Published online Oct 28, 2014. doi: 10.3748/wjg.v20.i40.14686
Revised: April 27, 2014
Accepted: June 2, 2014
Published online: October 28, 2014
Processing time: 366 Days and 18.9 Hours
Patients with liver cirrhosis exhibit several features of gut dysfunction which may contribute to the development of cirrhosis complications as well as have an impact on nutritional status and health-related quality of life. Gastrointestinal symptoms are common in cirrhosis and their pathophysiology probably involves factors related to liver disease severity, psychological distress, and gut dysfunction (e.g., increased gastric sensitivity to distension and delayed gut transit). They may lead to reduced food intake and, thus, may contribute to the nutritional status deterioration in cirrhotic patients. Although tense ascites appears to have a negative impact on meal-induced accommodation of the stomach, published data on gastric accommodation in cirrhotics without significant ascites are not unanimous. Gastric emptying and small bowel transit have generally been shown to be prolonged. This may be related to disturbances in postprandial glucose, insulin, and ghrelin levels, which, in turn, appear to be associated to insulin resistance, a common finding in cirrhosis. Furthermore, small bowel manometry disturbances and delayed gut transit may be associated with the development of small bowel bacterial overgrowth. Finally, several studies have reported intestinal barrier dysfunction in patients with cirrhosis (especially those with portal hypertension), which is related to bacterial translocation and permeation of intestinal bacterial products, e.g., endotoxin and bacterial DNA, thus potentially being involved in the pathogenesis of complications of liver cirrhosis.
Core tip: Features of gut dysfunction are common in patients with cirrhosis and may have an impact on quality of life and nutritional status as well as contribute to the development of cirrhosis complications. Cirrhotic patients often report gastrointestinal symptoms. Their pathophysiology is complex, probably involving factors related to liver disease severity, psychological distress, and increased gastric sensitivity to distension as well as delayed gut transit. The latter is common in cirrhosis and may be related to postprandial glucose and hormone disturbances due to insulin resistance. Intestinal barrier dysfunction, potentially leading to bacterial translocation and permeation of bacterial products, has been frequently reported in cirrhotic patients, especially those with portal hypertension.
- Citation: Kalaitzakis E. Gastrointestinal dysfunction in liver cirrhosis. World J Gastroenterol 2014; 20(40): 14686-14695
- URL: https://www.wjgnet.com/1007-9327/full/v20/i40/14686.htm
- DOI: https://dx.doi.org/10.3748/wjg.v20.i40.14686
In recent years it has become widely recognized that liver cirrhosis may affect several organ systems such as the cardiovascular system[1,2], the respiratory system[3], the kidneys[4,5], and the skeletal system[6,7]. Cirrhosis has also been associated with varying degrees of malnutrition[8] and with alterations in the gastrointestinal (GI) tract[9]. Apart from the presence of structural changes in the GI tract, such as esophageal varices and portal hypertensive gastropathy, that may be the cause of GI bleeding and anemia, there have also been described abnormalities in the sensorimotor and barrier function of the gut in liver cirrhosis. These changes are of importance as they might contribute to malnutrition and health-related quality of life impairment in these patients, while impaired gut barrier function may also contribute to the development of cirrhosis complications, in particular bacterial infections.
Malnutrition is common in cirrhosis with a reported prevalence as high as 80%[8,10-13]. It is associated with increased morbidity and mortality[8] and it can compromise liver transplantation results[11]. Recently, severe muscle wasting (sarcopenia) has been shown to be present in 30%-41% of patients with cirrhosis and to be independently related to mortality in general[14] as well as in patients with hepatocellular cancer[15] and those listed for liver transplantation[16] in particular. Lean-mass depletion is also related to hepatic encephalopathy in liver transplant candidates with cirrhosis[17].
The pathogenesis of malnutrition in liver cirrhosis is not fully understood but poor dietary intake[8,18], increased energy expenditure[11,19-21], malabsorption[8,22] and poor synthetic capacity of the cirrhotic liver may be involved. Potential reasons for low energy intake include reduced appetite possibly associated with increased brain tryptophan availability[23], satiety due to ascites[24], poor palatability of low-sodium diets, and hepatic encephalopathy[8], GI symptoms[25,26], and gut dysfunction[27]. Increased glucose and lower ghrelin levels postprandially have also been suggested to be related to poor food intake and weight loss in cirrhosis[28]. Postprandial glucose and ghrelin alterations are probably associated with insulin resistance which is common in these patients[28].
Increased energy expenditure, although not a constant feature of cirrhosis, has also been reported to contribute to a negative energy balance[8,11,19-21,29-31]. Last, fat malabsorption has been reported to be frequent (especially in those with evidence of malnutrition)[22]. This may be related to the cholestasis often present in cirrhosis, but a reduction in the area of the intestinal absorptive surface has also been proposed in cirrhotics[32]. However, not all studies have found defective active absorption in these patients[22,33].
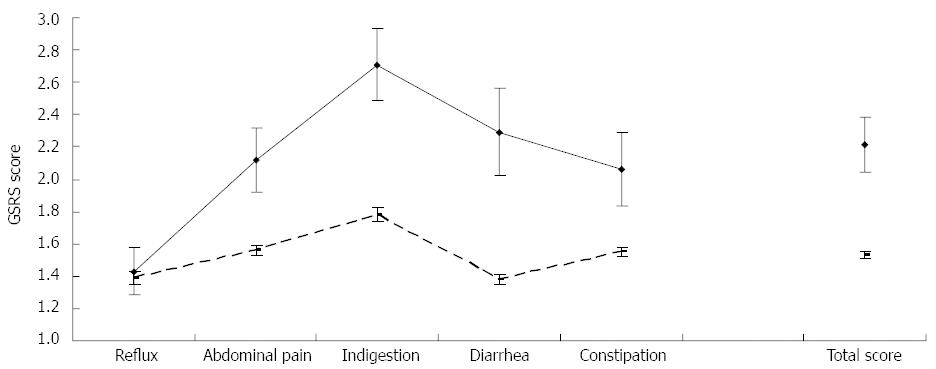
GI symptoms are common in cirrhotics compared to healthy controls (Figure 1)[25]. Overall, up to 80% of patients with cirrhosis have been reported to have one or more relevant GI symptoms[34]. The most common GI symptoms reported include abdominal bloating in 49.5% of patients, abdominal pain in 24%, belching in 18.7%, diarrhea in 13.3%, and constipation in 8%[34]. GI symptom severity appears to be related to liver disease severity[25], lactulose use[25], the presence of ascites[25], and psychological distress[26,34] as well as low serum testosterone levels[26]. The pathophysiology of GI symptoms, however, appears to be complex, and to also involve abnormalities in gut motility function as outlined later in this review. Although they improve following liver transplantation, GI symptoms remain of concern post-transplant, mainly due to diarrhea[26].
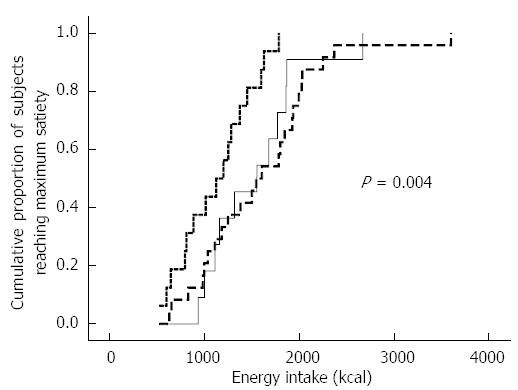
GI symptoms in cirrhosis are related to recent weight loss[25,26]. In an experiment in which subjects underwent a caloric satiation drinking test, patients with significant symptoms reached satiation earlier compared to patients without symptoms and healthy controls (Figure 2)[26]. Thus, GI symptoms appear to have an impact on meal induced satiety which may limit food intake. Last but not least, GI symptoms are associated with impaired physical and mental health-related quality of life in cirrhosis[25].
The structural effects of liver cirrhosis on the GI tract have been considered to be mainly associated with portal hypertension. A major endoscopic finding is varices most commonly located in the esophagus and/or the fundus of the stomach. Occasionally varices may be found in “ectopic” locations such as in the duodenum or in the rectum[35]. Esophageal varices develop in the majority of patients with cirrhosis, provided a long enough follow-up period[36,37]. They can be the site of GI bleeding, a potentially lethal complication[36,37].
Mucosal changes are also frequently encountered upon endoscopic examination of the GI tract in patients with cirrhosis[9,38]. Portal hypertensive intestinal vasculopathy is a term used to describe changes in the intestinal microcirculation secondary to longstanding portal hypertension[9]. Signs of portal hypertensive intestinal vasculopathy may be observed in all parts of the GI tract[9]. The prevalence of portal hypertensive gastropathy, with its characteristic mosaic appearance, has been reported in 20%-98% of cirrhotic patients[39], the wide variation probably being due to varying study quality and the different characteristics of the studied cirrhotic cohorts. Among 222 patients with cirrhosis without a history of variceal bleeding, medium or large esophageal varices, previous endoscopic therapy, or propranolol treatment, the prevalence of portal hypertensive gastropathy was reported to be 21.6%[40]. Major predictors of portal hypertensive gastropathy are the presence of esophageal varices and increased severity of cirrhosis[40], and it has been found to be associated to poor prognosis in cirrhotic patients[41]. Acute bleeding from portal hypertensive gastropathy has been reported to occur infrequently but may be severe[40,42], while chronic bleeding resulting in anemia may be a concern[40,42].
