Published online Mar 7, 2019. doi: 10.3748/wjg.v25.i9.1116
Peer-review started: November 1, 2018
First decision: December 5, 2018
Revised: February 15, 2019
Accepted: February 15, 2019
Article in press: February 15, 2019
Published online: March 7, 2019
Processing time: 129 Days and 8.3 Hours
Non-alcoholic steatohepatitis (NASH) has become one of the leading causes of liver disease in the western world. In obese patients weight reduction is recommended. Up to now there are no specific guidelines for weight loss in order to reduce hepatic fat content.
To investigate the effects of a 24-wk guided lifestyle intervention program compared to a meal replacement regimen based on soy protein.
Twenty-six subjects with NASH participated in a randomized single-center study. They were randomly assigned to either meal replacement group (MR-G) with soy-yogurt-honey preparation or to guided lifestyle change group (LC-G) with endurance activity and nutrition counselling. Serum alanine transaminase (ALT), aspartate transaminase (AST), lipid parameters, and adipokines were measured. Liver fat content and lipid composition were determined by magnetic resonance imaging and magnetic resonance spectroscopy. Body fat mass and lean body mass were assessed using Bod Pod® device. Pre- and post-intervention monitoring of parameters was performed. Statistical analyses were conducted with SPSS software, results were expressed as median (interquartile range).
Twenty-two subjects (MR-G, n = 11 and LC-G, n = 11) completed the study (9 women, 13 men; age 52.1 (15.0) years, body mass index (BMI) 32.3 (3.3) kg/m²). In both groups a significant weight loss was achieved (MR-G: -6.4 (3.6) kg, P < 0.01; LC-G: -9.1 (10.4) kg, P < 0.01). BMI dropped in both groups (MR-G: -2.3 (1.5) kg/m2, P = 0.003; LC-G: -3.0 (3.4) kg/m2, P = 0.006). Internal fat and hepatic lipid content were markedly reduced in both groups in comparable amount. There was a strong correlation between reduction in liver fat and decrease in ALT. Likewise, both groups showed an improvement in glycemic control and lipid profile. Changes in adipokines, particularly in adiponectin and leptin were closely related to intrahepatic lipid changes.
Comprehensive lifestyle intervention and meal replacement regimen have comparable effects on body and liver fat, as well as decrease in markers of hepatic inflammation among NASH patients.
Core tip: Non-alcoholic steatohepatitis (NASH) is a major cause of chronic liver disease. In obese patients weight reduction is recommended. We studied the effect of a soy protein-based meal replacement therapy and a therapeutic lifestyle intervention in a randomized controlled study of obese patients with NASH. Both groups significantly lost body fat and liver fat while muscle mass remained stable. Corresponding changes were found in blood lipids and adipokines. However, liver fat quality as mean chain length and saturation of lipids was modified differently by each intervention. The relevance of these findings has to be cleared by further studies.
- Citation: Deibert P, Lazaro A, Schaffner D, Berg A, Koenig D, Kreisel W, Baumstark MW, Steinmann D, Buechert M, Lange T. Comprehensive lifestyle intervention vs soy protein-based meal regimen in non-alcoholic steatohepatitis. World J Gastroenterol 2019; 25(9): 1116-1131
- URL: https://www.wjgnet.com/1007-9327/full/v25/i9/1116.htm
- DOI: https://dx.doi.org/10.3748/wjg.v25.i9.1116
Non-alcoholic steatohepatitis (NASH) has become one of the leading causes of liver disease in western countries. It is estimated that about 20% to 30% of adults in developed countries have excess fat accumulation in the liver, 50% among people with diabetes, and about 80% in the obese and morbidly obese[1]. The main feature of NASH is the presence of fat in the liver accompanied by signs of inflammation and/or damage. Without the latter, the condition is referred to as non-alcoholic fatty liver disease (NAFLD)[2].
NASH may lead to liver cirrhosis and portal hypertension with severe sequelae including hepatocellular carcinoma. It is the most rapidly growing indication for liver transplantation in patients with hepatocellular carcinoma in the United States[3] Though there are no established guidelines for the prevention or treatment of NASH an increase of physical activity or weight loss are recommended.
Physical activity has been known to improve insulin resistance, maintain weight loss, and improve liver histology in NASH patients. An increase in physical performance has been associated with improved hepatic metabolism, even independent of body weight reduction[4-7]. Physical activity increases hepatic fatty acid oxidation and decreases the intermediates of fatty acid synthesis, resulting in a decrease of hepatic steatosis[8]. Habitual leisure-time physical activity or aerobic exercise training may play a protective role in NAFLD[7,9,10]. However, there is no evidence on the specific kinds of exercise (e.g. in terms of duration, intensity) which will be of most benefit[11].
Weight loss due to caloric restriction has been proven to reduce hepatic fat content. With a gradual weight reduction under a balanced diet, Ueno et al[12] demonstrated significant reduction in hepatic steatosis and an improvement in hepatic inflammation and fibrosis. Hepatic lipid content is also influenced by other factors such as lipid composition of the diet and the condition of the anti-oxidant system[13,14]. However, the optimal dietary restrictions are still under debate, thus a clear recommendation for the patients is still lacking[15]. As insulin resistance is a key mechanism in both metabolic syndrome and NASH, observational studies consistently reported an association between higher liver fat content and high risk of coronary artery disease. There is an increased risk for cardiovascular disease in patients with NASH[16].
On the other hand, liver fat content seems to be a risk factor that is not strictly related to insulin resistance[6,17] and may be of further significance. With MRS liver fat content is quantifiable. This method is regarded as gold standard to detect the accumulation of liver fat in vivo[18]. Moreover, the chain length of stored fatty acids and the percentage of saturated lipids can be estimated noninvasively. In a previous randomized controlled study, it was shown that with respect to weight reduction the effect of therapeutic lifestyle changes is comparable to a meal replacement regimen based on soy protein[19]. Furthermore, parameters defining the metabolic syndrome can be improved with either intervention[20,21].
Fat storing cells are no longer considered as energy stores only, as they also influence the metabolism by secretion of polypeptide hormones known as adipokines. Adiponectin has anti-inflammatory, anti-diabetic, and anti-atherogenic properties[22]. Its expression and plasma concentration are inversely related to insulin resistance, metabolic syndrome and type 2 diabetes mellitus, as well as obesity. Leptin is secreted proportionally to the amount of white adipose mass. Its levels in the circulation depend on the amount of adipose tissue and the status of energy balance[23]. High levels of leptin in the circulation are associated with the severity of NAFLD[24]. On the other hand, fetuin A has been suggested as noninvasive biomarker of hepatic steatosis and as an early indicator of NAFLD[25,26]. Vaspin was seen to be associated with NAFLD and grade of hepatic inflammation[27,28]. However, other studies yielded conflicting results, thus the role of Vaspin in NAFLD remains unclear. Lastly, resistin has been positively associated with histological steatosis and portal inflammation[29].
This study aims to compare a guided intensive lifestyle intervention program and a soy protein-based meal replacement therapy in patients with NASH. The effects of a significant weight loss after 24 wk on liver fat content, lipid composition, and markers of liver inflammation were analyzed. Changes in abdominal, subcutaneous and intrahepatic fat, as well as body composition in both interventions were also studied. In a subgroup, the proportion of saturated and unsaturated lipids of intrahepatic fat was quantified and analyzed in relation to serum adipokines.
Patients eligible for participation were obese adults with body mass index (BMI) between 30 and 40 and with sonographic findings of fatty liver, as well as elevated liver enzymes [at least alanine transaminase (ALT) of > 20% the ULN]. Daily alcohol consumption had to be less than 20 g in males and less than 10g in females. Secondary causes of fatty liver disease other than overweight and obesity were excluded by anamnesis. The possibility and willingness to participate in a physical training program was another prerequisite.
Exclusion criteria included limited physical performance (ergometer test: < 75 Watt for 2 min), insufficiently treated arterial hypertension, insulin-dependent diabetes mellitus, renal disease with compromised renal function, psychiatric disorder, and intake of hormones. All subjects completed a comprehensive medical examination, routine blood tests, and ultrasound at the screening visit. Exercise tests were done using a cycling ergometer (Ergoline, Siemens, Germany) starting with a workload of 25 W, increasing by 25 W every 2 min until exhaustion. Written informed consent was provided by all subjects and the study protocol was approved by the Ethics Review Board of the University of Freiburg Medical Center.
The subjects were randomly assigned to the treatment groups using a random list. During the first six weeks of the program, the subjects in the meal replacement group (MR-G) were instructed to replace two daily meals with a commercially available soy-yogurt-honey preparation (Almased®) as recently described in a study by Koohkan et al[30]. In the following 18 wk, one daily meal was replaced by the preparation. In addition, the dietary intake of fat during this second phase was not to exceed 60g per day. The first 6-wk diet contained 1000 kcal per day for women and 1200 kcal for men, while in the following weeks the dietary program was aimed at a maximum of 1500 kcal for women and 1700 kcal for men. These guidelines were given at a group session after randomization by a dietician.
On the other hand, the lifestyle change group (LC-G) attended 6 weekly teaching sessions about nutrition and physical exercise. They had individual consultations pre-intervention and then again at week 6. All sessions were conducted by experts in nutritional counselling. Subjects received a diet overview handout in accordance with the guidelines set by the German Society of Nutrition and the German Society of Sports Medicine and Prevention. Here, the prescribed dietary program was a moderate fat, nutrient-balanced diet consisting of 1200 to 1500 kcal per day for women and 1500 to 1800 kcal per day for men. It contained approximately 50%-55% of the calories from carbohydrates, 25%-30% from fat, and 15%-20% from protein. The diet program was similar to the previous study by König et al[31].
Physical exercise was performed as a group session once a week during the first six weeks and twice a week thereafter. The group-based exercise sessions were led by a sport physiologist. Each participant was instructed to walk mainly at a specific heart rate reflecting 60%-75% of the individual estimated VO2max.
Magnetic resonance imaging (MRI) and magnetic resonance spectroscopy (MRS) measurements were performed with a 3T whole-body MRI system (Magnetom Trio a TIM system, Siemens Healthcare, Erlangen, Germany) using two six-channel body array coils for signal reception. Radiologists were blinded for treatment allocation. For abdominal fat-water imaging a previously optimised breath-hold spoiled 2D gradient echo protocol with four different echo times and a monopolar readout gradient was used[32]. Liver fat content and composition were measured by MRS using a single voxel PRESS (Point RESolved Spectroscopy) sequence with an echo time of TE = 35 ms. A cubic volume of interest (8 mL) was placed in the lateral part of the liver avoiding inclusion of larger blood vessels and subcutaneous fat. The MRS measurement was triggered with a 2D PACE (Prospective Acquisition Correction) navigator to minimize respiratory motion effects[33]. It was performed once with water suppression for a more robust lipid peak resolution and once without water suppression for acquisition of a water reference signal.
