Published online May 28, 2017. doi: 10.3748/wjg.v23.i20.3744
Peer-review started: January 19, 2017
First decision: February 10, 2016
Revised: February 26, 2016
Accepted: March 21, 2017
Article in press: March 21, 2017
Published online: May 28, 2017
Processing time: 129 Days and 22.2 Hours
Schwannomas are neurogenic tumors that arise from the neural sheaths of peripheral nerves. These tumors can be located in any area of the human body; the most common locations are the head, neck, trunk and extremities. Pancreatic schwannomas are very rare. Over the past 40 years, only 67 cases of pancreatic schwannomas have been reported in the English literature. Here we present a case of pancreatic schwannoma in a 62-year-old male. The tumor was revealed by ultrasound and computed tomography in the neck and body of the pancreas. An accurate diagnosis was difficult to obtain preoperatively. The patient consented to the performance of a laparotomy, and the mass was found in the neck and body of the pancreas and successfully treated using a spleen-preserving distal pancreatectomy with splenic artery and vein preservation. The procedure has only been reported in one other case of pancreatic schwannoma; here we present the second reported case. Macroscopically, the tumor was well circumscribed, gray-white in color and 3.3 cm × 2.8 cm in size. Microscopically, the tumor cells were spindle-shaped and had a palisading arrangement with no atypia, which are results compatible with a benign tumor. Both hypercellular and hypocellular areas were visible. Immunohistochemically, the tumor cells were strongly positive for S-100 protein. The tumor was definitively diagnosed as a schwannoma of the pancreatic neck and body. The patient was followed for 72 mo and has been doing well without any complications.
Core tip: Over the past 40 years, only 67 cases of pancreatic schwannoma have been reported in the English literature. An accurate preoperative diagnosis is difficult to obtain. Here, we present the case of a patient with a pancreatic schwannoma who underwent spleen-preserving distal pancreatectomy. This surgical intervention has only been previously reported in one case of pancreatic schwannoma. After surgery, the patient recovered quickly and had a good prognosis. In this case report, we share our experience in the diagnosis and treatment of a rare pancreatic schwannoma and performed a literature review to deepen the understanding of the subject.
- Citation: Xu SY, Wu YS, Li JH, Sun K, Hu ZH, Zheng SS, Wang WL. Successful treatment of a pancreatic schwannoma by spleen-preserving distal pancreatectomy. World J Gastroenterol 2017; 23(20): 3744-3751
- URL: https://www.wjgnet.com/1007-9327/full/v23/i20/3744.htm
- DOI: https://dx.doi.org/10.3748/wjg.v23.i20.3744
Schwannomas are mesenchymal tumors that originate from the Schwann cells of peripheral nerves[1]. Schwannomas are generally encapsulated, and over 90% are benign[2]. These tumors can occur in patients of all ages, with an equal frequency in males and females, and are most often reported in patients between 20 and 50 years of age[3]. A considerable number of these patients are asymptomatic, and the tumors are found incidentally[4]. Schwannomas can show either monosomy 22 or loss of 22q material; the definitive pathogenesis of the tumor remains uncertain[1]. Occasionally, the tumor can become cystic, hemorrhagic, calcified or even ossified[5]. Surgery may be the optimal treatment for schwannomas, after which patients generally have a good prognosis[6]. Although schwannomas can develop in any part of the body, the most common locations include the head, neck, trunk and extremities[7]. Schwannomas in the pancreas are extremely rare. To our knowledge, over the past 40 years, only 67 cases have been reported in the English literature[8-68]. In the present study, we present a case of a pancreatic schwannoma that was successfully treated using a spleen-preserving distal pancreatectomy technique and performed a review of the available literature.
