Published online May 27, 2020. doi: 10.4254/wjh.v12.i5.239
Peer-review started: December 9, 2019
First decision: January 6, 2020
Revised: March 26, 2020
Accepted: April 23, 2020
Article in press: April 23, 2020
Published online: May 27, 2020
Processing time: 169 Days and 21.4 Hours
Spontaneous bacterial peritonitis (SBP) is an important prognostic factor for outcomes in patients with cirrhosis. Antibiotic prophylaxis is recommended in patients at high risk for developing SBP, but the choice of antibiotics remains unclear.
To evaluate the efficacy of various antibiotics for prophylaxis of SBP based on randomized control trials (RCTs).
Electronic databases were searched through November 2018 for RCTs evaluating the efficacy of therapies for primary or secondary prophylaxis of SBP. The primary outcome was the development of SBP. Sensitivity analyses limited to studies of primary or secondary prophylaxis and studies reported after 2010 were performed. The secondary outcome was the risk of all-cause mortality or transplant. The outcomes were assessed by rank of therapies based on network meta-analyses. Individual meta-analyses were also performed.
Thirteen RCTs (1742 patients) including norfloxacin, ciprofloxacin, rifaximin, trimethoprim-sulfamethoxazole (TMP-SMX), or placebo/no comparator were identified. Individual meta-analyses showed superiority of rifaximin over norfloxacin as well as norfloxacin and TMP-SMX over placebo. Network meta-analysis demonstrated the rank of efficacy in reducing the risk of SBP as: Rifaximin, ciprofloxacin, TMP-SMX, norfloxacin, and placebo/no comparator. Rifaximin ranked highest in sensitivity analyses limited to studies of primary or secondary prophylaxis and studies reported after 2010. Similarly, rifaximin ranked highest in reducing the risk of death/transplant.
The present comprehensive network meta-analysis provides RCT based evidence for superior efficacy of rifaximin compared to other antibiotics for the prophylaxis of SBP and reducing risk of death/transplant. Further RCTs are warranted to confirm our findings.
Core tip: Spontaneous bacterial peritonitis (SBP) is an important prognostic factor for outcomes in patients with cirrhosis. We performed a systematic review and network meta-analysis of randomized control trials evaluating the efficacy of antibiotics for primary or secondary prophylaxis of SBP. Rifaximin ranked highest in reducing the risk of SBP as well as the risk of death/transplant. Our comprehensive network meta-analysis provides randomized control trials-based evidence for superior efficacy of rifaximin compared to other antibiotics for the prophylaxis of SBP and reducing the risk of death/transplant.
- Citation: Faust N, Yamada A, Haider H, Komaki Y, Komaki F, Micic D, Sakuraba A. Systemic review and network meta-analysis: Prophylactic antibiotic therapy for spontaneous bacterial peritonitis. World J Hepatol 2020; 12(5): 239-252
- URL: https://www.wjgnet.com/1948-5182/full/v12/i5/239.htm
- DOI: https://dx.doi.org/10.4254/wjh.v12.i5.239
Spontaneous bacterial peritonitis (SBP) is the most common infection seen in patients with advanced liver cirrhosis and ascites[1,2]. Development of SBP can lead to renal dysfunction, hepatic encephalopathy, and deterioration of hepatic function, which adversely affect survival. Despite advances in treatment, in-hospital mortality of patients with SBP remains as high as 25%-30%[3]. Risk factors for the development of SBP include ascites protein levels < 1 g/dL, high serum bilirubin, prior episodes of SBP, and advanced liver disease[4,5]. Recurrences are also common following a single episode of SBP and are seen in up to 69% of infected patients within one year[6]. Thus, the first onset of SBP is an important prognosticator for health outcomes in patients with advanced liver disease. The use of antibiotics in patients with variceal bleeding and as secondary prophylaxis of SBP is recommended by the American Association for Study of Liver Diseases[7] and European Association for the Study of the Liver[8] guidelines[7,9,10]. However, evidence for the role and choice of antibiotics in both primary and secondary prophylaxis in the absence of gastrointestinal (GI) bleeding remains unclear.
Antibiotic prophylaxis has been shown to reduce the incidence of SBP in patients who are at high risk[11,12]. Overgrowth, translocation, and dissemination of intestinal bacteria are early steps in the pathogenesis of SBP and are more prevalent in cirrhotic patients compared to non-cirrhotic controls[13,14]. The majority of SBP are caused by Escherichia coli or other gram-negative bacteria, though gram-positive bacteria have been increasingly seen in the setting of antibiotic resistance[15,16]. Antibiotic prophylaxis primarily works via decontamination of the gut, thus lowering the bacterial reserves available for translocation. Guidelines recommend ceftriaxone for patients with advanced cirrhosis and GI bleeding or norfloxacin twice daily for seven days with severe liver disease as these patients are at high-risk for developing SBP. Trimethoprim/sulfamethoxazole (TMP-SMX) and ciprofloxacin are also listed as effective alternatives[7,10]. Additionally, two recent meta-analysis by Goel et al[17] and Sidhu et al[18] suggested a benefit for primary or secondary SBP prophylaxis in using rifaximin, a gut-selective antibiotic, compared to norfloxacin.
Several randomized control trials (RCTs) and cohort studies have demonstrated efficacy of various antibiotics, either in comparison to placebo or other antibiotics for prophylaxis of SBP[19]. Yet the number of trials remains small, and comparisons between antibiotics remains sparse, thus limiting our ability to compare treatments which have been studied separately. A network meta-analysis can be used to study outcomes of multiple interventions within the same disease process[20,21]. This study uses a network meta-analysis method to rank and provide a comprehensive evaluation of recommended options for primary and secondary antibiotic prophylaxis of SBP based on RCTs.
We performed this study according to a previously defined protocol and in accordance with the PRISMA for Network Meta-Analyses (PRISMA-NMA) guidelines[22]. The protocol of this meta-analysis has been registered to the International prospective register of systematic reviews (PROSPERO)[23]. We conducted a systemic literature search of PubMed/MEDLINE, Google scholar, Scopus, EMBASE and Cochrane Central Register of Controlled Trials (inception to November 1, 2018) for studies assessing the efficacy of antibiotic prophylaxis for SBP. For Google scholar, only the first 1000 articles were reviewed at each search as results are not provided past this number. We also searched abstracts from medical conferences (Digestive Disease Week, American College of Gastroenterology, United European Gastroenterology Week, and AASLD) and bibliographies of identified articles for additional references.
Only RCTs evaluating the efficacy of one or more antibiotic interventions for prophylaxis (primary or secondary) of SBP or reported it as an outcome were eligible for inclusion. Studies of SBP prophylaxis in the setting of GI bleeding were excluded. Control arms were placebo, no treatment, or alternative treatments. For the purpose of this study, placebo and no treatment arms were combined and are aggregately referred to as placebo from this point forward. Inclusion was not restricted based on age, sex, or duration of study. No geographic restrictions were placed on eligible articles and articles in languages other than English were translated if necessary. Studies were searched with a combination of terms including “spontaneous bacterial peritonitis”, “prophylaxis”, “antibiotics” and “randomized”. Terms were searched as both medical subject headings and free text and were combined using the set operators. Two authors (Faust N and Yamada A) independently screened potential titles and abstracts in the primary search in order to identify articles addressing the question of interest. The full text of selected articles was then evaluated for eligibility and content areas of disagreement or uncertainty were resolved based on discussion and consensus between the two authors and principal investigator.
Data was abstracted using a standardized data abstraction form. Study characteristics including the authors, location, year of study, study period, sample size, mean age of patients, sex of patients, inclusion and exclusion criteria, antibiotics used, and endpoints were collected. Outcomes and adverse events were extracted for each study when reported. The Jadad scale, a validated method for assessing the methodological quality of a clinical trial, was used to assess the quality of each included study[24]. Cochrane scores were also used as a qualitative measure for bias[25].