Cirrhotics compared to healthy controls, have been shown to have higher plasma gastrin[43] and higher prevalence of peptic ulcers[44,45]. In an endoscopic study, the annual incidence rate of peptic ulcers observed in 140 patients undergoing endoscopic follow-up was 4.3%[46]. Ulcers are associated with decompensated cirrhosis[47] but are asymptomatic in up to 2/3 of cases[46]. In a meta-analysis, the prevalence of helicobacter pylori infection has been found to be higher in cirrhotics with compared to those without peptic ulcer disease[48], but its role in the pathogenesis of peptic ulcers in these patients has been questioned[49] with alcohol consumtion and portal hypertension being hypothsized as major contributing factors[50]. Cirrhotic patients have a significantly increased risk of peptic ulcer bleeding and re-bleeding compared to the general population[51,52]. However, their prognosis during an ulcer bleeding episode may not differ drastically from that of non-cirrhotic patients[50].
In the fasting state, the proximal stomach smooth muscle maintains a tonic contractile activity[53-55]. During and after food ingestion, a relaxation of the proximal stomach occurs, providing the meal with a reservoir and enabling a volume increase without a rise in pressure (gastric accommodation reflex)[53,54,56-59].
Impaired gastric accommodation has been associated with upper GI symptoms, such as early satiety, bloating, and epigastric pain, in patients with functional dyspepsia[60,61], diabetes[62], prior fundoplication surgery[63], vagotomy and partial gastrectomy[64].
Gastric barostat studies, using a polyethylene balloon placed in the fundus of the stomach, are generally considered to be the gold standard for the evaluation of gastric accommodation[59]. However, other types of tests such as abdominal ultrasound, magnetic resonance imaging, and single-photon emission computed tomography (SPECT) are also commonly used[59].
Thus far, three studies have assessed gastric accommodation in cirrhosis. In an ultrasonographic study, performed in patients with alcoholic cirrhosis (n = 21), meal-induced accommodation was found to be reduced compared to controls[65]. Similarly, in a study employing SPECT, cirrhotic patients with tense ascites (n = 15) were found to have impaired accommodation compared to healthy controls[66]. Not unexpectedly, accommodation improved following large-volume paracentesis, resulting in an increase in caloric intake[66]. In a third study, in which a gastric barostat was employed, meal-induced accommodation was found to be increased in patients with cirrhosis (n = 16, none with tense ascites) compared to healthy controls[27]. Although energy intake (assessed by means of food diaries) was related to gastric accommodation in controls (r = 0.67, P < 0.05), this relationship was found to be disrupted in cirrhotic patients (P > 0.1). Thus, although it appears reasonable that meal-induced accommodation is impaired in the presence of tense ascites[66], to date, it remains unclear how it is affected in patients with cirrhosis of different etiologies without significant ascites.
Gut stimuli, specifically gastric distension by food ingestion, may induce GI symptoms. It has been reported that gastric tone is important in determining gastric sensitivity to distension[55,67] and that in particular gastric wall tension determines perception of gastric distension, at least below nociception levels[68].
Hypersensitivity to gastric distension, defined as enhanced sensitivity to balloon distension of the proximal stomach, is present in a subset of functional dyspepsia patients[69,70] and it is associated with weight loss[69]. In a single study investigating sensory thresholds at gastric distention, no significant difference was found between patients with cirrhosis (n = 16) and healthy controls[27]. However, sensory thresholds were related to gastrointestinal symptom severity and liver disease severity, expressed as the Child-Pugh and MELD scores (lower threshold with increasing symptom and liver disease severity)[27].
Another way of assessing gastric motor function is measurement of gastric emptying. Delayed gastric emptying has traditionally been considered a mechanism that contributes to symptom generation in patients with GI motility disorders and systemic diseases affecting the GI tract[71].
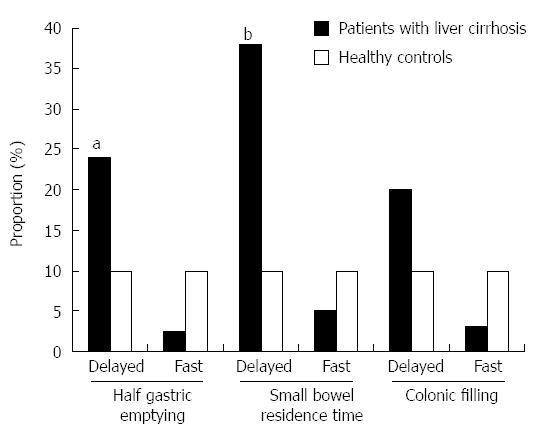
Most studies in cirrhosis have found gastric emptying to be delayed[72-76], but some controversy exists with other studies reporting normal[77-80], or accelerated[81] gastric emptying. Several factors may account for the divergence of results hitherto published, including selection of patient groups with different characteristics, selection of small patient groups or small control groups and use of different measurement methods. In a recent study from our group almost a quarter of stable patients with cirrhosis had delayed gastric emptying (Figure 3), which was associated with postprandial fullness and bloating[76]. Delayed gastric emptying was also related to postprandial hyperglycemia, hyperinsulinemia, and hypoghrelinemia[76]. The latter abnormalities appear to be associated to insulin resistance, which is frequent in cirrhosis. These findings are in accordance with published data showing that induced hyperglycemia is associated with reduced gut motility[82], delayed gastric emptying, decreased hunger[83], and increased postprandial symptoms[84] in healthy subjects. Physiological hyperglycemia has been shown to slow gastric emptying in diabetes mellitus[85] and healthy volunteers[86]. Experimental euglycemic hyperinsulinemia also impairs stomach and duodenal motility[87] and prolongs gastric emptying[87,88]. Gastric emptying time in cirrhosis has not been found to be related to portal pressure expressed as variceal pressure, as measured with a small pressure-sensitive capsule attached to a gastroscope[72] or as hepatic venous pressure gradient[80]. Finally, a role for autonomic dysfunction in the pathophysiology of delayed gastric emptying has also been proposed in these patients[89].
Manometry studies have shown disturbed gut motility in liver cirrhosis[90-93]. An abnormal propagation pattern of pressure waves with a high number of long clusters and frequent waves propagating in a retrograde fashion have been reported in cirrhotics, in particular those with portal hypertension[93]. Small bowel manometry disturbances have, anecdotally, been reported to improve following liver transplantation[94]. However, similar to investigations on gastric emptying, gut transit studies have shown contradictory results[72,77,79,80,95-97] in these patients, with most reporting prolonged small bowel transit times. In a recent study on gut transit in cirrhosis, about 35% of patients showed delayed small bowel residence times (Figure 3), which was related to increased diarrhea and abdominal pain[76]. These findings are in accordance with data from non-cirrhotic patients with unexplained GI symptoms whose small bowel transit was frequently slow in unexplained diarrheal disease[98]. Small bowel bacterial overgrowth is also common in cirrhosis[92,99] and appears to be related to liver disease severity[100], although it was only observed in patients with portal hypertension in one study[93]. Interestingly, patients with small bowel bacterial overgrowth have been also shown to have slower small bowel transit[72]. Furthermore, it has been reported that acceleration of orocecal transit using cisapride is associated with the abolishment of bacterial overgrowth in 80% of cirrhotic patients with bacterial overgrowth[101]. It is thus possible that delayed small bowel transit in cirrhosis may lead to the development of small bacterial overgrowth, which could contribute to the symptoms of abdominal pain and diarrhea. More importantly, small bacterial overgrowth has been speculated to be related to bacterial translocation and infectious complications, such as spontaneous bacterial peritonitis[92].
Intestinal permeability: The gut barrier includes immunogenic factors (such as mucosal lymphocytes and immunoglobulins) and the epithelial barrier (i.e., epithelial cells allowing selective intestinal permeability and their mucus layer)[102-104]. Central to the role of barrier function of the epithelial cells are the tight junctions and adherens junctions regulating paracellular transport[104]. As a barrier, the gut prevents the permeation of microorganisms or substances, such as luminal antigens and proinflammatory factors. At the same time it allows for selective permeation of certain substances such as nutrients[102,103].
Non-invasive methods have been used to assess gut barrier function by measuring the urinary excretion of orally administered test substances such as monosaccharides, disaccharides, and 51Cr-EDTA[102,105]. To address the complexity of factors affecting the results of gut permeability tests, the principle of differential urinary excretion of several test substances administered at the same time has been developed[105].
