Published online Sep 14, 2006. doi: 10.3748/wjg.v12.i34.5577
Revised: April 28, 2006
Accepted: May 22, 2006
Published online: September 14, 2006
A case of a large multiplex recurrent hydatid cyst involving the left gluteal muscle and the left iliopsoas, accompanied with degeneration of the musculature of the left upper leg is presented along with a review of the relevant literature. Very few such cases have been reported worldwide. The presented case is also distinguished by the involvement of muscles of distant anatomic areas.
- Citation: Drimousis PG, Stamou KM, Koutras A, Tsekouras DK, Zografos G. Unusual site of recurrent musculoskeletal hydatid cyst: Case report and brief review of the literature. World J Gastroenterol 2006; 12(34): 5577-5578
- URL: https://www.wjgnet.com/1007-9327/full/v12/i34/5577.htm
- DOI: https://dx.doi.org/10.3748/wjg.v12.i34.5577
Echinococcosis is a zoonotic infection caused by tapeworms of the genus Echinococcus which inhabits in the small intestine of carnivores. The adult worms produce eggs that are released with the feces and spread in various ways, such as through the wind, water or flies[2]. After ingestion by the host, the embryos migrate through the intestinal wall and are either arrested in the capillary bed of the liver developing into liver cysts, or manage to penetrate into systemic circulation thus ending up in remote organs. The lung, the brain, and the muscles or bones are the more frequently involved distant organs. Due to their physiologic role as capillary filters and their vast capillary volume, the liver and lung are most often affected. Other manifestations are found in 15% of the patients, with the skeletal system making up for 1%-4% of all cases[7]. Voluntary muscles are a very rare site of infection, counting for less than 1% of total[3].
In this report, we present a case of a large multiplex recurrent hydatid cyst involving the left gluteal muscle and the left iliopsoas, accompanied with degeneration of the musculature of the left upper leg. To our knowledge, less than 50 such cases have been reported in the literature worldwide. The presented case is also distinguished by the involvement of muscles of distant anatomic areas, while no liver, lung or bone lesions were identified.
A 78-year-old Caucasian male was admitted to our clinic, with a swelling of the waist and the left upper leg. The patient had been operated four times over the past 18 years for echinococcosis of the musculature of the left upper leg. During this period, he suffered recurrent swellings of the thigh that were treated as abscesses. His past medical record was otherwise unremarkable.
On physical examination, a mass was located in the left waist and the upper part of the left gluteus muscle. A communicating fistula with a daughter cyst was identified in the median part of the left gluteus muscle. Another communicating fistula extended from the daughter cyst to 5 cm above the knee joint where a third cyst was palpable. The aforementioned findings were also visible on ultrasound (US) and MRI studies. The lesions of the primary and daughter cyst in the waist and the communicating fistula were located superficially at the fascia of the left gluteus muscle (maximum diameter 10 cm).
There were no signs of calcification in any of these cysts. No liver or lung manifestations were present. Anti-echinococcal IgG was positive for infection (title 2,2, positive if > 1.1, ELISA).
The patient was submitted to perform a complete cystopericystectomy of both primary and daughter cysts and radical excision of the fistula. The overlying skin was excised and the surgical wound was primarily closed. The lesions were easily dissected from the underlying fascia that did not need removal. The cysts contained purulent material. The wound was drained for 24 h. The surgical specimen was submitted for histopathological examination which confirmed the diagnosis. The postoperative course was uneventful and the patient was discharged on the 6th postoperative day. He has been followed up for 16 mo and no recurrent cyst was evident on CT and MRI scan.
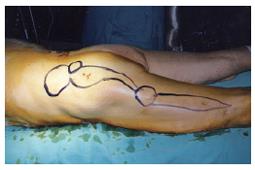
Soft tissue hydatid disease is rare even in endemic areas, such as the Mediterranean. Intramuscular lesions in the absence of liver, lung or bone manifestations are most uncommon[1,4]. In our case, we encountered an extended soft tissue disease with no signs of systemic infection but a history of multiple recurrences. To our knowledge, very few similar cases have been reported in the literature worldwide (Table 1). Recurrences had developed in the form of abscess-like lesions in multiple sites of the leg which is also uncommon in intramuscular infections. Quality of life of this patient was poor due to constant symptomatic hymenitis, possibly a result of chronic local inflammation. He also experienced mobilization difficulties (Figure 1).
| Author | n | Site of infection | Liver/lung/bone involvement |
| Merkle et al[2] | 8 | Iliopsoas, left adductor musculature, left femur, left medial gluteal muscle, musculature of right upper leg | Yes |
| Rieber et al[8] | 1 | Paravertebral structures | Yes |
| Sennaroglu et al | 1 | Infratemporal | Yes |
| Von Sinner[11] | 1 | Pelvic | Yes |
| Torricelli et al[12] | 14 | Bone infection with adjacent soft tissue involvement in 12 cases | |
| Aydin et al[13] | 1 | Cerebral | Yes |
| Duncan et al[4] | 1 | Biceps brachii | No |
| Dahniya et al[3] | 7 | 5 bone infections without soft tissue involvement, 2 primary intramuscular (left shoulder, rectus femoris and vastus lateralis) | No |
Determining the ideal therapeutic approach for a recurrent musculosceletal hydatid cyst can be quite challenging for the general surgeon. Moreover, the rarity of the disease renders the decision making on the favorable treatment quite difficult. Conservative treatment, complete excision and simple drainage have all been suggested as adequate[10]. Hydatid disease progresses slowly and is rarely life-threatening, especially when located in the soft tissue or muscles, thus supporting a more conservative therapeutic approach. Additionally, co-morbid conditions and advanced age of the patient as well as the surgeon’s experience are of great importance for the final decision. However, in case the disease causes profound disabilities or mobilization problems, complete cystopericystectomy should always be considered.
