Published online Jan 28, 2008. doi: 10.3748/wjg.14.636
Revised: November 14, 2007
Published online: January 28, 2008
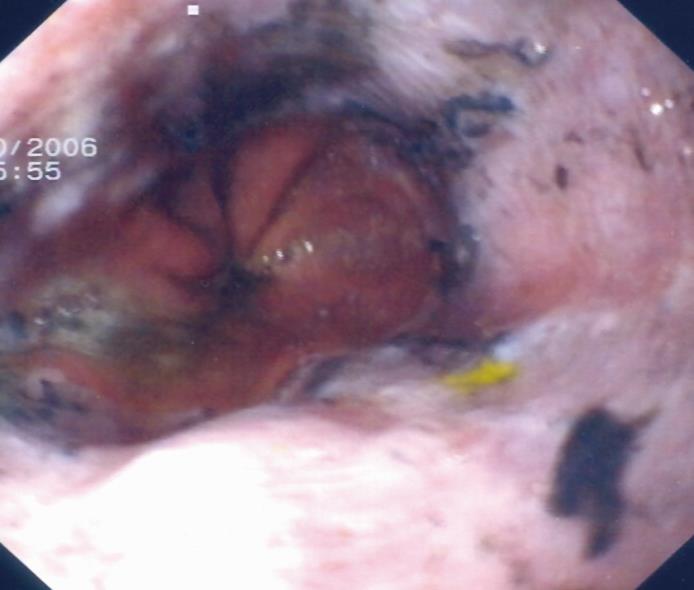
We present an unusual case of corrosive esophageal injury following liquid glue ingestion. The endoscopic findings were tissue sloughing and blackened appearance of the esophagogastric junction, due to caustic esophageal injuries following ingestion of glue containing toluene.
- Citation: Pace F, Greco S, Pallotta S, Bossi D, Trabucchi E, Porro GB. An uncommon cause of corrosive esophageal injury. World J Gastroenterol 2008; 14(4): 636-637
- URL: https://www.wjgnet.com/1007-9327/full/v14/i4/636.htm
- DOI: https://dx.doi.org/10.3748/wjg.14.636
Toluene is an aromatic hydrocarbon commonly used as an industrial solvent for the manufacturing of paints, chemicals, pharmaceuticals and rubber. It is commonly found as a glue in the household. It can be swallowed accidentally, can create a burning sensation, and cause gastrointestinal symptoms such as abdominal pain, nausea, vomiting and hematemesis. Their effect on the mouth, pharynx, larynx, esophagus and the rest of gastrointestinal system is unknown. However, no cases have been reported so far in English-language literature.
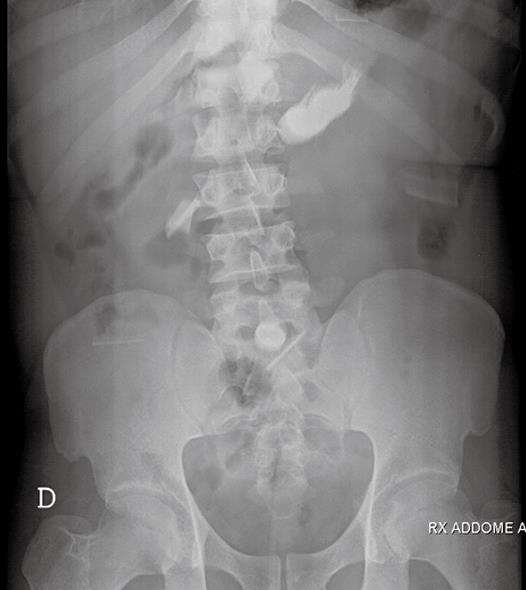
A 37-year-old man was brought to the surgical emergency department of our institution, reporting that he had been threatened by unknown persons 6 h earlier and forced to ingest liquid household glue (containing toluene) mixed with numerous coins and pins. The patient’s main complaints were vague: epigastric pain, nausea and vomiting. He was hemodynamically stable, but uncooperative. He did not smoke, nor was he an alcoholic or a drug addict. There were no signs of trauma or burns on the head and neck, except for a slight excoriation on the neck consistent with attempted strangulation, which proved to be self-inflicted. Chest and abdominal physical examinations were normal, except for moderate tenderness in the upper abdomen, without guarding. Laboratory tests were normal. Plain abdominal radiography revealed multiple sharp opacities in the stomach; in addition to these, an image of some pins was detected in a region consistent with the right lower quadrant (Figure 1). We performed upper gastrointestinal (GI) flexible endoscopy (Figure 2). The endoscopic findings were tissue sloughing and blackened appearance of the esophagogastric junction, due to caustic esophageal injuries, following liquid glue ingestion. An attempt was made to remove the foreign body endoscopically, but without success. The patient was scheduled for emergency surgical exploration.
Halogenated hydrocarbons, such as the solvent trichloroethane and methylene chloride, are known to produce hepatic and renal toxicity following chronic exposure, as well as central nervous system (CNS) effects with acute exposure[1], but corrosive GI injury has been never reported up to now. Endoscopic investigation furthermore showed metal pins and coins in the stomach. When approaching intestinal foreign body cases, location of the foreign body is of great importance in terms of management. The choice between outpatient treatment and surgical intervention will depend upon the localization and shape of the object. Although sharp objects pass through the gastrointestinal tract without difficulty in 90% of the cases, they may also be removed using fiberoptic gastroscopy without waiting. Early endoscopy is recommended in cases with objects wider than 2 cm and longer than 6 cm, since their passage through the pylorus and duodenum might become difficult. Sharp and pointed foreign bodies, as well as elongated foreign bodies, can be very challenging and difficult to manage. It is important to be extremely careful not to make this situation worse or to cause a complication, such as a perforated esophagus, that can be fatal. It should not be considered a defeat to have to remove a foreign body surgically, for this is sometimes the safest means [2]. In this case, the stomach was opened by longitudinal gastrotomy in the greater curvature and the foreign bodies were removed. The next day, on the basis of visual and auditive hallucinations, the patient left the surgical unit, refusing any treatment. A psychotic illness was diagnosed and mandatory treatment was given. The patient was referred for a psychiatric consultation and after one month of follow-up showed a satisfactory recovery.
| 1. | Goldfrank LR, Flomenbaum NE, Lewin NA. Hydrocarbons. 5th editor. New York: McGraw-Hill 1994; 1231-1241. |
| 2. | Eisen GM, Baron TH, Dominitz JA, Faigel DO, Goldstein JL, Johanson JF, Mallery JS, Raddawi HM, Vargo JJ 2nd, Waring JP. Guideline for the management of ingested foreign bodies. Gastrointest Endosc. 2002;55:802-806. |