Published online Sep 16, 2019. doi: 10.4253/wjge.v11.i9.486
Peer-review started: June 4, 2019
First decision: August 2, 2019
Revised: August 9, 2019
Accepted: August 27, 2019
Article in press: August 27, 2019
Published online: September 16, 2019
Processing time: 103 Days and 1.7 Hours
Hydrogen peroxide is one of the most common household disinfectants worldwide. Hydrogen peroxide has been documented as a rare cause of chemical colitis.
We present a case of 31 years old lady who presented to our hospital with rectal bleeding and abdominal pain after using hydrogen peroxide vaginal douche as an enema. She underwent colonoscopy which showed findings suggestive of chemical colitis and was managed conservatively. Hydrogen peroxide can induce chemical injury in the colon. Clinical presentation and endoscopic findings of chemical colitis are nonspecific. History taking is an important tool in identifying the underlying etiology. Review of literature showed few case reports, mostly were managed with oral antibiotics and conservative approach.
Chemical colitis is usually managed conservatively. Complications including perforation, stricture and peritonitis may happen and need aggressive treatment accordingly.
Core tip: Chemical colitis is a rare entity. Depending on the extent of injury, it may lead to serious complications like perforation, stricture and peritonitis. We here present a case of chemical colitis caused by use of hydrogen peroxide vaginal douche as an enema. Patient’s clinical condition improved with supportive care.
- Citation: Baiomi A, Patel H, Abbas H, Vootla V, Makker J. Chemical colitis caused by hydrogen peroxide vaginal douche: A case report. World J Gastrointest Endosc 2019; 11(9): 486-490
- URL: https://www.wjgnet.com/1948-5190/full/v11/i9/486.htm
- DOI: https://dx.doi.org/10.4253/wjge.v11.i9.486
Chemical colitis is an inflammation of the large intestine or colon, caused by exposure to chemicals which could be as a result of accidental contamination of endoscopes during the cleaning process or by use of enemas with accidental or intentional exposure to various chemicals. Glutaraldehyde, hydrogen peroxide (H2O2) and enemas for routine bowel cleansing or constipation relief or sexual practice are the most common causes of chemical colitis[1,2].
Here we present a rare case of diagnosed with chemical colitis due to hydrogen peroxide used as an enema.
A 31-year-old lady presented to our emergency room with rectal bleeding.
She was recently diagnosed with bacterial vaginosis for which she was treated with Hydrogen Peroxide vaginal douche. She has chronic constipation. She reported having no bowel movement during the past 3 days and she used her hydrogen peroxide vaginal douche as an enema to help her have a bowel movement. She presented with 2 episodes of rectal bleeding associated with left lower quadrant abdominal pain for 1 d.
She had a history of chronic constipation.
She denied smoking cigarettes, alcohol or illicit drug use. No history of previous surgeries. Family history was negative for any gastrointestinal cancers.
On presentation her vitals were stable with temperature 98.6 degrees F, pulse 80 beats per minute, respiratory rate 18/min and blood pressure 15.2/9.9 kPa. On general physical examination she appeared comfortable and not in acute distress. Abdominal examination was unremarkable.
Laboratory studies are shown in Table 1.
