Published online Jul 28, 2013. doi: 10.3748/wjg.v19.i28.4630
Revised: May 20, 2013
Accepted: June 1, 2013
Published online: July 28, 2013
Processing time: 124 Days and 10.7 Hours
This case report describes an unusual case of upper gastrointestinal (UGI) bleeding caused by a ruptured superior mesenteric artery (SMA) aneurysm in the duodenum in a patient with rheumatoid arthritis. The patient presented with UGI bleeding and hemorrhagic shock. Emergency UGI endoscopy could not identify the source of the bleeding because of excessive blood clots under the second portion of the duodenum. An SMA aneurysm with active contrast extravasation was diagnosed by computed tomography. The aneurysm, together with the fourth portion of the duodenum and the proximal portion of the jejunum, was surgically resected, and the SMA was skeletonized. On postoperative day 15, the patient was discharged from hospital under satisfactory conditions. Rheumatoid arthritis has been known to cause a wide spectrum of manifestations, and an SMA aneurysm is an unusual extra-articular manifestation. An SMA aneurysm rupture presenting as upper gastrointestinal bleeding is a rare complication with a high mortality rate. The clinician must be alert to this potential issue to achieve rapid diagnostic confirmation, and immediate surgical or radiological intervention.
Core tip: Gastrointestinal bleeding is a common medical emergency. Ruptured superior mesenteric artery aneurysm is an uncommon cause of gastrointestinal bleeding, with few cases reported previously. Diagnosis is difficult before surgery. We reported the successful diagnosis and treatment of such a case.
- Citation: Choo CH, Yen HH. Unusual upper gastrointestinal bleeding: Ruptured superior mesenteric artery aneurysm in rheumatoid arthritis. World J Gastroenterol 2013; 19(28): 4630-4632
- URL: https://www.wjgnet.com/1007-9327/full/v19/i28/4630.htm
- DOI: https://dx.doi.org/10.3748/wjg.v19.i28.4630
Upper gastrointestinal (UGI) bleeding is a common medical emergency. Patients usually present with hematemesis or melena, and are diagnosed after endoscopic evaluation. Peptic ulcers and esophagogastric varices account for most causes of UGI bleeding. A visceral aneurysm is an uncommon cause of gastrointestinal bleeding, and diagnosis is usually made after surgery. Here, we report an interesting case with pre-operative diagnosis of a ruptured superior mesenteric artery (SMA) aneurysm in the duodenum of a patient with rheumatoid arthritis.
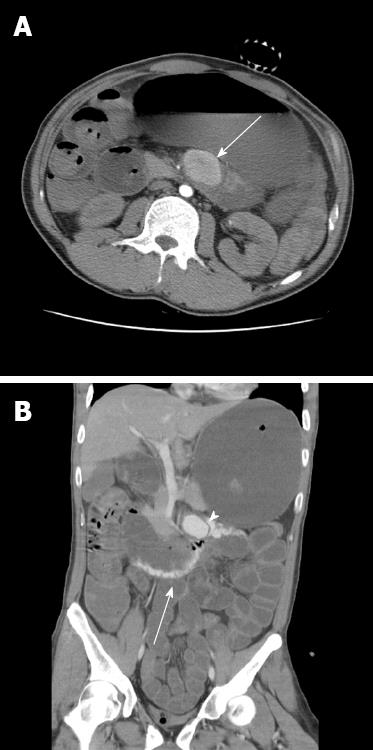
A 27-year-old man with a history of rheumatoid arthritis was brought to the emergency department because of an episode of coffee ground vomitus and dizziness. He suffered from melena for 2 d. His blood pressure was 89/52 mmHg and his heart rate was 106/min. He presented with alert consciousness in the emergency department. A nasogastric tube lavage revealed coffee ground material, and further investigation revealed hemoglobin levels of 8.1 g/dL. Emergency UGI endoscopy was performed after his hemodynamic status was stabilized with fluid hydration and blood transfusion. UGI endoscopy found excessive blood clots below the second portion of the duodenum. To identify the source of the bleeding, abdominal contrast-enhanced computed tomography (CT) was performed. The CT scan revealed an aneurysm about 3.9 cm in diameter at the jejunal mesentery; with active contrast extravasation into the fourth portion of the duodenum (Figure 1). The aneurysm, together with the fourth portion of the duodenum and the proximal portion of the jejunum, was surgically resected, and the SMA was skeletonized. Pathology revealed an aneurysm measuring 3.8 cm × 3.5 cm × 2.0 cm at the mesenteric side, with blood clots within the cystic space, as well as a focal rupture into the lumen of the small intestine.
