Published online May 23, 2015. doi: 10.5494/wjh.v5.i2.85
Peer-review started: September 28, 2014
First decision: December 17, 2014
Revised: January 8, 2015
Accepted: January 30, 2015
Article in press: February 2, 2015
Published online: May 23, 2015
Hypertension is an increasing health problem worldwide especially among the elderly. Its therapeutical importance is indicated by the caused organ damages like hypertensive heart disease (HHD) and heart failure with the subsequent higher morbidity and mortality in the population. In HHD ventricular hypertrophy develops as a compensatory mechanism for pressure overload but as the left ventricular compliance decreases, the process can transform into heart failure with firstly preserved and then into reduced ejection fraction (HFpEF, HFrEF). The main characteristics of underlying mechanisms involve cardiomyocyte growth, vessel changes, increased collagen production in all of which several mechanical stress induced neurohumoral agents, signal transduction pathways are involved. According to the new ESC and AHA guidelines five main groups of antihypertensive agents can be applied for decreasing blood pressure and for the prevention of organ damages. Occasionally, patients are not able to tolerate antihypertensive medication because of side effects, drug intolerance or interactions thus it is more difficult to reach the target blood pressure values. Therefore there are several efforts to complete the existing therapeutical possibilities against the development of organ damages like inhibition of Rho/ROCK pathway (e.g., statins), regulation of ROS formation, influence on mitochondrial biogenesis and enhancing recombinant adenovirus hepatocyte growth factor gene. Hypertension induced oxidative stress causes DNA breaks producing the activation of nuclear poly(ADP-ribose) polymerase-1 (PARP) enzyme that leads to energy depletion and unfavorable modulation of different kinase cascades. PARP activation promotes the development of HHD, and its transition to heart failure. Therefore inhibition of PARP-enzyme offers another new therapeutical approach among hypertensive patients. The purpose of this review is to give a comprehensive summary about the most significant mechanisms in HHD and an insight into new potential therapies.
Core tip: There is numerous literature dealing with hypertensive heart disease and its therapeutical opportunities. In our work we have tried to combine clinical aspects with experimental data, which represent the future scope of the therapeutical opportunities in the prevention of organ damages not only via antihypertensive effect.
- Citation: Magyar K, Gal R, Riba A, Habon T, Halmosi R, Toth K. From hypertension to heart failure. World J Hypertens 2015; 5(2): 85-92
- URL: https://www.wjgnet.com/2220-3168/full/v5/i2/85.htm
- DOI: https://dx.doi.org/10.5494/wjh.v5.i2.85
Hypertension is a major public health problem associated with high cardiovascular morbidity and mortality. Generally the prevalence of high blood pressure appears to be around 30%-45% in the whole population, which shows a higher prevalence with ageing. In case of adults, hypertension is defined as a systolic blood pressure of at least 140 mmHg and a diastolic of 90 mmHg according to the various guidelines (e.g., the new ESH/ESC guideline). However, there are some subgroups of patients in whom the goal blood pressure is different. For instance, the elderly can benefit from lowering systolic blood pressure only to between 140 and 150 mmHg. In diabetic patients, however, the target blood pressure is lower than in the general population. In these patients the diastolic blood pressure should be less than 85 mmHg. According to the concept of J-curve hypothesis, it can be harmful to reduce both systolic and diastolic blood pressure to markedly low values.
Hypertension is an important risk factor of cardiovascular diseases, stroke, renal disease and peripherial artery disease[1]. According to epidemiological data, hypertensive heart disease (HHD) is one of the most important hypertensive organ damage. The most common consequences of HHD are heart failure, ischemic heart disease and arrhythmias. The Framingham Heart Study showed that 20 mmHg elevation of systolic blood pressure is associated with 50% increased risk of heart failure[2]. Hypertension is of course not the sole factor contributing to the development of heart failure but multi-variate analysis using time-dependent modelling revealed that myocardial infarction conferred the greatest risk of developing heart failure. As a consequence of its high prevalence, hypertension carried the greatest population-attributable risk[3]. Thus blood pressure lowering (antihypertensive therapy) markedly reduces the incidence of major cardiovascular (CV) events like HHD and heart failure[4].
Registries proved that nearly half of the patients with heart failure have a preserved ejection fraction (HfpEF). HFpEF is most common among the elderly, women and patients with left ventricular hypertrophy[5].
Hypertensive heart disease encompasses a wide spectrum including asymptomatic cardiac hypertrophy and clinical heart failure (with either preserved or reduced ejection fraction). Elevated blood pressure changes the structure and function of blood vessels and left ventricle. These alterations are also known as remodeling, which is an adaptive mechanism in response to long-term changes in hemodynamic conditions, but it may also subsequently contribute to the pathophysiology of circulatory disorders[6,7].
Alterations in left ventricle, for instance hypertrophy and ischemia, predispose to heart failure in hypertensive patients. Cardiac hypertrophy is an adaptive response, a compensatory mechanism to pressure or volume overload directing to the attenuation of wall tension and the maintenance of cardiac output. The left ventricle mass can increase either as a result of wall thickening or ventricular dilation. The relative wall thickness (the ratio of the left ventricular wall thickness to diastolic diameter) determines the type of hypertrophy (eccentric or concentric). It is influenced by the type of overload (pressure or volume), by the neurohormonal activation (plasma renin level), extracellular matrix changes, concomitant diseases (coronary artery disease, diabetes mellitus, obesity), demographic and genetic factors (e.g., ACE gene polymorphism)[7,8].
