Published online Aug 26, 2013. doi: 10.13105/wjma.v1.i2.83
Revised: July 18, 2013
Accepted: August 4, 2013
Published online: August 26, 2013
Processing time: 189 Days and 11 Hours
AIM: To determine the prevalence of hypertension in the urban and rural population of India.
METHODS: Relevant studies were identified through computer based and manual searches using MEDLINE/ PubMed, Google scholar, EMBASE, Cochrane Library and reference lists of prevalence studies from January 2000 to June 2012. A total of 12 studies were included in the meta-analysis of hypertension in urban India and 10 studies in the analysis of hypertension in rural India after applying the inclusion and exclusion criteria. Estimates of prevalence were calculated using the random effect model for meta-analysis.
RESULTS: The electronic search using appropriate keywords identified 177 titles for prevalence of hypertension in urban India, of which 165 were excluded, and 133 titles for prevalence in rural India, of which 123 were excluded after applying the inclusion criteria. Twelve studies including 125333 subjects were analyzed to assess the prevalence of hypertension in the urban Indian population, whereas ten studies including 24800 subjects were analyzed to determine the prevalence of hypertension in the rural Indian population. The prevalence of hypertension in the urban population was estimated to be 40.8% (95%CI: 40.5%-41.0%) and that of hypertension in the rural population was 17.9% (95%CI: 17.5%-18.3%). It is evident that the prevalence of hypertension is significantly higher in the urban population of India compared to the rural.
CONCLUSION: Current evidence suggests that policies and interventions should be prioritized for reduction of hypertension in the adult Indian population, especially the urban population.
Core tip: A meta-analysis of prevalence studies on hypertension in India from January 2000 to June 2012 reveals a high prevalence of hypertension in the urban (40.8%) as well as rural population (17.9%). The prevalence of hypertension is markedly higher in the urban population compared to the rural population, but the prevalence in the rural population is also a matter of concern with almost every fifth individual at risk. This is indicative of the epidemiological transition, which must raise an alarm for policy makers and health care professionals. Primordial and primary prevention of hypertension can bring about a substantial reduction in cardiovascular morbidity and mortality which occurs as a consequence of hypertension.
- Citation: Midha T, Nath B, Kumari R, Rao YK, Pandey U. Prevalence of hypertension in India: A meta-analysis. World J Meta-Anal 2013; 1(2): 83-89
- URL: https://www.wjgnet.com/2308-3840/full/v1/i2/83.htm
- DOI: https://dx.doi.org/10.13105/wjma.v1.i2.83
Globally, the overall prevalence of hypertension or raised blood pressure in adults aged 25 and above was around 40% in 2008[1]. Worldwide, hypertension is estimated to cause 7.5 million deaths, about 12.8% of the total deaths. Hypertension accounts for 57 million disability adjusted life years (DALYS) or 3.7% of total DALYS[1]. The World Health Organization (WHO) has estimated that globally about 62% of cerebrovascular diseases and 49% of ischemic heart diseases are attributable to suboptimal blood pressure (systolic > 115 mmHg), with little variation by sex[2]. One in three adults worldwide has high blood pressure. Hypertension increases the risk of heart attack, stroke, kidney failure and many other associated co morbidities. Treating raised blood pressure and maintaining it below 140/90 mmHg is associated with a reduction in cardiovascular complications[1].
The theme for World Health Day (WHD) 2013 is “high blood pressure”[3]. The goal of WHD 2013 is to reduce heart attacks and strokes. Keeping in line with the WHO-Government of India Country Cooperation Strategy, the WHD 2013 events in India are aimed at raising the awareness amongst national policymakers, program managers and other stakeholders on the need to strengthen the Indian health system to make it competent enough to respond to hypertension and related co morbidities[3].
Hypertension is a controllable disease and it has been reported that targeted reductions in people with hypertension are expected to produce large reductions in the burden of cardiovascular disease[4]. According to the seventh report of the Joint National Committee (JNC-7) on prevention, detection, evaluation and treatment of high blood pressure, adoption of healthy lifestyles by all individuals is critical for the prevention of high blood pressure[5]. Accurate estimates of hypertension are therefore necessary to plan effective control measures.
A meta-analysis showed an increase in the prevalence of hypertension in India over the years from 1%-3% in 1950 to 10%-30.9% in 2002[6]. Another cause for concern is the epidemiological transition, as it is likely that the prevalence of risk factors, and consequently the prevalence of hypertension and cardiovascular diseases, would rise with the socioeconomic development of rural areas in India.