The patient was subsequently able to eat on postoperative day 7, and his condition was satisfactory. He was discharged from the hospital on postoperative day 15.
UGI bleeding is a common medical condition that results in high patient morbidity. UGI bleeding commonly presents with hematemesis or melena. It is important to take a careful history and perform a thorough physical examination to identify the possible source and etiology of the bleeding. Common causes of UGI bleeding include peptic ulcers, esophagogastric varices, erosive gastritis, Mallory-Weiss syndrome, angiodysplasia or Dieulafoy’s lesion. Peptic ulcers are responsible for approximately half of UGI bleedings[1].
Our patient with an SMA aneurysm rupture in the duodenum presenting as UGI bleeding was extremely rare; there have been only a few reported cases[2-4]. Overall, only 0.2% of the general population is found to have an aneurysm of the visceral arteries, and SMA aneurysms represent only 5.5% of all visceral aneurysms[5]. Unlike other splanchnic artery aneurysms, which are mostly asymptomatic, more than 90.0% of SMA aneurysms are symptomatic, manifesting primarily as nonspecific abdominal pain[6]. Rarely, an abdominal mobile pulsatile mass or abdominal bruit maybe found on physical examination. Common causes of SMA aneurysms include septic emboli, atherosclerosis, pancreatitis and trauma. Septic emboli account for about one-third of SMA aneurysms. Other uncommon causes are collagen vascular disease, connective tissue disease and neurofibromatosis[7]. Abdominal ultrasonography and CT are useful in identifying the type of aneurysm. However, up to 50.0% of SMA aneurysms present with a rupture, where hypovolemic shock, hemoperitoneum or acute abdomen are the first manifestations. Once an SMA aneurysm ruptures, a high intra-operative mortality rate of more than 30.0% has been reported in previous studies[8]. Therefore, in patients diagnosed with an SMA aneurysm, surgical resection or radiological intervention should be recommended before the aneurysm ruptures.
An SMA aneurysm is an unusual extra-articular manifestation of rheumatoid arthritis, and our patient had no other history contributing to the formation of an aneurysm, including septic embolic, trauma or atherosclerosis. Rheumatoid arthritis can cause a wide spectrum of manifestations, from clinically insignificant to life-threatening. In postmortem examinations, rheumatoid vasculitis occurred in approximately 25.0% of all patients with rheumatoid arthritis, whereas less than 1% of rheumatoid arthritis patients developed clinical signs of vasculitis[9]. Among these patients, 10%-38% will have gastrointestinal manifestations of vasculitis and this may be the first manifestation[10,11]. Cases of abdominal aneurysm rupture with syncope and hemorrhage, bowel infarction, and intestinal perforation have been described [10-13].
Therefore, in patients with rheumatoid arthritis who have UGI bleeding, diagnosis of a ruptured SMA aneurysm in the duodenum should be considered, and the clinician should be alert to this issue to achieve rapid confirmation and to save lives.