Bacterial infections are of concern in patients with cirrhosis, with spontaneous bacterial peritonitis being the most relevant[106,107]. They may occur as a consequence of repeated access of bacteria from the lumen to the mesenteric lymph nodes (translocation), and thereby to the ascitic fluid[108]. Intestinal permeability in liver cirrhosis has been variably reported as increased or normal[32,33,109-117]. Discrepancies among published studies may be partly explained by patient selection and choice of different measurement methods. Intestinal permeability assessed in cirrhosis with and without ascites by means of a four sugar permeability absorption test has been shown to be increased in the former group only[114]. Recent evidence suggests the presence of gut barrier dysfunction in patients with cirrhosis, especially those with severe liver disease[118]. For example Campillo et al[32] have found increased intestinal permeability in cirrhotics, particularly in those with bacterial infections. Intestinal hyperpermeability has also been shown to be more common in patients with a history of spontaneous bacterial peritonitis[117]. Increased permeability upon hospital admission has also been reported to be a predictor of bacterial infections in cirrhosis[119] and to be related to cirrhosis complications in general[118], although published studies are not unanimous[120].
Furthermore, permeation of intestinal bacterial products, e.g., endotoxin and bacterial DNA, may contribute to the activation of the immune system, derangement of the circulatory status, and induction of renal failure[108,121] as well as the development of hepatic encephalopathy in patients with cirrhosis[96,122,123]. This may occur through reduced hepatic clearance of endotoxin (component of the Gram negative bacterial wall) in cirrhotic patients and/or by means of increased cytokine production by the gut, for example by endotoxin-primed macrophages releasing nitric oxide and proinflammatory cytokines[124-127]. The proinflammatory status and nitric oxide release in cirrhosis may, in turn, disrupt further the gut barrier function[125], contribute to immune and hemodynamic derangement and cardiac dysfunction[124,126,128,129] as well as predict progression of liver disease[127]. Bacterial overgrowth, in particular overgrowth of pathogenic E.coli and Staphylococcal species, has been reported to be more frequent in cirrhotics with compared to those without minimal hepatic encephalopathy[96,122]. In a recent meta-analysis, the use of probiotics, prebiotics, and symbiotics, which have an effect on gut flora, was shown to be associated with significant improvement in hepatic encephalopathy[123]. Alcohol misuse in patients with liver disease is associated with increased intestinal permeability[130-132] and endotoxemia, which in turn may contribute to alcohol-induced liver damage by means of hepatic fibrosis stimulation[130]. Recent studies have shown that alcohol-induced gut leakiness and endotoxemia precedes steatohepatitis in patients with alcoholic liver disease and, thus, they are not a consequence of the latter[133]. This further suggests that a “leaky” gut may play an important role in the pathogenesis of chronic liver injury. Several mechanisms have been proposed to explain bacterial translocation such as intestinal bacterial overgrowth in conjunction with intestinal motility disturbances (outlined above), impairment of the intestinal barrier function, and alterations in the local immune defenses[121,134].
The pathophysiology of intestinal barrier dysfunction in cirrhosis is complex. First, alcohol and its metabolites, acetaldehyde and fatty acid ethyl esters, may contribute to the disruption of tight junctions, mainly through nitric oxide mediated oxidative stress and the generation of reactive oxygen species, and alterations in the cytoskeleton, but also through direct cell damage[135,136]. Portal hypertension per se may affect the integrity of intestinal barrier by causing edema in the gut wall with dilatation of the intercellular spaces[137]. Several studies have shown increased intestinal permeability in patients with portal hypertension compared to those without[114-116]. A recent study has shown that treatment with non-selective beta blockers reduces intestinal permeability as well as bacterial translocation in patients with cirrhosis[116]. Furthermore, microbial changes in the intestine, and in particular small intestinal bacterial overgrowth, may also affect the gut barrier[138], thereby increasing permeability, while compromised Paneth cell antimicrobial host defense has been shown to predispose to bacterial translocation in experimental cirrhosis[139]. Finally, altered expression of enterocyte tight junction proteins has been reported in patients with liver cirrhosis, in particular those with decompensated disease, and is correlated with levels of endotoxemia in these patients[140]. In particular, although tight junctions have been found to be normal ultrastructurally, claudin-2 a pore forming protein of tight junctions, is increased in decompensated cirrhosis[125] whereas the expression of the tight junction proteins occludin and claudin-1 have been shown to be significantly decreased[140]. These changes may, at least in part, explain the observed increased paracellular permeability in cirrhosis[40,125].
GI symptoms are common in patients with liver cirrhosis. Their pathophysiology is complex and probably involves factors related to liver disease severity, psychological distress, and gut dysfunction. GI symptoms are related to reduced energy intake and, thus, may contribute to weight loss and malnutrition. Identification of patients with GI symptoms could therefore help select candidates for nutritional therapy. Gastric sensorimotor function appears also to be altered. Although published data on gastric accommodation are not unanimous, not unexpectedly, tense ascites appears to have a negative impact on meal-induced accommodation of the stomach. Gastric emptying and small bowel transit are delayed, which may be related to disturbances in postprandial glucose, insulin, and ghrelin levels. These alterations, in turn, appear to be associated to insulin resistance, which is common in patients with cirrhosis. Delayed gut transit as well as small bowel manometry disturbances may be associated with the development of small bowel bacterial overgrowth. Future interventional studies should address potential causes of delayed gut transit, such as diabetes and insulin resistance. This could, possibly, help develop specific therapies improving energy intake but also reducing bacterial overgrowth. Finally, several studies have reported intestinal barrier dysfunction in patients with liver cirrhosis (especially those with portal hypertension), which is related to bacterial translocation and permeation of intestinal bacterial products, e.g., endotoxin and bacterial DNA, thus potentially being involved in the pathogenesis of complications of liver cirrhosis.
This paper is based on the author’s PhD thesis published in 2006 (https://gupea.ub.gu.se/handle/2077/3161) as well as on more recent research conducted in the field.
P- Reviewer: Festi D, Li YH, Mach TH, Manesis EK, Yang YP S- Editor: Ma YJ L- Editor: A E- Editor: Zhang DN
| 1. | Pozzi M, Carugo S, Boari G, Pecci V, de Ceglia S, Maggiolini S, Bolla GB, Roffi L, Failla M, Grassi G. Evidence of functional and structural cardiac abnormalities in cirrhotic patients with and without ascites. Hepatology. 1997;26:1131-1137. [PubMed] |
| 2. | Liu H, Song D, Lee SS. Cirrhotic cardiomyopathy. Gastroenterol Clin Biol. 2002;26:842-847. [PubMed] |
| 3. | Hoeper MM, Krowka MJ, Strassburg CP. Portopulmonary hypertension and hepatopulmonary syndrome. Lancet. 2004;363:1461-1468. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 344] [Cited by in RCA: 282] [Article Influence: 13.4] [Reference Citation Analysis (0)] |
| 4. | Cárdenas A. Hepatorenal syndrome: a dreaded complication of end-stage liver disease. Am J Gastroenterol. 2005;100:460-467. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 58] [Cited by in RCA: 48] [Article Influence: 2.4] [Reference Citation Analysis (0)] |
| 5. | Pham PT, Pham PC, Rastogi A, Wilkinson AH. Review article: current management of renal dysfunction in the cirrhotic patient. Aliment Pharmacol Ther. 2005;21:949-961. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 33] [Cited by in RCA: 24] [Article Influence: 1.2] [Reference Citation Analysis (0)] |
| 6. | Chen CC, Wang SS, Jeng FS, Lee SD. Metabolic bone disease of liver cirrhosis: is it parallel to the clinical severity of cirrhosis? J Gastroenterol Hepatol. 1996;11:417-421. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 99] [Cited by in RCA: 91] [Article Influence: 3.1] [Reference Citation Analysis (0)] |
