Copyright
©2010 Baishideng Publishing Group Co.
World J Gastroenterol. Oct 7, 2010; 16(37): 4709-4715
Published online Oct 7, 2010. doi: 10.3748/wjg.v16.i37.4709
Published online Oct 7, 2010. doi: 10.3748/wjg.v16.i37.4709
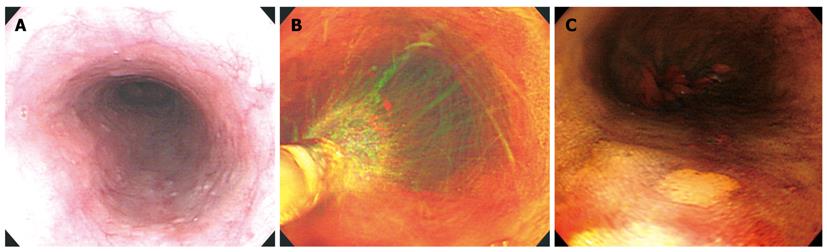
Figure 1 Screening chromoendoscopy.
A: After conventional examination using magnifying endoscope; B: 1.5% Lugol‘s solution was sprayed onto the entire esophagus; C: Iodine-unstained lesions were identified.
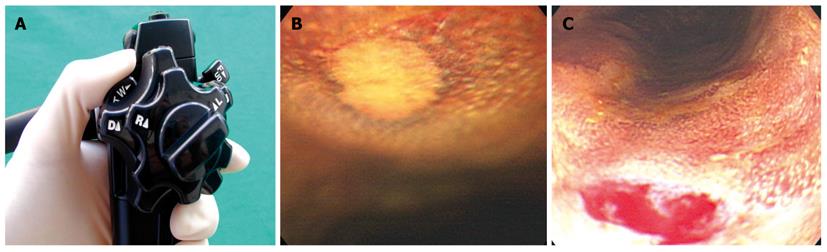
Figure 2 Magnifying endoscopy.
A and B: Magnified observations were performed on iodine-unstained lesions by pulling the zoom lever in a downward direction; C: After magnified observations, biopsy of iodine-unstained lesions was performed.
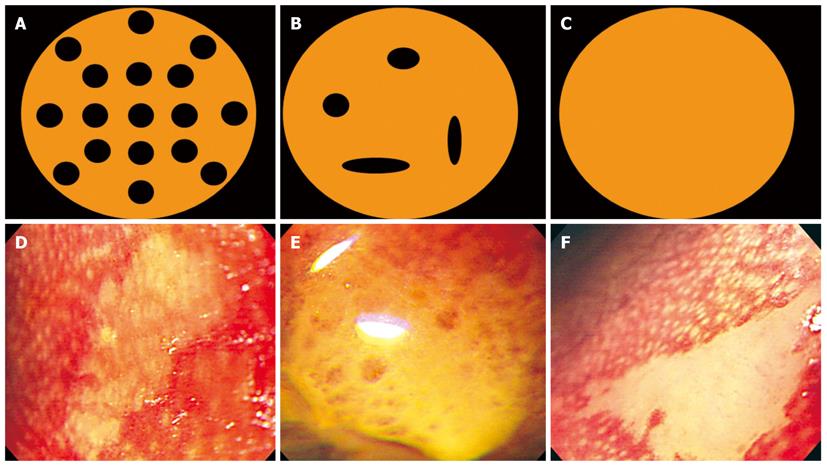
Figure 3 Type of papilla pattern.
Magnifying endoscopic findings in iodine unstained lesions were classified into the following three papilla patterns: Clear papilla pattern that showed regularly arranged white spots (Type A: A and D), fused papilla pattern that had a tendency to be fused but still had a distinguishable outline (Type B: B and E), non-visible papilla pattern that was amorphous, irregular and not stained at all (Type C: C and F).
