Published online Jul 14, 2013. doi: 10.3748/wjg.v19.i26.4177
Revised: April 24, 2013
Accepted: June 5, 2013
Published online: July 14, 2013
Processing time: 162 Days and 7.3 Hours
AIM: To increase satisfaction and diminish anxiety and shame during colonoscopy, we developed novel double pants (NDP) which consist of doubled fabrics with an inner hole. The aim of study was to compare satisfaction, anxiety and shame between NDP and conventional single pants (CSP).
METHODS: Total 160 consecutive examinees were randomly divided into NDP and CSP group. Before colonoscopy, questionnaires identifying state and trait anxiety were completed. After colonoscopy, questionnaires for overall satisfaction (Group Health Association of America 9) and pants-specific satisfaction (5-20), state anxiety (20-80), and shame (6-24) were interviewed.
RESULTS: Pants-specific satisfaction scores regarding willingness to repeat colonoscopy using same pants (3.3 ± 0.8 vs 2.1 ± 0.9, P < 0.001) and recommendation of same pants to other people (3.3 ± 0.7 vs 2.0 ± 1.0, P < 0.001) were significantly higher in NDP than CSP groups. State anxiety (33.0 ± 7.0 vs 35.4 ± 6.9, P = 0.028) and shame (6.6 ± 1.5 vs 8.1 ± 3.2, P = 0.001) after colonoscopy was lower in NDP group compared with CSP group.
CONCLUSION: The NDP contribute to increase satisfaction and decrease anxiety and shame after colonoscopy.
Core tip: We developed novel double pants (NDP) those are consisted of double fabrics with an inner hole. We compared the satisfaction, anxiety and shame between NDP and conventional single pants (CSP). The examinees in NDP group responded higher pants specific satisfaction, lower state anxiety after colonoscopy and lower shame score compared to those in CSP group. NDP developed in our institute may contribute to increase satisfaction and decrease anxiety and shame after colonoscopy.
- Citation: Chung SH, Park SJ, Hong JS, Hwang JY, Lee SA, Kim KR, Lee HS, Hong SP, Cheon JH, Kim TI, Kim WH. Comparison of double pants with single pants on satisfaction with colonoscopy. World J Gastroenterol 2013; 19(26): 4177-4184
- URL: https://www.wjgnet.com/1007-9327/full/v19/i26/4177.htm
- DOI: https://dx.doi.org/10.3748/wjg.v19.i26.4177
Colonoscopy has recently increased in importance worldwide due to its use in screening for colon polyps and colorectal cancer[1]. Even in institutions where conscious sedated colonoscopy is available, colonoscopy without sedation is still performed due to patient comorbidities, the economic burden of sedation, and examinee preference. There is considerable global variation in the prevalence of sedative endoscopy[2]. Most colonoscopies in the United States are performed as sedated procedures, but some countries rarely use sedation in colonoscopy[3,4].
Consideration of the factors affecting satisfaction during colonoscopy has also recently increased because satisfaction may represent an important quality indicator for colonoscopy[5,6]. Moreover, the satisfaction of examinees may be reduced by anxiety, shame, discomfort, and embarrassment[7-11]. Many factors have been identified which determine satisfaction, anxiety, and shame, including the circumstance of the endoscopy room, the clothing for the procedure, endoscopist’s skill, and the unfamiliarity of the medical staff with whom examinees interact during the procedure.
During colonoscopy at our center, examinees previously wear conventional single pants (CSP), where there is no hole for insertion of the scope. Examinees remove the CSP to below the level of the buttocks and expose their buttocks area during colonoscopy. Exposing the buttocks during colonoscopy can make examinees feel shameful and anxious, which can diminish their satisfaction with the colonoscopy. To decrease the shame and anxiety induced by exposing the buttocks of examinees wearing CSP during colonoscopy, we developed novel double pants (NDP). Examinees wearing NDP can undergo colonoscopy without taking off the inner pants. The smaller area of the buttock exposed by using NDP could minimize shame and anxiety during colonoscopy. Therefore we hypothesized that NDP could decrease shame and anxiety and increase satisfaction. We aimed to assess satisfaction, anxiety, and shame of patients wearing NDP compared with patients wearing CSP during colonoscopy through a prospective randomized single-center study. We also investigated the factors associated with patient satisfaction, anxiety, and shame during colonoscopy.
