Published online Aug 15, 2015. doi: 10.4251/wjgo.v7.i8.95
Peer-review started: February 22, 2015
First decision: March 20, 2015
Revised: May 12, 2015
Accepted: May 27, 2015
Article in press: May 28, 2015
Published online: August 15, 2015
Human tumors tend to activate the immune system regulatory checkpoints as a means of escaping immunosurveillance. For instance, interaction between program
death-1 (PD-1) and program death-ligand 1 (PD-L1) will
lead the activated T cell to a state of anergy. PD-L1 is upregulated on a wide range of cancer cells. Anti-PD-1 and anti-PD-L1 monoclonal antibodies (mAbs), called immune checkpoint inhibitors (ICIs), have consequently been designed to restore T cell activity. Accumulating data are in favor of an association between PD-L1 expression in tumors and response to treatment. A PD-L1 expression is present in 30% to 50% of digestive cancers. Multiple anti-PD-1 (nivolumab, pembrolizumab) and anti-PD-L1 mAbs (MPDL3280A, Medi4736) are under evaluation in digestive cancers. Preliminary results in metastatic gastric cancer with pembrolizumab are highly promising and phase II will start soon. In metastatic colorectal cancer (CRC), a phase III trial of MPDL3280A as maintenance therapy will shortly be initiated. Trials are also ongoing in metastatic CRC with high immune T cell infiltration (i.e., microsatellite instability). Major challenges are ahead in order to determine how, when and for which patients we should use these ICIs. New radiologic criteria to evaluate tumor response to ICIs are awaiting prospective validation. The optimal therapeutic sequence and association with cytotoxic chemotherapy needs to be established. Finally, biomarker identification will be crucial to selection of patients likely to benefit from ICIs.
Core tip: Anti-program death-1 and anti-program death-ligand 1 (PD-L1) monoclonal antibodies have been designed to restore T cell activity, since human tumors tend to activate this immune regulatory checkpoint as a means of escaping immunosurveillance. A PD-L1 expression is present in 30% to 50% of digestive cancers and accumulating data are in favor of an association between this PD-L1 expression and response to treatment, which make digestive cancers promising candidates for those breakthrough immunotherapies. We review the ongoing clinical trials and the major challenges ahead of us in order to learn how, when and for which patients we should use these therapeutics.
- Citation: Guillebon E, Roussille P, Frouin E, Tougeron D. Anti program death-1/anti program death-ligand 1 in digestive cancers. World J Gastrointest Oncol 2015; 7(8): 95-101
- URL: https://www.wjgnet.com/1948-5204/full/v7/i8/95.htm
- DOI: https://dx.doi.org/10.4251/wjgo.v7.i8.95
Up until recently, only melanoma and renal cell cancer (RCC) were considered as immunogenic tumors. But in 2012 the results of a phase I study with nivolumab, an anti program death-1 (PD-1) monoclonal antibody (mAb), showed clinical responses in non-small cell lung cancers (NSCLC), thereby introducing the notion that any tumor can respond to the immune checkpoint inhibition strategy[1]. To prevent autoimmunity, to allow peripheral tolerance (during a woman’s pregnancy, for instance) or to permit negative feed-back on immune reactions and secure immune system homeostasis, multiple immune checkpoints must be crossed so that immune response can occur and last. Human tumors tend to activate these immune checkpoints as a means of escaping immunosurveillance. That is one reason why new therapeutics called immune checkpoints inhibitors (ICIs) have been designed.
Cancer immunoediting is currently defined by three E’s: elimination, equilibrium and escape[2]. The first phase reflects active immunosurveillance, which facilitates tumor eradication and is mostly mediated by tumor-associated antigen-specific lymphocytes. The second phase refers to the period during which tumor growth is still prevented by the host immune system even though the surviving tumor and its stroma are also shaped by the immune response, which they learn how to downsize. Lastly, the escape phase describes tumor growth notwithstanding an immunologically intact environment due to selection of tumor cell variants during the equilibrium phase.