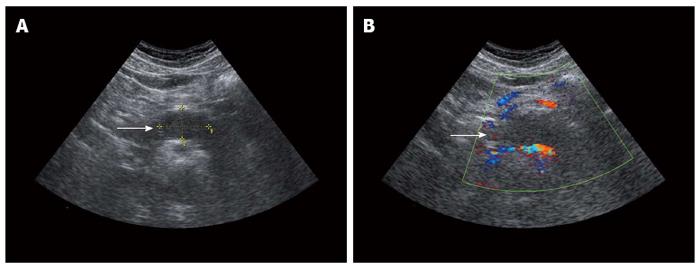
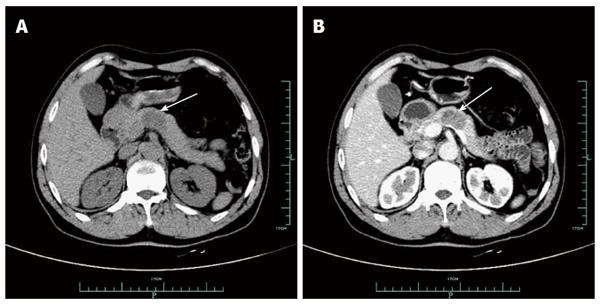
On January 6, 2011, a 62-year-old male was referred to our hospital because of a pancreatic mass that was found on ultrasound during a routine health examination at the local hospital. His abdomen was soft, non-tender, and non-distended, with no evidence of a palpable or pulsatile mass. There was no history of weight loss or trauma and no family history of significant disease. Abnormal laboratory results included an international normalized ratio of 1.16 (normal range: 0.85-1.15) and a thrombin time of 21.7 s (normal range: 14.5-21.5). Other laboratory results, which included tumor markers, were normal. The ultrasound showed a well-defined, low-density lesion measuring 3.7 cm × 2.3 cm in the neck and body of the pancreas (Figure 1A). No blood flow signal was detected within the lesion on color Doppler ultrasound (Figure 1B). An unenhanced computed tomography (CT) scan revealed a well-marginated and hypodense mass measuring 2.8 cm × 1.9 cm in the pancreatic neck and body (Figure 2A). On contrast-enhanced CT, the mass was slightly and heterogeneously enhanced (Figure 2B). Endoscopic ultrasound-fine needle aspiration (EUS-FNA) was also performed. However, we failed to acquire a tumor sample. Although imaging results were obtained, the mass in the pancreatic neck and body was still unable to be accurately diagnosed.
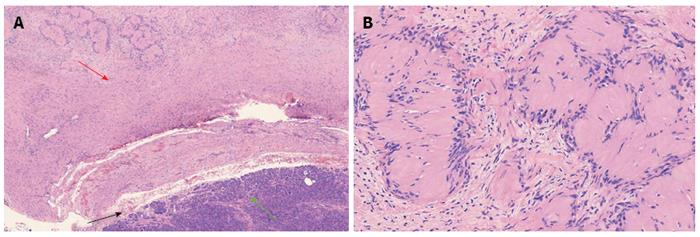
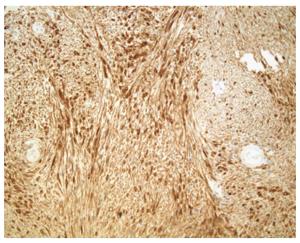
The patient consented to the performance of a laparotomy, and the mass was observed to originate from the pancreatic neck and body. We performed a spleen-preserving distal pancreatectomy with preservation of the splenic artery and vein. Intraoperative frozen pathology revealed a pancreatic schwannoma. Macroscopically, the mass was observed in the pancreatic neck and body, gray-white in color and 3.3 cm × 2.8 cm in size. Microscopically, the tumor cells were spindle-shaped and had a palisading arrangement with no atypia, which are results that are compatible with a benign tumor. Both hypercellular and hypocellular areas were visible (Figure 3). Immunohistochemically, the tumor cells were strongly positive for S-100 protein (Figure 4), but negative for SMA, CD34 and CD117. The tumor was definitively diagnosed as a schwannoma of the pancreatic neck and body. After surgery, the patient recovered smoothly and was discharged from the hospital 10 d later. The patient was followed for 72 mo and has been doing well without any further complications.
Schwannomas are neoplasms that originate from Schwann cells in nerve sheaths[69]. More than 90% of schwannomas are benign, and they account for approximately 5% of benign soft-tissue neoplasms[3]. Malignant schwannomas are rare and are usually associated with von Recklinghausen’s disease[70]. Schwannomas can occur in patients of all ages, with equal frequencies in males and females, and cases are most often reported in patients between 20 and 50 years of age[3]. Almost any site in the human body can be involved, although the head, neck, and extremities are the most reported areas of tumor development[71]. Schwannomas that originate from the nerve sheaths of the pancreas are extremely rare. Intra-pancreatic innervation includes the perivascular plexus, peri-acinous plexus and peri-insular plexus. These three plexuses connect with each other to form a net-like structure. However, the type of nerve fibers that produce the origination of pancreatic schwannomas has not yet been described. To our knowledge, over the past 40 years, only 67 cases of pancreatic schwannoma have been reported in the English literature[8-68]. Table 1 summarizes the important available clinicopathological characteristics of these 68 cases, which include the present case. Continuous variables are summarized as the mean ± SD and the range. Statistical analyses were conducted using SPSS version 20.0 for Windows (SPSS Inc., Chicago, IL).
