Published online Nov 10, 2015. doi: 10.5317/wjog.v4.i4.108
Peer-review started: May 9, 2015
First decision: July 10, 2015
Revised: September 9, 2015
Accepted: October 12, 2015
Article in press: October 13, 2015
Published online: November 10, 2015
Processing time: 185 Days and 12.4 Hours
AIM: To answer some questions related to the problem of ovarian simple cysts in asymptomatic postmenopausal women.
METHODS: A literature search and systematic review using MEDLINE (PubMed) database from 1980 to 2014 was performed using the following terms: “simple cyst”, “postmenopause”, “postmenopausal”, “ultrasound”, “ovary”, “ovarian”, “asymptomatic”. Papers not related to the topic, reviews, letters to editor, opinion letter, commentaries and studies published in non-English language were excluded. Two authors then reviewed the full paper of all the studies initially selected. This review does not claim to be a meta-analysis. Therefore, meta-analysis statistics were not applied and PRISMA guidelines were not strictly followed. Simple descriptive statistics were used providing absolute numbers and corresponding percentages as well as range.
RESULTS: Nine papers were ultimately included in this review, accounting for 98899 postmenopausal women. We have found that ovarian simple cysts are relatively common in asymptomatic postmenopausal women (prevalence: 8.7%). The risk of malignancy is very low (0.19%). More than 90% of these cysts were smaller than 5 cm. Bilaterality rate ranged from 3.7% to 15%. Histologically, most cysts are serous cystadenomas (61%). When managed conservatively, a significant number resolve spontaneously (46.1%) or remain unchanged (39%).
CONCLUSION: According to these data, conservative management should be the first option to offer to these women.
Core tip: The problem of ovarian simple cysts in asymptomatic postmenopausal women remains a controversial issue in gynecological practice. We have performed a literature review about this topic. We have found that ovarian simple cysts are relatively common in asymptomatic postmenopausal women. The risk of malignancy is very low. Histologically, most cysts are serous cystadenomas. When managed conservatively, a significant number resolve spontaneously or remain unchanged.
- Citation: Alcazar JL, Martinez N, Juez L, Caparros M, Salas A, Errasti T. Ovarian simple cysts in asymptomatic postmenopausal women detected at transvaginal ultrasound: A review of literature. World J Obstet Gynecol 2015; 4(4): 108-112
- URL: https://www.wjgnet.com/2218-6220/full/v4/i4/108.htm
- DOI: https://dx.doi.org/10.5317/wjog.v4.i4.108
The management of adnexal simple cysts in asymptomatic postmenopausal women remains a controversial issue in gynecological practice. Albeit management of these lesions has certainly evolved from a systematic surgical removal to a more conservative approach[1], many gynecologist are still reluctant to advise such a conservative management.
Some issues regarding to this entity remains unresolved such as the lesion’s size above which surgery should be advised, the risk of torsion, what factors are associated with the appearance of this lesion and for how long follow-up should be performed in case of conservative management and which control periodicity should be advised, what factors are associated to the appearance of this lesion. Most importantly, if the lesion is left in situ, which is the actual risk for developing a malignancy?
For this reason we decided to conduct a systematic review on the literature in an attempt to answer the following questions: (1) What should be considered an ovarian simple cyst? (2) What is the prevalence of ovarian simple cysts in asymptomatic postmenopausal women? (3) Which are the characteristics of these lesions? (4) What are the factors associated to the appearance of these lesions? (5) What is the natural history of these lesions if conservative management is chosen? (6) What is the most frequent histology if surgery is performed? (7) What is the risk of developing a malignancy? (8) What are the features associated with malignancy? and (9) What is the role of CA-125?
A systematic review of the literature in MEDLINE (PubMed) database was performed by one of the authors (JLA) from 1980 to 2014 was performed using the following terms: “simple cyst”, “postmenopause”, “postmenopausal”, “ultrasound”, “ovary”, “ovarian”, “asymptomatic”. This author screened titles and abstracts and excluded those papers not related to the topic, reviews, letters to editor, opinion letter, commentaries and studies published in non-English language.