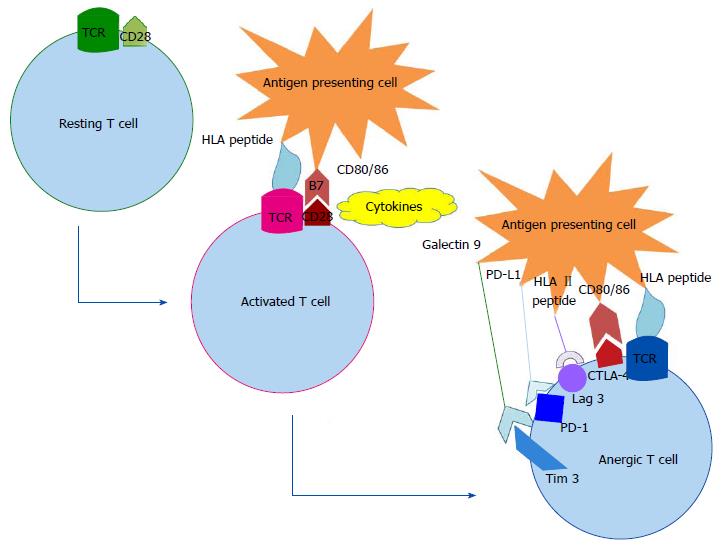
In order to be activated, a T lymphocyte needs an association of triggering signals. Antigen coupled with major histocompatibility complex recognition is the first step toward activation. A second signal arising from the interaction of co-stimulatory molecules of activation must occur, avoiding T cell anergy. CD28 is the most commonly cited example of co-stimulatory molecules, and it is constitutively expressed on the T cell surface. It binds to B7.1 (CD80) or B7.2 (CD86), which are primarily expressed on activated antigen-presenting cells. B7 molecules also interact with cytotoxic T lymphocyte associated antigen 4 (CTLA-4), which is expressed on T cells. CTLA-4 transmits an inhibitory signal to T cells to prevent early excessive T cell activation. The molecules involved are called immune checkpoint. PD-1 is more widely expressed than CTLA-4 and can be detected not only on T cells but also on B lymphocytes and natural killer cells. Program death-ligand 1 (PD-L1) expression is up-regulated by interferon-γ production, which follows T cell activation. PD-1/PD-L1 interaction allows for negative feedback on the immune response regulating effector T cell responses in peripheral tissues and leads to peripheral T cell tolerance[3,4] (Figure 1). PD-L1 expression is up-regulated on a wide range of cancer cells and tumor-infiltrating immune cells strongly involved in tumor immunosurveillance escape. Several ICIs have been developed so as to prevent those negative regulations of the host immune system.
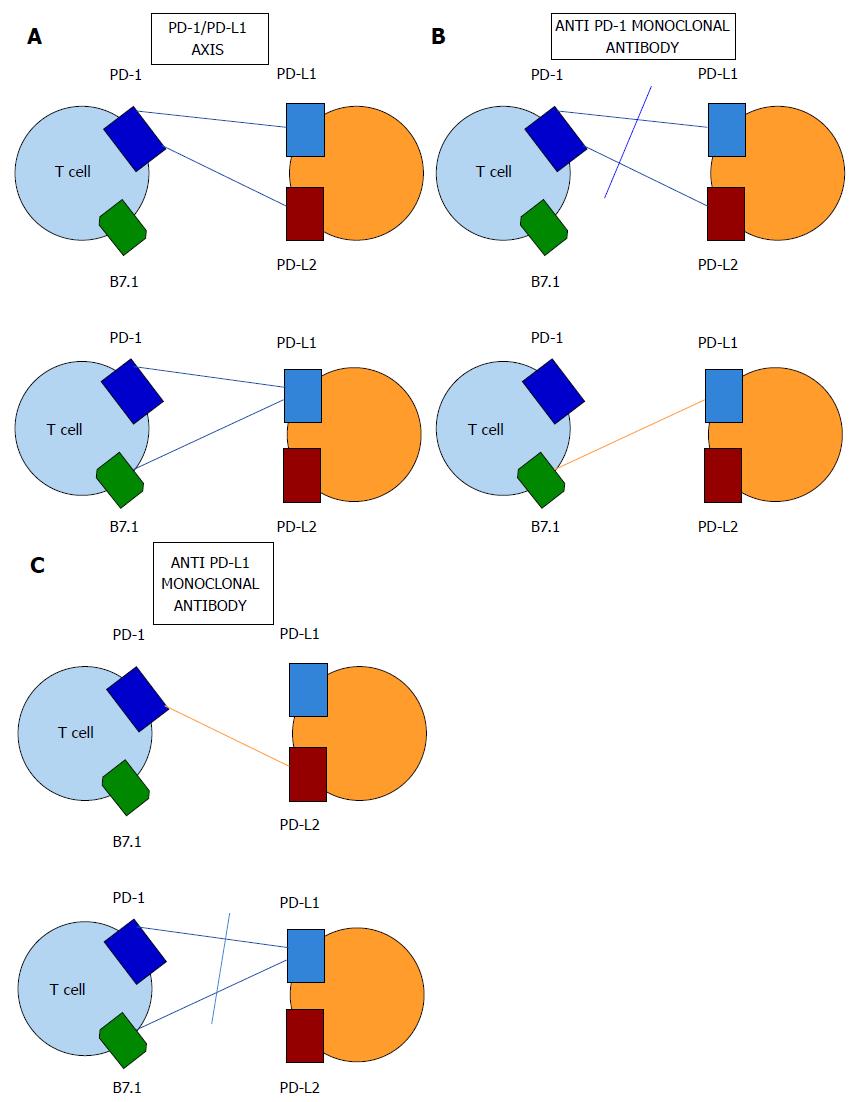
To boost immune responses, ipilimumab, an anti-CTLA-4 mAb has been designed and has produced good results in cases of melanoma. Its limiting toxicities are mostly autoimmunity since it seems to upregulate all immune reactions. The PD-1/PD-L1 axis can be targeted by either anti-PD-1 mAbs or anti-PD-L1 mAbs (Figure 2). Anti PD-1 mAbs target PD-1 interactions with both PD-L1 and program death-ligand 2 (PD-L2), while PD-L1 mAbs target interactions between PD-L1 and either PD-1 or B7.1. PD-1 mAbs have been approved for the treatment of unresectable melanoma and NSCLC and their development for bladder cancer and RCC is well-advanced. Targeting of the CTLA-4 pathway has changed the melanoma treatment landscape[5,6] but PD-1/PDL1 axis targeting is also highly promising in multiple tumors[1,7].
