Published online Sep 14, 2005. doi: 10.3748/wjg.v11.i34.5404
Revised: January 23, 2005
Accepted: January 26, 2005
Published online: September 14, 2005
Inflammatory bowel disease (IBD) is an idiopathic inflammatory disease of the gastrointestinal tract. The pathophysiology of IBD is probably the result of the complex interaction of genetic susceptibility and environmental influences. There is a well-known risk of thrombosis in patients with IBD. We present the case of a 53-year-old man with ulcerative colitis, who spontaneously developed intracranial sinus thrombosis that was treated with low molecular weight heparin. Literature was searched to assess the frequency and characteristics of cerebral sinus thrombosis in IBD and the role of certain etiopathological factors in such thrombotic patients.
- Citation: Umit H, Asil T, Celik Y, Tezel A, Dokmeci G, Tuncbilek N, Utku U, Soylu AR. Cerebral sinus thrombosis in patients with inflammatory bowel disease: A case report. World J Gastroenterol 2005; 11(34): 5404-5407
- URL: https://www.wjgnet.com/1007-9327/full/v11/i34/5404.htm
- DOI: https://dx.doi.org/10.3748/wjg.v11.i34.5404
Inflammatory bowel disease (IBD) is an idiopathic inflammatory disease of the gastrointestinal tract. The pathophysiology of IBD is probably the result of the complex interaction of genetic susceptibility and environmental influences. The exact pathogenesis of IBD is unknown. There is a well-known risk of thrombosis in patients with IBD. This pro-thrombotic state seen in IBD has been proposed as a factor contributing to the pathogenesis of IBD, especially in Crohn’s disease[1,2]. This conclusion is based on the presence of thrombi in the small vessels of mucosa and submucosa. Furthermore, some IBD patients have been successfully treated with heparin[3-6].
Thromboembolism is a serious complication of IBD patients. The yearly incidence of thromboembolic events in IBD is 13-64/1 000[7,8]. Corticosteroid usage to diminish inflammatory activity and concomitant abnormalities of coagulation cascade such as factor V mutations, protein C and S deficiency, prothrombin gene mutation, hyperhomo-cysteinemia could increase the risk of thromboembolic complications. On the other hand, some researchers found that the incidence (1.5/1 000 IBD patients per year) of venous thrombosis does not increase in IBD patients and that IBD patients have venous thrombosis earlier in life than non-IBD patients[9].
Deep venous thrombosis and pulmonary emboli are the most common thrombotic complications in IBD. However, cerebral vascular involvement is rare. It was reported that 92 of 7 199 IBD patients suffer from thrombotic complications, 9 of the 92 patients have cerebral vessel involvement[7].
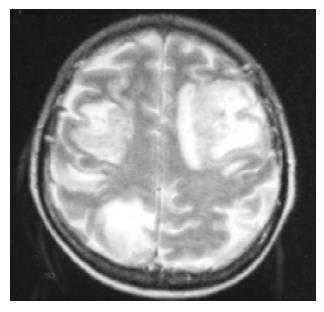
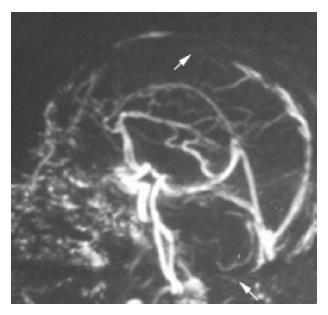
A 53-year-old man suffering from abdominal pain, bloody diarrhea (8-10 stools per day) and weight loss (10 kg in the past 3 mo) was admitted to our hospital in April 2003. On admission, his body temperature was 38°C. His physical examination revealed no abnormalities except for mild sinusal tachycardia (100 pulses/min). Neurological examination revealed no paralysis and sensory motor disturbances. The blood and stool cultures obtained on his first day of admission did not yield any pathogens. Microscopic stool examination revealed abundant leukocytes and erythrocytes. The stool C. Difficile toxin A assay was negative. Laboratory data showed elevated C reactive protein (CRP) levels and ESR, mild elevations of aminotransferases with ALT/AST ratio >1, mild thrombocytosis (568 000/mm3) and normochromic anemia with a hemoglobin value of 10 g/L. His colonoscopic evaluation revealed loss of mucosal vascular pattern, granularity and friability of the whole colonic mucosa and widespread pseudopolyps. Histopathological examination of the rectal mucosa showed an abundant infiltration of neutrophils, lymphocytes and plasma cells. Histopathology also revealed cryptitis and crypt abscess in some areas. The patient’s ultrasonography and carcinoembryonic antigen (CEA) levels were normal. Hepatotrophic virus (Hepatitis B and C) and autoimmune markers (anti-nuclear, anti-smooth muscle and anti-neutrophilic cytoplasmic antibodies) were negative. Based on these findings, the patient was diagnosed with moderately active ulcerative pancolitis and started on 4 g of sulfasalazine as anti-inflammatory therapy. Nutritional support was also provided. One week after treatment, his number of times of defecation decreased to 5 stools per day with no blood and the patient was afebrile. CRP levels decreased, thrombocytes