| n (%) or mean ± SD (range) | |
| Age (yr) (n = 67) | |
| Mean | 55.67 ± 15.13 (20-87) |
| Sex (male/female), (male %) (n = 67) | 30/37 (44.78) |
| Symptoms1 (n = 67) | |
| Asymptomatic | 25 (37.31) |
| Symptomatic | |
| Abdominal pain | 29 (43.28) |
| Weight loss | 9 (13.43) |
| Back pain | 4 (5.97) |
| Nausea/vomiting | 3 (4.48) |
| Anorexia | 2 (2.99) |
| Anemia | 2 (2.99) |
| Melena | 2 (2.99) |
| Jaundice | 2 (2.99) |
| Dyspepsia | 1 (1.49) |
| Abdominal discomfort | 1 (1.49) |
| Abdominal mass | 1 (1.49) |
| Location (n = 68) | |
| Head | 26 (38.24) |
| Head/body | 3 (4.41) |
| Neck/body | 1 (1.47) |
| Body | 14 (20.59) |
| Body/tail | 7 (10.29) |
| Tail | 8 (11.76) |
| Uncinate process | 8 (11.76) |
| Mean size (cm) (n = 63) | 5.75 ± 4.52 (1-20) |
| Benign | 59 (5.21 ± 3.89) (1-20) |
| Malignant | 4 (13.75 ± 6.24) (7-20) |
| Operation (n = 68) | |
| PD2 | 20 (29.41) |
| PPPD | 2 (2.94) |
| DP + splenectomy3 | 16 (23.53) |
| DP + splenic preservation | 2 (2.94) |
| Enucleation | 10 (14.71) |
| Central pancreatectomy | 1 (1.47) |
| Unresectable | 2 (2.94) |
| Refused | 1 (1.47) |
| Not specified | 13 (19.12) |
| Histology (n = 68) | |
| Malignant | 5 (7.35) |
| Benign | 62 (91.18) |
| Not specified | 1 (1.47) |
| Nature of tumor (n = 68) | |
| Solid | 21 (30.88) |
| Cystic | 27 (39.71) |
| Solid and cystic | 14 (20.59) |
| Not specified | 6 (8.82) |
| Mean follow-up months (n = 30) | 22.23 ± 19.56 (3-67) |
| No. of deaths | 0 |
Because the clinical symptoms and imaging characteristics of schwannomas are nonspecific, the accurate preoperative diagnosis of a pancreatic schwannoma is nearly impossible. A definitive diagnosis relies on the combined findings of the histopathological and immunohistochemical examination of surgical specimens. Microscopically, pancreatic schwannomas are usually encapsulated with varying relative amounts of the two histologic components of hypercellular Antoni A areas and hypocellular Antoni B areas[22]. The former is composed of closely packed spindle cells with occasional nuclear palisading. The latter consists of loosely arranged tumor cells and abundant myxoid stroma[13]. Over 90% of pancreatic schwannomas are benign. Thus far, only 5 (7.35%) malignant pancreatic schwannomas have been reported in the English literature[29,64,66-68]. Immunohistochemical staining showed that schwannomas are positive for S-100 protein, but negative for desmin, smooth muscle myosin, SMA, CD34 and CD117[23,72].
Imaging modalities including ultrasound, CT and magnetic resonance imaging (MRI) have a certain diagnostic value but lack specificity. On ultrasound, a pancreatic schwannoma is usually shown as a well-marginated hypodense lesion. On unenhanced CT scans, schwannomas are usually well-defined hypodense lesions with an associated capsule. Schwannomas with high Antoni A areas show a high density and appear inhomogenous. Schwannomas with high Antoni B areas appear cystic and show a low density[17]. On contrast-enhanced CT scans, Antoni A areas are enhanced, while Antoni B areas are unenhanced[14]. On MRI, schwannomas usually appear hypointense in T1-weighted images and inhomogeneous and hyperintense in T2-weighted images[23]. EUS-FNA may also be valuable for the preoperative diagnosis of schwannomas. Li et al[35] reported a pancreatic schwannoma that was definitively diagnosed by EUS-FNA. In the present study, EUS-FNA was also performed; however, we failed to acquire a sufficient sample of the tumor.
Surgery is the curative treatment for pancreatic schwannomas, and most cases are treated by laparotomy. Only one case of pancreatic schwannoma was treated using minimally invasive laparoscopic surgery (1.47%)[21]. Enucleation has been reported in 10 (14.71%) cases. Patients treated by minimally invasive surgery might have less pain and faster recovery. Since the tumor can be located in different sections of the pancreas, surgical approaches may vary. In the present case, we performed a spleen-preserving distal pancreatectomy for the mass that was found in the neck and body of the pancreas. To date, spleen-preserving distal pancreatectomy has only been reported in one other case of pancreatic schwannoma[38]; here we describe the second reported case. Compared with the traditional distal pancreatectomy and splenectomy for tumors in the body or tail of the pancreas, spleen-preserving distal pancreatectomy can not only offer complete resection of the tumor but also preserve the spleen. After complete removal of the tumor, patients usually have a good prognosis.
