Published online Apr 28, 2008. doi: 10.3748/wjg.14.2615
Revised: January 26, 2008
Published online: April 28, 2008
Stercoral ulceration results from impaction of hard fecal mass on the colonic wall and is a relatively unknown cause of lower gastrointestinal bleeding. In this report, we describe a case of lower gastrointestinal bleeding due to stercoral ulceration resulting from Sevelamer, a drug which is commonly associated with constipation.
- Citation: Madan P, Bhayana S, Chandra P, Hughes JI. Lower gastrointestinal bleeding: Association with Sevelamer use. World J Gastroenterol 2008; 14(16): 2615-2616
- URL: https://www.wjgnet.com/1007-9327/full/v14/i16/2615.htm
- DOI: https://dx.doi.org/10.3748/wjg.14.2615
Stercoral ulceration is defined as an ulcer caused by pressure necrosis from hard fecal mass (fecaloma) pressing on the colonic wall. It is a relatively unknown cause of lower gastrointestinal bleeding[1]. A prolonged history of constipation is present in almost 80% of the patients with this condition[1]. Sevelamer, a phosphate binder, is often used in treatment of hyperphosphatemia associated with chronic kidney diseases. It is associated with constipation in 8%-10% of the patients[2]. To the best of our knowledge, this is the first case in which stercoral ulceration as a cause of lower gastrointestinal bleed has been ascribed to Sevelamer use.
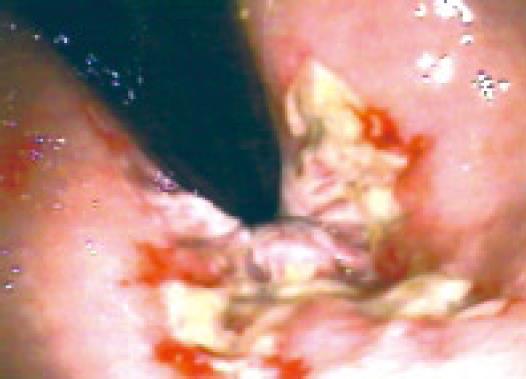
A 62-year-old woman presented with bleeding per rectum for one day. She reported a history of constipation which occurred 1 mo ago when she started taking Sevelamer. She had not had a bowel movement for several days and when she started straining in the toilet, “something gave way” and she passed two hard stools and started bleeding from rectum. The blood was bright red in color. She felt lightheaded and was brought to the hospital. Her previous medical history was significant for diabetes mellitus, end-stage renal disease, coronary artery disease and cerebrovascular accident with no residual deficit. Besides Sevelamer, she was also taking Clopidogrel but never had similar episodes of bleeding before. Physical examination revealed tachycardia and hypotension. Her hemoglobin dropped from baseline of 12 gm/dL to 9.5 gm/dL. She was stabilized with intravenous fluid, red blood cell transfusions and subjected to colonoscopy which revealed stercoral ulcers in rectum (Figure 1). Histological examination of the ulcer showed denuded mucosa with acute and chronic inflammation. Her bleeding stopped spontaneously and she did not have any further episodes of bleeding and was later discharged on stool softeners after stopping the offending drug.
The exact prevalence of stercoral ulceration in general population is unknown. Autopsy studies have revealed presences of stercoral ulceration in about 1.3%-5.7% of elderly institutionalized patients[34]. Stercoral ulcers are usually asymptomatic but may cause two dreaded complications: perforation and bleeding. However, these complications are rare in literature. Stercoral ulceration was first described in 1894 and since then less than 100 cases of stercoral ulceration associated perforation have been reported[1]. The number of stercoral ulceration presenting as hematochezia is even lower.
Severe constipation is considered to be the main causative factor in formation of stercoral ulceration and is present in 81% of the patients[1]. The elderly, debilitated or institutionalized patients on multiple medications are affected most frequently. Stercoral ulceration with consequent perforation has been reported in association with narcotics, amitriptyline, verapamil, immunosuppressive agents, aluminum based antacids and non-steroidal anti-inflammatory drugs (NSAIDs)[5–8]. The effect of NSAIDs might be related to its inhibitory effect on formation of mucosa protecting prostaglandins rather than constipation. We could not find any report in which stercoral ulceration had been found as the consequence of Sevelamer use.
Stercoral ulcers are caused by pressure necrosis from the hard fecaloma pressing on the colonic wall. The contours of stercoral ulcers are often well-demarcated corresponding to the shape of fecolith. A fecaloma is most likely to form in the distal colon where the stools are in the most dehydrated form. The fecaloma is frequently impacted at the site of recto-sigmoid junction which is also the narrowest part of the colon. As a result of impaction, the intraluminal pressure often exceeds the capillary perfusion pressure of the bowel wall predisposing the mucosa to necrosis and ulceration[1].
Treatment of stercoral ulceration depends upon the presenting symptoms. Complications arising from stercoral ulceration may lead to a 50% mortality in the population at risk due to accompanying comorbidities. The stercoral perforation is usually treated surgically and those presenting with massive hemorrhage may require emergent resection or endoscopic therapy[9].
A common clinical problem such as constipation can sometimes cause relatively unknown but potentially fatal complication such as stercoral ulceration. An internist should monitor development of constipation in a patient who is newly started on Sevelamer.
| 1. | Maurer CA, Renzulli P, Mazzucchelli L, Egger B, Seiler CA, Buchler MW. Use of accurate diagnostic criteria may increase incidence of stercoral perforation of the colon. Dis Colon Rectum. 2000;43:991-998. |
| 2. | UptoDate (Accessed April 20, 2007). Available from: URL: http://utdol.com/utd/content/topic.do?topicKey=drug_l_z/78586&selectedTitle=1~14&source=search_result. |
| 3. | Grinvalsky HT, Bowerman CI. Stercoraceous ulcers of the colon: relatively neglected medical and surgical problem. J Am Med Assoc. 1959;171:1941-1946. |
| 4. | Lal S, Brown GN. Some unusual complications of fecal impaction. Am J Proctol. 1967;18:226-231. |
| 6. | Haley TD, Long C, Mann BD. Stercoral perforation of the colon. A complication of methadone maintenance. J Subst Abuse Treat. 1998;15:443-444. |
| 7. | Doughty JC, Donald AK, Keogh G, Cooke TG. Stercoral perforation with verapamil. Postgrad Med J. 1994;70:525. |