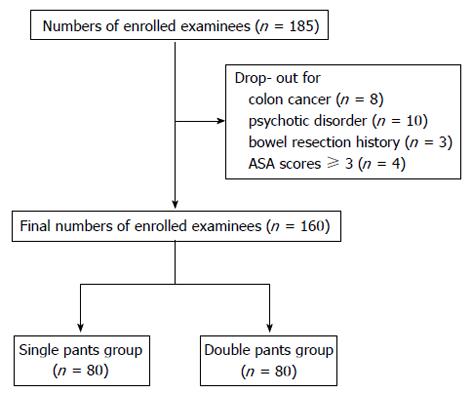
The study included examinees over 20 years old who agreed to undergo colonoscopy without sedation in the endoscopy unit of Severance Hospital, Yonsei University College of Medicine, Seoul, South Korea from January 2012 and July 2012. All of included people were the patients who visited the clinic for routine health check-up or for evaluating their mild gastrointestinal symptoms. Because we tried to minimize the selection bias of tertiary referral medical center, we excluded the patients who were referred by the physicians of primary or secondary medical center and needed more special care due to their objective medical problems. Before they signed at written informed consent, the nurse in outpatient clinic explained the purpose of the study. They got the information about not only the purpose of the study, but also the study design, the types of pants, the possible adverse events of procedure, and the contents of interview. Examinees under 20 years of age, those who had undergone colonoscopy within the past three years, those who were treated with an emergent colonoscopic procedure, those with a history of bowel resection surgery, inflammatory bowel disease (IBD), cancer, colostomy, ileostomy, psychotic disease including depression, anxiety disorder, or obsessive compulsive disorder, women who were pregnant or lactating, illiterate patients, foreigners, or examinees with American Society of Anesthesiologists (ASA) Scores of ≥ 3 were excluded. We used our preliminary survey data to perform a power calculation due to the lack of the prior published reports to guide this analysis. We calculated that a sample size of 80 participants was sufficient to detect an effect value of 0.5 (mean difference/common SD) at a significance level of 0.05% (two-sided) with 80% power and 20% drop-out rate. A total of 185 colonoscopy examinees were enrolled in this study between February 2012 and July 2012. Eight examinees were excluded because of colon cancer found during the colonoscopy, ten examinees were excluded because of psychologic disorder, three examinees were excluded because of a history of bowel resection, and four examinees were excluded because of ASA scores ≥ 3, as shown in Figure 1. Finally a total of 160 consecutive examinees were randomly divided into NDP and CSP groups. Participants in this study were randomly assigned to a “CSP group” or a “NDP group” using a permuted four-block randomization method. Biostatistician made permuted four-block randomization table and calculated the numbers of participants. All random code was contained in a closed box. The nurse in outpatient clinic enrolled the examinees. Before colonoscopy, participants, outcome assessors, and care providers (endoscopists and nurses) were blinded to assignment to the allocation because the third party examiner allocated the enrolled subjects regarding to the prepared permuted-block randomization table. Written informed consent was provided by all participants in the study.
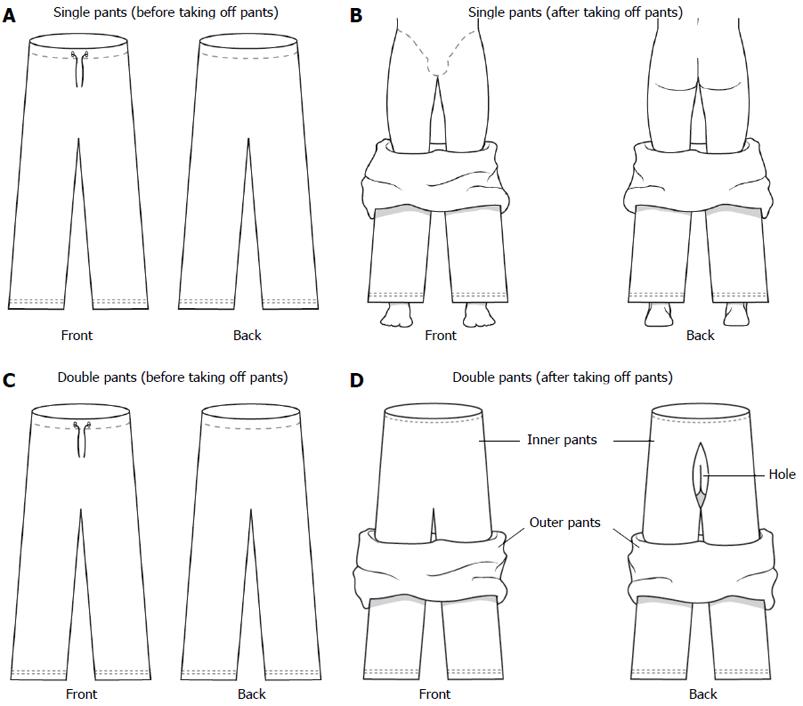
In CSP, there is no hole for insertion of the scope. Examinees remove the CSP to below the level of the buttocks and expose their buttocks area during colonoscopy, as shown in Figure 2A and B. NDP consist of single fabric only below the thigh, and doubled fabric from the hip to the thigh with a hole in the inner pants at the level of the buttocks. The hole is 25 cm wide and 15 cm long. Examinees wearing NDP can undergo colonoscopy without taking off the inner pants, as shown in Figure 2C and D. We supplied the 80 NDP (Bobo trading, Seoul, South Korea) to NDP group and 80 CSP (Seodaemun uniform, Seoul, South Korea) to CSP group. All patients got the pants in the hospital just before the procedure according to the randomized allocation by the nurse in outpatient clinic. The pants had been prepared with marking “A type’’ (CSP) and “B type’’ (NDP).
