Published online Dec 14, 2019. doi: 10.3748/wjg.v25.i46.6790
Peer-review started: October 30, 2019
First decision: November 9, 2019
Revised: December 1, 2019
Accepted: December 7, 2019
Article in press: December 7, 2019
Published online: December 14, 2019
Processing time: 44 Days and 18.6 Hours
Increasing levels of antibiotic resistance have reduced the Helicobacter pylori (H. pylori) eradication rates afforded by the standard triple therapy. Thus, 2-wk first-line four-drug regimens must be considered.
To analyze the eradication rates of modified bismuth-containing quadruple therapy (mBCQT) and concomitant therapy (CT), the associated adverse events, and compliance.
Patients infected with H. pylori were prospectively randomized to receive mBCQT or CT for 2 wk. mBCQT featured a proton pump inhibitor (PPI), bismuth, metronidazole, and tetracycline, taken twice daily. CT included a PPI, clarithromycin, metronidazole, and amoxicillin, taken twice daily. The 13C-urea breath test was performed no earlier than 4 wk after therapy concluded to confirm eradication. If either the histological or rapid urease test was positive, H. pylori infection was diagnosed.
The demographic characteristics of 68 patients who received mBCQT and 68 who received CT did not differ significantly. On intention-to-treat analysis, the eradication rate was 88.2% (60/68) in the mBCQT group and 79.4% (54/68) in the CT group (P = 0.162). By per-protocol analysis, the respective eradication rates were 98.4% (60/61) and 93.1% (54/58) (P = 0.199). More CT than mBCQT patients experienced adverse events [33.8% (23/68) mBCQT vs 51.5% (35/58) CT patients, respectively, P = 0.037]. All patients showed good compliance [85.3% (58/68) mBCQT vs 82.4% (56/68) CT patients, P = 0.641].
The H. pylori eradication rates of the 2-wk mBCQT and CT regimens are high. Most patients show good compliance, and more CT than mBCQT patients experience adverse events.
Core tip: Both modified bismuth-containing quadruple therapy and concomitant therapy proved to be useful empirical first-line treatment options for Helicobacter pylori eradication in an area exhibiting high-level clarithromycin resistance (> 15%).
- Citation: Kim SJ, Chung JW, Woo HS, Kim SY, Kim JH, Kim YJ, Kim KO, Kwon KA, Park DK. Two-week bismuth-containing quadruple therapy and concomitant therapy are effective first-line treatments for Helicobacter pylori eradication: A prospective open-label randomized trial. World J Gastroenterol 2019; 25(46): 6790-6798
- URL: https://www.wjgnet.com/1007-9327/full/v25/i46/6790.htm
- DOI: https://dx.doi.org/10.3748/wjg.v25.i46.6790
Helicobacter pylori (H. pylori) infection is the principal cause of peptic ulcer disease, mucosa-associated lymphoid tissue lymphoma, and gastric adenocarcinoma. H. pylori eradication cures or prevents these diseases[1]. However, H. pylori is becoming resistant to previously efficacious antibiotic regimens[2]. Clarithromycin resistance is increasing worldwide[2-4]. The eradication rate afforded by legacy triple therapy (LTT) (the historical first-line treatment for H. pylori infection; LTT includes clarithromycin) has declined over the past decade, and has decreased to near 80% or below in some countries of Asia and Europe[2-4]. Dual clarithromycin-/metronidazole-resistance of H. pylori is also of concern worldwide[5]. In South Korea, the dual resistance rate is 9.6%, and it is 19% [95% confidence interval (CI): 0%–39%] in the Eastern Mediterranean Region[5,6].
Thus, many studies have explored the efficacy of first-line alternatives to LTT; these include bismuth quadruple therapy (BQT) and concomitant therapy (CT)[7-13], which feature in the current guidelines[2,14-16]. The Maastricht V consensus concluded that, in areas exhibiting high-level (> 15%) clarithromycin resistance but low-level dual clarithromycin/metronidazole resistance (< 15%), BQT or CT should be recommended. In areas exhibiting high-level dual clarithromycin/metronidazole resistance (> 15%), BQT is the recommended first-line treatment (level of evidence: Low; grade and recommendation: High)[2]. The revised guidelines for the diagnosis and treatment of H. pylori infection in Korea recommend the use of bismuth-containing quadruple therapy (BCQT) if clarithromycin resistance is suspected[16]. A meta-analysis found that the eradication rate afforded by CT was slightly higher than that of sequential therapy (ST) [pooled odds ratio (OR) = 1.382, P = 0.03, intention-to-treat (ITT) analysis; 2.102, P = 0.001, per-protocol (PP) analysis][10]. However, only a few reports on the efficacy of BCQT and CT have appeared; direct comparisons are rare. Therefore, we performed a prospective, randomized controlled study comparing modified BCQT (mBCQT) and CT as potential first-line treatments for H. pylori infection.