Two authors (JLA, NM) then reviewed the full paper of all the studies initially selected according to the following criteria:
Inclusion criteria: (1) Study design: prospective cohort study; (2) Patients: postmenopausal asymptomatic women.
Exclusion criteria: (1) Sample size < 50 women; (2) Incomplete data about patients characteristics, follow-up, histology and malignancy rate; and (3) Ultrasound performed by transabdominal route. We decided exclude these studies because of the possibility of missing papillary projections using this route is higher and some not truly simple cysts could be as such. Disagreement between reviewers was solved by consensus.
This review does not claim to be a meta-analysis. Therefore, meta-analysis statistics were not applied and PRISMA guidelines[2] were not strictly followed. Simple descriptive statistics were used providing absolute numbers and corresponding percentages as well as range.
Additionally, since this is a review Institutional Review Board was waived.
A total of 79 papers were found after database search. First screen excluded 62 papers for the following reasons: paper not related to the topic (n = 42), review paper (n = 12), letter to editor or commentary paper (n = 4) and non-English language (n = 4).
Full paper was reviewed for 17 studies. Eight papers were excluded for the following reasons: retrospective design (n = 3), ultrasound evaluation performed by transabdominal route (n = 2), incomplete data (n = 3).
Therefore, nine papers were ultimately included in this review[3-11].
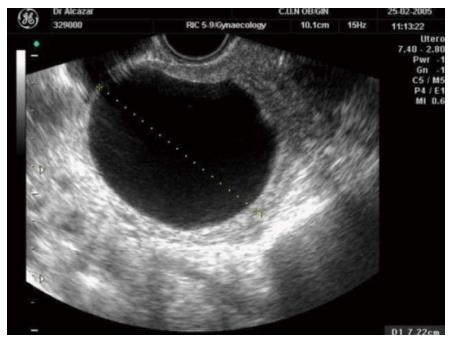
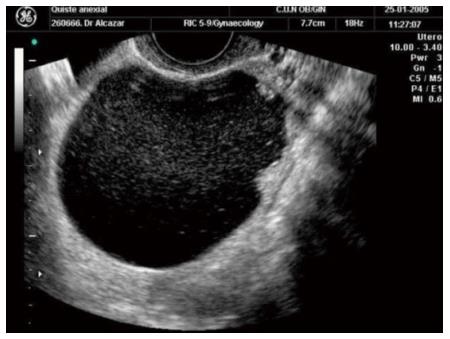
The vast majority of studies selected defined as simple cyst the presence of an oval or rounded anechoic thin-walled cyst without any irregularity in the internal wall (Figure 1)[1]. The presence of any wall irregularity or echogenic cyst’s content should not be considered as a simple cyst (Figure 2).
The nine studies included accounted for 98899 postmenopausal women. Two studies included only women with simple cysts[3,7]. Mean age reported in six studies, ranged from 55.5 years old to 65 years old.
The total number of simple cysts reported was 8600. Therefore, overall prevalence was 8.7% (95%CI: 8.5% to 8.9%). However, prevalence varied among different studies, ranging from 2.5% to 14.1%. Two studies with long term follow-up reported that the annual incidence of simple cysts ranged from 3% to 8%[10,11].
Most studies included cysts smaller than 5 cm in size[3-5,10,11]. However, three studies included cysts up to 10 cm[6,8,9] and one even up to 20 cm[7]. According to data derived from these studies more than 90% of these cysts were smaller than 5 cm.
Bilaterality rate was reported in three studies[8-10], ranging from 3.7% to 15%. Moreover, three or more cysts in the same woman has been reported in 5% of the cases[10].
Three studies have evaluated factors that could be associated to with the appearance of ovarian simple cysts in postmenopause.
Modesitt et al[8] reported that these lesions appeared more frequently in women under hormone replacement therapy (either estrogens alone or estrogens plus progestins) and in women with recent menopause.
Greenlee et al[10] performed a more exhaustive analysis in a large population. They found that ovarian simple cysts were associated with age (the younger the woman the higher the risk for simple cyst), non-smoking, previous history of surgery for benign gynecologic condition, previous history of ovarian benign cyst, higher education, precocious menopause and first pregnancy before 20 years old. No association was found with use of hormone replacement therapy, use of hormonal contraception, parity or history of infertility.
