Published online Aug 7, 2017. doi: 10.3748/wjg.v23.i29.5405
Peer-review started: January 11, 2017
First decision: February 9, 2017
Revised: March 7, 2017
Accepted: May 19, 2017
Article in press: May 19, 2017
Published online: August 7, 2017
Processing time: 210 Days and 16.9 Hours
To evaluated the differences in knowledge, adherence, attitudes, and beliefs about medicine in adolescents with inflammatory bowel disease (IBD) attending transition clinics.
We prospectively enrolled patients from July 2012 to June 2013. All adolescents who attended a tertiary-centre-based dedicated IBD transition clinic were invited to participate. Adolescent controls were recruited from university-affiliated gastroenterology offices. Participants completed questionnaires about their disease and reported adherence to prescribed therapy. Beliefs in Medicine Questionnaire was used to evaluate patients’ attitudes and beliefs. Beliefs of medication overuse, harm, necessity and concerns were rated on a Likert scale. Based on necessity and concern ratings, attitudes were then characterized as accepting, ambivalent, skeptical and indifferent.
One hundred and twelve adolescents were included and 59 attended transition clinics. Self-reported adherence rates were poor, with only 67.4% and 56.8% of patients on any IBD medication were adherent in the transition and control groups, respectively. Adolescents in the transition cohort held significantly stronger beliefs that medications were necessary (P = 0.0035). Approximately 20% of adolescents in both cohorts had accepting attitudes toward their prescribed medicine. However, compared to the control group, adolescents in the transition cohort were less skeptical of (6.8% vs 20.8%) and more ambivalent (61% vs 34%) (OR = 0.15; 95%CI: 0.03-0.75; P = 0.02) to treatment.
Attendance at dedicated transition clinics was associated with differences in attitudes in adolescents with IBD.
Core tip: Inflammatory bowel disease (IBD) transition clinics may improve care of adolescents. Comparing ones attended transition clinics to those didn’t, this study assessed adolescents with IBD’s self-reported adherence to prescribed therapy and evaluated their attitudes and beliefs using Beliefs in Medicine Questionnaire. Self-reported adherence rates were poor in both cohorts. Adolescents in the transition cohort held significantly stronger beliefs that medications were necessary. They were also less skeptical of and more ambivalent to prescribed treatments. Attendance at dedicated transition clinics was associated with differences in attitudes in adolescents with IBD.
- Citation: Fu N, Jacobson K, Round A, Evans K, Qian H, Bressler B. Transition clinic attendance is associated with improved beliefs and attitudes toward medicine in patients with inflammatory bowel disease. World J Gastroenterol 2017; 23(29): 5405-5411
- URL: https://www.wjgnet.com/1007-9327/full/v23/i29/5405.htm
- DOI: https://dx.doi.org/10.3748/wjg.v23.i29.5405
Inflammatory bowel disease (IBD) is a chronic, idiopathic, immune-mediated illness that typically follows a relapsing and remitting course[1]. Pediatric-onset IBD accounts for up to 25% of all IBD cases, and its natural history and health impacts can differ greatly from adult-onset IBD[2,3]. Adolescence is a critical period for physical, cognitive, emotional, and social development. Compared to their peers, adolescents with IBD often face additional challenges such as difficult decisions concerning therapeutic options, trouble with medication adherence, and potential anxiety surrounding health-related appointments and interventions[4].
Two commonly identified issues surrounding the transition of adolescents with IBD are this patient population’s limited disease-specific knowledge and poor adherence to medical therapy[5,6]. These are important elements for the establishment of self-management skills and protection against future disease flares. Many adult gastroenterologists feel the deficiencies in understanding among adolescents relating to their condition and treatment are prevalent and consequently represent a substantial barrier to successful transition[5,6]. Previous studies have demonstrated that adolescents with IBD could provide basic disease-related information such as their diagnosis and current medication; however, participants were unable to recall specifics pertaining to disease extent, medication side effects, previous surgery, and results of investigations[7,8]. Nonadherence to medical therapy in adolescents with IBD is reported to be very high, ranging from 50% to 75%[9-12]. Typical reasons for nonadherence to medication among adolescents with IBD include forgetfulness, feeling well, lack of time, interference with other activities, medication side effects, and complex medical regimens[9-12]. Medication nonadherence can lead to undesirable consequences such as disease flares, health deterioration, and increased healthcare utilization[13-16]. Important predictors of adherence to medical therapy are patients’ beliefs and attitudes toward medicine[17-22].
