present study analyzed GERD-related symptoms and the prevalence of endoscopic RE, based on the stage of H.pylori-related chronic gastritis at a single time point when endoscopy and history-taking were performed. A prospective study based on long-term follow-up observation is needed to more accurately assess GERD risks. However, acid reducers, including PPIs, are often prescribed to patients with upper abdominal symptoms, and various therapeutic modifications make such studies difficult to implement. The present study involved a group of workers, consisting of almost all males, who underwent endoscopy as part of regular checkup programs of gastric cancer screening. Thus, since most study subjects were men, this must be taken into account when interpreting the results. The present study clarified that H.pylori infection and CAG stage correlate closely with acid reflux and dysmotility symptoms. However, because GERD is a disease that is closely related to diet and lifestyle diseases such as obesity and diabetes[31-33], thorough investigation of the correlations of these factors to upper gastrointestinal symptoms is necessary using a GERD-specific questionnaire. Furthermore, ambulatory esophageal pH (with/without impedance) monitoring was not done in this study, and the term "NERD" might not be appropriate. NERD cases include functional heartburn cases in this study, and this should be taken into consideration when interpreting the data.
In conclusion, the present results suggest that the disease state of GERD was related to the stage of H.pylori-related chronic gastritis based on measurements of H.pylori-Ab titers and serum PG levels (Figure 1). These two serum markers can be measured conveniently, noninvasively, and relatively inexpensively. The reproducibility of test results is high, and many specimens can be measured at the same time. Like Japan, the prevalence of H.pylori infection is high and the development of CAG is closely involved with gastric cancer in East Asian countries, such as China and Korea and in Eastern Europe, and Middle and South America. Conducting serum tests along with routine endoscopic examination is useful not only for gastric cancer screening, but also to obtain more information about patients with reflux disease.
We have classified the progression of Helicobacter pylori (H.pylori)-related chronic gastritis into 4 groups (A-D) on the basis of two serum parameters, H.pylori antibody (H.pylori-Ab) titer and serum pepsinogen (PG) level, as a screening test for extensive chronic atrophic gastritis (CAG), and reported a stepwise increase in the incidence of gastric cancer. In this study, the association of H.pylori-related chronic gastritis progression with upper gastrointestinal symptoms and gastroesophageal reflux disease (GERD) was evaluated, because there are only a few previous studies in which this association has been examined.
This study can help us to understand the natural history of GERD, as well as other illnesses including gastric cancer.
Conducting serum tests along with routine endoscopic examination is useful for not only gastric cancer screening, but also to obtain more information about patients with GERD.
A prospective study based on long-term follow-up observation is needed to more accurately assess GERD risks.
H.pylori-related chronic gastritis stage: The groups were determined by the results of the 2 serologic tests (H.pylori-Ab and PG). This classification reflects each stage of the serial changes in stomach mucosa induced by chronic H.pylori infection. The H.pylori-free healthy condition corresponds to 2 negative tests (Group A). With the establishment of H.pylori infection, the antibody test becomes positive (Group B). As the infection spreads, the PG test also turns positive (Group C). Group C has extensive CAG. Intestinal metaplasia develops and spreads in the presence of CAG, leading to reduction of the bacterial load in the stomach. This results in a negative specific antibody test (Group D). Thus, Group D comprises those subjects with metaplastic gastritis.
This article provides interesting data about H.pylori-Ab and serum PG levels in subjects with GERD. These data are of epidemiological interest and provide some insight into theoretical aspects.
