Published online May 28, 2021. doi: 10.3748/wjg.v27.i20.2521
Peer-review started: January 22, 2021
First decision: March 29, 2021
Revised: April 11, 2021
Accepted: April 26, 2021
Article in press: April 26, 2021
Published online: May 28, 2021
Processing time: 117 Days and 11.4 Hours
Inflammatory bowel disease, encompassing Crohn’s disease (CD) and ulcerative colitis, are chronic immune-mediated inflammatory bowel diseases (IBD) that primarily affect the gastrointestinal tract with periods of activity and remission. Large body of evidence exist to strengthen the prognostic role of endoscopic evaluation for both disease activity and severity and it remains the gold standard for the assessment of mucosal healing. Mucosal healing has been associated with improved clinical outcomes with prolonged remission, decreased hospitalization, IBD-related surgeries and colorectal cancer risk. Therefore, endoscopic objectives in IBD have been incorporated as part of standard care. With the known increased risk of colorectal cancer in IBD, although prevention strategies continue to develop, regular surveillance for early detection of neoplasia continue to be paramount in IBD patients’ care. It is thanks to evolving technology and visualization techniques that surveillance strategies are continuously advancing. Therapeutic endoscopic options in IBD have also been expanding, from surgery sparing therapies such as balloon dilation of fibrostenotic strictures in CD to endoscopic mucosal resection of neoplastic lesions. In this review article, we discuss the current evidence on the use of endoscopy as part of standard of care of IBD, its role in surveillance of neoplasia, and the role of interventional endoscopic therapies.
Core Tip: Endoscopy is critical to the diagnosis of inflammatory bowel diseases (IBD) and is increasingly being used for disease monitoring and management to achieve the therapeutic goal of mucosa healing. In this review, we focus on the utility of endoscopy as a therapeutic objective, in disease monitoring, and in surveillance to detect and prevent neoplasia. We will also discuss the evolving role of endoscopic therapeutic interventions in IBD.
- Citation: Núñez F P, Krugliak Cleveland N, Quera R, Rubin DT. Evolving role of endoscopy in inflammatory bowel disease: Going beyond diagnosis. World J Gastroenterol 2021; 27(20): 2521-2530
- URL: https://www.wjgnet.com/1007-9327/full/v27/i20/2521.htm
- DOI: https://dx.doi.org/10.3748/wjg.v27.i20.2521
Inflammatory bowel diseases (IBD), including ulcerative colitis (UC) and Crohn's disease (CD) are immune-mediated inflammatory diseases that primarily affect the gastrointestinal tract with periods of activity and remission[1,2]. The diagnosis of IBD requires endoscopic and histological evaluation of the intestinal mucosa, combined with the proper clinical presentation and setting[3]. Endoscopy allows us to differentiate CD from UC and define its severity by visualization of the colonic mucosa, its vascular pattern, mucosal lesions, as well as patterns locations of inflammation including assessment of involvement of the terminal ileum and perianal region[4].
In the absence of effective treatment, intestinal inflammation is often progressive and cumulative, leading to complications such as strictures, fistulas that require surgery, and in the long term, the risk of dysplasia or colorectal cancer (CRC)[5]. There is also evidence that such cumulative damage may result in mucosal dysfunction, with dysmotility and hypersensitivity[6]. Therefore, endoscopic control has become part of the objective treatment pillar of IBD and mucosa healing is a preferred goal of treatment[7].
In this review we will focus on the usefulness of endoscopy as a therapeutic objective, in follow-up and surveillance to detect and to prevent the development of dysplasia and CRC, and its evolving utility in interventional therapies.
Mucosal healing is recommended as a therapeutic objective in patients with IBD. This objective is associated with a better prognosis, lower rates of hospitalizations, lower risk of relapse and the need for surgery[8,9]. After the STRIDE consensus (selecting therapeutic targets in inflammatory bowel disease), it is recommended to evaluate the colonic mucosa looking for the resolution of ulcers and the friability of the mucosa 6-9 mo after starting therapy in CD and 3-6 mo in UC[10].
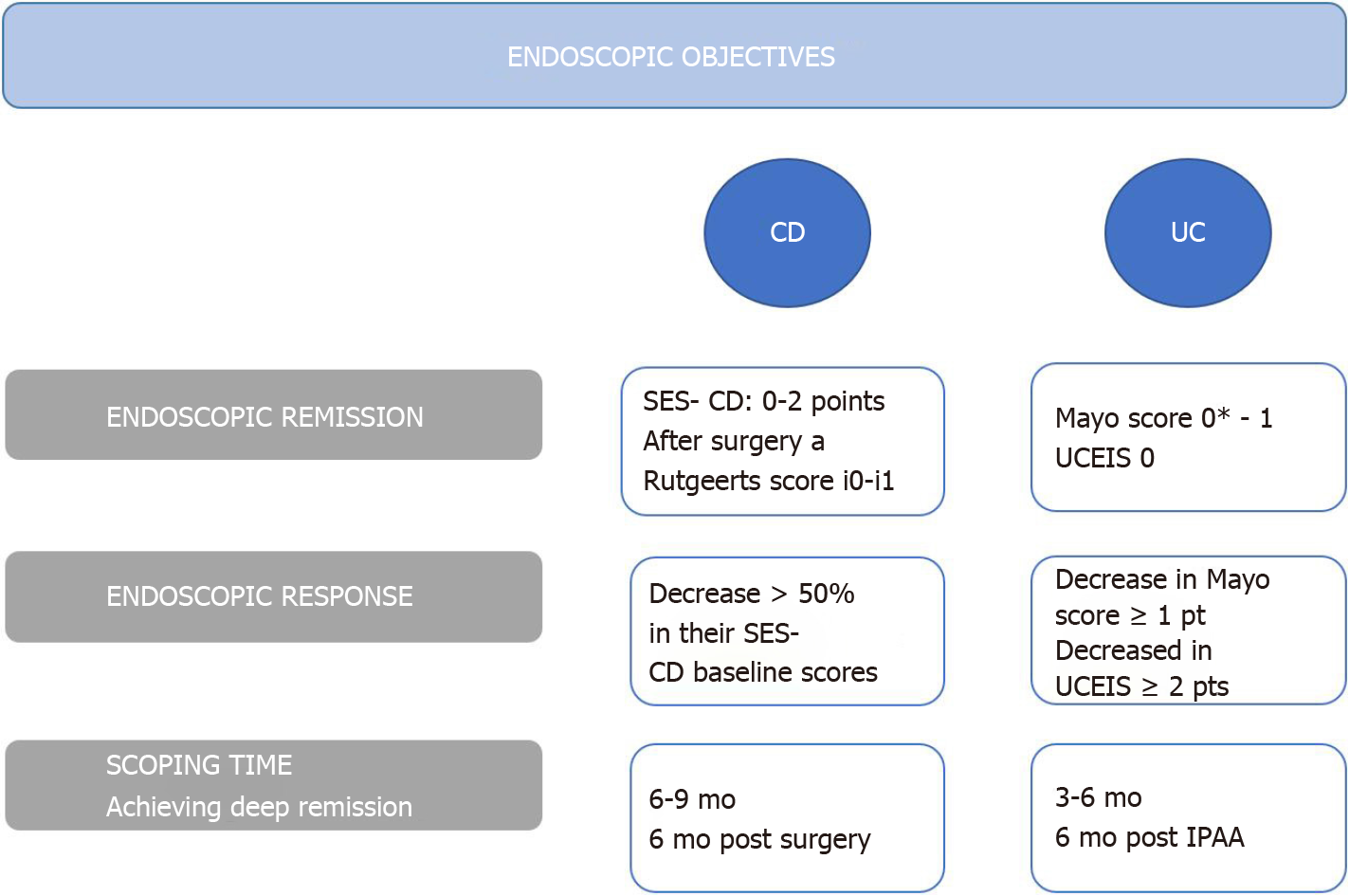
Other reviews have supported this approach as well[11,12]. It has been suggested that endoscopic remission in UC should be defined as a Ulcerative Colitis Endoscopic Index of Severity (UCEIS) of 0 or a Mayo Endoscopic Score (MES) of 0 or 1. However, in follow-up studies, a higher percentage/risk of relapse has been observed in patients who had reached a MES 1 index compared to the group with a MES 0 index (36.6% vs 9.4% with P < 0.001)[13]. On the other hand, an endoscopic response has been defined as a decrease in ≥ 1 degrees of the MES or a decrease in ≥ 2 points of the UCEIS[14,15].