In this study the only one nurse, as the third party examiner, interviewed the patients before and after the procedure to exclude interviewer’s influence on the answers in this study. Before colonoscopy, examinees underwent a one-on-one interview in a quiet, separated room with a third-party examiner in which they completed questionnaires identifying state and trait anxiety, marital status, education, and residence. After colonoscopy, examinees had a similar one-on-one interview to complete the questionnaires, which included the Group Health Association of America 9 (GHAA 9) scales and questions regarding pant-specific satisfaction, state anxiety, and shame. After colonoscopy, examinees’ pain during colonoscopy was assessed after the procedure and scored from 0 to 10 using a face pain scale (0-very happy, no pain, 2-hurts just a little bit, 4-hurts a little more, 6-hurts even more, 8-hurts a lot, 10-hurts as much as you can imagine; don’t have to be crying to feel this much pain)[12].
Professional endoscopists who had performed more than 1000 colonoscopies performed all of the study colonoscopy procedures with a standard colonoscope (CF Q240L, CF Q240I, CF H260AI, CF Q260AI; Olympus Optical Co, Ltd, Tokyo, Japan). The indication for colonoscopy, ASA status, Ottawa quality scale, procedural time, number of polyps, number of examinees with polyps, method of polyp removal, rates of adverse events after polyp removal, rates of successful cecal approach, and gender difference between examinees and endoscopists in the NDP and CSP groups were investigated.
Satisfaction: The questionnaires measuring satisfaction included 14 questions regarding the examinees’ colonoscopy experience. Nine of the questions regarding overall satisfaction were derived from a previously validated GHAA 9 satisfaction survey[13]. These questions used a 5-point scale to grade satisfaction (1: poor, 2: fair, 3: good, 4: very good, 5: excellent). A score of more than 3 was considered a favorable response. Five questions were asked to elicit pants-specific satisfaction as related to the following: difficulty of defecation wearing the pants; difficulty in position change during the colonoscopy; worriness about the exposed buttock area; willingness to try the same pants for the next exam; and recommendation of the same pants to other people. The five pants-specific satisfaction questions used a 4-point scale to grade satisfaction (1, not at all; 2, somewhat; 3, moderately so; 4, very much so). Three of the five questions were negative questions about satisfaction and thus scored in reverse. Scores on pants-specific satisfaction ranged between 5 and 20.
Anxiety: The trait anxiety questionnaire has been shown to reflect the general disposition of patients or stable tendency for anxiety, while the state questionnaire reflects a patient’s anxiety related to a particular set of circumstances[9,14]. The trait and state questionnaires each consists of 20 statements, and all answers were graded using a 4-point scale (1, not at all; 2, somewhat; 3, moderately so; 4, very much so). Seven of the 20 questions from the STAI−Trait anxiety and 10 of the 20 questions from the STAI-State anxiety were negative questions and scored in reverse. The scores of the trait and state questionnaire range between 20 and 80, and higher scores reflected higher anxiety.
Shame: Among the experienced shame scale, 4 questions were used to measure body shame during colonoscopy[15]. We designed another 2 questions to measure shame following the exposure of the body during position change for the colonoscopy and exposure of the buttock area while walking to the colonoscopy room. In total, 6 different questions were used to measure shame. All answers were graded using a 4-point scale (1, not at all; 2, somewhat; 3, moderately so; 4, very much so). Scores on the body shame questionnaire ranged between 6 and 24, and higher scores reflected higher level of shame.
Informed consent was obtained from each patient included in the study. The study protocol conforms to the ethical guidelines of the 1975 Declaration of Helsinki (6th revision, 2008) as reflected in a prior approval by the institution’s human research committee. The study protocol was approved by the ethical committee of Yonsei University College of Medicine. The study protocol was also approved by clinicaltrial.gov (NCT 01524042).
All differences in CSP and NDP were examined using SPSS Statistics (version 18.0.0, IBM Corp., Armonk, NY, United States). Continuous variables were compared using Student’s t test, while categorical data were analyzed using the χ2 test (Fisher’s exact test) between two groups. Univariate and multivariate linear regression analysis were used to assess independent predictive factors associated with satisfaction, state anxiety after colonoscopy, and shame. For multivariate analysis, variables with P < 0.1 by univariate analysis were included. All statistical tests were two-tailed and considered statistically significant with a P value < 0.05.