| 7. | Monegal A, Navasa M, Guañabens N, Peris P, Pons F, Martinez de Osaba MJ, Rimola A, Rodés J, Muñoz-Gómez J. Osteoporosis and bone mineral metabolism disorders in cirrhotic patients referred for orthotopic liver transplantation. Calcif Tissue Int. 1997;60:148-154. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 155] [Cited by in RCA: 140] [Article Influence: 5.0] [Reference Citation Analysis (0)] |
| 8. | Matos C, Porayko MK, Francisco-Ziller N, DiCecco S. Nutrition and chronic liver disease. J Clin Gastroenterol. 2002;35:391-397. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 82] [Cited by in RCA: 72] [Article Influence: 3.1] [Reference Citation Analysis (0)] |
| 9. | Viggiano TR, Gostout CJ. Portal hypertensive intestinal vasculopathy: a review of the clinical, endoscopic, and histopathologic features. Am J Gastroenterol. 1992;87:944-954. [PubMed] |
| 10. | Campillo B, Bories PN, Pornin B, Devanlay M. Influence of liver failure, ascites, and energy expenditure on the response to oral nutrition in alcoholic liver cirrhosis. Nutrition. 1997;13:613-621. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 47] [Cited by in RCA: 45] [Article Influence: 1.6] [Reference Citation Analysis (0)] |
| 11. | Selberg O, Böttcher J, Tusch G, Pichlmayr R, Henkel E, Müller MJ. Identification of high- and low-risk patients before liver transplantation: a prospective cohort study of nutritional and metabolic parameters in 150 patients. Hepatology. 1997;25:652-657. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 253] [Cited by in RCA: 234] [Article Influence: 8.4] [Reference Citation Analysis (0)] |
| 12. | Roongpisuthipong C, Sobhonslidsuk A, Nantiruj K, Songchitsomboon S. Nutritional assessment in various stages of liver cirrhosis. Nutrition. 2001;17:761-765. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 92] [Cited by in RCA: 86] [Article Influence: 3.6] [Reference Citation Analysis (0)] |
| 13. | Campillo B, Richardet JP, Scherman E, Bories PN. Evaluation of nutritional practice in hospitalized cirrhotic patients: results of a prospective study. Nutrition. 2003;19:515-521. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 124] [Cited by in RCA: 104] [Article Influence: 4.7] [Reference Citation Analysis (2)] |
| 14. | Montano-Loza AJ, Meza-Junco J, Prado CM, Lieffers JR, Baracos VE, Bain VG, Sawyer MB. Muscle wasting is associated with mortality in patients with cirrhosis. Clin Gastroenterol Hepatol. 2012;10:166-73, 173.e1. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 537] [Cited by in RCA: 608] [Article Influence: 46.8] [Reference Citation Analysis (0)] |
| 15. | Meza-Junco J, Montano-Loza AJ, Baracos VE, Prado CM, Bain VG, Beaumont C, Esfandiari N, Lieffers JR, Sawyer MB. Sarcopenia as a prognostic index of nutritional status in concurrent cirrhosis and hepatocellular carcinoma. J Clin Gastroenterol. 2013;47:861-870. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 165] [Cited by in RCA: 202] [Article Influence: 16.8] [Reference Citation Analysis (0)] |
| 16. | Tandon P, Ney M, Irwin I, Ma MM, Gramlich L, Bain VG, Esfandiari N, Baracos V, Montano-Loza AJ, Myers RP. Severe muscle depletion in patients on the liver transplant wait list: its prevalence and independent prognostic value. Liver Transpl. 2012;18:1209-1216. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 383] [Cited by in RCA: 435] [Article Influence: 33.5] [Reference Citation Analysis (0)] |
| 17. | Kalaitzakis E, Josefsson A, Castedal M, Henfridsson P, Bengtsson M, Andersson B, Björnsson E. Hepatic encephalopathy is related to anemia and fat-free mass depletion in liver transplant candidates with cirrhosis. Scand J Gastroenterol. 2013;48:577-584. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 21] [Cited by in RCA: 26] [Article Influence: 2.2] [Reference Citation Analysis (0)] |
| 18. | Davidson HI, Richardson R, Sutherland D, Garden OJ. Macronutrient preference, dietary intake, and substrate oxidation among stable cirrhotic patients. Hepatology. 1999;29:1380-1386. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 29] [Cited by in RCA: 26] [Article Influence: 1.0] [Reference Citation Analysis (0)] |
| 19. | Müller MJ, Lautz HU, Plogmann B, Bürger M, Körber J, Schmidt FW. Energy expenditure and substrate oxidation in patients with cirrhosis: the impact of cause, clinical staging and nutritional state. Hepatology. 1992;15:782-794. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 205] [Cited by in RCA: 182] [Article Influence: 5.5] [Reference Citation Analysis (0)] |
| 20. | Müller MJ, Böttcher J, Selberg O, Weselmann S, Böker KH, Schwarze M, von zur Mühlen A, Manns MP. Hypermetabolism in clinically stable patients with liver cirrhosis. Am J Clin Nutr. 1999;69:1194-1201. [PubMed] |
| 21. | Madden AM, Morgan MY. Resting energy expenditure should be measured in patients with cirrhosis, not predicted. Hepatology. 1999;30:655-664. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 61] [Cited by in RCA: 51] [Article Influence: 2.0] [Reference Citation Analysis (0)] |
| 22. | Romiti A, Merli M, Martorano M, Parrilli G, Martino F, Riggio O, Truscelli A, Capocaccia L, Budillon G. Malabsorption and nutritional abnormalities in patients with liver cirrhosis. Ital J Gastroenterol. 1990;22:118-123. [PubMed] |
| 23. | Laviano A, Cangiano C, Preziosa I, Riggio O, Conversano L, Cascino A, Ariemma S, Rossi Fanelli F. Plasma tryptophan levels and anorexia in liver cirrhosis. Int J Eat Disord. 1997;21:181-186. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 1] [Reference Citation Analysis (0)] |
| 24. | Scolapio JS, Ukleja A, McGreevy K, Burnett OL, O’Brien PC. Nutritional problems in end-stage liver disease: contribution of impaired gastric emptying and ascites. J Clin Gastroenterol. 2002;34:89-93. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 12] [Cited by in RCA: 10] [Article Influence: 0.4] [Reference Citation Analysis (0)] |
| 25. | Kalaitzakis E, Simrén M, Olsson R, Henfridsson P, Hugosson I, Bengtsson M, Björnsson E. Gastrointestinal symptoms in patients with liver cirrhosis: associations with nutritional status and health-related quality of life. Scand J Gastroenterol. 2006;41:1464-1472. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 86] [Cited by in RCA: 84] [Article Influence: 4.4] [Reference Citation Analysis (1)] |
| 26. | Kalaitzakis E, Josefsson A, Castedal M, Henfridsson P, Bengtsson M, Andersson B, Björnsson E. Gastrointestinal symptoms in patients with cirrhosis: a longitudinal study before and after liver transplantation. Scand J Gastroenterol. 2013;48:1308-1316. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 12] [Cited by in RCA: 15] [Article Influence: 1.3] [Reference Citation Analysis (0)] |
| 27. | Kalaitzakis E, Simrén M, Abrahamsson H, Björnsson E. Role of gastric sensorimotor dysfunction in gastrointestinal symptoms and energy intake in liver cirrhosis. Scand J Gastroenterol. 2007;42:237-246. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 17] [Cited by in RCA: 19] [Article Influence: 1.1] [Reference Citation Analysis (0)] |
| 28. | Kalaitzakis E, Bosaeus I, Ohman L, Björnsson E. Altered postprandial glucose, insulin, leptin, and ghrelin in liver cirrhosis: correlations with energy intake and resting energy expenditure. Am J Clin Nutr. 2007;85:808-815. [PubMed] |
| 29. | Greco AV, Mingrone G, Benedetti G, Capristo E, Tataranni PA, Gasbarrini G. Daily energy and substrate metabolism in patients with cirrhosis. Hepatology. 1998;27:346-350. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 71] [Cited by in RCA: 62] [Article Influence: 2.3] [Reference Citation Analysis (0)] |
| 30. | Merli M, Riggio O, Romiti A, Ariosto F, Mango L, Pinto G, Savioli M, Capocaccia L. Basal energy production rate and substrate use in stable cirrhotic patients. Hepatology. 1990;12:106-112. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 114] [Cited by in RCA: 105] [Article Influence: 3.0] [Reference Citation Analysis (0)] |
| 31. | Ockenga J, Bischoff SC, Tillmann HL, Rifai K, Widjaja A, Böker KH, Manns MP, Brabant G. Elevated bound leptin correlates with energy expenditure in cirrhotics. Gastroenterology. 2000;119:1656-1662. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 44] [Cited by in RCA: 44] [Article Influence: 1.8] [Reference Citation Analysis (0)] |
| 32. | Campillo B, Pernet P, Bories PN, Richardet JP, Devanlay M, Aussel C. Intestinal permeability in liver cirrhosis: relationship with severe septic complications. Eur J Gastroenterol Hepatol. 1999;11:755-759. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 108] [Cited by in RCA: 106] [Article Influence: 4.1] [Reference Citation Analysis (0)] |