The Crohn's Disease Endoscopic Index of Severity (CDEIS) and Simple Endoscopic Score for Crohn's Disease (SES-CD) are validated and reproducible indices in CD[16]. However, remission thresholds have been arbitrarily determined considering endoscopic remission with a SES-CD 0-2 index and after surgery a Rutgeerts i0-i1[17,18]. Endoscopic response is defined as a decrease greater than 50% in SES-CD or CDEIS[19] (Figure 1). STRIDE-II maintained endoscopic criteria for UC and CD[20].
One of the most important postoperative endoscopy studies was the multicenter POCER (postoperative Crohn's endoscopic recurrence), which included 17 centers in Australia and New Zealand[21]. Authors recommend performing a control endoscopy six months after surgery, regardless of the risk factors for recurrence, since approximately 60% may recur (80% if they have high risk factors vs 30% in those with low risk). In this control endoscopy the anastomosis and the terminal ileum are to be evaluated and assessed for recurrence. High risk factors for recurrence include the following: disease in those under 30 years of age, a penetrating phenotype, presence of perianal disease or having two or more surgeries[22]. The therapeutic objectives in endoscopy are fundamental to avoid future complications of the disease, and are summarized in Figure 2.
CRC is the third most frequent neoplasm in the general population, with an incidence of 1.8 million new cases per year, being the second cause of cancer mortality in the world[23]. IBD presents a higher risk of CRC, and traditionally it was considered that patients with IBD had a 2% increase in CRC risk at 10 years of disease, 8% at 20 years and 18% after 30 years of evolution[24]. However, the estimated risk of neoplasia in recent years has been lower, possibly due to more effective therapies[25] as well as better prevention strategies. A subsequent meta-analysis identified a 2.4-fold risk of CRC in UC patients, with a higher risk in male patients, younger age at diagnosis and extensive disease. Cumulative absolute risk of developing CRC was 0.4 % at 10 years and 1.1%- 5.3% at 20 years[26].
Other risk factors to consider are a family history of CRC or its association with primary sclerosing cholangitis[27]. Studies in CD have identified risk factors similar to those in UC, including diagnosis at an early age, prolonged disease, distal location, and penetrating phenotype[28]. Perianal fistulas have also been identified to have a risk of neoplastic transformation[29] (Table 1).
| CRC risk | ||
| Patient related factors | Disease related factors | |
| UC | CD | |
| Male sex; Longer duration of the disease or younger age of diagnosis; Prior History of colon neoplasia; History of CRC in first degree relative; Especially if < 50 yr old; Primary sclerosing colangitis | Extensive colitis; Severity of inflammation; Early onset of disease; Mass/stenosis; Pseudopolyps | Early onset of disease; Younger age of diagnosis; Perianal disease; Colonic extension; Bypassed segments of bowel strictures |
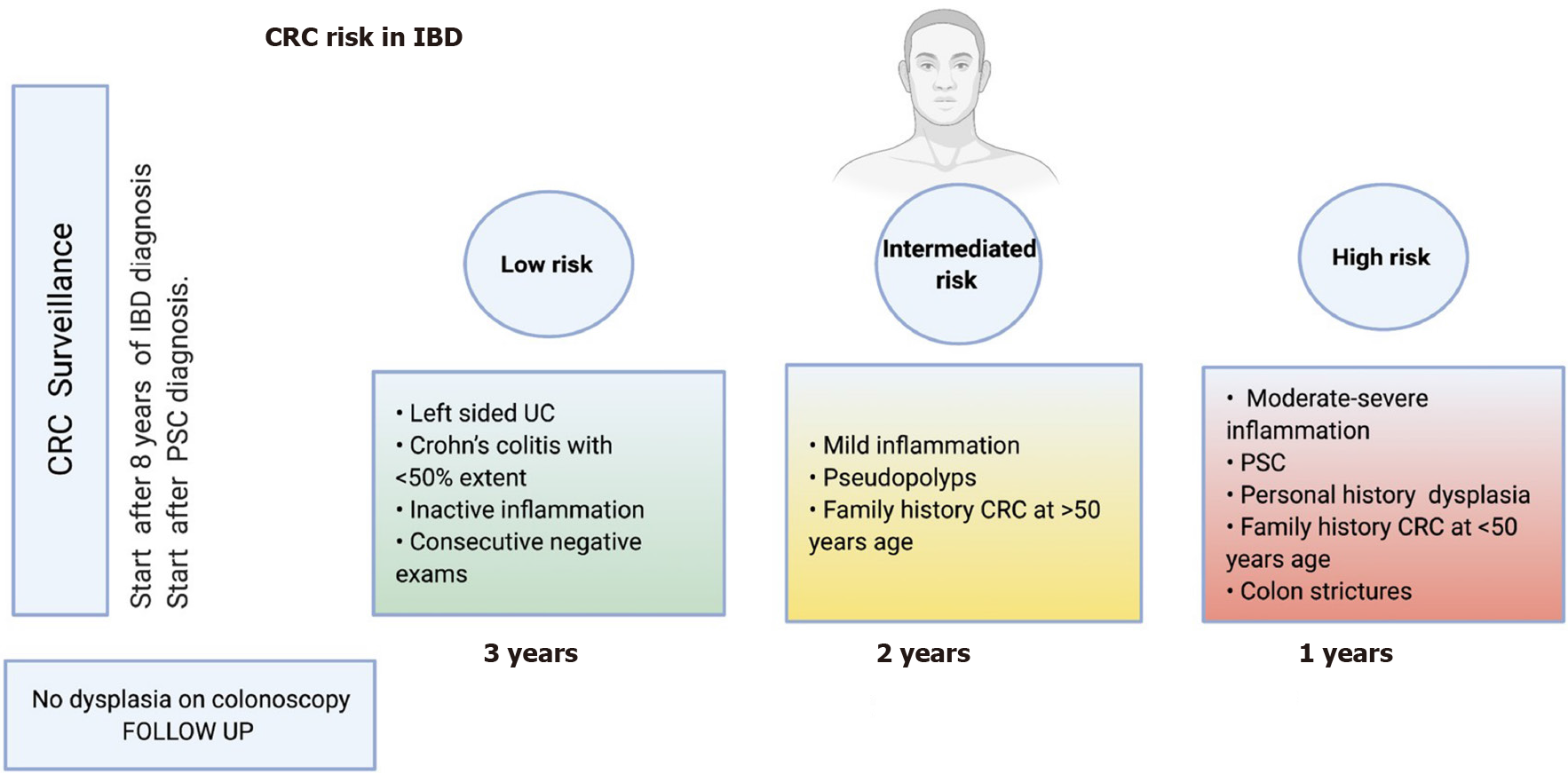
A screening endoscopic evaluation for dysplasia or colon cancer has been recommended 8 years after diagnosis in UC patients with an extension beyond the rectum or in CD patients with an extension over 30% of the colon or that compromises more than one segment[30]. In 2017, a Cochrane systematic review reported that those patients who were in endoscopic surveillance had a lower mortality associated with CRC compared to those who were not followed up [8.5% vs 22.3%, respectively; odds ratio (OR) 0.36, 95% confidence interval (CI): 0.19-0.69][31].