In conclusion, the finding of a schwannoma in the pancreas is extremely rare. Over the past 40 years, only 67 cases of pancreatic schwannoma have been reported in the English literature. Although multiple imaging modalities are currently available, it is challenging to obtain an accurate diagnosis prior to the performance of surgery, which is the optimal treatment for pancreatic schwannomas. Spleen-preserving distal pancreatectomy has only been reported in one previous case. After complete resection of the tumor, patients with pancreatic schwannoma usually have a good prognosis.
On January 6, 2011, a 62-year-old male was referred to the authors’ hospital because of a pancreatic mass found during a routine health examination at the local hospital.
The patient’s abdomen was soft, non-tender, and non-distended, with no evidence of a palpable or a pulsatile mass.
Intraductal papillary mucinous neoplasm, mucinous cystic neoplasm, solid pseudopapillary tumor, pancreatic endocrine tumor or pancreatic ductal adenocarcinoma.
Abnormal laboratory results included an international normalized ratio of 1.16 (normal range: 0.85-1.15) and a thrombin time of 21.7 s (normal range: 14.5-21.5). Other laboratory results, including tumor markers, were normal.
Ultrasound showed a well-defined, low-density lesion measuring 3.7 cm × 2.3 cm in the pancreatic neck and body. No blood flow signal was detected by color Doppler ultrasound within the lesion. An unenhanced CT scan revealed a well-marginated and hypodense mass measuring 2.8 cm × 1.9 cm in the pancreatic neck and body. On contrast-enhanced CT, the mass was slightly and heterogeneously enhanced. Although they obtained these imaging results, the mass in the pancreatic neck and body was still unable to be definitively diagnosed.
Macroscopically, the mass was shown in the pancreatic neck and body, gray-white in color and 3.3 cm × 2.8 cm in size. Microscopically, the tumor cells were spindle-shaped and had a palisading arrangement with no atypia, which are results that are compatible with a benign tumor. Both hypercellular and hypocellular areas were visible. Immunohistochemically, the tumor cells were strongly positive for S-100 protein, but negative for SMA, CD34 and CD117. The tumor was definitively diagnosed as a schwannoma of the pancreatic neck and body.
The patient underwent a spleen-preserving distal pancreatectomy.
Schwannoma in the pancreas is extremely rare. Over the past 40 years, only 67 cases of pancreatic schwannomas have been reported in the English literature. To date, the use of a spleen-preserving distal pancreatectomy has only been reported in one other case.
Imaging modalities, including ultrasound, CT and magnetic resonance imaging, have a certain diagnostic value but lack specificity in the diagnosis of pancreatic schwannoma. Surgery is the curative treatment for the tumor. Since the tumor can be located in different sections of the pancreas, surgical approaches may vary. After complete resection of the tumor, patients with pancreatic schwannomas usually have a good prognosis.
This study shares the experience in the diagnosis and the treatment of a rare pancreatic schwannoma with an accompanying literature review to deepen the understanding of the subject. The information in this paper is useful for readers.
Manuscript source: Unsolicited manuscript
Specialty type: Gastroenterology and hepatology
Country of origin: China
Peer-review report classification
Grade A (Excellent): A
Grade B (Very good): 0
Grade C (Good): C
Grade D (Fair): 0
Grade E (Poor): 0
P- Reviewer: Bandyopadhyay SK, Nickel F S- Editor: Qi Y L- Editor: Wang TQ E- Editor: Wang CH
| 1. | Le Guellec S. Nerve sheath tumours. Ann Pathol. 2015;35:54-70. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 18] [Cited by in RCA: 21] [Article Influence: 1.9] [Reference Citation Analysis (0)] |
| 2. | Xu SY, Guo H, Shen Y, Sun K, Xie HY, Zhou L, Zheng SS, Wang WL. Multiple schwannomas synchronously occurring in the porta hepatis, liver, and gallbladder: first case report. Medicine (Baltimore). 2016;95:e4378. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 10] [Cited by in RCA: 13] [Article Influence: 1.4] [Reference Citation Analysis (0)] |
| 3. | Das Gupta TK, Brasfield RD. Tumors of peripheral nerve origin: benign and malignant solitary schwannomas. CA Cancer J Clin. 1970;20:228-233. [PubMed] |