were in normal limit but mild anemia persisted. During the second week of therapy the platelet count was 130 000/mm3. Sulfasalazine was discontinued and 40 mg prednisolone was started. On the third day of corticosteroid treatment, the patient complained of weakness of the right arm and leg. His neurological examination revealed left sided hemiparesis. Motor strength was 2/5 and 4/5 in upper and lower left extremities, respectively. The patient had mild dysarthria. Deep tendon reflexes were brisk. Plantar response in left side was extensive. Cranial CT scan and T2 weighted magnetic resonance imaging showed bifrontal and right parietal infarction (Figure 1). Sagittal MRI venography revealed signal dropout in the superior sagittal sinus and right transverse sinus (Figure 2). We started low molecular weight heparin (LMWH) therapy immediately. The patient also developed focal motor seizures. He became unconscious (Glasgow coma score was 6) 3 d after the first neurological sign. He was on therapy of LMWH and control CT showed no additional abnormality. Laboratory tests for coagulation abnormalities revealed heterozygous factor V Leiden gene mutation. The patient died of pulmonary nosocomial infection and sepsis 2 wk after the onset of neurological findings.
Extraintestinal manifestations are common in ulcerative colitis and Crohn’s disease occurring in at least 25-40% of patients and can be classified as related to disease activity or not[10]. If secondary systemic effects of therapy on disease and complications are also included, almost all patients have extraintestinal manifestations.
Thromboembolism is a serious complication of IBD patients. Intravascular thrombosis in mucosal blood vessels may play a role in the pathogenesis of IBD. Some studies indicate that heparin may benefit the treatment of IBD[3-6]. There are some conflicting data about the incidence of thrombotic events in IBD patients. The risk factors, relationship between disease activity, corticosteroid use and thrombotic events, incidence of concomitant coagulation disorders and effect of corticosteroid on thrombosis in IBD patients are still not completely understood. Grip et al[9] found that the incidence of venous thrombosis does not increase in IBD patients. However, studies showed that the incidence of thrombotic complications increases in IBD patients[7,8]. These contradictory data may be related to the changing management of IBD patients. Nowadays, IBD patients are less frequently hospitalized and immobilized. This may be the reason why the current incidence of thrombotic complications is lower in IBD patients[9].
Pro-thrombotic factors (anti-cardiolipin antibodies, hyperhomocysteinemia and changes in the lipid spectrum), IBD-induced alterations in plasma and mucosal hemostasis (increased endothelial activation and tissue factor expression, and impaired inhibition of coagulation in IBD), and changes secondary to inflammation have been suggested as the explanatory factors for the high prevalence of thromboemb-olism in IBD patients. The balance between pro-coagulant and pro-fibrinolytic factors seems to favor plasma hypercoagulability in IBD patients. Inflammation-induced changes in serum, endothelial cells and platelets induce plasma alterations resulting in coagulation activation, whereas coagulation activation induces pro-inflammatory effects, thus providing a looping chain of reactions[11].
van Bodegraven et al[12] studied hemostatic imbalance in active and quiescent ulcerative colitis and found that coagulation and fibrinolytic cascades are activated in active ulcerative colitis and 20% of patients are in remission with a hemostatic imbalance in favor of coagulation. The clinical significance of these phenomena is unknown. Meanwhile previous studies have shown that activated plasma coagulation markers increase in clinically quiescent IBD[13]. Thus, clinical activity of the disease may increase the risk, but it is probably of minor importance.
Hyperhomocysteinemia and coagulation cascade abnormalities in IBD patients have been studied[14-16]. Hyperhomocysteinemia is common in IBD patients but elevated total homocysteine levels do not contribute to the development of thrombotic complications[17].
No correlation is found between hereditary conditions predisposing to thrombosis such as factor V mutation, prothrombin gene mutation, MTHFR mutation, proteins C and S, antithrombin III deficiencies and IBD[18]. Thus, higher prevalence of thrombosis in IBD patients is not due to genetic linkage. Taken together, existing data indicate that thrombosis in IBD patients is due to multifactors.