Endoscopic surveillance requires optimal control of the disease, including mucosal healing. This will allow for early recognition of neoplasia[3]. It has even been recommended that surveillance should be performed with fecal calprotectin levels under 100 μg/g[32] to improve visualization. It should not be forgotten that optimal bowel preparation is essential for the detection of lesions[33].
Dysplasia is defined as a neoplastic alteration of the intestinal epithelium that remains restricted within the basement membrane, without invasion of the lamina propria. These lesions can be low (LGD) or high grade (HGD). The distinction between these two depends on the distribution of nuclei within the mucosa. LGD maintains hyperchromatic nuclei located in the basal half of cells, whereas HGD presents nuclear stratification and loss of cell polarity[34].
Lesions found can be polypoid or flat, the latter being the most frequent. Flat lesions are associated with higher rate of neoplasia, common in regions that are or have been involved by IBD[35]. These lesions tend to be subtle and can be multifocal, requiring meticulous and trained endoscopists[36]. Furthermore, since dysplasia can be difficult to distinguish from epithelial regeneration secondary to inflammation[37], it is recommended that biopsies are evaluated by two expert pathologists[38].
Dye-based chromoendoscopy (DCE) is an image-enhanced endoscopic technique in which topical dyes such as methylene blue or indigo carmine are applied allowing a detailed view of the mucosa and a targeted evaluation of suspicious lesions[39]. It has reported a higher performance in detecting dysplasia in the analysis per patient OR 2.05 (95%CI: 1.26-3.35) and analysis by type of lesion OR 2.79 (95%CI: 2.08-3.73)[40]. On the other hand, Feuerstein et al[41] observed that DCE was more effective in identifying dysplasia compared to standard white light endoscopy (WLE), but without reaching significant differences compared to high-definition WLE (HD-WLE). Recently, a retrospective analysis, has shown no difference in the detection of dysplasia using DCE compared to HD-WLE, although withdrawal times were longer with DCE (24.6 min vs 15.4 min, P < 0.001)[42].
SCENIC (Surveillance for Colorectal Endoscopic Neoplasia Detection and Management in Inflammatory Bowel Disease Patients: International Consensus) recommends a surveillance study with high-definition colonoscopy or chromoendoscopy when standard white-light exam are performed[30]. The American College of Gastroenterology 2019 guidelines suggest targeted biopsies as an option with high-definition scopes. This approach is evolving as the technology is advancing. In the absence of augmenting imaging by high-definition or chromo, systematic sampling of the mucosa with random biopsies are recommended for every 10 cm of colon[3,37].
Virtual chromoendoscopy (VCE) [which includes narrow banding imaging (Oympus NBI), i-SCAN (Pentax) and Fujinon Fuji Intelligent Chromo-Endoscopy] is an optical imaging technique that uses filters to enhance the contrast of both the mucosa and the superficial vasculature, allowing a better evaluation of the mucosa. Bisschops et al[43], conducted a multicenter study with UC patients comparing DCE vs NBI. No significant difference was reported between these techniques in detecting neoplastic lesions (OR 1.02, 95%CI: 0.44-2.35, P = 0.964). The SCENIC consensus guidelines state that VCE should not replace DCE. Undoubtedly, larger studies are lacking to evaluate the usefulness of these techniques. The 2019 ACG guidelines recommend the use of DCE or NBI for the surveillance of dysplasia (conditional recommendation, low quality of evidence)[44].
