Published online Sep 7, 2011. doi: 10.3748/wjg.v17.i33.3795
Revised: December 1, 2010
Accepted: December 8, 2010
Published online: September 7, 2011
Minimally invasive surgery started spreading worldwide in 1987, when the first laparoscopic cholecystectomy was performed. Meanwhile, improvement of endoscopic equipment and instruments allowed gastroenterologists to attempt more aggressive endoluminal interventions, even beyond the wall barrier. The first transgastric peritoneoscopy, in 2004, brought to light the concept of natural orifice transluminal endoscopic surgery (NOTES). The idea of incisionless surgery is attractive and has become a new goal for both surgeons and other people interested in this field of investigation. The authors present a review of all developments concerning NOTES, including animal studies and human experience.
- Citation: Moreira-Pinto J, Lima E, Correia-Pinto J, Rolanda C. Natural orifice transluminal endoscopy surgery: A review. World J Gastroenterol 2011; 17(33): 3795-3801
- URL: https://www.wjgnet.com/1007-9327/full/v17/i33/3795.htm
- DOI: https://dx.doi.org/10.3748/wjg.v17.i33.3795
Surgery has experienced a huge development in the past three decades after Dr. Philippe Mouret performed the first laparoscopic cholecystectomy in 1987. Since then, minimally invasive surgery has begun to spread worldwide[1]. This was largely in part due to patient demands for laparoscopic surgery’s advantages - shorter hospital stays, less pain, and smaller, less disfiguring scars[2]. The improvement of available equipment and instruments allowed more and more surgical procedures to be made through a minimally invasive approach, rapidly becoming a standard practice in most procedures.
At the same time, progresses in gastrointestinal endoscopy have made it an indispensable and multifaceted instrument for diagnosis and therapy. Besides endoluminal procedures, gastroenterologists attempted some interventions beyond the wall barrier, such as pseudocyst drainage[3] and percutaneous endoscopic gastrostomy[4]. However, it was not until 2004 that Kalloo et al[5] published the first report of a true transluminal procedure, a transgastric peritoneoscopy in a porcine model, which brought to light the concept of natural orifice transluminal endoscopic surgery (NOTES). The idea of incisionless surgery was attractive and has now become a new goal for both surgeons and other people interested in this field of investigation.
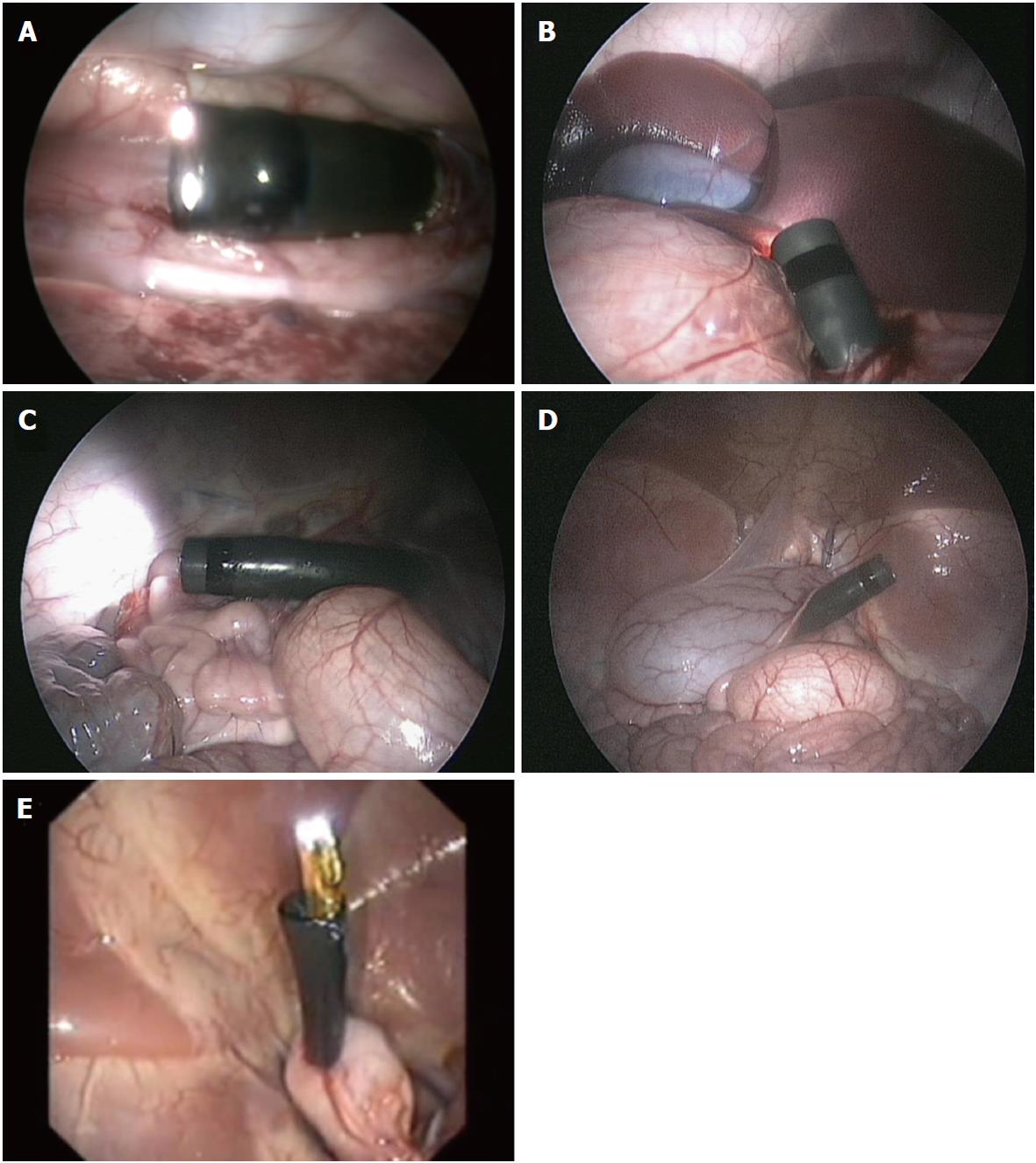
The term NOTES describes novel endoscopic interventions on internal organs performed through natural orifices[6]. In this new approach, endoscopes enter the abdominal and thoracic cavities via any single or combination of natural orifices - mouth, urethra, vagina, and anus. Depending on the orifice, rigid or flexible equipment can be used. The lower “short-ways” (bladder, colon or vagina) allow the easy passage of rigid or flexible instruments into the abdominal cavity, but the upper “long-ways” (esophagus and stomach) require flexible equipment[7] (Figure 1).
