Copyright
©2008 The WJG Press and Baishideng.
World J Gastroenterol. Jun 7, 2008; 14(21): 3306-3312
Published online Jun 7, 2008. doi: 10.3748/wjg.14.3306
Published online Jun 7, 2008. doi: 10.3748/wjg.14.3306
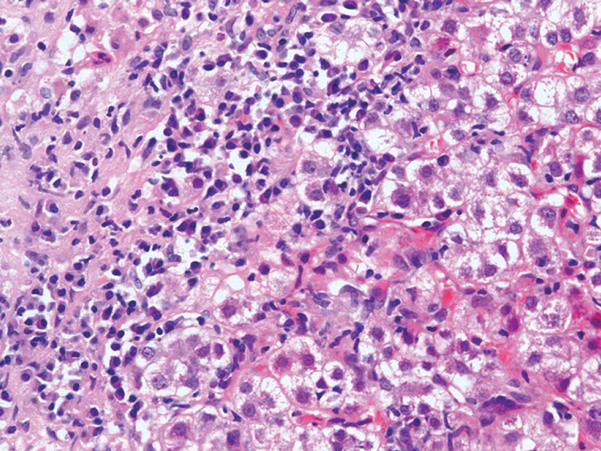
Figure 1 The portal and periportal inflammatory infiltrate characteristic of autoimmune hepatitis is composed by lymphocytes and plasma cells (interface hepatitis) (HE, × 40, provided by Dr.
Alberto Quaglia).
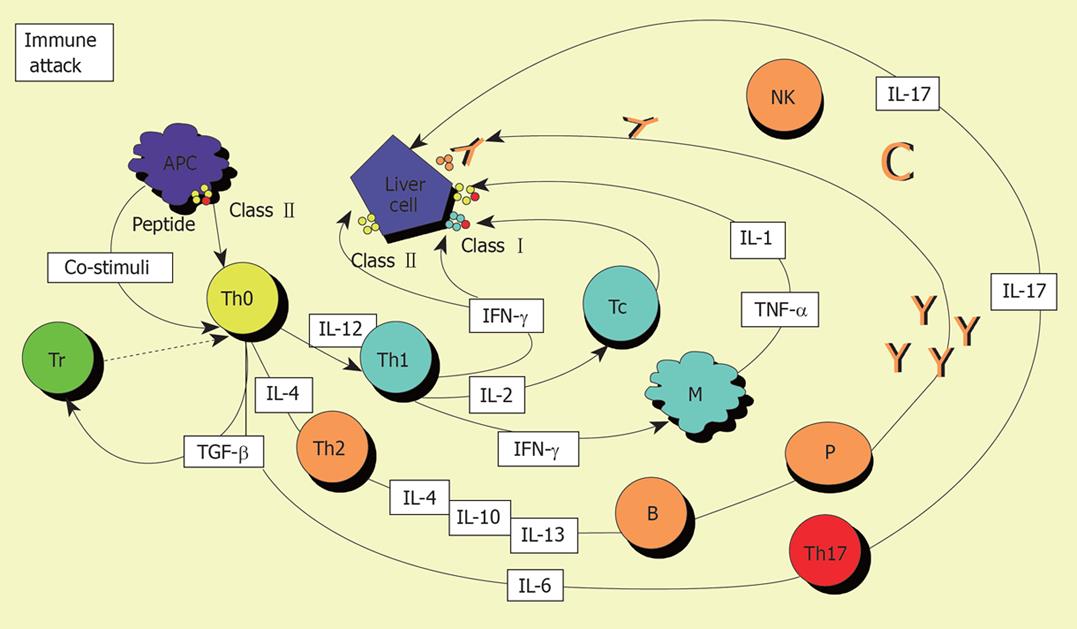
Figure 2 Autoimmune attack to the liver cell.
A specific autoantigenic peptide is presented to an uncommitted T helper (Th0) lymphocyte within the HLA class II molecule of an antigen-presenting cell (APC). Th0 cells become activated and, according to the presence in the microenvironment of IL-12 or IL-4 and the nature of the antigen, differentiate into Th1 or Th2 and initiate a series of immune reactions determined by the cytokines they produce: Th2 secrete mainly IL-4, IL-10 and IL-13, and direct autoantibody production by B lymphocytes; Th1 secrete IL-2 and IFN-γ, which stimulate T cytotoxic (Tc) lymphocytes, enhance expression of class I and induce expression of class II HLA molecules on hepatocytes and activate macrophages; activated macrophages release IL-1 and tumour necrosis factor alpha (TNF-α). If regulatory T cells do not oppose, a variety of effector mechanisms are triggered: liver cell destruction could derive from the action of Tc lymphocytes; cytokines released by Th1 and recruited macrophages; complement activation or engagement of Fc receptor-bearing cells such as natural killer (NK) lymphocytes by the autoantibody bound to the hepatocyte surface. The role of the recently described Th17 cells, which arise in the presence of transforming growth factor beta (TGF-β) and IL-6, is under investigation.
- Citation: Vergani D, Mieli-Vergani G. Aetiopathogenesis of autoimmune hepatitis. World J Gastroenterol 2008; 14(21): 3306-3312
- URL: https://www.wjgnet.com/1007-9327/full/v14/i21/3306.htm
- DOI: https://dx.doi.org/10.3748/wjg.14.3306