Reconstruction of fat and water images was performed using the graph cuts algorithm[34]. Segmentation of subcutaneous and internal adipose tissue (AT), including visceral AT, muscular fat, and bone marrow was conducted in the abdominal region with an active contour algorithm[35]. The classification of adipose tissue topography proposed by Shen et al. was adopted[36]. Fat quantification was performed as previously described by Ludwig et al[37].
The liver spectra were fitted and quantified with LCModel[32] using a dedicated analysis protocol for lipid detection in the liver. The lipid signal was modelled with peaks at [0.9, 1.3, 1.6, 2.1, 2.3, 2.8, 4.1, 4.3, 5.2, 5.3] ppm by LCModel.
Lipid peak quantification was considered reliable if the quantification error estimated by LCModel was smaller than 10%. Subjects were only included in the analysis of MRS-based parameters if all lipid resonances could be quantified with an estimated error margin of less than 10%.
The total fat signal (FS) was quantified as the sum of the integrated lipid peaks at 0.9 ppm, 1.3 ppm and 1.6 ppm, the water signal (WS) as the integrated water peak in the non-water-suppressed spectra. The integrated signals were corrected with the relaxation constants reported by Hamilton et al[38] using T2W = 23 ms for water and T2F = 62 ms for the lipid signal. Consequently, the intrahepatic lipid (IHL) content was calculated as: IHL = [FS*exp (TE/T2F)]/[FS*exp (TE/T2F) + WS*exp (TE/T2W)].
Lipid chain length, saturated lipid component, total unsaturated lipid component, and fraction of unsaturated lipids were determined as described by Ye et al[39,40].
For measuring body composition the technique of air displacement plethysmography (Bod Pod® device, Cosmed, Germany) was used[41,42]. Waist circumference was taken with a non-distensible tape measure following the anthropometric standardization guidelines[43].
The data collected upon enrolment and after 6 and 24 wk included the anthropometrics (i.e. body weight, waist and abdominal circumference), together with self-reported medical history, blood pressure, glucose, and serum lipids. Adipokines (i.e. leptin, adiponectin, resistin, vaspin, and fetuin A) were measured by commercially available ELISA tests (DSL Deutschland GmbH, Sinsheim, Germany). All other laboratory analyses were done in the central laboratory of the University of Freiburg Medical Center using clinical routine methods.
The primary study endpoint was the change in IHL content. Assuming an average IHL content of 23±7% based on the computations by Sullivan et al[44] , detecting a change of 10% with a power of 0.95 and an error of 0.05 at least eight participants were necessary. Evaluations of efficacy variables were analyzed in an exploratory manner. Descriptive statistical methods were used to analyze the variables. Results were expressed as median (interquartilrange IQR). To test the absolute and relative change of the parameters, a signed-rank test was used. All P values were two-sided and a P value of 0.05 or less was considered statistically significant. Bivariate associations between variables of interest were assessed by Spearman’s rank correlations (ρ). To evaluate potentially predictive variables of IHL content a multivariate regression with backward elimination of variables was performed. All statistical analyses were calculated using SPSS software (version 25.0.0).
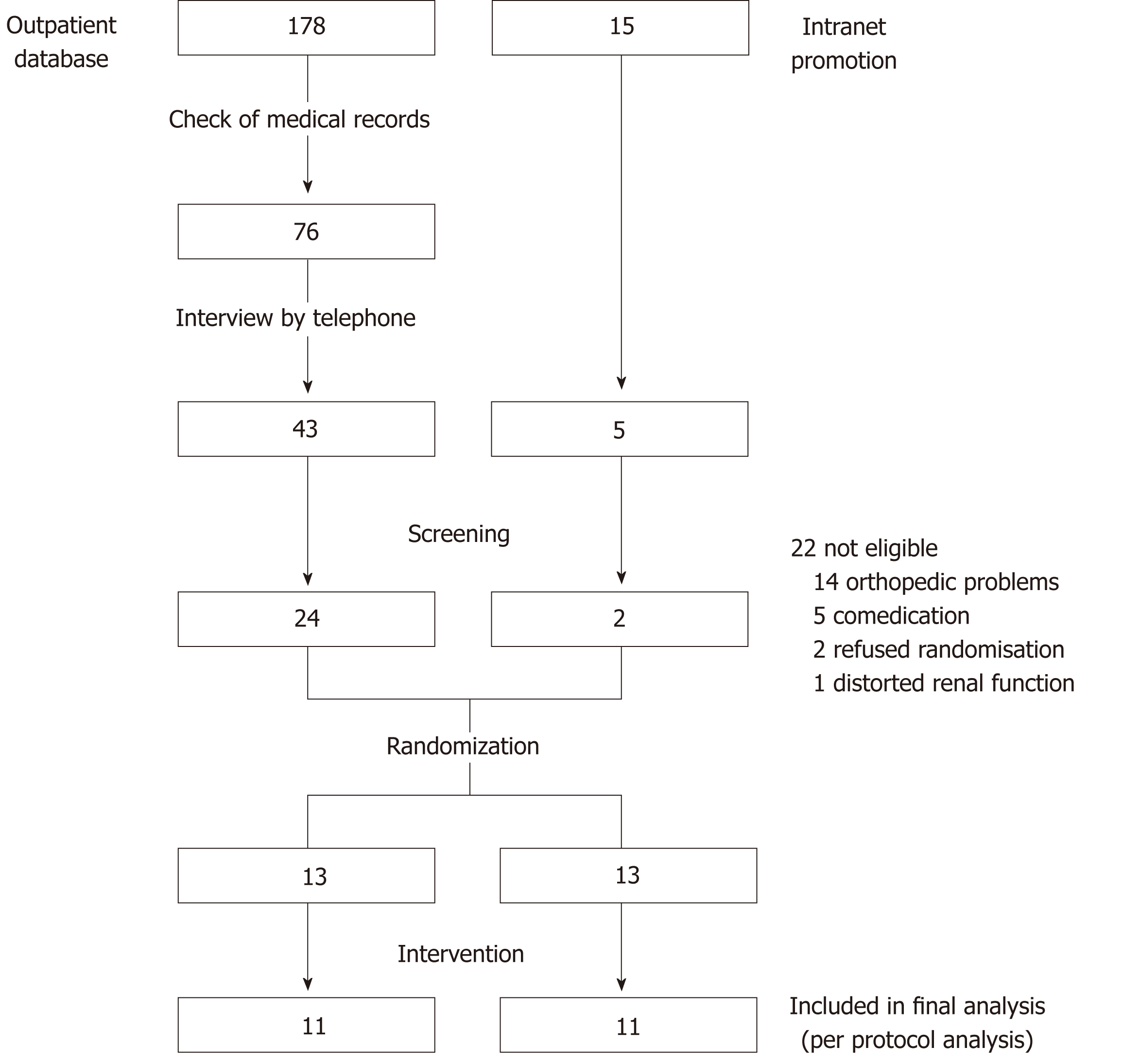
One hundred seventy-eight patient records with a diagnosis of NASH were reviewed from the outpatient database of the Department of Sports Medicine and Department of Gastroenterology and Hepatology (Figure 1). Seventy-six eligible subjects were contacted and interviewed concerning the study’s exclusion criteria, in which 43 patients were invited for screening. Fifteen patients responded to the study announcement via Intranet and five of them were invited for initial screening. Overall, 48 prospective subjects were invited for screening and this led to 26 eligible participants who were randomized to the study groups. A total of 22 patients (LC-G = 11, MR-G = 11) completed the study and attended at least 75% of the meetings/training sessions and consultation visits. All of these patients were evaluated at baseline (pre-intervention) and final visit (post-intervention). Four participants dropped out because of not having attended the necessary number of sessions. Baseline data showed that both groups were comparable in all parameters of interest (Table 1).