We performed a prospective, open-label, randomized controlled trial in a single tertiary medical center. Patients who underwent endoscopy between February 2016 and August 2017 at Gachon University Gil Hospital, and who received first-of-life diagnoses of peptic ulcer disease, gastritis, gastric polyps, or early gastric cancer, and who then underwent endoscopic mucosal resection, were initially included.
Sample size calculations were performed before the trial began. We assumed, based on previous studies, that the eradication rate of CT was 90%. With little data on BCQT, we assumed an eradication rate of 85% and calculated that a sample size of 60 patients in each of the two groups was necessary (α = 0.05, power 80%, non-inferiority limit of -10%-10%). The actual sample size was increased to 136 patients to account for patient drop-out.
Of these patients, 136 with confirmed H. pylori infections [at least two positive results on either or both of a histological test (Giemsa staining) and the rapid urease test] were enrolled. The 136 patients were randomly divided into two 68-patient groups using a computer-generated block randomization table; the groups received 2-wk treatments with either mBCQT or CT.
The 13C-urea breath test was performed at 6 wk to 8 wk after antibiotic suspension.
The primary outcome was the eradication rate of H. pylori, as determined by ITT and PP analysis. The secondary outcomes were adverse events and compliance.
The study was approved by the Clinical Research Ethics Committee of Gachon University Gil Hospital (approval No. GCIRB2016-006). Written informed consent was obtained from all patients enrolled in the study.
When either Giemsa staining or rapid urease test (HP kit; Chong Kun Dang Bio, Seoul, South Korea) was positive upon upper gastrointestinal endoscopy, H. pylori infection was diagnosed.
The mBCQT regimen featured lansoprazole (Lanston LFDT Tab.) 30 mg, tripotassium bismuth dicitrate 600 mg (Denol Tab.), tetracycline (Tetracycline Cap.) 1000 mg, and metronidazole (Flasinyl Tab.) 500 mg twice daily for 2 wk. CT featured lansoprazole (Lanston LFDT Tab.) 30 mg, clarithromycin (Kloma Tab.) 500 mg, amoxicillin (Amoxapen Cap.) 1000 mg, and metronidazole (Flasinyl® Tab.) 500 mg twice daily for 2 wk.
Inadequate drug compliance was defined as ingestion of less than 90% of the total recommended dose. Adverse effects were defined as unexpected symptoms that developed between the commencement and 4 wk after completion of treatment.
The 13C-urea breath test (UBiT-IR 300/13C-Urea breath test system; Otsuka, Tokyo, Japan) was performed no earlier than 4 wk after treatment concluded, at which time no patient had taken proton pump inhibitors for at least 2 wk. Eradication failure was defined as a positive (delta 2.5) breath test.
IBM SPSS statistical software (ver. 22.0; IBM Corp, Armonk, NY, United States) was used for all analyses. We employed the χ2 test to compare discrete variables and the independent t-test to compare continuous variables. We ensured that our sample size had a sufficient non-inferiority margin.