The aim of this study was to explore the attitudes toward, and beliefs about, medical therapy among adolescents with IBD. Additionally, this study compared the differences in disease-specific knowledge and adherence to medical therapy between adolescents who attended the IBD transition clinics and those who did not.
British Columbia (BC) is the third largest province in Canada with a population of 4.4 million[23]. Ninety-five percent of all children diagnosed with IBD in BC are treated at the BC Children’s Hospital (BCCH), a tertiary-care academic hospital. An IBD transition clinic was established at BCCH in 2010. Annually, approximately 80 adolescents with IBD graduate from BCCH, typically at around 17 to 18 years of age.
Adolescents selected to attend the transition clinics are usually those with a more complex disease course or those receiving anti-tumor necrosis factor (anti-TNF) agents. Many of them have disease phenotypes such as extensive or pancolitis; upper tract, extended small bowel involvement, stricturing or penetrating Crohn’s disease (CD); or have required surgical resections. Adolescents who have had adverse effects or intolerances to conventional IBD medications are also chosen. Approximately half of the adolescents graduating from BCCH attended the transition clinics.
Adolescents attending the IBD transition clinics were jointly assessed by adult and pediatric IBD specialists and nurses. Most adolescents, prior to transfer of care, attended the transition clinic up to twice in their last year at BCCH. The transition clinics served as the final summative clinical visits. During the transition clinic visits, medical/surgical histories, past/current medications, and future therapeutic plans of the patient were thoroughly reviewed. Both adult and pediatric IBD specialists discussed each patient in detail with each other and with the patient to establish a comprehensive plan. Adolescents were reminded of the importance of IBD medications, potential side effects of the medications, and the need for regular monitoring of blood work. Pediatric IBD nurse assisted in creating a one-page concise summary for the patients to take home after the clinic. Complete summaries were later prepared and provided to patients and the adult gastroenterologists who received the transfer of care.
Another form of care transfer was direct referrals to adult gastroenterologist. Selected documents depicting patients’ diagnosis, therapies and progressions were sent to the receiving adult gastroenterologists along with a discharge/transfer summary from BCCH. The adolescents then attend regular adult gastroenterology clinics for consultation and meet their physicians at the appointment.
Unlike direct care transfer, the transition clinics provide an intermediate step for the adolescents to become acquainted with the differences in practice styles between pediatric and adult settings. The transition clinic visit is longer but not as frequent as the usual adult gastroenterology appointment. Both pediatric and adult IBD nurses are present to give additional support. Although adolescents graduating from BCCH are typically referred to adult gastroenterologists based on geographical locations and their residence in BC, many adolescents attended the transitions clinics are preferentially referred to university-affiliated IBD specialists as opposed to community-based gastroenterologists.
We prospectively enrolled IBD patients from July 1st, 2012 to June 30th, 2013. All adolescents within 1 year of their attendance at the BCCH IBD transition clinics were invited to participate as the study cohort. Aged-matched patients who did not attend the transition clinics but were being treated at a university affiliated gastroenterology office served as the control cohort.
Study invitation letters and web-linked questionnaires were delivered via secured personalized emails to potential participants (73 transition and 75 control). Follow-up telephone calls, to provide further details or to clarify any questions, were placed to all adolescents interested in participating in the study. All available clinical charts were reviewed and compared with responses provided by the participants. All participants provided signed informed consent. The study received full institutional ethics approval.
All participants completed an online questionnaire regarding their disease and their adherence to prescribed medical therapy (see Supplementary Table 1). Attitudes and beliefs about medical therapy were assessed using the Beliefs about Medicine Questionnaire (BMQ) (see Supplementary Table 2), a validated 17-question tool evaluating patient opinions on medical therapy[24,25]. The BMQ assesses both specific and general beliefs about medicine; specific beliefs include those relating to either necessity or concerns, while general beliefs include those relating to overuse or harm. Respondents indicate their degree of agreement with each statement about medicine on a five-point Likert scale (1 = strongly disagree, 5 = strongly agree). The BMQ has been used in various chronic diseases and recently in IBD[20,21,24], and has consistently demonstrated greater adherence to be associated with a stronger perception of necessity and fewer concerns relating to treatment[26]. Additionally, the BMQ allows for further analysis of patient attitudes toward medicine by delineation of respondents into one of 4 attitudinal groups: “accepting” (high necessity, low concerns), “ambivalent” (high necessity, high concerns), “skeptical” (low necessity, high concerns), or “indifferent” (low necessity, low concerns)[21,22].