Several studies have demonstrated an association between pretreatment PD-L1 expression and tumor responses to anti-PD-1/PD-L1 therapies in melanoma, bladder cancer and NSCLC[1,8]. A PD-L1/PD-1 positive tumor should consequently be a good candidate for these treatments. For example, Dong et al[9] found 53% of PD-L1 positive colon carcinomas. Later, Droeser et al[10] studied PD-L1 expression in 1420 colorectal cancer (CRC). Strong PD-L1 positivity was found in 36% and 29%, respectively in mismatch repair (MMR)-proficient and deficient (dMMR) CRC. dMMR CRC has been associated with high level of tumor-infiltrating lymphocytes (TIL) and a good prognosis[11]. In other digestive cancers, especially in esophageal, gastric and pancreatic cancers, a PD-L1 expression was found in 30%-50% of cases[12-15].
Preliminary results are available for two anti-PD-1 mAbs (nivolumab and pembrolizumab) in digestive cancers. Nineteen patients with CRC were enrolled in the phase I study of nivolumab, but no efficacy was demonstrated[1]. However, nivolumab is currently being evaluated in multiple digestive cancers both alone and in combination with other ICIs (such as ipilumumab or anti-Lag 3) or with immune system stimulators. A phase II clinical trial of nivolumab vs nivolumab plus ipilimumab in recurrent and metastatic colon cancer with a stratification between dMMR and pMMR status is ongoing. Pembrolizumab has been evaluated in gastric cancer and preliminary results were presented at the 2014 European Society for Medical Oncology meeting and updated at the 2015 American Society of Clinical Oncology Gastro Intestinal symposium[14]. In this trial, only PD-L1 positive tumors were eligible. Thirty-nine patients were enrolled and 67% had received at least two prior chemotherapy regimens. The overall response rate was 22%. The 6-mo progression-free survival and overall survival rates were 24% and 69%, respectively. Four patients experienced grade 3 to 4 adverse events and one patient died due to treatment-related hypoxia. A phase II study will shortly be initiated with pembrolizumab monotherapy or in combination with cisplatin and 5 fluoro-uracil (5FU) in advanced gastric cancer treatment. Pembrolizumab is also currently under investigation in pancreatic cancer and in combination with aflibercept in CRC.