| 33. | Budillon G, Parrilli G, Pacella M, Cuomo R, Menzies IS. Investigation of intestine and liver function in cirrhosis using combined sugar oral loads. J Hepatol. 1985;1:513-524. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 27] [Cited by in RCA: 25] [Article Influence: 0.6] [Reference Citation Analysis (0)] |
| 34. | Fritz E, Hammer J. Gastrointestinal symptoms in patients with liver cirrhosis are linked to impaired quality of life and psychological distress. Eur J Gastroenterol Hepatol. 2009;21:460-465. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 27] [Cited by in RCA: 33] [Article Influence: 2.1] [Reference Citation Analysis (0)] |
| 35. | Kotfila R, Trudeau W. Extraesophageal varices. Dig Dis. 1998;16:232-241. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 24] [Cited by in RCA: 22] [Article Influence: 0.8] [Reference Citation Analysis (0)] |
| 36. | Burroughs AK, McCormick PA. Natural history and prognosis of variceal bleeding. Baillieres Clin Gastroenterol. 1992;6:437-450. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 39] [Cited by in RCA: 38] [Article Influence: 1.2] [Reference Citation Analysis (0)] |
| 37. | Gunnarsdottir SA, Olsson R, Björnsson ES. Characteristics, prognosis and outcome of patients with oesophageal varices in a university hospital in Sweden 1994-1999. Scand J Gastroenterol. 2005;40:1462-1468. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 10] [Cited by in RCA: 9] [Article Influence: 0.5] [Reference Citation Analysis (0)] |
| 38. | Hosking SW. Congestive gastropathy in portal hypertension: variations in prevalence. Hepatology. 1989;10:257-258. [PubMed] |
| 39. | Cubillas R, Rockey DC. Portal hypertensive gastropathy: a review. Liver Int. 2010;30:1094-1102. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 62] [Cited by in RCA: 53] [Article Influence: 3.5] [Reference Citation Analysis (0)] |
| 40. | Merli M, Nicolini G, Angeloni S, Gentili F, Attili AF, Riggio O. The natural history of portal hypertensive gastropathy in patients with liver cirrhosis and mild portal hypertension. Am J Gastroenterol. 2004;99:1959-1965. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 75] [Cited by in RCA: 67] [Article Influence: 3.2] [Reference Citation Analysis (0)] |
| 41. | Kim MY, Choi H, Baik SK, Yea CJ, Won CS, Byun JW, Park SY, Kwon YH, Kim JW, Kim HS. Portal hypertensive gastropathy: correlation with portal hypertension and prognosis in cirrhosis. Dig Dis Sci. 2010;55:3561-3567. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 42] [Cited by in RCA: 39] [Article Influence: 2.6] [Reference Citation Analysis (1)] |
| 42. | Primignani M, Carpinelli L, Preatoni P, Battaglia G, Carta A, Prada A, Cestari R, Angeli P, Gatta A, Rossi A. Natural history of portal hypertensive gastropathy in patients with liver cirrhosis. The New Italian Endoscopic Club for the study and treatment of esophageal varices (NIEC). Gastroenterology. 2000;119:181-187. [PubMed] |
| 43. | Konturek SJ, Gonciarz M, Gonciarz Z, Bielanski W, Mazur W, Mularczyk A, Konturek PC, Goetze JP, Rehfeld JF. Progastrin and its products from patients with chronic viral hepatitis and liver cirrhosis. Scand J Gastroenterol. 2003;38:643-647. [PubMed] |
| 44. | Wu CS, Lin CY, Liaw YF. Helicobacter pylori in cirrhotic patients with peptic ulcer disease: a prospective, case controlled study. Gastrointest Endosc. 1995;42:424-427. [PubMed] |
| 45. | Chen LS, Lin HC, Hwang SJ, Lee FY, Hou MC, Lee SD. Prevalence of gastric ulcer in cirrhotic patients and its relation to portal hypertension. J Gastroenterol Hepatol. 1996;11:59-64. [PubMed] |
| 46. | Siringo S, Burroughs AK, Bolondi L, Muia A, Di Febo G, Miglioli M, Cavalli G, Barbara L. Peptic ulcer and its course in cirrhosis: an endoscopic and clinical prospective study. J Hepatol. 1995;22:633-641. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 68] [Cited by in RCA: 68] [Article Influence: 2.3] [Reference Citation Analysis (0)] |
| 47. | Siringo S, Bolondi L, Piscaglia F, Gaetani M, Misitano B, Carbone C, Corinaldesi R, Burroughs AK. Peptic ulcer in patients with liver cirrhosis: a retrospective endoscopic and clinical study. Ital J Gastroenterol Hepatol. 1997;29:62-68. [PubMed] |
| 48. | Vergara M, Calvet X, Roqué M. Helicobacter pylori is a risk factor for peptic ulcer disease in cirrhotic patients. A meta-analysis. Eur J Gastroenterol Hepatol. 2002;14:717-722. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 40] [Cited by in RCA: 40] [Article Influence: 1.7] [Reference Citation Analysis (0)] |
| 49. | Chang SS, Hu HY. Helicobacter pylori is not the predominant etiology for liver cirrhosis patients with peptic ulcer disease. Eur J Gastroenterol Hepatol. 2013;25:159-165. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 9] [Cited by in RCA: 13] [Article Influence: 1.1] [Reference Citation Analysis (0)] |
| 50. | Rudler M, Rousseau G, Benosman H, Massard J, Deforges L, Lebray P, Poynard T, Thabut D. Peptic ulcer bleeding in patients with or without cirrhosis: different diseases but the same prognosis? Aliment Pharmacol Ther. 2012;36:166-172. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 31] [Cited by in RCA: 26] [Article Influence: 2.0] [Reference Citation Analysis (0)] |
| 51. | Luo JC, Leu HB, Hou MC, Huang CC, Lin HC, Lee FY, Chang FY, Chan WL, Lin SJ, Chen JW. Cirrhotic patients at increased risk of peptic ulcer bleeding: a nationwide population-based cohort study. Aliment Pharmacol Ther. 2012;36:542-550. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 47] [Cited by in RCA: 49] [Article Influence: 3.8] [Reference Citation Analysis (0)] |
| 52. | Hsu YC, Lin JT, Chen TT, Wu MS, Wu CY. Long-term risk of recurrent peptic ulcer bleeding in patients with liver cirrhosis: a 10-year nationwide cohort study. Hepatology. 2012;56:698-705. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 56] [Cited by in RCA: 65] [Article Influence: 5.0] [Reference Citation Analysis (0)] |
| 53. | Azpiroz F, Malagelada JR. Physiological variations in canine gastric tone measured by an electronic barostat. Am J Physiol. 1985;248:G229-G237. [PubMed] |
| 54. | Azpiroz F, Malagelada JR. Vagally mediated gastric relaxation induced by intestinal nutrients in the dog. Am J Physiol. 1986;251:G727-G735. [PubMed] |
| 55. | Azpiroz F, Malagelada JR. Gastric tone measured by an electronic barostat in health and postsurgical gastroparesis. Gastroenterology. 1987;92:934-943. [PubMed] |
| 56. | Jahnberg T, Abrahamsson H, Jansson G, Martinson J. Gastric relaxatory response to feeding before and after vagotomy. Scand J Gastroenterol. 1977;12:225-228. [PubMed] |
| 57. | Tack J, Demedts I, Meulemans A, Schuurkes J, Janssens J. Role of nitric oxide in the gastric accommodation reflex and in meal induced satiety in humans. Gut. 2002;51:219-224. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 157] [Cited by in RCA: 158] [Article Influence: 6.9] [Reference Citation Analysis (0)] |
| 58. | Kuiken SD, Vergeer M, Heisterkamp SH, Tytgat GN, Boeckxstaens GE. Role of nitric oxide in gastric motor and sensory functions in healthy subjects. Gut. 2002;51:212-218. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 70] [Cited by in RCA: 73] [Article Influence: 3.2] [Reference Citation Analysis (0)] |
| 59. | De Schepper HU, Cremonini F, Chitkara D, Camilleri M. Assessment of gastric accommodation: overview and evaluation of current methods. Neurogastroenterol Motil. 2004;16:275-285. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 97] [Cited by in RCA: 97] [Article Influence: 4.6] [Reference Citation Analysis (0)] |
| 60. | Gilja OH, Hausken T, Wilhelmsen I, Berstad A. Impaired accommodation of proximal stomach to a meal in functional dyspepsia. Dig Dis Sci. 1996;41:689-696. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 207] [Cited by in RCA: 200] [Article Influence: 6.9] [Reference Citation Analysis (0)] |
| 61. | Tack J, Piessevaux H, Coulie B, Caenepeel P, Janssens J. Role of impaired gastric accommodation to a meal in functional dyspepsia. Gastroenterology. 1998;115:1346-1352. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 771] [Cited by in RCA: 762] [Article Influence: 28.2] [Reference Citation Analysis (0)] |
| 62. | Undeland KA, Hausken T, Gilja OH, Aanderud S, Berstad A. Gastric meal accommodation studied by ultrasound in diabetes. Relation to vagal tone. Scand J Gastroenterol. 1998;33:236-241. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 43] [Cited by in RCA: 51] [Article Influence: 1.9] [Reference Citation Analysis (0)] |