Deep venous thrombosis and pulmonary emboli are the most common thrombotic complications in IBD patients, however, cerebral vascular involvement is rare. It was reported that IBD patients are relatively young and have no other relevant risk factors except for IBD[19].
Cerebral venous and dural sinus thrombosis in association with IBD is rare and few cases have been reported[20-24]. Some clinical characteristics of these patients are summarized in Table 1. The frequency of cerebral venous thromboembolic complications in ulcerative colitis patients appears to be greater than that in patients with Crohn’s disease. The superior sagittal sinus and lateral sinuses are commonly involved[25-27]. Less frequently, isolated cortical venous thromboses have been reported[22]. Although one case that present with sagittal sinus thrombosis 10 years after proctocolectomy for ulcerative colitis has been reported, these cerebral venous thrombotic events occur more frequently in patients with active inflammatory bowel disease[28-32]. The most frequent symptoms and signs are headache, paresis, seizures, dysphasia and papilla edema. Approximately 1/3 of patients have some coagulation abnormalities such as FV Leiden mutation, hyperhomocysteinemia, positive anti-cardiolipin antibodies[20,26,27]. The clinical outcome is devastating[33-37].
| Reference | Sex | Age | IBDactivity | IBDlocation | IBDduration | CNS circulationinvolved | Outcome | Coagulation studies | Miscellaneous |
| Gonera et al.[20] | F | 30 | Active | Pancolitis | - | SSS | Recovered | Functional | Deep |
| APC resistance, | venous | ||||||||
| hyperhomocysteinemia | thrombosis | ||||||||
| Tsujikawa et al.[21] | M | 27 | Active | Recto-sigmoid | 9 yr | SSS | Recovered | - | - |
| Derdeyn et al.[22] | F | 26 | Remission | - | - | Isolated cortical | Residual | - | Deep |
| vein (sylvian vein) | venous | ||||||||
| thrombosis | |||||||||
| Das et al.[23] | M | 31 | Active | Pancolitis | - | SSS | Death | - | Pulmonary |
| emboli | |||||||||
| at autopsy | |||||||||
| M | 20 | Active | Pancolitis | 2 yr | SSS and superficial | Death | Pulmonaryemboli | ||
| cerebral veins | at autopsy | ||||||||
| Philips et al.[24] | F | 35 | - | - | - | SSS, TS, StS | - | - | |
| Recovered | |||||||||
| F | 14 | - | - | - | SSS, vein of labbe | Recovered | - | - | |
| Srivastava et al.[25] | M | 29 | Remission | - | 6 mo | SSS, left sigmoid | Recovered | No abnormality found | - |
| sinus | |||||||||
| Papi et al.[26] | F | 33 | Active | - | First attack | Superior, inferior | Residual | Lupus | Impending |
| long. Sinuses | anticoagulant positive | megacolon | |||||||
| Kao et al.[27] | - | 14 | - | - | 3 yr | SSS, vein of labbe | Residual | ANCA positive | |
| - | 7 | - | - | 4 mo | Transverse and | Residual | Elevated | - | |
| sigmoid sinuses | anticardiolipin | ||||||||
| antibody | |||||||||
| - | 20 | - | - | 6 yr | SSS and | Recovered | Elevated | - | |
| transverse sinuses | anticardiolipin | ||||||||
| antibody | |||||||||
| - | 13 | - | - | 18 mo | SSS, cortical | Recovered | Hyperhomocysteinemia, | - | |
| veins, TS, SS | heterozygous for | ||||||||
| prothrombin gene | |||||||||
| Kiff et al.[28] | F | 26 | Active | Pancolitis | First attack | Straight sinus | Death | - | In the |
| and great cerebral | postpartum | ||||||||
| vein of Galen | period | ||||||||
| Markowitz et al.[30] | M | 14 | Active | Pancolitis | 9 mo | Left sigmoid | Residual | - | - |
| and lateral sinuses | |||||||||
| Borda et al.[31] | M | 23 | Active | - | - | All major | Death | - | Pulmonary |
| venous sinuses | emboli, | ||||||||
| renal vein | |||||||||
| thrombosis | |||||||||
| Schneiderman et al.[32] | F | 12 | Active | - | - | Straight sinus, | Death | - | - |
| vein of galen | |||||||||
| Lam et al.[33] | F | 28 | - | Pancolitis | - | - | Residual | - | - |
| Averback et al.[34] | F | 25 | Remission | - | - | - | Death | - | - |
| Yerby et al.[35] | M | 28 | Remission | Pancolitis | - | - | Recovered | - | 10 yr after |
| proctocolectomy | |||||||||
| Bewermeyer et al.[36] | F | 35 | Active | - | - | Inf. Sagittal | Death | - | - |
| sinus, StS | |||||||||
| Gil-Peralta et al.[37] | F | 48 | Active | - | - | Superficial | Death | - | - |
| cortical veins | |||||||||
| Musio et al.[29] | M | 24 | - | Pancolitis | 2 yr | SSS | Recovered | - | - |
| Present study | M | 53 | Active | Pancolitis | First attack | SSS | Death | F V Leiden | Nosocomial |
| heterozygous | pulmonary | ||||||||
| mutant | infection, | ||||||||
| sepsis | |||||||||
| Total | F:11 | Mean: | Active: | Pancolitis: | - | - | - | - | - |
| M: 9 | 25.6 yr | 12 remission:4 | 10 RS: 1 |
In conclusion, cerebral venous thrombosis is a devastating complication of IBD, especially, ulcerative colitis. The diagnosis of these patients depends on the demonstration of the thrombus by neuroimaging.