Sustained hypertrophy is often the initial step towards the progression of congestive heart failure[7].
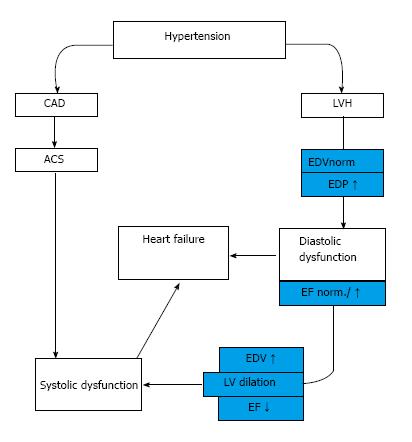
It is now well known that symptomatic heart failure can occur either in the setting of reduced (HFrEF) or preserved ejection fraction (HFpEF)[9]. The classic course of HHD progression is a so-called “burned-out” of left ventricle in which hypertension leads to concentric hypertrophy followed by diastolic and finally systolic insufficiency[10].
In an other group of hypertensive patients the development of myocardial infarction causes directly systolic heart failure (HFrEF) independently from hypertrophy[8] (Figure 1).
High blood pressure caused alterations in cardiac structure and function, eventually resulting in impaired myocardial performance, coronary haemodynamics and apoptosis.
It has been well established that pathogenesis of HHD involves all components of the heart, including myocytes and non-myocytic cells, such as fibroblasts and endothelial cells, extracellular matrix proteins, fibrillar collagen, and coronary vessels[11].
Structural remodeling of HHD is characterized by enlarged cardiac myocytes with altered energy metabolism, fibroblast proliferation and activation, fibroblast-myofibroblast transformation and excessive collagen deposition, which all lead to a more rigid myocardium[12,13]. Coronary resistance vessels are also affected, perivascular fibrosis of intramyocardial coronary arteries and arterioles produce intimal-medial thickening[14].
The remodeling and growth regulation of the heart involve several mechanisms including neurogenic, humoral, autocrine and paracrine factors.
The activation of renin-angiotensin-aldosterone system (RAAS) is one of the most important processes, which contribute to the development of hypertension including vasoconstriction, generation of reactive oxygen species (ROS), vascular inflammation, vascular and cardiac remodeling (hypertrophy and fibrosis). Therefore the RAAS system plays a prominent part in accelerating hypertensive organ damages[15,16]. Moreover angiotensin converting enzyme (ACE) is responsible for the production of angiotensin II (Ang II), which correlates to left ventricle hypertrophy. Individuals have different plasma ACE concentrations due to the insertion/deletion polymorphism of ACE gene, which also shows a close relationship to ventricular hypertrophy[12].
Mineralocorticoids have a physiological role in volume regulation, but they also activate the sympathetic nervous system (SNS), which results in baroreceptor dysfunction, impaired arterial compliance and marked myocardial and vascular fibrosis[17].
The sympathetic hyperactivity rises blood pressure directly (even without RAAS activation), possesses metabolic effects (e.g., insulin resistance) and facilitates the development of LVH.
It has been well established that pathogenesis of cardiac remodeling is also associated with insulin resistance, increased activity of insulin-like growth factor-1 and myocardial pro-fibrotic matricellular protein osteopontin, thyroid hormons and the elevated level of brain and atrial natriuretic peptides[12].
It is well known that hypertension induced oxidative stress plays an important role in the development of cardiac injury. Potential sources of ROS are the NADPH oxidases, nitric oxide synthase, lipoxygenases, cyclo-oxygenases, xanthine oxidase, cytochrome P450 enzymes, and the mitochondrial respiratory chain[18]. ROS mediated damages are implicated in endothelial dysfunction, inflammation, hypertrophy, apoptosis, cell migration, fibrosis and angiogenesis[19]. ROS impair the function of ion-channels and decrease the amount of high energy phosphates. These changes can result in alterations of myocyte and smooth muscle cell calcium homeostasis leading to increased cell proliferation[20]. Oxidative stress can lead to single stranded DNA breaks and changes in signaling pathways evolving alterations in LV structural and mechanical properties[21].
The single stranded DNA breaks provoke the activation of nuclear poly(ADP-ribose) polymerase-1 (PARP) enzyme, which can decrease the cellular NAD+ and ATP pools leading to energy depletion with inadequate glycolysis and mitochondrial respiration, promoting apoptotic or necrotic cell death[21-25].
The activation of PARP-enzyme has a central role in the pathophysiology of several cardiovascular diseases including the development of HHD, transition of HHD to HF by influencing collagen production via modulation of different kinase cascades[21,22]. Cellular adaptations of the heart are typically initiated by stress responsive signaling pathways, which serve as central transducers of cardiac hypertrophic growth and/or ventricular dilation.