| 63. | Wijnhoven BP, Salet GA, Roelofs JM, Smout AJ, Akkermans LM, Gooszen HG. Function of the proximal stomach after Nissen fundoplication. Br J Surg. 1998;85:267-271. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 50] [Cited by in RCA: 50] [Article Influence: 1.9] [Reference Citation Analysis (0)] |
| 64. | Le Blanc-Louvry I, Savoye G, Maillot C, Denis P, Ducrotté P. An impaired accommodation of the proximal stomach to a meal is associated with symptoms after distal gastrectomy. Am J Gastroenterol. 2003;98:2642-2647. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 19] [Cited by in RCA: 16] [Article Influence: 0.7] [Reference Citation Analysis (0)] |
| 65. | Izbéki F, Kiss I, Wittmann T, Várkonyi TT, Légrády P, Lonovics J. Impaired accommodation of proximal stomach in patients with alcoholic liver cirrhosis. Scand J Gastroenterol. 2002;37:1403-1410. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 23] [Cited by in RCA: 21] [Article Influence: 0.9] [Reference Citation Analysis (0)] |
| 66. | Aqel BA, Scolapio JS, Dickson RC, Burton DD, Bouras EP. Contribution of ascites to impaired gastric function and nutritional intake in patients with cirrhosis and ascites. Clin Gastroenterol Hepatol. 2005;3:1095-1100. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 54] [Cited by in RCA: 63] [Article Influence: 3.2] [Reference Citation Analysis (0)] |
| 67. | Notivol R, Coffin B, Azpiroz F, Mearin F, Serra J, Malagelada JR. Gastric tone determines the sensitivity of the stomach to distention. Gastroenterology. 1995;108:330-336. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 121] [Cited by in RCA: 113] [Article Influence: 3.8] [Reference Citation Analysis (0)] |
| 68. | Distrutti E, Azpiroz F, Soldevilla A, Malagelada JR. Gastric wall tension determines perception of gastric distention. Gastroenterology. 1999;116:1035-1042. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 171] [Cited by in RCA: 159] [Article Influence: 6.1] [Reference Citation Analysis (0)] |
| 69. | Tack J, Caenepeel P, Fischler B, Piessevaux H, Janssens J. Symptoms associated with hypersensitivity to gastric distention in functional dyspepsia. Gastroenterology. 2001;121:526-535. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 410] [Cited by in RCA: 410] [Article Influence: 17.1] [Reference Citation Analysis (0)] |
| 70. | Björnsson E, Sjöberg J, Ringström G, Norström M, Simrén M, Abrahamsson H. Effects of duodenal lipids on gastric sensitivity and relaxation in patients with ulcer-like and dysmotility-like dyspepsia. Digestion. 2003;67:209-217. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 23] [Cited by in RCA: 24] [Article Influence: 1.1] [Reference Citation Analysis (0)] |
| 71. | Tack J. Gastric motor and sensory function. Curr Opin Gastroenterol. 2005;21:665-672. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 21] [Cited by in RCA: 16] [Article Influence: 0.8] [Reference Citation Analysis (0)] |
| 72. | Sadik R, Abrahamsson H, Björnsson E, Gunnarsdottir A, Stotzer PO. Etiology of portal hypertension may influence gastrointestinal transit. Scand J Gastroenterol. 2003;38:1039-1044. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 61] [Cited by in RCA: 67] [Article Influence: 3.0] [Reference Citation Analysis (0)] |
| 73. | Acalovschi M, Dumitraşcu DL, Csakany I. Gastric and gall bladder emptying of a mixed meal are not coordinated in liver cirrhosis--a simultaneous sonographic study. Gut. 1997;40:412-417. [PubMed] |
| 74. | Galati JS, Holdeman KP, Dalrymple GV, Harrison KA, Quigley EM. Delayed gastric emptying of both the liquid and solid components of a meal in chronic liver disease. Am J Gastroenterol. 1994;89:708-711. [PubMed] |
| 75. | Schoonjans R, Van Vlem B, Vandamme W, Van Vlierberghe H, Van Heddeghem N, Van Biesen W, Mast A, Sas S, Vanholder R, Lameire N. Gastric emptying of solids in cirrhotic and peritoneal dialysis patients: influence of peritoneal volume load. Eur J Gastroenterol Hepatol. 2002;14:395-398. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 27] [Cited by in RCA: 22] [Article Influence: 1.0] [Reference Citation Analysis (0)] |
| 76. | Kalaitzakis E, Sadik R, Holst JJ, Ohman L, Björnsson E. Gut transit is associated with gastrointestinal symptoms and gut hormone profile in patients with cirrhosis. Clin Gastroenterol Hepatol. 2009;7:346-352. [PubMed] |
| 77. | Galati JS, Holdeman KP, Bottjen PL, Quigley EM. Gastric emptying and orocecal transit in portal hypertension and end-stage chronic liver disease. Liver Transpl Surg. 1997;3:34-38. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 31] [Cited by in RCA: 31] [Article Influence: 1.1] [Reference Citation Analysis (0)] |
| 78. | Van Thiel DH, Fagiuoli S, Wright HI, Chien MC, Gavaler JS. Gastrointestinal transit in cirrhotic patients: effect of hepatic encephalopathy and its treatment. Hepatology. 1994;19:67-71. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 34] [Cited by in RCA: 23] [Article Influence: 0.7] [Reference Citation Analysis (0)] |
| 79. | Madsen JL, Brinch K, Hansen EF, Fuglsang S. Gastrointestinal motor function in patients with portal hypertension. Scand J Gastroenterol. 2000;35:490-493. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 16] [Cited by in RCA: 20] [Article Influence: 0.8] [Reference Citation Analysis (0)] |
| 80. | Karlsen S, Fynne L, Grønbæk H, Krogh K. Small intestinal transit in patients with liver cirrhosis and portal hypertension: a descriptive study. BMC Gastroenterol. 2012;12:176. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 12] [Cited by in RCA: 17] [Article Influence: 1.3] [Reference Citation Analysis (1)] |
| 81. | Dumitrascu DL, Barnert J, Wienbeck M. Gastric emptying in liver cirrhosis. The effect of the type of meal. Eur J Gastroenterol Hepatol. 1997;9:1073-1080. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 10] [Cited by in RCA: 10] [Article Influence: 0.4] [Reference Citation Analysis (0)] |
| 82. | Björnsson ES, Urbanavicius V, Eliasson B, Attvall S, Smith U, Abrahamsson H. Effects of hyperglycemia on interdigestive gastrointestinal motility in humans. Scand J Gastroenterol. 1994;29:1096-1104. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 73] [Cited by in RCA: 71] [Article Influence: 2.3] [Reference Citation Analysis (0)] |
| 83. | Jones KL, Berry M, Kong MF, Kwiatek MA, Samsom M, Horowitz M. Hyperglycemia attenuates the gastrokinetic effect of erythromycin and affects the perception of postprandial hunger in normal subjects. Diabetes Care. 1999;22:339-344. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 72] [Cited by in RCA: 68] [Article Influence: 2.6] [Reference Citation Analysis (0)] |
| 84. | Hebbard GS, Sun WM, Dent J, Horowitz M. Hyperglycaemia affects proximal gastric motor and sensory function in normal subjects. Eur J Gastroenterol Hepatol. 1996;8:211-217. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 72] [Cited by in RCA: 70] [Article Influence: 2.4] [Reference Citation Analysis (0)] |
| 85. | Horowitz M, Harding PE, Maddox AF, Wishart JM, Akkermans LM, Chatterton BE, Shearman DJ. Gastric and oesophageal emptying in patients with type 2 (non-insulin-dependent) diabetes mellitus. Diabetologia. 1989;32:151-159. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 293] [Cited by in RCA: 273] [Article Influence: 7.6] [Reference Citation Analysis (0)] |
| 86. | Horowitz M, Edelbroek MA, Wishart JM, Straathof JW. Relationship between oral glucose tolerance and gastric emptying in normal healthy subjects. Diabetologia. 1993;36:857-862. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 374] [Cited by in RCA: 335] [Article Influence: 10.5] [Reference Citation Analysis (0)] |
| 87. | Eliasson B, Björnsson E, Urbanavicius V, Andersson H, Fowelin J, Attvall S, Abrahamsson H, Smith U. Hyperinsulinaemia impairs gastrointestinal motility and slows carbohydrate absorption. Diabetologia. 1995;38:79-85. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 55] [Cited by in RCA: 52] [Article Influence: 1.7] [Reference Citation Analysis (0)] |
| 88. | Kong MF, King P, Macdonald IA, Blackshaw PE, Perkins AC, Armstrong E, Buchanan KD, Tattersall RB. Effect of euglycaemic hyperinsulinaemia on gastric emptying and gastrointestinal hormone responses in normal subjects. Diabetologia. 1998;41:474-481. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 15] [Cited by in RCA: 15] [Article Influence: 0.6] [Reference Citation Analysis (0)] |
| 89. | Verne GN, Soldevia-Pico C, Robinson ME, Spicer KM, Reuben A. Autonomic dysfunction and gastroparesis in cirrhosis. J Clin Gastroenterol. 2004;38:72-76. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 43] [Cited by in RCA: 43] [Article Influence: 2.0] [Reference Citation Analysis (0)] |