| 4. | Tao L, Xu S, Ren Z, Lu Y, Kong X, Weng X, Xie Z, Hu Z. Laparoscopic resection of benign schwannoma in the hepatoduodenal ligament: A case report and review of the literature. Oncol Lett. 2016;11:3349-3353. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 10] [Cited by in RCA: 11] [Article Influence: 1.2] [Reference Citation Analysis (0)] |
| 5. | Xu SY, Sun K, Xie HY, Zhou L, Zheng SS, Wang WL. Hemorrhagic, calcified, and ossified benign retroperitoneal schwannoma: First case report. Medicine (Baltimore). 2016;95:e4318. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 12] [Cited by in RCA: 19] [Article Influence: 2.1] [Reference Citation Analysis (0)] |
| 6. | Bhattacharyya AK, Perrin R, Guha A. Peripheral nerve tumors: management strategies and molecular insights. J Neurooncol. 2004;69:335-349. [PubMed] |
| 7. | Ariel IM. Tumors of the peripheral nervous system. CA Cancer J Clin. 1983;33:282-299. [PubMed] |
| 8. | Pecero-Hormigo MD, Costo-Campoamor A, Cordero PG, Fernandez-Gonzalez N, Molina-Infante J. Pancreatic tail schwannoma. Gastroenterol Hepatol. 2016; Epub ahead of print. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 5] [Cited by in RCA: 5] [Article Influence: 0.6] [Reference Citation Analysis (0)] |
| 9. | Crinò SF, Bernardoni L, Manfrin E, Parisi A, Gabbrielli A. Endoscopic ultrasound features of pancreatic schwannoma. Endosc Ultrasound. 2016;5:396-398. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 18] [Cited by in RCA: 36] [Article Influence: 4.0] [Reference Citation Analysis (0)] |
| 10. | Xu SY, Sun K, Owusu-Ansah KG, Xie HY, Zhou L, Zheng SS, Wang WL. Central pancreatectomy for pancreatic schwannoma: A case report and literature review. World J Gastroenterol. 2016;22:8439-8446. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in CrossRef: 12] [Cited by in RCA: 15] [Article Influence: 1.7] [Reference Citation Analysis (0)] |
| 11. | Nishikawa T, Shimura K, Tsuyuguchi T, Kiyono S, Yokosuka O. Contrast-enhanced harmonic EUS of pancreatic schwannoma. Gastrointest Endosc. 2016;83:463-464. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 12] [Cited by in RCA: 15] [Article Influence: 1.7] [Reference Citation Analysis (0)] |
| 12. | Mourra N, Calvo J, Arrive L. Incidental Finding of Cystic Pancreatic Schwannoma Mimicking a Neuroendocrine Tumor. Appl Immunohistochem Mol Morphol. 2016;24:149-150. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 7] [Cited by in RCA: 8] [Article Influence: 0.9] [Reference Citation Analysis (0)] |
| 13. | Duma N, Ramirez DC, Young G, Nikias G, Karpeh M, Bamboat ZM. Enlarging Pancreatic Schwannoma: A Case Report and Review of the Literature. Clin Pract. 2015;5:793. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 14] [Cited by in RCA: 15] [Article Influence: 1.5] [Reference Citation Analysis (0)] |
| 14. | Ohbatake Y, Makino I, Kitagawa H, Nakanuma S, Hayashi H, Nakagawara H, Miyashita T, Tajima H, Takamura H, Ninomiya I. A case of pancreatic schwannoma - The features in imaging studies compared with its pathological findings: Report of a case. Clin J Gastroenterol. 2014;7:265-270. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 19] [Cited by in RCA: 20] [Article Influence: 1.8] [Reference Citation Analysis (0)] |
| 15. | Kim JY, Song JS, Park H, Byun JH, Song KB, Kim KP, Kim SC, Hong SM. Primary mesenchymal tumors of the pancreas: single-center experience over 16 years. Pancreas. 2014;43:959-968. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 45] [Cited by in RCA: 55] [Article Influence: 5.0] [Reference Citation Analysis (0)] |
| 16. | J D, R S, K C, Devi NR. Pancreatic schwannoma - a rare case report. J Clin Diagn Res. 2014;8:FD15-FD16. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 4] [Cited by in RCA: 14] [Article Influence: 1.3] [Reference Citation Analysis (0)] |
| 17. | Ciledag N, Arda K, Aksoy M. Pancreatic schwannoma: A case report and review of the literature. Oncol Lett. 2014;8:2741-2743. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 14] [Cited by in RCA: 16] [Article Influence: 1.5] [Reference Citation Analysis (0)] |
| 18. | Val-Bernal JF, Mayorga M, Sedano-Tous MJ. Schwannomatosis presenting as pancreatic and submandibular gland schwannoma. Pathol Res Pract. 2013;209:817-822. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 13] [Cited by in RCA: 10] [Article Influence: 0.8] [Reference Citation Analysis (0)] |