Science Editor Wang XL and Guo SY Language Editor Elsevier HK
| 1. | Dhillon AP, Anthony A, Sim R, Wakefield AJ, Sankey EA, Hudson M, Allison MC, Pounder RE. Mucosal capillary thrombi in rectal biopsies. Histopathology. 1992;21:127-133. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 100] [Cited by in F6Publishing: 104] [Article Influence: 3.3] [Reference Citation Analysis (0)] |
| 2. | Wakefield AJ, Sawyerr AM, Dhillon AP, Pittilo RM, Rowles PM, Lewis AA, Pounder RE. Pathogenesis of Crohn's disease: multifocal gastrointestinal infarction. Lancet. 1989;2:1057-1062. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 409] [Cited by in F6Publishing: 424] [Article Influence: 12.1] [Reference Citation Analysis (0)] |
| 3. | Folwaczny C, Wiebecke B, Loeschke K. Unfractioned heparin in the therapy of patients with highly active inflammatory bowel disease. Am J Gastroenterol. 1999;94:1551-1555. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 87] [Cited by in F6Publishing: 90] [Article Influence: 3.6] [Reference Citation Analysis (0)] |
| 4. | Gaffney PR, Doyle CT, Gaffney A, Hogan J, Hayes DP, Annis P. Paradoxical response to heparin in 10 patients with ulcerative colitis. Am J Gastroenterol. 1995;90:220-223. [PubMed] [Cited in This Article: ] |
| 5. | Törkvist L, Thorlacius H, Sjöqvist U, Bohman L, Lapidus A, Flood L, Agren B, Raud J, Löfberg R. Low molecular weight heparin as adjuvant therapy in active ulcerative colitis. Aliment Pharmacol Ther. 1999;13:1323-1328. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 77] [Cited by in F6Publishing: 82] [Article Influence: 3.3] [Reference Citation Analysis (0)] |
| 6. | Papa A, Danese S, Gasbarrini A, Gasbarrini G. Review article: potential therapeutic applications and mechanisms of action of heparin in inflammatory bowel disease. Aliment Pharmacol Ther. 2000;14:1403-1409. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 55] [Cited by in F6Publishing: 60] [Article Influence: 2.5] [Reference Citation Analysis (0)] |
| 7. | Talbot RW, Heppell J, Dozois RR, Beart RW. Vascular complications of inflammatory bowel disease. Mayo Clin Proc. 1986;61:140-145. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 408] [Cited by in F6Publishing: 407] [Article Influence: 10.7] [Reference Citation Analysis (0)] |
| 8. | Edwards FC, Truelove SC. The course and prognosis of ulcerative colitis. iii. complications. Gut. 1964;5:1-22. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 516] [Cited by in F6Publishing: 577] [Article Influence: 9.6] [Reference Citation Analysis (0)] |
| 9. | Grip O, Svensson PJ, Lindgren S. Inflammatory bowel disease promotes venous thrombosis earlier in life. Scand J Gastroenterol. 2000;35:619-623. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 81] [Cited by in F6Publishing: 92] [Article Influence: 3.8] [Reference Citation Analysis (0)] |
| 10. | Isaacs KL. Extra-intestinal manifestations. Advanced therapy of inflam-matory bowel disease. Hamilton, London: B.C. Decker Inc 2001; 267-270. [Cited in This Article: ] |
| 11. | van Bodegraven AA. Haemostasis in inflammatory bowel diseases: clinical relevance. Scand J Gastroenterol Suppl. 2003;239:51-62. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 17] [Cited by in F6Publishing: 21] [Article Influence: 1.1] [Reference Citation Analysis (0)] |
| 12. | van Bodegraven AA, Schoorl M, Baak JP, Linskens RK, Bartels PC, Tuynman HA. Hemostatic imbalance in active and quiescent ulcerative colitis. Am J Gastroenterol. 2001;96:487-493. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 26] [Cited by in F6Publishing: 26] [Article Influence: 1.1] [Reference Citation Analysis (0)] |
