Copyright
©The Author(s) 2018.
World J Gastroenterol. Jul 14, 2018; 24(26): 2853-2866
Published online Jul 14, 2018. doi: 10.3748/wjg.v24.i26.2853
Published online Jul 14, 2018. doi: 10.3748/wjg.v24.i26.2853
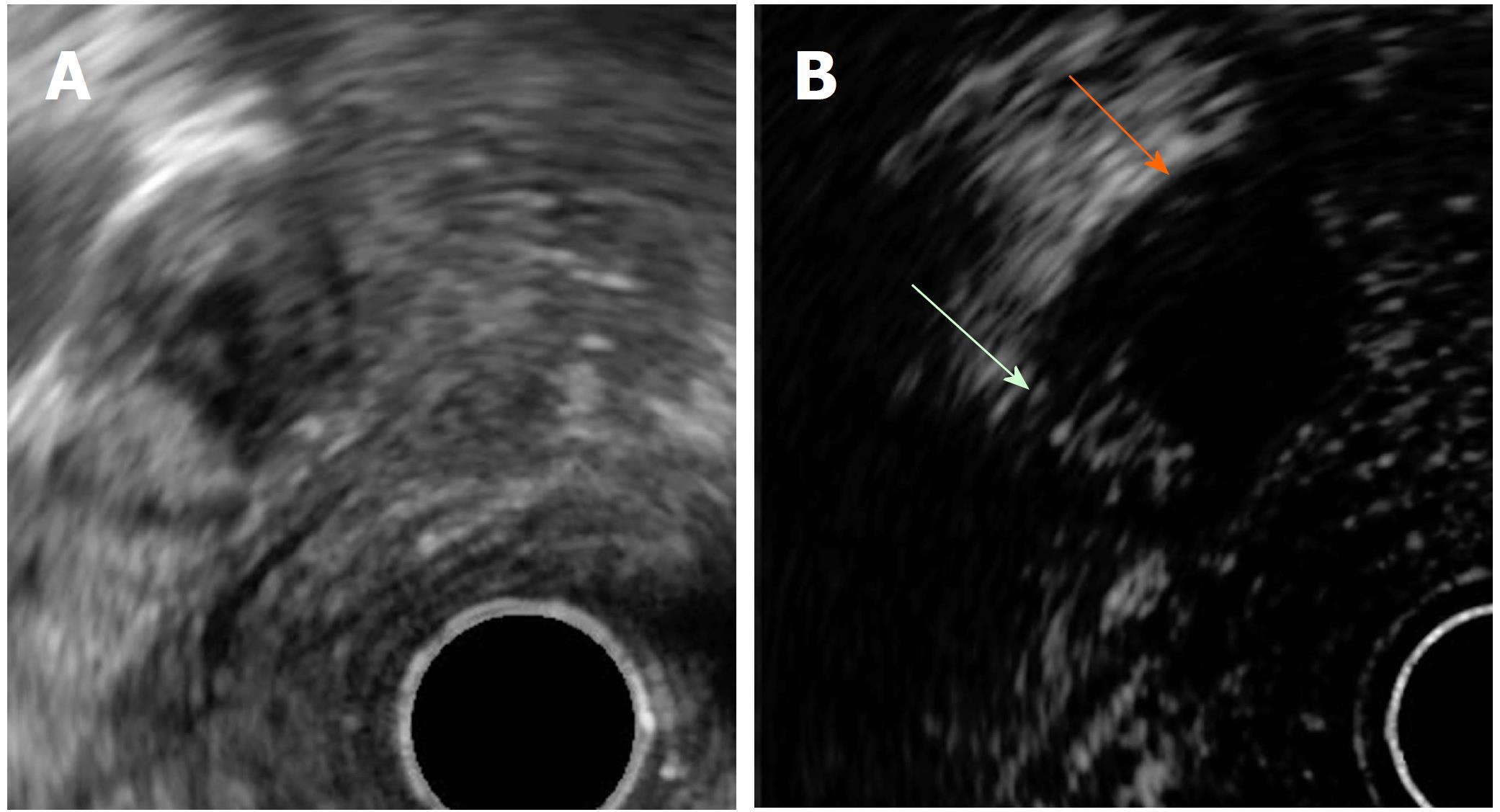
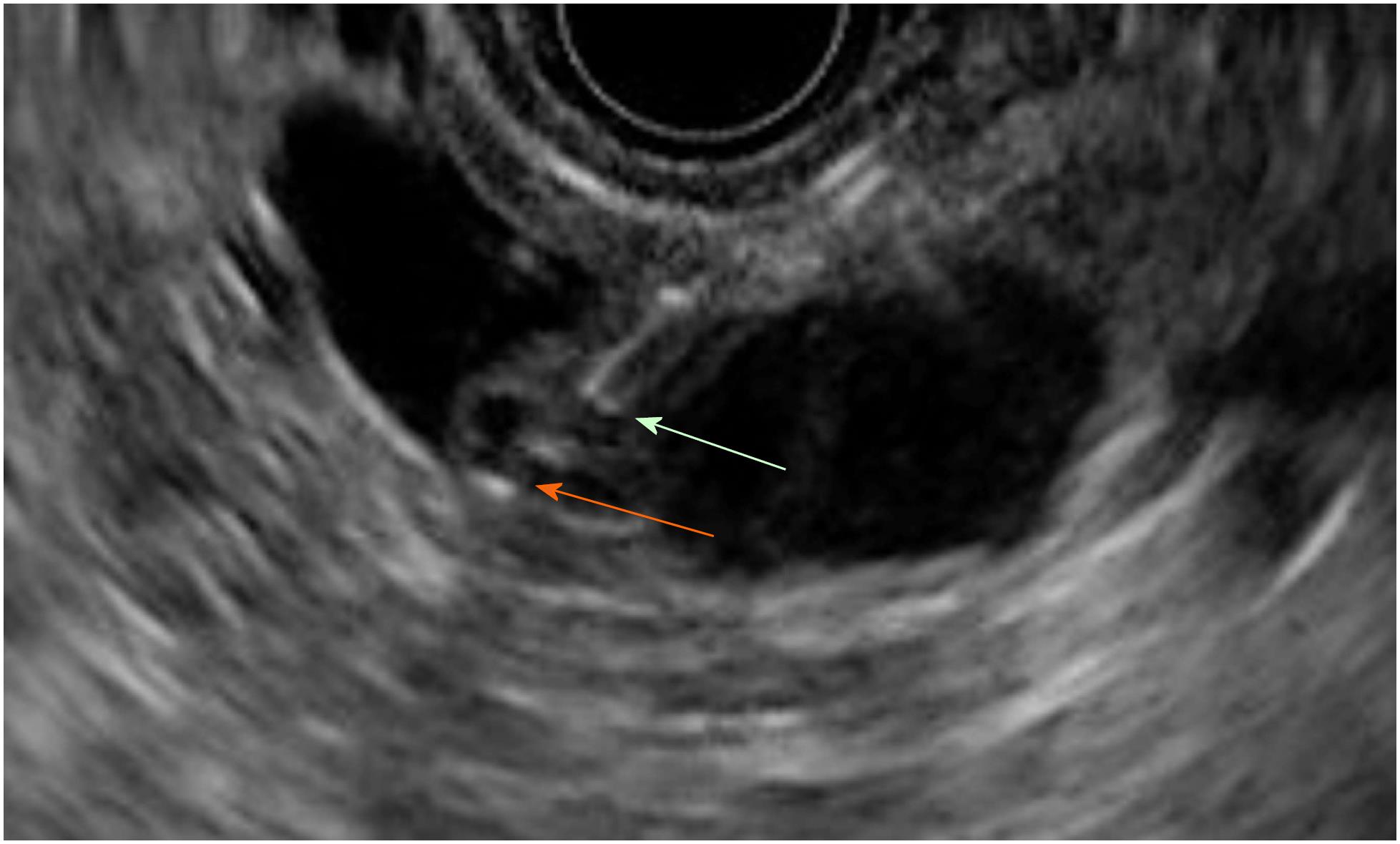
Figure 1 Mural nodule and mucus in branch duct type intraductal pancreatic mucinous neoplasms.
