INTRODUCTION
Accessory spleens are congenital foci of healthy splenic tissues that are separate from the main body of the spleen[1]. They arise from the fusion failure of the splenic anlage located in the dorsal mesogastrium in the fifth week of fetal life[2]. Accessory spleen is relatively common and is seen in 10%-30% of patients at autopsy[3,4], and in 16% of patients undergoing contrast-enhanced computed tomography (CT) of the abdomen[3]. Typically, accessory spleen appears as a well-marginated round solitary nodule smaller than 2 cm and enhances homogeneously on the contrast-enhanced image[3,5]. It is located at the splenic hilum or adjacent to the pancreatic tail in most cases[3,6]. Although it is usually asymptomatic and incidentally discovered, accessory spleen is clinically important in certain patients[7-17]. It is likely that some accessory spleens simulate tumors arising from adjacent organs such as the kidney, adrenal grand and pancreas[3-10].
In the present case, the accessory spleen was excepti-onally large, measuring more than 5 cm and presented a submucosal tumor (SMT) of the stomach at endoscopy. In this regard, 99mTechnetium sulfur colloid scintigraphy was useful for a definite diagnosis.
CASE REPORT
A 62-year-old man presented with a 4-wk duration of upper abdominal discomfort. His past and family histories were non-contributory. He did not smoke and drink alcohol, and received no previous gastrointestinal surgeries including splenectomy. On admission, physical examination and laboratory data including peripheral blood counts and liver function tests were all unremarkable. Upper gastrointestinal endoscopy revealed a submucosal tumor (SMT) with a bridging fold at the posterior wall of the upper gastric fundus (Figure 1). Endoscopic ultrasonography revealed a tumor having homogenous echogenicity with central blood vessels, and its origin being extragastric (Figure 2). An abdominal contrast-enhanced computed tomography (CT) showed that a well-marginated ovoid mass, approximately 6 cm in diameter (Figure 3A), enhanced homogenously to a similar degree as splenic parenchyma. It was supplied by a vascular branch arising from the splenic artery (Figure 3B). An exceptionally enlarged accessory spleen was suspected, but for a more definite diagnosis, 99mtechnetium sulfur colloid scintigraphy was done and the mass was confirmed to be splenic tissues (Figure 4). A diagnosis of accessory spleen manifesting as a gastric SMT was made. As complications associated with an accessory spleen can rarely include torsion of a wandering accessory spleen or bleeding caused by spontaneous rupture[14-17], the patient is now carefully followed in outpatient clinic.
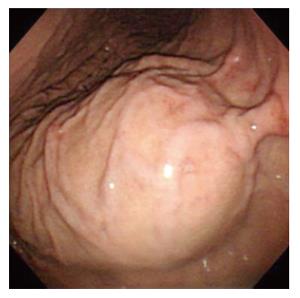
Figure 1 Gastroscopy showing submucosal tumor at the posterior wall of the upper corpus.
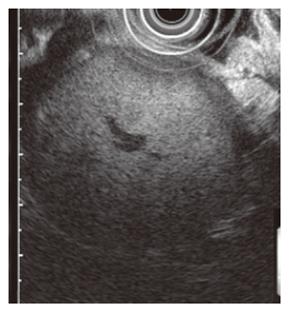
Figure 2 Endoscopic ultrasono-graphy showing extragastric mass with homogenous echogenecity with central vessels.
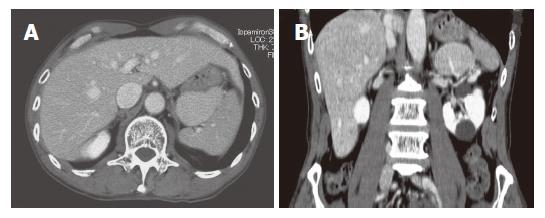
Figure 3 An abdominal contrast-enhanced CT.
A: A well-marginated ovoid mass, approximately 6 cm in diameter; B: Supplied by a vascular branch arising from the splenic artery. There are renal cysts.
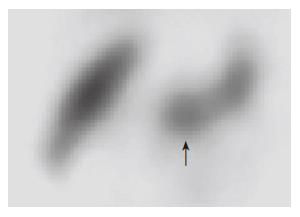
Figure 4 99mTech-netium sulfur colloid scintigraphy confirms the mass to be splenic tissues.
DISCUSSION
We reported herein a quite large accessory spleen, approximately 6 cm in diameter, adjoining the stomach, appearing as a gastric SMT at endoscopy. In a large cohort of patients, where abdominal CT scans were performed in 1000 consecutive series, the diameters of accessory spleens varied between 8 and 32 mm, with a mean of 16.8 mm[3]. Beahrs et al[4] observed no accessory spleen larger than 2.5 cm among more than 8000 abdominal CT examinations of patients with normal-sized intact spleen. It has been reported that accessory spleens had compensatory hypertrophy as a result of previous splenectomy, which sometimes reached 3-5 cm in size[4]. The accessory spleen seen in the present case seems to be exceptionally large despite no history of splenectomy.
CT is the imaging technique most commonly used to evaluate the abdomen and therefore, familiarity with CT features of accessory spleens is helpful in the differential diagnosis[3,6]. They are round or oval and the attenuation is identical to that of the proper splenic parenchyma both before and after administration of contrast medium[3,6]. On dynamic CT, supplying vascular branches arising from the splenic artery were found in less than 43.3%[3], as seen in our patient. In addition, endoscopic ultrasonography revealed that the mass with the homogenous parenchymal texture originated from extragastric tissues. Based on these findings, an accessory spleen was suspected. Some accessory spleens, however, can mimic an enlarged lymph node as well as a tumor arising from adjacent organs such as the adrenal gland, pancreas and kidney[14-17]. In fact, differentiation from a hypervascular pancreatic neoplasm (e.g. islet tumor) is sometimes challenging[3]. Similarly, accessory spleens may be differentiated from metastatic lesions or lymphadenopathy when they enhanced to the same degree as the spleen[3]. In such cases, 99mTechnetium sulfur colloid scintigraphy provides an easily accomplished method to establish the identity of ectopic splenic and hepatic tissues[4-6]. Actually, the large mass mimicking gastric SMT could be readily identified by the radionuclide imaging in the present case, leading to the definite diagnosis of accessory spleen.
Ectopic splenic tissue may be caused by autotrans-plantation of splenic cells within the peritoneal cavity resulting from traumatic disruption of the splenic capsule[18,19]. It is called splenosis, the nodules are more numerous and widespread, and often occur in locations inconsistent with accessory spleens[18,19]. Our patient had neither historic nor anatomic features of splenosis.
Although an accessory spleen is an incidental finding with no clinical significance in most patients[3,6], the detection and characterization would be occasionally important in the clinical scenarios[11-17]. Accessory spleens may become symptomatic because of torsion, spontaneous rapture, hemorrhage and cystic formation[14-17]. A surgeon's awareness of their presence may be important when the intention is to remove functional splenic tissues[11-13]. The return of splenic function caused by compensatory enlargement of ectopic splenic tissues has been implicated in the recurrence of hematologic disorders such as thrombocytopenic purpura[11-13]. For these reasons, the present patient was to be carefully followed up by imaging examinations including CT. Since his clinical course is uneventful and the patient remains asymptomatic without any abnormalities in physical and laboratory examinations, splenectomy has not been considered yet.