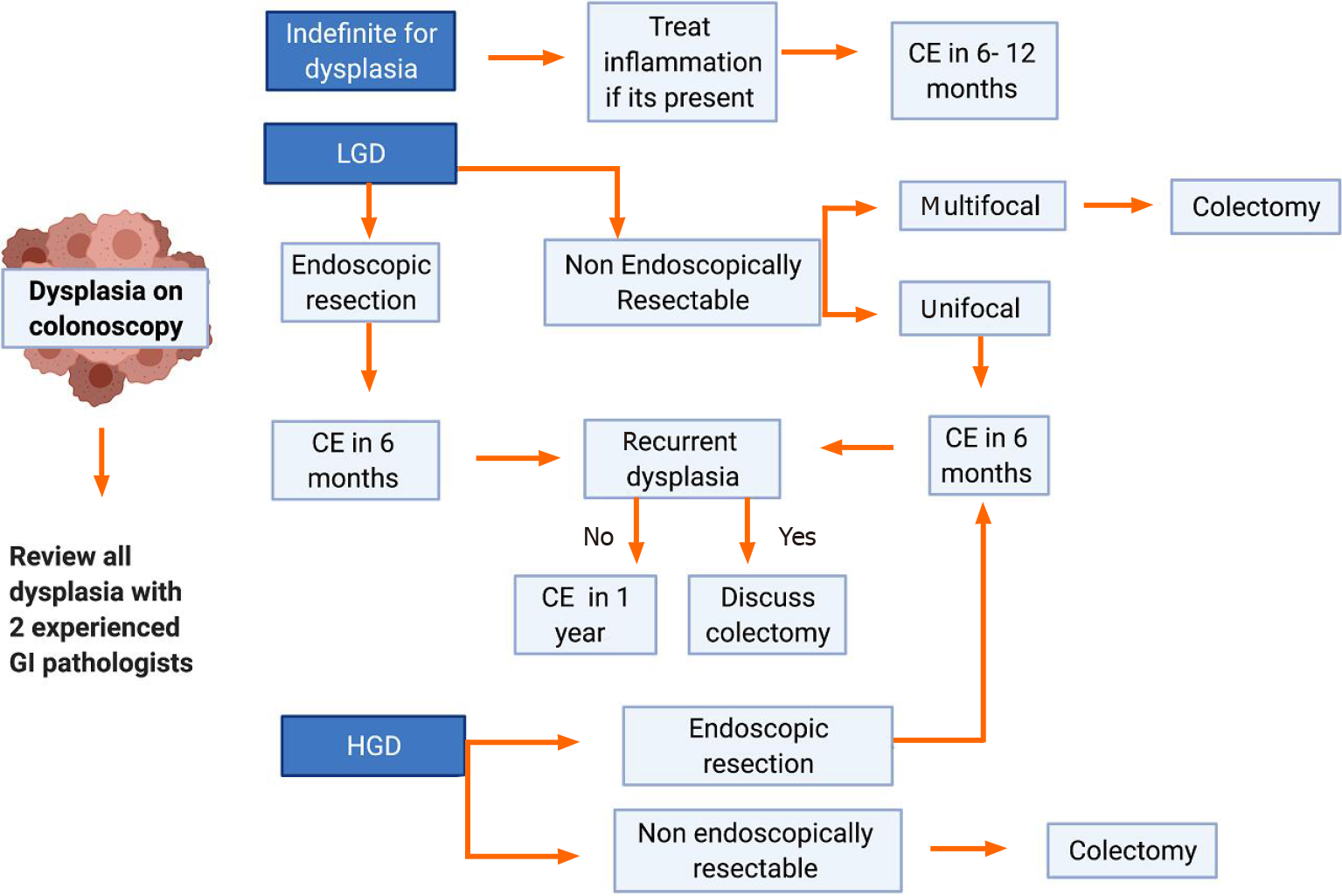
Once dysplasia has been identified, its respectability is essential to interrupt the carcinogenic sequence and thus reduce the incidence of CRC. The different management guidelines indicate that active surveillance and endoscopic follow-up should be performed according to the type of dysplasia found and the patient's risk factors. In Figures 3 and 4 the subsequent management is summarized. In selected patients, segmental resection without proctocolectomy is possible[45].
Currently, therapeutic endoscopic interventions are considered in four areas: stenosis, fistulas, complications associated with surgery and neoplasms associated with colitis[46]. We will review the latter in a separate chapter.
For its diagnosis, an endoscopic evaluation and radiologic exams are required, which may be a magnetic resonance enterography or an abdomen-pelvis computed tomographic enterography[47]. It is important to record the number of stenoses, their location, their composition (inflammatory, fibrotic), morphology, size, as well as the detection of complications such as abscesses or fistulas[48].
There are three endoscopic therapeutic options in those stenoses smaller than 5 cm; endoscopic balloon dilation, endoscopic stricturotomy or stent placement, the latter with a very low level of evidence[49]. Endoscopic balloon dilation would have a lower risk of bleeding, but a higher risk of perforation. However, retrospective studies have shown it is a safe technique in patients with CD, with more than 40% of patients asymptomatic and without requiring surgery in a subsequent follow-up[50]. Endoscopic stricturotomy is in evolution and may be an effective procedure in treating fibrotic, distal or anastomotic stenosis. The technique is based on an electro-incision, allowing control of the depth and location of the cut, and with a lower risk of perforation. In a small reported experience surgery free survival in IBD to non-IBD patients undergoing endoscopic stricturotomy, there was no statistically significant difference between the groups[51].
Endoscopic injections of steroids or anti-tumor necrosis factor agents in conjunction with endoscopic balloon dilation have been reported in series of cases with the intention of reducing the need for future dilation with inconsistent results[52,53].
In recurrent or refractory stenoses, self-expanding metal stents, covered metal stents or biodegradable metal stents have been used with good results[54,55]. These can be placed endoscopically with or without fluoroscopic guidance but must be maintained for at least 4 wk[56].
The penetrating phenotype may be primary or a result of a long-standing CD. The goals of endoscopic treatment are drainage, closure of the fistulas and preventing them from becoming complex[48]. In a cohort of 29 patients, about 90% achieved resolution of their fistulas by endoscopic fistulotomy[57]. This type of therapy might be performed in superficial, short and enteroenteric fistulas[56]. In addition, it is possible to close the fistula endoscopically by means of a clip, avoiding the formation of abscesses. This has been reported to be achieved with through-the-scope clips or over-the-scope clips, even with reports in perianal fistulas[48]. Further work is needed in this area, with clarification of risks, benefits, and approach to combination with medical interventions.
Post-surgery complications may present as dehiscence of the suture/staple line or present later with stenosis of the anastomosis, causing obstructive problems[58]. Endoscopic management of suture dehiscence has been described in clinical cases or case series, reporting lumen integrity in over 80%[59]. Approximately 11% of patients with UC require an ileal pouch anal anastomoses for their management[60], where strictures may develop in anastomosis, in the pouch or in the afferent loop. Postoperative strictures can be managed endoscopically with balloon dilations or stricturotomy. Endoscopic interventions should be avoided in periods of increased inflammation given the increased risk of perforation[21].
Endoscopic evaluation is essential to achieve current therapeutic goals in IBD, which focus on mucosal healing[61,62]. In cases in which the objectives are not achieved, endoscopic assessments direct therapeutic optimization in order to achieve them. Importantly, endoscopic assessment has a key role in prognostication and disease monitoring to control modifiable risk factors for worse clinical outcomes, with a focus on control of inflammation and prevention of complications. Among these, the incidence of CRC has a significant impact on patient morbidity and mortality, and its early diagnosis is a crucial element in IBD management. The evolution of endoscopic visualization techniques, such as the use of VCE and DCE, allow a better detection and characterization of premalignant endoscopic lesions, avoiding the risks of advanced stages[63]. Additionally, evolving endoscopic therapies allow greater minimally invasive therapeutic options for the treatment of stenosis and fistulas as an alternative to surgical management with lower morbidity.
Manuscript source: Invited manuscript
Corresponding Author's Membership in Professional Societies: American Gastroenterological Association; American College of Gastroenterology; and American Society for Gastrointestinal Endoscopy.