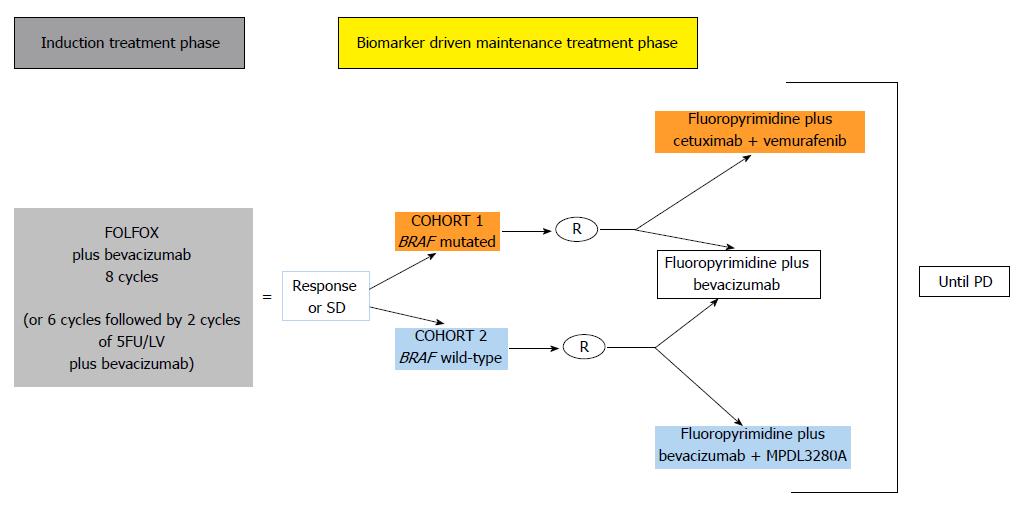
Now focusing on anti-PD-L1 mAbs (BMS936559, MPDL3280A and MEDI4736) results in digestive cancers, the phaseIstudy with BMS936559 enrolled eighteen patients with CRC, fourteen with pancreatic cancer and seven with gastric cancer. None of the gastric cancer patients could be included in the efficacy analysis and no objective response was observed in either CRC or in pancreatic cancer[7]. MPDL3280A showed very promising results in metastatic bladder cancer[8], NSCLC and RCC[16] but so far no result has been presented in digestive cancer. However, clinical trials are ongoing in combination with immune-modulating therapies (ipilumumab or interferon-α) and in combination with bevacizumab, MEK inhibitor or CD40 agonist. Finally, the MODUL trial is a randomized phase III multicenter trial with biomarker-driven maintenance therapy in metastatic CRC first-line treatment (Figure 3). After a four-month FOLFOX plus bevacizumab induction therapy, patients with disease control will be treated by maintenance therapy with 5FU, cetuximab and vemurafenib in BRAF mutated tumors or with 5FU, bevacizumab and MPDL3280A in BRAF wild-type tumors (the control arm will be 5FU and bevacizumab in both cohorts). MPDL3280A and MEDI4736 are both human IgG1 PD-L1 mAbs whose Fc domain has been engineered to prevent antibody-dependent cell-mediated cytotoxicity (ADCC). Indeed, PD-L1 can be expressed by the tumor-infiltrating immune cells, including T cells and if ADCC was induced, the latter would be killed, which would be counterproductive. The results of the MEDI4736 multi-arm dose expansion study were presented at the 2014 ASCO meeting and updated at the 2014 ESMO meeting. A disease control rate of approximately 20% was observed across all relevant histology (10 mg/kg every two weeks), especially in hepatocellular carcinoma (19 patients), gastro-esophageal cancer (28 patients) and pancreatic cancer (29 patients)[15]. Tolerance was acceptable with 5.6% grade 3-4 adverse events, and no autoimmunity was reported. A study with MEDI4736 in dMMR CRC and pMMR CRC presenting with high TIL infiltration is scheduled to start.