Disease-specific knowledge among the adolescents was assessed by comparing responses provided on the questionnaire to information available in their clinical charts. If necessary, the patient’s healthcare professionals were consulted for clarification. Level of basic knowledge such as the type of IBD (CD or ulcerative colitis, without specifying disease location) and previous gastrointestinal surgery (yes or no) was formally evaluated by comparing physician records and patient responses. Information on disease phenotypes and current IBD-specific medication (yes or no for mesalamines, immunomodulators, anti-TNF agents) was also collected. The general concern among healthcare professionals about the increased risks of loss to follow up in the adolescent population prompted us to collect the self-reported physician contact/follow up rate. Self-reported adherence to prescribed medical therapy was recorded and subsequently dichotomized by classifying those who were missing less than 30% of prescribed therapy as adherent. This cuff-off, as opposed to conventional 20%, was selected to account for previously observed high nonadherence rate in the adolescent population. Self-reporting of adherence was used for ease of data collection although it carries a known risk of overestimation[22,27,28].
The BMQ responses were examined in several ways, as per published literature[21,24,25]. The individual scores for each subclass (necessity, concerns, overuse, harm) were summed and analyzed as a continuous variable or a scaled score by dividing the summed value with the number of questions in each subclass. A higher score indicated stronger agreement with the scale constructs. A necessity-concerns differential was also calculated by subtracting the summed concerns score from the summed necessity score. A higher differential signified greater belief in the necessity of treatment. Finally, to explore attitudes toward medicine in a clinical meaningful way, we divided the patients into one of four attitudinal groups (“accepting”, “ambivalent”, “skeptical”, or “indifferent”) based on whether their scaled necessity and concerns scores were above or below midpoint (< 3 or ≥ 3). Self-reported medication adherence of participants was then correlated to their attitudes and beliefs. Comparisons between adolescents who attended the transition clinics and those did not were also performed.
Statistical analyses were conducted using SAS Version 9.2 (Cary, NC, United States). The sample size calculation determined that 42 participants per cohort was required in order to detect a 30% difference while assuming 40% nonadherence rate in the study cohort and bearing an 80% power. All statistical tests were two-sided with a 0.05 significance level.
Continuous variables were summarized as means and standard deviations. Categorical variables were reported as counts and percentages. Comparisons between groups were conducted using two-sample t-test for continuous data and χ2 or Fisher’s exact test when appropriate for categorical data.
Logistic regression modelling was performed to explore the association of transition clinic use with medication adherence. Attitudes toward medicine were analyzed with the use of a multinomial logistic regression model. Linear regression was conducted to assess the impact of the transition clinic on beliefs about medicine. All models were adjusted for pre-specified confounding variables including age, gender, diagnosis, disease duration, surgical history, and medication use.
A total of 112 adolescents participated in the study. Of those, 59 attended transition clinics. The response rates were 81% and 71% for transition and control group, respectively. Most adolescents continued to have physician contact (with family physicians or adult gastroenterologists) after leaving the pediatric setting (transition vs control: 85.1% vs 87.3%). The predominant reasons for care discontinuation were difficulty obtaining accepting physicians and a belief that physician assessments were not needed.
Demographic data were similar between cohorts (Table 1). However, the transition group had a higher proportion of patients with CD (79.7% vs 64.2%), and on both anti-TNF medication and immunomodulator therapy (23.2% vs 9.3%), compared to controls. Similar levels of disease-specific knowledge and self-reported adherence rates were found between cohorts (Table 2). Approximately 80% of the adolescents reported their basic knowledge (diagnosis and surgical history) in concordance with physician reports. Awareness of specific disease phenotype was similar in both transition and control groups (65.5% vs 60.4%; P = 0.69). Self-reported adherence to any medication was poor among adolescents with IBD in both transition and control groups (67.4% vs 56.8%). No significant difference was observed between the two groups on self-reported adherence (OR = 1.38; 95%CI: 0.49-3.86; P = 0.54).