India accounts for 17% of the world’s population, the second largest in the world, and hence it contributes largely to the statistics of any disease in the world[7]. Given the fact that hypertension is on the rise in developing countries like India, this meta-analysis was designed to consolidate the available data to find out the current prevalence of hypertension in urban and rural India.
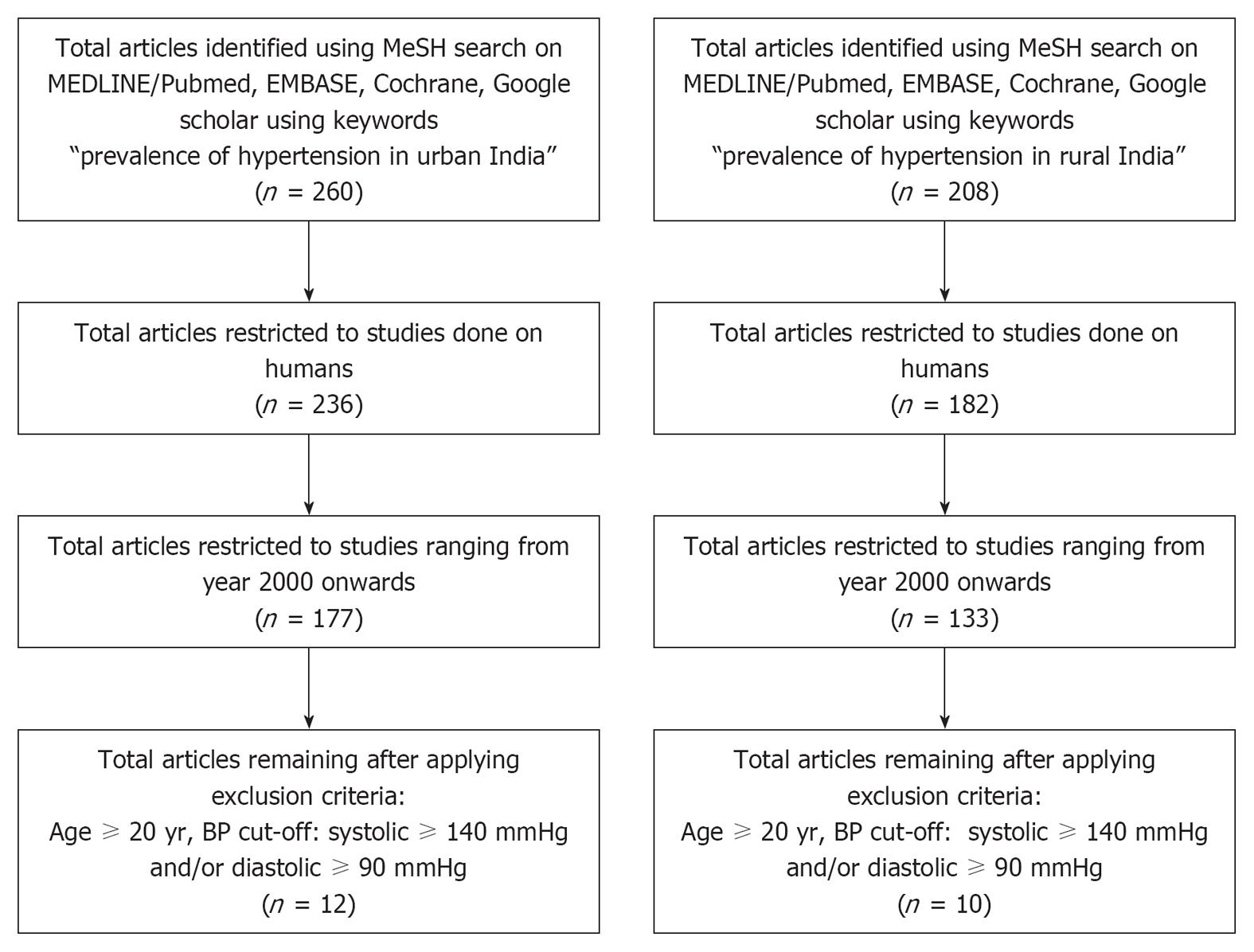
We searched MEDLINE/PubMed, Google scholar, EMBASE, Cochrane Library and reference lists of prevalence studies from January 2000 to June 2012. Internet searches used permutations of medical subject headings for prevalence studies on hypertension in India. The following keywords were looked for individually or in association: hypertension, India, prevalence, blood pressure, systolic, diastolic, mmHg. The limits included were: English for the language category and humans for the study category (Figure 1).