The primary outcome for this study was the proportion of patients who developed SBP in each intervention arm. Incidence of SBP was determined in each study by a combination of clinical characteristics (fever, abdominal pain), cytologic criteria, and ascitic fluid cultures. The secondary outcome was the risk of death/transplant as assessed by the proportion of patients who died or were transplanted in each intervention arm due to any cause. Data was extracted as intention-to-treat whenever allowed by individual RCT reporting. Outcomes were assessed by risk difference between the two treatment arms.
We performed the following subgroup analyses: (1) Excluding studies with low quality as assessed with the Jadad scale ≤ 2; (2) Analysis of primary prophylaxis, including only patients without a history of SBP; (3) Analysis of secondary prophylaxis including only patients with a history of SBP; and (4) Analysis of studies performed after 2010 (after rifaximin was approved by United States Food and Drug Administration to reduce the risk of hepatic encephalopathy).
The network meta-analysis is a technical method which allows readers to visualize and interpret data for the relative merits of multiple interventions in a given condition. This synthesis of data allows preservation of the randomization within each trial[26]. Two assumptions necessary for the validity of the network meta-analysis’ mixed comparisons are that the data across sets is transitively related and consistent[27].
In the framework of this study, transitivity is a measure of methodological homogeneity and can be assumed when the data sets for two direct comparison studies are similar in their distributions. Such is the case when subject demographics for the included studies are similar in distribution, and subjects for any given study eligible for any of the interventions based on eligibility and exclusion criteria across all studies. Still, some clinical and methodological heterogeneity is expected across studies. The Bayesian Markov chain Monte Carlo method was used account for this[28]. Our model contained parameters describing the relative treatment effect of each treatment compared with each other and a common comparator (placebo). Other treatment comparisons were derived by analyzing differences between model parameters.
Consistency refers to statistical heterogeneity, or the degree to which disagreements in study specific treatment effects exist beyond what can be explained by chance[29]. RCT consistency in this study was measured using the node-splitting method. The results were presented as median effect sizes along with 95% confidence intervals (CIs). No significant inconsistency was present when 95%CIs of inconsistency factors included zero or when a large P value (> 0.05) for the comparison between direct and indirect effects in the node splitting analysis was found.
Each Bayesian Markov chain Monte Carlo cycle provided a ranking of the treatments according to the estimated effect size and the full set of simulations. We calculated the surface under the cumulative ranking (SUCRA) probabilities[20]. SUCRAs expressed as percentages compare each intervention to an imaginary intervention that is always the best without uncertainty. The ranking probability for each drug, i.e., the most efficacious, the second-best, the third-best, and so on, was calculated and the overall ranks were interpreted by SUCRA technique. The larger SUCRAs denote more effective interventions.
For direct meta-analysis, we evaluated the presence of heterogeneity across trials of each therapy by using the I2 statistic. An I2 value of < 25% indicates low heterogeneity, 25%-75% moderate heterogeneity, and > 75% high heterogeneity, respectively[30]. We also evaluated the presence of heterogeneity across trials of each therapy by using the statistic Q and used a P value of < 0.10 as evidence of statistically significant heterogeneity[31]. All analysis was performed with ADDIS 1.× (drugis.org)[32]. We followed the Cochrane Handbook for Systematic Reviews of Interventions in the report of this meta-analysis[25].
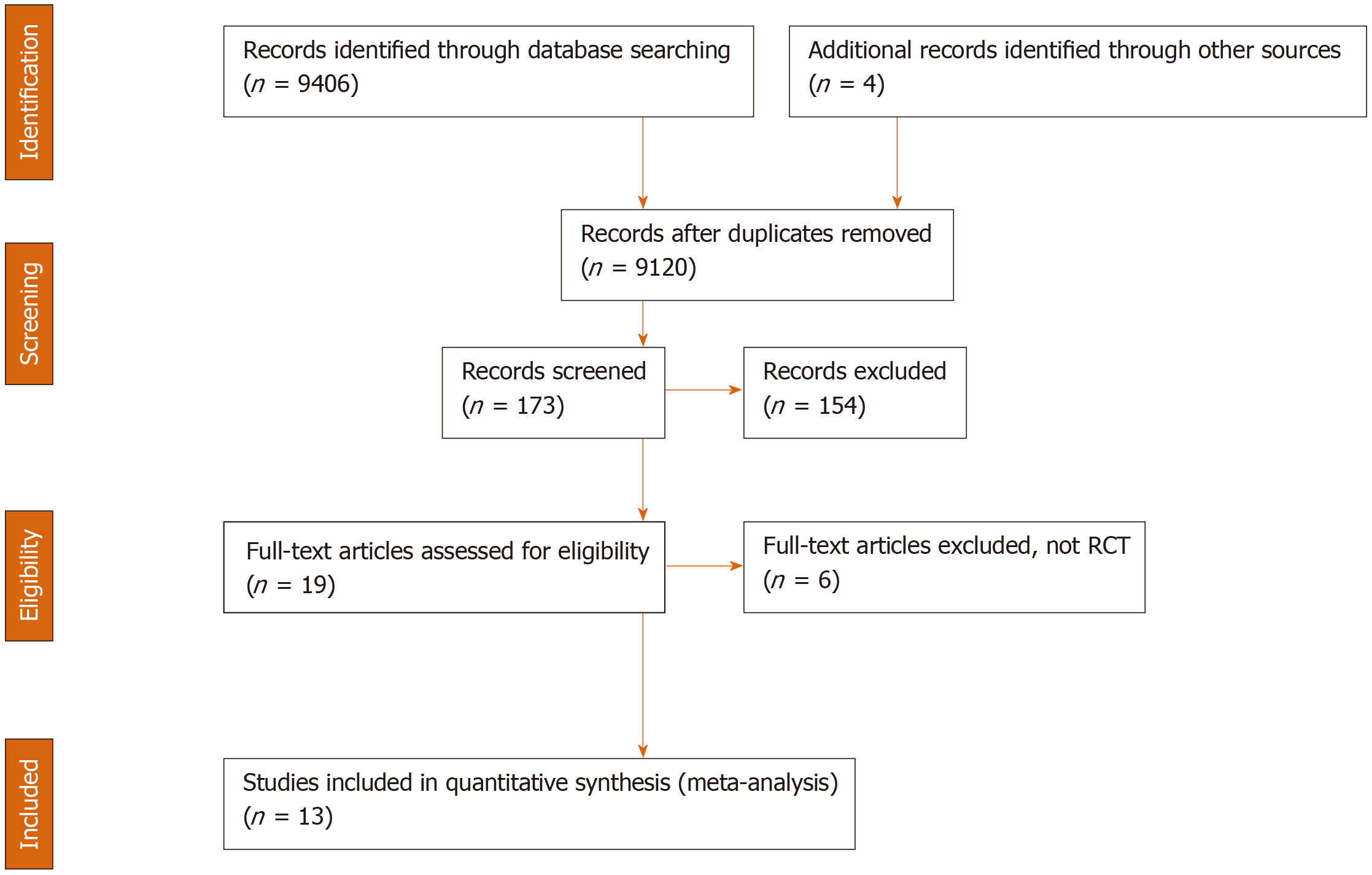
Literature review identified 171 citations through the initial search. We excluded 154 titles and abstracts after initial screening and assessed 18 articles for eligibility (Figure 1). Ultimately, 13 RCTs, including a total of 1757 patients, were included in the evaluation of 5 interventions for SBP prophylaxis: Norfloxacin, ciprofloxacin, rifaximin, trimethoprim-sulfamethoxazole (TMP-SMX), and placebo. All studies were parallel studies and 5 were placebo-controlled trials. Inclusion criteria for participants among each study included diagnosis of cirrhosis by clinical diagnosis, imaging, liver biopsy, laboratory values and/or presence of ascites. Exclusion criteria included documented anaphylaxis to one of the study interventions, hepatocellular carcinoma or other neoplasias that could shorten life expectancy, bacterial infection at admission, HIV infection or hepatic encephalopathy, and pregnant and lactating women. All trials included ascitic fluid PMN count in the diagnosis of SBP. The majority of trials diagnosed SBP with PMN ≥ 250, with one study using diagnostic criteria of polymorphonuclear cells ≥ 350. The majority of the studies included advanced cirrhotic patients (Child-Pugh class B or C) with alcoholic or viral hepatitis as its cause. The study by Assem et al[33] included a treatment group that alternated norfloxacin and rifaximin, but it was excluded from our analysis. Five studies used antibiotics for primary prophylaxis (excluded patients with a history SBP and the remainder contained a mixed cohort of patients with or without a history of SBP. Seven and 6 studies were published before and after 2010, respectively. All 3 studies that included rifaximin were published after 2015 and compared its efficacy to norfloxacin in a non-double-blinded manner[33-35]. A summary of individual study characteristics and outcome data for the included studies are summarized in Table 1. The median JADAD for all included studies was 3, with individual scores for each study ranging from 1 to 4. JADAD scores and Cochrane meta-analysis bias scores are shown in Table 2.