| 13. | Chiarantini E, Valanzano R, Liotta AA, Cellai AP, Fedi S, Ilari I, Prisco D, Tonelli F, Abbate R. Hemostatic abnormalities in inflammatory bowel disease. Thromb Res. 1996;82:137-146. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 67] [Cited by in F6Publishing: 62] [Article Influence: 2.2] [Reference Citation Analysis (0)] |
| 14. | Papa A, De Stefano V, Danese S, Chiusolo P, Persichilli S, Casorelli I, Zappacosta B, Giardina B, Gasbarrini A, Leone G. Hyperhomocysteinemia and prevalence of polymorphisms of homocysteine metabolism-related enzymes in patients with inflammatory bowel disease. Am J Gastroenterol. 2001;96:2677-2682. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 61] [Cited by in F6Publishing: 68] [Article Influence: 3.0] [Reference Citation Analysis (0)] |
| 15. | Bjerregaard LT, Nederby NJ, Fredholm L, Brandslund I, Munkholm P, Hey H. Hyperhomocysteinaemia, coagulation pathway activation and thrombophilia in patients with inflammatory bowel disease. Scand J Gastroenterol. 2002;37:62-67. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 31] [Cited by in F6Publishing: 34] [Article Influence: 1.5] [Reference Citation Analysis (0)] |
| 16. | Romagnuolo J, Fedorak RN, Dias VC, Bamforth F, Teltscher M. Hyperhomocysteinemia and inflammatory bowel disease: prevalence and predictors in a cross-sectional study. Am J Gastroenterol. 2001;96:2143-2149. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 69] [Cited by in F6Publishing: 76] [Article Influence: 3.3] [Reference Citation Analysis (0)] |
| 17. | Oldenburg B, Fijnheer R, van der Griend R, vanBerge-Henegouwen GP, Koningsberger JC. Homocysteine in inflammatory bowel disease: a risk factor for thromboembolic complications? Am J Gastroenterol. 2000;95:2825-2830. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 71] [Cited by in F6Publishing: 80] [Article Influence: 3.3] [Reference Citation Analysis (0)] |
| 18. | Vecchi M, Sacchi E, Saibeni S, Meucci G, Tagliabue L, Duca F, De Franchis R. Inflammatory bowel diseases are not associated with major hereditary conditions predisposing to thrombosis. Dig Dis Sci. 2000;45:1465-1469. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 60] [Cited by in F6Publishing: 68] [Article Influence: 2.8] [Reference Citation Analysis (0)] |
| 19. | Lossos A, River Y, Eliakim A, Steiner I. Neurologic aspects of inflammatory bowel disease. Neurology. 1995;45:416-421. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 166] [Cited by in F6Publishing: 152] [Article Influence: 5.2] [Reference Citation Analysis (0)] |
| 20. | Gonera RK, Timmerhuis TP, Leyten AC, van der Heul C. Two thrombotic complications in a patient with active ulcerative colitis. Neth J Med. 1997;50:88-91. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 11] [Cited by in F6Publishing: 12] [Article Influence: 0.4] [Reference Citation Analysis (0)] |
| 21. | Tsujikawa T, Urabe M, Bamba H, Andoh A, Sasaki M, Koyama S, Fujiyama Y, Bamba T. Haemorrhagic cerebral sinus thrombosis associated with ulcerative colitis: a case report of successful treatment by anticoagulant therapy. J Gastroenterol Hepatol. 2000;15:688-692. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 22] [Cited by in F6Publishing: 26] [Article Influence: 1.1] [Reference Citation Analysis (0)] |
| 22. | Derdeyn CP, Powers WJ. Isolated cortical venous thrombosis and ulcerative colitis. AJNR Am J Neuroradiol. 1998;19:488-490. [PubMed] [Cited in This Article: ] |
| 23. | Das R, Vasishta RK, Banerjee AK. Aseptic cerebral venous thrombosis associated with idiopathic ulcerative colitis: a report of two cases. Clin Neurol Neurosurg. 1996;98:179-182. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 10] [Cited by in F6Publishing: 13] [Article Influence: 0.5] [Reference Citation Analysis (0)] |