The main goal for NOTES is avoiding skin incisions. Other theoretical advantages include: decreased post-operative pain, reduction/elimination of general anesthesia, performance of procedures in an outpatient or even office setting, and possibly cost reduction. Moreover, eliminating skin incision avoids associated complications such as wound infections and hernias, as well as reduction in hospital stay, faster return to bowel function, improved cosmetic outcomes, and increased overall patient satisfaction[2].
The first challenge in NOTES is getting good and clean access to the cavity we want to “scope” (Table 1). The first mention of natural orifice procedure dates back to the 1940s, when culdoscopies were performed using an endoscope passed through the recto-uterine pouch to view pelvic organs, as well as to perform sterilization procedures[8]. At that time, these procedures did not gain much popularity and were restricted to some gynecological procedures. Recently, however, they were recovered by NOTES development. In 2002, Gettman et al[9] published one pure transvaginal nephrectomy along a series of hybrid transvaginal nephrectomy in a porcine model.
| Transesophageal | Transgastric | Transvesical | Transvaginal | Transcolonic | |
| Rigid instruments | No | No | Yes | Yes | Yes |
| Available in both genders | Yes | Yes | Yes | No | Yes |
| Sterility | No | No | Yes | No | No |
| Size | Wide | Wide | Up to 6 mm | Wide | Wide |
| Closur | Endoscopic (in study) | Endoscopic (in study) | Endoscopic (in study) | Direct suture | Endoscopic (in study) |
| Specimen retrieval | Not reported | Possible | Not reported | Possible | Possible |
Taking advantage of the great developments in gastrointestinal endoscopy, some pioneers began working on the transgastric approach to the abdominal cavity. The first published description of transgastric peritoneoscopy was in 2004 by Kalloo et al[5], in a porcine model. Since then, a number of successful transgastric procedures have been attempted and performed[10-20]. These initial studies also identified major limitations of the isolated transgastric approach, mainly in more complex procedures such as cholecystectomy, first described in 2005 by Park et al[21]. Lack of triangulation and platform stability were the main problems identified. Searching for solutions to these problems, researchers tried other ways of entering the abdominal cavity. Fong et al[22-24] published the first transcolonic peritoneoscopy followed by a series of transcolonic procedures. The access from below gives a good, direct view of the upper abdominal cavity. Having that in mind, Lima et al[25] published the first transvesical endoscopic peritoneoscopy. And subsequently our group used a combination of transgastric and transvesical approaches to solve the problem of triangulation, and managed to do a series of cholecystectomies and nephrectomies in porcine models[26,27].
To accomplish NOTES procedures in the thorax, Sumiyama et al[28] proposed the transesophageal access. Transvesical-transdiaphragmatic thoracoscopy[29], transgastric-transdiaphragmatic thoracoscopy[30], and transtracheal thoracoscopy[31] have been suggested as well. Although the transesophageal method has been preferred as a direct entry to the thorax and posterior mediastinum, this permitted several simple thoracic procedures in porcine models[32-38].
Despite the enthusiasm for NOTES, there are still some hurdles to be overcome. The initial concern is the potential for intra-abdominal infection and spillage from the viscerotomy. Infection must first be prevented by using a clean access site. Most transgastric protocols also follow a 24 h liquid formula diet, intravenous antibiotics and stomach irrigation with sterile water and antibiotic solution. Despite these precautions, even a sterile overtube used to protect the endoscope from oral contamination becomes contaminated on oral insertion and can transport bacteria to both the stomach and the peritoneal cavity[2]. Surprisingly, Narula et al[39] reported no infections after gastrotomy in patients undergoing diagnostic transgastric peritoneoscopy without previous gastric decontamination. The authors considered that the same degree of contamination of the peritoneal cavity is expected as in any operation performed with an open viscus.
There is also some controversy about the need for endoscope sterilization. In a recent literature review, Spaun et al[40] concluded that, although difficult, it is possible to terminally sterilize flexible endoscopes. Steris System 1™ that uses 0.2% peracetic acid was the cheapest and fastest sterilization method and scored second in the risk of recontamination. Ethylene oxide gas sterilization has the lowest risk of recontamination, but is the slowest and most expensive method. The authors recommend sterile instrumentation for clinical NOTES until well-designed and randomized clinical trials are available and guidelines are published.
Concerning viscerotomy closure, gastrotomy has been the most studied and the methods under investigation could also be applied to the colon, esophagus or bladder, depending on the circumstances. Several methods have been proposed for stomach closure, including: conventional endoscopic clips, over-the-scope clip (OTSC) system, septal occluders, T-tags, T-bars for tissue opposing, as well as more complex suturing devices such as the Eagle Claw VII, NDO Plicator, USGI Endosurgical Operating System, and linear endoscopic staplers. Most of these devices still have limitations that need improving, but OTSC shows the most promising results[41]. More recently, the Padlock-G clip have been described as also showing promising results[42]. Colonic closure in animal studies has been performed using the same techniques and devices as those used for gastrotomy closure. Transanal endoscopic microsurgery has been used for a long time, and has been useful for colonic closure in hybrid NOTES procedures in humans[43]. For vesicotomy closure, Lima et al[44] recently reported the first successful endoscopic closure using a suturing kit (T-fasteners with a locking clinch). Easy and safe closure has been the main advantage for transvaginal route acceptance. Closure after transvaginal access is readily and routinely performed by using standard surgical techniques. Even if closure were to fail, there would be little, if any, clinical significance, because of the extremely low risk of infection or hernia.