The studies that met all of the following criteria were included in the present meta-analysis: (1) they were prevalence studies; (2) the study design was cross-sectional; (3) the age group included in the study was 20 years and above; (4) the study was conducted in the Indian population; (5) the cut-off for classification of hypertension was systolic blood pressure ≥ 140 mmHg and/or diastolic blood pressure ≥ 90 mmHg; and (6) the study contained original data. All the studies had a cross-sectional design and blood pressure measurement on a single visit was considered. Exclusion criteria: reviews, letters to editors, case series and case-control studies were not included because of insufficient data for analysis.
Data was analyzed using the statistical software Comprehensive Meta-analysis V2. The random effect model was used to calculate the estimate of the prevalence of hypertension rather than the fixed effect model. The random effect model takes into account any heterogeneity inherent in the meta-analysis.
The electronic search in Pubmed, using the keywords “prevalence of hypertension in urban India”, identified 177 titles, of which 165 were excluded based on review of titles, abstracts and text after applying the inclusion criteria. To avoid bias due to selection criteria and blood pressure criteria used in various studies, age, blood pressure cut-off and study design criteria were taken into consideration. The remaining 12 studies were included in the analysis. Similarly, following electronic search in Pubmed, using the keywords “prevalence of hypertension in rural India”, we identified 133 titles, of which 123 were excluded based on review of titles, abstracts and text after applying the inclusion criteria. The remaining 10 were included in the analysis.
In total, 12 studies were included in the meta-analysis of hypertension in urban India and 10 studies in the analysis of hypertension in rural India.
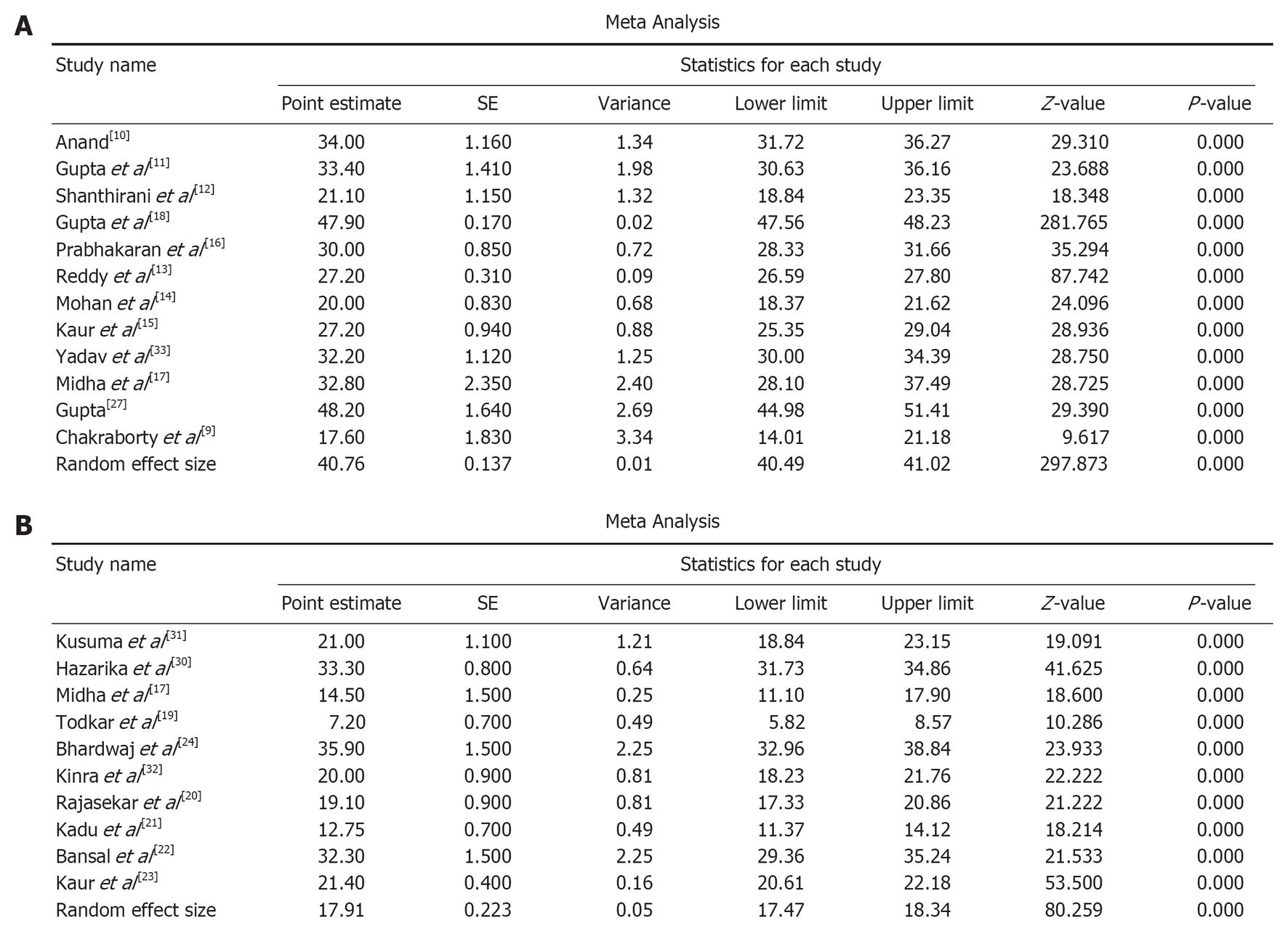