Peer reviewers: Young-Tae Bak, MD, PhD, Professor, Division of Gastroenterology, Department of Internal Medicine, Korea University, Guro Hospital, 97 Gurodong-gil, Guro-gu, Seoul 152-703, South Korea; Oscar Tatsuya Teramoto-Matsubara, MedCenter, Av. Paseo de las Palmas 745-102, Lomas de Chapultepec, Mexico D.F. 11000, Mexico; Peter Born, MD, Professor, D-80634 second Department of Medicine, Red Cross Hospital, Munich, Germany
S- Editor Zhang HN L- Editor Hughes D E- Editor Zhang L
| 1. | Vakil N, van Zanten SV, Kahrilas P, Dent J, Jones R. The Montreal definition and classification of gastroesophageal reflux disease: a global evidence-based consensus. Am J Gastroenterol. 2006;101:1900-1920; quiz 1943. |
| 2. | Fass R. Symptom assessment tools for gastroesophageal reflux disease (GERD) treatment. J Clin Gastroenterol. 2007;41:437-444. |
| 3. | Carlsson R, Dent J, Bolling-Sternevald E, Johnsson F, Junghard O, Lauritsen K, Riley S, Lundell L. The usefulness of a structured questionnaire in the assessment of symptomatic gastroesophageal reflux disease. Scand J Gastroenterol. 1998;33:1023-1029. |
| 4. | Kusano M, Shimoyama Y, Sugimoto S, Kawamura O, Maeda M, Minashi K, Kuribayashi S, Higuchi T, Zai H, Ino K. Development and evaluation of FSSG: frequency scale for the symptoms of GERD. J Gastroenterol. 2004;39:888-891. |
| 5. | Kusano M, Shimoyama Y, Kawamura O, Maeda M, Kuribayashi S, Nagoshi A, Zai H, Moki F, Horikoshi T, Toki M. Proton pump inhibitors improve acid-related dyspepsia in gastroesophageal reflux disease patients. Dig Dis Sci. 2007;52:1673-1677. |
| 6. | Miyamoto M, Haruma K, Takeuchi K, Kuwabara M. Frequency scale for symptoms of gastroesophageal reflux disease predicts the need for addition of prokinetics to proton pump inhibitor therapy. J Gastroenterol Hepatol. 2008;23:746-751. |
| 7. | Miki K, Ichinose M, Shimizu A, Huang SC, Oka H, Furihata C, Matsushima T, Takahashi K. Serum pepsinogens as a screening test of extensive chronic gastritis. Gastroenterol Jpn. 1987;22:133-141. |
| 8. | Ohata H, Kitauchi S, Yoshimura N, Mugitani K, Iwane M, Nakamura H, Yoshikawa A, Yanaoka K, Arii K, Tamai H. Progression of chronic atrophic gastritis associated with Helicobacter pylori infection increases risk of gastric cancer. Int J Cancer. 2004;109:138-143. |
| 9. | Mukoubayashi C, Yanaoka K, Ohata H, Arii K, Tamai H, Oka M, Ichinose M. Serum pepsinogen and gastric cancer screening. Intern Med. 2007;46:261-266. |
| 10. | Enomoto S, Maekita T, Ohata H, Yanaoka K, Oka M, Ichinose M. Novel risk markers for gastric cancer screening: Present status and future prospects. World J Gastrointest Endosc. 2010;2:381-387. |
| 11. | Yamaji Y, Mitsushima T, Ikuma H, Okamoto M, Yoshida H, Kawabe T, Shiratori Y, Saito K, Yokouchi K, Omata M. Inverse background of Helicobacter pylori antibody and pepsinogen in reflux oesophagitis compared with gastric cancer: analysis of 5732 Japanese subjects. Gut. 2001;49:335-340. |
| 12. | Shirota T, Kusano M, Kawamura O, Horikoshi T, Mori M, Sekiguchi T. Helicobacter pylori infection correlates with severity of reflux esophagitis: with manometry findings. J Gastroenterol. 1999;34:553-559. |
| 13. | Haruma K, Hamada H, Mihara M, Kamada T, Yoshihara M, Sumii K, Kajiyama G, Kawanishi M. Negative association between Helicobacter pylori infection and reflux esophagitis in older patients: case-control study in Japan. Helicobacter. 2000;5:24-29. |
| 14. | Koike T, Ohara S, Sekine H, Iijima K, Abe Y, Kato K, Toyota T, Shimosegawa T. Helicobacter pylori infection prevents erosive reflux oesophagitis by decreasing gastric acid secretion. Gut. 2001;49:330-334. |
| 15. | Fujiwara Y, Higuchi K, Shiba M, Yamamori K, Watanabe Y, Sasaki E, Tominaga K, Watanabe T, Oshitani N, Arakawa T. Differences in clinical characteristics between patients with endoscopy-negative reflux disease and erosive esophagitis in Japan. Am J Gastroenterol. 2005;100:754-815. |