| Laboratory test | Results (Normal range) | ||
| Day-1 | Day-2 | Day-3 | |
| Hemoglobin | 12.8 g/dL (12-16 g/dl) | 10.9 g/dL (12-16 g/dL) | 10.4 g/dL (12-16g/dL) |
| Hematocrit | 38.9% (42%-51%) | 33.0% (42%-51%) | 31.2 % (42%-51%) |
| Leucocyte count | 19.7 k/μL (4.8-10.8 k/μL) | 14.2 k/μL (4.8-10.8 k/μL) | 10.9 k/μL (4.8-10.8 k/μL) |
| Platelet count | 449000/μL (150000-400000/μL) | 373000/μL (150000-400000/μL) | 330000/μL (150000-400000/μL) |
| Blood urea nitrogen | 9 mg/dL (8-26 mg/dL) | 8 mg/dL (8-26 mg/dL) | 5 mg/dL (8-26 mg/dL) |
| Serum creatinine | 0.8 mg/dL (0.5-1.5 mg/dL) | 0.8 mg/dL (0.5-1.5 mg/dL) | 0.7 mg/dL (0.5-1.5 mg/dL) |
| Serum albumin | 4.5 g/dL (3.2-4.6 g/dL) | ||
| Serum total bilirubin | 0.9 mg/dL (0.2-1.1 mg/dL) | ||
| Alkaline phosphatase | 88 unit/L (43-160 unit/L) | ||
| Serum alanine aminotransferase | 11 unit/L (5-40 unit/L) | ||
| Serum aspartate transaminase | 16 unit/L (9-36 unit/L) | ||
| Serum lipase | 17 unit/L (< 61 unit/L) | ||
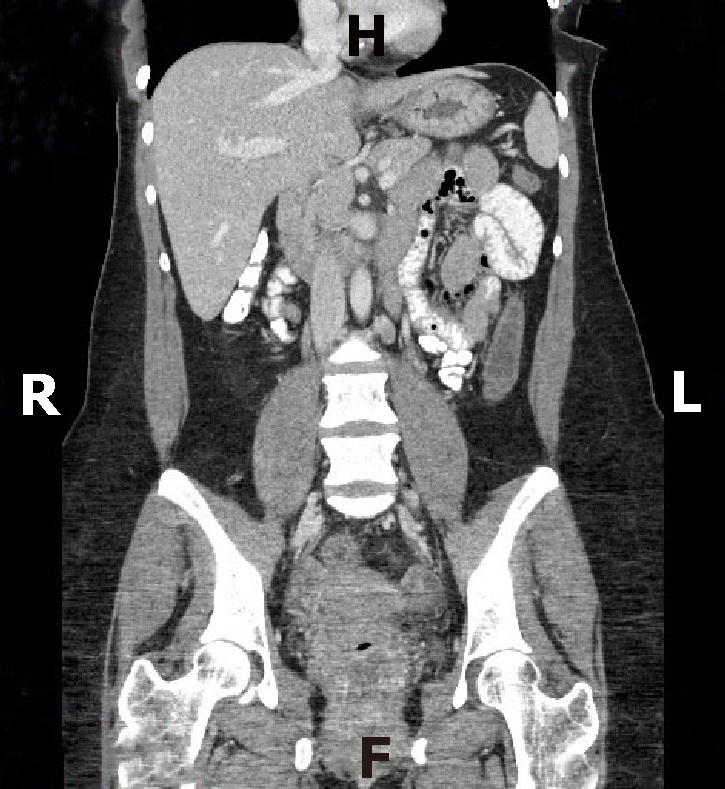
Computed tomography (CT) of the abdomen with oral and intravenous contrast (Figure 1) was done which showed diffuse bowel wall thickening involving the distal transverse colon, descending colon, sigmoid colon and rectum consistent with colitis. No bowel obstruction was noted.
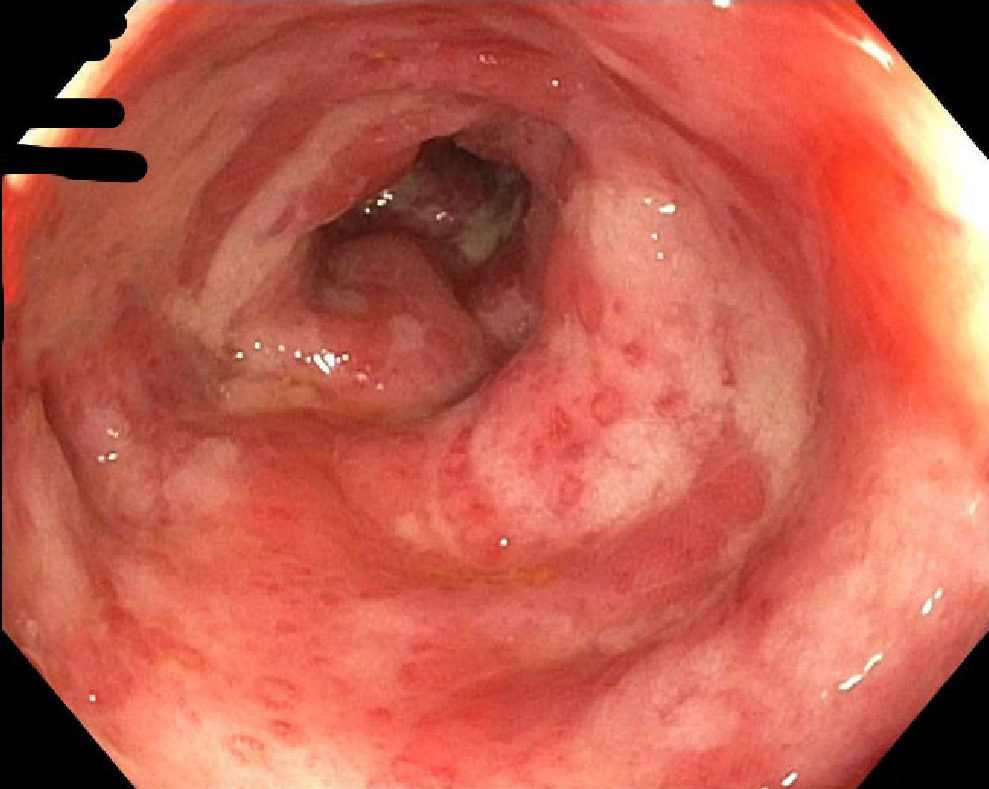
Patient had colonoscopy which showed severe inflammation characterized by congestion (edema), erythema, friability, loss of vascularity and confluent ulcerations found in a continuous and circumferential pattern from the rectum to the sigmoid colon until 30 cm from anal verge (Figure 2). The descending colon was spared. Biopsies were taken with a cold forcep for histology and it showed colonic mucosa with mucosal erosion, extravasated red blood cells with hyalinization of lamina propria with mild glandular atrophic changes which was mostly related to chemical injury.
The final diagnosis of the presented case is chemical colitis secondary to hydrogen peroxide.
Patient received intravenous hydration with normal saline and intravenous antibiotics including Ceftriaxone and Metronidazole.
Patient was discharged home on oral antibiotics and was seen for a follow up as outpatient where she reported resolution of her symptoms.
Chemical colitis occurs as a result of potentially caustic chemicals coming in contact with colonic mucosa. The most common causes of chemical colitis are - glutaraldehyde, alcohol, radiocontrast agents, formalin, ergotamine, sulfuric acid, acetic acid, ammonia soap, sodium hydroxide, hydrogen peroxide, herbal medicines, and potassium permanganate[3].