Specialty type: Gastroenterology and hepatology
Country/Territory of origin: United States
Peer-review report’s scientific quality classification
Grade A (Excellent): A
Grade B (Very good): B
Grade C (Good): 0
Grade D (Fair): 0
Grade E (Poor): 0
P-Reviewer: Fan RY, Joshi H S-Editor: Gao CC L-Editor: A P-Editor: Liu JH
| 1. | Ungaro R, Mehandru S, Allen PB, Peyrin-Biroulet L, Colombel JF. Ulcerative colitis. Lancet. 2017;389:1756-1770. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 2199] [Cited by in RCA: 2487] [Article Influence: 310.9] [Reference Citation Analysis (2)] |
| 2. | Loftus EV Jr. Crohn's Disease: Etiology, Complications, Assessment, Therapy, and Management. Gastroenterol Clin North Am. 2017;46:xiii-xixv. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 3] [Cited by in RCA: 9] [Article Influence: 1.1] [Reference Citation Analysis (1)] |
| 3. | Maaser C, Sturm A, Vavricka SR, Kucharzik T, Fiorino G, Annese V, Calabrese E, Baumgart DC, Bettenworth D, Borralho Nunes P, Burisch J, Castiglione F, Eliakim R, Ellul P, González-Lama Y, Gordon H, Halligan S, Katsanos K, Kopylov U, Kotze PG, Krustinš E, Laghi A, Limdi JK, Rieder F, Rimola J, Taylor SA, Tolan D, van Rheenen P, Verstockt B, Stoker J; European Crohn’s and Colitis Organisation [ECCO] and the European Society of Gastrointestinal and Abdominal Radiology [ESGAR]. ECCO-ESGAR Guideline for Diagnostic Assessment in IBD Part 1: Initial diagnosis, monitoring of known IBD, detection of complications. J Crohns Colitis. 2019;13:144-164. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1242] [Cited by in RCA: 1169] [Article Influence: 194.8] [Reference Citation Analysis (0)] |
| 4. | Zilli A, Capogreco A, Furfaro F, Allocca M, Roda G, Loy L, Fiorino G, Danese S. Improving quality of care in endoscopy of inflammatory bowel disease: can we do better? Expert Rev Gastroenterol Hepatol. 2020;14:819-828. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 2] [Reference Citation Analysis (1)] |
| 5. | Vatn MH. Natural history and complications of IBD. Curr Gastroenterol Rep. 2009;11:481-487. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 43] [Cited by in RCA: 44] [Article Influence: 2.9] [Reference Citation Analysis (0)] |
| 6. | Torres J, Billioud V, Sachar DB, Peyrin-Biroulet L, Colombel JF. Ulcerative colitis as a progressive disease: the forgotten evidence. Inflamm Bowel Dis. 2012;18:1356-1363. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 157] [Cited by in RCA: 213] [Article Influence: 16.4] [Reference Citation Analysis (0)] |
| 7. | Nuñez F P, Mahadevan U, Quera R, Bay C, Ibañez P. Treat-to-target approach in the management of inflammatory Bowel disease. Gastroenterol Hepatol. 2021;44:312-319. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 14] [Cited by in RCA: 12] [Article Influence: 3.0] [Reference Citation Analysis (0)] |
| 8. | Colombel JF, Rutgeerts P, Reinisch W, Esser D, Wang Y, Lang Y, Marano CW, Strauss R, Oddens BJ, Feagan BG, Hanauer SB, Lichtenstein GR, Present D, Sands BE, Sandborn WJ. Early mucosal healing with infliximab is associated with improved long-term clinical outcomes in ulcerative colitis. Gastroenterology. 2011;141:1194-1201. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 643] [Cited by in RCA: 728] [Article Influence: 52.0] [Reference Citation Analysis (0)] |
| 9. | Colombel JF, Rutgeerts PJ, Sandborn WJ, Yang M, Camez A, Pollack PF, Thakkar RB, Robinson AM, Chen N, Mulani PM, Chao J. Adalimumab induces deep remission in patients with Crohn's disease. Clin Gastroenterol Hepatol 2014; 12: 414-22. e5. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 180] [Cited by in RCA: 187] [Article Influence: 17.0] [Reference Citation Analysis (0)] |
| 10. | Peyrin-Biroulet L, Sandborn W, Sands BE, Reinisch W, Bemelman W, Bryant RV, D'Haens G, Dotan I, Dubinsky M, Feagan B, Fiorino G, Gearry R, Krishnareddy S, Lakatos PL, Loftus EV Jr, Marteau P, Munkholm P, Murdoch TB, Ordás I, Panaccione R, Riddell RH, Ruel J, Rubin DT, Samaan M, Siegel CA, Silverberg MS, Stoker J, Schreiber S, Travis S, Van Assche G, Danese S, Panes J, Bouguen G, O'Donnell S, Pariente B, Winer S, Hanauer S, Colombel JF. Selecting Therapeutic Targets in Inflammatory Bowel Disease (STRIDE): Determining Therapeutic Goals for Treat-to-Target. Am J Gastroenterol. 2015;110:1324-1338. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1487] [Cited by in RCA: 1409] [Article Influence: 140.9] [Reference Citation Analysis (115)] |
| 11. | Ungaro R, Colombel JF, Lissoos T, Peyrin-Biroulet L. A Treat-to-Target Update in Ulcerative Colitis: A Systematic Review. Am J Gastroenterol. 2019;114:874-883. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 115] [Cited by in RCA: 176] [Article Influence: 29.3] [Reference Citation Analysis (0)] |
| 12. | Rutgeerts P, Diamond RH, Bala M, Olson A, Lichtenstein GR, Bao W, Patel K, Wolf DC, Safdi M, Colombel JF, Lashner B, Hanauer SB. Scheduled maintenance treatment with infliximab is superior to episodic treatment for the healing of mucosal ulceration associated with Crohn's disease. Gastrointest Endosc. 2006;63:433-442; quiz 464. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 409] [Cited by in RCA: 400] [Article Influence: 21.1] [Reference Citation Analysis (0)] |
| 13. | Barreiro-de Acosta M, Vallejo N, de la Iglesia D, Uribarri L, Bastón I, Ferreiro-Iglesias R, Lorenzo A, Domínguez-Muñoz JE. Evaluation of the Risk of Relapse in Ulcerative Colitis According to the Degree of Mucosal Healing (Mayo 0 vs 1): A Longitudinal Cohort Study. J Crohns Colitis. 2016;10:13-19. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 126] [Cited by in RCA: 178] [Article Influence: 19.8] [Reference Citation Analysis (0)] |
| 14. | Vuitton L, Peyrin-Biroulet L, Colombel JF, Pariente B, Pineton de Chambrun G, Walsh AJ, Panes J, Travis SP, Mary JY, Marteau P. Defining endoscopic response and remission in ulcerative colitis clinical trials: an international consensus. Aliment Pharmacol Ther. 2017;45:801-813. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 113] [Cited by in RCA: 110] [Article Influence: 13.8] [Reference Citation Analysis (0)] |