| Transition | Control | P value | |
| n (%) ormean ± SD | n (%) ormean ± SD | ||
| Gender | |||
| Female | 23 (40.4) | 31 (56.4) | 0.13 |
| Diagnosis | |||
| CD | 47 (79.7) | 34 (64.2) | 0.07 |
| UC/IBDU | 12 (20.3) | 19 (35.8) | |
| Age (yr) | |||
| At diagnosis | 13.0 ± 2.9 | 13.0 ± 3.8 | 0.87 |
| Current | 19.7 ± 1.3 | 20.6 ± 1.2 | 0.0012 |
| Disease duration (yr) | 6.9 ± 3.2 | 7.6 ± 3.9 | 0.30 |
| Prior GI surgery | 13 (22.0) | 12 (21.8) | 0.98 |
| Medication1 | |||
| 5-ASA | 14 (25.0) | 20 (37.0) | 0.24 |
| IM | 17 (30.4) | 12 (22.2) | 0.33 |
| Anti-TNF | 6 (10.7) | 6 (11.1) | 1.00 |
| Combination | 13 (23.2) | 5 (9.3) | 0.07 |
| Any | 43 (76.8) | 37 (68.5) | 0.33 |
| Regular blood work | 45 (80.4) | 30 (55.6) | 0.012 |
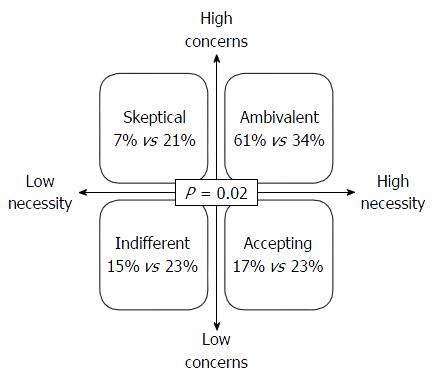
The beliefs about and attitudes toward medicine among the adolescents were assessed using the BMQ. Adolescents in the transition cohort held significantly stronger beliefs that medications were necessary (3.4 vs 3.0, P = 0.0035), but had comparable concerns (3.2 vs 3.1, P = 0.29) toward those medications (Table 3). A higher necessity-concern differential was also noted in the transition cohort (0.2 vs -0.06, P = 0.11). The higher differential signifies a greater belief in the necessity of treatment. Both groups had comparable general beliefs (overuse or harm) about medicine. Overall, approximately 20% of adolescents had an accepting attitude toward their prescribed medication. However, the transition cohort was less likely to be skeptical (6.8% vs 20.8%) and more likely to be ambivalent (61% vs 34%) to their treatment compared to controls (OR = 0.15, 95%CI: 0.03-0.75; P = 0.02) (Figure 1).
| Transition | Control | P value | |
| n (%) ormean ± SD | n (%) ormean ± SD | ||
| Beliefs about medicine1 | |||
| Specific | |||
| Necessity | 17.2 ± 3.8 | 15.0 ± 4.0 | 0.00353 |
| 3.4 ± 0.8 | 3.0 ± 0.8 | ||
| Concern | 16.1 ± 4.0 | 15.3 ± 3.5 | 0.29 |
| 3.2 ± 0.8 | 3.1 ± 0.7 | ||
| Differential | 1.1 ± 4.7 | -0.3 ± 4.7 | 0.11 |
| 0.2 ± 0.9 | -0.06 ± 0.9 | ||
| General | |||
| Overuse | 9.7 ± 2.5 | 9.4 ± 2.9 | 0.63 |
| 3.2 ± 0.8 | 3.1 ± 1.0 | ||
| Harm | 14.9 ± 2.7 | 14.7 ± 2.8 | 0.70 |
| 3.7 ± 0.7 | 3.7 ± 0.7 | ||
| Attitudes toward medicine2 | |||
| Accepting | 10 (16.9) | 12 (22.6) | 0.45 |
| Ambivalent | 36 (61.0) | 18 (34.0) | 0.0043 |
| Skeptical | 4 (6.8) | 11 (20.8) | 0.033 |
| Indifferent | 9 (15.3) | 12 (22.6) | 0.32 |
| Composite | 0.023 |
Appropriate transitioning of pediatric patients with IBD into an adult setting is an important and complex process. Common difficulties identified among adolescents with IBD include poor knowledge related to their disease and a lack of adherence to medical therapy[5,6]. Despite the potential for inflation of adherence rates due to self-reporting[27], we still observed rates as low as 56.8% for medication and 60% for blood work. These data are comparable to previously reported adherence rates of 50%-75% for adolescents with IBD[9-12]. Similarly, adherence rates among adolescents with other chronic diseases such as asthma and diabetes, as well as those who have undergone procedures where subsequent nonadherence to medication can greatly compromise treatment efficacy (e.g., hematopoietic stem cell transplant), are also reported to be low (40%-80%)[15,29,30].