Concerning adequate exposure and visualization, pneumoperitoneum is a key component. Air insufflated in an uncontrolled manner through the endoscope results in wide fluctuations in intraperitoneal pressures, overdistension of the abdomen, and adverse hemodynamic effects. Insufflated air can also leak around the endoscope resulting in bowel overdistension[2]. Many authors are now using a Veress needle to inject carbon dioxide and safely control its pressure inside the abdomen[45]. Despite this, new insufflators are being adapted to both deliver and monitor carbon dioxide through the endoscope[46]. There is a great debate whether CO2 or room air should be used. The effect of CO2 with respect to laparoscopy has suggested an overall attenuated inflammatory response that may provide a further immunologic benefit. The acidic environment created has been the main contributing factor believed to facilitate this physiologic result. Conversely, ‘‘room air’’ laparoscopy has been shown to generate a greater inflammatory response, but a recent case-control study did not find a significant difference between the peritoneal inflammatory response of NOTES vs laparoscopy with carbon dioxide and air pneumoperitoneum[47].
As previously stated, maintaining spatial orientation and triangulation of instruments is challenging when using a flexible endoscope. Moreover, flexible endoscopes are difficult to stabilize inside the abdominal cavity and can only pass flexible instruments which are too flaccid for retraction. This challenge can be overcome with adequate training, a combination of different routes, and with the constant development of new instruments. Transvaginal, transcolonic and transvesical routes allow the introduction of rigid equipment, and except in the transvesical route, the instruments can be used either through a rigid endoscope or in parallel with a flexible endoscope. Additionally, these access routes coming from the lower abdomen permit a good direct visualization of the upper abdomen. In some cases, one can use an additional transabdominal port. This has been named hybrid NOTES and has been seen as an intermediate step of great help in the training and development of NOTES[48]. Recently, magnets are being managed to provide the vigorous traction and countertraction required to advance NOTES procedures[49]. A new magnetic anchoring and guidance system allows concurrent use of multiple working instruments and control of an intra-abdominal camera. It has been used to perform transvaginal, single-port cholecystectomy[50]. Finally, one of the hurdles of NOTES is getting solid organs out of the thoracic and abdominal cavities. Excision of larger organs such as a kidney, or a gallbladder filled with stones through a small trocar orifice is a huge challenge. The transvaginal access has a big advantage in this matter and has been used for specimen retrieval in most NOTES procedures. On the other hand, transvaginal access is only an option in female patients.
In 2003, Rao and Reddy[51] performed the first NOTES procedure in humans. The authors carried out a transgastric appendectomy in a male patient presenting severe burn lesions in his abdominal wall using a conventional flexible endoscope with two working channels. Only in 2007, was there the first published human NOTES procedure. Marks et al[52] performed a transgastric rescue of a prematurely dislodge gastrostomy tube. The authors advanced a standard gastroscope through the previous gastrostomy, a performed peritoneoscopy, and suctioned away intra-abdominal free fluid. In that same year, another case reported the first human transvesical peritoneoscopy using a flexible ureteroscope during a standard laparoscopic robot-assisted prostatectomy[53].
The first natural orifice transluminal cholecystectomy in humans was performed in Strasbourg, France[54]. A 30-year-old woman with symptomatic cholelithiasis was submitted to cholecystectomy using a standard double-channel flexible gastroscope and standard endoscopic instruments. A 2-mm transabdominal needle port was used to insufflate carbon dioxide, to monitor the pneumoperitoneum, and to retract the gallbladder. Colpotomy was closed using conventional instruments. The patient had no post-operative pain and no scars, and was discharged on the second post-operative day. Shortly after that, the same technique was used by a team in Brazil, and by another in Italy[55,56].
In 2007, a group of investigators from Ohio, United States used transgastric peritoneoscopy after standard laparoscopy to diagnose pancreatic masses[57]. In 9 out of 10 patients, transgastric abdominal exploration corroborated the decision to proceed to open exploration made during traditional laparoscopic exploration. The average time of diagnostic laparoscopy was 12.3 min, compared to the 24.8 min taken for the transgastric route. Closure of the gastrotomy was obviated through its integration into the primary operation, whether that involved a resection with curative intent or palliation. No cross-contamination of the peritoneum or infectious complications was noted.
Other procedures using exclusively natural orifice transluminal procedures in humans have been performed - transgastric and transduodenal pancreatic necrosectomy[58], transvaginal incisional hernia repair[59], transvaginal liver, diaphragm, ovaries, and peritoneum biopsies[60], and transvaginal appendectomy[61]. This last one is especially important, as two of the three cases presented had an umbilical port inserted in order to complete appendectomy. As seen before in cholecystectomy, the use of a transabdominal port is essential to make natural orifice approaches feasible or at least easier at this time. Hybrid NOTES procedures are seen as a safe way to accomplish pure NOTES in the future. For this aim, hybrid procedures are developing in humans and achieving new goals like transvaginal nephrectomy[62], transrectal rectosigmoidectomy[63], sleeve gastrectomy[64], transvaginal liver resection[65], transvaginal splenectomy[66], transgastric cholecystectomy[67], transanal rectal cancer resection[43], intragastric stapled cystogastrostomy of a pancreatic pseudocyst[68], and adjustable gastric banding[69].
In 2009, de Sousa et al[70] published the first series of pure NOTES transvaginal cholecystectomies. The authors performed four cholecystectomies using two endoscopes introduced simultaneously in the abdominal cavity through a transvaginal incision. Dissection was accomplished with conventional endoscopic instruments. Ligation of the cystic duct and artery was performed using endoscopic clips. Vaginal closure was achieved using the direct-vision suture technique. More recently, Bessler et al[71] described a different technique for pure NOTES cholecystectomy in a 35-year-old-woman. Instead of using two endoscopes, the authors used an extra-long 5-mm articulating retractor placed into the abdomen via a separate colpotomy made under direct vision using the flexible endoscope in a retroflexed position. This method overcame the retracting limitations that obliged the use of a transabdominal port.
