Published online Nov 16, 2011. doi: 10.4253/wjge.v3.i11.228
Revised: December 14, 2010
Accepted: April 25, 2011
Published online: November 16, 2011
The authors report the case of a primary small bowel lymphoma discovered incidentally in a 33-year-old male following ileal intubation at colonoscopy. The patient subsequently underwent curative treatment with chemotherapy. This case not only highlights the importance of routine ileoscopy but also the successful use of chemotherapy in a disease for which the optimal treatment modality has not been well characterized.
- Citation: Donnellan F, Moran S, Patchett SE. An incidentaloma at ileal intubation. World J Gastrointest Endosc 2011; 3(11): 228-230
- URL: https://www.wjgnet.com/1948-5190/full/v3/i11/228.htm
- DOI: https://dx.doi.org/10.4253/wjge.v3.i11.228
Primary small bowel lymphoma is uncommon. It usually presents as a surgical emergency, including obstruction or perforation. While surgery is the mainstay of management, other treatment modalities have been used successfully. We report a case of lymphoma involving the terminal ileum discovered at routine ileal intubation and successfully treated with chemotherapy.
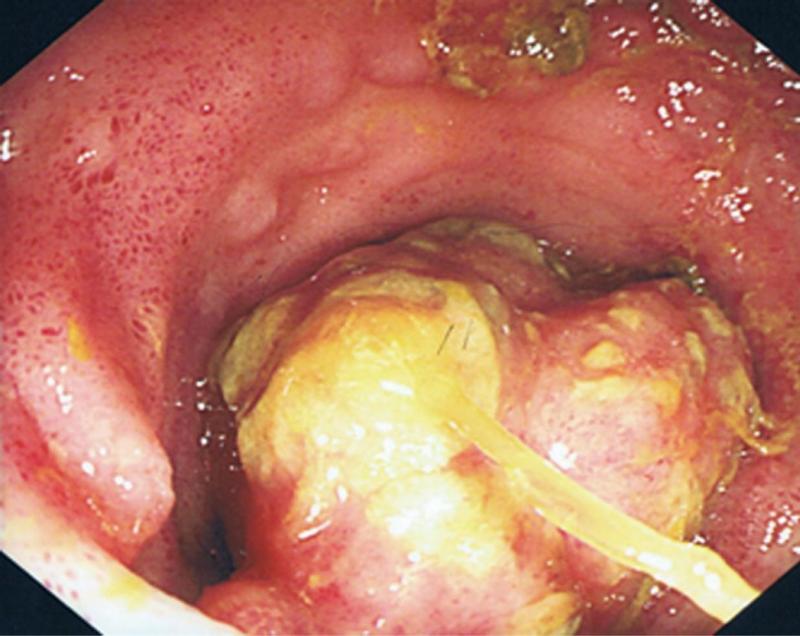
A 33-year-old male with an unremarkable medical history presented to the outpatient department with a 3 mo history of left iliac fosse discomfort and intermittent rectal bleeding. The patient denied nausea, vomiting or a change in bowel habit. The patient underwent colonoscopy which demonstrated unremarkable colonic mucosa. However, intubation of the terminal ileum revealed a 4 cm non-obstructing mass lesion just proximal to the ileocecal valve (Figure 1).
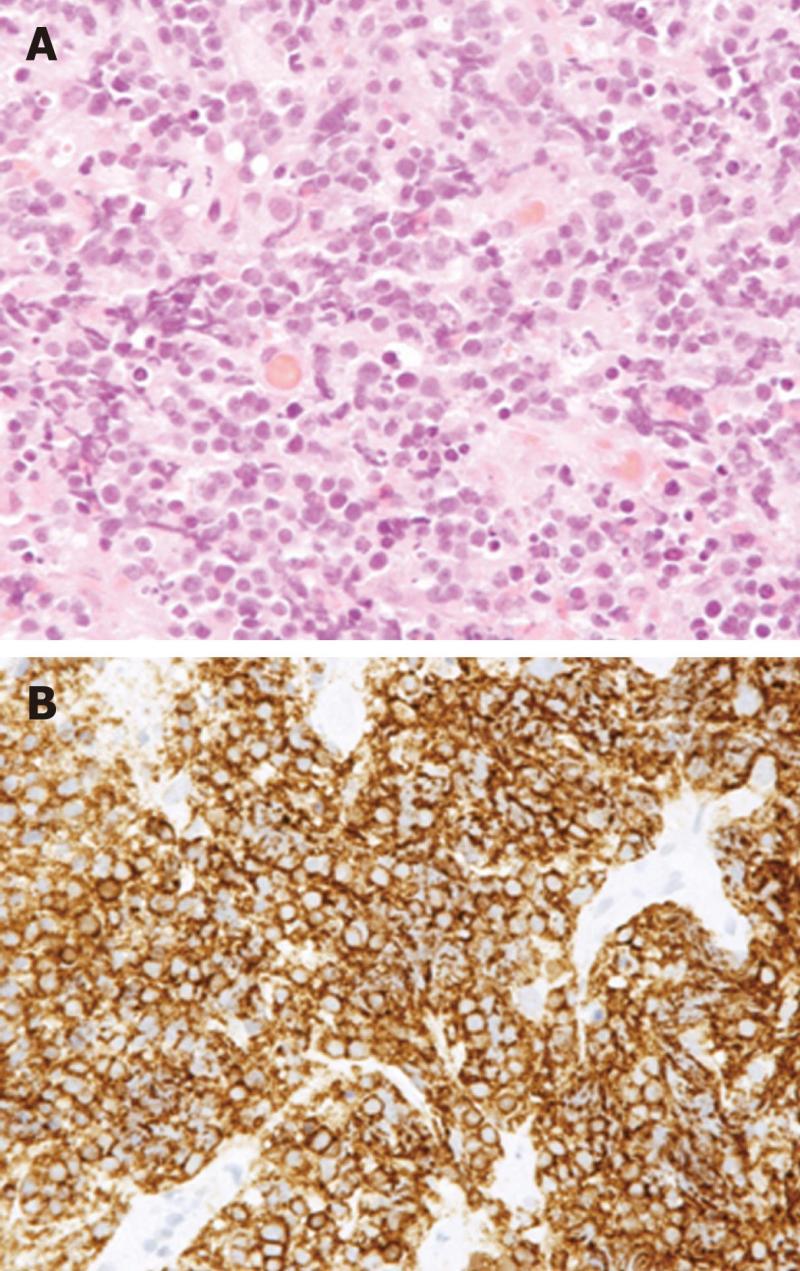
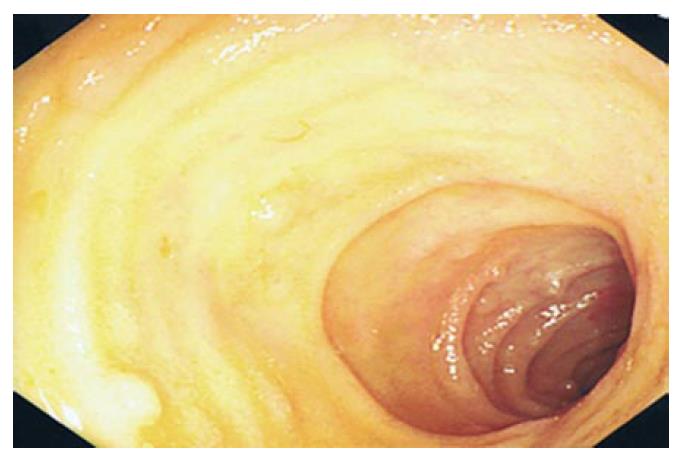