| 15. | Negreanu L, Voiosu T, State M, Voiosu A, Bengus A, Mateescu BR. Endoscopy in inflammatory bowel disease: from guidelines to real life. Therap Adv Gastroenterol. 2019;12:1756284819865153. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 21] [Cited by in RCA: 15] [Article Influence: 2.5] [Reference Citation Analysis (0)] |
| 16. | Daperno M, Comberlato M, Bossa F, Biancone L, Bonanomi AG, Cassinotti A, Cosintino R, Lombardi G, Mangiarotti R, Papa A, Pica R, Rizzello F, D'Incà R, Orlando A. Inter-observer agreement in endoscopic scoring systems: preliminary report of an ongoing study from the Italian Group for Inflammatory Bowel Disease (IG-IBD). Dig Liver Dis. 2014;46:969-973. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 61] [Cited by in RCA: 85] [Article Influence: 7.7] [Reference Citation Analysis (0)] |
| 17. | Rutgeerts P, Geboes K, Vantrappen G, Beyls J, Kerremans R, Hiele M. Predictability of the postoperative course of Crohn's disease. Gastroenterology. 1990;99:956-963. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1226] [Cited by in RCA: 1223] [Article Influence: 34.9] [Reference Citation Analysis (0)] |
| 18. | Rivière P, Vermeire S, Irles-Depe M, Van Assche G, Rutgeerts P, de Buck van Overstraeten A, Denost Q, Wolthuis A, D'Hoore A, Laharie D, Ferrante M. No Change in Determining Crohn's Disease Recurrence or Need for Endoscopic or Surgical Intervention With Modification of the Rutgeerts' Scoring System. Clin Gastroenterol Hepatol. 2019;17:1643-1645. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 36] [Cited by in RCA: 58] [Article Influence: 9.7] [Reference Citation Analysis (0)] |
| 19. | Vuitton L, Marteau P, Sandborn WJ, Levesque BG, Feagan B, Vermeire S, Danese S, D'Haens G, Lowenberg M, Khanna R, Fiorino G, Travis S, Mary JY, Peyrin-Biroulet L. IOIBD technical review on endoscopic indices for Crohn's disease clinical trials. Gut. 2016;65:1447-1455. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 120] [Cited by in RCA: 154] [Article Influence: 17.1] [Reference Citation Analysis (0)] |
| 20. | Turner D, Ricciuto A, Lewis A, D'Amico F, Dhaliwal J, Griffiths AM, Bettenworth D, Sandborn WJ, Sands BE, Reinisch W, Schölmerich J, Bemelman W, Danese S, Mary JY, Rubin D, Colombel JF, Peyrin-Biroulet L, Dotan I, Abreu MT, Dignass A; International Organization for the Study of IBD. STRIDE-II: An Update on the Selecting Therapeutic Targets in Inflammatory Bowel Disease (STRIDE) Initiative of the International Organization for the Study of IBD (IOIBD): Determining Therapeutic Goals for Treat-to-Target strategies in IBD. Gastroenterology. 2021;160:1570-1583. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 473] [Cited by in RCA: 1643] [Article Influence: 410.8] [Reference Citation Analysis (1)] |
| 21. | De Cruz P, Kamm MA, Hamilton AL, Ritchie KJ, Krejany EO, Gorelik A, Liew D, Prideaux L, Lawrance IC, Andrews JM, Bampton PA, Gibson PR, Sparrow M, Leong RW, Florin TH, Gearry RB, Radford-Smith G, Macrae FA, Debinski H, Selby W, Kronborg I, Johnston MJ, Woods R, Elliott PR, Bell SJ, Brown SJ, Connell WR, Desmond PV. Crohn's disease management after intestinal resection: a randomised trial. Lancet. 2015;385:1406-1417. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 375] [Cited by in RCA: 444] [Article Influence: 44.4] [Reference Citation Analysis (0)] |
| 22. | Bhattacharya A, Shen B, Regueiro M. Endoscopy in Postoperative Patients with Crohn's Disease or Ulcerative Colitis. Does It Translate to Better Outcomes? Gastrointest Endosc Clin N Am. 2019;29:487-514. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 6] [Cited by in RCA: 6] [Article Influence: 1.0] [Reference Citation Analysis (0)] |
| 23. | Bray F, Ferlay J, Soerjomataram I, Siegel RL, Torre LA, Jemal A. Global cancer statistics 2018: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries. CA Cancer J Clin. 2018;68:394-424. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 53206] [Cited by in RCA: 55853] [Article Influence: 7979.0] [Reference Citation Analysis (132)] |
| 24. | Eaden JA, Abrams KR, Mayberry JF. The risk of colorectal cancer in ulcerative colitis: a meta-analysis. Gut. 2001;48:526-535. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1985] [Cited by in RCA: 2079] [Article Influence: 86.6] [Reference Citation Analysis (1)] |
| 25. | Herrinton LJ, Liu L, Levin TR, Allison JE, Lewis JD, Velayos F. Incidence and mortality of colorectal adenocarcinoma in persons with inflammatory bowel disease from 1998 to 2010. Gastroenterology. 2012;143:382-389. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 235] [Cited by in RCA: 246] [Article Influence: 18.9] [Reference Citation Analysis (0)] |
| 26. | Jess T, Rungoe C, Peyrin-Biroulet L. Risk of colorectal cancer in patients with ulcerative colitis: a meta-analysis of population-based cohort studies. Clin Gastroenterol Hepatol. 2012;10:639-645. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 581] [Cited by in RCA: 660] [Article Influence: 50.8] [Reference Citation Analysis (0)] |
| 27. | Beaugerie L, Itzkowitz SH. Cancers complicating inflammatory bowel disease. N Engl J Med. 2015;372:1441-1452. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 351] [Cited by in RCA: 419] [Article Influence: 41.9] [Reference Citation Analysis (0)] |
| 28. | Scaringi S, Di Martino C, Zambonin D, Fazi M, Canonico G, Leo F, Ficari F, Tonelli F. Colorectal cancer and Crohn's colitis: clinical implications from 313 surgical patients. World J Surg. 2013;37:902-910. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 14] [Cited by in RCA: 19] [Article Influence: 1.6] [Reference Citation Analysis (0)] |
| 29. | Connell WR, Sheffield JP, Kamm MA, Ritchie JK, Hawley PR, Lennard-Jones JE. Lower gastrointestinal malignancy in Crohn's disease. Gut. 1994;35:347-352. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 124] [Cited by in RCA: 98] [Article Influence: 3.2] [Reference Citation Analysis (0)] |
