Published online Jun 14, 2013. doi: 10.3748/wjg.v19.i22.3528
Revised: April 11, 2013
Accepted: May 7, 2013
Published online: June 14, 2013
Processing time: 108 Days and 15.6 Hours
Delayed liver laceration following transjugular intrahepatic portosystemic shunt (TIPS) is a serious and likely underdiagnosed complication. It is however an important complication following TIPS, which remains one of the most technically challenging interventional procedures performed. In addition to laceration, a number of complications regarding bleeding and perforation are well described following TIPS procedures. We feel the adoption of techniques such as ours and that of other authors described in the literature using an ultrasound-guided percutaneous transhepatic approach with a small caliber needle provides a safer and less traumatic procedure and should reduce complications of bleeding and almost completely eliminate the risk of liver laceration. Our procedure was successfully performed under conscious sedation rather than general anaesthesia further reducing the overall procedural risk to the patient.
Core tip: Transjugular intrahepatic portosystemic shunt (TIPS) for complications of portal hypertension is commonly formed by accessing a portal vein branch from a metal cannula wedged in a hepatic vein. A number of serious procedural complications including bleeding and perforation following TIPS have been described. We feel the adoption of techniques such as ours and that of other authors described in the literature using an ultrasound-guided percutaneous transhepatic approach with a small caliber needle provides a safer and less traumatic procedure and should reduce complications of bleeding and almost completely eliminate the risk of liver laceration.
- Citation: Leong S, Kok HK, Govender P, Torreggiani W. Reducing risk of transjugular intrahepatic portosystemic shunt using ultrasound guided single needle pass. World J Gastroenterol 2013; 19(22): 3528-3530
- URL: https://www.wjgnet.com/1007-9327/full/v19/i22/3528.htm
- DOI: https://dx.doi.org/10.3748/wjg.v19.i22.3528
We read with interest the excellent article by Liu et al[1] regarding the delayed liver laceration following transjugular intrahepatic portosystemic shunt (TIPS) for portal hypertension. This is a serious and likely underdiagnosed complication. It is however an important complication following TIPS, which remains one of the most technically challenging interventional procedures performed. In addition to laceration, a number of complications regarding bleeding and perforation are well described following TIPS procedures.
In their paper, Liu et al[1] correctly established a number of factors which contribute to bleeding and liver injury following TIPS: (1) liver cirrhosis with coagulopathy; (2) liver parenchyma and vascular injury during TIPS; and (3) early stent anticoagulation with low molecular weight heparin. While we fully agree with these postulations, we feel that another important factor is the needle size used for percutaneous access and tract creation between the portal vein and the hepatic veins during TIPS. In our department, we have recently adopted a new technique utilising a 22-gauge microneedle and percutaneous liver puncture under direct ultrasound visualisation that dramatically decreases the risk of laceration.
This modification may help refine and improve the outcome of patients undergoing TIPS placement. The creation of the shunt between the portal and hepatic veins is traditionally performed under fluoroscopic guidance, and is considered the most difficult step in the establishment of a TIPS[2], and is usually successful only after several punctures[3]. This “blind” fluoroscopic procedure can be refined with fluoroscopic methods including wedged hepatic venography[4] and superior mesenteric artery arterial portography[5]. Ultrasound assisted TIPS which facilitates the creation of the portosystemic shunt have also been described including placement of metallic overlying skin markers[6], placement of metallic coils adjacent to or microwire placement within the portal vein[7]. These methods attempt to reduce the time spent achieving the portosystemic shunt and thus, the risk of bleeding complications.
More interestingly, the removal of the step requiring blind puncture of the portal vein has been described in the recent literature. Raza et al[8] described a single-pass technique to access the right portal and right hepatic veins under ultrasound guidance using an 18-gauge, 20-cm Chiba needle (Cook) with a technical success rate of 73% and no evidence of post-procedure puncture site haemorrhage. Liang et al[2] also achieved 100% technical success and no evidence of post-TIPS internal hemorrhage with a similar technique in patients with severely distorted liver parenchyma to obtain a left portal vein and inferior vena cava (IVC) shunt, using an 18-gauge, 20-cm needle. Whilst small in patient numbers, these studies highlight the feasibility of ultrasound guidance to reduce the number of punctures required to achieve a portosystemic shunt, which thus reduces the risk of bleeding.