| 90. | Chesta J, Defilippi C, Defilippi C. Abnormalities in proximal small bowel motility in patients with cirrhosis. Hepatology. 1993;17:828-832. [PubMed] |
| 91. | Madrid AM, Cumsille F, Defilippi C. Altered small bowel motility in patients with liver cirrhosis depends on severity of liver disease. Dig Dis Sci. 1997;42:738-742. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 79] [Cited by in RCA: 85] [Article Influence: 3.0] [Reference Citation Analysis (0)] |
| 92. | Chang CS, Chen GH, Lien HC, Yeh HZ. Small intestine dysmotility and bacterial overgrowth in cirrhotic patients with spontaneous bacterial peritonitis. Hepatology. 1998;28:1187-1190. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 173] [Cited by in RCA: 181] [Article Influence: 6.7] [Reference Citation Analysis (0)] |
| 93. | Gunnarsdottir SA, Sadik R, Shev S, Simrén M, Sjövall H, Stotzer PO, Abrahamsson H, Olsson R, Björnsson ES. Small intestinal motility disturbances and bacterial overgrowth in patients with liver cirrhosis and portal hypertension. Am J Gastroenterol. 2003;98:1362-1370. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 130] [Cited by in RCA: 144] [Article Influence: 6.5] [Reference Citation Analysis (0)] |
| 94. | Madrid AM, Brahm J, Buckel E, Silva G, Defilippi C. Orthotopic liver transplantation improves small bowel motility disorders in cirrhotic patients. Am J Gastroenterol. 1997;92:1044-1045. [PubMed] |
| 95. | Nagasako CK, de Oliveira Figueiredo MJ, de Souza Almeida JR, Lorena SL, Akasaka HM, Pavan CR, Yamanaka A, Pereira TS, Soares EC, Mesquita MA. Investigation of autonomic function and orocecal transit time in patients with nonalcoholic cirrhosis and the potential influence of these factors on disease outcome. J Clin Gastroenterol. 2009;43:884-889. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 12] [Cited by in RCA: 14] [Article Influence: 0.9] [Reference Citation Analysis (0)] |
| 96. | Gupta A, Dhiman RK, Kumari S, Rana S, Agarwal R, Duseja A, Chawla Y. Role of small intestinal bacterial overgrowth and delayed gastrointestinal transit time in cirrhotic patients with minimal hepatic encephalopathy. J Hepatol. 2010;53:849-855. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 126] [Cited by in RCA: 152] [Article Influence: 10.1] [Reference Citation Analysis (0)] |
| 97. | Chander Roland B, Garcia-Tsao G, Ciarleglio MM, Deng Y, Sheth A. Decompensated cirrhotics have slower intestinal transit times as compared with compensated cirrhotics and healthy controls. J Clin Gastroenterol. 2013;47:888-893. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 29] [Cited by in RCA: 42] [Article Influence: 3.5] [Reference Citation Analysis (0)] |
| 98. | Sadik R, Stotzer PO, Simrén M, Abrahamsson H. Gastrointestinal transit abnormalities are frequently detected in patients with unexplained GI symptoms at a tertiary centre. Neurogastroenterol Motil. 2008;20:197-205. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 60] [Cited by in RCA: 68] [Article Influence: 4.0] [Reference Citation Analysis (0)] |
| 99. | Casafont Morencos F, de las Heras Castaño G, Martín Ramos L, López Arias MJ, Ledesma F, Pons Romero F. Small bowel bacterial overgrowth in patients with alcoholic cirrhosis. Dig Dis Sci. 1996;41:552-556. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 109] [Cited by in RCA: 108] [Article Influence: 3.7] [Reference Citation Analysis (0)] |
| 100. | Pande C, Kumar A, Sarin SK. Small-intestinal bacterial overgrowth in cirrhosis is related to the severity of liver disease. Aliment Pharmacol Ther. 2009;29:1273-1281. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 97] [Cited by in RCA: 107] [Article Influence: 6.7] [Reference Citation Analysis (0)] |
| 101. | Pardo A, Bartolí R, Lorenzo-Zúñiga V, Planas R, Viñado B, Riba J, Cabré E, Santos J, Luque T, Ausina V. Effect of cisapride on intestinal bacterial overgrowth and bacterial translocation in cirrhosis. Hepatology. 2000;31:858-863. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 120] [Cited by in RCA: 123] [Article Influence: 4.9] [Reference Citation Analysis (0)] |
| 102. | DeMeo MT, Mutlu EA, Keshavarzian A, Tobin MC. Intestinal permeation and gastrointestinal disease. J Clin Gastroenterol. 2002;34:385-396. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 187] [Cited by in RCA: 183] [Article Influence: 8.0] [Reference Citation Analysis (0)] |
| 103. | Farhadi A, Banan A, Fields J, Keshavarzian A. Intestinal barrier: an interface between health and disease. J Gastroenterol Hepatol. 2003;18:479-497. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 338] [Cited by in RCA: 386] [Article Influence: 17.5] [Reference Citation Analysis (0)] |
| 104. | Scaldaferri F, Pizzoferrato M, Gerardi V, Lopetuso L, Gasbarrini A. The gut barrier: new acquisitions and therapeutic approaches. J Clin Gastroenterol. 2012;46 Suppl:S12-S17. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 130] [Cited by in RCA: 150] [Article Influence: 11.5] [Reference Citation Analysis (0)] |
| 105. | Bjarnason I, MacPherson A, Hollander D. Intestinal permeability: an overview. Gastroenterology. 1995;108:1566-1581. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 627] [Cited by in RCA: 630] [Article Influence: 21.0] [Reference Citation Analysis (0)] |
| 106. | Fernández J, Navasa M, Gómez J, Colmenero J, Vila J, Arroyo V, Rodés J. Bacterial infections in cirrhosis: epidemiological changes with invasive procedures and norfloxacin prophylaxis. Hepatology. 2002;35:140-148. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 661] [Cited by in RCA: 629] [Article Influence: 27.3] [Reference Citation Analysis (0)] |
| 107. | Arvaniti V, D’Amico G, Fede G, Manousou P, Tsochatzis E, Pleguezuelo M, Burroughs AK. Infections in patients with cirrhosis increase mortality four-fold and should be used in determining prognosis. Gastroenterology. 2010;139:1246-156, 1246-156. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 720] [Cited by in RCA: 836] [Article Influence: 55.7] [Reference Citation Analysis (0)] |
| 108. | Francés R, Muñoz C, Zapater P, Uceda F, Gascón I, Pascual S, Pérez-Mateo M, Such J. Bacterial DNA activates cell mediated immune response and nitric oxide overproduction in peritoneal macrophages from patients with cirrhosis and ascites. Gut. 2004;53:860-864. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 94] [Cited by in RCA: 96] [Article Influence: 4.6] [Reference Citation Analysis (0)] |
| 109. | Pascual S, Such J, Esteban A, Zapater P, Casellas JA, Aparicio JR, Girona E, Gutiérrez A, Carnices F, Palazón JM. Intestinal permeability is increased in patients with advanced cirrhosis. Hepatogastroenterology. 2003;50:1482-1486. [PubMed] |
| 110. | Ersöz G, Aydin A, Erdem S, Yüksel D, Akarca U, Kumanlioglu K. Intestinal permeability in liver cirrhosis. Eur J Gastroenterol Hepatol. 1999;11:409-412. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 48] [Cited by in RCA: 51] [Article Influence: 2.0] [Reference Citation Analysis (0)] |
| 111. | Bac DJ, van der Berg JWO, Wilson JHP. Small bowel wall function in patients with advanced liver cirrhosis and portal hypertension: studies on permeability and luminal bacterial overgrowth. Eur J Gastroenterol Hepatol. 1993;5:383-387. [DOI] [Full Text] |
| 112. | Fujii T, Seki T, Maruoka M, Tanaka J, Kawashima Y, Watanabe T, Sawamura T, Inoue K. Lactulose-L-rhamnose intestinal permeability test in patients with liver cirrhosis. Hepatol Res. 2001;19:158-169. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 22] [Cited by in RCA: 25] [Article Influence: 1.0] [Reference Citation Analysis (0)] |
| 113. | Huglo D, De Botton S, Canva-Delcambre V, Colombel JF, Wallaert B, Steinling M, Marchandise X. Simultaneous determination of pulmonary and intestinal permeability in patients with alcoholic liver cirrhosis. Eur J Nucl Med. 2001;28:1505-1511. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 14] [Cited by in RCA: 17] [Article Influence: 0.7] [Reference Citation Analysis (0)] |
| 114. | Zuckerman MJ, Menzies IS, Ho H, Gregory GG, Casner NA, Crane RS, Hernandez JA. Assessment of intestinal permeability and absorption in cirrhotic patients with ascites using combined sugar probes. Dig Dis Sci. 2004;49:621-626. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 57] [Cited by in RCA: 64] [Article Influence: 3.0] [Reference Citation Analysis (0)] |
| 115. | Kalaitzakis E, Johansson JE, Bjarnason I, Björnsson E. Intestinal permeability in cirrhotic patients with and without ascites. Scand J Gastroenterol. 2006;41:326-330. [PubMed] |