| 30. | Laine L, Kaltenbach T, Barkun A, McQuaid KR, Subramanian V, Soetikno R; SCENIC Guideline Development Panel. SCENIC international consensus statement on surveillance and management of dysplasia in inflammatory bowel disease. Gastroenterology 2015; 148: 639-651. e28. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 344] [Cited by in RCA: 390] [Article Influence: 39.0] [Reference Citation Analysis (0)] |
| 31. | Bye WA, Nguyen TM, Parker CE, Jairath V, East JE. Strategies for detecting colon cancer in patients with inflammatory bowel disease. Cochrane Database Syst Rev. 2017;9:CD000279. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 16] [Cited by in RCA: 28] [Article Influence: 3.5] [Reference Citation Analysis (0)] |
| 32. | Iacucci M, Cannatelli R, Tontini GE, Panaccione R, Danese S, Fiorino G, Matsumoto T, Kochhar GS, Shen B, Kiesslich R, Ghosh S. Improving the quality of surveillance colonoscopy in inflammatory bowel disease. Lancet Gastroenterol Hepatol. 2019;4:971-983. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 17] [Cited by in RCA: 34] [Article Influence: 6.8] [Reference Citation Analysis (0)] |
| 33. | Megna B, Weiss J, Ley D, Saha S, Pfau P, Grimes I, Li Z, Caldera F. Clear liquid diet before bowel preparation predicts successful chromoendoscopy in patients with inflammatory bowel disease. Gastrointest Endosc 2019; 89: 373-379. e2. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 14] [Cited by in RCA: 21] [Article Influence: 3.5] [Reference Citation Analysis (0)] |
| 34. | Itzkowitz SH, Harpaz N. Diagnosis and management of dysplasia in patients with inflammatory bowel diseases. Gastroenterology. 2004;126:1634-1648. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 319] [Cited by in RCA: 311] [Article Influence: 14.8] [Reference Citation Analysis (0)] |
| 35. | Vieth M, Behrens H, Stolte M. Sporadic adenoma in ulcerative colitis: endoscopic resection is an adequate treatment. Gut. 2006;55:1151-1155. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 78] [Cited by in RCA: 67] [Article Influence: 3.5] [Reference Citation Analysis (0)] |
| 36. | Lakatos PL, Lakatos L. Risk for colorectal cancer in ulcerative colitis: changes, causes and management strategies. World J Gastroenterol. 2008;14:3937-3947. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in CrossRef: 339] [Cited by in RCA: 322] [Article Influence: 18.9] [Reference Citation Analysis (0)] |
| 37. | Mattar MC, Lough D, Pishvaian MJ, Charabaty A. Current management of inflammatory bowel disease and colorectal cancer. Gastrointest Cancer Res. 2011;4:53-61. [PubMed] |
| 38. | Cairns SR, Scholefield JH, Steele RJ, Dunlop MG, Thomas HJ, Evans GD, Eaden JA, Rutter MD, Atkin WP, Saunders BP, Lucassen A, Jenkins P, Fairclough PD, Woodhouse CR; British Society of Gastroenterology; Association of Coloproctology for Great Britain and Ireland. Guidelines for colorectal cancer screening and surveillance in moderate and high risk groups (update from 2002). Gut. 2010;59:666-689. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 897] [Cited by in RCA: 808] [Article Influence: 53.9] [Reference Citation Analysis (2)] |
| 39. | American Society for Gastrointestinal Endoscopy Standards of Practice Committee. , Shergill AK, Lightdale JR, Bruining DH, Acosta RD, Chandrasekhara V, Chathadi KV, Decker GA, Early DS, Evans JA, Fanelli RD, Fisher DA, Fonkalsrud L, Foley K, Hwang JH, Jue TL, Khashab MA, Muthusamy VR, Pasha SF, Saltzman JR, Sharaf R, Cash BD, DeWitt JM. The role of endoscopy in inflammatory bowel disease. Gastrointest Endosc 2015; 81: 1101-21. e1-13. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 230] [Cited by in RCA: 259] [Article Influence: 25.9] [Reference Citation Analysis (0)] |
| 40. | Har-Noy O, Katz L, Avni T, Battat R, Bessissow T, Yung DE, Engel T, Koulaouzidis A, Eliakim R, Ben-Horin S, Kopylov U. Chromoendoscopy, Narrow-Band Imaging or White Light Endoscopy for Neoplasia Detection in Inflammatory Bowel Diseases. Dig Dis Sci. 2017;62:2982-2990. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 27] [Cited by in RCA: 35] [Article Influence: 4.4] [Reference Citation Analysis (0)] |
| 41. | Feuerstein JD, Rakowsky S, Sattler L, Yadav A, Foromera J, Grossberg L, Cheifetz AS. Meta-analysis of dye-based chromoendoscopy compared with standard- and high-definition white-light endoscopy in patients with inflammatory bowel disease at increased risk of colon cancer. Gastrointest Endosc 2019; 90: 186-195. e1. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 81] [Cited by in RCA: 71] [Article Influence: 11.8] [Reference Citation Analysis (0)] |
| 42. | Clarke K, Kang M, Gorrepati VS, Stine JG, Tinsley A, Williams E, Moyer M, Coates M. Dysplasia detection is similar between chromoendoscopy and high-definition white-light colonoscopy in inflammatory bowel disease patients: a US-matched case-control study. Int J Colorectal Dis. 2020;35:2301-2307. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 10] [Cited by in RCA: 10] [Article Influence: 2.0] [Reference Citation Analysis (0)] |
| 43. | Bisschops R, Bessissow T, Joseph JA, Baert F, Ferrante M, Ballet V, Willekens H, Demedts I, Geboes K, De Hertogh G, Vermeire S, Rutgeerts P, Van Assche G. Chromoendoscopy vs narrow band imaging in UC: a prospective randomised controlled trial. Gut. 2018;67:1087-1094. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 67] [Cited by in RCA: 100] [Article Influence: 14.3] [Reference Citation Analysis (0)] |
| 44. | Rubin DT, Ananthakrishnan AN, Siegel CA, Sauer BG, Long MD. ACG Clinical Guideline: Ulcerative Colitis in Adults. Am J Gastroenterol. 2019;114:384-413. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 870] [Cited by in RCA: 1042] [Article Influence: 173.7] [Reference Citation Analysis (0)] |
| 45. | Krugliak Cleveland N, Ollech JE, Colman RJ, Rodriquez D, Hirsch A, Cohen RD, Hanauer SB, Hart J, Hurst R, Rubin DT. Efficacy and Follow-up of Segmental or Subtotal Colectomy in Patients With Colitis-Associated Neoplasia. Clin Gastroenterol Hepatol. 2019;17:205-206. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 13] [Cited by in RCA: 23] [Article Influence: 3.8] [Reference Citation Analysis (0)] |