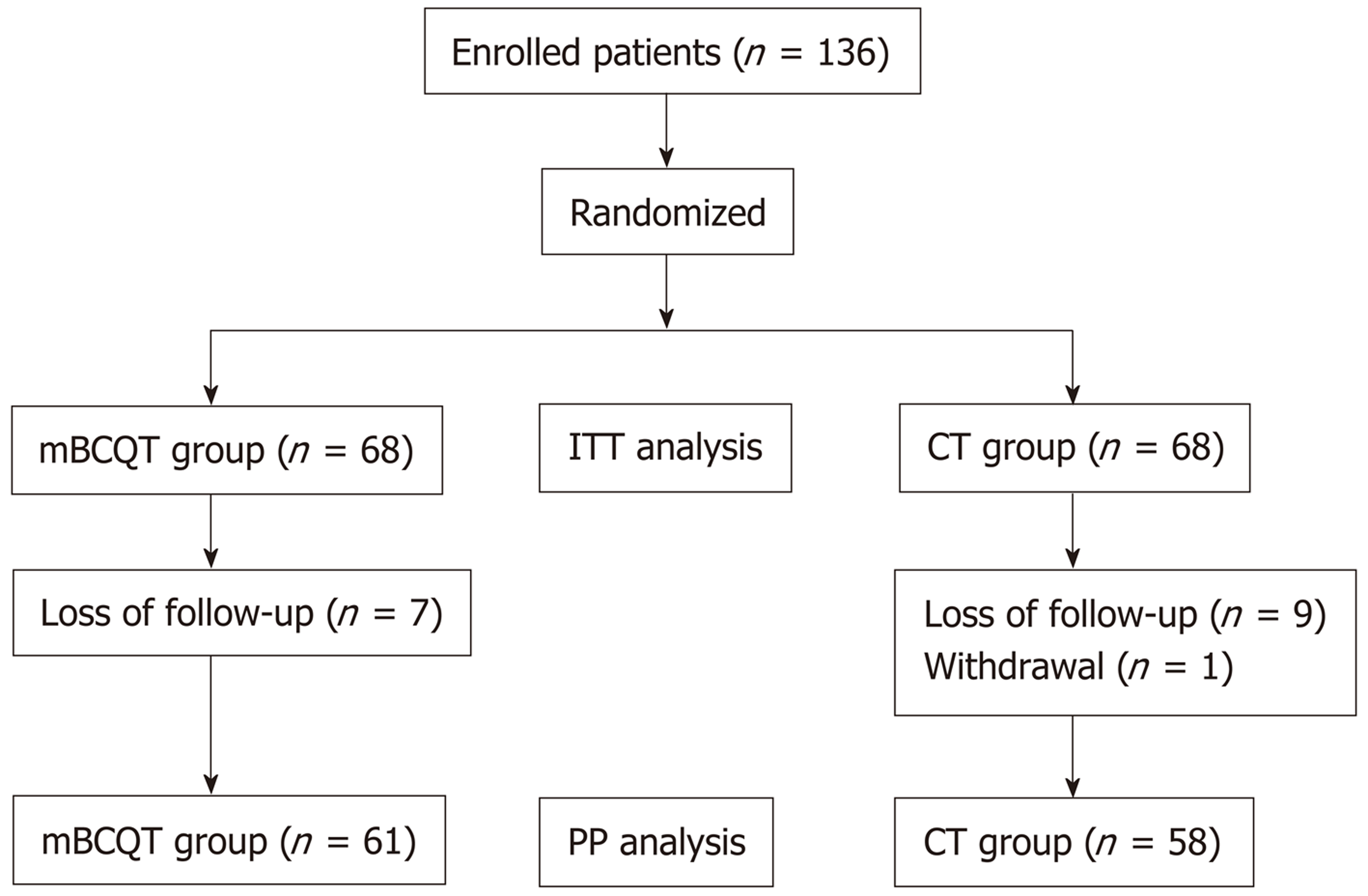
A total of 136 patients were randomly divided into two groups of 68 patients each and compared via ITT analysis. Seven mBCQT patients were excluded because of loss to follow-up. Nine CT patients were lost to follow-up and one patient withdrew. The remaining 61 patients in the mBCQT group and 58 in the CT group were compared via PP analysis (Figure 1).
The mean age of mBCQT and CT group patients was 57.37 ± 11.31 and 60.09 ± 9.93 years, respectively (P = 0.138). The demographic characteristics of the two groups did not differ significantly (Table 1).
| Variable | mBCQT treatment (n = 68) | CT treatment (n = 68) | P value |
| Age (yr) | 57.37 ± 11.31 | 60.09 ± 9.93 | 0.138 |
| Gender (male:female) | 40:28 | 32:36 | 0.169 |
| Height (m) | 1.64 ± 0.09 | 1.63 ± 0.08 | 0.420 |
| Weight (kg) | 64.61 ± 9.23 | 63.27 ± 9.69 | 0.409 |
| BMI (kg/m2) | 24.05 ± 2.88 | 23.87 ± 2.91 | 0.704 |
| Smoking | 12 (17.6) | 14 (20.6) | 0.663 |
| Alcohol | 18 (26.5) | 18 (26.5) | 0.999 |
| Gastric and/or duodenal ulcer | 27 (39.7) | 19 (27.9) | 0.147 |
ITT analysis revealed an eradication rate of 88.2% (60/68) in the mBCQT group and 79.4% (54/68) in the CT group (P = 0.162). PP analysis revealed that the eradication rates in the mBCQT group and CT group were 98.4% (60/61) and 93.1% (54/58), respectively (P = 0.199) (Table 2). ITT analysis showed that the eradication rates in both the mBCQT and CT groups were close to 80%, but the PP values for both groups were over 90%.