| Therapy/control | Ref. | Yr | Dosage of therapy | Control | Mean follow-up | History of SBP/% | ITT/PP | SBP diagnosis criteria | n (total) | Therapy | Control | ||||
| n | Developed SBP | Deaths/transplant | n | Developed SBP | Death/transplant | ||||||||||
| Ciprofloxacin vs placebo | Terg et al[45] | 2008 | Ciprofloxacin 500 mg daily | Placebo | 7.6-7.8 mo | Excluded | ITT | Ascites PMN > 250/mm3 | 100 | 50 | 2/50 | 6/50 | 50 | 7/50 | 15/50 |
| Norfloxacin vs placebo | Ginés et al[46] | 1990 | Norfloxacin 400 mg daily | Placebo | 6.4 mo | Included/20.0% | ITT | Abdominal pain, fever, ascites PMN > 350/mm3 | 80 | 40 | 5/40 | 7/40 | 40 | 14/40 | 11/40 |
| Norfloxacin vs no treatment | Novella et al[47] | 1997 | Norfloxacin 400 mg daily | No treatment | 43 wk | Excluded | ITT | Ascites PMN > 250/mm3, positive ascitic fluid culture | 109 | 56 | 1/56 | 13/56 | 53 | 9/53 | 16/53 |
| Norfloxacin vs placebo | Grangé et al[48] | 1998 | Norfloxacin 400 mg daily | Placebo | 6 mo | Excluded | ITT | Ascites PMN > 250/mm3, positive ascitic fluid culture | 107 | 53 | 0/53 | 8/53 | 54 | 5/54 | 11/54 |
| Norfloxacin vs placebo | Fernández et al[49] | 2007 | Norfloxacin 400 mg daily | Placebo | 12 mo | Excluded | ITT | Ascites PMN > 250/mm3 | 68 | 35 | 2/35 | 16/35 | 33 | 10/33 | 19/33 |
| Norfloxacin vs placebo | Moreau et al[50] | 2018 | Norfloxacin 400 mg daily | Placebo | 6 mo | Included/88.3% | ITT | Ascites PMN > 250/mm3 | 291 | 144 | 10/144 | 36/144 | 147 | 17/147 | 42/147 |
| Norfloxacin vs ciprofloxacin | Yim et al[51] | 2018 | Norfloxacin 400 mg daily | Ciprofloxacin 750 mg weekly | 12 mo | Included/88.7% | ITT/PP | Ascites PMN > 250/mm3 | 124 | 62 | 4/55 | 15/62 | 62 | 3/57 | 16/62 |
| Rifaximin vs norfloxacin | Mostafa et al[34] | 2015 | Rifaximin 800 mg daily | Norfloxacin 400 mg daily | 6 mo | Included/100% | ITT | Ascites PMN > 250/mm3 | 70 | 40 | 0/40 | 0/40 | 30 | 5/30 | 0/30 |
| Rifaximin vs norfloxacin | Elfert et al[35] | 2016 | Rifaximin 1200 mg daily | Norfloxacin 400 mg daily | 6 mo | Included/ 100% | ITT/PP | Ascites PMN > 250/mm3 | 262 | 131 | 4/103 | 18/131 | 131 | 13/92 | 32/131 |
| Rifaximin vs norfloxacin | Assem et al[33] | 2016 | Rifaximin 1100 mg daily | Norfloxacin 400 mg daily | 6 mo | Excluded | ITT/PP | Ascites PMN > 250/mm3 | 334 | 82 | 8/64 | 8/82 | 78 | 13/57 | 11/78 |
| Trimethoprim-sulfamethoxazole vs no treatment | Singh et al[52] | 1995 | TMP-SMX 160/800 mg 5 d per week | No treatment | 90 d | Included/73.3% | ITT | Ascites PMN > 250/mm3 | 60 | 30 | 1/30 | 2/30 | 30 | 8/30 | 6/30 |
| Trimethoprim-sulfamethoxazole vs norfloxacin | Alvarez et al[53] | 2005 | TMP-SMX 160/800 mg 5 d per week | Norfloxacin 400 mg daily | 163-182 d | Included/38.6% | NA | Ascites PMN > 250/mm3 | 57 | 25 | 4/25 | 5/25 | 32 | 3/32 | 7/32 |
| Trimethoprim-sulfamethoxazole vs norfloxacin | Lontos et al[54] | 2014 | TMP-SMX 160/800 mg daily | Norfloxacin 400 mg daily | 208-251 d | Included/26.2% | ITT | Ascites PMN > 250/mm3 | 80 | 40 | 2/40 | 22/40 | 40 | 2/40 | 18/40 |
| Study | 1 Was the study describ-ed as randomiz-ed? | 2 Was the randomi-zation scheme describ-ed and appropriate? | 3 Was the study describ-ed as double-blind? | 4 Was the method of double blinding appropri-ate? | 5 Was there a descrip-tion of dropouts and withdra-wals? | Total JADAD Score | Sequen-ce genera-tion (for arm randomi-zation) | Alloca-tion conceal-ed | Blinding of outcom-es | Incomple-te outcome data address-ed | ITT | Sample size calcula-tion |
| Ginés et al[46] | O | NA | O | O | O | 4 | X | X | O | O | O | O |
| Singh et al[52] | O | NA | X | NA | X | 1 | ? | ? | X | ? | O | X |
| Novella et al[47] | O | NA | X | NA | O | 2 | ? | ? | X | ? | O | X |
| Grangé et al[48] | O | NA | O | NA | O | 3 | ? | ? | ? | O | O | O |
| Alvarez et al[53] | O | NA | X | NA | X | 1 | O | O | X | ? | ? | X |
| Fernández et al[49] | O | O | O | NA | O | 4 | O | O | O | O | O | O |
| Terg et al[45] | O | O | O | NA | O | 4 | O | O | O | O | O | O |
| Lontos et al[54] | O | O | X | NA | O | 3 | O | X | X | O | O | O |
| Mostafa et al[34] | O | NA | X | NA | X | 1 | O | X | X | ? | O | O |
| Elfert et al[35] | O | O | X | NA | O | 3 | O | X | X | ? | O | O |
| Assem et al[33] | O | O | X | NA | O | 3 | O | X | X | ? | O | O |
| Yim et al[51] | O | O | X | NA | O | 3 | O | X | X | ? | O | O |
| Moreau et al[50] | O | O | O | O | O | 5 | O | O | O | O | O | O |
Individual meta-analyses were performed to compare the efficacy between each antibiotic. It should be noted that the number of studies in each meta-analysis was small ranging from 1-5. Superiority of norfloxacin and TMP-SMX over placebo were demonstrated in meta-analyses including 5 and 1 study, respectively (Supplementary Figure 1B and C). One study comparing ciprofloxacin to placebo demonstrated a non-significant superiority of ciprofloxacin over placebo (Supplementary Figure 1A). Three studies compared rifaximin to norfloxacin, and the meta-analysis showed superiority of rifaximin over norfloxacin with no heterogeneity (Supplementary Figure 1D). Two studies and one study compared TMP-SMX to norfloxacin and ciprofloxacin to norfloxacin, respectively, and the meta-analyses showed no difference between the two agents (Supplementary Figure 1E and F).