| Group | P value | ||||
| Meal replacement | Lifestyle change | ||||
| Median | IQR | Median | IQR | ||
| Sex (m/f) | 8/3 | 5/6 | |||
| Age (yr) | 57.0 | 8.0 | 54.0 | 14.0 | 0.27 |
| Height (m) | 1.80 | 0.1 | 1.74 | 0.2 | 0.44 |
| Weight (kg) | 101.1 | 30.5 | 99.5 | 11.1 | 0.37 |
| BMI (kg/m2) | 32.2 | 3.4 | 32.4 | 3.7 | 0.65 |
| Waist circumference (cm) | 115.0 | 18.0 | 109.0 | 12.0 | 0.17 |
| AST (U/L) | 42.0 | 20.0 | 37.0 | 18.0 | 0.33 |
| ALT (U/L) | 64.0 | 16.0 | 61.0 | 60.0 | 0.80 |
| Glucose (mg/dL) | 96.0 | 25.0 | 106.0 | 39.0 | 0.85 |
| HbA1c (%) | 5.7 | 1.0 | 5.8 | 1.0 | 0.80 |
| Creatinine (mg/dL) | 0.9 | 0.1 | 0.9 | 0.3 | 0.76 |
| Cholesterol (mg/dL) | 217.0 | 77.0 | 212.0 | 46.0 | 1.00 |
| HDL-Cholesterol (mg/dL) | 48.7 | 11.5 | 49.2 | 24.0 | 0.61 |
| LDL_Cholesterol (mg/dL) | 142.7 | 53.8 | 135.2 | 38.0 | 0.70 |
| Triglycerides (mg/dL) | 134.0 | 132.0 | 122.0 | 123.0 | 0.33 |
| Adiponectin (µg/mL) | 3.4 | 4.4 | 4.2 | 3.8 | 0.90 |
| Leptin (ng/mL) | 8.0 | 8.3 | 15.2 | 17.1 | 0.44 |
| Vaspin (mg/mL) | 0.2 | 0.2 | 0.2 | 0.4 | 0.07 |
| Fetuin A (g/L) | 0.4 | 0.1 | 0.4 | 0.2 | 0.95 |
| Resistin (ng/mL) | 4.4 | 2.6 | 4.0 | 2.6 | 0.37 |
| Max. Performance (Watt/kg) | 175.0 | 75.0 | 150.0 | 100.0 | 0.61 |
| Fat mass (kg) | 40.4 | 12.3 | 44.2 | 15.7 | 0.61 |
| Lean body mass (kg) | 59.6 | 12.3 | 55.8 | 15.7 | 0.61 |
| MRI subcutaneous fat (kg) | 9.2 | 4.4 | 9.5 | 4.1 | 0.70 |
| MRI internal fat (kg) | 6.9 | 3.8 | 5.5 | 1.6 | 0.12 |
| MRI total fat (kg) | 16.4 | 5.4 | 14.8 | 4.4 | 0.65 |
| Intrahepatic lipid content | 16.9 | 17.8 | 18.0 | 13.5 | 1.00 |
| Saturated lipid component | 15.5 | 8.5 | 15.0 | 5.1 | 0.78 |
| Total unsaturated lipid comp. | 4.7 | 3.8 | 2.8 | 1.5 | 0.16 |
| Fraction unsaturated lipids | 0.6 | 0.3 | 0.6 | 0.3 | 0.24 |
| Mean chain length | 30.8 | 6.5 | 27.0 | 5.8 | 0.11 |
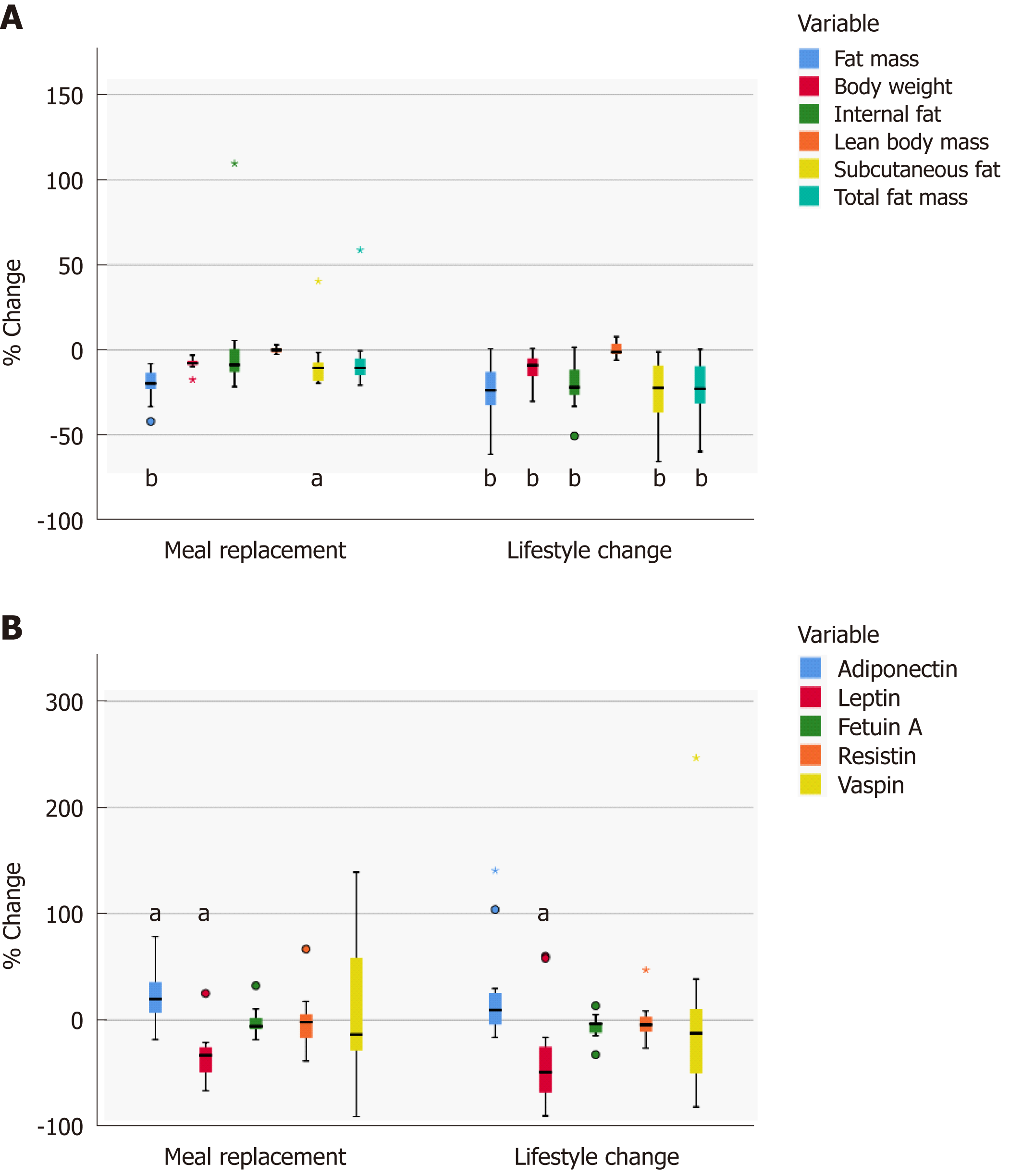
Within 6 wk both groups showed a significant reduction in body weight (MR-G: 101.1 (30.5) to 94.8 (23.7) kg; P < 0.01; LC-G: 99.5 (11.1) kg to 83.3 (26.4) kg, P < 0.01). As shown in Table 2, after 24 wk the MR-G had reduced mean body weight of 6.4 (3.6) kg and the LC-G 9.1 (10.4) kg (P = ns between the groups). BMI was reduced from 32.2 (3.4) to 29.6 (3.3) in the MR-G and from 32.4 (3.7) to 29.3 (4.5) in the LC-G. In the MR-G waist circumference was more reduced in comparison to the LC-G. Changes were comparable between both groups, resulting in statistically significant lower values at the final visit (P < 0.001). The BodPod analysis at baseline and final visit showed a stable lean body mass in both groups, whereas body fat mass was reduced significantly in both interventions (Figure 2A).
| Change in | Group | P between groups | |||
| Meal replacement | Lifestyle change | ||||
| Median | IQR | Median | IQR | ||
| Weight (kg) | -6.4 | 3.6 | -9.1b | 10.4 | 0.48 |
| BMI (kg/m2) | -2.3b | 1.5 | -3.0b | 3.4 | 0.48 |
| Waist circumference (cm) | -4.0b | 5.0 | -7.0b | 10.5 | 0.65 |
| AST (U/L) | -4.0a | 14.0 | -15.0a | 14.0 | 0.30 |
| ALT (U/L) | -8.0b | 22.0 | -18.0b | 35.0 | 0.19 |
| Glucose (mg/dL) | -10.0 | 20.0 | -20.0a | 31.0 | 0.70 |
| HbA1c (%) | -0.1 | 0.4 | -0.3a | 0.3 | 0.65 |
| Creatinine (mg/dL) | 0.0 | 0.1 | 0.0 | 0.1 | 0.56 |
| Cholesterol (mg/dL) | -8.0 | 29.0 | -3.0 | 44.5 | 0.99 |
| HDL-Cholesterol (mg/dL) | 2.9 | 10.1 | 1.4 | 11.1 | 0.40 |
| LDL-Cholesterol (mg/dL) | 3.9 | 22.1 | 6.8 | 29.0 | 0.61 |
| Triglycerides (mg/dL) | -43.0a | 137.0 | -9.0 | 74.5 | 0.65 |
| Adiponectin (µg/mL) | 0.3a | 1.1 | 0.1 | 2.9 | 0.48 |
| Leptin (ng/mL) | -2.4a | 3.5 | -12.8a | 15.1 | 0.27 |
| Vaspin (mg/mL) | 0.0 | 0.1 | 0.0 | 0.3 | 0.70 |
| Fetuin A (g/L) | 0.0 | 0.1 | 0.0 | 0.0 | 0.85 |
| Resistin (ng/mL) | -0.1 | 2.0 | 0.2 | 1.3 | 0.95 |
| Max. Performance (Watt/kg) | 0.0 | 29.8 | 6.3a | 21.9 | 0.03 |
| Fat mass (kg) | -6.0b | 4.2 | -9.3b | 11.1 | 0.30 |
| Lean body mass (kg) | 0.0 | 1.7 | -0.7 | 2.0 | 0.95 |
| MRI subcutaneous fat (kg) | -1.1a | 0.9 | -2.0b | 3.1 | 0.06 |
| MRI internal fat (kg) | -0.5 | 0.9 | -0.9b | 1.1 | 0.09 |
| MRI total fat (kg) | -1.6 | 2.2 | -3.0b | 4.2 | 0.06 |
| Intrahepatic lipid content | -10.3b | 8.4 | -11.8a | 15.4 | 0.20 |
| Saturated lipid component | -5.1 | 7.0 | -2.0a | 4.1 | 0.92 |
| Total unsaturated lipid comp. | -2.0b | 1.0 | 0.2 | 4.9 | 0.05 |
| Fraction unsaturated lipids | -0.1 | 0.2 | 0.0 | 0.3 | 0.61 |
| Mean chain length | -8.0a | 6.2 | -1.4 | 10.0 | 0.03 |
ALT and AST values decreased in both treatment regimens, the change being more pronounced in the LC-G (Table 2). Both changes were significant within each group (P < 0.05) and no significant difference was found between the two groups. The relative change in ALT was correlated with the relative change in abdominal fat (ρ = 0.70; P < 0.01), subcutaneous fat (ρ = 0.72, P < 0.01), internal fat (ρ = 0.65; P < 0.01), and change in AST (ρ = 0.96; P < 0.01). There was a weaker correlation to relative change in body fat mass (ρ = 0.52; P < 0.05) and to relative change in waist circumference (ρ = 0.48; P < 0.05).
Cholesterol did not significantly decrease in both groups, whereas there was a significant decrease in triglycerides only in the MR-G. HDL-cholesterol showed a slight but non-significant increase in both groups, while LDL-cholesterol was nearly unchanged (both P = n.s.). Fasting glucose and HbA1c-values were reduced in both groups, this reduction was more pronounced in the LC-G. However, the decrease did not differ significantly between groups. Serum creatinine values were initially comparable and were unchanged in both groups.
In terms of adipokines, adiponectin showed a slight increase in both groups, whereas leptin showed a significant decrease over the 24-wk study period in both groups. Vaspin, resistin, and fetuin A did not show significant changes over the period of 24 wk (Figure 2B).