P- Reviewer Skok P S- Editor Wen LL L- Editor Stewart GJ E- Editor Zhang DN
| 1. | Jutabha R, Jensen DM. Management of upper gastrointestinal bleeding in the patient with chronic liver disease. Med Clin North Am. 1996;80:1035-1068. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 68] [Cited by in RCA: 54] [Article Influence: 1.9] [Reference Citation Analysis (0)] |
| 2. | Maloney RD, Nealon TF, Roberts EA. Massive bleeding from a ruptured superior mesenteric artery aneurysm duodenum. Arch Surg. 1976;111:286-288. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 15] [Cited by in RCA: 15] [Article Influence: 0.3] [Reference Citation Analysis (0)] |
| 3. | Tolga Muftuoglu MA, Aktekin A, Gurleyik G, Saglam A. A ruptured aneurysm of superior mesenteric artery to duodenum and reconstruction with saphenous vein graft. Eur J Vasc Endovasc Surg. 2003;25:590-591. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 8] [Cited by in RCA: 10] [Article Influence: 0.5] [Reference Citation Analysis (0)] |
| 4. | Zhao J. Massive upper gastrointestinal bleeding due to a ruptured superior mesenteric artery aneurysm duodenum fistula. J Vasc Surg. 2008;48:735-737. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 17] [Cited by in RCA: 19] [Article Influence: 1.1] [Reference Citation Analysis (0)] |
| 5. | Haruta N, Asahara T, Fukuda T, Matsuda M, Dohi K. Ruptured superior mesenteric artery aneurysm occurring in association with a heterotopic pancreas: report of a case. Surg Today. 1999;29:656-659. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 8] [Cited by in RCA: 9] [Article Influence: 0.3] [Reference Citation Analysis (0)] |
| 6. | Carr SC, Mahvi DM, Hoch JR, Archer CW, Turnipseed WD. Visceral artery aneurysm rupture. J Vasc Surg. 2001;33:806-811. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 191] [Cited by in RCA: 174] [Article Influence: 7.3] [Reference Citation Analysis (0)] |
| 7. | Pasha SF, Gloviczki P, Stanson AW, Kamath PS. Splanchnic artery aneurysms. Mayo Clin Proc. 2007;82:472-479. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 228] [Cited by in RCA: 217] [Article Influence: 12.1] [Reference Citation Analysis (0)] |
| 8. | Stone WM, Abbas M, Cherry KJ, Fowl RJ, Gloviczki P. Superior mesenteric artery aneurysms: is presence an indication for intervention? J Vasc Surg. 2002;36:234-237; discussion 237. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 150] [Cited by in RCA: 129] [Article Influence: 5.6] [Reference Citation Analysis (0)] |
| 9. | Burt RW, Berenson MM, Samuelson CO, Cathey WJ. Rheumatoid vasculitis of the colon presenting as pancolitis. Dig Dis Sci. 1983;28:183-188. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 27] [Cited by in RCA: 27] [Article Influence: 0.6] [Reference Citation Analysis (0)] |
| 10. | Achkar AA, Stanson AW, Johnson CM, Srivatsa SS, Dale LC, Weyand CM. Rheumatoid vasculitis manifesting as intra-abdominal hemorrhage. Mayo Clin Proc. 1995;70:565-569. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 27] [Cited by in RCA: 27] [Article Influence: 0.9] [Reference Citation Analysis (0)] |
| 11. | Jacobsen SE, Petersen P, Jensen P. Acute abdomen in rheumatoid arthritis due to mesenteric arteritis. A case report and review. Dan Med Bull. 1985;32:191-193. [PubMed] |
| 12. | Pagnoux C, Mahr A, Cohen P, Guillevin L. Presentation and outcome of gastrointestinal involvement in systemic necrotizing vasculitides: analysis of 62 patients with polyarteritis nodosa, microscopic polyangiitis, Wegener granulomatosis, Churg-Strauss syndrome, or rheumatoid arthritis-associated vasculitis. Medicine (Baltimore). 2005;84:115-128. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 280] [Cited by in RCA: 256] [Article Influence: 12.8] [Reference Citation Analysis (0)] |
| 13. | Babian M, Nasef S, Soloway G. Gastrointestinal infarction as a manifestation of rheumatoid vasculitis. Am J Gastroenterol. 1998;93:119-120. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 25] [Cited by in RCA: 25] [Article Influence: 0.9] [Reference Citation Analysis (0)] |