Hydrogen peroxide is one of the most common household disinfectants in the world. It is used to disinfect wounds and there are hundreds of remedies utilizing hydrogen peroxide including its use to bleach hair, antiseptic mouth rinse, whiten nails, remove stain from teeth, clear up acne[4], and relieve ear infections and vaginal douche to treat bacterial vaginosis[5].
Depending on the degree of inflammation, the presentation of chemical colitis may vary from asymptomatic patient to abdominal pain, bloating, nausea, vomiting, watery or bloody diarrhea, fever or severe sepsis with peritonitis, bowel stricture, perforation and rectovaginal fistula formation. Physical examination usually is unremarkable for mild cases. In severe cases with extensive inflammation and perforation, physical examination may reveal signs of peritonitis with acute abdomen[6-9].
Diagnostic tests usually include contrast enhanced abdominal CT which may show thickening of the colonic wall with pericolonic inflammation. It may also show stricture and fistula formation depending on the extent of injury and timing of presentation. Colonoscopy or flexible sigmoidoscopy with biopsy should be performed in all hemodynamically stable patients to assess the extent of injury. Colonoscopy may show evidence of colitis with inflammation, ulceration, granulation tissue, edema and exudates. Histological features of chemical colitis range from non-specific colitis with erosions, ulceration, extravasated red blood cells to glandular atrophy with hyalinization of lamina propria and evidence of ischemic colitis[2,3,5].
Since the clinical presentation, imaging, endoscopic and histological findings are nonspecific, the diagnosis of chemical colitis can be challenging, and it depends on detailed history taking. The management of chemical colitis is usually conservative with discontinuation of the offending agent, fluid replacement and a short course of antibiotics. Use of steroids locally or in systemic form has also been described. Some researchers advise using short term mesalamine for about 2 wk. Depending on the depth and extent of injury, patients may develop gastrointestinal bleeding, perforation, colonic rupture[10] and rarely require colectomy for ischemic colitis and/or peritonitis[7]. A recent review of literature by Pawar et al[11] reported 21 cases of hydrogen peroxide induced colitis. Most cases in that series presented with abdominal pain and bleeding per rectum, and most of the cases were diagnosed using CT scan and /or sigmoidoscopy with biopsy. Majority were managed conservatively and recovery period ranged from 3 d to 8 mo[11].