| Eradication rate | P value | ||
| mBCQT Treatment | CT Treatment | ||
| ITT analysis | 88.2 (60/68) | 79.4 (54/68) | 0.162 |
| PP analysis | 98.4 (60/61) | 93.1 (54/58) | 0.199 |
Most of the adverse symptoms affected the digestive system. No serious side effect was noted in any patient. The adverse effect rates in the mBCQT group and CT group were 33.8% (23/68) and 51.5% (35/68), respectively, i.e., slightly higher in the CT group (P = 0.037). The compliance level was 85.3% in the mBCQT group and 82.4% in the CT group (Table 3).
| mBCQT treatment (n = 68) | CT treatment (n = 68) | P value | |
| Diarrhea | 1.5 (1) | 13.2 (9) | 0.009 |
| Feces discoloration | 5.9 (4) | 0 (0) | 0.119 |
| Nausea | 16.2 (11) | 16.2 (11) | 0.999 |
| Taste disturbance | 5.9 (4) | 14.7 (10) | 0.090 |
| Miscellaneous | 22.1 (15) | 20.6 (14) | 0.834 |
| Total adverse events | 33.8 (23) | 51.5 (35) | 0.037 |
| Compliance1 | 85.3 (58) | 82.4 (56) | 0.641 |
Both mBCQT and CT proved to be useful empirical first-line treatment options for H. pylori eradication. In an area exhibiting high-level clarithromycin resistance (> 15%), both regimens were effective on ITT analysis (mBCQT, 88.2%; CT, 79.4%; P = 0.162) and PP analysis (mBCQT, 98.4%; CT, 93.1%; P = 0.199)[16,17]. mBCQT was somewhat, but not significantly, better than CT, by about 8% on ITT analysis and 5% on PP analysis. A large randomized trial performed in Taiwan reported similar results. The cited work used culture to identify clarithromycin-susceptible and -resistant strains, and predicted the efficacy of various drug regimens accordingly. The predicted efficacy of 10-d BQT was greater than that of 10-d CT and 14-d LTT in regions exhibiting high-level clarithromycin resistance, as revealed by multivariate analysis. Similarly, CT was more effective than LTT[8]. A prospective study performed in Spain yielded results similar to ours; 10-d BQT (using capsules) and 14-d CT, employed as first-line eradication treatments in an area of high-level clarithromycin resistance, were equally effective[12]. A South Korean study found that 10-d PAM-B therapy (rabeprazole 20 mg, amoxicillin 1 g, metronidazole 750 mg, and tripotassium dicitratobismuthate 600 mg twice daily) compared favorably with 14-d CT. The eradication rate of CT was similar to that of the present study, but the PAM-B eradication rate could not be directly compared to the CT data because the regimens differed markedly (ITT analysis, 88.1% vs 83.0%, P = 0.299; PP analysis, 96.6% vs 95.5%, P = 0.743). The incidence of adverse events was lower than that in our study (23.0% vs 25.2%, P = 0.776), perhaps because the duration of 10-d CT of the cited study was shorter than that of our CT[13]. The effects of treatment duration on eradication rates and side effects should be studied in future. Both of our regimens featured multiple drugs; compliance remains an issue, but the relatively high eradication rates may reflect good compliance[18]. Our mBCQT regimen featured twice-daily dosing, unlike previous studies. Dore et al[19] reported that daily two- or four-dose second-line regimens afforded similar eradication rates.
Also, our mBCQT regimen used a higher dose of tetracycline than other regimens (1000 mg twice daily). A previous Korean study revealed that the extent of tetracycline resistance was relatively low (minimal inhibitory concentration ≥ 2.0 mg/mL, 0%–3.3% of isolates), perhaps attributable to a reduction in tetracycline prescriptions when medical practice and pharmaceutical dispensing were separated in 2000[6,20,21]. The tetracycline resistance rate was 0.7% in Spain, 0.5% in the United Kingdom, and 0.5% in Hong Kong; in many countries, the rate was 0%[22]. Some studies have explored the efficacy of tetracycline-/amoxicillin-containing regimens. A Korean study comparing a 10-d ST and 14-d PBAT regimen (40 mg pantoprazole, 600 mg bismuth subcitrate, 1 g tetracycline, and 1 g amoxicillin, twice a day) found that ST seemed to be more effective; however, neither regimen afforded ‘excellent’ eradication (over 90%)[23]. A Taiwanese study found that quadruple therapy featuring tetracycline and amoxicillin effectively rescued patients in whom triple therapy failed (78% rescue on ITT analysis and 89% on PP analysis). However, apart from our mBCQT regimen, ST featuring tetracycline was associated with relatively low-level eradication[24]. These variable results may reflect the fact that both tetracycline and amoxicillin are not very active against H. pylori, or that the drugs may act antagonistically[23]. In most studies, tetracycline was taken four times daily, but twice-daily regimens are more appropriate and probably also improve compliance; tetracycline is a time-dependent (half-life, 8–10 h) antibiotic agent exhibiting a long post-antibiotic effect. Further studies are needed to explore the adequacy of currently used tetracycline dosages and durations[23].