After analysis of 125333 subjects from twelve studies, the prevalence of hypertension in the urban Indian population was found to be 40.8% (95%CI: 40.5%-41.0%) (Table 1). Ten studies including 24800 subjects were analysed and the prevalence of hypertension in the rural population was estimated to be 17.9% (95%CI: 17.5%-18.3%) (Table 1). Figure 2 shows the meta-analysis of prevalence of hypertension in the urban and rural Indian population respectively. The overall prevalence rate is represented by the random effect size which was estimated to be 40.8% in urban and 17.9% in the rural population.
| First author | Place | Age group (yr) | Sample size | Prevalence |
| In the urban Indian population | ||||
| Anand[10] | Maharashtra | 30-60 | 1662 | 34.0 |
| Gupta et al[11] | Rajasthan | > 20 | 1123 | 33.4 |
| Shanthirani et al[12] | Tamil Nadu | > 20 | 1262 | 21.1 |
| Gupta et al[18] | Maharashtra | > 35 | 88653 | 47.9 |
| Prabhakaran et al[16] | Delhi | 20-59 | 2935 | 30.0 |
| Reddy et al[13] | Multi-centric | 20-69 | 19973 | 27.7 |
| Mohan et al[14] | Tamil Nadu | > 20 | 2350 | 20.0 |
| Kaur et al[15] | Tamil Nadu | 18-69 | 2262 | 27.2 |
| Yadav et al[33] | Uttar Pradesh | > 30 | 1746 | 32.2 |
| Midha et al[17] | Uttar Pradesh | > 20 | 400 | 32.8 |
| Gupta[27] | Multi-centric | 35-70 | 926 | 48.2 |
| Chakraborty et al[9] | West Bengal | 18-60 | 433 | 17.6 |
| In the rural Indian population | ||||
| Kusuma et al[31] | Andhra Pradesh | > 20 | 1316 | 21.0 |
| Hazarika et al[30] | Assam | > 30 | 3180 | 33.3 |
| Midha et al[17] | Uttar Pradesh | > 20 | 400 | 14.5 |
| Todkar et al[19] | Maharashtra | > 20 | 1297 | 7.2 |
| Bhardwaj et al[24] | Himachal Pradesh | > 18 | 1092 | 35.9 |
| Kinra et al[32] | Multi-centric | 20-69 | 1983 | 20.0 |
| Rajasekar et al[20] | Tamil Nadu | > 30 | 1905 | 19.1 |
| Kadu et al[21] | Maharashtra | > 18 | 2196 | 12.8 |
| Bansal et al[22] | Uttarakhand | > 15 | 968 | 32.3 |
| Kaur et al[23] | Tamil Nadu | 25-64 | 10463 | 21.4 |
In the present meta-analysis, the prevalence of hypertension was estimated to be 40.8% in urban and 17.9% in the rural Indian population. Gupta et al[8] reported the highest prevalence of hypertension (48.2%) in a recent multi-centric study, conducted in the urban population of India. However, Chakraborty et al[9] observed a lower prevalence of hypertension (17.6%) possibly because of the lower age group (18-60 years) and lower socioeconomic strata (slum dwellers) included in the study.