The nature of the lesion should be well documented and evaluated. Radical surgical therapy is especially indicated in cases of unilocular manifestations as only this method offers hope of permanent cure[9]. Therapeutic dilemmas could arise in cases of extended disease with many muscles or muscle layers in different sites of the body which are communicating via fistulas. Communication between lesions should always be suspected and revealed, even if primary and daughter cysts are distant. Complete surgical treatment should include the primary lesion, the daughter cysts and the communicating fistulas as a whole specimen.
Hydatid disease may occur anywhere in the musculo-skeletal system, from the big toe to the crown of the head[5,6,8]. In endemic areas, echinococcosis should be always suspected and bared in mind in the differential diagnosis of cystic lesions in soft tissue, even if the radiological appearance is not typical. Once the diagnosis is established, the surgeon should consider performing a radical procedure aiming in minimizing the possibility of a recurrence.
S- Editor Wang J L- Editor Kumar M E- Editor Bai SH
| 1. | Alldred AJ, Nisbet NW. Hydatid disease of bone in Australasia. J Bone Joint Surg Br. 1964;46:260-267. [PubMed] |
| 2. | Bourée P. Hydatidosis: dynamics of transmission. World J Surg. 2001;25:4-9. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 39] [Cited by in RCA: 45] [Article Influence: 1.9] [Reference Citation Analysis (0)] |
| 3. | Dahniya MH, Hanna RM, Ashebu S, Muhtaseb SA, el-Beltagi A, Badr S, el-Saghir E. The imaging appearances of hydatid disease at some unusual sites. Br J Radiol. 2001;74:283-289. [PubMed] |
| 4. | Duncan GJ, Tooke SM. Echinococcus infestation of the biceps brachii. A case report. Clin Orthop Relat Res. 1990;247-250. [PubMed] |
| 5. | Guthrie JA, Lawton JO, Chalmers AG. Case report: The MR appearances of primary intramuscular hydatid disease. Clin Radiol. 1996;51:377-379. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 31] [Cited by in RCA: 32] [Article Influence: 1.1] [Reference Citation Analysis (0)] |
| 6. | Lewall DB. Hydatid disease: biology, pathology, imaging and classification. Clin Radiol. 1998;53:863-874. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 118] [Cited by in RCA: 111] [Article Influence: 4.1] [Reference Citation Analysis (0)] |
| 7. | Merkle EM, Schulte M, Vogel J, Tomczak R, Rieber A, Kern P, Goerich J, Brambs HJ, Sokiranski R. Musculoskeletal involvement in cystic echinococcosis: report of eight cases and review of the literature. AJR Am J Roentgenol. 1997;168:1531-1534. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 82] [Cited by in RCA: 83] [Article Influence: 3.0] [Reference Citation Analysis (0)] |
| 8. | Rieber A, Brambs HJ, Friedl P. [CT in echinococcosis of the lumbar spine and paravertebral structures]. Rofo. 1989;151:379-380. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 2] [Cited by in RCA: 4] [Article Influence: 0.1] [Reference Citation Analysis (0)] |
| 9. | Saimot AG. Medical treatment of liver hydatidosis. World J Surg. 2001;25:15-20. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 82] [Cited by in RCA: 83] [Article Influence: 3.5] [Reference Citation Analysis (0)] |
| 10. | Sielaff TD, Taylor B, Langer B. Recurrence of hydatid disease. World J Surg. 2001;25:83-86. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 53] [Cited by in RCA: 60] [Article Influence: 2.5] [Reference Citation Analysis (0)] |
| 11. | von Sinner WN. A case of primary osseous pelvic hydatid disease (Echinococcus granulosus). Rofo. 1991;155:88-90. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 5] [Cited by in RCA: 7] [Article Influence: 0.2] [Reference Citation Analysis (0)] |
| 12. | Torricelli P, Martinelli C, Biagini R, Ruggieri P, De Cristofaro R. Radiographic and computed tomographic findings in hydatid disease of bone. Skeletal Radiol. 1990;19:435-439. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 58] [Cited by in RCA: 56] [Article Influence: 1.6] [Reference Citation Analysis (0)] |
| 13. | Aydin Y, Barlas O, Yolaş C, Aydin IH, Ceviz A, Aladağ A, Oren D, Akdemir D. Alveolar hydatid disease of the brain. Report of four cases. J Neurosurg. 1986;65:115-119. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 18] [Cited by in RCA: 19] [Article Influence: 0.5] [Reference Citation Analysis (0)] |