Despite all the enthusiasm around NOTES, other clinical advantages besides the absence of skin incision remain to be fully proven. Although most studies claim that greater operative time would be compensated by shorter hospital stays, prospective control studies are lacking[72]. Hensel et al[73] reported a retrospective case-control study where hybrid transvaginal cholecystectomy group showed a lower need for analgesics, faster mobilization, more comfortable recovery and a shorter hospital stay than the conventional laparoscopy group.
Finally, patients’ perspectives and expectations about NOTES are not yet fully understood. An interesting questionnaire-based study was derived to identify their preferences between different available surgical options upon a hypothetical scenario of an acute appendicitis[74]. Single port surgery (SPS) was the most popular method followed by conventional laparoscopy. Open surgery and NOTES were the least preferred. Choosing between SPS and NOTES only, 80.6% opted for SPS, 11.8% NOTES, and 5.6% declined surgery. The most popular route of access for NOTES was oral (37.7%). Another study asked women about their concerns and opinions regarding transvaginal surgery[75]. The majority of women (68%) indicated that they would want a transvaginal procedure in the future because of decreased risk of hernia and decreased operative pain (90% and 93%, respectively), while only 39% were concerned with the improved cosmesis of NOTES surgery. Of the women polled, nulliparous women and those under age 45 years were significantly more often concerned with how transvaginal surgery may affect healthy sexual life and fertility issues. Of the women who would not prefer transvaginal surgery, a significant number indicated concerns over infectious issues.
NOTES promises a new and innovative era of minimal access surgery based on traditional laparoscopic and endoscopic techniques. Researchers all over the world are investigating ways to improve NOTES procedures in order to make it easier and safer. With careful development of new equipment and techniques, NOTES may be a reasonable option to conventional laparoscopic procedures. It may even become the method of choice for selected surgical procedures in the future.
Peer reviewer: Akihito Nagahara, Associate Professor, Department of Gastroenterology, Juntendo University School of Medicine, 2-1-1 Hongo Bunkyo-ku, Tokyo 113-8421, Japan
S-editor Tian L L-editor Rutherford A E-editor Li JY
| 1. | Spaner SJ, Warnock GL. A brief history of endoscopy, laparoscopy, and laparoscopic surgery. J Laparoendosc Adv Surg Tech A. 1997;7:369-373. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 136] [Cited by in RCA: 115] [Article Influence: 4.1] [Reference Citation Analysis (0)] |
| 2. | Shafi BM, Mery CM, Binyamin G, Dutta S. Natural orifice translumenal endoscopic surgery (NOTES). Semin Pediatr Surg. 2006;15:251-258. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 14] [Cited by in RCA: 17] [Article Influence: 0.9] [Reference Citation Analysis (0)] |
| 3. | Rogers BH, Cicurel NJ, Seed RW. Transgastric needle aspiration of pancreatic pseudocyst through an endoscope. Gastrointest Endosc. 1975;21:133-134. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 57] [Cited by in RCA: 44] [Article Influence: 0.9] [Reference Citation Analysis (0)] |
| 4. | Gauderer MW, Ponsky JL, Izant RJ. Gastrostomy without laparotomy: a percutaneous endoscopic technique. J Pediatr Surg. 1980;15:872-875. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1408] [Cited by in RCA: 1299] [Article Influence: 28.9] [Reference Citation Analysis (1)] |
| 5. | Kalloo AN, Singh VK, Jagannath SB, Niiyama H, Hill SL, Vaughn CA, Magee CA, Kantsevoy SV. Flexible transgastric peritoneoscopy: a novel approach to diagnostic and therapeutic interventions in the peritoneal cavity. Gastrointest Endosc. 2004;60:114-117. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1037] [Cited by in RCA: 904] [Article Influence: 43.0] [Reference Citation Analysis (0)] |
| 6. | Rattner D, Kalloo A. ASGE/SAGES Working Group on Natural Orifice Translumenal Endoscopic Surgery. October 2005. Surg Endosc. 2006;20:329-333. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 619] [Cited by in RCA: 530] [Article Influence: 27.9] [Reference Citation Analysis (0)] |
| 7. | Bessler M, Stevens PD, Milone L, Parikh M, Fowler D. Transvaginal laparoscopically assisted endoscopic cholecystectomy: a hybrid approach to natural orifice surgery. Gastrointest Endosc. 2007;66:1243-1245. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 205] [Cited by in RCA: 176] [Article Influence: 9.8] [Reference Citation Analysis (0)] |
| 8. | Halim I, Tavakkolizadeh A. NOTES: The next surgical revolution? Int J Surg. 2008;6:273-276. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 23] [Cited by in RCA: 25] [Article Influence: 1.4] [Reference Citation Analysis (0)] |
| 9. | Gettman MT, Lotan Y, Napper CA, Cadeddu JA. Transvaginal laparoscopic nephrectomy: development and feasibility in the porcine model. Urology. 2002;59:446-450. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 1] [Reference Citation Analysis (0)] |
| 10. | Kantsevoy SV, Hu B, Jagannath SB, Vaughn CA, Beitler DM, Chung SS, Cotton PB, Gostout CJ, Hawes RH, Pasricha PJ. Transgastric endoscopic splenectomy: is it possible? Surg Endosc. 2006;20:522-525. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 236] [Cited by in RCA: 232] [Article Influence: 12.2] [Reference Citation Analysis (0)] |