Anand[10] (34.0%), Gupta et al[11] (33.4%) and Shanthirani et al[12] (21.1%) in the early 2000s, and Reddy et al[13] (27.7%), Mohan et al[14] (20.0%), Kaur et al[15] (27.2%), Prabhakaran et al[16] (30.0%) and Midha et al[17] (32.8%) in the mid 2000s have observed that the prevalence of hypertension ranged between 20%-40% throughout the decade. However, no significant trend has been observed in the prevalence of hypertension among the studies conducted down the years. The findings of Gupta et al[18] reveal a prevalence of 47.9% from Mumbai, Maharashtra, probably because of the stressful lifestyle of subjects in a metropolitan city. The result of the meta-analysis summarizes all these findings and shows the prevalence of hypertension as 40.8% in the urban population of India.
In the rural population, the lowest prevalence (7.2%) was observed by Todkar et al[19] in Maharashtra. Midha et al[17] (14.5%), Rajasekar et al[20] (19.1%) and Kadu et al[21] (12.8%) have reported a lower prevalence compared to Bansal et al[22] (32.3%) and Kaur et al[23] (21.4%). Despite the lack of an obvious trend, the prevalence of hypertension in the rural population is rising swiftly to match up to the urban rates. Bhardwaj et al[24] reported the highest prevalence of hypertension (35.9%) in the rural population of Himachal Pradesh. The meta-analysis revealed a prevalence rate of 17.9% among the rural population.
From the available data, it is obvious that the prevalence of hypertension is higher in the urban population of India compared to the rural. No consistent trends are visible with respect to regional variations. In rural populations, the prevalence of hypertension is higher in Himachal Pradesh, while in urban studies prevalence rate is higher in Maharashtra[18,24]. The prevalence rate of hypertension was amongst the highest in metropolitan cities like Mumbai[18]. Moreover, the prevalence of hypertension in rural populations is steadily increasing and is approaching the rates of the urban population. Several studies have reported that there are significant urban-rural differences in metabolic cardiovascular risk factors[25]. Prevalence of smoking is greater in rural men while all other risk factors, such as sedentary lifestyle, obesity, central obesity, hypercholesterolemia, diabetes and the metabolic syndrome, are more common in urban men and women[26]. Most studies on urban-rural differences in cardiovascular risk factors from Haryana, Delhi, Rajasthan and Tamil Nadu have reported greater prevalence of multiple CVD risk factors in the urban population[27]. As a result, cardiovascular diseases are epidemic in the urban regions of low income countries such as India. However, greater prevalence of cardiovascular risk factors in urban areas in India is in contrast to high income countries where the CVD risk factors are equal in urban and rural areas[28]. Similarly, it has been observed that in the more developed states of India, such as Kerala, the rural-urban differences in cardiometabolic risk factors have largely disappeared and the risk factors are equal or slightly greater in the rural population[29]. Hazarika et al[30] reported that even in the rural population of Assam, body mass index and waist-hip ratio were significant risk factors of hypertension. Kusuma et al[31] confirmed the hypothesis that acculturation/modernization may elevate the risk of hypertension and that prevalence is generally low among traditional population groups. Kinra et al[32] suggested that a nutrition transition (coexistence of over-nutrition and under-nutrition) may have progressed to some parts of rural India. He observed that obesity, dyslipidemia, diabetes and hypertension were more prevalent in higher socioeconomic groups in the rural areas. This epidemiological transition is a cause for serious concern as it is likely that the prevalence of risk factors, and thereby the prevalence of hypertension and cardiovascular diseases, would rise with the socioeconomic development of rural areas.
Yadav et al[33] observed that there was a high prevalence of cardiovascular risk factors in the general population [central obesity (86.7%), elevated LDL cholesterol (22.8%), abnormal glucose tolerance (41.6%) and smoking (20.3% of males)]. Two or more of the cardiovascular risk factors were present in a higher proportion of hypertensives (66%, OR = 3.0, P < 0.0001) and pre-hypertensives, (56%, OR = 2.0, P < 0.0001) compared to normotensive subjects (39%). The current rate of hypertension in the urban areas and the rising trend in the rural population is a warning to institute lifestyle changes in the community in order to put a halt to the increasing rates.
The high prevalence of hypertension in the urban and rural population in India presents a formidable challenge to the Indian health system. In countries like India, the out-of-pocket expenditures incurred for non-communicable diseases (NCDs) like hypertension are high, which hits the impoverished households the most. Medicines for these chronic diseases account for a large portion of expenditure. Therefore, population based prevention strategies have a high impact and are cost-effective as these target lifestyle change. Interventions utilizing the power of public policies for reducing salt, fat, sugar and alcohol intake through regulatory and consumer education approaches; increasing physical activity through sound urban planning and creation of activity-promoting environments; increasing fruit and vegetable intake through appropriate agricultural and pricing mechanisms; and implementing comprehensive tobacco control have the potential to prevent a large proportion of disease events in the whole population[34].