| 19. | Poosawang W, Kiatkungwankai P. Pancreatic schwannoma: A case report and review of literature. J Med Assoc Thai. 2013;96:112-116. [PubMed] |
| 20. | Barresi L, Tarantino I, Granata A, Traina M. Endoscopic ultrasound-guided fine-needle aspiration diagnosis of pancreatic schwannoma. Dig Liver Dis. 2013;45:523. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 10] [Cited by in RCA: 12] [Article Influence: 1.0] [Reference Citation Analysis (0)] |
| 21. | Abu-Zaid A, Azzam A, Abou Al-Shaar H, Alshammari AM, Amin T, Mohammed S. Pancreatic tail schwannoma in a 44-year-old male: a case report and literature review. Case Rep Oncol Med. 2013;2013:416713. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 3] [Cited by in RCA: 9] [Article Influence: 0.8] [Reference Citation Analysis (0)] |
| 22. | Di Benedetto F, Ballarin R, Spaggiari M, Pecchi A, Gerunda GE. Role of intraoperative ultrasonography for pancreatic schwannoma. J Surg Oncol. 2012;105:859-860. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 5] [Cited by in RCA: 6] [Article Influence: 0.5] [Reference Citation Analysis (0)] |
| 23. | Moriya T, Kimura W, Hirai I, Takeshita A, Tezuka K, Watanabe T, Mizutani M, Fuse A. Pancreatic schwannoma: Case report and an updated 30-year review of the literature yielding 47 cases. World J Gastroenterol. 2012;18:1538-1544. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in CrossRef: 50] [Cited by in RCA: 52] [Article Influence: 4.0] [Reference Citation Analysis (0)] |
| 24. | Paik KY, Choi SH, Heo JS, Choi DW. Solid tumors of the pancreas can put on a mask through cystic change. World J Surg Oncol. 2011;9:79. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 19] [Cited by in RCA: 20] [Article Influence: 1.4] [Reference Citation Analysis (0)] |
| 25. | Kim G, Choi YS, Kim HJ, Do JH, Park ES. Pancreatic benign schwannoma: combined with hemorrhage in an internal cyst. J Dig Dis. 2011;12:138-141. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 9] [Cited by in RCA: 10] [Article Influence: 0.7] [Reference Citation Analysis (0)] |
| 26. | Liegl B, Bodo K, Martin D, Tsybrovskyy O, Lackner K, Beham A. Microcystic/reticular schwannoma of the pancreas: a potential diagnostic pitfall. Pathol Int. 2011;61:88-92. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 21] [Cited by in RCA: 23] [Article Influence: 1.5] [Reference Citation Analysis (0)] |
| 27. | Kinhal VA, Ravishankar TH, Melapure AI, Jayaprakasha G, Range Gowda BC. Pancreatic schwannoma: Report of a case and review of literature. Indian J Surg. 2010;72:296-298. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 13] [Cited by in RCA: 14] [Article Influence: 0.9] [Reference Citation Analysis (0)] |
| 28. | Dorsey F, Taggart MW, Fisher WE. Image of the month. Pancreatic schwannoma. Arch Surg. 2010;145:913-914. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 9] [Cited by in RCA: 11] [Article Influence: 0.7] [Reference Citation Analysis (0)] |
| 29. | Stojanovic MP, Radojkovic M, Jeremic LM, Zlatic AV, Stanojevic GZ, Jovanovic MA, Kostov MS, Katic VP. Malignant schwannoma of the pancreas involving transversal colon treated with en-bloc resection. World J Gastroenterol. 2010;16:119-122. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 9] [Reference Citation Analysis (0)] |
| 30. | Suzuki S, Kaji S, Koike N, Harada N, Hayashi T, Suzuki M, Hanyu F, Ban S. Pancreatic schwannoma: a case report and literature review with special reference to imaging features. JOP. 2010;11:31-35. [PubMed] |
| 31. | Aggarwal G, Satsangi B, Shukla S, Lahoti BK, Mathur RK, Maheshwari A. Rare asymptomatic presentations of schwannomas in early adolescence: three cases with review of literature. Int J Surg. 2010;8:203-206. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 11] [Cited by in RCA: 14] [Article Influence: 0.9] [Reference Citation Analysis (0)] |
| 32. | Oshima M, Yachida S, Suzuki Y. Pancreatic schwannoma in a 32-year-old woman mimicking a solid-pseudopapillary neoplasm. Clin Gastroenterol Hepatol. 2010;8:e1-e2. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 9] [Cited by in RCA: 10] [Article Influence: 0.7] [Reference Citation Analysis (0)] |