Both interventions reduced the total abdominal fat as estimated by MRI. However, it was significantly reduced only with lifestyle intervention (MR-G: 16.4 (5.4) kg to 15.0 (5.4) kg; P = n.s., LC-G: 14.8 (4.4) kg to 13.4 (2.3) kg; P < 0.05; difference between groups P = 0.06, Figure 2A). There was significant reduction of subcutaneous fat in both groups, being more pronounced in the lifestyle intervention group (P = 0.06 between groups). Furthermore, the LC-G lost more internal fat than the MR-G, however this difference was not statistically significant between the groups. The ratio of relative internal fat loss to subcutaneous fat loss was comparable in both groups (MR-G: 0.42, LC-G: 0.36; P = n.s.).
Adiponectin and leptin showed weak correlations to total abdominal fat mass as estimated by MRI (adiponectin: ρ = 0.24; leptin: ρ = 0.60) or Bodpod device (adiponectin: ρ = 0.58; Leptin: ρ = 0.88), waist circumference (adiponectin: ρ = -0.01; leptin: ρ = 0.06) or BMI (adiponectin: ρ = -0.09; leptin: ρ = 0.33). Furthermore, fetuin A, vaspin, and resistin showed no relevant correlations to such parameters (ρ < 0.2 for all). However, adiponectin changes were inversely related to changes in body weight (ρ = -0.25), fat mass (ρ = -0.30), reduction in waist circumference (ρ = -0.13) and total abdominal fat (ρ = -0.13). Leptin changes were correlated to changes in body weight (ρ = 0.65), fat mass (ρ = 0.63), waist circumference (ρ = 0.39) and total abdominal fat (ρ = 0.49).
The baseline saturated lipid component was correlated with waist circumference (ρ = 0.4; P = n.s.), as well as with subcutaneous fat (ρ = 0.44; P < 0.01), total abdominal fat (ρ = 0.54; P < 0.01) and body fat mass as estimated by the BodPod device (ρ = 0.57; P < 0.01). It was not correlated with internal fat (ρ = 0.07; P = n.s.). By multivariate regression analysis IHL content was negatively correlated to total unsaturated lipid component and positively correlated to mean chain length. The fraction of unsaturated lipids and the total unsaturated lipid compound did not significantly predict IHL and were eliminated from the model. In a second model IHL content could not be predicted by total abdominal fat measured by MRI, waist to hip ratio, fat mass measured by BodPod, waist circumference or weight.
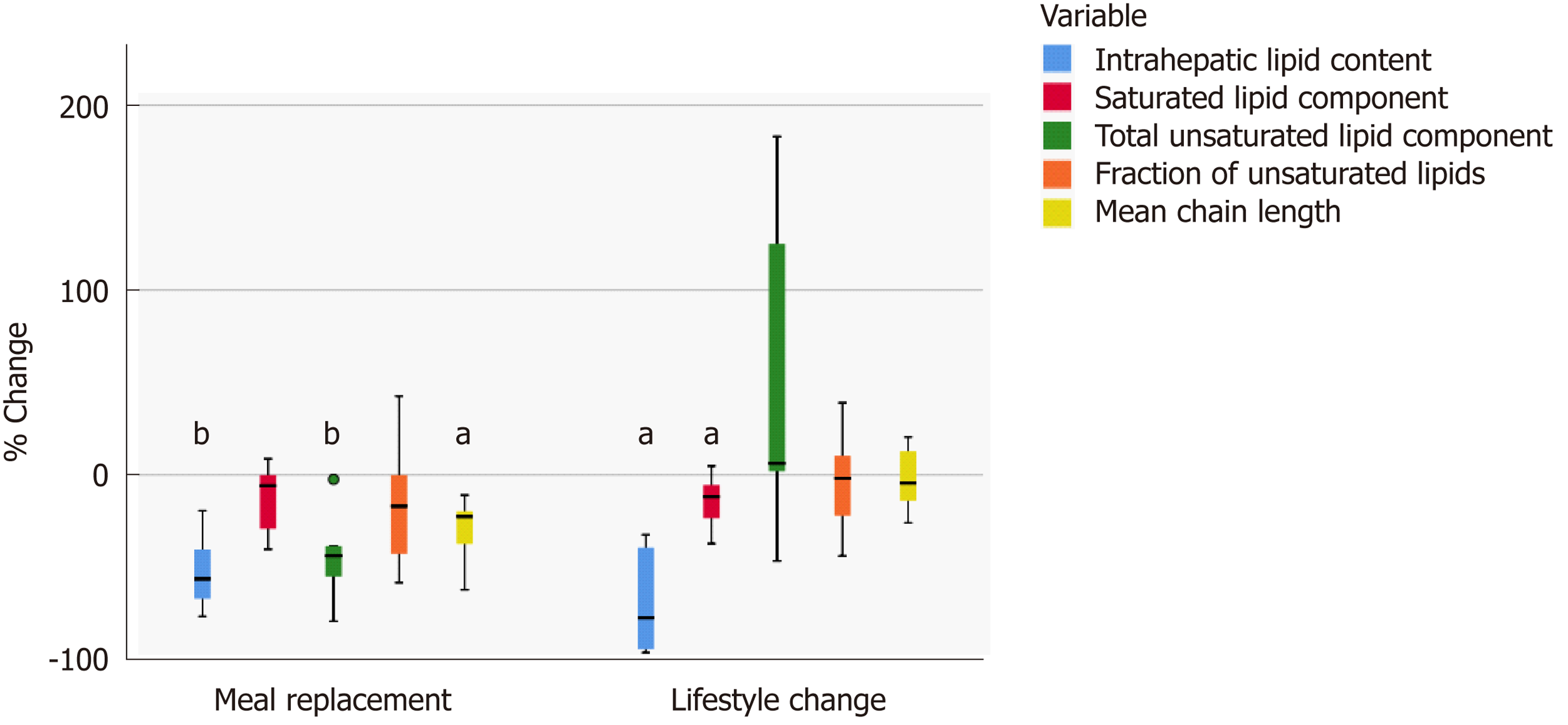
In both intervention groups there was a highly significant reduction of liver fat content (MR-G: -56.2 (30.5)%; P < 0.01; LC-G: -77.2 (57.8)%; P < 0.05 Figure 3), being correlated to weight change (ρ = 0.77 in MR-G and ρ = 0.88 in LS-G).
The IHL composition was not differentiable in all cases since in some spectra insufficient spectral quality did not allow for accurate quantification of all underlying resonances. Therefore, in a subgroup intrahepatic lipids were analyzed and characterized with regard to IHL component, saturated lipid component, and fraction of unsaturated lipids. Furthermore, the mean chain length of intrahepatic lipids was estimated. Changes of the saturated lipid component could be calculated in 15 participants and changes of the unsaturated lipid component in 16 participants, respectively.
The IHL content and the saturated lipid component decreased during the intervention in both groups (MR-G: IHL content: 16.9 (17.8) to 6.7 (10.2), P < 0.01; LC-G: 18.0 (13.5) to 5.5 (10.2); P < 0.05; MR-G: saturated lipid component: 15.5 (8.5) to 14.3 (2.6), P = n.s.; LC-G: 15.0 (5.2) to 13.0 (5.5), P < 0.05, Figure 3). The fraction of unsaturated lipids showed a decrease only in the meal replacement group (MR-G: 0.6 (0.3) to 0.48 (0.38), P = n.s.; LS-G: 0.6 (0.3) to 0.6 (0.3), P = n.s.). Mean chain length was significantly reduced only in the meal-replacement group [MR-G: 30.8 (6.5) to 25.5 (7.3), P < 0.05; LC-G: 27.0 (5.8) to 31.4 (13.3), P = n.s.] (Figure 3).
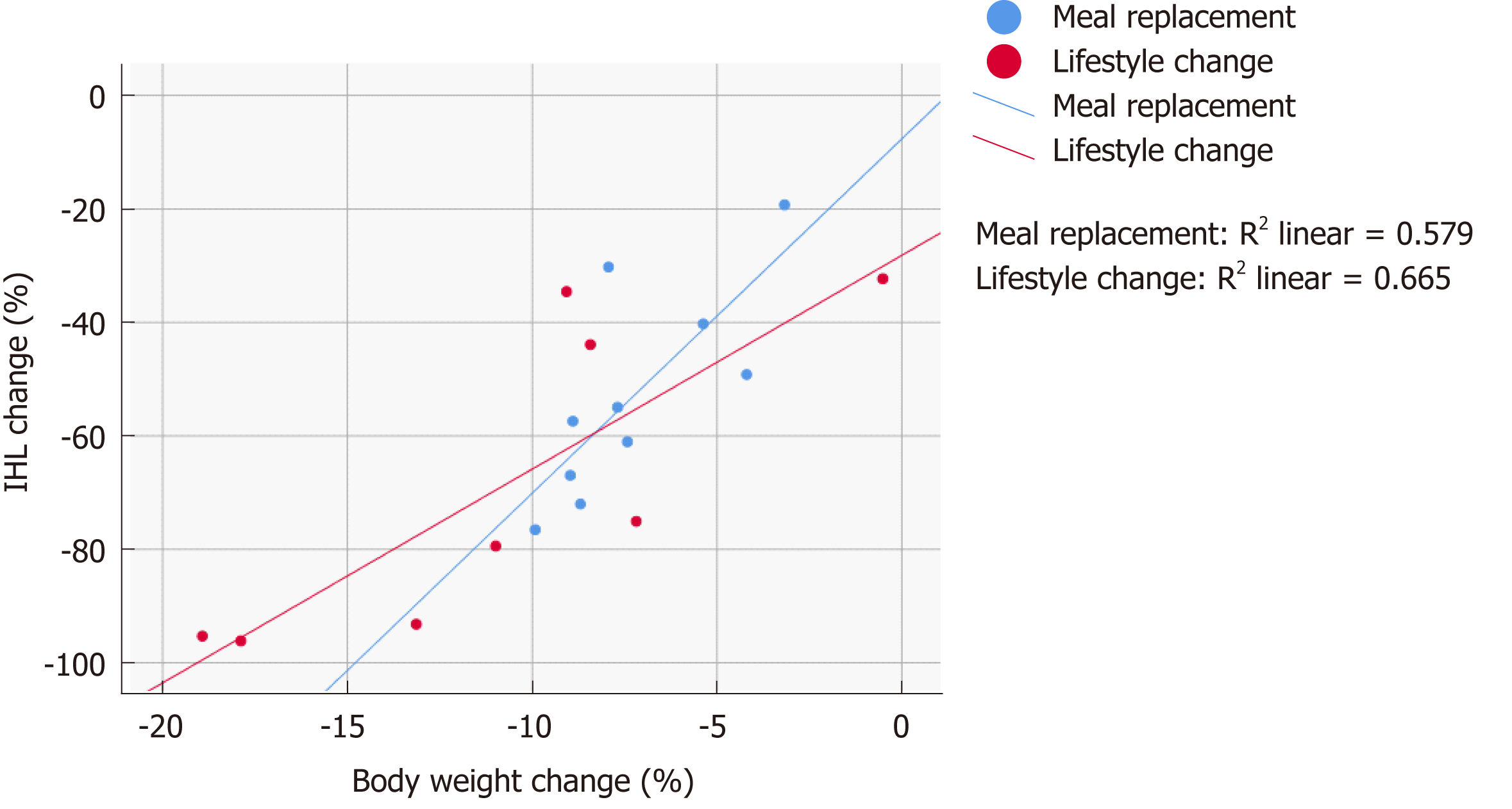
The relative change in IHL content was correlated to relative weight change in both groups (MR-G: ρ = 0.77, LC-G: ρ = 0.88), as well as to relative changes in internal fat (MR-G: ρ = 0.67, LC-G: ρ = 0.81), fat mass (MR-G: ρ = 0.77, LC-G: ρ = 0.71), and waist circumference (MR-G: ρ = 0.46, LC-G: ρ = 0.83). The relative change in IHL content as a function of relative weight loss was slightly more pronounced in the MR-G (Figure 4).