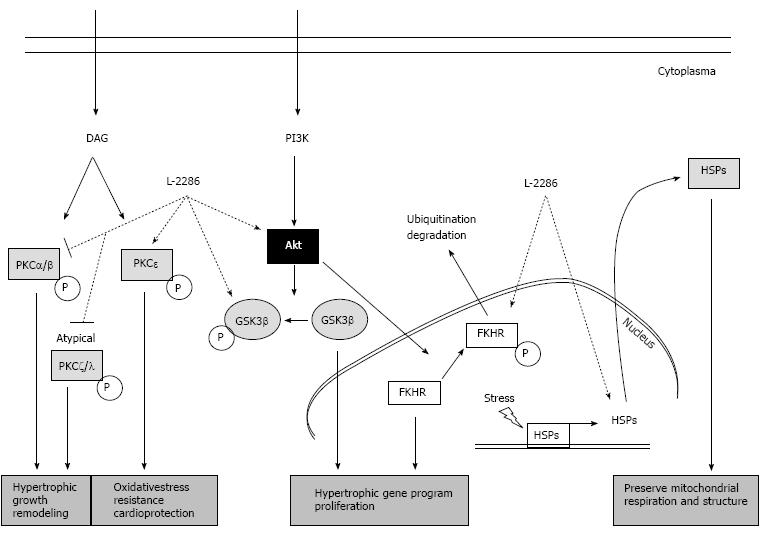
These signaling pathways include extracellular signal-regulated protein kinases (ERK), p38 mitogen-activated protein kinases (p38-MAPK), c-Jun NH2-terminal kinases (JNK), several protein kinase C (e.g., PKC delta and epsilon) isoforms and Akt-1/glycogen synthase kinase-3b (GSK-3β) signaling cascade. These cascades have also been implicated in affecting the decision of myocytes to either survive (Akt-1/GSK-3β, ERK, PKCepsilon, JAK) or undergo programmed cell death (p38 MAPK, PKC delta, JNK)[20-22] (Figure 2).
It has been observed that RhoA/ROCK pathway is also involved in hypertension and in the development of consequent cardiac hypertrophy. It has a close relationship to Ang II, which can increase ROCK activity and contributes to the maintenance of hypertension, to the increased medial thickness and perivascular fibrosis in coronary arteries[26]. This mechanism also affects stretch-induced ERK activation and vascular smooth muscle cell growth[27].
The main goal of antihypertensive therapy is the prevention of organ damages thus the prevention of life-threatening consequences such as stroke, myocardial infarction HHD or heart failure[1]. Although previous clinical trials focused mainly on improving mortality in HF, nowadays it is recognized that preventing heart failure is better for the patients and financially it is cost-effective for the health care system. It is well-known that effective antihypertensive therapy reduces the incidence of heart failure by more than fifty percent[28].
Based on current guidelines, the cornerstones of antihypertensive pharmacological therapy are diuretics, beta-blockers, angiotensin converting enzyme inhibitors (ACE-I), angiotensin receptor blockers (ARB) and calcium antagonists (CA)[29].
Blocking sympathetic hyperactivity is thought to be an essential tool in the treatment of CV diseases. Besides the blood pressure lowering effect of beta-blockers, they are able to reduce sympathetic overactivation. Moreover, they reverse left ventricular remodeling and can decrease the incidence of heart failure. Among diuretics, the thiazides mean the first line of choice because of efficacy and price. They are recommended in left ventricular hypertrophy, and can reduce cardiovascular morbidity and mortality.
ARBs and especially ACE-inhibitors significantly decrease all cause mortality in patients with hypertension. ACE-I can both prevent developing HF and decrease LV and vascular wall remodeling. A large body of evidence suggests that all of these are induced by the downregulation of enzymatic pathways involved in the interstitial collagen formation. CA effectively reduce blood pressure by dilating arteries with decreasing Ca(2+) influx into smooth muscle cells of the arterial wall. They can be used in combination therapy with most of the antihypertensive drugs. According to the statement of ESC and ESH, all above mentioned drugs are suitable for the initiation and maintenance of antihypertensive treatment because the main benefits of these drugs are due to the lowering of BP per se and are largely independent of the drugs employed[28].
Although there is an increasing number of effective antihypertensive drugs that can be used in the clinical practice, there are many patients who can not reach the goal blood pressure. In the United States, there are approximately 70 million hypertensive patients and about 40 million of them do not have their blood pressure under proper control. The main factors in the background of this phenomenon are side effects, drug intolerance or interactions and therefore poor adherence of patients to the prescribed medication[29]. Therefore in the last several years experimental researches tried to focus on treatments that alleviate end-organ damage itself without lowering blood pressure.
This approach is supported firstly by large trials with statin therapy. The main role of statins was the prevention of coronary artery disease, myocardial infarction and other adverse cardiovascular events. Statins possess both lipid-dependent and lipid independent effects. They are able to lessen inflammation, improve endothelial function and decrease thrombogenicity[30].