There was no significant difference in baseline characteristics including age, gender, marital status, education, and residence in the study population and in the NDP and CSP groups in Table 1. There were no significant differences in the endoscopic characteristics of study population including indication for colonoscopy, Ottawa quality scale, procedural time, number of polyps, number of examinees with polyps, method of polyp removal, rates of adverse events after polyp removal, rates of successful cecal approach, pain scale, and gender difference between examinees and endoscopists in the NDP and CSP groups, as shown in Table 2.
| CSP (n = 80) | NDP (n = 80) | P value | |
| Age (yr) | 59.1 ± 11.4 | 59.4 ± 11.7 | 0.847 |
| 20 ≤ age < 40 | 3 (3.8) | 5 (6.2) | |
| 40 ≤ age < 60 | 38 (47.5) | 43 (53.8) | |
| age ≥ 60 | 39 (48.7) | 32 (40) | |
| Gender | 0.210 | ||
| Male | 41 (51.3) | 45 (56.3) | |
| Female | 39 (48.7) | 35 (43.7) | |
| Marital status | > 0.999 | ||
| Married | 75 (93.8) | 76 (96.0) | |
| Single or divorced | 5 (6.2) | 4 (4.0) | |
| Education | 0.320 | ||
| Middle school | 20 (25.0) | 13 (16.2) | |
| High school | 31 (38.8) | 28 (35.0) | |
| University | 22 (27.5) | 32 (40.0) | |
| Graduate school | 7 (8.7) | 7 (8.8) | |
| Residence | 0.609 | ||
| Urban | 73 (91.3) | 70 (87.5) | |
| Rural | 7 (8.7) | 10 (12.5) | |
| ASA status | 0.896 | ||
| Class I | 32 (40) | 36 (45.0) | |
| Class II | 48 (60) | 44 (55.0) | |
| Class III | 0 (0.0) | 0 (0.0) | |
| Class IV | 0 (0.0) | 0 (0.0) | |
| Class V | 0 (0.0) | 0 (0.0) |
| CSP (n = 80) | NDP (n = 80) | P value | |
| Indication of colonoscopy | 0.260 | ||
| Abnormality on other study | 2 (2.5) | 4 (5.0) | |
| Stool occult blood positive | 9 (11.2) | 13 (16.2) | |
| Screening | 47 (58.8) | 42 (52.5) | |
| Anemia | 0.0 (0) | 1.0 (1.2) | |
| Diarrhea | 3(3.8) | 4 (5.0) | |
| Surveillance after polyp removal | 6 (7.5) | 11 (13.8) | |
| Abdominal pain | 13 (16.2) | 5 (6.3) | |
| Ottawa Quality Scale | 3.9 ± 2.5 | 4.3 ± 2.8 | 0.382 |
| Procedural time (min) | |||
| Insertion | 10.7 ± 8.5 | 8.6 ± 5.5 | 0.059 |
| Withdrawal | 12.8 ± 6.2 | 11.8 ± 5.5 | 0.309 |
| Number of polyp | 1.1 ± 1.8 | 0.8 ± 1.5 | 0.266 |
| Number of examinees with polyps | 47 (58.8) | 42 (52.5) | 0.525 |
| Method of polyp removal | 0.521 | ||
| Biopsy | 25 (52.1) | 22 (56.4) | |
| Snaring polypectomy | 15 (31.3) | 8 (20.5) | |
| Endoscopic mucosal resection | 8 (16.6) | 9 (23.1) | |
| Adverse events | |||
| Bleeding | 0 (0.0) | 0 (0.0) | - |
| Perforation | 0 (0.0) | 0 (0.0) | - |
| Cecal approach | 80 (100) | 80 (100) | - |
| Pain scale1 | 3.5 ± 2.7 | 3.7 ± 2.4 | 0.719 |
| Genders between examinee and endoscopist | 0.525 | ||
| Same gender | 42 (52.5) | 47 (58.8) | |
| Different gender | 38 (47.5) | 33 (41.2) | |
There was no significant difference in GHAA9 score (Likert scale, 0-5) between the NDP and CSP groups. There were high favorable response rates (FRRs) which were greater than 90% for waiting time, waiting on procedure day, personal manner of physician and support staff, technical skills, adequacy of explanation, overall rating of the visit, and willingness to have the procedure repeated by the same physician and at the same facility in Table 3. In terms of pants-specific satisfaction in Table 3, the CSP group worried more about exposing the buttock area during the colonoscopy than did the NDP group (3.3 ± 0.7 vs 2.9 ± 0.7, P < 0.001). The NDP group was more willing to wear same pants when they undergo their next colonoscopy than the CSP group (3.3 ± 0.8 vs 2.1 ± 0.9, P < 0.001). The NDP group was also more willing to recommend other people wear the same pants when they undergo their own colonoscopies than the CSP group (3.3 ± 0.7 vs 2.0 ± 1.0, P < 0.001). A significantly lower shame score was estimated in the NDP group compared with CSP group (6.6 ± 1.5 vs 8.1 ± 3.2, P < 0.001), which is shown in Table 3.