Chemical colitis can result from various chemical injuries to the colon, including hydrogen peroxide which is available over the counter as a wound disinfectant and a vaginal douche. In this case hydrogen peroxide was used as an enema to relieve constipation which resulted in chemical colitis. Bowel rest, discontinuation of exposure to the toxic agent, and broad-spectrum antibiotics resulted in complete resolution of the symptoms.
Manuscript source: Unsolicited manuscript
Specialty type: Gastroenterology and hepatology
Country of origin: United States
Peer-review report classification
Grade A (Excellent): 0
Grade B (Very good): 0
Grade C (Good): C
Grade D (Fair): 0
Grade E (Poor): 0
P-Reviewer: Sitkin S S-Editor: Wang JL L-Editor: A E-Editor: Zhou BX
| 1. | Meyer CT, Brand M, DeLuca VA, Spiro HM. Hydrogen peroxide colitis: a report of three patients. J Clin Gastroenterol. 1981;3:31-35. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 34] [Cited by in RCA: 36] [Article Influence: 0.8] [Reference Citation Analysis (0)] |
| 2. | Sheibani S, Gerson LB. Chemical colitis. J Clin Gastroenterol. 2008;42:115-121. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 45] [Cited by in RCA: 46] [Article Influence: 2.7] [Reference Citation Analysis (0)] |
| 3. | Kurdaş OO, Sezikli M, Cetinkaya ZA, Güzelbulut F, Yaşar B, Coşgun S, Değirmenci AS. Glutaraldehyde-induced colitis: three case reports. Indian J Gastroenterol. 2009;28:221-223. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 7] [Cited by in RCA: 8] [Article Influence: 0.5] [Reference Citation Analysis (0)] |
| 4. | Ríos-Castillo AG, González-Rivas F, Rodríguez-Jerez JJ. Bactericidal Efficacy of Hydrogen Peroxide-Based Disinfectants Against Gram-Positive and Gram-Negative Bacteria on Stainless Steel Surfaces. J Food Sci. 2017;82:2351-2356. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 40] [Cited by in RCA: 46] [Article Influence: 5.8] [Reference Citation Analysis (0)] |
| 5. | Chaithongwongwatthana S, Limpongsanurak S, Sitthi-Amorn C. Single hydrogen peroxide vaginal douching versus single-dose oral metronidazole for the treatment of bacterial vaginosis: a randomized controlled trial. J Med Assoc Thai. 2003;86 Suppl 2:S379-S384. [PubMed] |
| 6. | Brynjolfsson G. Colonic injury from hydrogen peroxide. N Engl J Med. 1967;277:662. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 2] [Cited by in RCA: 2] [Article Influence: 0.0] [Reference Citation Analysis (0)] |
| 7. | Cammarota G, Cesaro P, Cazzato A, Fedeli P, Riccioni ME, Sparano L, Vitale G, Costamagna G, Gasbarrini G, Larocca LM. Hydrogen peroxide-related colitis (previously known as "pseudolipomatosis"): a series of cases occurring in an epidemic pattern. Endoscopy. 2007;39:916-919. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 12] [Cited by in RCA: 12] [Article Influence: 0.7] [Reference Citation Analysis (0)] |
| 8. | Schwartz E, Dabezies MA, Krevsky B. Hydrogen peroxide injury to the colon. Dig Dis Sci. 1995;40:1290-1291. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 3] [Cited by in RCA: 3] [Article Influence: 0.1] [Reference Citation Analysis (0)] |
| 9. | Sheehan JF, Brynjolfsson G. Ulcerative colitis following hydrogen peroxide enema: case report and experimental production with transient emphysema of colonic wall and gas embolism. Lab Invest. 1960;9:150-168. [PubMed] |
| 10. | Offenbacher J, Kristol D, Cain D, Kim P, Nguyen V. An Emergency Department Presentation of Severe Colitis After a Home Hydrogen Peroxide Enema. J Emerg Med. 2019;. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 2] [Cited by in RCA: 2] [Article Influence: 0.3] [Reference Citation Analysis (0)] |
| 11. | Pawar D, Calara A, Jacob R, Beck N, Peiris AN. Hydrogen Peroxide Induced Colitis: A Case Report and Literature Review. Case Rep Gastrointest Med. 2017;2017:6432063. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 4] [Cited by in RCA: 4] [Article Influence: 0.5] [Reference Citation Analysis (1)] |