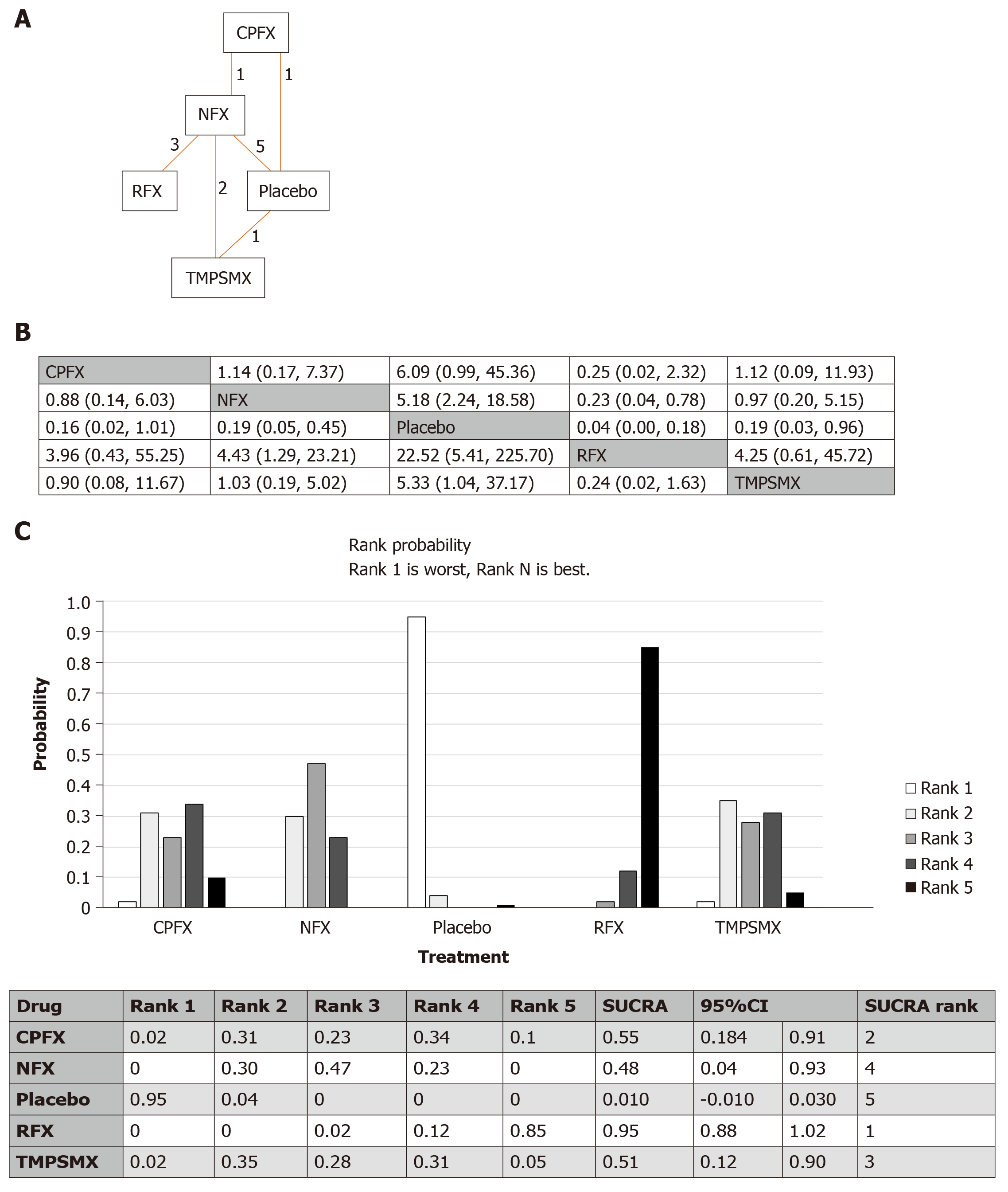
There were 5 studies comparing norfloxacin to placebo, 3 studies comparing norfloxacin to rifaximin, and two studies comparing norfloxacin to TMP-SMX. The remainder of comparisons (ciprofloxacin vs placebo, norfloxacin vs ciprofloxacin, TMP-SMX vs no treatment) included only one study each. The network of all intervention comparisons analyzed for efficacy of SBP prophylaxis is shown in Figure 2A. The network meta-analysis for the relative effects of each treatment for SBP prophylaxis is shown in Figure 2B. SUCRA interpretations of the rank probability for efficacy is shown in Figure 2C, with larger SUCRA scores indicating higher efficacy. In ascending order, the treatments ranked as (1) rifaximin; (2) ciprofloxacin; (3) TMP-SMX; (4) norfloxacin; and (5) placebo. Most of the 95%CIs of SUCRA for active treatments overlapped with each other, but none of those overlapped with the one of placebo. Similar results were found when we excluded studies with low quality (Jadad scale ≤ 2) (Supplementary Figure 2).
The results were shown to meet criteria for consistency based on the inconsistency model analyses and node-splitting analyses. The median inconsistency factors for norfloxacin/placebo/TMP-SMX and ciprofloxacin/norfloxacin/placebo were -0.26 [95%CI: (-2.85, 1.36)] and 0.06 [95%CI: -1.92, 2.41]. Comparison data from the node split model did not show significant differences between the direct and indirect effects (ciprofloxacin vs norfloxacin, P = 0.72; ciprofloxacin vs placebo, P = 0.91; norfloxacin vs placebo, P = 0.64; norfloxacin vs TMP-SMX, P = 0.35; placebo vs TMP-SMX, P = 0.35) supporting the consistency of the network meta-analysis.
As part of the subgroup analysis, we performed a network meta-analysis among the 5 studies that used antibiotics for primary prophylaxis of SBP (Supplementary Figure 3). In ascending order, the treatments ranked as (1) rifaximin; (2) norfloxacin; (3) ciprofloxacin; and (4) placebo. There was no study that used TMP-SMX for primary prophylaxis, thus, it was not included in this particular network meta-analysis. Network meta-analysis undertaken among the 8 studies that included patients who used antibiotics for secondary prophylaxis of SBP (Supplementary Figure 4), demonstrated that the treatments ranked as (1) rifaximin; (2) ciprofloxacin; (3) TMP-SMX; (4) norfloxacin; and (5) placebo. When network meta-analysis was performed among the 6 studies that were published after 2010 (Supplementary Figure 5), the treatments ranked in ascending order as (1) rifaximin; (2) TMP-SMX; (3) ciprofloxacin; (4) norfloxacin; and (5) placebo.
Individual meta-analyses assessing the risk of death/transplant are shown in Supplementary Figure 6. One study compared ciprofloxacin to placebo and 3 studies compared rifaximin to norfloxacin, and the meta-analyses showed superiority of ciprofloxacin and rifaximin over their comparators in reducing the risk of death, respectively (Supplementary Figure 6A and D). The remainder of the individual meta-analyses demonstrated no significant superiority between each treatment arm. It should be noted that the number of studies in each meta-analysis was small ranging from 1-5.