A: EUS B mode image. B: Contrast harmonic EUS image. Microbubbles in a mural nodule (green arrow). No bubbles in a mucus clot (orange arrow). EUS: Endoscopic ultrasonography.
Figure 2 Needle-based confocal laser endomicroscopy probe in a 19G needle.
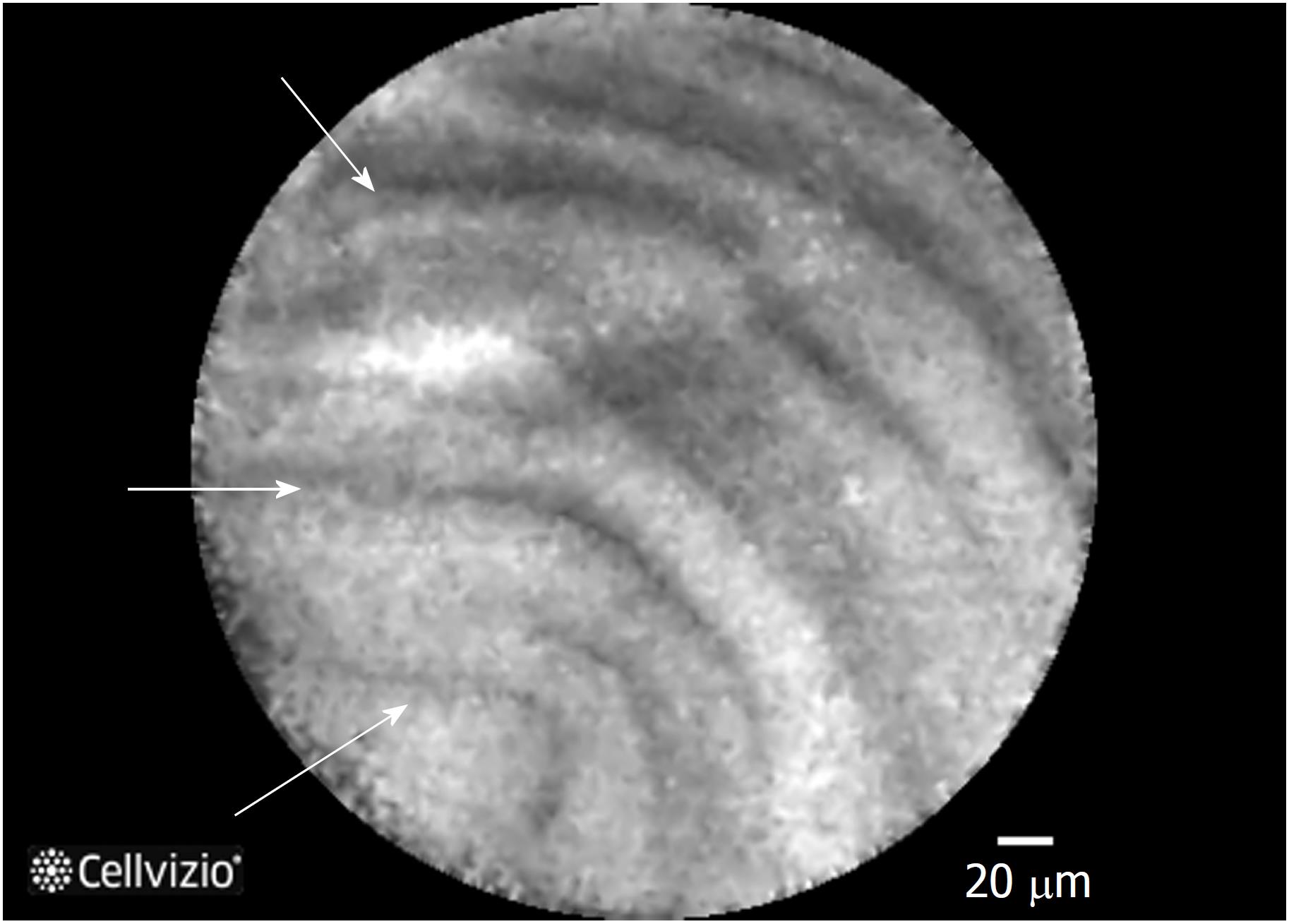
Figure 3 Needle-based confocal laser endomicroscopy image of an intraductal pancreatic mucinous neoplasms displaying multiple papillary projections.