In the background of the favorable pleiotropic effects of statins, we need to mention the modulation of intracellular pathways, involved in cell growth regulation/apoptosis and gene expression (Ras, Rac, Rab and Rho)[30,31]. It has already been demonstrated primarily in experimental but also in human studies that high dose atorvastatin inhibits the synthesis of isoprenoids, which are functionally important in the Rho/Rho-associated coiled-coil containing kinase (ROCK) pathway[30]. Moreover, the inhibition of Rho/ROCK pathway by statins may cause improvement in endothelial function and decrease vascular inflammation and atherosclerosis. The localization of these proteins has been shown in vascular smooth muscle cells but their role needs to be determined in the context of atherosclerosis. These findings open an option for specific ROCK1 or ROCK2 inhibitors, which could have greater therapeutic effect with less toxicity[30]. Furthermore, statins decrease the number of angiotensin-1 receptors through RhoA, Ras, Rac1 and the Rho/kinase system, which regulates the ROS formation through NADPH oxidase[32].
The ASCOT-LLA study revealed the role of statins in the prevention of CV events among hypertensive patients[33,34]. Large clinical trials demonstrated that statin therapy may provide clinical benefits to patients with heart failure. Analysis of the Daunia Heart Failure Registry in 2013 elucidated that treatments with atorvastatin are associated with fewer cardiac deaths and better left ventricular performance[35,36].
Mitochondrial dysfunction also seems to be an important factor in the development of HHD[29,37,38]. Another therapeutic strategy can be the stimulation of mitochondrial biogenesis through the AMPK or the eNOS/Nitric Oxide/Cyclic Guanosine Monophosphate pathway[37-43]. Resveratrol, which has a well-known positive effect in the prevention of cardiovascular diseases, is a potent stimulator of the mitochondrial biogenesis[44-49]. An other way is to augment the mitochondrium against oxidative stress. ACE-I and ATII receptor blockers, which are originally antihypertensive drugs, bear antioxidant properties beside blood pressure lowering effect. However, it is not clear whether they target mitochondrial reactive oxygen species (ROS) formation directly or indirectly[50,51]. Thirdly, regulating mitochondrial iron homeostasis and reducing mitochondrial iron content may also yield to cardioprotection because of inhibition of hydroxyl radical formation and mitigation of oxidative stress[36].
There is an expanding number of evidence that the previously mentioned resveratrol significantly attenuates the development of cardiac dysfunction[52]. This ability is already proved in spontaneously hypertensive rats (SHR), transverse aortic constricted rats (TAC), models of hypertension and pressure overload-induced heart failure. Although resveratrol alone does not have any systolic or diastolic blood pressure lowering effect, in TAC rats resveratrol markedly increased glutathione, sodium oxide dismutase 2 levels and decreased 4-hydroxy-2-nonenal - a marker of lipid peroxidation - and LV macrophage and mast cell infiltration. Furthermore, a combination of resveratrol with hydralazine treatment significantly reduced blood pressure, improved systolic and diastolic function, decreased fibrosis and improved vascular geometry. The low-dose resveratrol itself was unable to reach these favourable actions. However, resveratrol alone alleviated cardiac fibrosis and some of the functional abnormalities in SHRs[53].
The cardiomyocyte function enhancer ranolazine reduces myoplasmic free Ca(2+) during diastole at high-stimulus rates. Therefore ranolazine showed to be effective in reducing diastolic dysfunction with inhibition of the increased late sodium current in the SHR leading to reduced Ca(2+) overload[54].
Hu et al[55] found that HGF expression is attenuated in hypertrophic and fibrotic myocardium of spontaneolusly hypertensive rats (SHR) and injected recombinant adenovirus hepatocyte growth factor gene (Ad-HGF gene) in the left ventricular free wall. The upregulation of myocardial HGF expression in SHR animals significantly suppressed myocardial fibrosis, collagen I content, LVMI, LVEDP, and increased -dP/dtmax value[55].
In the last decade PARP inhibitors received growing attention. Although they do not have any antihypertensive effect, our workgroup demonstrated that an isoquinoline derivative PARP-inhibitor, i.e., L-2286 has beneficial effects against oxidative cell damage, ischemia-reperfusion injury and the development of postinfarction, or long-term high blood pressure-induced heart failure in hypertensive animals (SHR)[21,22,25,56,57]. The PARP-inhibitor treatment significantly decreased the collagen deposition in the myocardium thus with echocardiography less prominent septal and posterior wall thickness could be measured. Moreover, in old SHR animals the transition of already developed HHD into manifest heart failure was also blocked by pharmacological PARP-inhibition. In an other long-term experiment, PARP-inhibitors decreased also the hypertensive remodeling of the great vessels in spontaneously hypertensive rats. Our experimental data also proved that the influence on the Akt-1/GSK-3β, MAPKs, MKP-1 and PKC pathways could be the underlying mechanism behind the PARP-inhibition[21,22,25,56,57].
The concept that it is possible to prevent organ damages without blood pressure lowering effect in hypertension is very promising since the goal blood pressure can not be reached in a high number of patients. This is why PARP-inhibitor co-administration could give us a potential new therapeutical approach beside the antihypertensive therapy to prevent hypertension induced organ damages.