To further reduce the risk of bleeding in these patients who are often coagulopathic, it is suggested to use a further modification of Raza et al[8] and Liang et al’s[2] technique using initial access with a 22-gauge, 20-cm Chiba needle (Cook) in an attempt to reduce the bleeding risk from the most challenging step of the TIPS procedure, especially in high risk patients. This method has also been described in a small series by Gazzera et al[9] in 8 patients with 100% technical success. This method requires pre-procedural drainage of ascites, if present, under ultrasound guidance with a 7-8 Fr pigtail catheter. Embolisation of the transhepatic needle tract can also be considered[8] especially in cases where ascites is present[2]. Where available, intravascular ultrasound may be useful to guide shunt creation especially in cases with portal vein thrombosis, distorted anatomy, Budd-Chiari syndrome or hepatic tumors[10].
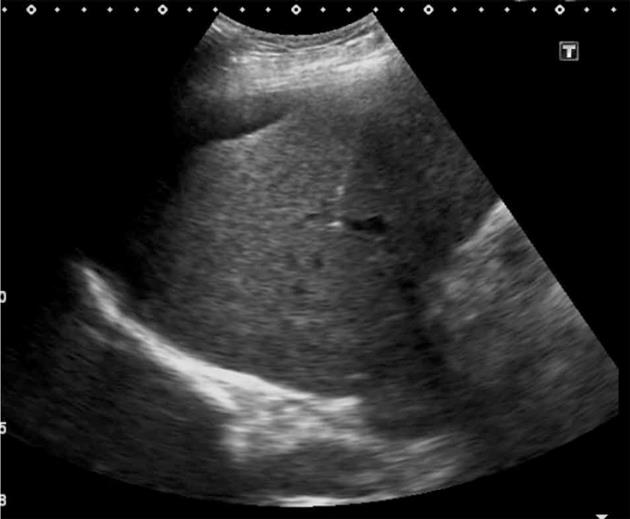
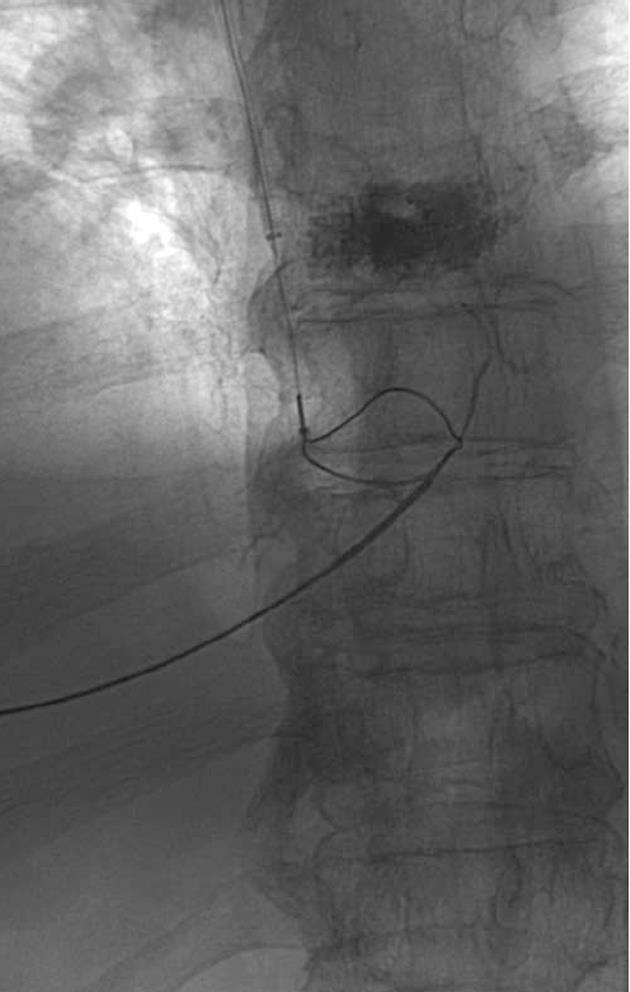
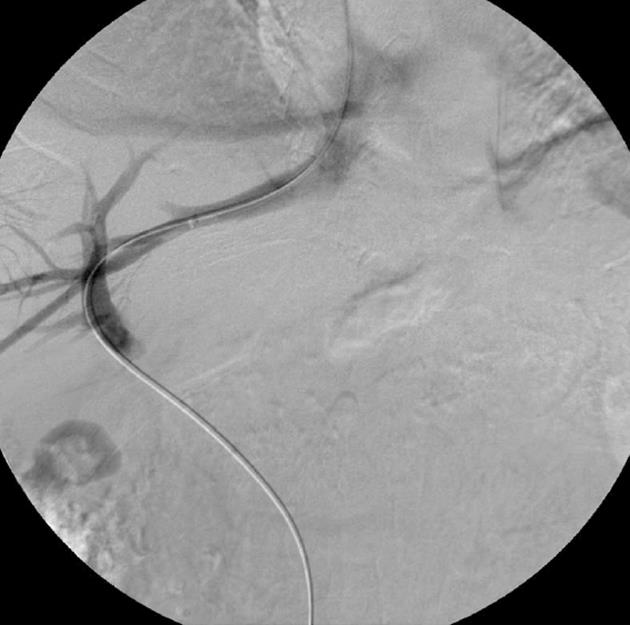
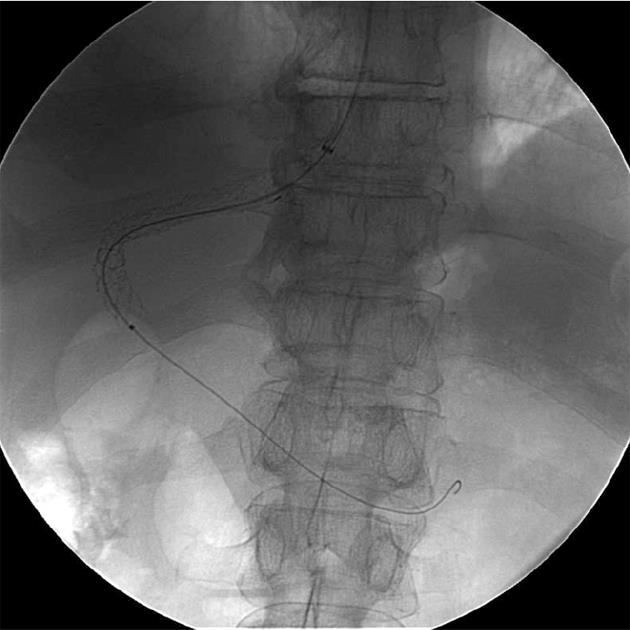
We recently adopted a modified transhepatic single-needle pass for TIPS in our institution. It involved a 53-year-old male with cirrhosis undergoing TIPS for refractory ascites. His pre-procedure work up revealed a Child-Pugh B and Model for End-stage Liver Disease score of 14. Prior to the modified TIPS procedure, the ascites was drained under ultrasound guidance. Following this, both the neck and abdomen were prepared for a combined transjugular and transhepatic approach followed by administration of conscious sedation with intravenous midazolam and fentanyl. Using real time ultrasound guidance, the right portal vein (Figure 1) was punctured with a 22-gauge, 20-cm Chiba needle (Cook) close to the bifurcation of the main portal vein (MPV), with entry confirmed by aspiration of blood. Following this, the needle