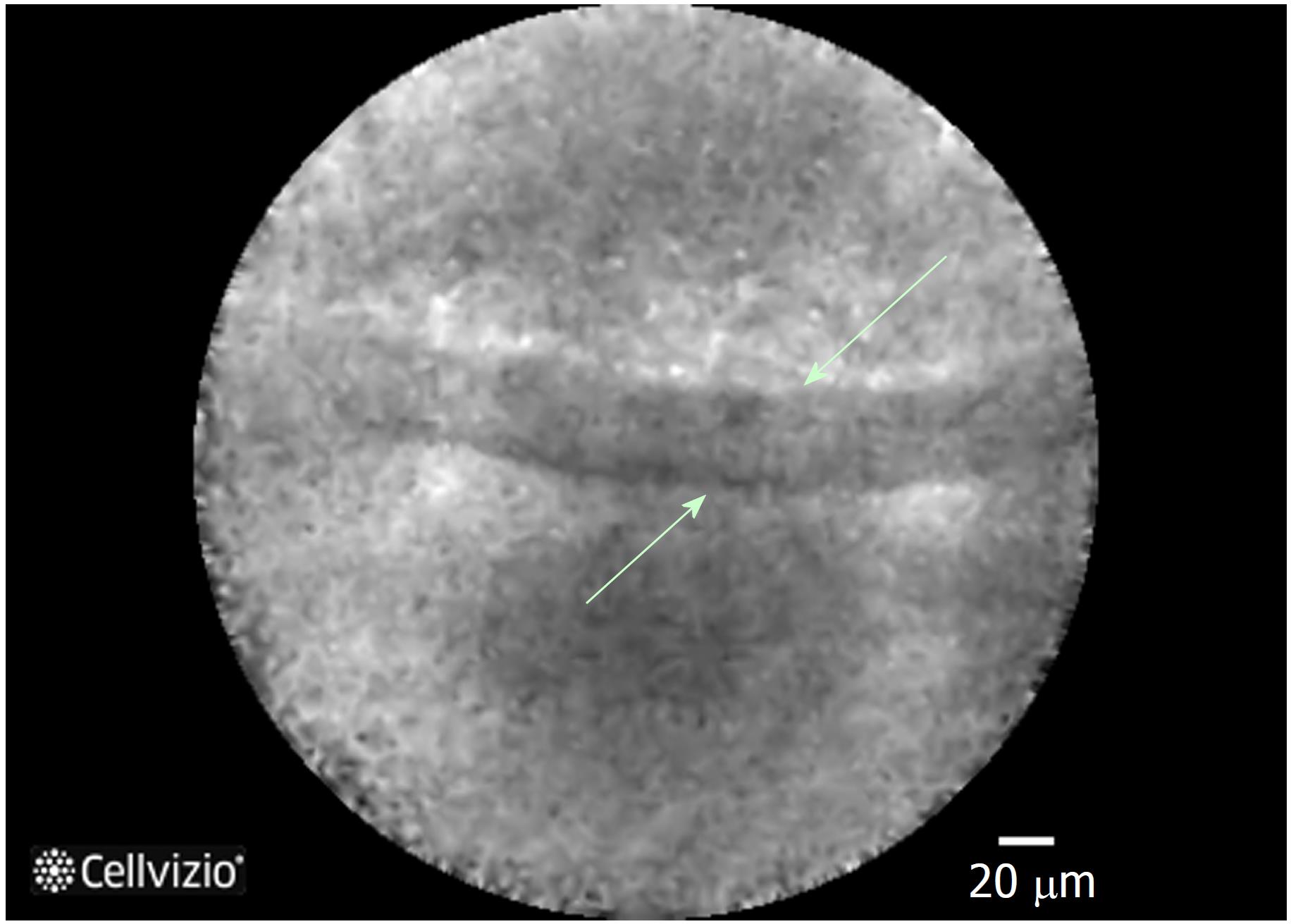
Figure 4 Needle-based confocal laser endomicroscopy image of the superficial vascular network pattern of a serous cystadenoma.