Sharma et al[11] found that previous hysterectomy, age and weight were significantly associated with simple cysts.
Data about the natural history of ovarian simple cysts in asymptomatic postmenopausal women on follow-up has been reported in eight studies[3-6,8-11]. The mean follow-up ranged from 18 to 71 mo.
Ovarian simple cysts resolved spontaneously in almost half of the cases (46.1%). Spontaneous resolution rate ranged from 0% to 69.4%, depending on the study.
Factors associated to resolution were age (the younger the woman the higher the probability of resolution)[6,9], cyst’s size (the smaller the size the higher the probability of resolution)[5], the number of cysts (more than 2 cysts was associated to a lower probability of resolution)[10].
Among those cysts that have not resolved, many number did not change in size or aspect (39%; range 23% to 96%[3,4,5,8,9,11]). Among those that changed in appearance most of them developed septations or solid areas[5,8].
Detailed data about histology of surgically removed cysts were reported on six studies[3,5-9]. The total number of cysts removed was 525. Three hundreds and thirty-six were removed after diagnosis and 189 during follow-up. Only on study reported median time elapsed from diagnosis up to removal (27 mo)[9].
Simple cyst and serous cystadenoma were the most frequent histologies (61%, 155/254) followed by cystadenofibroma (8%, 20/254) and para-ovarian cyst (5%, 14/254).
Other reported histologic diagnoses were endometrioma, dermoid cyst, hydrosalpinx and mucinous cystadenoma.
Overall 16 malignancies among 8600 simple cysts were reported[7,9-11]. This represents a malignancy rate of 0.19%.
Greenlee et al[10] reported on 15735 women enrolled in the PLCO (Prostate, Lung, Colorectal and Ovarian Cancer) Screening Trial. Nine women (0.41%) among those 2217 diagnosed as having a simple cyst developed an ovarian cancer. Whereas, 55 out of 12638 (0.44%) without a simple cyst developed an ovarian malignancy. The relative risk for those with ovarian simple cyst was 0.93 (95%CI: 0.46-1.88).
Sharma et al[11] reported on 48230 women enrolled in the UKCTOCS (United Kingdom Collaborative Trial of Ovarian Cancer Screening) study. At first scan, 22194 women had normal ovaries visualized, 21943 women had non-visualized one or both ovaries, 1234 women had an inclusion cyst (simple cyst < 10 mm) and 197 had an inclusion cyst and a simple cyst (simple cyst > 10 mm). After a median follow-up of 3 years, and considering only women with both ovaries visualized and those with inclusion and/or simple cyst, three women (0.2%) with only inclusion cyst and one woman (0.5%) with inclusion and simple cyst developed an ovarian malignancy. Twenty nine out of 22194 women in whom both ovaries were visualized and were normal developed an ovarian cancer. The relative risk for women with inclusion cyst was 1.92 (95%CI: 0.62-5.92) and relative risk for women with inclusion cyst and simple cyst was 4.01 (95%CI: 0.69-22.92).
This is probably the most interesting question. However, the information provided in the studies evaluated for this mini-review is scanty. From data reported from three studies[7,9,11] including eight ovarian cancers, we observed that most of them (6/8) were stage I and in 5/8 the size of the cyst was < 5 cm in 5 out of 8 cases.
Tumor marker CA-125 was used in all studies but two[7,11]. Some studies established normal CA-125 level (< 35 UI/mL) as an inclusion criteria[4,8-10] and most of them assessed CA-125 during follow-up[3-6,9,10]. However, three studies did not report specific information about CA-125 levels[6,8,10].
Those studies that reported data about CA-125 during follow-up reported no significant changes of this tumor marker during follow-up, even in those cases with sonographic changes in the ovarian simple cyst[3-5]. In the study by Castillo et al[9], there was one case of ovarian malignancy. In this case CA-125 raised during follow-up (45 UI/mL).
In this systematic review, we have addressed the issue of ovarian simple cysts in asymptomatic postmenopausal women.