Hypertension is easily diagnosable and treatable with lifestyle modifications and effective medicines. Furthermore, hypertension control provides an entry point to deal with other NCDs as any intervention will help to concomitantly address other NCDs as well. This has been taken into cognizance in the newly launched National Programme for Prevention and Control of Cancer, Diabetes, Cardiovascular Diseases and Stroke (NPCDCS), which has hypertension and diabetes as the main focus areas[34]. National strategies will focus on prevention and health promotion as the key to reduce disease burden. Health education programs that promote exercise, weight reduction, early diagnosis and screening are some of the key interventions that will be promoted at various levels of heath facilities[35]. Under the NPCDCS, the strategy for early diagnosis of chronic NCDs will consist of opportunistic screening of persons above the age of 30 years at the point of primary contact with any health care facility[35]. The NCD clinics mandated under NPCDCS could be leveraged to facilitate guidelines based hypertension management with emphasis on generic drugs and those recommended by the Indian Public Health Standards[34].
In conclusion, the high prevalence of hypertension in the urban population and a rising prevalence in the rural population must raise an alarm for policy makers and health care professionals as this is an area where primordial and primary prevention measures can bring about a substantial reduction in cardiovascular morbidity and mortality in the future.
Given the limited amount of data available on the prevalence of hypertension in India, studies conducted in subjects with different bio-social characteristics have been included in the meta-analysis. Nevertheless, the pooled estimate does provide an overview of the magnitude of the problem of hypertension in the Indian population.
The overall prevalence of hypertension in adults aged 25 and over was around 40% in the world in 2008 and a meta-analysis estimated a prevalence of 10-30.9% in India in 2002. This shift in epidemiological profile presents a unique challenge to India’s health system as rates of cardiovascular and metabolic disease like hypertension and diabetes, obesity and cancer rise, tuberculosis, diarrheal disease and water borne illnesses remain widespread. According to a 2012 World Health Organization report, non communicable diseases are responsible for two-thirds of the total morbidity burden and about 53% of total deaths in India. Hypertension provides an entry point to other non-communicable diseases. Therefore, a precise estimate of the prevalence of hypertension in the urban and rural population of the India is required to assess the magnitude of the problem that has to be addressed.
Very few studies are available on the prevalence of hypertension in India. A consolidated estimate of hypertension from various studies conducted in different regions of the country can aid the development of preventive strategies. The difference in prevalence between the urban and rural population has also been studied to provide an insight to the kind of preventive and promotive services required.
It is possible that an insight into the magnitude of the problem of hypertension can help in shaping the preventive programs and policies specific for the rural and urban population.
Very few multi-centric studies are available in India; therefore, the main application of this meta-analysis is to consolidate the available data to determine the burden of hypertension in country.
A meta-analysis integrates the quantitative findings from separate but similar studies and provides a numerical estimate of the overall effect of interest. Different weights are assigned to the different studies for calculating the summary or pooled effect. The weighting is related with the inverse of the standard error (and therefore indirectly to the sample size) reported in the studies. Studies with smaller standard error and larger sample size are given more weight in the calculation of the pooled effect size. The meta-analysis table lists the prevalence of hypertension (expressed as a percentage), with their 95%CI found in the individual studies included in the meta-analysis. The pooled proportion (prevalence) with 95%CI is given for the random effects model. The random effects model will tend to give a more conservative estimate (i.e., with wider confidence interval), but the results are more valid as they take into account any inherent heterogeneity. Under the random effects model, the true effects in the studies are assumed to vary between studies and the summary effect is the weighted average of the effects reported in the different studies.
This manuscript is a meta-analysis on the prevalence of hypertension in India. Its results have provided evidence for policies and interventions for hypertension. It is well written.