was advanced into the right hepatic vein under real-time ultrasound guidance, with confirmation of entry by blood aspiration. A 0.018-inch Nitinol guidewire was then advanced into the hepatic vein, IVC and right atrium. The tract was upsized with a 7-Fr co-axial introducer system. The introducer and stiffner was then removed allowing passage of a 0.035-inch Amplatz Ultrastiff guidewire (Cook) into the right atrium. The right internal jugular vein was the accessed under ultrasound guidance using a micropuncture set (Cook) comprising of a 21-gauge needle, 0.018-inch guidewire and 4-Fr co-axial catheter. This was then upsized to a 6-Fr long vascular sheath into the right atrium. At this point, a 25-mm diameter Amplatz Gooseneck Snare (ev3 Inc) was used to snare the transhepatic wire, achieving through and through access (Figure 2). The sheath was then advanced into the hepatic vein over the transhepatic-transjugular wire until resistance was met. A 6 mm × 20 mm and 8 mm × 20 mm angioplasty balloon catheter (Powerflex Pro, Cordis) was advanced over the wire and the hepatic and portal vein tract was dilated. The sheath was advanced into the dilated tract, and contrast was injected through the sheath to confirm intraportal position. A 0.035-inch, 260-cm long hydrophilic wire (Glidewire Advantage, Terumo, Japan) and 5-Fr Berenstein catheter was then introduced through the transjugular sheath and manipulated into the MPV and then into the superior mesenteric vein (Figure 3). The transhepatic–transjugular wire was removed at this stage, and the 6-Fr sheath was replaced with a 10-Fr sheath. The procedure was completed as a conventional TIPS with deployment of a 10 mm × 70 mm (Viatorr, WL Gore and Associates) TIPS endoprosthesis stent (Figure 4). The patient remained stable with an uncomplicated post-procedural course and was discharged after 3 d with a satisfactory baseline post-TIPS ultrasound.