| 33. | Mummadi RR, Nealon WH, Artifon EL, Fleming JB, Bhutani MS. Pancreatic Schwannoma presenting as a cystic lesion. Gastrointest Endosc. 2009;69:341; discussio 341. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 10] [Cited by in RCA: 13] [Article Influence: 0.8] [Reference Citation Analysis (0)] |
| 34. | Gupta A, Subhas G, Mittal VK, Jacobs MJ. Pancreatic schwannoma: literature review. J Surg Educ. 2009;66:168-173. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 27] [Cited by in RCA: 24] [Article Influence: 1.5] [Reference Citation Analysis (0)] |
| 35. | Li S, Ai SZ, Owens C, Kulesza P. Intrapancreatic schwannoma diagnosed by endoscopic ultrasound-guided fine-needle aspiration cytology. Diagn Cytopathol. 2009;37:132-135. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 33] [Cited by in RCA: 38] [Article Influence: 2.4] [Reference Citation Analysis (0)] |
| 36. | Tafe LJ, Suriawinata AA. Cystic pancreatic schwannoma in a 46-year-old man. Ann Diagn Pathol. 2008;12:296-300. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 11] [Cited by in RCA: 14] [Article Influence: 0.8] [Reference Citation Analysis (0)] |
| 37. | Hirabayashi K, Yasuda M, Umemura S, Itoh H, Itoh J, Yazawa N, Imaizumi T, Osamura RY. Cytological features of the cystic fluid of pancreatic schwannoma with cystic degeneration. A case report. JOP. 2008;9:203-208. [PubMed] |
| 38. | Okuma T, Hirota M, Nitta H, Saito S, Yagi T, Ida S, Okamura S, Chikamoto A, Iyama K, Takamori H. Pancreatic schwannoma: report of a case. Surg Today. 2008;38:266-270. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 14] [Cited by in RCA: 16] [Article Influence: 0.9] [Reference Citation Analysis (0)] |
| 39. | Tofigh AM, Hashemi M, Honar BN, Solhjoo F. Rare presentation of pancreatic schwannoma: a case report. J Med Case Rep. 2008;2:268. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 17] [Cited by in RCA: 20] [Article Influence: 1.2] [Reference Citation Analysis (0)] |
| 40. | Fasanella KE, Lee KK, Kaushik N. Clinical challenges and images in GI. Benign schwannoma of the pancreatic head. Gastroenterology. 2007;132:489, 830. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 8] [Cited by in RCA: 10] [Article Influence: 0.6] [Reference Citation Analysis (0)] |
| 41. | Di Benedetto F, Spaggiari M, De Ruvo N, Masetti M, Montalti R, Quntini C, Ballarin R, Di Sandro S, Costantini M, Gerunda GE. Pancreatic schwannoma of the body involving the splenic vein: case report and review of the literature. Eur J Surg Oncol. 2007;33:926-928. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 22] [Cited by in RCA: 25] [Article Influence: 1.3] [Reference Citation Analysis (0)] |
| 42. | Yu RS, Sun JZ. Pancreatic schwannoma: CT findings. Abdom Imaging. 2006;31:103-105. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 30] [Cited by in RCA: 35] [Article Influence: 1.8] [Reference Citation Analysis (0)] |
| 43. | Wu YL, Yan HC, Chen LR, Chen J, Gao SL, Li JT. Pancreatic benign schwannoma treated by simple enucleation: case report and review of literature. Pancreas. 2005;31:286-288. [PubMed] |
| 44. | Novellas S, Chevallier P, Saint Paul MC, Gugenheim J, Bruneton JN. MRI features of a pancreatic schwannoma. Clin Imaging. 2005;29:434-436. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 28] [Cited by in RCA: 31] [Article Influence: 1.6] [Reference Citation Analysis (0)] |
| 45. | Soumaoro LT, Teramoto K, Kawamura T, Nakamura N, Sanada T, Sugihara K, Arii S. Benign schwannoma of the pancreas. J Gastrointest Surg. 2005;9:288-290. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 16] [Cited by in RCA: 21] [Article Influence: 1.1] [Reference Citation Analysis (0)] |
| 46. | Bui TD, Nguyen T, Huerta S, Gu M, Hsiang D. Pancreatic schwannoma. A case report and review of the literature. JOP. 2004;5:520-526. [PubMed] |
| 47. | Akiyoshi T, Ueda Y, Yanai K, Yamaguchi H, Kawamoto M, Toyoda K, Hayashi T, Ohuchida J. Melanotic schwannoma of the pancreas: report of a case. Surg Today. 2004;34:550-553. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 25] [Cited by in RCA: 27] [Article Influence: 1.3] [Reference Citation Analysis (0)] |
| 48. | von Dobschuetz E, Walch A, Werner M, Hopt UT, Adam U. Giant ancient schwannoma of pancreatic head treated by extended pancreatoduodenectomy. Pancreatology. 2004;4:505-508. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 19] [Cited by in RCA: 19] [Article Influence: 0.9] [Reference Citation Analysis (0)] |