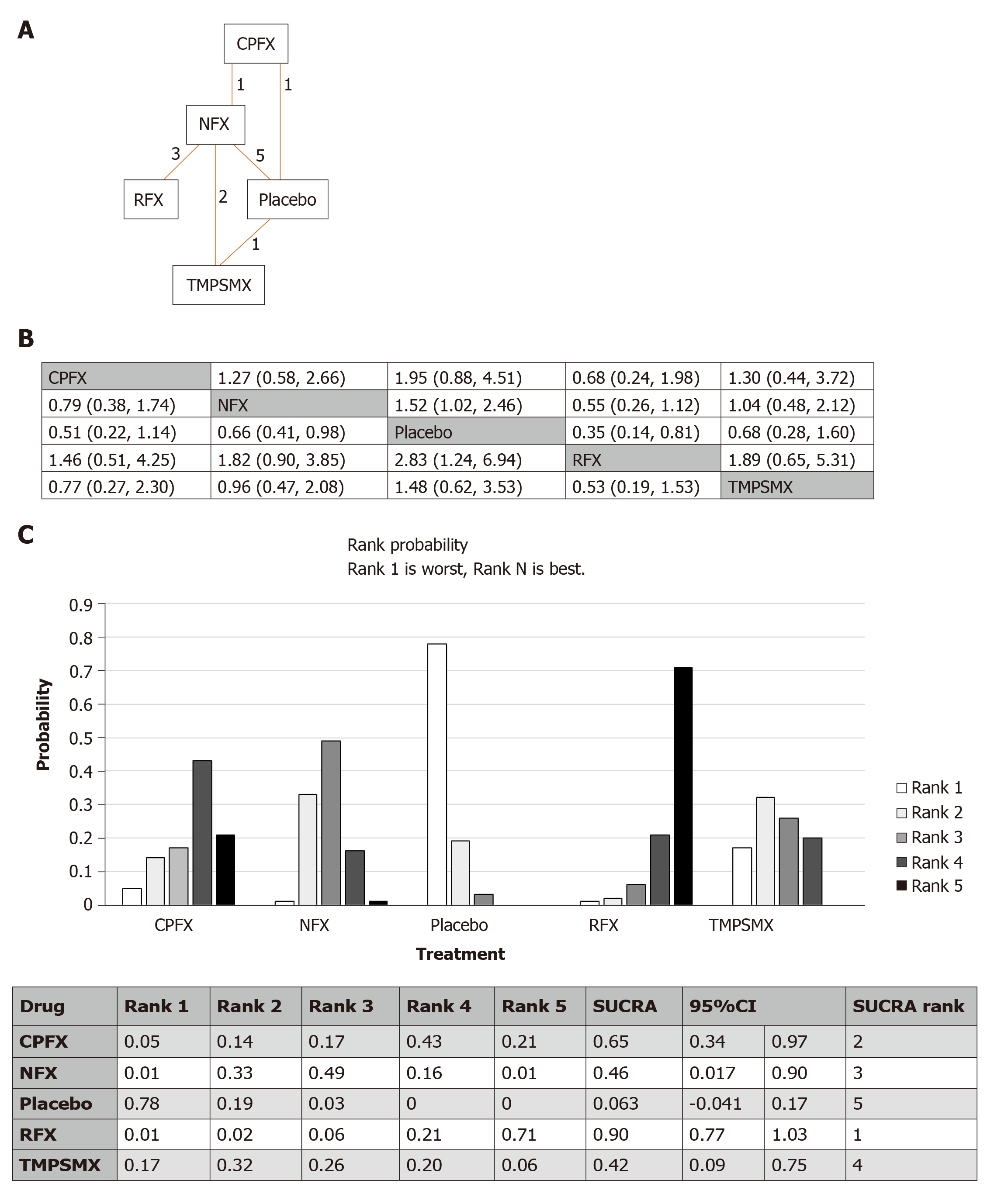
The network of all intervention comparisons analyzed for efficacy of risk reduction of death is shown in Figure 3A. The network meta-analysis for the relative effects of each treatment is shown in Figure 3B. SUCRA interpretations of the rank probability for efficacy is shown in Figure 3C and, in ascending order, the treatments ranked as (1) rifaximin; (2) ciprofloxacin; (3) norfloxacin; (4) TMP-SMX; and (5) placebo. The median inconsistency factors for norfloxacin/placebo/TMP-SMX and ciprofloxacin/norfloxacin/placebo were -0.22 [95%CI: (-1.64, 0.56)] and -0.20 [95%CI: (-1.39, 0.50)], which met the criteria for consistency. Comparison data from the node split model did not show significant differences between the direct and indirect effects (ciprofloxacin vs norfloxacin, P = 0.25; ciprofloxacin vs placebo, P = 0.21; norfloxacin vs placebo, P = 0.09; norfloxacin vs TMP-SMX, P = 0.35; placebo vs TMP-SMX, P = 0.20) supporting the consistency of the network meta-analysis.
In this systematic review and meta-analysis, we compared and assessed the efficacy of different antibiotic treatments for SBP prophylaxis in individuals with advanced cirrhosis. This was done in order to validate current treatment recommendations and to perform indirect comparisons of active treatments where no or few direct randomized comparison trials existed. Among the four antibiotics and placebo included in the meta-analysis, rifaximin was the most effective in preventing SBP, followed by ciprofloxacin, TMP-SMX, norfloxacin, and placebo. Similarly, rifaximin ranked highest in reducing the risk of death.
Current guidelines from the AASLD and EASL recommend prophylactic treatment with intravenous ceftriaxone or oral norfloxacin for the prevention of SBP in the setting of GI bleeding and severe liver disease[10]. Norfloxacin is recommended for primary prophylaxis in cirrhotic patients with low ascitic fluid protein concentration and/or high serum bilirubin levels as they are at high risk of developing a first episode of SBP. Furthermore, norfloxacin is also recommended for secondary prophylaxis because recurrent SBP is common[7,10]. Our study validates results from two meta-analyses by Goel et al[17] and Sidhu et al[18], which found a reduction in the development of SBP with the use of rifaximin compared to the recommended norfloxacin regimens. A recent network meta-analysis by Facciorusso et al[2] reported moderate evidence for norfloxacin and ciprofloxacin in primary prophylaxis of SBP, and low quality evidence for the use of rifaximin. This difference may be accounted for by the inclusion of studies that included both patients with primary prophylaxis and with a history of SBP in our study. Such studies were included in our primary outcome of combined primary and secondary prevention, but not in our subgroup analyses due to lack of subgroup randomization and incomplete information. Analyses of treatment effects in these subgroups are therefore subject to additional biases when compared to complete cohorts[36]. Our network meta-analysis provides evidence for superiority of rifaximin over the other studied antibiotics, which could otherwise not be compared by direct meta-analysis. Furthermore, ciprofloxacin and TMP-SMX ranked higher than norfloxacin in reducing the risk of SBP. Ciprofloxacin also ranked higher than norfloxacin in reducing the risk of death. Selective decontamination likely reduces the incidence of bacterial translocation of causative microflora through the gut. Evidence suggests that this effect may be compounded by or contributed to decreased expression of bacterial virulence factors and adhesion molecules[37,38]. Increased antibiotic efficacy with rifaximin has been seen in other GI diseases such as small intestinal bacterial overgrowth and traveler’s diarrhea, which may also be working preferably in the setting of SBP prophylaxis[39,40].
Rifaximin also has a favorable side effect profile compared to other antibiotics, particularly with respect to the development of antibiotic resistant flora. The use of fluoroquinolones such as norfloxacin, which have traditionally been used for SBP prophylaxis, is associated with the development of resistant bacterial strains. Concurrently, there has been a recent shift in cases of documented SBP from being caused by gram-negative organisms to being caused by gram-positive organisms[41,42]. This is particularly seen in cases of SBP in patients on norfloxacin prophylaxis and may contribute to the increased efficacy of rifaximin seen in trials vs norfloxacin, as the infective organisms are more likely to be may be gram-positive that fall under the spectrum covered by rifaximin.
A major limitation of our study is the rather sparse geometry of the network due to the small number of RCTs. This effect is compounded by the range in quality of the studies used, with a JADAD score of less than three in 4 of the 11 studies used. Scores were most often lowered by the fact that practitioners and participants were not blinded to treatments and outcomes in some of the studies. However, we confirmed that a similar result was found when excluding studies with low quality scores. Several studies also contained elements indicative of bias and heterogeneity as determined by Cochrane meta-analysis criteria, and many of the studies analyzed were relatively smaller in size. The studies that included rifaximin all compared its efficacy to norfloxacin and there were no studies comparing rifaximin to placebo or other antibiotics, therefore limiting direct comparison with other agents. This further affirms the need for network meta-analyses in order to simultaneously compare the efficacy of multiple agents. Disagreement between direct and indirect comparisons may raise concerns for the validity of a network meta-analysis, however, the robustness of our network meta-analysis was supported by the inconsistency model that demonstrated no such inconsistency. Rank probabilities identified in this network meta-analysis can be plotted against the possible ranks for all competing treatments[43,44]. We used SUCRA as a numerical summary to supplement the cumulative ranking[44], however, the results should be interpreted with caution as there is no means to statistically assess the difference of the SUCRA values[44]. Most studies did not differentiate between primary and secondary prophylaxis, but we found similar results when network meta-analysis was limited to studies using antibiotics for either primary or secondary prophylaxis. The time span of included studies ranged from the 1990s to 2018 which may have seen a change in bacteriology of organisms causing SBP, however subgroup analysis including studies that were reported after 2010 demonstrated similar outcome. The results of the secondary outcome in our network meta-analysis, the reduction in the risk of death/transplant, needs to be approached with caution as it was not a primary outcome in any of the included studies. The included studies did not take other decision points into account, such as cost or quality of life. Furthermore, other factors such as demographics, concomitant proton inhibitor use, or past antibiotic use, which could confound outcomes, could not be assessed in the present study.