The histology from the ileal mass, with immunohistochemical staining positive for the markers L26, Bcl-6 and CD10, revealed a large diffuse B-cell non-Hodgkin’s lymphoma (Figure 2). The patient was diagnosed with a primary gastrointestinal lymphoma confined to the terminal ileum following positron emission tomography computed tomography (PET CT) scanning and a bone marrow examination. The lactate dehydrogenase level was elevated at 805 IU/L (110-300). The patient underwent chemotherapy with a 6-cycle regimen of Cyclophosphamide 750 mg/m2 intravenously (IV) day 1, Adriamycin 50 mg/m2 IV day 1, Vincristine 1.4 mg/m2 IV day 1, Prednisolone 50 mg twice daily orally days 1-5 (CHOP) and Rituximab 375 mg/m2 IV day 1. Colonoscopy performed 3 mo post-treatment demonstrated a normal terminal ileum (Figure 3). Subsequent biopsies from the terminal ileum were also unremarkable. A PET CT scan was also normal. On the basis of the endoscopic and radiological responses, the patient was not considered for radiotherapy.
The gastrointestinal tract, accounting for up to 40% of all extranodal disease, is the most commonly involved site for primary extranodal non-Hodgkin’s lymphoma. The most frequent primary sites are the stomach and small intestine, accounting for 60% and 20% respectively[1]. While the lymphoma in our patient was discovered as an incidental finding following routine ileal intubation, small intestinal lymphoma typically presents with abdominal pain, weight loss or acute surgical conditions such as obstruction and perforation[2,3].
In contrast to gastric lymphoma, the optimal treatment modality for primary small bowel lymphoma has not been well characterized. Surgery alone[4,5], or in combination with chemotherapy[6,7], is considered the mainstay of treatment for localized disease. However, some reports have demonstrated benefit from sole treatment with either chemo- or radiotherapy in localized disease[8,9].