The changes in the IHL were studied in relation to changes in adipokines. The latter correlate to the change in IHL content, being more apparent in the LC-G. Adiponectin rose as IHL content decreased, while leptin declined with a reduction of IHL content. Resistin, vaspin and fetuin A showed only weak correlations to adipokines.
Maximum performance in ergometer testing was improved only in the LC-G, with an increase of maximum cycling power. In terms of the measured muscle mass (fat free mass, ffm) by Bodpod®, only the LC-G showed a significant increase in performance (MR-G: 2.9 (0.6) W/kg ffm to 2.7 (0.4) W/kg ffM, P = n.s.; LC-G: 2.8 (0.9) W/kg ffm to 3.2 (0.8) W/kg ffm; P < 0.05).
This study aimed to compare a meal replacement regimen with lifestyle change as intervention for patients with NASH. The results showed that based on the parameters of interest (i.e., IHL content, body composition, metabolic/biochemical parameters, and anthropometrics) both interventions yielded comparable results specifically in terms of reducing body fat mass, IHL content, and hepatic inflammation.
The reduction of IHL content in this study was more pronounced than in another intervention study using mainly aerobic training programs, with a mobilization of liver fat of 30.2% in the exercise only group and 49.8% in the diet and exercise group[44]. A recent systematic review suggested that an exercise program at 70% VO2max is ideal for mobilizing fat from liver among NAFLD patients[45]. The exercise program used in this study was in accordance with such recommendation and was well tolerated by all of the participants. Studies comparing different exercise programs additive to a dietary intervention demonstrated that the effect of physical activity was minor compared to that of a reduction of caloric intake or change in macronutrients[46-49]. The lifestyle education program used in this study aimed to motivate participants to perform at least 150 min (but preferably 300 min) of moderate-intensity physical activity per week. Participants had to attend two exercise sessions per week, doing sports at an intensity based on the suggested heart rate reflecting 60%-65% VO2max which had been tested individually.
The nutritional counselling encouraged participants to reduce caloric intake and motivated them to engage in sports. Due to this intensive program the reduction in body weight was more pronounced in the LC-G than among the participants of the MR-G. However, metabolic changes and changes in IHL content were comparable.
Participants of the MR-G received instructions on the meal replacement regimen in a group session at the beginning of the study and were further advised individually after 6 wk. Both treatment strategies led to a loss of fat mass while preserving muscle mass, a desirable goal of weight reduction interventions that had been previously described[19]. The increased mean metabolic turnover in the LC-G was about 5.7 MET/wk, corresponding to a caloric increment of 430 kcal/wk. Increasing physical activity is indispensable in a long-term weight control program[50]. In a period of one year these behavioral changes may result in a 3.4 kg loss in body weight. However, it has been shown that a dietary intervention has long-term effects in liver fat and metabolism despite body weight regain[51].
Both groups showed a reduction in cholesterol and triglycerides, as well as an increase in HDL-cholesterol - however, only the decrease in triglycerides in the MR-G was significant. Soy protein with intact isoflavones may decrease total cholesterol, LDL-cholesterol and triacylglycerols and increase HDL-cholesterol[52,53], mimicking the effects of exercise on lipid parameters. The protein content of the nutrition appeared to have a distinct effect on liver fat. An isocaloric protein rich diet, high in animal or plant protein, is able to reduce liver fat by 36%-48%[54]. In terms of body weight change, the MR-G lost more IHL content per loss of body weight than the LC-G. Furthermore, the main weight reduction in the LC-G was initiated through caloric restriction, thus this might have influenced the results. However, physical exercise may lead to a decrease in the intramyocellular lipid content that has been linked to insulin sensitivity[49].
In this study, fasting glucose levels and HbA1c levels decreased similarly in both groups, thus both interventions seemed to be equally effective in improving insulin sensitivity. As NASH is associated with cardiovascular morbidity and mortality[55-58], in addition to an improved glucose tolerance, an improvement in physical fitness and muscular performance is supposed to be beneficial. Expectedly, physical fitness was improved only in the LC-G.
The IHL content was quantified by MRS. With this technique not only the amount of hepatic lipids can be determined with high accuracy[59] but also the mean chain length and percentage of saturated as well as unsaturated lipids may be estimated. However, it should be noted that the calculation of these lipid composition parameters is subject to systematic errors mainly arising from different T2 relaxation of the underlying resonances which cannot be corrected. Therefore, the values calculated in this study should not be regarded as absolute quantities but rather as correlates of the corresponding parameters. With both interventions the IHL content was reduced by more than 50%. The higher reduction in the LC-G was due to a higher extent in body weight reduction in this group. The quality of IHL was more influenced by the meal replacement. In this group the total unsaturated lipid component decreased significantly as did the mean chain length.
A comparable reduction in liver fat was seen in a subgroup of adults with type 2 diabetes examined in the Look AHEAD trial (-50,8% in the lifestyle intervention group)[60] and in patients with NAFLD after gastric banding surgery (-50%)[61]. An exercise intervention in patients with NAFLD led to a weight reduction of -2.5 kg and a change in intrahepatic triglyceride content of 48%[62]. Other interventions have not reduced liver fat content by a similar percentage[7,44,48,55]. An aerobic exercise training that did not lead to a change in BMI led to a decrease in the IHL content of 10.3% ± 4.6%[44], while the combination of aerobic exercise and resistance training led to a reduction of IHL content of 16% ± 24%[63]. Four weeks of aerobic cycling exercise program which significantly reduced visceral adipose tissue volume by 12% without changing BMI was able to decrease IHL by 21%[7].
The adipokines showed comparable changes in both groups. There was a marked decrease in leptin with both interventions while adiponectin, vaspin, resistin, and fetuin A showed no significant changes over the 24-wk period. Leptin correlates with severity of steatosis and BMI[64], while fetuin A expression is more prominent in NASH[65]. Both showed no significant changes in both interventions. However, the relative changes in leptin and fetuin A were correlated to the changes in saturated lipid component in the LC-G. Likewise, the study demonstrated no significant changes in the levels of resistin, which is linked to abdominal adiposity and elevated triglycerides[29]. Vaspin which is associated to obesity and insulin resistance[28] also showed no significant changes. In contrast, there is a weak correlation to changes in saturated and unsaturated lipid components. It can be concluded that not only the IHL component is of importance, but also the proportion of saturated and unsaturated lipids since these correlate to adipokines. This may explain why some authors report similar levels among NASH patients and controls in contrast to others reporting higher levels among NAFLD patients[66].
The intervention-induced mobilization of intrahepatic fat was different in both groups. With a soy-based meal replacement, saturated and unsaturated lipids were reduced in a comparable amount, whereas lifestyle intervention preferentially led to a loss of saturated liver fat. Furthermore, the mean chain length was markedly reduced only in the MR-G. The changes in the adipokines adiponectin and leptin were correlated to changes in saturated and unsaturated intrahepatic fats, both in the opposite manner. The alterations of liver fat quality were different between both groups, as shown in Figure 3. The results of this study demonstrate that interventions may not only lead to a reduction of liver fat, but also to a change of liver fat quality. Several studies proved a beneficial effect of a dietary approach to an increase in intrahepatic unsaturated fat in NASH. In a model of rats with NASH the administration of omega-3 polyunsaturated fatty acids improved the spectrum of adipokines significantly[67]. In patients with fatty liver disease the hepatic fat content was associated with high energy, high fat, and high saturated fat intake[68]. By a modulation of fat consumption with increased intake of omega-3 polyunsaturated fatty acids in NASH adipokines and markers of hepatic inflammation were changed positively[69]. On the other hand, hepatic n-3 polyunsaturated fatty acid depletion promotes steatosis and insulin resistance in mice and humans[70]. Therefore, a non-invasive analysis of hepatic fat quality may identify a group of NASH patients which could benefit most from supplementation.
In terms of study limitations, the gold standard of assessing hepatic inflammation and fibrosis, as well as lipid content is still histopathological analysis. Presently, 1H-MRI analysis is a standard method to quantify hepatic steatosis. However, it is not able to assess inflammation or fibrosis. For evaluating fibrosis the non-invasive Fibroscan is conventionally used. In the present study, the focus was on changes in body composition and related IHL changes. Moreover, it was not possible to ascertain whether the caloric restriction in the MR-Group or a specific effect of the soy-yogurt-honey preparation led to the different composition of liver fat. However, our study once more confirmed, that with a supplementation of high quality proteins a significant weight reduction without loss of muscle mass is achievable. Finally, the study sample was not large enough to analyze study participant subgroups (i.e., sex and age groups). The small sample size of the study was partly determined by the exclusion criteria, ruling out patients taking hormonal replacement/substitution, anti-diabetic drugs or lipid-lowering drugs.
The comparability of both intervention strategies suggests the need for further studies to evaluate the course of hepatic fibrosis in patients with NASH succeeding in a weight reduction program. For physicians managing NASH patients, this study suggests that a soy protein-based meal replacement therapy may be an alternative to a therapeutic lifestyle change, considering the patient’s demands and circumstances. The different changes in hepatic lipid characteristics in each intervention need to be further evaluated.