| FRR, n (%) | Likert scale (mean ± SD) | |||||
| CSP | NDP | P value | CSP | NDP | P value | |
| GHAA9 | ||||||
| Appointment wait time | 73 (91.3) | 72 (90.0) | > 0.999 | 3.7 ± 0.7 | 3.6 ± 0.9 | 0.351 |
| Waiting on procedure day | 74 (92.5) | 76 (95.0) | 0.746 | 3.8 ± 0.8 | 3.9 ± 0.8 | 0.649 |
| Personal manner of physician | 78 (97.5) | 79 (98.8) | > 0.999 | 4.4 ± 0.6 | 4.4 ± 0.6 | 0.712 |
| Technical skills of physician | 74 (92.5) | 76 (95.0) | 0.746 | 4.1 ± 0.8 | 4.1 ± 0.7 | 0.564 |
| Personal manner of support staff | 77 (96.3) | 78 (97.5) | > 0.999 | 4.3 ± 0.7 | 4.0 ± 0.5 | 0.546 |
| Adequacy of explanation of what was done | 74 (92.5) | 78 (97.5) | 0.276 | 4.0 ± 0.6 | 4.0 ± 0.5 | 0.902 |
| Overall rating of visit | 75 (93.8) | 74 (92.5) | > 0.999 | 3.9 ± 0.6 | 3.9 ± 0.6 | 0.806 |
| Yes/No questions | ||||||
| Would have procedure by same physician: Yes | 78 (97.5) | 77 (96.3) | > 0.999 | |||
| Would have procedure at same facility: Yes | 79 (98.8) | 79 (98.8) | > 0.999 | |||
| Pants specific satisfaction | ||||||
| Difficulty in defecation | 3.7 ± 0.5 | 3.8 ± 0.4 | 0.106 | |||
| Difficulty in position change | 3.7 ± 0.5 | 3.8 ± 0.3 | 0.175 | |||
| Worriness about exposing buttock area in procedure | 3.3 ± 0.7 | 2.9 ± 0.7 | < 0.001 | |||
| Will to wear same pants at next colonoscopy | 2.1 ± 0.9 | 3.3 ± 0.8 | < 0.001 | |||
| Will to recommend to other people to wear same pants | 2.0 ± 1.0 | 3.3 ± 0.7 | < 0.001 | |||
| Before colonoscopy | ||||||
| Total scores of trait anxiety | 39.2 ± 8.8 | 39.4 ± 8.2 | 0.904 | |||
| Total scores of state anxiety | 37.9 ± 8.2 | 39.9 ± 8.8 | 0.144 | |||
| After colonoscopy | ||||||
| Total scores of state anxiety | 35.4 ± 6.9 | 33.0 ± 7.0 | 0.028 | |||
| Total scores of shame | 8.1 ± 3.2 | 6.6 ± 1.5 | < 0.001 | |||
| Change of state anxiety before and after the procedure | -2.4 ± 7.6 | -6.9 ± 8.4 | 0.001 | |||
To investigate the predictive factors related to satisfaction, state anxiety, and shame after colonoscopy, univariate and multivariate regression analysis was performed (Table 4). In the multivariate analysis of pants-specific satisfaction, unmarried examinees had less pants-specific satisfaction than married examinees [B (SE) = -1.82 (0.61), P = 0.004], and the NDP group had higher pants-specific satisfaction than the CSP group [B (SE) = 2.72 (0.28), P < 0.001]. In multivariate analysis of state anxiety after the colonoscopy, female participants had higher state anxiety score after the procedure than males [B (SE) = 3.52 (1.14), P = 0.002]. Unmarried examinees had higher state anxiety score after colonoscopy than married examinees [B (SE) = 4.45 (2.22), P = 0.047]. Urban examinees had higher state anxiety score after colonoscopy than rural examinees [B (SE) = 4.68 (1.70), P = 0.007]. The NDP group had a tendency of lower state anxiety score after colonoscopy than the CSP group [B (SE) = -1.80 (1.04), P = 0.086]. In the multivariate analysis of shame, female examinees had higher shame score than male examinees [B (SE) = 1.25 (0.37), P = 0.001]. Unmarried examinees also had higher shame score than married examinees [B (SE) = 2.78 (0.81), P = 0.001]. The NDP group had lower shame score than the CSP group [B (SE) = -1.37 (0.37), P = 0.001].
