Published online Jun 28, 2008. doi: 10.3748/wjg.14.3922
Revised: May 30, 2008
Accepted: June 6, 2008
Published online: June 28, 2008
This case report describes a 69-year-old man presen-ting with an extensive subcutaneous emphysema in his neck and generalized peritonitis caused by a lower gastrointestinal tract perforation. This case emphasizes that subcutaneous emphysema patients with negative thoracic findings should be scrutinized for signs of retroperitoneal hollow viscus perforation.
- Citation: Schmidt GB, Bronkhorst MW, Hartgrink HH, Bouwman LH. Subcutaneous cervical emphysema and pneumomediastinum due to a lower gastrointestinal tract perforation. World J Gastroenterol 2008; 14(24): 3922-3923
- URL: https://www.wjgnet.com/1007-9327/full/v14/i24/3922.htm
- DOI: https://dx.doi.org/10.3748/wjg.14.3922
Pneumomediastinum usually occurs following esopha-geal or chest trauma. It can also occur spontaneously in association with asthma, excessive coughing, or straining. Cervical emphysema occurs when air moves through tissue planes into subcutaneous areas of the face and neck. Subcutaneous neck emphysema, pneumomediastinum, and retropneumoperitoneum have been reported infrequently following colonoscopic perforation. Iatrogenic colonic perforation is a serious but rare complication of colonoscopy. A perforation risk rate of 0.12% has been reported[1].
Subcutaneous emphysema caused by non-traumatic perforations of the colon is extremely rare. However, it should be considered when no obvious case can be found for the origin of subcutaneous emphysema or a pneumomediastinum.
A 69-year-old man presented himself at the Accident and Emergency Department with a 6-h history of swelling in the neck, an altered voice and abdominal pain. He was treated for a painful fifth rib on the left which was caused by a metastasis of an unknown primary tumor. Analysis for the primary tumor was ongoing, but not yet concluded. Radiotherapy was started and prednisolone was prescribed.
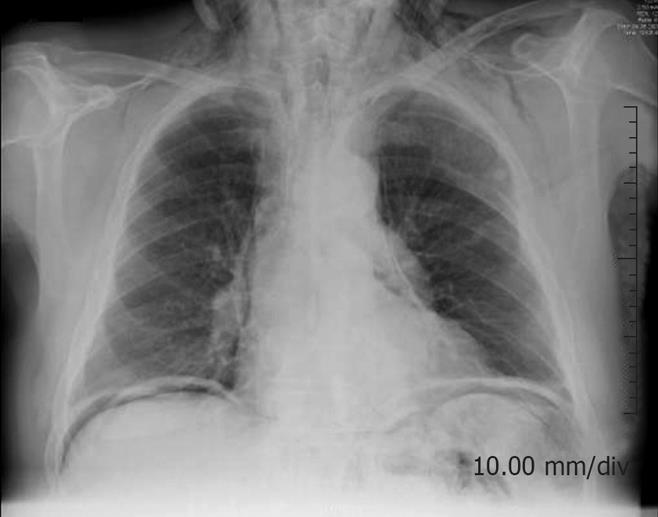
Physical examination revealed signs of extensive subcutaneous emphysema in his neck and generalized peritonitis. Laboratory blood and urine tests were normal apart from an elevated white cell count of 23 × 109 cells/L. A plain radiograph of the thorax showed free intraperitoneal air, pneumomediastinum and extensive subcutaneous emphysema, but no sign of pneumothorax (Figure 1).
An explorative laparotomy was performed, a perforation of the small bowel and the caecum was found, which were oversew. There were two perforations of the sigmoid but no palpable tumor. A sigmoid resection was performed with a permanent colostomy. The proximal end of the distal segment was oversew and left in place with a blind rectal pouch. The patient was admitted to the Intensive Care Unit after operation. Pathological examination showed diverticulitis with a perforation, and no tumor was found in the resected sigmoid.
After consultation with the patient and his family, the patient received no further surgical treatment. The patient died of respiratory arrest 12 d after surgery.
Non-traumatic subcutaneous emphysema is a rare presentation of lower gastrointestinal tract perforation due to colorectal cancer or diverticulitis[2–6].
As the rectosigmoid is located in the retroperito-neum, injury can be present in the absence of peritonitis. Mediastinal and cervical emphysema may develop due to dissection of air via contiguous tissue planes, which occurs along the perivascular adventitia to the anterior pararenal space, through the diaphragmatic hiatus along the adventitia of great vessels to the mediastinum and pericardium/or pretracheal fascia to the neck[78]. Subcutaneous emphysema patients with negative thoracic findings should be scrutinized for signs of retroperitoneal hollow viscus perforation to improve their outcome.
| 1. | Lüning TH, Keemers-Gels ME, Barendregt WB, Tan AC, Rosman C. Colonoscopic perforations: a review of 30,366 patients. Surg Endosc. 2007;21:994-997. |
| 2. | Chu S, Glare P. Subcutaneous emphysema in advanced cancer. J Pain Symptom Manage. 2000;19:73-77. |
| 3. | Morita T, Matsuda T, Tei Y, Takada T. Nontraumatic subcutaneous emphysema from rectal cancer perforation completely resolved after intensive pain control. J Pain Symptom Manage. 2006;32:3-4. |
| 4. | Hur T, Chen Y, Shu GH, Chang JM, Cheng KC. Spontaneous cervical subcutaneous and mediastinal emphysema secondary to occult sigmoid diverticulitis. Eur Respir J. 1995;8:2188-2190. |
| 5. | Nedrebø T. [Subcutaneous emphysema in gastrointestinal tract perforation]. Tidsskr Nor Laegeforen. 1992;112:2855-2856. |
| 6. | Pretre R, Rohner A. [Pneumomediastinum and subcuta-neous cervical emphysema as signs of rectosigmoid perforation]. Gastroenterol Clin Biol. 1992;16:460-462. |
| 7. | Fitzgerald SD, Denk A, Flynn M, Longo WE, Vernava AM 3rd. Pneumopericardium and subcutaneous emphysema of the neck. An unusual manifestation of colonoscopic perforation. Surg Endosc. 1992;6:141-143. |