In conclusion, comprehensive lifestyle intervention and meal replacement regimen had comparable effects in terms of weight reduction, body and liver fat content, and markers of hepatic inflammation among patients with NASH. Lifestyle change may be the ideal approach associated with improved physical fitness and muscular performance, while meal replacement could be an alternative intervention depending on patient’s characteristics, level of motivation, and other life circumstances. The two described approaches changed the amount and quality of IHL content with regard to fatty acid chain length and ratio of saturated/unsaturated lipids. The impact of these findings needs further investigation.
Non-alcoholic steatohepatitis (NASH) is one of the leading causes of chronic liver disease in western countries. The ideal approach to reduce hepatic inflammation and liver fat content is not found yet. Dietary restrictions and physical activity have been shown to be effective, however there is no gold standard established so far.
Many different dietary approaches may be effective in weight reduction. We have shown that by meal replacement therapy with a high-quality soy protein supplementation as well as by comprehensive lifestyle change a weight reduction without loss of muscle mass is achievable. Both interventions can reduce fat mass and liver fat mass. However, blood lipids are changed in different ways with these two interventions. Now we wanted to study whether liver fat quality is differently affected with either intervention.
The main questions of this study were: is there a correlation between loss of liver fat and reduction in body fat, and is one intervention superior to the other in this respect? Is it possible to analyze liver fat quality, and is there a difference in changes in liver fat quality between the two therapeutic interventions?
For body composition analysis a Bod pod device was used. Liver fat content was measured by magnetic resonance imaging. For analysis of liver fat quality a magnetic resonance spectroscopy protocol was adapted to quantify the mean chain length and grade of saturation of liver fat. For meal replacement therapy we used a commercially available product based on a soy-yogurt-honey preparation. The lifestyle intervention program consisted of guided exercise sessions orientated on individual exercise capacity and dietary counselling.
Both groups significantly reduced body mass index, fat mass and liver fat content. The lifestyle intervention group showed a tendency for greater weight loss. In both groups ALT and AST declined significantly. Triglycerides significantly decreased only in meal replacement group. With respect to liver fat quality the grade of saturation and mean chain length of hepatic fatty acids were quantifiable in a subset of participants. Total unsaturated lipids and mean chain length were significantly reduced only by meal replacement.
With both interventions body fat and liver fat content were significantly reduced. Though the participants tended to lose more weight by lifestyle intervention the reduction of liver fat was comparable in both groups. Thus, for the reduction in liver fat a meal replacement strategy could be more effective in relation to body weight loss than a lifestyle intervention. This study confirms the finding of preserving muscle mass during a weight reduction period once high quality protein supplementation or physical activity is added in a guided and supervised manner. The pronounced reduction of serum triglycerides is attributed to specific soy properties. Given the study protocol further analysis of liver fat in humans by magnetic resonance spectroscopy was possible. Both interventions had different effects on liver fat quality.
In conclusion, with both approaches a significant weight loss and loss of intrahepatic fat content is achievable. Reduction in fat content is accompanied by a decline in hepatic inflammation, reflected in reduction of aminotransferases. In patients with NASH both therapeutic interventions can be advocated in order to reduce liver fat content and hepatic inflammation.
Both interventions had distinct effects on liver fat quality. The reduction of serum triglycerides is a known effect of soy protein supplementation thus, we hypothesize that the different changes in liver fat quality were also related to soy protein intake. However, the physiologic consequence of a shortened chain length or of a different grade of saturation in hepatic lipids is not clear yet. This has to be addressed in future investigations. Furthermore, our research results demonstrated the practicability of magnetic resonance spectroscopy to analyze liver fat quality. The validity has to be confirmed by further studies.
Manuscript source: Invited manuscript
Specialty type: Gastroenterology and hepatology
Country of origin: Germany
Peer-review report classification
Grade A (Excellent): A
Grade B (Very good): B, B
Grade C (Good): 0
Grade D (Fair): 0
Grade E (Poor): 0
P- Reviewer: Chatzigeorgiou A, Skrypnyk I, Vespasiani-Gentilucci U S- Editor: Gong ZM L- Editor: A E- Editor: Huang Y
| 1. | Zelber-Sagi S, Ratziu V, Oren R. Nutrition and physical activity in NAFLD: an overview of the epidemiological evidence. World J Gastroenterol. 2011;17:3377-3389. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in CrossRef: 210] [Cited by in RCA: 225] [Article Influence: 16.1] [Reference Citation Analysis (1)] |
| 2. | Definition Facts of NAFLD & NASH | NIDDK [Internet]. Natl. Inst. Diabetes Dig. Kidney Dis. [cited 2017 Aug 16]. Available from: https://www.niddk.nih.gov/health-information/liver-disease/nafld-nash/definition-facts. |
| 3. | Wong RJ, Cheung R, Ahmed A. Nonalcoholic steatohepatitis is the most rapidly growing indication for liver transplantation in patients with hepatocellular carcinoma in the U.S. Hepatology. 2014;59:2188-2195. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 520] [Cited by in RCA: 586] [Article Influence: 53.3] [Reference Citation Analysis (0)] |
| 4. | Church TS, Kuk JL, Ross R, Priest EL, Biltoft E, Blair SN. Association of cardiorespiratory fitness, body mass index, and waist circumference to nonalcoholic fatty liver disease. Gastroenterology. 2006;130:2023-2030. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 184] [Cited by in RCA: 196] [Article Influence: 10.3] [Reference Citation Analysis (0)] |
| 5. | Perseghin G, Lattuada G, De Cobelli F, Ragogna F, Ntali G, Esposito A, Belloni E, Canu T, Terruzzi I, Scifo P, Del Maschio A, Luzi L. Habitual physical activity is associated with intrahepatic fat content in humans. Diabetes Care. 2007;30:683-688. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 231] [Cited by in RCA: 225] [Article Influence: 12.5] [Reference Citation Analysis (0)] |
| 6. | McMillan KP, Kuk JL, Church TS, Blair SN, Ross R. Independent associations between liver fat, visceral adipose tissue, and metabolic risk factors in men. Appl Physiol Nutr Metab. 2007;32:265-272. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 36] [Cited by in RCA: 35] [Article Influence: 1.9] [Reference Citation Analysis (0)] |
| 7. | Johnson NA, Sachinwalla T, Walton DW, Smith K, Armstrong A, Thompson MW, George J. Aerobic exercise training reduces hepatic and visceral lipids in obese individuals without weight loss. Hepatology. 2009;50:1105-1112. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 418] [Cited by in RCA: 440] [Article Influence: 27.5] [Reference Citation Analysis (0)] |
| 8. | Rector RS, Uptergrove GM, Morris EM, Borengasser SJ, Laughlin MH, Booth FW, Thyfault JP, Ibdah JA. Daily exercise vs. caloric restriction for prevention of nonalcoholic fatty liver disease in the OLETF rat model. Am J Physiol Gastrointest Liver Physiol. 2011;300:G874-G883. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 109] [Cited by in RCA: 119] [Article Influence: 8.5] [Reference Citation Analysis (0)] |
| 9. | Zelber-Sagi S, Nitzan-Kaluski D, Goldsmith R, Webb M, Zvibel I, Goldiner I, Blendis L, Halpern Z, Oren R. Role of leisure-time physical activity in nonalcoholic fatty liver disease: a population-based study. Hepatology. 2008;48:1791-1798. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 222] [Cited by in RCA: 224] [Article Influence: 13.2] [Reference Citation Analysis (0)] |
| 10. | Bae JC, Suh S, Park SE, Rhee EJ, Park CY, Oh KW, Park SW, Kim SW, Hur KY, Kim JH, Lee MS, Lee MK, Kim KW, Lee WY. Regular exercise is associated with a reduction in the risk of NAFLD and decreased liver enzymes in individuals with NAFLD independent of obesity in Korean adults. PLoS One. 2012;7:e46819. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 124] [Cited by in RCA: 129] [Article Influence: 9.9] [Reference Citation Analysis (0)] |
| 11. | Conjeevaram HS, Tiniakos DG. Editorial: Exercise for NAFLD: does intensity matter? Am J Gastroenterol. 2011;106:470-475. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 8] [Cited by in RCA: 8] [Article Influence: 0.6] [Reference Citation Analysis (0)] |
| 12. | Ueno T, Sugawara H, Sujaku K, Hashimoto O, Tsuji R, Tamaki S, Torimura T, Inuzuka S, Sata M, Tanikawa K. Therapeutic effects of restricted diet and exercise in obese patients with fatty liver. J Hepatol. 1997;27:103-107. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 426] [Cited by in RCA: 404] [Article Influence: 14.4] [Reference Citation Analysis (0)] |
| 13. | Puri P, Baillie RA, Wiest MM, Mirshahi F, Choudhury J, Cheung O, Sargeant C, Contos MJ, Sanyal AJ. A lipidomic analysis of nonalcoholic fatty liver disease. Hepatology. 2007;46:1081-1090. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 914] [Cited by in RCA: 1042] [Article Influence: 57.9] [Reference Citation Analysis (1)] |
| 14. | Wilfred de Alwis NM, Day CP. Genes and nonalcoholic fatty liver disease. Curr Diab Rep. 2008;8:156-163. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 54] [Cited by in RCA: 53] [Article Influence: 3.1] [Reference Citation Analysis (0)] |