| 116. | Reiberger T, Ferlitsch A, Payer BA, Mandorfer M, Heinisch BB, Hayden H, Lammert F, Trauner M, Peck-Radosavljevic M, Vogelsang H. Non-selective betablocker therapy decreases intestinal permeability and serum levels of LBP and IL-6 in patients with cirrhosis. J Hepatol. 2013;58:911-921. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 223] [Cited by in RCA: 254] [Article Influence: 21.2] [Reference Citation Analysis (0)] |
| 117. | Scarpellini E, Valenza V, Gabrielli M, Lauritano EC, Perotti G, Merra G, Dal Lago A, Ojetti V, Ainora ME, Santoro M. Intestinal permeability in cirrhotic patients with and without spontaneous bacterial peritonitis: is the ring closed? Am J Gastroenterol. 2010;105:323-327. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 74] [Cited by in RCA: 92] [Article Influence: 6.1] [Reference Citation Analysis (0)] |
| 118. | Pijls KE, Jonkers DM, Elamin EE, Masclee AA, Koek GH. Intestinal epithelial barrier function in liver cirrhosis: an extensive review of the literature. Liver Int. 2013;33:1457-1469. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 75] [Cited by in RCA: 96] [Article Influence: 8.0] [Reference Citation Analysis (0)] |
| 119. | Kim BI, Kim HJ, Park JH, Park DI, Cho YK, Sohn CI, Jeon WK, Kim HS, Kim DJ. Increased intestinal permeability as a predictor of bacterial infections in patients with decompensated liver cirrhosis and hemorrhage. J Gastroenterol Hepatol. 2011;26:550-557. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 31] [Cited by in RCA: 32] [Article Influence: 2.3] [Reference Citation Analysis (0)] |
| 120. | Benjamin J, Singla V, Arora I, Sood S, Joshi YK. Intestinal permeability and complications in liver cirrhosis: A prospective cohort study. Hepatol Res. 2013;43:200-207. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 30] [Cited by in RCA: 34] [Article Influence: 2.8] [Reference Citation Analysis (0)] |
| 121. | Guarner C, Soriano G. Bacterial translocation and its consequences in patients with cirrhosis. Eur J Gastroenterol Hepatol. 2005;17:27-31. [PubMed] |
| 122. | Liu Q, Duan ZP, Ha DK, Bengmark S, Kurtovic J, Riordan SM. Synbiotic modulation of gut flora: effect on minimal hepatic encephalopathy in patients with cirrhosis. Hepatology. 2004;39:1441-1449. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 444] [Cited by in RCA: 454] [Article Influence: 21.6] [Reference Citation Analysis (0)] |
| 123. | Shukla S, Shukla A, Mehboob S, Guha S. Meta-analysis: the effects of gut flora modulation using prebiotics, probiotics and synbiotics on minimal hepatic encephalopathy. Aliment Pharmacol Ther. 2011;33:662-671. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 153] [Cited by in RCA: 135] [Article Influence: 9.6] [Reference Citation Analysis (0)] |
| 124. | Albillos A, de la Hera A, González M, Moya JL, Calleja JL, Monserrat J, Ruiz-del-Arbol L, Alvarez-Mon M. Increased lipopolysaccharide binding protein in cirrhotic patients with marked immune and hemodynamic derangement. Hepatology. 2003;37:208-217. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 320] [Cited by in RCA: 342] [Article Influence: 15.5] [Reference Citation Analysis (0)] |
| 125. | Du Plessis J, Vanheel H, Janssen CE, Roos L, Slavik T, Stivaktas PI, Nieuwoudt M, van Wyk SG, Vieira W, Pretorius E. Activated intestinal macrophages in patients with cirrhosis release NO and IL-6 that may disrupt intestinal barrier function. J Hepatol. 2013;58:1125-1132. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 112] [Cited by in RCA: 145] [Article Influence: 12.1] [Reference Citation Analysis (0)] |
| 126. | Montes-de-Oca M, Blanco MJ, Marquez M, Soto MJ, Fernandez-Gutiérrez C, Rodriguez-Ramos C, Giron-Gonzalez JA. Haemodynamic derangement in human immunodeficiency virus-infected patients with hepatitis C virus-related cirrhosis: the role of bacterial translocation. Liver Int. 2011;31:850-858. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 13] [Cited by in RCA: 11] [Article Influence: 0.8] [Reference Citation Analysis (0)] |
| 127. | Sandler NG, Koh C, Roque A, Eccleston JL, Siegel RB, Demino M, Kleiner DE, Deeks SG, Liang TJ, Heller T. Host response to translocated microbial products predicts outcomes of patients with HBV or HCV infection. Gastroenterology. 2011;141:1220-130, 1220-130. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 250] [Cited by in RCA: 252] [Article Influence: 18.0] [Reference Citation Analysis (0)] |
| 128. | Vlachogiannakos J, Saveriadis AS, Viazis N, Theodoropoulos I, Foudoulis K, Manolakopoulos S, Raptis S, Karamanolis DG. Intestinal decontamination improves liver haemodynamics in patients with alcohol-related decompensated cirrhosis. Aliment Pharmacol Ther. 2009;29:992-999. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 127] [Cited by in RCA: 138] [Article Influence: 8.6] [Reference Citation Analysis (0)] |
| 129. | Karagiannakis DS, Vlachogiannakos J, Anastasiadis G, Vafiadis-Zouboulis I, Ladas SD. Frequency and severity of cirrhotic cardiomyopathy and its possible relationship with bacterial endotoxemia. Dig Dis Sci. 2013;58:3029-3036. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 38] [Cited by in RCA: 33] [Article Influence: 2.8] [Reference Citation Analysis (0)] |
| 130. | Keshavarzian A, Holmes EW, Patel M, Iber F, Fields JZ, Pethkar S. Leaky gut in alcoholic cirrhosis: a possible mechanism for alcohol-induced liver damage. Am J Gastroenterol. 1999;94:200-207. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 278] [Cited by in RCA: 275] [Article Influence: 10.6] [Reference Citation Analysis (0)] |
| 131. | Bjarnason I, Peters TJ, Wise RJ. The leaky gut of alcoholism: possible route of entry for toxic compounds. Lancet. 1984;1:179-182. [PubMed] |
| 132. | Parlesak A, Schäfer C, Schütz T, Bode JC, Bode C. Increased intestinal permeability to macromolecules and endotoxemia in patients with chronic alcohol abuse in different stages of alcohol-induced liver disease. J Hepatol. 2000;32:742-747. [PubMed] |
| 133. | Keshavarzian A, Farhadi A, Forsyth CB, Rangan J, Jakate S, Shaikh M, Banan A, Fields JZ. Evidence that chronic alcohol exposure promotes intestinal oxidative stress, intestinal hyperpermeability and endotoxemia prior to development of alcoholic steatohepatitis in rats. J Hepatol. 2009;50:538-547. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 289] [Cited by in RCA: 284] [Article Influence: 17.8] [Reference Citation Analysis (0)] |
| 134. | Ramachandran A, Balasubramanian KA. Intestinal dysfunction in liver cirrhosis: Its role in spontaneous bacterial peritonitis. J Gastroenterol Hepatol. 2001;16:607-612. [PubMed] |
| 135. | Elamin EE, Masclee AA, Dekker J, Jonkers DM. Ethanol metabolism and its effects on the intestinal epithelial barrier. Nutr Rev. 2013;71:483-499. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 119] [Cited by in RCA: 133] [Article Influence: 11.1] [Reference Citation Analysis (0)] |
| 136. | Tang Y, Forsyth CB, Farhadi A, Rangan J, Jakate S, Shaikh M, Banan A, Fields JZ, Keshavarzian A. Nitric oxide-mediated intestinal injury is required for alcohol-induced gut leakiness and liver damage. Alcohol Clin Exp Res. 2009;33:1220-1230. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 88] [Cited by in RCA: 93] [Article Influence: 5.8] [Reference Citation Analysis (0)] |
| 137. | Norman DA, Atkins JM, Seelig LL, Gomez-Sanchez C, Krejs GJ. Water and electrolyte movement and mucosal morphology in the jejunum of patients with portal hypertension. Gastroenterology. 1980;79:707-715. [PubMed] |
| 138. | Yu LC, Wang JT, Wei SC, Ni YH. Host-microbial interactions and regulation of intestinal epithelial barrier function: From physiology to pathology. World J Gastrointest Pathophysiol. 2012;3:27-43. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in CrossRef: 157] [Cited by in RCA: 176] [Article Influence: 13.5] [Reference Citation Analysis (2)] |
| 139. | Teltschik Z, Wiest R, Beisner J, Nuding S, Hofmann C, Schoelmerich J, Bevins CL, Stange EF, Wehkamp J. Intestinal bacterial translocation in rats with cirrhosis is related to compromised Paneth cell antimicrobial host defense. Hepatology. 2012;55:1154-1163. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 130] [Cited by in RCA: 148] [Article Influence: 11.4] [Reference Citation Analysis (0)] |
| 140. | Assimakopoulos SF, Tsamandas AC, Tsiaoussis GI, Karatza E, Triantos C, Vagianos CE, Spiliopoulou I, Kaltezioti V, Charonis A, Nikolopoulou VN. Altered intestinal tight junctions’ expression in patients with liver cirrhosis: a pathogenetic mechanism of intestinal hyperpermeability. Eur J Clin Invest. 2012;42:439-446. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 137] [Cited by in RCA: 144] [Article Influence: 11.1] [Reference Citation Analysis (1)] |