| 16. | Corley DA, Kubo A, Levin TR, Block G, Habel L, Rumore G, Quesenberry C, Buffler P, Parsonnet J. Helicobacter pylori and gastroesophageal reflux disease: a case-control study. Helicobacter. 2008;13:352-360. |
| 17. | Grande M, Cadeddu F, Villa M, Attina GM, Muzi MG, Nigro C, Rulli F, Farinon AM. Helicobacter pylori and gastroesophageal reflux disease. World J Surg Oncol. 2008;6:74. |
| 18. | Chen TS, Chang FY, Lee SD. Serodiagnosis of Helicobacter pylori infection: comparison and correlation between enzyme-linked immunosorbent assay and rapid serological test results. J Clin Microbiol. 1997;35:184-186. |
| 19. | Ichinose M, Miki K, Furihata C, Kageyama T, Hayashi R, Niwa H, Oka H, Matsushima T, Takahashi K. Radioimmunoassay of serum group I and group II pepsinogens in normal controls and patients with various disorders. Clin Chim Acta. 1982;126:183-191. |
| 20. | Watanabe Y, Kurata JH, Mizuno S, Mukai M, Inokuchi H, Miki K, Ozasa K, Kawai K. Helicobacter pylori infection and gastric cancer. A nested case-control study in a rural area of Japan. Dig Dis Sci. 1997;42:1383-1387. |
| 21. | Ichinose M, Yahagi N, Oka M, Ikeda H, Miki K, Omata M. Screening for gastric cancer in Japan. Cancer screening for common malignancies. Totowa, New Jersey: Humana Press 2001; 87-102. |
| 22. | Armstrong D, Bennett JR, Blum AL, Dent J, De Dombal FT, Galmiche JP, Lundell L, Margulies M, Richter JE, Spechler SJ. The endoscopic assessment of esophagitis: a progress report on observer agreement. Gastroenterology. 1996;111:85-92. |
| 23. | Kusano M, Ino K, Yamada T, Kawamura O, Toki M, Ohwada T, Kikuchi K, Shirota T, Kimura M, Miyazaki M. Interobserver and intraobserver variation in endoscopic assessment of GERD using the “Los Angeles” classification. Gastrointest Endosc. 1999;49:700-704. |
| 24. | Miwa H, Minoo T, Hojo M, Yaginuma R, Nagahara A, Kawabe M, Ohkawa A, Asaoka D, Kurosawa A, Ohkusa T. Oesophageal hypersensitivity in Japanese patients with non-erosive gastro-oesophageal reflux diseases. Aliment Pharmacol Ther. 2004;20 Suppl 1:112-117. |
| 25. | Asaka M, Kato M, Kudo M, Katagiri M, Nishikawa K, Koshiyama H, Takeda H, Yoshida J, Graham DY. Atrophic changes of gastric mucosa are caused by Helicobacter pylori infection rather than aging: studies in asymptomatic Japanese adults. Helicobacter. 1996;1:52-56. |
| 26. | Kuipers EJ, Perez-Perez GI, Meuwissen SG, Blaser MJ. Helicobacter pylori and atrophic gastritis: importance of the cagA status. J Natl Cancer Inst. 1995;87:1777-1780. |
| 27. | Ogura K, Kanai F, Maeda S, Yoshida H, Ogura M, Lan KH, Hirota K, Kawabe T, Shiratori Y, Omata M. High prevalence of cytotoxin positive Helicobacter pylori in patients unrelated to the presence of peptic ulcers in Japan. Gut. 1997;41:463-468. |
| 28. | Raghunath A, Hungin AP, Wooff D, Childs S. Prevalence of Helicobacter pylori in patients with gastro-oesophageal reflux disease: systematic review. BMJ. 2003;326:73728. |
| 29. | Somi MH, Fattahi E, Fouladi RF, Karimi M, Bonyadi R, Baballou Z. An inverse relation between CagA+ strains of Heli-cobacter pylori infection and risk of erosive GERD. Saudi Med J. 2008;29:393-396. |
| 30. | Watabe H, Mitsushima T, Yamaji Y, Okamoto M, Wada R, Kokubo T, Doi H, Yoshida H, Kawabe T, Omata M. Predicting the development of gastric cancer from combining Helicobacter pylori antibodies and serum pepsinogen status: a prospective endoscopic cohort study. Gut. 2005;54:764-768. |
| 31. | Mishima I, Adachi K, Arima N, Amano K, Takashima T, Moritani M, Furuta K, Kinoshita Y. Prevalence of endoscopically negative and positive gastroesophageal reflux disease in the Japanese. Scand J Gastroenterol. 2005;40:1005-1009. |
| 32. | Hampel H, Abraham NS, El-Serag HB. Meta-analysis: obesity and the risk for gastroesophageal reflux disease and its complications. Ann Intern Med. 2005;143:199-211. |
| 33. | Kinekawa F, Kubo F, Matsuda K, Fujita Y, Tomita T, Uchida Y, Nishioka M. Relationship between esophageal dysfunction and neuropathy in diabetic patients. Am J Gastroenterol. 2001;96:2026-2032. |