| 11. | Jagannath SB, Kantsevoy SV, Vaughn CA, Chung SS, Cotton PB, Gostout CJ, Hawes RH, Pasricha PJ, Scorpio DG, Magee CA. Peroral transgastric endoscopic ligation of fallopian tubes with long-term survival in a porcine model. Gastrointest Endosc. 2005;61:449-453. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 298] [Cited by in RCA: 278] [Article Influence: 13.9] [Reference Citation Analysis (0)] |
| 12. | Wagh MS, Merrifield BF, Thompson CC. Endoscopic transgastric abdominal exploration and organ resection: initial experience in a porcine model. Clin Gastroenterol Hepatol. 2005;3:892-896. [PubMed] |
| 13. | Merrifield BF, Wagh MS, Thompson CC. Peroral transgastric organ resection: a feasibility study in pigs. Gastrointest Endosc. 2006;63:693-697. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 177] [Cited by in RCA: 170] [Article Influence: 8.9] [Reference Citation Analysis (0)] |
| 14. | Wagh MS, Merrifield BF, Thompson CC. Survival studies after endoscopic transgastric oophorectomy and tubectomy in a porcine model. Gastrointest Endosc. 2006;63:473-478. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 196] [Cited by in RCA: 193] [Article Influence: 10.2] [Reference Citation Analysis (0)] |
| 15. | Kantsevoy SV, Jagannath SB, Niiyama H, Chung SS, Cotton PB, Gostout CJ, Hawes RH, Pasricha PJ, Magee CA, Vaughn CA. Endoscopic gastrojejunostomy with survival in a porcine model. Gastrointest Endosc. 2005;62:287-292. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 312] [Cited by in RCA: 291] [Article Influence: 14.6] [Reference Citation Analysis (0)] |
| 16. | Fritscher-Ravens A, Mosse CA, Ikeda K, Swain P. Endoscopic transgastric lymphadenectomy by using EUS for selection and guidance. Gastrointest Endosc. 2006;63:302-306. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 93] [Cited by in RCA: 80] [Article Influence: 4.2] [Reference Citation Analysis (0)] |
| 17. | Matthes K, Yusuf TE, Willingham FF, Mino-Kenudson M, Rattner DW, Brugge WR. Feasibility of endoscopic transgastric distal pancreatectomy in a porcine animal model. Gastrointest Endosc. 2007;66:762-766. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 34] [Cited by in RCA: 37] [Article Influence: 2.1] [Reference Citation Analysis (0)] |
| 18. | Sumiyama K, Gostout CJ, Rajan E, Bakken TA, Deters JL, Knipschield MA, Hawes RH, Kalloo AN, Pasricha PJ, Chung S. Pilot study of the porcine uterine horn as an in vivo appendicitis model for development of endoscopic transgastric appendectomy. Gastrointest Endosc. 2006;64:808-812. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 63] [Cited by in RCA: 55] [Article Influence: 2.9] [Reference Citation Analysis (0)] |
| 19. | Hu B, Kalloo AN, Chung SS, Cotton PB, Gostout CJ, Hawes RH, Pasricha PJ, Isakovich NV, Nakajima Y, Kawashima K. Peroral transgastric endoscopic primary repair of a ventral hernia in a porcine model. Endoscopy. 2007;39:390-393. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 37] [Cited by in RCA: 30] [Article Influence: 1.7] [Reference Citation Analysis (0)] |
| 20. | Onders R, McGee MF, Marks J, Chak A, Schilz R, Rosen MJ, Ignagni A, Faulx A, Elmo MJ, Schomisch S. Diaphragm pacing with natural orifice transluminal endoscopic surgery: potential for difficult-to-wean intensive care unit patients. Surg Endosc. 2007;21:475-479. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 56] [Cited by in RCA: 54] [Article Influence: 2.8] [Reference Citation Analysis (0)] |
| 21. | Park PO, Bergström M, Ikeda K, Fritscher-Ravens A, Swain P. Experimental studies of transgastric gallbladder surgery: cholecystectomy and cholecystogastric anastomosis (videos). Gastrointest Endosc. 2005;61:601-606. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 343] [Cited by in RCA: 314] [Article Influence: 15.7] [Reference Citation Analysis (0)] |
| 22. | Fong DG, Pai RD, Thompson CC. Transcolonic endoscopic abdominal exploration: a NOTES survival study in a porcine model. Gastrointest Endosc. 2007;65:312-318. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 151] [Cited by in RCA: 135] [Article Influence: 7.5] [Reference Citation Analysis (0)] |
| 23. | Pai RD, Fong DG, Bundga ME, Odze RD, Rattner DW, Thompson CC. Transcolonic endoscopic cholecystectomy: a NOTES survival study in a porcine model (with video). Gastrointest Endosc. 2006;64:428-434. [PubMed] [DOI] [Full Text] |
| 24. | Fong DG, Pai RD, Thompson CC. Transcolonic hepatic wedge resection in a porcine model [abstract]. Gastrointest Endosc. 2006;63:AB10. [DOI] [Full Text] |
| 25. | Lima E, Rolanda C, Pêgo JM, Henriques-Coelho T, Silva D, Carvalho JL, Correia-Pinto J. Transvesical endoscopic peritoneoscopy: a novel 5 mm port for intra-abdominal scarless surgery. J Urol. 2006;176:802-805. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 139] [Cited by in RCA: 117] [Article Influence: 6.2] [Reference Citation Analysis (0)] |
| 26. | Rolanda C, Lima E, Pêgo JM, Henriques-Coelho T, Silva D, Moreira I, Macedo G, Carvalho JL, Correia-Pinto J. Third-generation cholecystectomy by natural orifices: transgastric and transvesical combined approach (with video). Gastrointest Endosc. 2007;65:111-117. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 144] [Cited by in RCA: 125] [Article Influence: 6.9] [Reference Citation Analysis (0)] |