We feel the adoption of techniques such as ours and that of other authors described in the literature using an ultrasound-guided percutaneous transhepatic approach with a small caliber needle provides a safer and less traumatic procedure and should reduce complications of bleeding and almost completely eliminate the risk of liver laceration. Finally, our procedure was successfully performed under conscious sedation rather than general anaesthesia further reducing the overall procedural risk to the patient.
In conclusion, the authors should be commended for publication of this important complication of liver laceration following TIPS, which remains one of the most technically challenging interventional procedures but we hope that adoption of a microneedle controlled approach will potentially eliminate such complications.
P- Reviewer Izumi N S- Editor Wang JL L- Editor A E- Editor Xiong L
| 1. | Liu K, Fan XX, Wang XL, He CS, Wu XJ. Delayed liver laceration following transjugular intrahepatic portosystemic shunt for portal hypertension. World J Gastroenterol. 2012;18:7405-7408. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in CrossRef: 5] [Cited by in RCA: 7] [Article Influence: 0.5] [Reference Citation Analysis (0)] |
| 2. | Liang HL, Liu WC, Huang JS, Chen MC, Lai KH, Pan HB, Chen CK. TIPS in patients with cranial porta hepatis: ultrasound-guided transhepatic portohepatic-portocaval puncture in single needle pass. AJR Am J Roentgenol. 2011;196:914-918. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1] [Cited by in RCA: 4] [Article Influence: 0.3] [Reference Citation Analysis (0)] |
| 3. | Zemel G, Becker GJ, Bancroft JW, Benenati JF, Katzen BT. Technical advances in transjugular intrahepatic portosystemic shunts. Radiographics. 1992;12:615-622; discussion 623-624. [PubMed] |
| 4. | Freedman AM, Sanyal AJ, Tisnado J, Shiffman ML, Luketic VA, Fisher RA, Posner MP. Results with percutaneous transjugular intrahepatic portosystemic stent-shunts for control of variceal hemorrhage in patients awaiting liver transplantation. Transplant Proc. 1993;25:1087-1089. [PubMed] |
| 5. | Rees CR, Niblett RL, Lee SP, Diamond NG, Crippin JS. Use of carbon dioxide as a contrast medium for transjugular intrahepatic portosystemic shunt procedures. J Vasc Interv Radiol. 1994;5:383-386. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 50] [Cited by in RCA: 51] [Article Influence: 1.6] [Reference Citation Analysis (0)] |
| 6. | Nöldge G, Rössle M, Richter GM, Perarnau JM, Palmaz JC. [Modelling the transjugular intrahepatic portosystemic shunt using a metal prosthesis: requirements of the stent]. Radiologe. 1991;31:102-107. [PubMed] |
| 7. | Roizental M, Kane RA, Takahashi J, Kruskal J, Crenshaw WB, Perry L, Stokes K, Clouse ME. Portal vein: US-guided localization prior to transjugular intrahepatic portosystemic shunt placement. Radiology. 1995;196:868-870. [PubMed] |
| 8. | Raza SA, Walser E, Hernandez A, Chen K, Marroquin S. Transhepatic puncture of portal and hepatic veins for TIPS using a single-needle pass under sonographic guidance. AJR Am J Roentgenol. 2006;187:W87-W91. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 31] [Cited by in RCA: 33] [Article Influence: 1.7] [Reference Citation Analysis (0)] |
| 9. | Gazzera C, Fonio P, Gallesio C, Camerano F, Doriguzzi Breatta A, Righi D, Veltri A, Gandini G. Ultrasound-guided transhepatic puncture of the hepatic veins for TIPS placement. Radiol Med. 2013;118:379-385. [PubMed] |
| 10. | Farsad K, Fuss C, Kolbeck KJ, Barton RE, Lakin PC, Keller FS, Kaufman JA. Transjugular intrahepatic portosystemic shunt creation using intravascular ultrasound guidance. J Vasc Interv Radiol. 2012;23:1594-1602. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 51] [Cited by in RCA: 61] [Article Influence: 4.7] [Reference Citation Analysis (0)] |