Studies have investigated factors that may influence adherence rates in adolescents. Some modifiable aspects include lifestyle, medication regimen, social/healthcare support, knowledge, beliefs, and attitudes[9,10,17,18,21,22,25,30-34]. A substantial proportion of adolescents in this study had general basic knowledge about their disease type. However, it was difficult to detect subtle and more refined differences in knowledge between the two groups. Similar to reports by Fishman et al[7] and Benchimol et al[8], we noted a limited number of adolescents who were aware of their disease location and/or phenotype. Compared to controls, slightly more adolescents in the transition cohort were better informed of their disease phenotype. This may be a result of more intense education and healthcare support provided[30,32-34]. Indeed, increased knowledge and awareness of disease has been associated with better adherence in adolescents with other chronic diseases typically diagnosed in childhood (e.g., asthma)[30,34].
Attitudes and beliefs regarding medication are strong predictors of adherence to medical therapy[21,22,24-26]. Compared to controls, adolescents in the transition cohort showed significantly stronger beliefs about the necessity of medical therapy. They were also more ambivalent and less skeptical toward medication. Patients with IBD who have an “accepting” attitude have been found to be least likely to be nonadherent compared to those with one of the other three attitudes[21,22]. Augmented education sessions such as review on the importance of IBD medications, their side effects and the need for regular monitoring blood works provided in the transition clinics may contribute to the observed difference in attitudes. It is likely that adolescents attending the transition clinics are more aware of the necessity of medical therapy, but remain concerned about the potential side effects, leading to their ambivalent attitudes. Nonetheless, that our study did not demonstrate a significant difference between cohorts in adherence to therapy, suggests that other factors, together with beliefs and attitudes, influence adherence[9,10,17,18,21,22,25,30-34]. Therefore, clinicians not only should thoroughly review planned medical therapy with the adolescents but also explore other potential aspects such as finance, cultural practices, family and social stability that may impact adherence[9,10,17,32].
One potential limitation of this study was that the control cohort included patients from a university-affiliated clinic, many of whom were treated by an IBD specialist and as such may have received education comparable to those in the transition group. Therefore, some of the observed differences may be diminished. Additionally, characteristics such as socioeconomic status, ethnicities and locations of residence (urban vs. rural) may affect the adolescents’ beliefs and were not collected in this study.
To our knowledge, this is the first study assessing the impact of transition clinics on the knowledge, attitudes, and beliefs of medical therapy in adolescent patients with IBD. This study also explored the differences in adherence rates. Future studies should focus on determining ways to improve knowledge and adherence among adolescents, as well as the impact of transition clinics on long-term outcomes. Moreover, healthcare professionals should work on determining factors that are essential to conducting successful transition clinics.
In conclusion, adolescents with IBD were found to have low overall adherence to medical therapy, despite exhibiting adequate general knowledge about their disease. Attendance at dedicated transition clinics was associated with adolescents who held a stronger belief that medical therapies were necessary and carried attitudes that were more ambivalent (high necessity, high concerns), but less skeptical (low necessity, high concerns) toward their prescribed therapies.
Commonly identified issues surrounding the transition of adolescents with inflammatory bowel disease (IBD) are this patient population’s limited disease-specific knowledge and poor adherence to medical therapy. Medication nonadherence can lead to undesirable consequences. Important predictors of adherence to medical therapy are patients’ beliefs and attitudes toward medicine.
Adolescence is a vulnerable period. Determining key factors associated with successful transition of adolescents with IBD to adult service may minimize complications. Previous studies have demonstrated that adolescents with IBD could only provide basic disease-related information. Nonadherence to medical therapy in adolescents with IBD is reported to be very high, ranging from 50% to 75%.