| 24. | Philips MF, Bagley LJ, Sinson GP, Raps EC, Galetta SL, Zager EL, Hurst RW. Endovascular thrombolysis for symptomatic cerebral venous thrombosis. J Neurosurg. 1999;90:65-71. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 95] [Cited by in F6Publishing: 96] [Article Influence: 3.8] [Reference Citation Analysis (0)] |
| 25. | Srivastava AK, Khanna N, Sardana V, Gaekwad S, Prasad K, Behari M. Cerebral venous thrombosis in ulcerative colitis. Neurol India. 2002;50:215-217. [PubMed] [Cited in This Article: ] |
| 26. | Papi C, Ciaco A, Acierno G, Di Battista G, Talamanca LF, Lo Russo F, Natali G, Capurso L. Severe ulcerative colitis, dural sinus thrombosis, and the lupus anticoagulant. Am J Gastroenterol. 1995;90:1514-1517. [PubMed] [Cited in This Article: ] |
| 27. | Kao A, Dlugos D, Hunter JV, Mamula P, Thorarensen O. Anticoagulation therapy in cerebral sinovenous thrombosis and ulcerative colitis in children. J Child Neurol. 2002;17:479-482. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 31] [Cited by in F6Publishing: 32] [Article Influence: 1.5] [Reference Citation Analysis (0)] |
| 28. | Kiff RS, Denton GW. Fatal cerebral venous thrombosis complicating acute ulcerative colitis. Am J Gastroenterol. 1989;84:577-578. [PubMed] [Cited in This Article: ] |
| 29. | Musio F, Older SA, Jenkins T, Gregorie EM. Case report: cerebral venous thrombosis as a manifestation of acute ulcerative colitis. Am J Med Sci. 1993;305:28-35. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 21] [Cited by in F6Publishing: 28] [Article Influence: 0.9] [Reference Citation Analysis (0)] |
| 30. | Markowitz RL, Ment LR, Gryboski JD. Cerebral thromboembolic disease in pediatric and adult inflammatory bowel disease: case report and review of the literature. J Pediatr Gastroenterol Nutr. 1989;8:413-420. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 37] [Cited by in F6Publishing: 38] [Article Influence: 1.1] [Reference Citation Analysis (0)] |
| 31. | Borda IT, Southern RF, Brown WF. Cerebral venous thrombosis in ulcerative colitis. Gastroenterology. 1973;64:116-119. [PubMed] [Cited in This Article: ] |
| 32. | Schneiderman JH, Sharpe JA, Sutton DM. Cerebral and retinal vascular complications of inflammatory bowel disease. Ann Neurol. 1979;5:331-337. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 87] [Cited by in F6Publishing: 93] [Article Influence: 2.1] [Reference Citation Analysis (0)] |
| 33. | Lam A, Borda IT, Inwood MJ, Thomson S. Coagulation studies in ulcerative colitis and Crohn's disease. Gastroenterology. 1975;68:245-251. [PubMed] [Cited in This Article: ] |
| 34. | Averback P. Primary cerebral venous thrombosis in young adults: the diverse manifestations of an underrecognized disease. Ann Neurol. 1978;3:81-86. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 69] [Cited by in F6Publishing: 74] [Article Influence: 1.6] [Reference Citation Analysis (0)] |
| 35. | Yerby MS, Bailey GM. Superior sagittal sinus thrombosis 10 years after surgery for ulcerative colitis. Stroke. 1980;11:294-296. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 26] [Cited by in F6Publishing: 28] [Article Influence: 0.6] [Reference Citation Analysis (0)] |
| 36. | Bewermeyer H, Dreesbach HA, Krakamp B. Cerebral venous and sinus thrombosis in ulcerative colitis. Rofo. 1985;143:597-598. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 5] [Cited by in F6Publishing: 5] [Article Influence: 0.1] [Reference Citation Analysis (0)] |
| 37. | Gil-Peralta A, Salazar JA, Chinchón I, Alberca R. Cerebral venous thrombosis and ulcerative colitis. Med Clin (Barc). 1982;79:332-335. [PubMed] [Cited in This Article: ] |