Published online Oct 28, 2009. doi: 10.3748/wjg.15.5112
Revised: September 7, 2009
Accepted: September 14, 2009
Published online: October 28, 2009
A previous study has shown that liver or combined liver-kidney transplantation can be a valuable surgical technique for the treatment of polycystic liver disease. Herein, we present the case of a 35-year-old woman with polycystic liver disease, who underwent orthotopic liver transplantation (OLT) on November 11, 2008. The whole-size graft was taken from a deceased donor (a 51-year-old man who died of a heart attack). Resection in a patient with massive hepatomegaly is very difficult. Thus, after intercepting the portal hepatic vein, left hepatectomy was performed, then the vena cava was intercepted, the second and third porta hepatic isolated, and finally, right hepatectomy was performed. OLT was performed successfully. The recipient did well after transplantation. This case suggested that OLT is an effective therapeutic option for polycystic liver disease and left hepatectomy can be performed first during OLT if the liver is over enlarged.
- Citation: Jiang WW, Zhang F, Pu LY, Wang XH, Kong LB. Liver transplantation for polycystic liver with massive hepatomegaly: A case report. World J Gastroenterol 2009; 15(40): 5112-5113
- URL: https://www.wjgnet.com/1007-9327/full/v15/i40/5112.htm
- DOI: https://dx.doi.org/10.3748/wjg.15.5112
A previous study has shown that liver or combined liver-kidney transplantation can be a valuable surgical technique for the treatment of polycystic liver disease[1]. Here, we present the case of a 35-year-old woman with polycystic liver disease, who underwent orthotopic liver transplantation (OLT) on November 11, 2008.
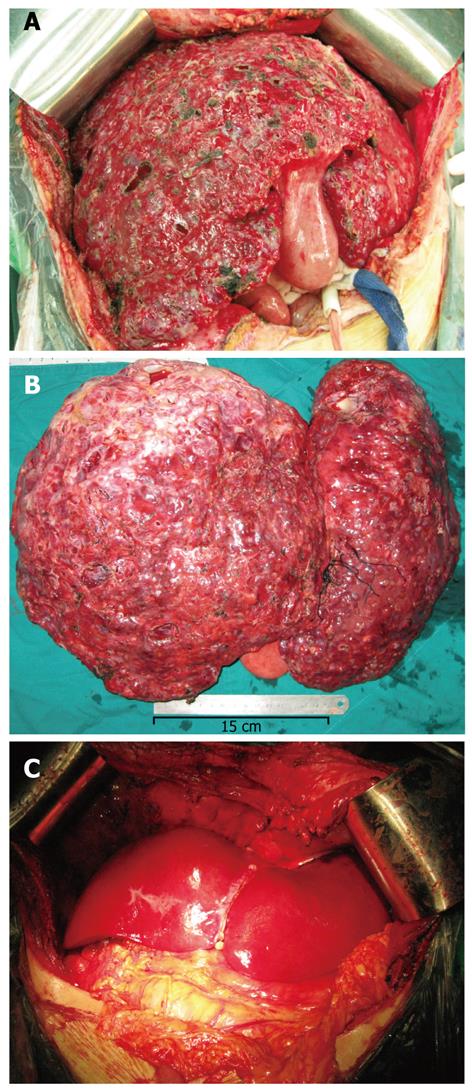
In October 2008, a 35-year-old woman with a body weight of 52 kg was admitted to the Liver Transplantation Center, the First Affiliated Hospital of Nanjing Medical University to undergo liver transplantation. This patient had a significant family history of polycystic disease, and her mother had died of dyscrasia that resulted from polycystic liver and kidney diseases. She had normal liver function [alanine aminotransferase (ALT) 35.7 U/L, aspartate aminotransferase (AST) 21.7 U/L, total bilirubin 16.5 μmol/L, and prothrombin time 13.8 s], and normal renal function (urea 4.33 mmol/L, creatinine 77 μmol/L, glomerular filtration rate 62.4 mL/min), but had dyspnea, anorexia, abdominal pain, hypertension, increased abdominal girth, mild ascites, and a liver span of 20 cm below the left costal margin and 25 cm below the right costal margin before transplantation. OLT was performed on November 11, 2008, and the whole-size graft was taken from a 51-year-old man who had died of a heart attack. The blood phenotypes of the donor and recipient were type A, RH (+). OLT was performed, but resection of the massive hepatomegaly was very difficult, because the enlarged polycystic liver occupied nearly the whole epigastric zone and mid abdomen (Figure 1A), which resulted in a small surgical space, especially for manipulation of hepatic blood vessels behind the liver. Thus, after intercepting the portal vein and vena cava, left hepatectomy was performed, followed by isolation of the hepatic veins and short hepatic veins at the posterior of the liver, and finally, right hepatectomy. OLT was then performed successfully (Figure 1C). The excised liver weighed 10.2 kg (approximate 20% of the body weight), which contained innumerable cysts and a large amount of cystic fluid (Figure 1B). The recipient did well after transplantation, and the hospitalization period was 21 d.