Although several effective novel and modern antihypertensive therapies were introduced in the last decade, hypertension caused organ damages, especially HHD and heart failure, remain a leading cause of morbidity and mortality in hypertensive patients. That is the reason for the growing number of researches trying to focus on treatments that alleviate end-organ damage itself even without lowering blood pressure. Several drugs, like statins or PARP-inhibitors exert beneficial effect on intracellular signaling, and could be an important part of the treatment of hypertensive patients in the future.
P- Reviewer: Satoh S S- Editor: Ji FF L- Editor: A E- Editor: Lu YJ
| 1. | Mancia G, Fagard R, Narkiewicz K, Redon J, Zanchetti A, Böhm M, Christiaens T, Cifkova R, De Backer G, Dominiczak A. 2013 ESH/ESC guidelines for the management of arterial hypertension: the Task Force for the Management of Arterial Hypertension of the European Society of Hypertension (ESH) and of the European Society of Cardiology (ESC). Eur Heart J. 2013;34:2159-2219. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 3156] [Cited by in F6Publishing: 3139] [Article Influence: 285.4] [Reference Citation Analysis (0)] |
| 2. | Haider AW, Larson MG, Franklin SS, Levy D. Systolic blood pressure, diastolic blood pressure, and pulse pressure as predictors of risk for congestive heart failure in the Framingham Heart Study. Ann Intern Med. 2003;138:10-16. [PubMed] [Cited in This Article: ] |
| 3. | Levy D, Larson MG, Vasan RS, Kannel WB, Ho KK. The progression from hypertension to congestive heart failure. JAMA. 1996;275:1557-1562. [PubMed] [Cited in This Article: ] |
| 4. | ALLHAT Collaborative Research Group. Major cardiovascular events in hypertensive patients randomized to doxazosin vs chlorthalidone: the antihypertensive and lipid-lowering treatment to prevent heart attack trial (ALLHAT). ALLHAT Collaborative Research Group. JAMA. 2000;283:1967-1975. [PubMed] [Cited in This Article: ] |
| 5. | Yancy CW, Jessup M, Bozkurt B, Butler J, Casey DE, Drazner MH, Fonarow GC, Geraci SA, Horwich T, Januzzi JL. 2013 ACCF/AHA guideline for the management of heart failure: a report of the American College of Cardiology Foundation/American Heart Association Task Force on Practice Guidelines. J Am Coll Cardiol. 2013;62:e147-e239. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 4116] [Cited by in F6Publishing: 4473] [Article Influence: 406.6] [Reference Citation Analysis (0)] |
| 6. | Gibbons GH, Dzau VJ. The emerging concept of vascular remodeling. N Engl J Med. 1994;330:1431-1438. [PubMed] [Cited in This Article: ] |
| 7. | Kokubo M, Uemura A, Matsubara T, Murohara T. Noninvasive evaluation of the time course of change in cardiac function in spontaneously hypertensive rats by echocardiography. Hypertens Res. 2005;28:601-609. [PubMed] [Cited in This Article: ] |
| 8. | Drazner MH. The progression of hypertensive heart disease. Circulation. 2011;123:327-334. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 463] [Cited by in F6Publishing: 505] [Article Influence: 38.8] [Reference Citation Analysis (1)] |
| 9. | Bursi F, Weston SA, Redfield MM, Jacobsen SJ, Pakhomov S, Nkomo VT, Meverden RA, Roger VL. Systolic and diastolic heart failure in the community. JAMA. 2006;296:2209-2216. [PubMed] [Cited in This Article: ] |
| 10. | Meerson FZ. Compensatory hyperfunction of the heart and cardiac insufficiency. Circ Res. 1962;10:250-258. [PubMed] [Cited in This Article: ] |
| 11. | Susic D, Varagic J, Ahn J, Matavelli L, Frohlich ED. Long-term mineralocorticoid receptor blockade reduces fibrosis and improves cardiac performance and coronary hemodynamics in elderly SHR. Am J Physiol Heart Circ Physiol. 2007;292:H175-H179. [PubMed] [Cited in This Article: ] |
| 12. | Lip GY, Felmeden DC, Li-Saw-Hee FL, Beevers DG. Hypertensive heart disease. A complex syndrome or a hypertensive ‘cardiomyopathy’? Eur Heart J. 2000;21:1653-1665. [PubMed] [Cited in This Article: ] |
| 13. | Levick S, Loch D, Rolfe B, Reid RC, Fairlie DP, Taylor SM, Brown L. Antifibrotic activity of an inhibitor of group IIA secretory phospholipase A2 in young spontaneously hypertensive rats. J Immunol. 2006;176:7000-7007. [PubMed] [Cited in This Article: ] |
| 14. | Schwartzkopff B, Frenzel H, Dieckerhoff J, Betz P, Flasshove M, Schulte HD, Mundhenke M, Motz W, Strauer BE. Morphometric investigation of human myocardium in arterial hypertension and valvular aortic stenosis. Eur Heart J. 1992;13 Suppl D:17-23. [PubMed] [Cited in This Article: ] |