In conclusion, this systematic review and network meta-analysis of RCTs comparing multiple antibiotics for prophylaxis of SBP suggests that rifaximin is the most effective for the outcomes of preventing SBP and reducing all-cause mortality in high risk cirrhotic patients. Further comparative studies, particularly with appropriate randomization and larger power, are warranted to confirm these findings.
Spontaneous bacterial peritonitis (SBP) confers significant mortality with high rates of recurrence. Prevention is therefore indicated and of great importance in cirrhotic individuals with ascites and either significant hepatic disease, gastrointestinal (GI) bleeding, or history of SBP.
Yet data is sparse regarding the choice of antibiotic when comparing the previous gold standard, norfloxacin, to other agents including ciprofloxacin, trimethoprim-sulfamethoxazole (TMP-SMX), and the GI selective agent rifaximin. The network meta-analysis technique allows us to make indirect comparisons across studies using common comparators.
Our present study uses this technique to rank and evaluate recommended therapies for primary and secondary prophylaxis of SBP.
Thirteen randomized control trials including a total of 1757 patient were analyzed. Individual meta-analyses showed superiority of rifaximin over norfloxacin as well as norfloxacin and TMP-SMX over placebo. Network meta-analysis demonstrated the rank of efficacy in reducing the combined primary and secondary risk of SBP as: Rifaximin, ciprofloxacin, TMP-SMX, norfloxacin, and placebo/no comparator. Rifaximin ranked highest in sensitivity analyses limited to studies of either primary or secondary prophylaxis alone, and in studies reported after 2010. Similarly, rifaximin ranked highest in reducing the risk of death/transplant.
This study provides new evidence for superiority of rifaximin compared to norfloxacin in both primary and secondary SBP prophylaxis. In summary, this conclusion is supported by decreased mortality when rifaximin is used for primary or secondary prophylaxis compared to norfloxacin, ciprofloxacin, and TMP-SMX as shown in individual and network meta-analyses. Other new insights from this study were that rifaximin still performed best in a subgroup analysis of studies done after the year 2010, after the recommendation was made for rifaximin use in hepatic encephalopathy.
Therefore, this study proposes the new hypothesis that the common use of rifaximin for hepatic encephalopathy in decompensated cirrhosis does not decrease its effectiveness in SBP prophylaxis. Additional molecular and biochemical data is needed to explain the beneficial effect of rifaximin. However, our data supports the hypothesis that rifaximin’s selective decontamination of the GI tract, favorable resistance profile, and ability to decrease bacterial translocation across the gut may all contribute to its superiority for prophylaxis. Implications of these results for clinical practice include reconsideration of current AASLD guidelines to recommend rifaximin over norfloxacin as the first line agent for SBP prophylaxis.
The next steps in this area of study should include additional data from large studies with direct comparisons between each antibiotic. Randomized control trial methods should be used in future research studies in order to confirm our meta-analysis findings.
Manuscript source: Invited manuscript
Specialty type: Gastroenterology and hepatology
Country/Territory of origin: United States
Peer-review report’s scientific quality classification
Grade A (Excellent): 0
Grade B (Very good): 0
Grade C (Good): C, C
Grade D (Fair): 0
Grade E (Poor): 0
P-Reviewer: Dou XG, Sievert W S-Editor: Dou Y L-Editor: A E-Editor: Wu YXJ
| 1. | Garcia-Tsao G. Current Management of the Complications of Cirrhosis and Portal Hypertension: Variceal Hemorrhage, Ascites, and Spontaneous Bacterial Peritonitis. Dig Dis. 2016;34:382-386. [PubMed] |
| 2. | Facciorusso A, Papagiouvanni I, Cela M, Buccino VR, Sacco R. Comparative efficacy of long-term antibiotic treatments in the primary prophylaxis of spontaneous bacterial peritonitis. Liver Int. 2019;39:1448-1458. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 20] [Cited by in RCA: 19] [Article Influence: 3.2] [Reference Citation Analysis (0)] |
| 3. | Saab S, Hernandez JC, Chi AC, Tong MJ. Oral antibiotic prophylaxis reduces spontaneous bacterial peritonitis occurrence and improves short-term survival in cirrhosis: a meta-analysis. Am J Gastroenterol. 2009;104:993-1001; quiz 1002. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 70] [Cited by in RCA: 66] [Article Influence: 4.1] [Reference Citation Analysis (0)] |
| 4. | Llach J, Rimola A, Navasa M, Ginès P, Salmerón JM, Ginès A, Arroyo V, Rodés J. Incidence and predictive factors of first episode of spontaneous bacterial peritonitis in cirrhosis with ascites: relevance of ascitic fluid protein concentration. Hepatology. 1992;16:724-727. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 145] [Cited by in RCA: 126] [Article Influence: 3.8] [Reference Citation Analysis (0)] |
| 5. | Runyon BA. Low-protein-concentration ascitic fluid is predisposed to spontaneous bacterial peritonitis. Gastroenterology. 1986;91:1343-1346. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 228] [Cited by in RCA: 207] [Article Influence: 5.3] [Reference Citation Analysis (0)] |
| 6. | Titó L, Rimola A, Ginès P, Llach J, Arroyo V, Rodés J. Recurrence of spontaneous bacterial peritonitis in cirrhosis: frequency and predictive factors. Hepatology. 1988;8:27-31. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 284] [Cited by in RCA: 246] [Article Influence: 6.6] [Reference Citation Analysis (0)] |
| 7. | Runyon BA; AASLD. Introduction to the revised American Association for the Study of Liver Diseases Practice Guideline management of adult patients with ascites due to cirrhosis 2012. Hepatology. 2013;57:1651-1653. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 514] [Cited by in RCA: 519] [Article Influence: 43.3] [Reference Citation Analysis (1)] |
| 8. | Oakley JR, Jagelman DG, Fazio VW, Lavery IC, Weakley FL, Easley K, Farmer RG. Complications and quality of life after ileorectal anastomosis for ulcerative colitis. Am J Surg. 1985;149:23-30. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 52] [Cited by in RCA: 40] [Article Influence: 1.0] [Reference Citation Analysis (0)] |
| 9. | Chavez-Tapia NC, Barrientos-Gutierrez T, Tellez-Avila F, Soares-Weiser K, Mendez-Sanchez N, Gluud C, Uribe M. Meta-analysis: antibiotic prophylaxis for cirrhotic patients with upper gastrointestinal bleeding - an updated Cochrane review. Aliment Pharmacol Ther. 2011;34:509-518. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 162] [Cited by in RCA: 184] [Article Influence: 13.1] [Reference Citation Analysis (0)] |
| 10. | European Association for the Study of the Liver. EASL clinical practice guidelines on the management of ascites, spontaneous bacterial peritonitis, and hepatorenal syndrome in cirrhosis. J Hepatol. 2010;53:397-417. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1125] [Cited by in RCA: 1132] [Article Influence: 75.5] [Reference Citation Analysis (0)] |
| 11. | Soriano G, Guarner C, Teixidó M, Such J, Barrios J, Enríquez J, Vilardell F. Selective intestinal decontamination prevents spontaneous bacterial peritonitis. Gastroenterology. 1991;100:477-481. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 158] [Cited by in RCA: 133] [Article Influence: 3.9] [Reference Citation Analysis (0)] |