| 49. | Paranjape C, Johnson SR, Khwaja K, Goldman H, Kruskal JB, Hanto DW. Clinical characteristics, treatment, and outcome of pancreatic Schwannomas. J Gastrointest Surg. 2004;8:706-712. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 36] [Cited by in RCA: 39] [Article Influence: 1.9] [Reference Citation Analysis (0)] |
| 50. | Tan G, Vitellas K, Morrison C, Frankel WL. Cystic schwannoma of the pancreas. Ann Diagn Pathol. 2003;7:285-291. [PubMed] |
| 51. | Almo KM, Traverso LW. Pancreatic schwannoma: an uncommon but important entity. J Gastrointest Surg. 2001;5:359-363. [PubMed] |
| 52. | Lee JS, Kim HS, Jung JJ, Han SW, Kim YB. Ancient schwannoma of the pancreas mimicking a cystic tumor. Virchows Arch. 2001;439:697-699. [PubMed] |
| 53. | Morita S, Okuda J, Sumiyoshi K, Taketani M, Moriguchi A, Katsu K, Tanigawa N. Pancreatic Schwannoma: report of a case. Surg Today. 1999;29:1093-1097. [PubMed] |
| 54. | Brown SZ, Owen DA, O’Connell JX, Scudamore CH. Schwannoma of the pancreas: a report of two cases and a review of the literature. Mod Pathol. 1998;11:1178-1182. [PubMed] |
| 55. | Hsiao WC, Lin PW, Chang KC. Benign retroperitoneal schwannoma mimicking a pancreatic cystic tumor: case report and literature review. Hepatogastroenterology. 1998;45:2418-2420. [PubMed] |
| 56. | Feldman L, Philpotts LE, Reinhold C, Duguid WP, Rosenberg L. Pancreatic schwannoma: report of two cases and review of the literature. Pancreas. 1997;15:99-105. [PubMed] |
| 57. | Ferrozzi F, Bova D, Garlaschi G. Pancreatic schwannoma: report of three cases. Clin Radiol. 1995;50:492-495. [PubMed] |
| 58. | Sugiyama M, Kimura W, Kuroda A, Muto T. Schwannoma arising from peripancreatic nerve plexus. AJR Am J Roentgenol. 1995;165:232. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 14] [Cited by in RCA: 17] [Article Influence: 0.6] [Reference Citation Analysis (0)] |
| 59. | Steven K, Burcharth F, Holm N, Pedersen IK. Single stage pancreaticoduodenectomy (Whipple’s procedure), radical cystectomy and bladder substitution with the urethral Kock reservoir. Case report. Scand J Urol Nephrol. 1994;28:199-200. [PubMed] |
| 60. | Melato M, Bucconi S, Marus W, Spivach A, Perulli A, Mucelli RP. The schwannoma: an uncommon type of cystic lesion of the pancreas. Ital J Gastroenterol. 1993;25:385-387. [PubMed] |
| 62. | Urban BA, Fishman EK, Hruban RH, Cameron JL. CT findings in cystic schwannoma of the pancreas. J Comput Assist Tomogr. 1992;16:492-493. [PubMed] |
| 63. | Burd DA, Tyagi G, Bader DA. Benign schwannoma of the pancreas. AJR Am J Roentgenol. 1992;159:675. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 18] [Cited by in RCA: 22] [Article Influence: 0.7] [Reference Citation Analysis (0)] |
| 64. | Coombs RJ. Case of the season. Malignant neurogenic tumor of duodenum and pancreas. Semin Roentgenol. 1990;25:127-129. [PubMed] |
| 65. | Liessi G, Barbazza R, Sartori F, Sabbadin P, Scapinello A. CT and MR imaging of melanocytic schwannomas; report of three cases. Eur J Radiol. 1990;11:138-142. [PubMed] |
| 66. | Walsh MM, Brandspigel K. Gastrointestinal bleeding due to pancreatic schwannoma complicating von Recklinghausen’s disease. Gastroenterology. 1989;97:1550-1551. [PubMed] |
| 67. | Eggermont A, Vuzevski V, Huisman M, De Jong K, Jeekel J. Solitary malignant schwannoma of the pancreas: report of a case and ultrastructural examination. J Surg Oncol. 1987;36:21-25. [PubMed] |
| 68. | Móller Pedersen V, Hede A, Graem N. A solitary malignant schwannoma mimicking a pancreatic pseudocyst. A case report. Acta Chir Scand. 1982;148:697-698. [PubMed] |
| 69. | Das Gupta TK, Brasfield RD, Strong EW, Hajdu SI. Benign solitary Schwannomas (neurilemomas). Cancer. 1969;24:355-366. [PubMed] |
| 70. | Trifero M, Frattaroli FM, Ciccone AM, Guadalaxara A, Oddi G, Pappalardo G. Retroperitoneal malignant schwannoma. A case report. Tumori. 1994;80:238-240. [PubMed] |
| 71. | Abell MR, Hart WR, Olson JR. Tumors of the peripheral nervous system. Hum Pathol. 1970;1:503-551. [PubMed] |
| 72. | Weiss SW, Langloss JM, Enzinger FM. Value of S-100 protein in the diagnosis of soft tissue tumors with particular reference to benign and malignant Schwann cell tumors. Lab Invest. 1983;49:299-308. [PubMed] |