| 15. | Sun Y, Weber KT. Angiotensin II and aldosterone receptor binding in rat heart and kidney: response to chronic angiotensin II or aldosterone administration. J Lab Clin Med. 1993;122:404-411. [PubMed] [Cited in This Article: ] |
| 16. | Ronald GV. Systemic hypertension: Mechanisms and diagnosis. Braunwald’s heart disease. Textbook of cardiovascular medicine. Eds Bonow OR. Philadelphia: Elservier Saunders 2012; 935-954. [Cited in This Article: ] |
| 17. | MacFadyen RJ, Barr CS, Struthers AD. Aldosterone blockade reduces vascular collagen turnover, improves heart rate variability and reduces early morning rise in heart rate in heart failure patients. Cardiovasc Res. 1997;35:30-34. [PubMed] [Cited in This Article: ] |
| 18. | Puddu P, Puddu GM, Cravero E, Rosati M, Muscari A. The molecular sources of reactive oxygen species in hypertension. Blood Press. 2008;17:70-77. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 55] [Cited by in F6Publishing: 47] [Article Influence: 2.9] [Reference Citation Analysis (0)] |
| 19. | Csiszar A, Pacher P, Kaley G, Ungvari Z. Role of oxidative and nitrosative stress, longevity genes and poly(ADP-ribose) polymerase in cardiovascular dysfunction associated with aging. Curr Vasc Pharmacol. 2005;3:285-291. [PubMed] [Cited in This Article: ] |
| 20. | Bendhack LM, Sharma RV, Bhalla RC. Altered signal transduction in vascular smooth muscle cells of spontaneously hypertensive rats. Hypertension. 1992;19:II142-II148. [PubMed] [Cited in This Article: ] |
| 21. | Bartha E, Solti I, Kereskai L, Lantos J, Plozer E, Magyar K, Szabados E, Kálai T, Hideg K, Halmosi R. PARP inhibition delays transition of hypertensive cardiopathy to heart failure in spontaneously hypertensive rats. Cardiovasc Res. 2009;83:501-510. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 52] [Cited by in F6Publishing: 56] [Article Influence: 3.7] [Reference Citation Analysis (0)] |
| 22. | Deres L, Bartha E, Palfi A, Eros K, Riba A, Lantos J, Kalai T, Hideg K, Sumegi B, Gallyas F. PARP-inhibitor treatment prevents hypertension induced cardiac remodeling by favorable modulation of heat shock proteins, Akt-1/GSK-3β and several PKC isoforms. PLoS One. 2014;9:e102148. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 26] [Cited by in F6Publishing: 27] [Article Influence: 2.7] [Reference Citation Analysis (0)] |
| 23. | Pacher P, Szabó C. Role of poly(ADP-ribose) polymerase 1 (PARP-1) in cardiovascular diseases: the therapeutic potential of PARP inhibitors. Cardiovasc Drug Rev. 2007;25:235-260. [PubMed] [Cited in This Article: ] |
| 24. | Baines CP, Molkentin JD. STRESS signaling pathways that modulate cardiac myocyte apoptosis. J Mol Cell Cardiol. 2005;38:47-62. [PubMed] [Cited in This Article: ] |
| 25. | Palfi A, Toth A, Hanto K, Deres P, Szabados E, Szereday Z, Kulcsar G, Kalai T, Hideg K, Gallyas F. PARP inhibition prevents postinfarction myocardial remodeling and heart failure via the protein kinase C/glycogen synthase kinase-3beta pathway. J Mol Cell Cardiol. 2006;41:149-159. [PubMed] [Cited in This Article: ] |
| 26. | Kataoka C, Egashira K, Inoue S, Takemoto M, Ni W, Koyanagi M, Kitamoto S, Usui M, Kaibuchi K, Shimokawa H. Important role of Rho-kinase in the pathogenesis of cardiovascular inflammation and remodeling induced by long-term blockade of nitric oxide synthesis in rats. Hypertension. 2002;39:245-250. [PubMed] [Cited in This Article: ] |
| 27. | Zeidan A, Nordström I, Albinsson S, Malmqvist U, Swärd K, Hellstrand P. Stretch-induced contractile differentiation of vascular smooth muscle: sensitivity to actin polymerization inhibitors. Am J Physiol Cell Physiol. 2003;284:C1387-C1396. [PubMed] [Cited in This Article: ] |
| 28. | McMurray JJ, Adamopoulos S, Anker SD, Auricchio A, Böhm M, Dickstein K, Falk V, Filippatos G, Fonseca C, Gomez-Sanchez MA. ESC Guidelines for the diagnosis and treatment of acute and chronic heart failure 2012: The Task Force for the Diagnosis and Treatment of Acute and Chronic Heart Failure 2012 of the European Society of Cardiology. Developed in collaboration with the Heart Failure Association (HFA) of the ESC. Eur Heart J. 2012;33:1787-1847. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 3411] [Cited by in F6Publishing: 3448] [Article Influence: 287.3] [Reference Citation Analysis (0)] |
| 29. | Ong KL, Cheung BM, Man YB, Lau CP, Lam KS. Prevalence, awareness, treatment, and control of hypertension among United States adults 1999-2004. Hypertension. 2007;49:69-75. [PubMed] [Cited in This Article: ] |