P- Reviewers Bergese SD, Tan XR S- Editor Wen LL L- Editor Roemmele A E- Editor Zheng XM
| 1. | World Health Organization. Global Health Repository. Available from: http://www.who.int/gho/ncd/risk_factors/blood_pressure_prevalence_text/en/index.html. Last accessed April 24, 2013. |
| 2. | World Health Report-2002. Reducing Risks, Promoting Healthy Life. Chapter 4, p-12. Available from: http://www.who.int/whr/2002/en/whr02_ch4.pdf. Last accessed April 24, 2013. |
| 3. | Available from: http://www.who.int/world-health-day/en/. Last accessed April 24, 2013. |
| 4. | Rodgers A, Lawes C, MacMahon S. Reducing the global burden of blood pressure-related cardiovascular disease. J Hypertens Suppl. 2000;18:S3-S6. [PubMed] |
| 5. | Chobanian AV, Bakris GL, Black HR, Cushman WC, Green LA, Izzo JL, Jones DW, Materson BJ, Oparil S, Wright JT. The Seventh Report of the Joint National Committee on Prevention, Detection, Evaluation, and Treatment of High Blood Pressure: the JNC 7 report. JAMA. 2003;289:2560-2572. [PubMed] |
| 6. | Padmavati S. Prevention of heart disease in India in the 21st century: need for a concerted effort. Indian Heart J. 2002;54:99-102. [PubMed] |
| 7. | World Development Report-2006. Equity and Development. A co-publication of the World Bank and Oxford University Press. . |
| 8. | Gupta R, Pandey RM, Misra A, Agrawal A, Misra P, Dey S, Rao S, Menon VU, Kamalamma N, Vasantha Devi KP. High prevalence and low awareness, treatment and control of hypertension in Asian Indian women. J Hum Hypertens. 2012;26:585-593. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 27] [Cited by in RCA: 32] [Article Influence: 2.3] [Reference Citation Analysis (0)] |
| 9. | Chakraborty R, Bose K, Kozieł S. Waist circumference in determining obesity and hypertension among 18-60 years old Bengalee Hindu male slum dwellers in Eastern India. Ann Hum Biol. 2011;38:669-675. [PubMed] |
| 10. | Anand MP. Prevalence of hypertension amongst Mumbai executives. J Assoc Physicians India. 2000;48:1200-1201. [PubMed] |
| 11. | Gupta R, Gupta VP, Sarna M, Bhatnagar S, Thanvi J, Sharma V, Singh AK, Gupta JB, Kaul V. Prevalence of coronary heart disease and risk factors in an urban Indian population: Jaipur Heart Watch-2. Indian Heart J. 2002;54:59-66. [PubMed] |
| 12. | Shanthirani CS, Pradeepa R, Deepa R, Premalatha G, Saroja R, Mohan V. Prevalence and risk factors of hypertension in a selected South Indian population--the Chennai Urban Population Study. J Assoc Physicians India. 2003;51:20-27. [PubMed] |
| 13. | Reddy KS, Prabhakaran D, Chaturvedi V, Jeemon P, Thankappan KR, Ramakrishnan L, Mohan BV, Pandav CS, Ahmed FU, Joshi PP. Methods for establishing a surveillance system for cardiovascular diseases in Indian industrial populations. Bull World Health Organ. 2006;84:461-469. [PubMed] |
| 14. | Mohan V, Deepa M, Farooq S, Datta M, Deepa R. Prevalence, awareness and control of hypertension in Chennai--The Chennai Urban Rural Epidemiology Study (CURES-52). J Assoc Physicians India. 2007;55:326-332. [PubMed] |
| 15. | Kaur P, Rao TV, Sankarasubbaiyan S, Narayanan AM, Ezhil R, Rao SR, Gupte MD. Prevalence and distribution of cardiovascular risk factors in an urban industrial population in south India: a cross-sectional study. J Assoc Physicians India. 2007;55:771-776. [PubMed] |
| 16. | Prabhakaran D, Shah P, Chaturvedi V, Ramakrishnan L, Manhapra A, Reddy KS. Cardiovascular risk factor prevalence among men in a large industry of northern India. Natl Med J India. 2005;18:59-65. [PubMed] |
| 17. | Midha T, Idris MZ, Saran RK, Srivastav AK, Singh SK. Prevalence and determinants of hypertension in the urban and rural population of a north Indian district. East Afr J Public Health. 2009;6:268-273. [PubMed] |
| 18. | Gupta PC, Gupta R, Pednekar MS. Hypertension prevalence and blood pressure trends in 88 653 subjects in Mumbai, India. J Hum Hypertens. 2004;18:907-910. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 29] [Cited by in RCA: 29] [Article Influence: 1.5] [Reference Citation Analysis (1)] |