This study was the first to show that dedicated transition clinics were associated with differences in beliefs and attitudes. Adolescents who attended held a stronger belief that medical therapies were necessary and carried attitudes that were more ambivalent (high necessity, high concerns), but less skeptical (low necessity, high concerns) toward their prescribed therapies.
This study showed association between attendance to transition clinic with differences in beliefs and attitudes towards medical therapy. Future studies should focus on determining the impact of transition clinics on long-term outcomes. Moreover, healthcare professionals should work on determining factors that are essential to conducting successful transition clinics.
IBD, encompassing Crohn’s disease and ulcerative colitis, is a chronic, idiopathic, immune-mediated illness that typically follows a relapsing and remitting course. Transition is defined as the purposeful planned movement of adolescents and young adults from child-centered to adult-oriented healthcare system. Beliefs about Medicine Questionnaire (BMQ) is a validated 17-question tool that evaluates both specific and general beliefs about medicine. BMQ allows for further analysis of attitudes toward medicine.
The authors reported transition clinic attendance is associated with improved beliefs and attitudes toward medicine in patients with IBD. The article is informative and well-presented.
Manuscript source: Unsolicited manuscript
Specialty type: Gastroenterology and hepatology
Country of origin: Canada
Peer-review report classification
Grade A (Excellent): A
Grade B (Very good): B
Grade C (Good): 0
Grade D (Fair): 0
Grade E (Poor): 0
P- Reviewer: Chiba T, Rosen DJ S- Editor: Gong ZM L- Editor: A E- Editor: Zhang FF
| 1. | Cosnes J, Gower-Rousseau C, Seksik P, Cortot A. Epidemiology and natural history of inflammatory bowel diseases. Gastroenterology. 2011;140:1785-1794. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1390] [Cited by in RCA: 1558] [Article Influence: 111.3] [Reference Citation Analysis (1)] |
| 2. | Benchimol EI, Fortinsky KJ, Gozdyra P, Van den Heuvel M, Van Limbergen J, Griffiths AM. Epidemiology of pediatric inflammatory bowel disease: a systematic review of international trends. Inflamm Bowel Dis. 2011;17:423-439. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 749] [Cited by in RCA: 711] [Article Influence: 50.8] [Reference Citation Analysis (0)] |
| 3. | Abraham BP, Mehta S, El-Serag HB. Natural history of pediatric-onset inflammatory bowel disease: a systematic review. J Clin Gastroenterol. 2012;46:581-589. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 158] [Cited by in RCA: 140] [Article Influence: 10.8] [Reference Citation Analysis (0)] |
| 4. | Goodhand J, Hedin CR, Croft NM, Lindsay JO. Adolescents with IBD: the importance of structured transition care. J Crohns Colitis. 2011;5:509-519. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 82] [Cited by in RCA: 95] [Article Influence: 6.8] [Reference Citation Analysis (0)] |
| 5. | Hait EJ, Barendse RM, Arnold JH, Valim C, Sands BE, Korzenik JR, Fishman LN. Transition of adolescents with inflammatory bowel disease from pediatric to adult care: a survey of adult gastroenterologists. J Pediatr Gastroenterol Nutr. 2009;48:61-65. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 120] [Cited by in RCA: 119] [Article Influence: 7.4] [Reference Citation Analysis (0)] |
| 6. | Sebastian S, Jenkins H, McCartney S, Ahmad T, Arnott I, Croft N, Russell R, Lindsay JO. The requirements and barriers to successful transition of adolescents with inflammatory bowel disease: differing perceptions from a survey of adult and paediatric gastroenterologists. J Crohns Colitis. 2012;6:830-844. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 107] [Cited by in RCA: 98] [Article Influence: 7.5] [Reference Citation Analysis (0)] |
| 7. | Fishman LN, Barendse RM, Hait E, Burdick C, Arnold J. Self-management of older adolescents with inflammatory bowel disease: a pilot study of behavior and knowledge as prelude to transition. Clin Pediatr (Phila). 2010;49:1129-1133. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 73] [Cited by in RCA: 76] [Article Influence: 5.1] [Reference Citation Analysis (0)] |