Since ICIs seem as promising in digestive cancer as in other tumors, the same major challenges will be faced. Firstly, since initial progression is not rare, there arises the need for novel criteria to evaluate tumor response to immunotherapeutic agents. As with anti-angiogenic therapies, a tumor burden increase or appearance of new lesions can precede objective response and caution should be used before drawing any conclusion on disease progression[1,6,8,16]. Immune cell infiltration can explain these features. Recently, immune-related response criteria have been defined and await prospective validation[17]. In any case, progression should be confirmed by a new radiological evaluation four weeks later. Secondly, optimal therapeutic sequences need to be established since most studies have included patients with advanced tumors. As of now no data are available in first-line therapy or in the adjuvant setting, but promising results with ipilimumab in melanoma have been reported[18]. Thirdly, in solid tumors, ICIs will probably need to be combined with chemotherapy, which could cause some problems, given the detrimental effects that chemotherapy can exert on the immune system. Combination with an immunogenic chemotherapy such as oxaliplatin should nonetheless be a good option. Finally, biomarkers are eagerly awaited to enable selection of the patients most likely to benefit from these ICIs. Only 20% to 30% of patients show objective response and in addition to inefficacy, patients are exposed to unnecessary toxicity. PD-L1 expression seems to correlate with clinical outcome but objective responses have been observed in PD-L1 negative tumors. Moreover, definition of a PD-L1 positive tumor needs standardization, given that the threshold of positivity varies between 1% and 5% across different studies and also given that PD-L1 expression can be analyzed either on tumor cells or on tumor-infiltrating cells[16,19]. In melanoma, a predictive model using CD8, PD-1 and PD-L1 positive cells at invasive margins and the tumor center has been correlated with a treatment response but requires prospective validation[20]. In addition, the expression of PD-L1 could be different in primary tumors at the beginning of the disease compared to metachronous metastasis several months later.
Many digestive cancers are candidates for the anti-PD-1/PD-L1 axis blockade (Table 1) but we have still got to elucidate for whom, when and how to use them. dMMR CRCs are good candidates due to their high TIL infiltration associated with their high load of frameshift mutations[21]. dMMR CRCs are associated with high-CD8 cytotoxic T cells but also with up-regulation of at least five negative regulatory immune checkpoint molecules (PD-1, PD-L1, CTLA-4, LAG-3, IDO)[22]. One limit to use of ICIs in dMMR CRC could be that it represents only 5% of stage IV CRCs. Nevertheless, both nivolumab and pembrolizumab are currently being tested in this particular subset.
| Monoclonal antibody | Antibody description | Association | Tumors |
| MPDL3280A | Anti-PD-L1 Engineered | MODUL trial: Phase III biomarker driven maintenance therapy | Metastatic colorectal cancer |
| Human | |||
| IgG11 | |||
| Medi 4736 | Anti-PD-L1 | None | Immunological subsets of advanced colorectal cancer |
| Engineered | |||
| Human | |||
| IgG11 | |||
| Nivolumab | Anti-PD-1 | Nab-paclitaxel +/- Gemcitabine | Pancreatic cancer |
| Fully human | |||
| IgG42 | |||
| GVAX pancreas vaccine + CRS-207 | Pancreatic cancer | ||
| None | Squamous cell carcinoma of the anal canal | ||
| Ipilimumab | Recurrent and metastatic colon cancer | ||
| None | Hepatocellular carcinoma | ||
| None | Advanced or recurrent gastric cancer | ||
| Pembrolizumab | Anti-PD-1 | None | Resectable or borderline resectable pancreas cancer |
| Humanized | |||
| IgG42 | |||
| None | Advanced gastro-intestinal cancers | ||
| None | Metastastic colorectal cancer with and without microsatellite instability |
P- Reviewer: Evans DC, Koukourakis GV, Stanojevic GZ S- Editor: Gong XM L- Editor: A E- Editor: Jiao XK