Multiple interconnected vessels (green arrows). Red cells inside displayed as black structures (orange arrow).
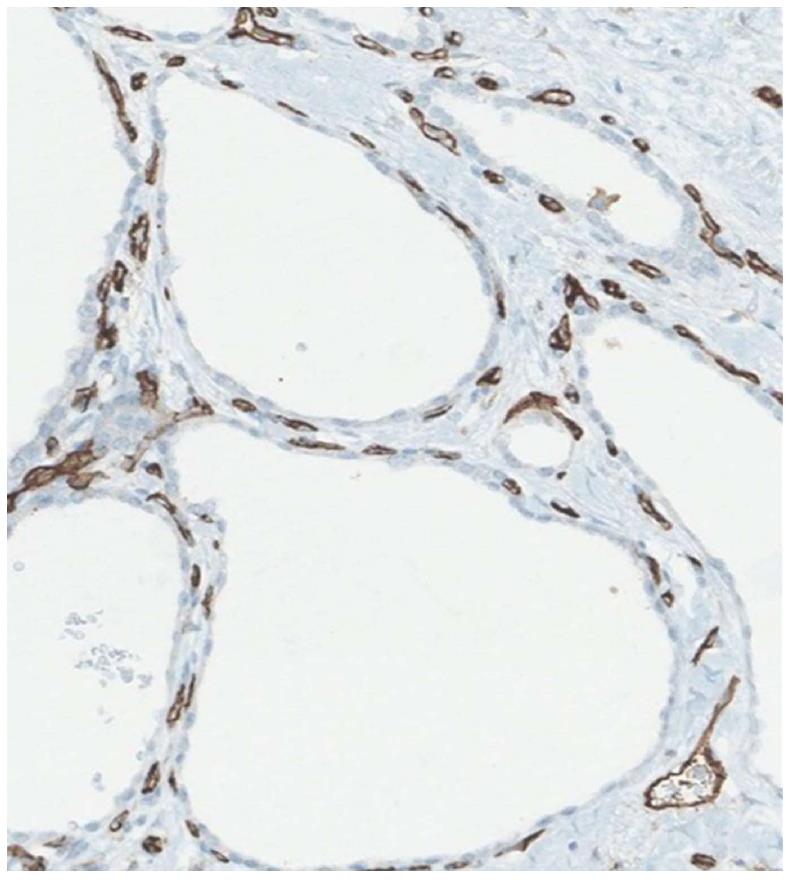
Figure 5 Staining with a vascular marker of serous cystadenomas histological specimen.
Capillary necklace with subepithelial vessels showed in brown.
Figure 6 Epithelial border image in a mucinous cystadenoma at needle-based confocal laser endomicroscopy.
Figure 7 Heterogeneous sized grey and white particles in a pseudocyst at needle-based confocal laser endomicroscopy.
Figure 8 Moray forceps.
Figure 9 Moray forceps inside a cyst.
Green arrow: The tip of the 19G needle. Orange arrow: The tip of the Moray forceps grasping the cyst wall.