| Predictive factors | Outcome (pants specific satisfaction) | Outcome (state anxiety after colonoscopy) | Outcome (shame after colonoscopy) | |||||||||
| Univariate | Multivariate | Univariate | Multivariate | Univariate | Multivariate | |||||||
| B (SE) | P value | B (SE) | P value | B (SE) | P value | B (SE) | P value | B (SE) | P value | B (SE) | P value | |
| Sex | ||||||||||||
| Male | Ref. | Ref. | Ref. | Ref. | Ref. | |||||||
| Female | 0.04 (0.36) | 0.913 | 4.29 (1.06) | 0.913 | 3.52 (1.14) | 0.002 | 1.31 (0.40) | 0.001 | 1.25 (0.37) | 0.001 | ||
| Age | -0.02 (0.01) | 0.104 | 0.01 (0.04) | 0.104 | -0.01 (0.01) | 0.928 | ||||||
| Marital status | ||||||||||||
| Married | Ref. | Ref. | Ref. | Ref. | Ref. | Ref. | ||||||
| Unmarried | -1.6 (0.7) | 0.033 | -1.82 (0.61) | 0.004 | 4.48 (2.40) | 0.033 | 4.45 (2.22) | 0.047 | 2.79 (0.87) | 0.002 | 2.78 (0.81) | 0.001 |
| Education | ||||||||||||
| Middle school | Ref. | Ref. | Ref. | |||||||||
| High school | -0.04 (0.49) | 0.931 | -1.81 (1.53) | 0.931 | -0.01 (0.57) | 0.998 | ||||||
| University | 0.27 (0.50) | 0.506 | -2.64 (1.55) | 0.506 | 0.22 (0.58) | 0.697 | ||||||
| Graduate school | 0.57 (0.73) | 0.430 | -2.50 (2.24) | 0.430 | 0.15 (0.84) | 0.853 | ||||||
| Type of pants | ||||||||||||
| CSP | Ref. | Ref. | Ref. | Ref. | Ref. | Ref. | ||||||
| NDP | 2.70 (0.29) | < 0.001 | 2.72 (0.28) | < 0.001 | -2.43 (1.10) | < 0.001 | -1.80 (1.04) | 0.086 | -1.47 (0.39) | < 0.001 | -1.37 (0.37) | 0.001 |
| Residence | ||||||||||||
| Rural area | Ref. | Ref. | Ref. | Ref. | ||||||||
| Urban area | -0.46 (0.58) | 0.430 | 4.2 (1.7) | 0.430 | 4.68 (1.70) | 0.007 | 0.93 (0.67) | 0.165 | ||||
| Genders between examinee and endoscopist | ||||||||||||
| Same gender | Ref. | Ref. | Ref. | Ref. | ||||||||
| Different gender | -0.36 (0.36) | 0.308 | 3.90 (1.07) | < 0.001 | 1.45 (1.15) | 0.209 | 0.65 (0.41) | 0.115 | ||||
In this study, we compared the satisfaction, anxiety and shame between NDP and CSP with prospective randomized control trial. The examinees in NDP group responded with higher pants-specific satisfaction, lower state anxiety after colonoscopy, and lower shame scores compared to those in CSP group. Thus, the NDP developed at our institution may contribute to increased satisfaction and decreased anxiety and shame after colonoscopy.
Although there have been a wide range of studies regarding satisfaction[1,16-20] and anxiety[9,21-23] during colonoscopy, our study was unique because it specifically addressed colonoscopic pants and investigated the differences in emotional change by the type of colonoscopic pants participants wore. Colonoscopic pants were designed considering the maximization of the efficiency of colonoscopies and hygiene aspects. Various types of colonoscopic pants have been used at different institutions. In some centers, examinees wear CSP or pants with a hole in the buttock area with a movable flap, which can potentially expose buttock area during walking. In other centers, examinees wear single pants with hole in the buttocks and outer gown to hide the hole, which is likely inferior to the NDP we describe in terms of repair and maintenance expenses.
In our study there was no significant difference in GHAA 9 patient satisfaction between NDP and CSP groups as the contents of GHAA 9 were not closely connected with satisfaction regarding colonoscopic pants. However, in the survey of pants-specific satisfaction, the NDP group showed increased satisfaction than the CSP group in terms of their willingness to wear the same pants in the next time and to recommend the same pants to other people. High patient satisfaction during colonoscopy may result in a higher rate of compliance with screening and clinical surveillance programs[1]. The American Society for Gastrointestinal Endoscopy and the American College of Gastroenterology recommends assessment of patient satisfaction during colonoscopy to evaluate the quality of colonoscopy[5,6].
The sensitivity related to the psychological aspects including anxiety and shame might partly depends on the different characteristics including age, gender, behavior, social environment and sensitivity of the society. As example lower anxiety scores was reported to be associated with older age, male sex, lower income, experience of previous colonoscopy and lower education[9]. During gastrointestinal endoscopic procedures, female examinees have been reported to have higher state and trait anxiety levels than male examinees[10,22]. In our study, female, unmarried, urban examinees and CSP group had more state anxiety after colonoscopy than that of their male, married, rural examinees and NDP group counterparts. The differences of shame and state of anxiety after colonoscopy between the two groups were moderate in most of the items. But, the difference in change of state of anxiety before and after the procedure might be clinically significant. Because all participants are healthy persons in psychological aspect at baseline, even moderate change of anxiety level after colonoscopy could result in decreased satisfaction of the procedure and reduced compliance to next examinations in clinical practice.