| 27. | Lima E, Rolanda C, Pêgo JM, Henriques-Coelho T, Silva D, Osório L, Moreira I, Carvalho JL, Correia-Pinto J. Third-generation nephrectomy by natural orifice transluminal endoscopic surgery. J Urol. 2007;178:2648-2654. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 105] [Cited by in RCA: 84] [Article Influence: 4.7] [Reference Citation Analysis (0)] |
| 28. | Sumiyama K, Gostout CJ, Rajan E, Bakken TA, Knipschield MA. Transesophageal mediastinoscopy by submucosal endoscopy with mucosal flap safety valve technique. Gastrointest Endosc. 2007;65:679-683. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 124] [Cited by in RCA: 115] [Article Influence: 6.4] [Reference Citation Analysis (0)] |
| 29. | Lima E, Henriques-Coelho T, Rolanda C, Pêgo JM, Silva D, Carvalho JL, Correia-Pinto J. Transvesical thoracoscopy: a natural orifice translumenal endoscopic approach for thoracic surgery. Surg Endosc. 2007;21:854-858. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 89] [Cited by in RCA: 76] [Article Influence: 4.2] [Reference Citation Analysis (0)] |
| 30. | De Palma GD, Siciliano S, Addeo P, Salvatori F, Persico M, Masone S, Rega M, Maione F, Coppola Bottazzi E, Serrao E. A NOTES approach for thoracic surgery: transgastric thoracoscopy via a diaphragmatic incision in a survival porcine model. Minerva Chir. 2010;65:11-15. [PubMed] |
| 31. | Yang C, Liu HP, Chu Y, Liu YH, Wu CY, Ko PJ, Liu HP. Video. Natural orifice transtracheal evaluation of the thoracic cavity and mediastinum. Surg Endosc. 2010;24:2905-2907. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 9] [Cited by in RCA: 10] [Article Influence: 0.7] [Reference Citation Analysis (0)] |
| 32. | Willingham FF, Gee DW, Lauwers GY, Brugge WR, Rattner DW. Natural orifice transesophageal mediastinoscopy and thoracoscopy. Surg Endosc. 2008;22:1042-1047. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 49] [Cited by in RCA: 45] [Article Influence: 2.5] [Reference Citation Analysis (0)] |
| 33. | Fritscher-Ravens A, Patel K, Ghanbari A, Kahle E, von Herbay A, Fritscher T, Niemann H, Koehler P. Natural orifice transluminal endoscopic surgery (NOTES) in the mediastinum: long-term survival animal experiments in transesophageal access, including minor surgical procedures. Endoscopy. 2007;39:870-875. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 77] [Cited by in RCA: 65] [Article Influence: 3.6] [Reference Citation Analysis (0)] |
| 34. | Gee DW, Willingham FF, Lauwers GY, Brugge WR, Rattner DW. Natural orifice transesophageal mediastinoscopy and thoracoscopy: a survival series in swine. Surg Endosc. 2008;22:2117-2122. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 48] [Cited by in RCA: 46] [Article Influence: 2.7] [Reference Citation Analysis (0)] |
| 35. | Woodward T, McCluskey D, Wallace MB, Raimondo M, Mannone J, Smith CD. Pilot study of transesophageal endoscopic surgery: NOTES esophagomyotomy, vagotomy, lymphadenectomy. J Laparoendosc Adv Surg Tech A. 2008;18:743-745. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 28] [Cited by in RCA: 24] [Article Influence: 1.5] [Reference Citation Analysis (0)] |
| 36. | Pauli EM, Mathew A, Haluck RS, Ionescu AM, Moyer MT, Shope TR, Rogers AM. Technique for transesophageal endoscopic cardiomyotomy (Heller myotomy): video presentation at the Society of American Gastrointestinal and Endoscopic Surgeons (SAGES) 2008, Philadelphia, PA. Surg Endosc. 2008;22:2279-2280. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 20] [Cited by in RCA: 23] [Article Influence: 1.4] [Reference Citation Analysis (0)] |
| 37. | Fritscher-Ravens A, Cuming T, Jacobsen B, Seehusen F, Ghanbari A, Kahle E, von Herbay A, Koehler P, Milla P. Feasibility and safety of endoscopic full-thickness esophageal wall resection and defect closure: a prospective long-term survival animal study. Gastrointest Endosc. 2009;69:1314-1320. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 27] [Cited by in RCA: 28] [Article Influence: 1.8] [Reference Citation Analysis (0)] |
| 38. | Turner BG, Gee DW, Cizginer S, Konuk Y, Karaca C, Willingham F, Mino-Kenudson M, Morse C, Rattner DW, Brugge WR. Feasibility of endoscopic transesophageal thoracic sympathectomy (with video). Gastrointest Endosc. 2010;71:171-175. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 15] [Cited by in RCA: 16] [Article Influence: 1.1] [Reference Citation Analysis (0)] |
| 39. | Narula VK, Hazey JW, Renton DB, Reavis KM, Paul CM, Hinshaw KE, Needleman BJ, Mikami DJ, Ellison EC, Melvin WS. Transgastric instrumentation and bacterial contamination of the peritoneal cavity. Surg Endosc. 2008;22:605-611. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 67] [Cited by in RCA: 73] [Article Influence: 4.1] [Reference Citation Analysis (0)] |
| 40. | Spaun GO, Goers TA, Pierce RA, Cassera MA, Scovil S, Swanstrom LL. Use of flexible endoscopes for NOTES: sterilization or high-level disinfection? Surg Endosc. 2010;24:1581-1588. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 14] [Cited by in RCA: 13] [Article Influence: 0.8] [Reference Citation Analysis (0)] |
| 41. | Rolanda C, Lima E, Silva D, Moreira I, Pêgo JM, Macedo G, Correia-Pinto J. In vivo assessment of gastrotomy closure with over-the-scope clips in an experimental model for varicocelectomy (with video). Gastrointest Endosc. 2009;70:1137-1145. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 17] [Cited by in RCA: 18] [Article Influence: 1.1] [Reference Citation Analysis (0)] |