Although neither of our regimens was associated with serious side effects, the overall incidence of side effects was relatively high. Further efforts to reduce side effects, perhaps via addition of probiotics, are essential[25]. Previous studies have found that certain probiotics, such as Lactobacillus genus and Bacillus clausii, reduce gastrointestinal problems and other side effects of eradication therapies[2,26]. It has been suggested that the increase in H. pylori eradication seen with use of these probiotics is not a direct effect of the probiotics, but a result of the associated reduction in side effects of therapy[2,26].
Although both regimens seemed to be effective first-line therapies, their efficacy in terms of salvage therapy have not been confirmed. The Maastricht V guidelines indicate that, after failure of non-BQT, levofloxacin triple therapy is appropriate[2]. However, according to the World Health Organization, quinolone resistance has been reported in over 30% of all regions, and primary levofloxacin resistance in over 15%, except Europe[5,20,22]. Therefore, it is necessary to consider rescue regimens containing drugs associated with low H. pylori resistance rates.
One study of rifabutin-based therapy reported an eradication rate over 70% (72.7%, 95%CI: 67.3%–77.7%, PP analysis; 71.5%, 95%CI: 66.1%–76.5%, ITT analysis)[27]. Although rifabutin-resistant H. pylori has been reported, rifabutin-based regimens may be useful as rescue therapies because rifabutin can be used without culture and antibiotic susceptibility testing[27]. Also, furazolidone-resistant H. pylori is rare; the drug afforded satisfactory eradication rates (relative risk = 1.17, 95%CI: 1.05–1.31)[28]. In a multivariate analysis, an increased eradication rate when using high-dose furazolidone was noted (OR = 1.5, 95%CI: 1.3-2.7; P < 0.001)[29]. According to a recent in vitro analysis, there were no strains resistant to rifabutin or furazolidone among multi-drug resistant H. pylori (minimum inhibitory concentration < 0.008 and < 0.5 μg/mL, respectively). This suggests that rifabutin- and furazolidone-containing regimens have promise as rescue therapies[30]. However, there is controversy over the use of furazolidone-containing regimens because of the drug’s potential carcinogenicity. Thus, furazolidone-containing regimens are recommended only in areas with high rates of resistance and for patients who have multiple prior treatment failures and have received patient counseling[29,31].
The limitations of this study included the small number of patients, due to the single-center design. Also, we did not culture H. pylori. The strengths of our study include its randomized controlled design and the acceptable therapeutic efficacy in both the mBCQT and CT groups. In conclusion, both mBCQT and CT are promising empirical first-line regimens in an area exhibiting high-level clarithromycin resistance. However, mBCQT is somewhat preferable, considering both side effects and compliance. A large-scale prospective study is required to validate our findings.
Helicobacter pylori (H. pylori) is becoming resistant to previously efficacious antibiotic regimens, including clarithromycin. The eradication rate afforded by legacy triple therapy (LTT), which includes clarithromycin, has declined over the past decade.
Many studies have explored the efficacy of first-line alternatives to LTT. However, only a few studies on the efficacy of bismuth-containing quadruple therapy (BCQT) and concomitant therapy (CT) have been conducted.
To determine the eradication rates of H. pylori and compare adverse events and compliance in groups of patients who received modified BCQT (mBCQT) and CT regimens.
We performed a prospective, open-label, randomized controlled trial with 2-week mBCQT and CT regimens.
Both mBCQT and CT regimens were effective on intention-to-treat and per-protocol analysis. Most patients showed good compliance. More CT than mBCQT patients experienced adverse events.
Both mBCQT and CT proved to be useful empirical first-line treatment options for H. pylori eradication in an area exhibiting high-level clarithromycin resistance
A large-scale prospective study is required to validate mBCQT and CT as empirical first-line treatment options for H. pylori eradication. The effects of treatment duration on eradication rates and side effects should be studied in future.