| 1. | Topalian SL, Hodi FS, Brahmer JR, Gettinger SN, Smith DC, McDermott DF, Powderly JD, Carvajal RD, Sosman JA, Atkins MB. Safety, activity, and immune correlates of anti-PD-1 antibody in cancer. N Engl J Med. 2012;366:2443-2454. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 8900] [Cited by in F6Publishing: 9309] [Article Influence: 775.8] [Reference Citation Analysis (0)] |
| 2. | Dunn GP, Old LJ, Schreiber RD. The three Es of cancer immunoediting. Annu Rev Immunol. 2004;22:329-360. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 1859] [Cited by in F6Publishing: 1881] [Article Influence: 94.1] [Reference Citation Analysis (0)] |
| 3. | Badoual C, Combe P, Gey A, Granier C, Roussel H, De Guillebon E, Oudard S, Tartour E. [PD-1 and PDL-1 expression in cancer: significance and prognostic value]. Med Sci (Paris). 2013;29:570-572. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 6] [Cited by in F6Publishing: 7] [Article Influence: 0.6] [Reference Citation Analysis (0)] |
| 4. | Keir ME, Butte MJ, Freeman GJ, Sharpe AH. PD-1 and its ligands in tolerance and immunity. Annu Rev Immunol. 2008;26:677-704. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 3785] [Cited by in F6Publishing: 3807] [Article Influence: 237.9] [Reference Citation Analysis (0)] |
| 5. | Hodi FS, O’Day SJ, McDermott DF, Weber RW, Sosman JA, Haanen JB, Gonzalez R, Robert C, Schadendorf D, Hassel JC. Improved survival with ipilimumab in patients with metastatic melanoma. N Engl J Med. 2010;363:711-723. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 10799] [Cited by in F6Publishing: 11106] [Article Influence: 793.3] [Reference Citation Analysis (0)] |
| 6. | Robert C, Thomas L, Bondarenko I, O’Day S, Weber J, Garbe C, Lebbe C, Baurain JF, Testori A, Grob JJ. Ipilimumab plus dacarbazine for previously untreated metastatic melanoma. N Engl J Med. 2011;364:2517-2526. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 3331] [Cited by in F6Publishing: 3269] [Article Influence: 251.5] [Reference Citation Analysis (0)] |
| 7. | Brahmer JR, Tykodi SS, Chow LQ, Hwu WJ, Topalian SL, Hwu P, Drake CG, Camacho LH, Kauh J, Odunsi K. Safety and activity of anti-PD-L1 antibody in patients with advanced cancer. N Engl J Med. 2012;366:2455-2465. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 5599] [Cited by in F6Publishing: 5891] [Article Influence: 490.9] [Reference Citation Analysis (0)] |
| 8. | Powles T, Eder JP, Fine GD, Braiteh FS, Loriot Y, Cruz C, Bellmunt J, Burris HA, Petrylak DP, Teng SL. MPDL3280A (anti-PD-L1) treatment leads to clinical activity in metastatic bladder cancer. Nature. 2014;515:558-562. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 1718] [Cited by in F6Publishing: 1823] [Article Influence: 202.6] [Reference Citation Analysis (0)] |
| 9. | Dong H, Strome SE, Salomao DR, Tamura H, Hirano F, Flies DB, Roche PC, Lu J, Zhu G, Tamada K. Tumor-associated B7-H1 promotes T-cell apoptosis: a potential mechanism of immune evasion. Nat Med. 2002;8:793-800. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 2838] [Cited by in F6Publishing: 3288] [Article Influence: 149.5] [Reference Citation Analysis (0)] |
| 10. | Droeser RA, Hirt C, Viehl CT, Frey DM, Nebiker C, Huber X, Zlobec I, Eppenberger-Castori S, Tzankov A, Rosso R. Clinical impact of programmed cell death ligand 1 expression in colorectal cancer. Eur J Cancer. 2013;49:2233-2242. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 286] [Cited by in F6Publishing: 344] [Article Influence: 31.3] [Reference Citation Analysis (0)] |
| 11. | Gatalica Z, Snyder CL, Yeatts K, Xiao N, Holterman D, Lynch HT. Programmed death 1 (PD-1) lymphocytes and ligand (PD-L1) in colorectal cancer and their relationship to microsatellite instability status. Available from: http://meetinglibrary.asco.org/content/133958-144. [Cited in This Article: ] |