| 19. | Todkar SS, Gujarathi VV, Tapare VS. Period prevalence and sociodemographic factors of hypertension in rural maharashtra: a cross-sectional study. Indian J Community Med. 2009;34:183-187. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 27] [Cited by in RCA: 26] [Article Influence: 1.6] [Reference Citation Analysis (0)] |
| 20. | Rajasekar VD, Krishnagopal L, Mittal A, Singh Z, Purty AJ, Binu VS, Iillayabharathi V. Prevalence and risk factors for hypertension in a rural area of Tamil Nadu, South India. Indian J Med Spec. 2012;3:12-17. [RCA] [DOI] [Full Text] [Cited by in Crossref: 2] [Cited by in RCA: 3] [Article Influence: 0.2] [Reference Citation Analysis (0)] |
| 21. | Kadu AV, Mane SS, Lakde RN, Vedpathak VL, Gaikwad AE, Choudhari SG. Prevalence of Hypertension in the Rural Community of Central Maharashtra, India. Int J Med Public Health. 2012;2; 39-45. |
| 22. | Bansal SK, Saxena V, Kandpal SD, Gray WK, Walker RW, Goel D. The prevalence of hypertension and hypertension risk factors in a rural Indian community: A prospective door-to-door study. J Cardiovasc Dis Res. 2012;3:117-123. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 31] [Cited by in RCA: 40] [Article Influence: 3.1] [Reference Citation Analysis (0)] |
| 23. | Kaur P, Rao SR, Radhakrishnan E, Rajasekar D, Gupte MD. Prevalence, awareness, treatment, control and risk factors for hypertension in a rural population in South India. Int J Public Health. 2012;57:87-94. [PubMed] |
| 24. | Bhardwaj R, Kandori A, Marwah R, Vaidya P, Singh B, Dhiman P, Sharma A. Prevalence, awareness and control of hypertension in rural communities of Himachal Pradesh. J Assoc Physicians India. 2010;58:423-424, 429. [PubMed] |
| 25. | Gupta R, Joshi P, Mohan V, Reddy KS, Yusuf S. Epidemiology and causation of coronary heart disease and stroke in India. Heart. 2008;94:16-26. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 208] [Cited by in RCA: 223] [Article Influence: 13.1] [Reference Citation Analysis (0)] |
| 26. | Gupta R, Gupta VP. Urban-rural differences in coronary risk factors do not fully explain greater urban coronary heart disease prevalence. J Assoc Physicians India. 1997;45:683-686. |
| 27. | Gupta R. Epidemiology and regional variations in cardiovascular disease and risk factors in India. J Prev Cardiol. 2011;1:7-15. |
| 28. | Stuckler D. Population causes and consequences of leading chronic diseases: a comparative analysis of prevailing explanations. Milbank Q. 2008;86:273-326. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 117] [Cited by in RCA: 110] [Article Influence: 6.5] [Reference Citation Analysis (0)] |
| 29. | Thankappan KR, Shah B, Mathur P, Sarma PS, Srinivas G, Mini GK, Daivadanam M, Soman B, Vasan RS. Risk factor profile for chronic non-communicable diseases: results of a community-based study in Kerala, India. Indian J Med Res. 2010;131:53-63. [PubMed] |
| 30. | Hazarika NC, Narain K, Biswas D, Kalita HC, Mahanta J. Hypertension in the native rural population of Assam. Natl Med J India. 2004;17:300-304. [PubMed] |
| 31. | Kusuma YS, Babu BV, Naidu JM. Prevalence of hypertension in some cross-cultural populations of Visakhapatnam district, South India. Ethn Dis. 2004;14:250-259. [PubMed] |
| 32. | Kinra S, Bowen LJ, Lyngdoh T, Prabhakaran D, Reddy KS, Ramakrishnan L, Gupta R, Bharathi AV, Vaz M, Kurpad AV. Sociodemographic patterning of non-communicable disease risk factors in rural India: a cross sectional study. BMJ. 2010;341:c4974. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 133] [Cited by in RCA: 137] [Article Influence: 9.1] [Reference Citation Analysis (0)] |
| 33. | Yadav S, Boddula R, Genitta G, Bhatia V, Bansal B, Kongara S, Julka S, Kumar A, Singh HK, Ramesh V. Prevalence & risk factors of pre-hypertension & hypertension in an affluent north Indian population. Indian J Med Res. 2008;128:712-720. [PubMed] |
| 34. | Mohan S, Campbell N, Chockalingam A. Time to effectively address hypertension in India. Indian J Med Res. 2013;137:627-631. [PubMed] |
| 35. | Operational guidelines. National programme for prevention and control of cancer, diabetes, cardiovascular diseases and stroke (NPCDCS). Directorate General of Health Services.Ministry of Health and Family Welfare. Government of India. Available from: http://health.bih.nic.in/Docs/Guidelines/Guidelines-NPCDCS.pdf. Last accessed August 2013. |