Manuscript source: Invited Manuscript
Specialty type: Gastroenterology and hepatology
Country of origin: South Korea
Peer-review report classification
Grade A (Excellent): 0
Grade B (Very good): B, B, B, B
Grade C (Good): C
Grade D (Fair): 0
Grade E (Poor): 0
P-Reviewer: Cheng H, Durazzo M, Fagoonee S, Ierardi E S-Editor: Tang JZ L-Editor: Wang TQ E-Editor: Zhang YL
| 1. | de Brito BB, da Silva FAF, Soares AS, Pereira VA, Santos MLC, Sampaio MM, Neves PHM, de Melo FF. Pathogenesis and clinical management of Helicobacter pylori gastric infection. World J Gastroenterol. 2019;25:5578-5589. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in CrossRef: 198] [Cited by in RCA: 167] [Article Influence: 27.8] [Reference Citation Analysis (15)] |
| 2. | Malfertheiner P, Megraud F, O'Morain CA, Gisbert JP, Kuipers EJ, Axon AT, Bazzoli F, Gasbarrini A, Atherton J, Graham DY, Hunt R, Moayyedi P, Rokkas T, Rugge M, Selgrad M, Suerbaum S, Sugano K, El-Omar EM; European Helicobacter and Microbiota Study Group and Consensus panel. Management of Helicobacter pylori infection-the Maastricht V/Florence Consensus Report. Gut. 2017;66:6-30. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 2220] [Cited by in RCA: 1984] [Article Influence: 248.0] [Reference Citation Analysis (1)] |
| 3. | Gong EJ, Yun SC, Jung HY, Lim H, Choi KS, Ahn JY, Lee JH, Kim DH, Choi KD, Song HJ, Lee GH, Kim JH. Meta-analysis of first-line triple therapy for helicobacter pylori eradication in Korea: is it time to change? J Korean Med Sci. 2014;29:704-713. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 70] [Cited by in RCA: 70] [Article Influence: 6.4] [Reference Citation Analysis (0)] |
| 4. | Pellicano R, Zagari RM, Zhang S, Saracco GM, Moss SF. Pharmacological considerations and step-by-step proposal for the treatment of Helicobacter pylori infection in the year 2018. Minerva Gastroenterol Dietol. 2018;64:310-321. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 31] [Cited by in RCA: 32] [Article Influence: 4.6] [Reference Citation Analysis (1)] |
| 5. | Savoldi A, Carrara E, Graham DY, Conti M, Tacconelli E. Prevalence of Antibiotic Resistance in Helicobacter pylori: A Systematic Review and Meta-analysis in World Health Organization Regions. Gastroenterology. 2018;155:1372-1382.e17. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 617] [Cited by in RCA: 822] [Article Influence: 117.4] [Reference Citation Analysis (0)] |
| 6. | Chung JW, Jung YK, Kim YJ, Kwon KA, Kim JH, Lee JJ, Lee SM, Hahm KB, Lee SM, Jeong JY, Yun SC. Ten-day sequential versus triple therapy for Helicobacter pylori eradication: a prospective, open-label, randomized trial. J Gastroenterol Hepatol. 2012;27:1675-1680. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 54] [Cited by in RCA: 52] [Article Influence: 4.0] [Reference Citation Analysis (0)] |
| 7. | Yeo YH, Shiu SI, Ho HJ, Zou B, Lin JT, Wu MS, Liou JM, Wu CY; Taiwan Gastrointestinal Disease and Helicobacter Consortium. First-line Helicobacter pylori eradication therapies in countries with high and low clarithromycin resistance: a systematic review and network meta-analysis. Gut. 2018;67:20-27. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 62] [Cited by in RCA: 57] [Article Influence: 8.1] [Reference Citation Analysis (0)] |
| 8. | Liou JM, Fang YJ, Chen CC, Bair MJ, Chang CY, Lee YC, Chen MJ, Chen CC, Tseng CH, Hsu YC, Lee JY, Yang TH, Luo JC, Chang CC, Chen CY, Chen PY, Shun CT, Hsu WF, Hu WH, Chen YN, Sheu BS, Lin JT, Wu JY, El-Omar EM, Wu MS; Taiwan Gastrointestinal Disease and Helicobacter Consortium. Concomitant, bismuth quadruple, and 14-day triple therapy in the first-line treatment of Helicobacter pylori: a multicentre, open-label, randomised trial. Lancet. 2016;388:2355-2365. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 93] [Cited by in RCA: 134] [Article Influence: 14.9] [Reference Citation Analysis (0)] |
| 9. | Lee H, Kim BJ, Kim SG, Kim JI, Choi IJ, Lee YC, Kim JG, Kim JJ; Korean College of Helicobacter and Upper Gastrointestinal Research. Concomitant, sequential, and 7-day triple therapy in first-line treatment of Helicobacter pylori infection in Korea: study protocol for a randomized controlled trial. Trials. 2017;18:549. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 4] [Cited by in RCA: 5] [Article Influence: 0.6] [Reference Citation Analysis (0)] |