| 12. | Nomi T, Sho M, Akahori T, Hamada K, Kubo A, Kanehiro H, Nakamura S, Enomoto K, Yagita H, Azuma M. Clinical significance and therapeutic potential of the programmed death-1 ligand/programmed death-1 pathway in human pancreatic cancer. Clin Cancer Res. 2007;13:2151-2157. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 645] [Cited by in F6Publishing: 674] [Article Influence: 39.6] [Reference Citation Analysis (0)] |
| 13. | Ohigashi Y, Sho M, Yamada Y, Tsurui Y, Hamada K, Ikeda N, Mizuno T, Yoriki R, Kashizuka H, Yane K. Clinical significance of programmed death-1 ligand-1 and programmed death-1 ligand-2 expression in human esophageal cancer. Clin Cancer Res. 2005;11:2947-2953. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 566] [Cited by in F6Publishing: 615] [Article Influence: 32.4] [Reference Citation Analysis (0)] |
| 14. | Muro K, Bang YJ, Shankaran V, Geva R, Catenacci DVT, Gupta S, Eder JP, Berger R, Gonzalez EJ, Ray A. Relationship between PD-L1 expression and clinical outcomes in patients (Pts) with advanced gastric cancer treated with the anti-PD-1 monoclonal antibody pembrolizumab (Pembro; MK-3475) in KEYNOTE-012. Available from: http://meetinglibrary.asco.org/content/140536-158. [Cited in This Article: ] |
| 15. | Lutzky J, Antonia SJ, Blake-Haskins A, Li X, Robbins PB, Shalabi AM, Vasselli J, Ibrahim RA, Khleif S, Segal NH. A phase 1 study of MEDI4736, an anti–PD-L1 antibody, in patients with advanced solid tumors. Available from: http://meetinglibrary.asco.org/content/133649-144. [Cited in This Article: ] |
| 16. | Herbst RS, Soria JC, Kowanetz M, Fine GD, Hamid O, Gordon MS, Sosman JA, McDermott DF, Powderly JD, Gettinger SN. Predictive correlates of response to the anti-PD-L1 antibody MPDL3280A in cancer patients. Nature. 2014;515:563-567. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 3369] [Cited by in F6Publishing: 3871] [Article Influence: 430.1] [Reference Citation Analysis (0)] |
| 17. | Wolchok JD, Hoos A, O’Day S, Weber JS, Hamid O, Lebbé C, Maio M, Binder M, Bohnsack O, Nichol G. Guidelines for the evaluation of immune therapy activity in solid tumors: immune-related response criteria. Clin Cancer Res. 2009;15:7412-7420. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 2311] [Cited by in F6Publishing: 2361] [Article Influence: 157.4] [Reference Citation Analysis (0)] |
| 18. | Eggermont AM, Chiarion-Sileni V, Grob JJ, Dummer R, Wolchok JD, Schmidt H, Hamid O, Robert C, Ascierto PA, Richards JM. Ipilimumab versus placebo after complete resection of stage III melanoma: Initial efficacy and safety results from the EORTC 18071 phase III trial. Available from: http://meetinglibrary.asco.org/content/130118-144. [Cited in This Article: ] |
| 19. | Granier C, Roussel H, de Guillebon E, Ladoire S, Combe P, Vano Y, Fabre E, Oudard S, Badoual C, Tartour E. Biomarkers from the tumor microenvironment to predict clinical response to checkpoint inhibitors. J OncoPathology. 2014;2. [DOI] [Cited in This Article: ] |
| 20. | Tumeh PC, Harview CL, Yearley JH, Shintaku IP, Taylor EJ, Robert L, Chmielowski B, Spasic M, Henry G, Ciobanu V. PD-1 blockade induces responses by inhibiting adaptive immune resistance. Nature. 2014;515:568-571. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 4180] [Cited by in F6Publishing: 4796] [Article Influence: 532.9] [Reference Citation Analysis (0)] |
| 21. | Tougeron D, Fauquembergue E, Rouquette A, Le Pessot F, Sesboüé R, Laurent M, Berthet P, Mauillon J, Di Fiore F, Sabourin JC. Tumor-infiltrating lymphocytes in colorectal cancers with microsatellite instability are correlated with the number and spectrum of frameshift mutations. Mod Pathol. 2009;22:1186-1195. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 115] [Cited by in F6Publishing: 124] [Article Influence: 8.3] [Reference Citation Analysis (0)] |
| 22. | Llosa NJ, Cruise M, Tam A, Wicks EC, Hechenbleikner EM, Taube JM, Blosser RL, Fan H, Wang H, Luber BS. The vigorous immune microenvironment of microsatellite instable colon cancer is balanced by multiple counter-inhibitory checkpoints. Cancer Discov. 2015;5:43-51. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 889] [Cited by in F6Publishing: 1045] [Article Influence: 104.5] [Reference Citation Analysis (0)] |