We have found that this type of lesions is common in this group of women. This finding is in agreement with data from autopsy studies[12,13]. Another finding in agreement with autopsy studies is that most cysts are small and that the most common histology is simple cyst or serous cystadenoma.
Transvaginal ultrasound route is essential for ascertaining that the lesion is actually a simple cyst, since small papillary projections might be missed using transabdominal ultrasound[14].
Patient’s characteristics consistently associated with the presence of a simple ovarian cyst in postmenopausal women are age and previous history of pelvic or gynecologic surgery. This, in fact, is not surprising since younger postmenopausal women may have residual ovarian activity and many of these simple cysts could be “functional cysts” developed from this residual activity. This fact may also explain why the probability of spontaneous resolution is higher in women with recent menopause. On the other hand, previous pelvic surgery increases the risk of peritoneal cysts that may resemble ovarian simple cysts.
No study reported data about complications such as torsion or rupture. Therefore, albeit it is not possible to draw definitive conclusions regarding these complications. However, it seems that they are uncommon in ovarian simple cysts during the menopause.
Additionally no study reported information about when and for how long follow-up should be performed in those cysts that had not resolved spontaneously.
Regarding surgery in most studies there is no data reported about the surgical approach. The authors think that laparoscopic cyst removal should be the best approach when surgery is decided[15].
Probably one of the most important findings in our review is that related to the risk of malignancy of these lesions. Actually, in the two largest studies published so far the relative risk of developing an ovarian malignancy in postmenopausal women with ovarian simple cyst was not increased as compared with those postmenopausal women without ovarian simple cyst.
Postmenopausal simple cysts in asymptomatic women management remains as an unsolved issue in gynecological practice. This is relevant because of surgery has been traditionally performed. However, recent data challenge this concept showing that conservative management should be offered to these women.
A number of papers have been published addressing this question in the last fifteen years. However, adequate systematic reviews are lacking.
The paper offers an updated systematic review about this topic. According to the authors’ findings in this mini-review, it could be assumed that ovarian simple cysts are common in asymptomatic postmenopausal women. The risk of malignancy is very low and having a simple ovarian cyst does not seem to increase the risk of developing an ovarian cancer. Many of them will resolve spontaneously or will remain unchanged during follow-up. The role of CA-125 at diagnosis and for following-up remains to be determined. Data about the use of CA-125 are scanty in the studies reviewed. Most studies used CA-125 as inclusion criteria and during follow-up. In most cases CA-125 did not change, even in those cysts that changed during follow-up. Only in one case of carcinoma the value of CA-125 was reported as elevated. In the authors’ opinion, the role of routine CA-125 assessment in the follow-up of postmenopausal ovarian simple cyst would be arguable. The authors’ review has some limitations. First, the authors did not perform a formal meta-analysis. Therefore, conclusions based on statistical inferences cannot be drawn. Second, the number of studies included is small. Third, studies are considerably heterogeneous in design and data reported. However, some questions remain unanswered and future research is needed to try to answer these questions: (1) Which cysts are at higher risk for developing a malignancy? (2) Is follow-up needed for these lesions? (3) For how long these cysts should be followed-up? and (4) Which follow-up protocol should be implemented?
The results of the analysis may have a relevant clinical impact since the authors have shown that ovarian simple cysts are common in asymptomatic postmenopausal women and the risk of malignancy is very low. These findings should modify the traditional surgical management of these lesions for a more conservative one. However, there is still a room for research since some questions remain unanswered (see above).
This is an interesting manuscript.