There were some limitations to our study. Endoscopists could not be completely blinded to the types of colonoscopic pants worn because they ultimately saw which pants they were wearing during the colonoscopic procedure. However, the outcome assessors were blinded during the total period of study. In addition, all the endoscopists who performed the colonoscopy were excluded from the outcome assessors. And there was no questionnaire for endoscopists in this study. Examinees with cancer or IBD were suspected to have higher anxiety levels during colonoscopy, and thus were excluded. Therefore understanding the satisfaction, anxiety, and satisfaction of these particular examinees would require further investigation. Most of examinees in this study were over 40 years old and more than half of examinees underwent colonoscopy for screening purposes; the number of young unmarried examinees was very small in this study, and the level of anxiety, shame and satisfaction in this group may be significantly different. For a more ideal comparision of anxiety, shame and satisfaction during colonoscopy between the NDP and CSP group, it would be better for one examinee to wear single pants and double pants during colonoscopy, but this was not logistically feasible. To compensate for this limitation in state anxiety we measured the change in state anxiety before and after colonoscopy in the same examinees.
In conclusion, the examinees in the NDP group had higher pants-specific satisfaction and lower state anxiety and lower shame after colonoscopy compared to CSP group. Therefore NDP could help to increase satisfaction and decrease anxiety and shame after colonoscopy. Future studies should continue to investigate factors for anxiety, shame and satisfaction.
We thank Mr. Dong-Su Jang for help in preparing the specimens and figures.
Exposing buttocks during colonoscopy can make examinees feel unsatisfied, anxious, and shameful. To increase satisfaction and diminish anxiety and shame during colonoscopy, the authors developed novel double pants (NDP) which consist of doubled fabrics with an inner hole.
Pants-specific satisfaction scores regarding willingness to repeat colonoscopy using same pants and recommendation of same pants to other people were significantly higher in NDP than conventional single pants (CSP) groups. State anxiety and shame after colonoscopy was lower in NDP group compared with CSP group.
Although there have been a wide range of studies regarding satisfaction and anxiety during colonoscopy, this study was unique because it specifically addressed colonoscopic pants. The authors developed NDP, which consist of single fabric only below the thigh, and doubled fabric from the hip to the thigh with a hole in the inner pants at the level of the buttocks. Examinees wearing NDP can undergo colonoscopy without taking off the inner pants.
Through these findings, the NDP developed at our institution may contribute to increased satisfaction and decrease anxiety and shame after colonoscopy.
NDP are single fabric only below the thigh, and doubled fabric from the hip to the thigh with a hole in the inner pants at the level of the buttocks. The hole is 25 cm wide and 15 cm long.
Satisfaction studies are important in relationship with the compliance of colorectal cancer screening programs and less so in the group of patients with specific suspicion of diseases affecting the anus, rectum or colon. This complex study is well designed and analyzed. The topic of the manuscript is interesting and the work performed is ambitious.
P- Reviewers Blom J, Bordas JM, Bujanda L S- Editor Zhai HH L- Editor A E- Editor Ma S
| 1. | Seip B, Bretthauer M, Dahler S, Friestad J, Huppertz-Hauss G, Høie O, Kittang E, Nyhus S, Pallenschat J, Sandvei P. Patient satisfaction with on-demand sedation for outpatient colonoscopy. Endoscopy. 2010;42:639-646. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 29] [Cited by in RCA: 37] [Article Influence: 2.5] [Reference Citation Analysis (0)] |
| 2. | Porostocky P, Chiba N, Colacino P, Sadowski D, Singh H. A survey of sedation practices for colonoscopy in Canada. Can J Gastroenterol. 2011;25:255-260. [PubMed] |
| 3. | Cohen LB, Wecsler JS, Gaetano JN, Benson AA, Miller KM, Durkalski V, Aisenberg J. Endoscopic sedation in the United States: results from a nationwide survey. Am J Gastroenterol. 2006;101:967-974. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 331] [Cited by in RCA: 357] [Article Influence: 18.8] [Reference Citation Analysis (0)] |
| 4. | Froehlich F, Harris JK, Wietlisbach V, Burnand B, Vader JP, Gonvers JJ. Current sedation and monitoring practice for colonoscopy: an International Observational Study (EPAGE). Endoscopy. 2006;38:461-469. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 71] [Cited by in RCA: 67] [Article Influence: 3.5] [Reference Citation Analysis (0)] |