| 42. | Romanelli JR, Desilets DJ, Earle DB. Natural orifice transluminal endoscopic surgery gastrotomy closure in porcine explants with the Padlock-G clip using the Lock-It system. Endoscopy. 2010;42:306-310. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 15] [Cited by in RCA: 18] [Article Influence: 1.2] [Reference Citation Analysis (0)] |
| 43. | Sylla P, Rattner DW, Delgado S, Lacy AM. NOTES transanal rectal cancer resection using transanal endoscopic microsurgery and laparoscopic assistance. Surg Endosc. 2010;24:1205-1210. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 507] [Cited by in RCA: 534] [Article Influence: 35.6] [Reference Citation Analysis (0)] |
| 44. | Lima E, Rolanda C, Osório L, Pêgo JM, Silva D, Henriques-Coelho T, Carvalho JL, Bergström M, Park PO, Mosse CA. Endoscopic closure of transmural bladder wall perforations. Eur Urol. 2009;56:151-157. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 33] [Cited by in RCA: 35] [Article Influence: 2.1] [Reference Citation Analysis (0)] |
| 45. | Ko CW, Shin EJ, Buscaglia JM, Clarke JO, Magno P, Giday SA, Chung SS, Cotton PB, Gostout CJ, Hawes RH. Preliminary pneumoperitoneum facilitates transgastric access into the peritoneal cavity for natural orifice transluminal endoscopic surgery: a pilot study in a live porcine model. Endoscopy. 2007;39:849-853. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 28] [Cited by in RCA: 24] [Article Influence: 1.3] [Reference Citation Analysis (0)] |
| 46. | Bergström M, Swain P, Park PO. Measurements of intraperitoneal pressure and the development of a feedback control valve for regulating pressure during flexible transgastric surgery (NOTES). Gastrointest Endosc. 2007;66:174-178. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 39] [Cited by in RCA: 40] [Article Influence: 2.2] [Reference Citation Analysis (0)] |
| 47. | Trunzo JA, McGee MF, Cavazzola LT, Schomisch S, Nikfarjam M, Bailey J, Mishra T, Poulose BK, Lee YJ, Ponsky JL. Peritoneal inflammatory response of natural orifice translumenal endoscopic surgery (NOTES) versus laparoscopy with carbon dioxide and air pneumoperitoneum. Surg Endosc. 2010;24:1727-1736. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 27] [Cited by in RCA: 25] [Article Influence: 1.7] [Reference Citation Analysis (0)] |
| 48. | Shih SP, Kantsevoy SV, Kalloo AN, Magno P, Giday SA, Ko CW, Isakovich NV, Meireles O, Hanly EJ, Marohn MR. Hybrid minimally invasive surgery--a bridge between laparoscopic and translumenal surgery. Surg Endosc. 2007;21:1450-1453. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 43] [Cited by in RCA: 47] [Article Influence: 2.6] [Reference Citation Analysis (0)] |
| 49. | Ryou M, Thompson CC. Magnetic retraction in natural-orifice transluminal endoscopic surgery (NOTES): addressing the problem of traction and countertraction. Endoscopy. 2009;41:143-148. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 33] [Cited by in RCA: 32] [Article Influence: 2.0] [Reference Citation Analysis (0)] |
| 50. | Scott DJ, Tang SJ, Fernandez R, Bergs R, Goova MT, Zeltser I, Kehdy FJ, Cadeddu JA. Completely transvaginal NOTES cholecystectomy using magnetically anchored instruments. Surg Endosc. 2007;21:2308-2316. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 162] [Cited by in RCA: 142] [Article Influence: 7.9] [Reference Citation Analysis (0)] |
| 51. | Rao GV, Reddy DN. Transgastric appendectomy in humans. Montreal: World Congress of Gastroenterology 2006; . |
| 52. | Marks JM, Ponsky JL, Pearl JP, McGee MF. PEG "Rescue": a practical NOTES technique. Surg Endosc. 2007;21:816-819. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 97] [Cited by in RCA: 78] [Article Influence: 4.3] [Reference Citation Analysis (0)] |
| 53. | Gettman MT, Blute ML. Transvesical peritoneoscopy: initial clinical evaluation of the bladder as a portal for natural orifice translumenal endoscopic surgery. Mayo Clin Proc. 2007;82:843-845. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 93] [Cited by in RCA: 79] [Article Influence: 4.4] [Reference Citation Analysis (0)] |
| 54. | Marescaux J, Dallemagne B, Perretta S, Wattiez A, Mutter D, Coumaros D. Surgery without scars: report of transluminal cholecystectomy in a human being. Arch Surg. 2007;142:823-86; discussion 823-86. [PubMed] |
| 55. | Zorron R, Maggioni LC, Pombo L, Oliveira AL, Carvalho GL, Filgueiras M. NOTES transvaginal cholecystectomy: preliminary clinical application. Surg Endosc. 2008;22:542-547. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 185] [Cited by in RCA: 169] [Article Influence: 9.4] [Reference Citation Analysis (0)] |
| 56. | Forgione A, Maggioni D, Sansonna F, Ferrari C, Di Lernia S, Citterio D, Magistro C, Frigerio L, Pugliese R. Transvaginal endoscopic cholecystectomy in human beings: preliminary results. J Laparoendosc Adv Surg Tech A. 2008;18:345-351. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 72] [Cited by in RCA: 68] [Article Influence: 4.0] [Reference Citation Analysis (0)] |
| 57. | Hazey JW, Narula VK, Renton DB, Reavis KM, Paul CM, Hinshaw KE, Muscarella P, Ellison EC, Melvin WS. Natural-orifice transgastric endoscopic peritoneoscopy in humans: Initial clinical trial. Surg Endosc. 2008;22:16-20. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 174] [Cited by in RCA: 158] [Article Influence: 8.8] [Reference Citation Analysis (0)] |
| 58. | Escourrou J, Shehab H, Buscail L, Bournet B, Andrau P, Moreau J, Fourtanier G. Peroral transgastric/transduodenal necrosectomy: success in the treatment of infected pancreatic necrosis. Ann Surg. 2008;248:1074-1080. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 82] [Cited by in RCA: 76] [Article Influence: 4.5] [Reference Citation Analysis (0)] |