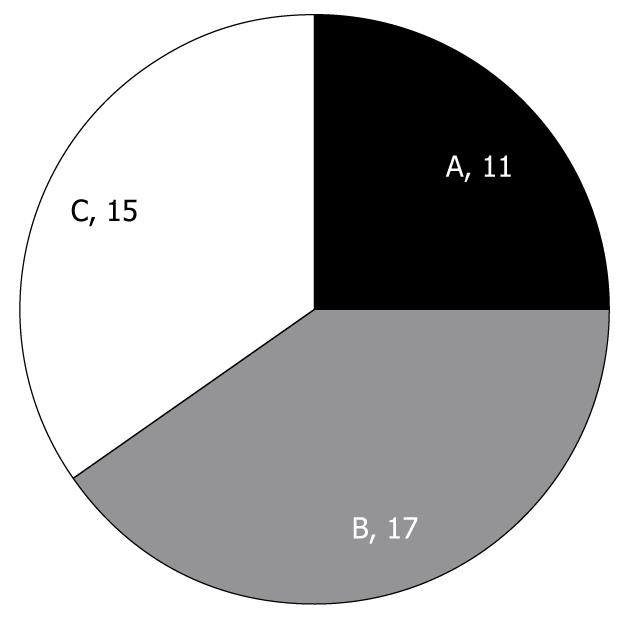
Figure 4 Distribution of types of papilla pattern on magnifying endoscopy.
Total number: 43; A: Clear papilla; B: Fused papilla; C: Non-visible papilla.
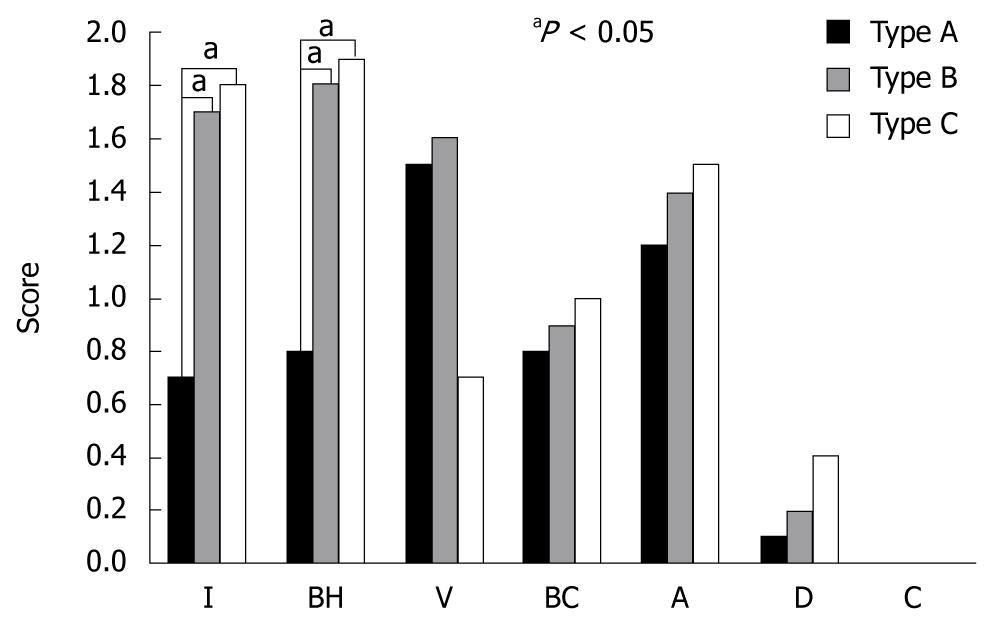
Figure 5 Relationship between types of papilla pattern and histological findings.
I: Inflammatory cell infiltration; BH: Basal cell hyperplasia; V: Vascular lake; BC: Balloon cell; A: Acanthosis; D: Dysplasia; C: Carcinoma. (All dysplasias were low-grade).
- Citation: Choi IS, Jang JY, Cho WY, Lee TH, Kim HG, Lee BY, Jeong SW, Cho JY, Lee JS, Jin SY. Usefulness of magnifying endoscopy for iodine-unstained lesions in a high-risk esophageal cancer population. World J Gastroenterol 2010; 16(37): 4709-4715
- URL: https://www.wjgnet.com/1007-9327/full/v16/i37/4709.htm
- DOI: https://dx.doi.org/10.3748/wjg.v16.i37.4709