| 8. | Benchimol EI, Walters TD, Kaufman M, Frost K, Fiedler K, Chinea Z, Zachos M. Assessment of knowledge in adolescents with inflammatory bowel disease using a novel transition tool. Inflamm Bowel Dis. 2011;17:1131-1137. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 76] [Cited by in RCA: 84] [Article Influence: 6.0] [Reference Citation Analysis (0)] |
| 9. | Ingerski LM, Baldassano RN, Denson LA, Hommel KA. Barriers to oral medication adherence for adolescents with inflammatory bowel disease. J Pediatr Psychol. 2010;35:683-691. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 54] [Cited by in RCA: 63] [Article Influence: 3.9] [Reference Citation Analysis (0)] |
| 10. | Hommel KA, Baldassano RN. Brief report: Barriers to treatment adherence in pediatric inflammatory bowel disease. J Pediatr Psychol. 2010;35:1005-1010. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 50] [Cited by in RCA: 55] [Article Influence: 3.4] [Reference Citation Analysis (0)] |
| 11. | Greenley RN, Stephens KA, Nguyen EU, Kunz JH, Janas L, Goday P, Schurman JV. Vitamin and mineral supplement adherence in pediatric inflammatory bowel disease. J Pediatr Psychol. 2013;38:883-892. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 17] [Cited by in RCA: 20] [Article Influence: 1.7] [Reference Citation Analysis (0)] |
| 12. | Mackner LM, Crandall WV. Oral medication adherence in pediatric inflammatory bowel disease. Inflamm Bowel Dis. 2005;11:1006-1012. [PubMed] |
| 13. | Kane S, Huo D, Aikens J, Hanauer S. Medication nonadherence and the outcomes of patients with quiescent ulcerative colitis. Am J Med. 2003;114:39-43. [PubMed] |
| 14. | Cervený P, Bortlík M, Kubena A, Vlcek J, Lakatos PL, Lukás M. Nonadherence in inflammatory bowel disease: results of factor analysis. Inflamm Bowel Dis. 2007;13:1244-1249. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 114] [Cited by in RCA: 120] [Article Influence: 6.7] [Reference Citation Analysis (0)] |
| 15. | McGrady ME, Hommel KA. Medication adherence and health care utilization in pediatric chronic illness: a systematic review. Pediatrics. 2013;132:730-740. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 153] [Cited by in RCA: 161] [Article Influence: 13.4] [Reference Citation Analysis (0)] |
| 16. | Higgins PD, Rubin DT, Kaulback K, Schoenfield PS, Kane SV. Systematic review: impact of non-adherence to 5-aminosalicylic acid products on the frequency and cost of ulcerative colitis flares. Aliment Pharmacol Ther. 2009;29:247-257. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 125] [Cited by in RCA: 128] [Article Influence: 8.0] [Reference Citation Analysis (2)] |
| 17. | Hanghøj S, Boisen KA. Self-reported barriers to medication adherence among chronically ill adolescents: a systematic review. J Adolesc Health. 2014;54:121-138. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 121] [Cited by in RCA: 135] [Article Influence: 12.3] [Reference Citation Analysis (0)] |
| 18. | Kane SV. Systematic review: adherence issues in the treatment of ulcerative colitis. Aliment Pharmacol Ther. 2006;23:577-585. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 214] [Cited by in RCA: 223] [Article Influence: 11.7] [Reference Citation Analysis (0)] |
| 19. | Sewitch MJ, Abrahamowicz M, Barkun A, Bitton A, Wild GE, Cohen A, Dobkin PL. Patient nonadherence to medication in inflammatory bowel disease. Am J Gastroenterol. 2003;98:1535-1544. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 229] [Cited by in RCA: 222] [Article Influence: 10.1] [Reference Citation Analysis (0)] |
| 20. | Ediger JP, Walker JR, Graff L, Lix L, Clara I, Rawsthorne P, Rogala L, Miller N, McPhail C, Deering K. Predictors of medication adherence in inflammatory bowel disease. Am J Gastroenterol. 2007;102:1417-1426. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 197] [Cited by in RCA: 216] [Article Influence: 12.0] [Reference Citation Analysis (0)] |