Polycystic liver disease is a rare, benign disorder[2]. Symptoms of polycystic liver disease are related mainly to the size of the liver. Patients with massive hepatomegaly may suffer from abdominal pain, vena caval obstruction, hypertension, hemorrhage, cyst infections, dyspnea, increased abdominal girth, and poor quality of life[3-6]. Cyst fenestration can be used to ameliorate the symptoms of massive hepatomegaly, but symptom relief is only temporary. Previous studies have shown that cyst aspiration, liver or combined liver-kidney transplantation may be a valuable surgical technique for the treatment of polycystic liver disease[1,7]. The first patient to undergo liver transplantation for polycystic liver-kidney disease was in 1988, however, the patient died intraoperatively from intractable bleeding[1].
In the present case, resection of massive hepatomegaly was very difficult, because the enlarged polycystic liver occupied nearly the whole epigastric zone and mid abdomen, therefore, the surgical space was very small, especially for manipulation of the hepatic veins and short hepatic veins at the posterior of the liver. During transplantation, cyst fenestration was used, but the volume of the liver could not be reduced significantly. Thus, after intercepting the portal vein and the vena cava, left hepatectomy was performed, followed by isolation of the hepatic veins and short hepatic veins, and finally, right hepatectomy. OLT was performed successfully. Left liver resection may be an effective treatment of choice, if the space is too small for manipulation of liver blood vessels behind the liver.
Peer reviewer: Dr. Shoji Kubo, Department of Hepato-Billiary-Pancreatic Surgery, Osaka City University Graduate School of Medicine, Osaka, 545-8585, Japan
S- Editor Cheng JX L- Editor Webster JR E- Editor Lin YP
| 1. | Kwok MK, Lewin KJ. Massive hepatomegaly in adult polycystic liver disease. Am J Surg Pathol. 1988;12:321-324. |
| 2. | Ramos A, Torres VE, Holley KE, Offord KP, Rakela J, Ludwig J. The liver in autosomal dominant polycystic kidney disease. Implications for pathogenesis. Arch Pathol Lab Med. 1990;114:180-184. |
| 3. | Jeyarajah DR, Gonwa TA, Testa G, Abbasoglu O, Goldstein R, Husberg BS, Levy MF, Klintmalm GB. Liver and kidney transplantation for polycystic disease. Transplantation. 1998;66:529-532. |
| 4. | Kornasiewicz O, Dudek K, Bugajski M, Najnigier B, Krawczyk M. Choice of transplantation techniques and indications for liver transplantation in polycystic liver disease in patients with no signs of end-stage liver disease. Transplant Proc. 2008;40:1536-1538. |
| 5. | Rossi M, Spoletini G, Bussotti A, Lai Q, Travaglia D, Ferretti S, Poli L, Ginanni Corradini S, Merli M, Novelli G. Combined liver-kidney transplantation in polycystic disease: case reports. Transplant Proc. 2008;40:2075-2076. |
| 6. | Kirchner GI, Rifai K, Cantz T, Nashan B, Terkamp C, Becker T, Strassburg C, Barg-Hock H, Wagner S, Lück R. Outcome and quality of life in patients with polycystic liver disease after liver or combined liver-kidney transplantation. Liver Transpl. 2006;12:1268-1277. |
| 7. | Russell RT, Pinson CW. Surgical management of polycystic liver disease. World J Gastroenterol. 2007;13:5052-5059. |