| 12. | Sheer TA, Runyon BA. Spontaneous bacterial peritonitis. Dig Dis. 2005;23:39-46. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 66] [Cited by in RCA: 70] [Article Influence: 3.5] [Reference Citation Analysis (0)] |
| 13. | Chang CS, Chen GH, Lien HC, Yeh HZ. Small intestine dysmotility and bacterial overgrowth in cirrhotic patients with spontaneous bacterial peritonitis. Hepatology. 1998;28:1187-1190. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 173] [Cited by in RCA: 181] [Article Influence: 6.7] [Reference Citation Analysis (0)] |
| 14. | Cirera I, Bauer TM, Navasa M, Vila J, Grande L, Taurá P, Fuster J, García-Valdecasas JC, Lacy A, Suárez MJ, Rimola A, Rodés J. Bacterial translocation of enteric organisms in patients with cirrhosis. J Hepatol. 2001;34:32-37. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 302] [Cited by in RCA: 308] [Article Influence: 12.8] [Reference Citation Analysis (0)] |
| 15. | Campillo B, Dupeyron C, Richardet JP, Mangeney N, Leluan G. Epidemiology of severe hospital-acquired infections in patients with liver cirrhosis: effect of long-term administration of norfloxacin. Clin Infect Dis. 1998;26:1066-1070. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 109] [Cited by in RCA: 101] [Article Influence: 3.7] [Reference Citation Analysis (0)] |
| 16. | Tandon P, Delisle A, Topal JE, Garcia-Tsao G. High prevalence of antibiotic-resistant bacterial infections among patients with cirrhosis at a US liver center. Clin Gastroenterol Hepatol. 2012;10:1291-1298. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 117] [Cited by in RCA: 125] [Article Influence: 9.6] [Reference Citation Analysis (0)] |
| 17. | Goel A, Rahim U, Nguyen LH, Stave C, Nguyen MH. Systematic review with meta-analysis: rifaximin for the prophylaxis of spontaneous bacterial peritonitis. Aliment Pharmacol Ther. 2017;46:1029-1036. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 47] [Cited by in RCA: 60] [Article Influence: 7.5] [Reference Citation Analysis (0)] |
| 18. | Sidhu GS, Go A, Attar BM, Mutneja HR, Arora S, Patel SA. Rifaximin versus norfloxacin for prevention of spontaneous bacterial peritonitis: a systematic review. BMJ Open Gastroenterol. 2017;4:e000154. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 13] [Cited by in RCA: 13] [Article Influence: 1.6] [Reference Citation Analysis (0)] |
| 19. | Bunchorntavakul C, Chamroonkul N, Chavalitdhamrong D. Bacterial infections in cirrhosis: A critical review and practical guidance. World J Hepatol. 2016;8:307-321. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 119] [Cited by in RCA: 149] [Article Influence: 16.6] [Reference Citation Analysis (2)] |
| 20. | Mills EJ, Thorlund K, Ioannidis JP. Demystifying trial networks and network meta-analysis. BMJ. 2013;346:f2914. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 456] [Cited by in RCA: 584] [Article Influence: 48.7] [Reference Citation Analysis (0)] |
| 21. | Komaki Y, Komaki F, Micic D, Yamada A, Suzuki Y, Sakuraba A. Pharmacologic therapies for severe steroid refractory hospitalized ulcerative colitis: A network meta-analysis. J Gastroenterol Hepatol. 2017;32:1143-1151. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 15] [Cited by in RCA: 10] [Article Influence: 1.3] [Reference Citation Analysis (0)] |
| 22. | Hutton B, Salanti G, Caldwell DM, Chaimani A, Schmid CH, Cameron C, Ioannidis JP, Straus S, Thorlund K, Jansen JP, Mulrow C, Catalá-López F, Gøtzsche PC, Dickersin K, Boutron I, Altman DG, Moher D. The PRISMA extension statement for reporting of systematic reviews incorporating network meta-analyses of health care interventions: checklist and explanations. Ann Intern Med. 2015;162:777-784. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 4165] [Cited by in RCA: 5294] [Article Influence: 529.4] [Reference Citation Analysis (1)] |
| 23. | Booth A. PROSPERO's progress and activities 2012/13. Syst Rev. 2013;2:111. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 31] [Cited by in RCA: 37] [Article Influence: 3.1] [Reference Citation Analysis (0)] |
| 24. | Jadad AR, Moore RA, Carroll D, Jenkinson C, Reynolds DJ, Gavaghan DJ, McQuay HJ. Assessing the quality of reports of randomized clinical trials: is blinding necessary? Control Clin Trials. 1996;17:1-12. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 12275] [Cited by in RCA: 12887] [Article Influence: 444.4] [Reference Citation Analysis (1)] |
| 25. | Higgins JPT, Green S. Cochrane Handbook for Systematic Reviews of Interventions Version 5.1.0. The Cochrane Collaboration, 2011. Available from: http://handbook-5-1.cochrane.org. |
| 26. | Dias S, Sutton AJ, Welton NJ, Ades AE. Evidence synthesis for decision making 6: embedding evidence synthesis in probabilistic cost-effectiveness analysis. Med Decis Making. 2013;33:671-678. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 35] [Cited by in RCA: 34] [Article Influence: 3.1] [Reference Citation Analysis (0)] |
| 27. | Cipriani A, Higgins JP, Geddes JR, Salanti G. Conceptual and technical challenges in network meta-analysis. Ann Intern Med. 2013;159:130-137. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 611] [Cited by in RCA: 777] [Article Influence: 64.8] [Reference Citation Analysis (0)] |
| 28. | Smith TC, Spiegelhalter DJ, Thomas A. Bayesian approaches to random-effects meta-analysis: a comparative study. Stat Med. 1995;14:2685-2699. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 410] [Cited by in RCA: 368] [Article Influence: 12.3] [Reference Citation Analysis (0)] |
| 29. | Salanti G. Indirect and mixed-treatment comparison, network, or multiple-treatments meta-analysis: many names, many benefits, many concerns for the next generation evidence synthesis tool. Res Synth Methods. 2012;3:80-97. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 823] [Cited by in RCA: 1168] [Article Influence: 89.8] [Reference Citation Analysis (0)] |
| 30. | Higgins JP, Thompson SG, Deeks JJ, Altman DG. Measuring inconsistency in meta-analyses. BMJ. 2003;327:557-560. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 39087] [Cited by in RCA: 46535] [Article Influence: 2115.2] [Reference Citation Analysis (3)] |
| 31. | Pereira TV, Patsopoulos NA, Salanti G, Ioannidis JP. Critical interpretation of Cochran's Q test depends on power and prior assumptions about heterogeneity. Res Synth Methods. 2010;1:149-161. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 64] [Cited by in RCA: 105] [Article Influence: 7.0] [Reference Citation Analysis (0)] |
| 32. | van Valkenhoef G, Tervonen T, Zwinkels T, de Brock B, Hillege H. ADDIS: A decision support system for evidence-based medicine. Decis Support Syst. 2013;55:459-475. [DOI] [Full Text] |
| 33. | Assem M, Elsabaawy M, Abdelrashed M, Elemam S, Khodeer S, Hamed W, Abdelaziz A, El-Azab G. Efficacy and safety of alternating norfloxacin and rifaximin as primary prophylaxis for spontaneous bacterial peritonitis in cirrhotic ascites: a prospective randomized open-label comparative multicenter study. Hepatol Int. 2016;10:377-385. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 50] [Cited by in RCA: 46] [Article Influence: 5.1] [Reference Citation Analysis (0)] |
| 34. | Mostafa T, Badra G, Abdallah M. The efficacy and the immunomodulatory effect of rifaximin in prophylaxis of spontaneous bacterial peritonitis in cirrhotic Egyptian patients. Turk J Gastroenterol. 2015;26:163-169. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 21] [Cited by in RCA: 29] [Article Influence: 3.2] [Reference Citation Analysis (0)] |
| 35. | Elfert A, Abo Ali L, Soliman S, Ibrahim S, Abd-Elsalam S. Randomized-controlled trial of rifaximin versus norfloxacin for secondary prophylaxis of spontaneous bacterial peritonitis. Eur J Gastroenterol Hepatol. 2016;28:1450-1454. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 77] [Cited by in RCA: 76] [Article Influence: 8.4] [Reference Citation Analysis (0)] |