Ileal intubation as part of the colonoscopic examination is a topic of great debate. It has been demonstrated that performing routine ileal intubation, when not indicated, is of little diagnostic value[10,11]. However, mastering this technique is an important part of colonoscopic training. Furthermore, visualization of ileal mucosa is the most definitive landmark that the colonoscopy has been successfully completed.
This case highlights the benefit of performing routine ileal intubation, which is a topic of great debate, and curative treatment of primary localized small bowel lymphoma with chemotherapy.
Peer reviewers: Carlo Maria Girelli, MD, 1st Division of Internal Medicine, Service of Gastroenterology and Digestive Endoscopy, Hospital of Busto Arsizio, Via A. da Brescia, 1 21052 Busto Arsizio (VA), Italy; Nobumi Tagaya, Associate Professor, Second Department of Surgery, Dokkyo Medical University, 880 Kitakobayashi, Mibu, Tochigi 321-0293, Japan
S- Editor Zhang SJ L- Editor Roemmele A E- Editor Zheng XM
| 1. | Rohatiner A, d'Amore F, Coiffier B, Crowther D, Gospodarowicz M, Isaacson P, Lister TA, Norton A, Salem P, Shipp M. Report on a workshop convened to discuss the pathological and staging classifications of gastrointestinal tract lymphoma. Ann Oncol. 1994;5:397-400. [PubMed] |
| 2. | Li B, Shi YK, He XH, Zou SM, Zhou SY, Dong M, Yang JL, Liu P, Xue LY. Primary non-Hodgkin lymphomas in the small and large intestine: clinicopathological characteristics and management of 40 patients. Int J Hematol. 2008;87:375-381. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 57] [Cited by in RCA: 68] [Article Influence: 4.3] [Reference Citation Analysis (0)] |
| 3. | Koch P, del Valle F, Berdel WE, Willich NA, Reers B, Hiddemann W, Grothaus-Pinke B, Reinartz G, Brockmann J, Temmesfeld A. Primary gastrointestinal non-Hodgkin's lymphoma: I. Anatomic and histologic distribution, clinical features, and survival data of 371 patients registered in the German Multicenter Study GIT NHL 01/92. J Clin Oncol. 2001;19:3861-3873. [PubMed] |
| 4. | Amer MH, el-Akkad S. Gastrointestinal lymphoma in adults: clinical features and management of 300 cases. Gastroenterology. 1994;106:846-858. [PubMed] |
| 5. | Yin L, Chen CQ, Peng CH, Chen GM, Zhou HJ, Han BS, Li HW. Primary small-bowel non-Hodgkin's lymphoma: a study of clinical features, pathology, management and prognosis. J Int Med Res. 2007;35:406-415. [PubMed] |
| 6. | Zinzani PL, Magagnoli M, Pagliani G, Bendandi M, Gherlinzoni F, Merla E, Salvucci M, Tura S. Primary intestinal lymphoma: clinical and therapeutic features of 32 patients. Haematologica. 1997;82:305-308. [PubMed] |
| 7. | Daum S, Ullrich R, Heise W, Dederke B, Foss HD, Stein H, Thiel E, Zeitz M, Riecken EO. Intestinal non-Hodgkin's lymphoma: a multicenter prospective clinical study from the German Study Group on Intestinal non-Hodgkin's Lymphoma. J Clin Oncol. 2003;21:2740-2746. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 186] [Cited by in RCA: 162] [Article Influence: 7.4] [Reference Citation Analysis (0)] |
| 8. | Ibrahim EM, Ezzat AA, El-Weshi AN, Martin JM, Khafaga YM, Al Rabih W, Ajarim DS, Al-Foudeh MO, Zucca E. Primary intestinal diffuse large B-cell non-Hodgkin's lymphoma: clinical features, management, and prognosis of 66 patients. Ann Oncol. 2001;12:53-58. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 62] [Reference Citation Analysis (1)] |
| 9. | Radman I, Kovacević-Metelko J, Aurer I, Nemet D, Zupancić-Salek S, Bogdanić V, Sertić D, Mrsić M, Pulanić R, Gasparović V. Surgical resection in the treatment of primary gastrointestinal non-Hodgkin's lymphoma: retrospective study. Croat Med J. 2002;43:555-560. [PubMed] |
| 10. | Jeong SH, Lee KJ, Kim YB, Kwon HC, Sin SJ, Chung JY. Diagnostic value of terminal ileum intubation during colonoscopy. J Gastroenterol Hepatol. 2008;23:51-55. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 46] [Cited by in RCA: 56] [Article Influence: 3.3] [Reference Citation Analysis (0)] |
| 11. | Kennedy G, Larson D, Wolff B, Winter D, Petersen B, Larson M. Routine ileal intubation during screening colonoscopy: a useful maneuver? Surg Endosc. 2008;22:2606-2608. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 21] [Cited by in RCA: 15] [Article Influence: 0.9] [Reference Citation Analysis (0)] |