| 21. | Horne R, Parham R, Driscoll R, Robinson A. Patients’ attitudes to medicines and adherence to maintenance treatment in inflammatory bowel disease. Inflamm Bowel Dis. 2009;15:837-844. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 193] [Cited by in RCA: 205] [Article Influence: 12.8] [Reference Citation Analysis (0)] |
| 22. | Moshkovska T, Stone MA, Clatworthy J, Smith RM, Bankart J, Baker R, Wang J, Horne R, Mayberry JF. An investigation of medication adherence to 5-aminosalicylic acid therapy in patients with ulcerative colitis, using self-report and urinary drug excretion measurements. Aliment Pharmacol Ther. 2009;30:1118-1127. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 40] [Cited by in RCA: 47] [Article Influence: 2.9] [Reference Citation Analysis (0)] |
| 23. | Census Population of BC and Canada. Victoria, BC: BCStats, 2011. Available from: http://www.bcstats.gov.bc.ca/StatisticsBySubject/Census/2011Census/PopulationHousing/BCCanada.aspx. |
| 24. | Horne R, Weinman J, Hankins M. The beliefs about medicines questionnaire: The development and evaluation of a new method for assessing the cognitive representation of medication. Psychol Health. 1999;14:1-24. |
| 25. | Horne R, Weinman J. Patients’ beliefs about prescribed medicines and their role in adherence to treatment in chronic physical illness. J Psychosom Res. 1999;47:555-567. [PubMed] |
| 26. | Horne R, Chapman SC, Parham R, Freemantle N, Forbes A, Cooper V. Understanding patients’ adherence-related beliefs about medicines prescribed for long-term conditions: a meta-analytic review of the Necessity-Concerns Framework. PLoS One. 2013;8:e80633. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 701] [Cited by in RCA: 783] [Article Influence: 65.3] [Reference Citation Analysis (0)] |
| 27. | Hommel KA, Davis CM, Baldassano RN. Objective versus subjective assessment of oral medication adherence in pediatric inflammatory bowel disease. Inflamm Bowel Dis. 2009;15:589-593. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 106] [Cited by in RCA: 108] [Article Influence: 6.8] [Reference Citation Analysis (0)] |
| 28. | Rapoff MA. Management of adherence and chronic rheumatic disease in children and adolescents. Best Pract Res Clin Rheumatol. 2006;20:301-314. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 30] [Cited by in RCA: 34] [Article Influence: 1.8] [Reference Citation Analysis (0)] |
| 29. | McGrady ME, Williams SN, Davies SM, Pai AL. Adherence to outpatient oral medication regimens in adolescent hematopoietic stem cell transplant recipients. Eur J Oncol Nurs. 2014;18:140-144. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 36] [Cited by in RCA: 39] [Article Influence: 3.3] [Reference Citation Analysis (0)] |
| 30. | Koster ES, Philbert D, Winters NA, Bouvy ML. Adolescents’ inhaled corticosteroid adherence: the importance of treatment perceptions and medication knowledge. J Asthma. 2015;52:431-436. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 42] [Cited by in RCA: 53] [Article Influence: 4.8] [Reference Citation Analysis (0)] |
| 31. | Greenley RN, Stephens M, Doughty A, Raboin T, Kugathasan S. Barriers to adherence among adolescents with inflammatory bowel disease. Inflamm Bowel Dis. 2010;16:36-41. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 46] [Cited by in RCA: 49] [Article Influence: 3.3] [Reference Citation Analysis (0)] |
| 32. | Reed-Knight B, Lewis JD, Blount RL. Association of disease, adolescent, and family factors with medication adherence in pediatric inflammatory bowel disease. J Pediatr Psychol. 2011;36:308-317. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 48] [Cited by in RCA: 48] [Article Influence: 3.2] [Reference Citation Analysis (0)] |
| 33. | Waters BM, Jensen L, Fedorak RN. Effects of formal education for patients with inflammatory bowel disease: a randomized controlled trial. Can J Gastroenterol. 2005;19:235-244. [PubMed] |
| 34. | Mosnaim G, Li H, Martin M, Richardson D, Belice PJ, Avery E, Ryan N, Bender B, Powell L. Factors associated with levels of adherence to inhaled corticosteroids in minority adolescents with asthma. Ann Allergy Asthma Immunol. 2014;112:116-120. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 42] [Cited by in RCA: 44] [Article Influence: 3.7] [Reference Citation Analysis (0)] |