| 30. | Sawada N, Liao JK. Rho/Rho-associated coiled-coil forming kinase pathway as therapeutic targets for statins in atherosclerosis. Antioxid Redox Signal. 2014;20:1251-1267. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 58] [Cited by in F6Publishing: 63] [Article Influence: 6.3] [Reference Citation Analysis (0)] |
| 31. | Nohria A, Prsic A, Liu PY, Okamoto R, Creager MA, Selwyn A, Liao JK, Ganz P. Statins inhibit Rho kinase activity in patients with atherosclerosis. Atherosclerosis. 2009;205:517-521. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 92] [Cited by in F6Publishing: 104] [Article Influence: 6.5] [Reference Citation Analysis (0)] |
| 32. | Nickenig G. Should angiotensin II receptor blockers and statins be combined? Circulation. 2004;110:1013-1020. [PubMed] [Cited in This Article: ] |
| 33. | Osende JI, Ruiz-Ortega M, Blanco-Colio LM, Egido J. Statins to prevent cardiovascular events in hypertensive patients. The ASCOT-LLA study. Nephrol Dial Transplant. 2004;19:528-531. [PubMed] [Cited in This Article: ] |
| 34. | O'Driscoll G, Green D, Taylor RR. Simvastatin, an HMG-coenzyme A reductase inhibitor, improves endothelial function within 1 month. Circulation. 1997;95:1126-1131. [PubMed] [Cited in This Article: ] |
| 35. | Correale M, Totaro A, Passero T, Abruzzese S, Musaico F, Ferraretti A, Ieva R, Di Biase M, Brunetti ND. Treatment with atorvastatin is associated with a better prognosis in chronic heart failure with systolic dysfunction: results from The Daunia Heart Failure Registry. Neth Heart J. 2013;21:408-416. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 11] [Cited by in F6Publishing: 12] [Article Influence: 1.1] [Reference Citation Analysis (0)] |
| 36. | Bayeva M, Gheorghiade M, Ardehali H. Mitochondria as a therapeutic target in heart failure. J Am Coll Cardiol. 2013;61:599-610. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 235] [Cited by in F6Publishing: 251] [Article Influence: 20.9] [Reference Citation Analysis (0)] |
| 37. | Balligand JL, Feron O, Dessy C. eNOS activation by physical forces: from short-term regulation of contraction to chronic remodeling of cardiovascular tissues. Physiol Rev. 2009;89:481-534. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 314] [Cited by in F6Publishing: 315] [Article Influence: 21.0] [Reference Citation Analysis (0)] |
| 38. | Manoury B, Montiel V, Balligand JL. Nitric oxide synthase in post-ischaemic remodelling: new pathways and mechanisms. Cardiovasc Res. 2012;94:304-315. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 16] [Cited by in F6Publishing: 18] [Article Influence: 1.5] [Reference Citation Analysis (0)] |
| 39. | Clementi E, Nisoli E. Nitric oxide and mitochondrial biogenesis: a key to long-term regulation of cellular metabolism. Comp Biochem Physiol A Mol Integr Physiol. 2005;142:102-110. [PubMed] [Cited in This Article: ] |
| 40. | Miyashita K, Itoh H, Tsujimoto H, Tamura N, Fukunaga Y, Sone M, Yamahara K, Taura D, Inuzuka M, Sonoyama T. Natriuretic peptides/cGMP/cGMP-dependent protein kinase cascades promote muscle mitochondrial biogenesis and prevent obesity. Diabetes. 2009;58:2880-2892. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 222] [Cited by in F6Publishing: 232] [Article Influence: 15.5] [Reference Citation Analysis (0)] |
| 41. | Nisoli E, Clementi E, Tonello C, Sciorati C, Briscini L, Carruba MO. Effects of nitric oxide on proliferation and differentiation of rat brown adipocytes in primary cultures. Br J Pharmacol. 1998;125:888-894. [PubMed] [Cited in This Article: ] |
| 42. | Nisoli E, Clementi E, Paolucci C, Cozzi V, Tonello C, Sciorati C, Bracale R, Valerio A, Francolini M, Moncada S. Mitochondrial biogenesis in mammals: the role of endogenous nitric oxide. Science. 2003;299:896-899. [PubMed] [Cited in This Article: ] |
| 43. | De Toni L, Strapazzon G, Gianesello L, Caretta N, Pilon C, Bruttocao A, Foresta C. Effects of type 5-phosphodiesterase inhibition on energy metabolism and mitochondrial biogenesis in human adipose tissue ex vivo. J Endocrinol Invest. 2011;34:738-741. [PubMed] [Cited in This Article: ] |
| 44. | Lagouge M, Argmann C, Gerhart-Hines Z, Meziane H, Lerin C, Daussin F, Messadeq N, Milne J, Lambert P, Elliott P. Resveratrol improves mitochondrial function and protects against metabolic disease by activating SIRT1 and PGC-1alpha. Cell. 2006;127:1109-1122. [PubMed] [Cited in This Article: ] |
| 45. | Takahashi S, Nakashima Y. Repeated and long-term treatment with physiological concentrations of resveratrol promotes NO production in vascular endothelial cells. Br J Nutr. 2012;107:774-780. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 28] [Cited by in F6Publishing: 32] [Article Influence: 2.5] [Reference Citation Analysis (0)] |