| 36. | Assmann SF, Pocock SJ, Enos LE, Kasten LE. Subgroup analysis and other (mis)uses of baseline data in clinical trials. Lancet. 2000;355:1064-1069. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 805] [Cited by in RCA: 797] [Article Influence: 31.9] [Reference Citation Analysis (0)] |
| 37. | Jiang ZD, Ke S, Dupont HL. Rifaximin-induced alteration of virulence of diarrhoea-producing Escherichia coli and Shigella sonnei. Int J Antimicrob Agents. 2010;35:278-281. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 69] [Cited by in RCA: 67] [Article Influence: 4.2] [Reference Citation Analysis (0)] |
| 38. | Brown EL, Xue Q, Jiang ZD, Xu Y, Dupont HL. Pretreatment of epithelial cells with rifaximin alters bacterial attachment and internalization profiles. Antimicrob Agents Chemother. 2010;54:388-396. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 69] [Cited by in RCA: 79] [Article Influence: 4.9] [Reference Citation Analysis (0)] |
| 39. | Gatta L, Scarpignato C. Systematic review with meta-analysis: rifaximin is effective and safe for the treatment of small intestine bacterial overgrowth. Aliment Pharmacol Ther. 2017;45:604-616. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 109] [Cited by in RCA: 166] [Article Influence: 20.8] [Reference Citation Analysis (0)] |
| 40. | Pimentel M. Review article: potential mechanisms of action of rifaximin in the management of irritable bowel syndrome with diarrhoea. Aliment Pharmacol Ther. 2016;43 Suppl 1:37-49. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 51] [Cited by in RCA: 52] [Article Influence: 5.8] [Reference Citation Analysis (1)] |
| 41. | Kim JH, Jeon YD, Jung IY, Ahn MY, Ahn HW, Ahn JY, Ku NS, Han SH, Choi JY, Ahn SH, Song YG, Han KH, Kim JM. Predictive Factors of Spontaneous Bacterial Peritonitis Caused by Gram-Positive Bacteria in Patients With Cirrhosis. Medicine (Baltimore). 2016;95:e3489. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 17] [Cited by in RCA: 17] [Article Influence: 1.9] [Reference Citation Analysis (0)] |
| 42. | Bajaj JS, Heuman DM, Hylemon PB, Sanyal AJ, White MB, Monteith P, Noble NA, Unser AB, Daita K, Fisher AR, Sikaroodi M, Gillevet PM. Altered profile of human gut microbiome is associated with cirrhosis and its complications. J Hepatol. 2014;60:940-947. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 659] [Cited by in RCA: 837] [Article Influence: 76.1] [Reference Citation Analysis (0)] |
| 43. | Cipriani A, Furukawa TA, Salanti G, Geddes JR, Higgins JP, Churchill R, Watanabe N, Nakagawa A, Omori IM, McGuire H, Tansella M, Barbui C. Comparative efficacy and acceptability of 12 new-generation antidepressants: a multiple-treatments meta-analysis. Lancet. 2009;373:746-758. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1208] [Cited by in RCA: 1073] [Article Influence: 67.1] [Reference Citation Analysis (0)] |
| 44. | Salanti G, Ades AE, Ioannidis JP. Graphical methods and numerical summaries for presenting results from multiple-treatment meta-analysis: an overview and tutorial. J Clin Epidemiol. 2011;64:163-171. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 2776] [Cited by in RCA: 2749] [Article Influence: 196.4] [Reference Citation Analysis (0)] |
| 45. | Terg R, Fassio E, Guevara M, Cartier M, Longo C, Lucero R, Landeira C, Romero G, Dominguez N, Muñoz A, Levi D, Miguez C, Abecasis R. Ciprofloxacin in primary prophylaxis of spontaneous bacterial peritonitis: a randomized, placebo-controlled study. J Hepatol. 2008;48:774-779. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 110] [Cited by in RCA: 89] [Article Influence: 5.2] [Reference Citation Analysis (0)] |
| 46. | Ginés P, Rimola A, Planas R, Vargas V, Marco F, Almela M, Forné M, Miranda ML, Llach J, Salmerón JM. Norfloxacin prevents spontaneous bacterial peritonitis recurrence in cirrhosis: results of a double-blind, placebo-controlled trial. Hepatology. 1990;12:716-724. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 427] [Cited by in RCA: 387] [Article Influence: 11.1] [Reference Citation Analysis (0)] |
| 47. | Novella M, Solà R, Soriano G, Andreu M, Gana J, Ortiz J, Coll S, Sàbat M, Vila MC, Guarner C, Vilardell F. Continuous versus inpatient prophylaxis of the first episode of spontaneous bacterial peritonitis with norfloxacin. Hepatology. 1997;25:532-536. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 141] [Cited by in RCA: 129] [Article Influence: 4.6] [Reference Citation Analysis (0)] |
| 48. | Grangé JD, Roulot D, Pelletier G, Pariente EA, Denis J, Ink O, Blanc P, Richardet JP, Vinel JP, Delisle F, Fischer D, Flahault A, Amiot X. Norfloxacin primary prophylaxis of bacterial infections in cirrhotic patients with ascites: a double-blind randomized trial. J Hepatol. 1998;29:430-436. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 142] [Cited by in RCA: 120] [Article Influence: 4.4] [Reference Citation Analysis (0)] |
| 49. | Fernández J, Navasa M, Planas R, Montoliu S, Monfort D, Soriano G, Vila C, Pardo A, Quintero E, Vargas V, Such J, Ginès P, Arroyo V. Primary prophylaxis of spontaneous bacterial peritonitis delays hepatorenal syndrome and improves survival in cirrhosis. Gastroenterology. 2007;133:818-824. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 508] [Cited by in RCA: 451] [Article Influence: 25.1] [Reference Citation Analysis (0)] |
| 50. | Moreau R, Elkrief L, Bureau C, Perarnau JM, Thévenot T, Saliba F, Louvet A, Nahon P, Lannes A, Anty R, Hillaire S, Pasquet B, Ozenne V, Rudler M, Ollivier-Hourmand I, Robic MA, d'Alteroche L, Di Martino V, Ripault MP, Pauwels A, Grangé JD, Carbonell N, Bronowicki JP, Payancé A, Rautou PE, Valla D, Gault N, Lebrec D; NORFLOCIR Trial Investigators. Effects of Long-term Norfloxacin Therapy in Patients With Advanced Cirrhosis. Gastroenterology. 2018;155:1816-1827.e9. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 134] [Cited by in RCA: 120] [Article Influence: 17.1] [Reference Citation Analysis (0)] |
| 51. | Yim HJ, Suh SJ, Jung YK, Yim SY, Seo YS, Lee YR, Park SY, Jang JY, Kim YS, Kim HS, Kim BI, Um SH. Daily Norfloxacin vs. Weekly Ciprofloxacin to Prevent Spontaneous Bacterial Peritonitis: A Randomized Controlled Trial. Am J Gastroenterol. 2018;113:1167-1176. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 16] [Cited by in RCA: 21] [Article Influence: 3.0] [Reference Citation Analysis (0)] |
| 52. | Singh N, Gayowski T, Yu VL, Wagener MM. Trimethoprim-sulfamethoxazole for the prevention of spontaneous bacterial peritonitis in cirrhosis: a randomized trial. Ann Intern Med. 1995;122:595-598. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 137] [Cited by in RCA: 118] [Article Influence: 3.9] [Reference Citation Analysis (0)] |
| 53. | Alvarez RF, Mattos AA, Corrêa EB, Cotrim HP, Nascimento TV. Trimethoprim-sulfamethoxazole versus norfloxacin in the prophylaxis of spontaneous bacterial peritonitis in cirrhosis. Arq Gastroenterol. 2005;42:256-262. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 24] [Cited by in RCA: 24] [Article Influence: 1.3] [Reference Citation Analysis (0)] |
| 54. | Lontos S, Shelton E, Angus PW, Vaughan R, Roberts SK, Gordon A, Gow PJ. A randomized controlled study of trimethoprim-sulfamethoxazole versus norfloxacin for the prevention of infection in cirrhotic patients. J Dig Dis. 2014;15:260-267. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 23] [Cited by in RCA: 29] [Article Influence: 2.6] [Reference Citation Analysis (0)] |