| 5. | Faigel DO, Pike IM, Baron TH, Chak A, Cohen J, Deal SE, Hoffman B, Jacobson BC, Mergener K, Petersen BT. Quality indicators for gastrointestinal endoscopic procedures: an introduction. Gastrointest Endosc. 2006;63:S3-S9. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 70] [Cited by in RCA: 75] [Article Influence: 3.9] [Reference Citation Analysis (0)] |
| 6. | Quality improvement of gastrointestinal endoscopy: guidelines for clinical application. From the ASGE. American Society for Gastrointestinal Endoscopy. Gastrointest Endosc. 1999;49:842-844. [PubMed] |
| 7. | Parker D. Human responses to colonoscopy. Gastroenterol Nurs. 1992;15:107-109. [PubMed] |
| 8. | Brandt LJ. Patients’ attitudes and apprehensions about endoscopy: how to calm troubled waters. Am J Gastroenterol. 2001;96:280-284. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 33] [Cited by in RCA: 45] [Article Influence: 1.9] [Reference Citation Analysis (0)] |
| 9. | Jones MP, Ebert CC, Sloan T, Spanier J, Bansal A, Howden CW, Vanagunas AD. Patient anxiety and elective gastrointestinal endoscopy. J Clin Gastroenterol. 2004;38:35-40. [PubMed] |
| 10. | Trevisani L, Sartori S, Putinati S, Gaudenzi P, Chiamenti CM, Gilli G, Grassi L, Abbasciano V. [Assessment of anxiety levels in patients during diagnostic endoscopy]. Recenti Prog Med. 2002;93:240-244. [PubMed] |
| 11. | Tønnesen H, Puggaard L, Braagaard J, Ovesen H, Rasmussen V, Rosenberg J. Stress response to endoscopy. Scand J Gastroenterol. 1999;34:629-631. [PubMed] |
| 12. | Warden V, Hurley AC, Volicer L. Development and psychometric evaluation of the Pain Assessment in Advanced Dementia (PAINAD) scale. J Am Med Dir Assoc. 2003;4:9-15. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 587] [Cited by in RCA: 606] [Article Influence: 27.5] [Reference Citation Analysis (0)] |
| 13. | Del Río AS, Baudet JS, Fernández OA, Morales I, Socas Mdel R. Evaluation of patient satisfaction in gastrointestinal endoscopy. Eur J Gastroenterol Hepatol. 2007;19:896-900. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 21] [Cited by in RCA: 26] [Article Influence: 1.4] [Reference Citation Analysis (0)] |
| 14. | Spielberger CD, Gorsuch RL, Lushene RE. STAI manual for the state-trait anxiety inventory (“self-evaluation questionnaire”). Palo Alto: Consulting Psychologists Press, Inc 1970; 1-23. |
| 15. | Andrews B, Qian M, Valentine JD. Predicting depressive symptoms with a new measure of shame: The Experience of Shame Scale. Br J Clin Psychol. 2002;41:29-42. [PubMed] |
| 16. | Nijjar UK, Edwards JA, Short MW. Patient satisfaction with family physician colonoscopists. J Am Board Fam Med. 2011;24:51-56. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1] [Cited by in RCA: 3] [Article Influence: 0.2] [Reference Citation Analysis (0)] |
| 17. | Lin OS, Kozarek RA, Arai A, Gluck M, Jiranek GC, Kowdley KV, McCormick SE, Schembre DB, Soon MS, Dominitz JA. The effect of periodic monitoring and feedback on screening colonoscopy withdrawal times, polyp detection rates, and patient satisfaction scores. Gastrointest Endosc. 2010;71:1253-1259. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 52] [Cited by in RCA: 62] [Article Influence: 4.1] [Reference Citation Analysis (0)] |
| 18. | Ko HH, Zhang H, Telford JJ, Enns R. Factors influencing patient satisfaction when undergoing endoscopic procedures. Gastrointest Endosc. 2009;69:883-891, quiz 891.e1. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 66] [Cited by in RCA: 88] [Article Influence: 5.5] [Reference Citation Analysis (0)] |
| 19. | Chartier L, Arthurs E, Sewitch MJ. Patient satisfaction with colonoscopy: a literature review and pilot study. Can J Gastroenterol. 2009;23:203-209. [PubMed] |
| 20. | Bytzer P, Lindeberg B. Impact of an information video before colonoscopy on patient satisfaction and anxiety - a randomized trial. Endoscopy. 2007;39:710-714. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 50] [Cited by in RCA: 56] [Article Influence: 3.1] [Reference Citation Analysis (0)] |
| 21. | Ersöz F, Toros AB, Aydoğan G, Bektaş H, Ozcan O, Arikan S. Assessment of anxiety levels in patients during elective upper gastrointestinal endoscopy and colonoscopy. Turk J Gastroenterol. 2010;21:29-33. [PubMed] |
| 22. | Mitsonis C, Dimopoulos N, Zavrou M, Psarra V, Giofkos C, Fiorakis C, Dimitriadis A, Valavanis D, Vousoura E, Zervas I. Panic Attack during Elective Gastrointestinal Endoscopy. Gastroenterol Res Pract. 2011;2011:162574. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 2] [Cited by in RCA: 6] [Article Influence: 0.4] [Reference Citation Analysis (0)] |
| 23. | Ovayolu N, Ucan O, Pehlivan S, Pehlivan Y, Buyukhatipoglu H, Savas MC, Gulsen MT. Listening to Turkish classical music decreases patients’ anxiety, pain, dissatisfaction and the dose of sedative and analgesic drugs during colonoscopy: a prospective randomized controlled trial. World J Gastroenterol. 2006;12:7532-7536. [PubMed] |