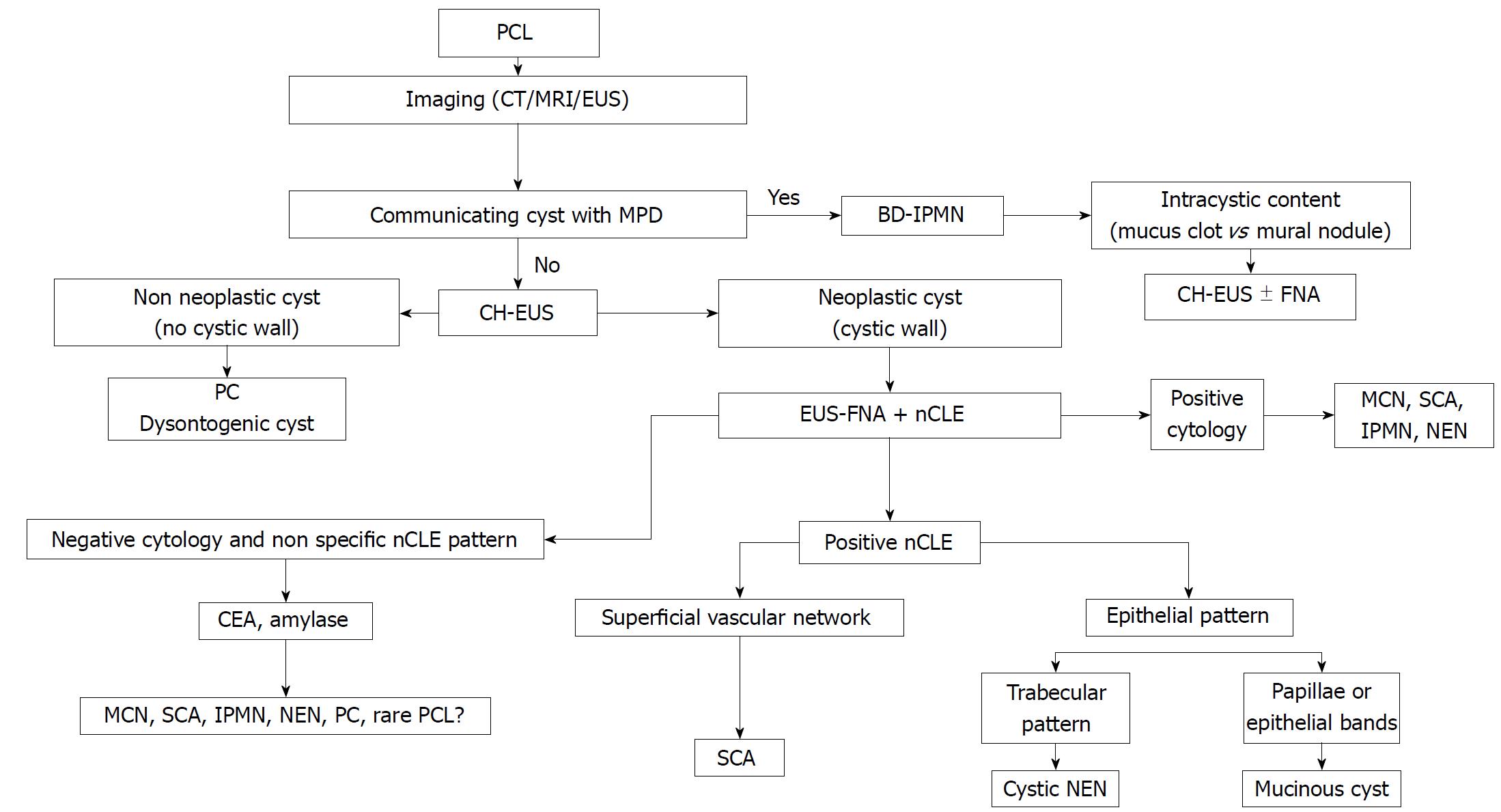
Figure 10 Diagnostic algorithm integrating new endoscopic ultrasonography-based technologies.
PCL: Pancreatic cystic lesión; PC: Pseudocyst; MPD: Main pancreatic cyst; BD-IPMN: Branch duct intraductal pancreatic mucinous neoplasm; MCN: Mucinous cystic neoplasm; SCA: Serous cystadenoma; NEN: Neuroendocrine tumour; CT: Computed tomography, MRI: Magnetic resonance imaging; EUS: Endoscopic ultrasonography; CH-EUS: Contrast harmonic enhanced EUS; EUS-FNA: EUS guided fine needle aspiration; nCLE: Needle-based confocal endomicroscopy.
- Citation: Alvarez-Sánchez MV, Napoléon B. New horizons in the endoscopic ultrasonography-based diagnosis of pancreatic cystic lesions. World J Gastroenterol 2018; 24(26): 2853-2866
- URL: https://www.wjgnet.com/1007-9327/full/v24/i26/2853.htm
- DOI: https://dx.doi.org/10.3748/wjg.v24.i26.2853