| 46. | Zang M, Xu S, Maitland-Toolan KA, Zuccollo A, Hou X, Jiang B, Wierzbicki M, Verbeuren TJ, Cohen RA. Polyphenols stimulate AMP-activated protein kinase, lower lipids, and inhibit accelerated atherosclerosis in diabetic LDL receptor-deficient mice. Diabetes. 2006;55:2180-2191. [PubMed] [Cited in This Article: ] |
| 47. | Thandapilly SJ, Wojciechowski P, Behbahani J, Louis XL, Yu L, Juric D, Kopilas MA, Anderson HD, Netticadan T. Resveratrol prevents the development of pathological cardiac hypertrophy and contractile dysfunction in the SHR without lowering blood pressure. Am J Hypertens. 2010;23:192-196. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 118] [Cited by in F6Publishing: 122] [Article Influence: 8.7] [Reference Citation Analysis (0)] |
| 48. | Biala A, Tauriainen E, Siltanen A, Shi J, Merasto S, Louhelainen M, Martonen E, Finckenberg P, Muller DN, Mervaala E. Resveratrol induces mitochondrial biogenesis and ameliorates Ang II-induced cardiac remodeling in transgenic rats harboring human renin and angiotensinogen genes. Blood Press. 2010;19:196-205. [PubMed] [Cited in This Article: ] |
| 49. | Rimbaud S, Ruiz M, Piquereau J, Mateo P, Fortin D, Veksler V, Garnier A, Ventura-Clapier R. Resveratrol improves survival, hemodynamics and energetics in a rat model of hypertension leading to heart failure. PLoS One. 2011;6:e26391. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 98] [Cited by in F6Publishing: 99] [Article Influence: 7.6] [Reference Citation Analysis (0)] |
| 50. | Yamazaki T, Tanimoto M, Gohda T, Ohara I, Hagiwara S, Murakoshi M, Matsumoto M, Kaneko S, Aoki T, Toyoda H. Combination effects of enalapril and losartan on lipid peroxidation in the kidneys of KK-Ay/Ta mice. Nephron Exp Nephrol. 2009;113:e66-e76. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 17] [Cited by in F6Publishing: 19] [Article Influence: 1.3] [Reference Citation Analysis (0)] |
| 51. | Goyal BR, Mehta AA. Beneficial role of spironolactone, telmisartan and their combination on isoproterenol-induced cardiac hypertrophy. Acta Cardiol. 2012;67:203-211. [PubMed] [Cited in This Article: ] |
| 52. | Tang PC, Ng YF, Ho S, Gyda M, Chan SW. Resveratrol and cardiovascular health - Promising therapeutic or hopeless illusion? Pharmacol Res. 2014;90C:88-115. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 56] [Cited by in F6Publishing: 54] [Article Influence: 5.4] [Reference Citation Analysis (0)] |
| 53. | Thandapilly SJ, Louis XL, Behbahani J, Movahed A, Yu L, Fandrich R, Zhang S, Kardami E, Anderson HD, Netticadan T. Reduced hemodynamic load aids low-dose resveratrol in reversing cardiovascular defects in hypertensive rats. Hypertens Res. 2013;36:866-872. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 32] [Cited by in F6Publishing: 34] [Article Influence: 3.1] [Reference Citation Analysis (0)] |
| 54. | Williams S, Pourrier M, McAfee D, Lin S, Fedida D. Ranolazine improves diastolic function in spontaneously hypertensive rats. Am J Physiol Heart Circ Physiol. 2014;306:H867-H881. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 19] [Cited by in F6Publishing: 18] [Article Influence: 1.8] [Reference Citation Analysis (0)] |
| 55. | Hu ZP, Bao Y, Chen DN, Cheng Y, Song B, Liu M, Li D, Wang BN. Effects of recombinant adenovirus hepatocyte growth factor gene on myocardial remodeling in spontaneously hypertensive rats. J Cardiovasc Pharmacol Ther. 2013;18:476-480. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 1] [Cited by in F6Publishing: 4] [Article Influence: 0.4] [Reference Citation Analysis (0)] |
| 56. | Magyar K, Deres L, Eros K, Bruszt K, Seress L, Hamar J, Hideg K, Balogh A, Gallyas F, Sumegi B. A quinazoline-derivative compound with PARP inhibitory effect suppresses hypertension-induced vascular alterations in spontaneously hypertensive rats. Biochim Biophys Acta. 2014;1842:935-944. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 16] [Cited by in F6Publishing: 17] [Article Influence: 1.7] [Reference Citation Analysis (0)] |
| 57. | Bartha E, Solti I, Szabo A, Olah G, Magyar K, Szabados E, Kalai T, Hideg K, Toth K, Gero D. Regulation of kinase cascade activation and heat shock protein expression by poly(ADP-ribose) polymerase inhibition in doxorubicin-induced heart failure. J Cardiovasc Pharmacol. 2011;58:380-391. [PubMed] [DOI] [Cited in This Article: ] [Cited by in F6Publishing: 1] [Reference Citation Analysis (0)] |