| 15. | Jensen MD, Ryan DH, Apovian CM, Ard JD, Comuzzie AG, Donato KA, Hu FB, Hubbard VS, Jakicic JM, Kushner RF, Loria CM, Millen BE, Nonas CA, Pi-Sunyer FX, Stevens J, Stevens VJ, Wadden TA, Wolfe BM, Yanovski SZ, Jordan HS, Kendall KA, Lux LJ, Mentor-Marcel R, Morgan LC, Trisolini MG, Wnek J, Anderson JL, Halperin JL, Albert NM, Bozkurt B, Brindis RG, Curtis LH, DeMets D, Hochman JS, Kovacs RJ, Ohman EM, Pressler SJ, Sellke FW, Shen WK, Smith SC, Tomaselli GF; American College of Cardiology/American Heart Association Task Force on Practice Guidelines; Obesity Society. 2013 AHA/ACC/TOS guideline for the management of overweight and obesity in adults: a report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines and The Obesity Society. Circulation. 2014;129:S102-S138. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 1717] [Cited by in RCA: 2042] [Article Influence: 170.2] [Reference Citation Analysis (0)] |
| 16. | Paschos P, Paletas K. Non alcoholic fatty liver disease and metabolic syndrome. Hippokratia. 2009;13:9-19. [PubMed] |
| 17. | Nguyen-Duy TB, Nichaman MZ, Church TS, Blair SN, Ross R. Visceral fat and liver fat are independent predictors of metabolic risk factors in men. Am J Physiol Endocrinol Metab. 2003;284:E1065-E1071. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 188] [Cited by in RCA: 181] [Article Influence: 8.2] [Reference Citation Analysis (0)] |
| 18. | Hayashi N, Miyati T, Minami T, Takeshita Y, Ryu Y, Matsuda T, Ohno N, Hamaguchi T, Kato K, Takamura T, Matsui O. Quantitative analysis of hepatic fat fraction by single-breath-holding MR spectroscopy with T₂ correction: phantom and clinical study with histologic assessment. Radiol Phys Technol. 2013;6:219-225. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 15] [Cited by in RCA: 15] [Article Influence: 1.2] [Reference Citation Analysis (0)] |
| 19. | Deibert P, König D, Schmidt-Trucksaess A, Zaenker KS, Frey I, Landmann U, Berg A. Weight loss without losing muscle mass in pre-obese and obese subjects induced by a high-soy-protein diet. Int J Obes Relat Metab Disord. 2004;28:1349-1352. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 82] [Cited by in RCA: 73] [Article Influence: 3.5] [Reference Citation Analysis (0)] |
| 20. | König D, Deibert P, Frey I, Landmann U, Berg A. Effect of meal replacement on metabolic risk factors in overweight and obese subjects. Ann Nutr Metab. 2008;52:74-78. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 36] [Cited by in RCA: 36] [Article Influence: 2.1] [Reference Citation Analysis (0)] |
| 21. | Deibert P, König D, Vitolins MZ, Landmann U, Frey I, Zahradnik HP, Berg A. Effect of a weight loss intervention on anthropometric measures and metabolic risk factors in pre- versus postmenopausal women. Nutr J. 2007;6:31. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 55] [Cited by in RCA: 61] [Article Influence: 3.4] [Reference Citation Analysis (0)] |
| 22. | Kadowaki T, Yamauchi T, Kubota N, Hara K, Ueki K, Tobe K. Adiponectin and adiponectin receptors in insulin resistance, diabetes, and the metabolic syndrome. J Clin Invest. 2006;116:1784-1792. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1945] [Cited by in RCA: 2061] [Article Influence: 108.5] [Reference Citation Analysis (0)] |
| 23. | Kelesidis T, Kelesidis I, Chou S, Mantzoros CS. Narrative review: the role of leptin in human physiology: emerging clinical applications. Ann Intern Med. 2010;152:93-100. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 470] [Cited by in RCA: 453] [Article Influence: 30.2] [Reference Citation Analysis (0)] |
| 24. | Polyzos SA, Aronis KN, Kountouras J, Raptis DD, Vasiloglou MF, Mantzoros CS. Circulating leptin in non-alcoholic fatty liver disease: a systematic review and meta-analysis. Diabetologia. 2016;59:30-43. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 188] [Cited by in RCA: 187] [Article Influence: 20.8] [Reference Citation Analysis (0)] |
| 25. | Huang Y, Huang X, Ding L, Wang P, Peng K, Chen Y, Dai M, Zhang D, Xu M, Bi Y, Wang W. Serum Fetuin-A Associated With Fatty Liver Index, Early Indicator of Nonalcoholic Fatty Liver Disease: A Strobe-Compliant Article. Medicine (Baltimore). 2015;94:e1517. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 10] [Cited by in RCA: 12] [Article Influence: 1.2] [Reference Citation Analysis (0)] |
| 26. | von Loeffelholz C, Horn P, Birkenfeld AL, Claus RA, Metzing BU, Döcke S, Jahreis G, Heller R, Hoppe S, Stockmann M, Lock JF, Rieger A, Weickert MO, Settmacher U, Rauchfuß F, Pfeiffer AF, Bauer M, Sponholz C. Fetuin A is a Predictor of Liver Fat in Preoperative Patients with Nonalcoholic Fatty Liver Disease. J Invest Surg. 2016;29:266-274. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 18] [Cited by in RCA: 17] [Article Influence: 1.9] [Reference Citation Analysis (0)] |
| 27. | Aktas B, Yilmaz Y, Eren F, Yonal O, Kurt R, Alahdab YO, Celikel CA, Ozdogan O, Imeryuz N, Kalayci C, Avsar E. Serum levels of vaspin, obestatin, and apelin-36 in patients with nonalcoholic fatty liver disease. Metabolism. 2011;60:544-549. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 53] [Cited by in RCA: 51] [Article Influence: 3.6] [Reference Citation Analysis (0)] |
| 28. | Genc H, Dogru T, Tapan S, Kara M, Ercin CN, Aslan F, Kantarcioglu M, Karslioglu Y, Sertoglu E, Erbil MK, Bagci S. Circulating vaspin and its relationship with insulin sensitivity, adiponectin, and liver histology in subjects with non-alcoholic steatohepatitis. Scand J Gastroenterol. 2011;46:1355-1361. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 13] [Cited by in RCA: 12] [Article Influence: 0.9] [Reference Citation Analysis (0)] |
| 29. | Shen C, Zhao CY, Wang W, Wang YD, Sun H, Cao W, Yu WY, Zhang L, Ji R, Li M, Gao J. The relationship between hepatic resistin overexpression and inflammation in patients with nonalcoholic steatohepatitis. BMC Gastroenterol. 2014;14:39. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 45] [Cited by in RCA: 48] [Article Influence: 4.4] [Reference Citation Analysis (0)] |
| 30. | Koohkan S, Schaffner D, Milliron BJ, Frey I, König D, Deibert P, Vitolins M, Berg A. The impact of a weight reduction program with and without meal-replacement on health related quality of life in middle-aged obese females. BMC Womens Health. 2014;14:45. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 11] [Cited by in RCA: 11] [Article Influence: 1.0] [Reference Citation Analysis (0)] |
| 31. | König D, Zdzieblik D, Deibert P, Berg A, Gollhofer A, Büchert M. Internal Fat and Cardiometabolic Risk Factors Following a Meal-Replacement Regimen vs. Comprehensive Lifestyle Changes in Obese Subjects. Nutrients. 2015;7:9825-9833. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 13] [Cited by in RCA: 18] [Article Influence: 1.8] [Reference Citation Analysis (0)] |
| 32. | Lange T, Buechert M, Baumstark MW, Deibert P, Gerner S, Rydén H, Seufert J, Korsten-Reck U. Value of MRI and MRS fat measurements to complement conventional screening methods for childhood obesity: MR Methods for Screening Childhood Obesity. J Magn Reson Imaging. 2015;42:1214-1222. [RCA] [DOI] [Full Text] [Cited by in Crossref: 7] [Cited by in RCA: 8] [Article Influence: 0.8] [Reference Citation Analysis (0)] |
| 33. | Thesen S, Heid O, Mueller E, Schad LR. Prospective acquisition correction for head motion with image-based tracking for real-time fMRI. Magn Reson Med. 2000;44:457-465. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 1] [Reference Citation Analysis (0)] |
| 34. | Hernando D, Kellman P, Haldar JP, Liang ZP. Robust water/fat separation in the presence of large field inhomogeneities using a graph cut algorithm. Magn Reson Med. 2010;63:79-90. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 195] [Cited by in RCA: 195] [Article Influence: 13.0] [Reference Citation Analysis (0)] |
| 35. | Kass M, Witkin A, Terzopoulos D. Snakes: Active contour models. Int J Comput Vis. 1988;1:321-331. [RCA] [DOI] [Full Text] [Cited by in Crossref: 11057] [Cited by in RCA: 3531] [Article Influence: 95.4] [Reference Citation Analysis (0)] |
| 36. | Shen W, Wang Z, Punyanita M, Lei J, Sinav A, Kral JG, Imielinska C, Ross R, Heymsfield SB. Adipose tissue quantification by imaging methods: a proposed classification. Obes Res. 2003;11:5-16. [PubMed] |
| 37. | Ludwig UA, Klausmann F, Baumann S, Honal M, Hövener JB, König D, Deibert P, Büchert M. Whole-body MRI-based fat quantification: a comparison to air displacement plethysmography. J Magn Reson Imaging. 2014;40:1437-1444. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 36] [Cited by in RCA: 35] [Article Influence: 3.2] [Reference Citation Analysis (0)] |
| 38. | Hamilton G, Yokoo T, Bydder M, Cruite I, Schroeder ME, Sirlin CB, Middleton MS. In vivo characterization of the liver fat 1H MR spectrum. NMR Biomed. 2011;24:784-790. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 404] [Cited by in RCA: 430] [Article Influence: 30.7] [Reference Citation Analysis (0)] |
| 39. | Ye Q, Danzer CF, Fuchs A, Wolfrum C, Rudin M. Hepatic lipid composition differs between ob/ob and ob/+ control mice as determined by using in vivo localized proton magnetic resonance spectroscopy. MAGMA. 2012;25:381-389. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 20] [Cited by in RCA: 16] [Article Influence: 1.2] [Reference Citation Analysis (0)] |
| 40. | Ye Q, Danzer CF, Fuchs A, Vats D, Wolfrum C, Rudin M. Longitudinal evaluation of hepatic lipid deposition and composition in ob/ob and ob/+ control mice. NMR Biomed. 2013;26:1079-1088. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 12] [Cited by in RCA: 10] [Article Influence: 0.8] [Reference Citation Analysis (0)] |
| 41. | McCrory MA, Gomez TD, Bernauer EM, Molé PA. Evaluation of a new air displacement plethysmograph for measuring human body composition. Med Sci Sports Exerc. 1995;27:1686-1691. [PubMed] |
| 42. | Anderson DE. Reliability of air displacement plethysmography. J Strength Cond Res. 2007;21:169-172. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 1] [Reference Citation Analysis (0)] |