| 46. | Shen B, Kochhar G, Hull TL. Bridging Medical and Surgical Treatment of Inflammatory Bowel Disease: The Role of Interventional IBD. Am J Gastroenterol. 2019;114:539-540. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 9] [Cited by in RCA: 11] [Article Influence: 1.8] [Reference Citation Analysis (0)] |
| 47. | Fletcher JG, Fidler JL, Bruining DH, Huprich JE. New concepts in intestinal imaging for inflammatory bowel diseases. Gastroenterology. 2011;140:1795-1806. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 101] [Cited by in RCA: 87] [Article Influence: 6.2] [Reference Citation Analysis (0)] |
| 48. | Gu YB, Zhong J; Chinese IBD Endoscopic Club. Endoscopic management of stricturing Crohn's disease. J Dig Dis. 2020;21:351-354. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 3] [Cited by in RCA: 2] [Article Influence: 0.4] [Reference Citation Analysis (0)] |
| 49. | Shen B, Kochhar G, Navaneethan U, Liu X, Farraye FA, Gonzalez-Lama Y, Bruining D, Pardi DS, Lukas M, Bortlik M, Wu K, Sood A, Schwartz DA, Sandborn WJ; Global Interventional Inflammatory Bowel Disease Group. Role of interventional inflammatory bowel disease in the era of biologic therapy: a position statement from the Global Interventional IBD Group. Gastrointest Endosc. 2019;89:215-237. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 42] [Cited by in RCA: 53] [Article Influence: 8.8] [Reference Citation Analysis (0)] |
| 50. | Tilmant M, Serrero M, Poullenot F, Bouguen G, Pariente B, Altwegg R, Basile P, Filippi J, Vanelslander P, Buisson A, Desjeux A, Laharie D, Le Balch E, Nachury M, Boivineau L, Savoye G, Hebuterne X, Poincloux L, Vuitton L, Brazier F, Yzet C, Lamrani A, Peyrin-Biroulet L, Fumery M. Endoscopic balloon dilation of colorectal strictures complicating Crohn's disease: a multicenter study. Clin Res Hepatol Gastroenterol. 2020;101561. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 3] [Cited by in RCA: 4] [Article Influence: 1.0] [Reference Citation Analysis (0)] |
| 51. | Zhang LJ, Lan N, Wu XR, Shen B. Endoscopic stricturotomy in the treatment of anastomotic strictures in inflammatory bowel disease (IBD) and non-IBD patients. Gastroenterol Rep (Oxf). 2020;8:143-150. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 6] [Cited by in RCA: 17] [Article Influence: 2.8] [Reference Citation Analysis (0)] |
| 52. | Swaminath A, Lichtiger S. Dilation of colonic strictures by intralesional injection of infliximab in patients with Crohn's colitis. Inflamm Bowel Dis. 2008;14:213-216. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 76] [Cited by in RCA: 74] [Article Influence: 4.4] [Reference Citation Analysis (0)] |
| 53. | Di Nardo G, Oliva S, Passariello M, Pallotta N, Civitelli F, Frediani S, Gualdi G, Gandullia P, Mallardo S, Cucchiara S. Intralesional steroid injection after endoscopic balloon dilation in pediatric Crohn's disease with stricture: a prospective, randomized, double-blind, controlled trial. Gastrointest Endosc. 2010;72:1201-1208. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 104] [Cited by in RCA: 92] [Article Influence: 6.1] [Reference Citation Analysis (0)] |
| 54. | Matsuhashi N, Nakajima A, Suzuki A, Yazaki Y, Takazoe M. Long-term outcome of non-surgical strictureplasty using metallic stents for intestinal strictures in Crohn's disease. Gastrointest Endosc. 2000;51:343-345. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 60] [Cited by in RCA: 54] [Article Influence: 2.2] [Reference Citation Analysis (0)] |
| 55. | Rodrigues C, Oliveira A, Santos L, Pires E, Deus J. Biodegradable stent for the treatment of a colonic stricture in Crohn's disease. World J Gastrointest Endosc. 2013;5:265-269. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in CrossRef: 31] [Cited by in RCA: 28] [Article Influence: 2.3] [Reference Citation Analysis (1)] |
| 56. | Chen M, Shen B. Endoscopic therapy for Kock pouch strictures in patients with inflammatory bowel disease. Gastrointest Endosc. 2014;80:353-359. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 14] [Cited by in RCA: 14] [Article Influence: 1.3] [Reference Citation Analysis (0)] |
| 57. | Kochhar G, Shen B. Endoscopic fistulotomy in inflammatory bowel disease (with video). Gastrointest Endosc. 2018;88:87-94. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 22] [Cited by in RCA: 25] [Article Influence: 3.6] [Reference Citation Analysis (0)] |
| 58. | Chen M, Shen B. Endoscopic Therapy in Crohn's Disease: Principle, Preparation, and Technique. Inflamm Bowel Dis. 2015;21:2222-2240. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 54] [Cited by in RCA: 56] [Article Influence: 5.6] [Reference Citation Analysis (0)] |
| 59. | Verlaan T, Bartels SA, van Berge Henegouwen MI, Tanis PJ, Fockens P, Bemelman WA. Early, minimally invasive closure of anastomotic leaks: a new concept. Colorectal Dis. 2011;13 Suppl 7:18-22. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 44] [Cited by in RCA: 41] [Article Influence: 2.9] [Reference Citation Analysis (0)] |
| 60. | Prudhomme M, Dozois RR, Godlewski G, Mathison S, Fabbro-Peray P. Anal canal strictures after ileal pouch-anal anastomosis. Dis Colon Rectum. 2003;46:20-23. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 81] [Cited by in RCA: 73] [Article Influence: 3.3] [Reference Citation Analysis (0)] |
| 61. | Agrawal M, Colombel JF. Treat-to-Target in Inflammatory Bowel Diseases, What Is the Target and How Do We Treat? Gastrointest Endosc Clin N Am. 2019;29:421-436. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 30] [Cited by in RCA: 34] [Article Influence: 5.7] [Reference Citation Analysis (0)] |
| 62. | Gupta A, Yu A, Peyrin-Biroulet L, Ananthakrishnan AN. Treat to Target: The Role of Histologic Healing in Inflammatory Bowel Diseases: A Systematic Review and Meta-analysis. Clin Gastroenterol Hepatol. 2020;. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 104] [Cited by in RCA: 97] [Article Influence: 24.3] [Reference Citation Analysis (0)] |
| 63. | Scoville EA, Schwartz DA. Endoscopy in inflammatory bowel disease: advances in disease management. Gastrointest Endosc. 2017;86:952-961. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 4] [Cited by in RCA: 5] [Article Influence: 0.6] [Reference Citation Analysis (0)] |