P- Reviewer: Iavazzo C, Khajehei M, Mohammed Usta I S- Editor: Ji FF L- Editor: A E- Editor: Wang CH
| 1. | Goldstein SR. Postmenopausal adnexal cysts: how clinical management has evolved. Am J Obstet Gynecol. 1996;175:1498-1501. [PubMed] |
| 2. | Liberati A, Altman DG, Tetzlaff J, Mulrow C, Gøtzsche PC, Ioannidis JP, Clarke M, Devereaux PJ, Kleijnen J, Moher D. The PRISMA statement for reporting systematic reviews and meta-analyses of studies that evaluate health care interventions: explanation and elaboration. PLoS Med. 2009;6:e1000100. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 11206] [Cited by in RCA: 11027] [Article Influence: 689.2] [Reference Citation Analysis (0)] |
| 3. | Auslender R, Atlas I, Lissak A, Bornstein J, Atad J, Abramovici H. Follow-up of small, postmenopausal ovarian cysts using vaginal ultrasound and CA-125 antigen. J Clin Ultrasound. 1996;24:175-178. [PubMed] |
| 4. | Aubert JM, Rombaut C, Argacha P, Romero F, Leira J, Gomez-Bolea F. Simple adnexal cysts in postmenopausal women: conservative management. Maturitas. 1998;30:51-54. [PubMed] |
| 5. | Conway C, Zalud I, Dilena M, Maulik D, Schulman H, Haley J, Simonelli K. Simple cyst in the postmenopausal patient: detection and management. J Ultrasound Med. 1998;17:369-372; quiz 373-374. [PubMed] |
| 6. | Bailey CL, Ueland FR, Land GL, DePriest PD, Gallion HH, Kryscio RJ, van Nagell JR. The malignant potential of small cystic ovarian tumors in women over 50 years of age. Gynecol Oncol. 1998;69:3-7. [PubMed] |
| 7. | Ekerhovd E, Wienerroith H, Staudach A, Granberg S. Preoperative assessment of unilocular adnexal cysts by transvaginal ultrasonography: a comparison between ultrasonographic morphologic imaging and histopathologic diagnosis. Am J Obstet Gynecol. 2001;184:48-54. [PubMed] |
| 8. | Modesitt SC, Pavlik EJ, Ueland FR, DePriest PD, Kryscio RJ, van Nagell JR. Risk of malignancy in unilocular ovarian cystic tumors less than 10 centimeters in diameter. Obstet Gynecol. 2003;102:594-599. [PubMed] |
| 9. | Castillo G, Alcázar JL, Jurado M. Natural history of sonographically detected simple unilocular adnexal cysts in asymptomatic postmenopausal women. Gynecol Oncol. 2004;92:965-969. [PubMed] |
| 10. | Greenlee RT, Kessel B, Williams CR, Riley TL, Ragard LR, Hartge P, Buys SS, Partridge EE, Reding DJ. Prevalence, incidence, and natural history of simple ovarian cysts among women & gt; 55 years old in a large cancer screening trial. Am J Obstet Gynecol. 2010;202:373.e1-373.e9. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 99] [Cited by in RCA: 77] [Article Influence: 5.1] [Reference Citation Analysis (0)] |
| 11. | Sharma A, Gentry-Maharaj A, Burnell M, Fourkala EO, Campbell S, Amso N, Seif MW, Ryan A, Parmar M, Jacobs I. Assessing the malignant potential of ovarian inclusion cysts in postmenopausal women within the UK Collaborative Trial of Ovarian Cancer Screening (UKCTOCS): a prospective cohort study. BJOG. 2012;119:207-219. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 31] [Cited by in RCA: 28] [Article Influence: 2.2] [Reference Citation Analysis (0)] |
| 12. | Valentin L, Skoog L, Epstein E. Frequency and type of adnexal lesions in autopsy material from postmenopausal women: ultrasound study with histological correlation. Ultrasound Obstet Gynecol. 2003;22:284-289. [PubMed] |
| 13. | Dørum A, Blom GP, Ekerhovd E, Granberg S. Prevalence and histologic diagnosis of adnexal cysts in postmenopausal women: an autopsy study. Am J Obstet Gynecol. 2005;192:48-54. [PubMed] |
| 14. | Valentin L. Use of morphology to characterize and manage common adnexal masses. Best Pract Res Clin Obstet Gynaecol. 2004;18:71-89. [PubMed] |
| 15. | Canis M, Rabischong B, Houlle C, Botchorishvili R, Jardon K, Safi A, Wattiez A, Mage G, Pouly JL, Bruhat MA. Laparoscopic management of adnexal masses: a gold standard? Curr Opin Obstet Gynecol. 2002;14:423-428. [PubMed] |