| 43. | Lohman TG, Roche AF, Martorell R. Anthropometric standardization reference manual. Champaign, IL: Human Kinetics Books; 1988; . |
| 44. | Sullivan S, Kirk EP, Mittendorfer B, Patterson BW, Klein S. Randomized trial of exercise effect on intrahepatic triglyceride content and lipid kinetics in nonalcoholic fatty liver disease. Hepatology. 2012;55:1738-1745. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 197] [Cited by in RCA: 210] [Article Influence: 16.2] [Reference Citation Analysis (0)] |
| 45. | Golabi P, Locklear CT, Austin P, Afdhal S, Byrns M, Gerber L, Younossi ZM. Effectiveness of exercise in hepatic fat mobilization in non-alcoholic fatty liver disease: Systematic review. World J Gastroenterol. 2016;22:6318-6327. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in CrossRef: 142] [Cited by in RCA: 130] [Article Influence: 14.4] [Reference Citation Analysis (1)] |
| 46. | Redman LM, Huffman KM, Landerman LR, Pieper CF, Bain JR, Muehlbauer MJ, Stevens RD, Wenner BR, Kraus VB, Newgard CB, Kraus WE, Ravussin E. Effect of caloric restriction with and without exercise on metabolic intermediates in nonobese men and women. J Clin Endocrinol Metab. 2011;96:E312-E321. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 38] [Cited by in RCA: 34] [Article Influence: 2.4] [Reference Citation Analysis (0)] |
| 47. | Devries MC, Samjoo IA, Hamadeh MJ, Tarnopolsky MA. Effect of endurance exercise on hepatic lipid content, enzymes, and adiposity in men and women. Obesity (Silver Spring). 2008;16:2281-2288. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 70] [Cited by in RCA: 62] [Article Influence: 3.6] [Reference Citation Analysis (0)] |
| 48. | Yoshimura E, Kumahara H, Tobina T, Matsuda T, Ayabe M, Kiyonaga A, Anzai K, Higaki Y, Tanaka H. Lifestyle intervention involving calorie restriction with or without aerobic exercise training improves liver fat in adults with visceral adiposity. J Obes. 2014;2014:197216. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 34] [Cited by in RCA: 42] [Article Influence: 3.8] [Reference Citation Analysis (0)] |
| 49. | Tamura Y, Tanaka Y, Sato F, Choi JB, Watada H, Niwa M, Kinoshita J, Ooka A, Kumashiro N, Igarashi Y, Kyogoku S, Maehara T, Kawasumi M, Hirose T, Kawamori R. Effects of diet and exercise on muscle and liver intracellular lipid contents and insulin sensitivity in type 2 diabetic patients. J Clin Endocrinol Metab. 2005;90:3191-3196. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 240] [Cited by in RCA: 234] [Article Influence: 11.7] [Reference Citation Analysis (0)] |
| 50. | Poirier P, Després JP. Exercise in weight management of obesity. Cardiol Clin. 2001;19:459-470. [PubMed] |
| 51. | Haufe S, Haas V, Utz W, Birkenfeld AL, Jeran S, Böhnke J, Mähler A, Luft FC, Schulz-Menger J, Boschmann M, Jordan J, Engeli S. Long-lasting improvements in liver fat and metabolism despite body weight regain after dietary weight loss. Diabetes Care. 2013;36:3786-3792. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 42] [Cited by in RCA: 53] [Article Influence: 4.4] [Reference Citation Analysis (0)] |
| 52. | Zhan S, Ho SC. Meta-analysis of the effects of soy protein containing isoflavones on the lipid profile. Am J Clin Nutr. 2005;81:397-408. [PubMed] |
| 53. | Anderson JW, Hoie LH. Weight loss and lipid changes with low-energy diets: comparator study of milk-based versus soy-based liquid meal replacement interventions. J Am Coll Nutr. 2005;24:210-216. [PubMed] |
| 54. | Markova M, Pivovarova O, Hornemann S, Sucher S, Frahnow T, Wegner K, Machann J, Petzke KJ, Hierholzer J, Lichtinghagen R, Herder C, Carstensen-Kirberg M, Roden M, Rudovich N, Klaus S, Thomann R, Schneeweiss R, Rohn S, Pfeiffer AF. Isocaloric Diets High in Animal or Plant Protein Reduce Liver Fat and Inflammation in Individuals With Type 2 Diabetes. Gastroenterology. 2017;152:571-585.e8. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 145] [Cited by in RCA: 190] [Article Influence: 23.8] [Reference Citation Analysis (0)] |
| 55. | Larson-Meyer DE, Newcomer BR, Heilbronn LK, Volaufova J, Smith SR, Alfonso AJ, Lefevre M, Rood JC, Williamson DA, Ravussin E; Pennington CALERIE Team. Effect of 6-month calorie restriction and exercise on serum and liver lipids and markers of liver function. Obesity (Silver Spring). 2008;16:1355-1362. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 169] [Cited by in RCA: 153] [Article Influence: 9.0] [Reference Citation Analysis (0)] |
| 56. | Targher G, Marra F, Marchesini G. Increased risk of cardiovascular disease in non-alcoholic fatty liver disease: causal effect or epiphenomenon? Diabetologia. 2008;51:1947-1953. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 278] [Cited by in RCA: 288] [Article Influence: 16.9] [Reference Citation Analysis (0)] |
| 57. | Marchesini G, Marzocchi R. Metabolic Syndrome and NASH. Clin Liver Dis. 2007;11:105-117, ix. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 90] [Cited by in RCA: 96] [Article Influence: 5.3] [Reference Citation Analysis (0)] |
| 58. | Misra VL, Khashab M, Chalasani N. Nonalcoholic fatty liver disease and cardiovascular risk. Curr Gastroenterol Rep. 2009;11:50-55. [PubMed] |
| 59. | Kang BK, Yu ES, Lee SS, Lee Y, Kim N, Sirlin CB, Cho EY, Yeom SK, Byun JH, Park SH, Lee MG. Hepatic fat quantification: a prospective comparison of magnetic resonance spectroscopy and analysis methods for chemical-shift gradient echo magnetic resonance imaging with histologic assessment as the reference standard. Invest Radiol. 2012;47:368-375. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 90] [Cited by in RCA: 88] [Article Influence: 6.8] [Reference Citation Analysis (0)] |
| 60. | Lazo M, Solga SF, Horska A, Bonekamp S, Diehl AM, Brancati FL, Wagenknecht LE, Pi-Sunyer FX, Kahn SE, Clark JM; Fatty Liver Subgroup of the Look AHEAD Research Group. Effect of a 12-month intensive lifestyle intervention on hepatic steatosis in adults with type 2 diabetes. Diabetes Care. 2010;33:2156-2163. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 250] [Cited by in RCA: 258] [Article Influence: 17.2] [Reference Citation Analysis (0)] |
| 61. | Heath ML, Kow L, Slavotinek JP, Valentine R, Toouli J, Thompson CH. Abdominal adiposity and liver fat content 3 and 12 months after gastric banding surgery. Metabolism. 2009;58:753-758. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 29] [Cited by in RCA: 28] [Article Influence: 1.8] [Reference Citation Analysis (0)] |
| 62. | Cuthbertson DJ, Shojaee-Moradie F, Sprung VS, Jones H, Pugh CJ, Richardson P, Kemp GJ, Barrett M, Jackson NC, Thomas EL, Bell JD, Umpleby AM. Dissociation between exercise-induced reduction in liver fat and changes in hepatic and peripheral glucose homoeostasis in obese patients with non-alcoholic fatty liver disease. Clin Sci (Lond). 2016;130:93-104. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 66] [Cited by in RCA: 98] [Article Influence: 9.8] [Reference Citation Analysis (1)] |
| 63. | Houghton D, Thoma C, Hallsworth K, Cassidy S, Hardy T, Burt AD, Tiniakos D, Hollingsworth KG, Taylor R, Day CP, McPherson S, Anstee QM, Trenell MI. Exercise Reduces Liver Lipids and Visceral Adiposity in Patients With Nonalcoholic Steatohepatitis in a Randomized Controlled Trial. Clin Gastroenterol Hepatol. 2017;15:96-102.e3. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 112] [Cited by in RCA: 141] [Article Influence: 17.6] [Reference Citation Analysis (0)] |
| 64. | Machado MV, Coutinho J, Carepa F, Costa A, Proença H, Cortez-Pinto H. How adiponectin, leptin, and ghrelin orchestrate together and correlate with the severity of nonalcoholic fatty liver disease. Eur J Gastroenterol Hepatol. 2012;24:1166-1172. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 55] [Cited by in RCA: 63] [Article Influence: 4.8] [Reference Citation Analysis (0)] |
| 65. | Kahraman A, Sowa JP, Schlattjan M, Sydor S, Pronadl M, Wree A, Beilfuss A, Kilicarslan A, Altinbaş A, Bechmann LP, Syn WK, Gerken G, Canbay A. Fetuin-A mRNA expression is elevated in NASH compared with NAFL patients. Clin Sci (Lond). 2013;125:391-400. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 41] [Cited by in RCA: 48] [Article Influence: 4.0] [Reference Citation Analysis (0)] |
| 66. | Polyzos SA, Kountouras J, Mantzoros CS. Leptin in nonalcoholic fatty liver disease: a narrative review. Metabolism. 2015;64:60-78. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 133] [Cited by in RCA: 165] [Article Influence: 16.5] [Reference Citation Analysis (0)] |
| 67. | Ding WJ, Wang Y, Fan JG. Regulation of adipokines by polyunsaturated fatty acids in a rat model of non-alcoholic steatohepatitis. Arch Iran Med. 2014;17:563-568. [PubMed] |
| 68. | Cheng Y, Zhang K, Chen Y, Li Y, Li Y, Fu K, Feng R. Associations between Dietary Nutrient Intakes and Hepatic Lipid Contents in NAFLD Patients Quantified by ¹H-MRS and Dual-Echo MRI. Nutrients. 2016;8. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 26] [Cited by in RCA: 35] [Article Influence: 3.9] [Reference Citation Analysis (0)] |
| 69. | Scorletti E, Bhatia L, McCormick KG, Clough GF, Nash K, Hodson L, Moyses HE, Calder PC, Byrne CD; WELCOME Study. Effects of purified eicosapentaenoic and docosahexaenoic acids in nonalcoholic fatty liver disease: results from the Welcome* study. Hepatology. 2014;60:1211-1221. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 226] [Cited by in RCA: 245] [Article Influence: 22.3] [Reference Citation Analysis (0)] |
| 70. | Pachikian BD, Essaghir A, Demoulin JB, Neyrinck AM, Catry E, De Backer FC, Dejeans N, Dewulf EM, Sohet FM, Portois L, Deldicque L, Molendi-Coste O, Leclercq IA, Francaux M, Carpentier YA, Foufelle F, Muccioli GG, Cani PD, Delzenne NM. Hepatic n-3 polyunsaturated fatty acid depletion promotes steatosis and insulin resistance in mice: genomic analysis of cellular targets. PLoS One. 2011;6:e23365. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 61] [Cited by in RCA: 65] [Article Influence: 4.6] [Reference Citation Analysis (0)] |