| 10. | Bae HJ, Kim JS, Kim BW, Nam YJ. Concomitant or Sequential Therapy as the First-line Therapy for Eradication of Helicobacter pylori Infection in Korea: A Systematic Review and Meta-analysis. Korean J Gastroenterol. 2018;71:31-37. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 13] [Cited by in RCA: 11] [Article Influence: 1.6] [Reference Citation Analysis (0)] |
| 11. | Chen MJ, Chen CC, Chen YN, Chen CC, Fang YJ, Lin JT, Wu MS, Liou JM; Taiwan Gastrointestinal Disease Helicobacter Consortium. Systematic Review with Meta-Analysis: Concomitant Therapy vs. Triple Therapy for the First-Line Treatment of Helicobacter pylori Infection. Am J Gastroenterol. 2018;113:1444-1457. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 25] [Cited by in RCA: 29] [Article Influence: 4.1] [Reference Citation Analysis (0)] |
| 12. | Macías-García F, Bastón-Rey I, de la Iglesia-García D, Calviño-Suárez C, Nieto-García L, Domínguez-Muñoz JE. Bismuth-containing quadruple therapy versus concomitant quadruple therapy as first-line treatment for Helicobacter Pylori infection in an area of high resistance to clarithromycin: A prospective, cross-sectional, comparative, open trial. Helicobacter. 2019;24:e12546. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 25] [Cited by in RCA: 23] [Article Influence: 3.8] [Reference Citation Analysis (0)] |
| 13. | Choe JW, Jung SW, Kim SY, Hyun JJ, Jung YK, Koo JS, Yim HJ, Lee SW. Comparative study of Helicobacter pylori eradication rates of concomitant therapy vs modified quadruple therapy comprising proton-pump inhibitor, bismuth, amoxicillin, and metronidazole in Korea. Helicobacter. 2018;23:e12466. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 27] [Cited by in RCA: 28] [Article Influence: 4.0] [Reference Citation Analysis (0)] |
| 14. | De Francesco V, Bellesia A, Ridola L, Manta R, Zullo A. First-line therapies for Helicobacter pylori eradication: a critical reappraisal of updated guidelines. Ann Gastroenterol. 2017;30:373-379. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 5] [Cited by in RCA: 15] [Article Influence: 1.9] [Reference Citation Analysis (0)] |
| 15. | Fallone CA, Chiba N, van Zanten SV, Fischbach L, Gisbert JP, Hunt RH, Jones NL, Render C, Leontiadis GI, Moayyedi P, Marshall JK. The Toronto Consensus for the Treatment of Helicobacter pylori Infection in Adults. Gastroenterology. 2016;151:51-69.e14. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 695] [Cited by in RCA: 636] [Article Influence: 70.7] [Reference Citation Analysis (0)] |
| 16. | Kim SG, Jung HK, Lee HL, Jang JY, Lee H, Kim CG, Shin WG, Shin ES, Lee YC; Korean College of Helicobacter and Upper Gastrointestinal Research. [Guidelines for the diagnosis and treatment of Helicobacter pylori infection in Korea, 2013 revised edition]. Korean J Gastroenterol. 2013;62:3-26. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 119] [Cited by in RCA: 97] [Article Influence: 8.8] [Reference Citation Analysis (1)] |
| 17. | Graham DY, Lu H, Yamaoka Y. A report card to grade Helicobacter pylori therapy. Helicobacter. 2007;12:275-278. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 244] [Cited by in RCA: 315] [Article Influence: 17.5] [Reference Citation Analysis (0)] |
| 18. | O'Connor JP, Taneike I, O'Morain C. Improving compliance with helicobacter pylori eradication therapy: when and how? Therap Adv Gastroenterol. 2009;2:273-279. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 43] [Cited by in RCA: 66] [Article Influence: 4.7] [Reference Citation Analysis (0)] |
| 19. | Dore MP, Tadeu V, Are B, Mura I, Fanciulli G, Massarelli G, Piana A. Efficacy of a "Rescue" Ciprofloxacin-Based Regimen for Eradication of Helicobacter pylori Infection after Treatment Failures. Gastroenterol Res Pract. 2012;2012:484591. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 8] [Cited by in RCA: 9] [Article Influence: 0.7] [Reference Citation Analysis (0)] |
| 20. | Chung JW, Lee GH, Jeong JY, Lee SM, Jung JH, Choi KD, Song HJ, Jung HY, Kim JH. Resistance of Helicobacter pylori strains to antibiotics in Korea with a focus on fluoroquinolone resistance. J Gastroenterol Hepatol. 2012;27:493-497. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 35] [Cited by in RCA: 38] [Article Influence: 2.9] [Reference Citation Analysis (0)] |