| 59. | Jacobsen GR, Thompson K, Spivack A, Fischer L, Wong B, Cullen J, Bosia J, Whitcomb E, Lucas E, Talamini M. Initial experience with transvaginal incisional hernia repair. Hernia. 2010;14:89-91. [PubMed] |
| 60. | Zorrón R, Soldan M, Filgueiras M, Maggioni LC, Pombo L, Oliveira AL. NOTES: transvaginal for cancer diagnostic staging: preliminary clinical application. Surg Innov. 2008;15:161-165. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 35] [Cited by in RCA: 35] [Article Influence: 2.1] [Reference Citation Analysis (0)] |
| 61. | Palanivelu C, Rajan PS, Rangarajan M, Parthasarathi R, Senthilnathan P, Prasad M. Transvaginal endoscopic appendectomy in humans: a unique approach to NOTES--world's first report. Surg Endosc. 2008;22:1343-1347. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 150] [Cited by in RCA: 136] [Article Influence: 8.0] [Reference Citation Analysis (0)] |
| 62. | Kaouk JH, White WM, Goel RK, Brethauer S, Crouzet S, Rackley RR, Moore C, Ingber MS, Haber GP. NOTES transvaginal nephrectomy: first human experience. Urology. 2009;74:5-8. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 86] [Cited by in RCA: 94] [Article Influence: 5.9] [Reference Citation Analysis (0)] |
| 63. | Sylla P, Willingham FF, Sohn DK, Gee D, Brugge WR, Rattner DW. NOTES rectosigmoid resection using transanal endoscopic microsurgery (TEM) with transgastric endoscopic assistance: a pilot study in swine. J Gastrointest Surg. 2008;12:1717-1723. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 94] [Cited by in RCA: 89] [Article Influence: 5.2] [Reference Citation Analysis (0)] |
| 64. | Ramos AC, Zundel N, Neto MG, Maalouf M. Human hybrid NOTES transvaginal sleeve gastrectomy: initial experience. Surg Obes Relat Dis. 2008;4:660-663. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 71] [Cited by in RCA: 111] [Article Influence: 6.5] [Reference Citation Analysis (0)] |
| 65. | Noguera JF, Dolz C, Cuadrado A, Olea JM, Vilella A. Transvaginal liver resection (NOTES) combined with minilaparoscopy. Rev Esp Enferm Dig. 2008;100:411-415. [PubMed] |
| 66. | Targarona EM, Gomez C, Rovira R, Pernas JC, Balague C, Guarner-Argente C, Sainz S, Trias M. NOTES-assisted transvaginal splenectomy: the next step in the minimally invasive approach to the spleen. Surg Innov. 2009;16:218-222. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 37] [Cited by in RCA: 45] [Article Influence: 2.8] [Reference Citation Analysis (0)] |
| 67. | Auyang ED, Hungness ES, Vaziri K, Martin JA, Soper NJ. Human NOTES cholecystectomy: transgastric hybrid technique. J Gastrointest Surg. 2009;13:1149-1150. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 61] [Cited by in RCA: 57] [Article Influence: 3.6] [Reference Citation Analysis (0)] |
| 68. | Rossini CJ, Moriarty KP, Angelides AG. Hybrid notes: incisionless intragastric stapled cystgastrostomy of a pancreatic pseudocyst. J Pediatr Surg. 2010;45:80-83. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 6] [Cited by in RCA: 9] [Article Influence: 0.6] [Reference Citation Analysis (0)] |
| 69. | Michalik M, Orlowski M, Bobowicz M, Frask A, Trybull A. The first report on hybrid NOTES adjustable gastric banding in human. Obes Surg. 2011;21:524-527. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 11] [Cited by in RCA: 15] [Article Influence: 1.1] [Reference Citation Analysis (0)] |
| 70. | de Sousa LH, de Sousa JA, de Sousa Filho LH, de Sousa MM, de Sousa VM, de Sousa AP, Zorron R. Totally NOTES (T-NOTES) transvaginal cholecystectomy using two endoscopes: preliminary report. Surg Endosc. 2009;23:2550-2555. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 44] [Cited by in RCA: 43] [Article Influence: 2.7] [Reference Citation Analysis (0)] |
| 71. | Bessler M, Gumbs AA, Milone L, Evanko JC, Stevens P, Fowler D. Video. Pure natural orifice transluminal endoscopic surgery (NOTES) cholecystectomy. Surg Endosc. 2010;24:2316-2317. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 18] [Cited by in RCA: 21] [Article Influence: 1.4] [Reference Citation Analysis (0)] |
| 72. | Cuadrado-Garcia A, Noguera JF, Olea-Martinez JM, Morales R, Dolz C, Lozano L, Vicens JC, Pujol JJ. Hybrid natural orifice transluminal endoscopic cholecystectomy: prospective human series. Surg Endosc. 2011;25:19-22. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 25] [Cited by in RCA: 24] [Article Influence: 1.6] [Reference Citation Analysis (0)] |
| 73. | Hensel M, Schernikau U, Schmidt A, Arlt G. Comparison between Transvaginal and Laparoscopic Cholecystectomy - A Retrospective Case-Control Study. Zentralbl Chir. 2010;[Epub ahead of print]. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 1] [Reference Citation Analysis (0)] |
| 74. | Rao A, Kynaston J, MacDonald ER, Ahmed I. Patient preferences for surgical techniques: should we invest in new approaches? Surg Endosc. 2010;24:3016-3025. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 43] [Cited by in RCA: 49] [Article Influence: 3.3] [Reference Citation Analysis (0)] |
| 75. | Peterson CY, Ramamoorthy S, Andrews B, Horgan S, Talamini M, Chock A. Women's positive perception of transvaginal NOTES surgery. Surg Endosc. 2009;23:1770-1774. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 72] [Cited by in RCA: 76] [Article Influence: 4.5] [Reference Citation Analysis (0)] |