| 21. | Choi WJ, Do GW, Lee GH. Changes in the antibiotic resistance rates of Helicobacter pylori strains isolated in tertiary medical institutions in Seoul. Korean J Med. 2014;86:308-313. [RCA] [DOI] [Full Text] [Cited by in Crossref: 8] [Cited by in RCA: 7] [Article Influence: 0.6] [Reference Citation Analysis (0)] |
| 22. | Thung I, Aramin H, Vavinskaya V, Gupta S, Park JY, Crowe SE, Valasek MA. Review article: the global emergence of Helicobacter pylori antibiotic resistance. Aliment Pharmacol Ther. 2016;43:514-533. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 410] [Cited by in RCA: 553] [Article Influence: 61.4] [Reference Citation Analysis (2)] |
| 23. | Lee JY, Kim N, Park KS, Kim HJ, Park SM, Baik GH, Shim KN, Oh JH, Choi SC, Kim SE, Kim WH, Park SY, Kim GH, Lee BE, Jo Y, Hong SJ. Comparison of sequential therapy and amoxicillin/tetracycline containing bismuth quadruple therapy for the first-line eradication of Helicobacter pylori: a prospective, multi-center, randomized clinical trial. BMC Gastroenterol. 2016;16:79. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 17] [Cited by in RCA: 14] [Article Influence: 1.6] [Reference Citation Analysis (0)] |
| 24. | Chi CH, Lin CY, Sheu BS, Yang HB, Huang AH, Wu JJ. Quadruple therapy containing amoxicillin and tetracycline is an effective regimen to rescue failed triple therapy by overcoming the antimicrobial resistance of Helicobacter pylori. Aliment Pharmacol Ther. 2003;18:347-353. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 47] [Cited by in RCA: 46] [Article Influence: 2.1] [Reference Citation Analysis (0)] |
| 25. | Dang Y, Reinhardt JD, Zhou X, Zhang G. The effect of probiotics supplementation on Helicobacter pylori eradication rates and side effects during eradication therapy: a meta-analysis. PLoS One. 2014;9:e111030. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 92] [Cited by in RCA: 108] [Article Influence: 9.8] [Reference Citation Analysis (1)] |
| 26. | Shi X, Zhang J, Mo L, Shi J, Qin M, Huang X. Efficacy and safety of probiotics in eradicating Helicobacter pylori: A network meta-analysis. Medicine (Baltimore). 2019;98:e15180. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 99] [Cited by in RCA: 92] [Article Influence: 15.3] [Reference Citation Analysis (0)] |
| 27. | Ribaldone DG, Fagoonee S, Astegiano M, Durazzo M, Morgando A, Sprujevnik T, Giordanino C, Baronio M, De Angelis C, Saracco GM, Pellicano R. Rifabutin-Based Rescue Therapy for Helicobacter pylori Eradication: A Long-Term Prospective Study in a Large Cohort of Difficult-to-Treat Patients. J Clin Med. 2019;8. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 38] [Cited by in RCA: 41] [Article Influence: 6.8] [Reference Citation Analysis (0)] |
| 28. | Zhuge L, Wang Y, Wu S, Zhao RL, Li Z, Xie Y. Furazolidone treatment for Helicobacter Pylori infection: A systematic review and meta-analysis. Helicobacter. 2018;23:e12468. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 34] [Cited by in RCA: 49] [Article Influence: 7.0] [Reference Citation Analysis (0)] |
| 29. | Zullo A, Ierardi E, Hassan C, De Francesco V. Furazolidone-based therapies for Helicobacter pylori infection: a pooled-data analysis. Saudi J Gastroenterol. 2012;18:11-17. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 33] [Cited by in RCA: 36] [Article Influence: 2.8] [Reference Citation Analysis (0)] |
| 30. | Choi YI, Jeong SH, Chung JW, Park DK, Kim KO, Kwon KA, Kim YJ, So S, Lee JH, Jeong JY, Lee SM. Rifabutin and Furazolidone Could Be the Candidates of the Rescue Regimen for Antibiotic-Resistant H. pylori in Korea. Can J Infect Dis Med Microbiol. 2019;2019:9351801. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 10] [Cited by in RCA: 11] [Article Influence: 1.8] [Reference Citation Analysis (1)] |
| 31. | Graham DY, Lu H. Furazolidone in Helicobacter pylori therapy: misunderstood and often unfairly maligned drug told in a story of French bread. Saudi J Gastroenterol. 2012;18:1-2. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 30] [Cited by in RCA: 31] [Article Influence: 2.4] [Reference Citation Analysis (0)] |