Published online Oct 18, 2015. doi: 10.5312/wjo.v6.i9.744
Peer-review started: March 15, 2015
First decision: April 17, 2015
Revised: July 15, 2015
Accepted: July 21, 2015
Article in press: July 23, 2015
Published online: October 18, 2015
We report a case of Ewings sarcoma (ES) involving the patella in a young female. ES of patella is a rare entity. The patient was presented with anterior knee pain and swelling arising from the patella. She was treated with neoadjuvant chemotherapy followed by wide excision of the patella and reconstruction of the extensor mechanism using split tendoachilles auto graft. The patella is an uncommon site for primary or metastatic tumors of the bone. ES, though rare, should be included in the differential diagnosis of swellings arising from the patella. Auto graft from the tendoachilles is a good alternative for reconstructing the extensor mechanism of the knee.
Core tip: We are presenting an article of Ewings sarcoma (ES) of the patella-a rare entity treated by a novel technique. The common reported tumors of the patella include chondroblastoma, giantcell tumor, osteosarcoma, metastasis, etc. We could not find any report on a single case of ES/PNET in the patella treated with patellectomy and extensor mechanism reconstruction using tendoachilles auto graft in the whole of English bio-medical literature. We present here a case of ES of the right patella in a 26 years old female. All reported extensor mechanism reconstructions after patellectomy were by tendoachilles allografts. We resorted to a novel technique of reconstruction of the extensor mechanism using tendoachilles auto graft.
- Citation: Valsalan RM, Zacharia B. Ewings sarcoma of patella: A rare entity treated with a novel technique of extensor mechanism reconstruction using tendoachilles auto graft. World J Orthop 2015; 6(9): 744-749
- URL: https://www.wjgnet.com/2218-5836/full/v6/i9/744.htm
- DOI: https://dx.doi.org/10.5312/wjo.v6.i9.744
Ewings sarcoma (ES) was first described by Ewing[1] in 1921 as a “diffuse endothelioma of bone”. The origin of these tumors is not definitively known. The two theories which support its origin suggest that these tumors arise from a primitive cell derived either from an embryologic tissue called the neural crest, or from resident cells in the body-mesenchymal stem cells. But it is not clear if this tumor is of mesenchymal or neuroectodermal origin. Now it has become clear that these entities comprise the same spectrum of neoplastic diseases known as the Ewing sarcoma family of tumors (EFT), which also includes malignant small-cell tumor of the chest wall (Askin tumor) and atypical ES[2,3]. The incidence of Ewing sarcoma is approximately three cases per 1 million per year[4]. EFT usually arises from the diaphysis or metadiaphyseal region of long bones. It also arises from the pelvic bones and ribs[2]. The patella is an uncommon site for primary or metastatic tumors of the bone. The fact that the patella is a sesamoid bone, developing from an endochondral centre with a relatively short period of growth, plays a role in making patella a least preferred site for primary tumors[5,6]. Primary tumors account for less than 0.06% of all bone tumors while metastatic lesions are even rarer[7]. We report a case of ES involving the patella in a young female. ES is a relatively uncommon tumour accounting for 6%-8% of primary malignant bone tumors[8]. Tumors of the patella are a rare cause of knee pain. Information available in the literature is largely in the form of isolated case reports and small case studies because of the rarity of patellar tumors[9,10]. Epiphysial tumors such as giant cell tumors and chondroblastomas are more common in the patella[11]. Christensen hypothesized that the immunity of patella to bone tumors is due to the absence of loss of growth restraint incident to active diaphysial growth and pressure epiphysis[5,6]. We were unable to find any documentation of ES of the patella treated with wide excision and extensor mechanism reconstruction using tendoachilles auto graft in the English medical literature. We discuss a case of ES of the patella in a 26 years old female.
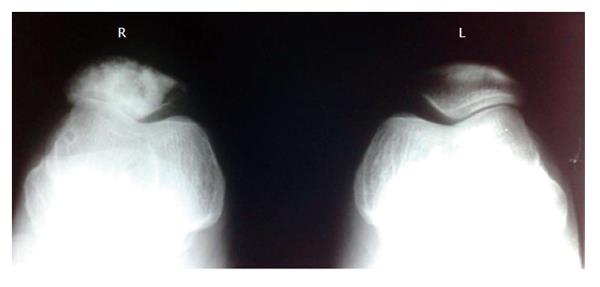
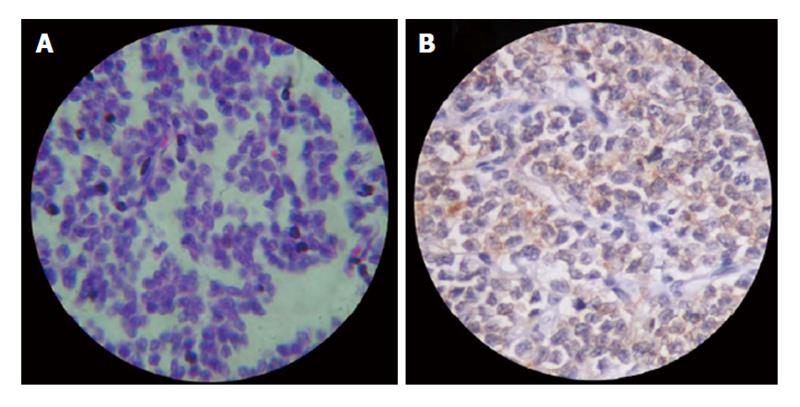
A 26 years old woman complained of anterior knee pain and swelling arising from the anterior aspect of right knee joint for the past two months. A private physician diagnosed prepatellar bursitis and treated with anti-inflammatory medications and rest that gave symptomatic relief for few days. At three months duration, patient noticed progressive increase in the size of the swelling and was referred to our institution. Initial examination showed a 19 cm × 16 cm × 10 cm firm, tender and warm swelling in the anterior aspect of right knee. Swelling was found to be arising from the right patella. There was no fixity to the skin. The movements of right knee were painful and the pain was worse while going up or downstairs and in squatting positions. The patient walked with a limp and preferred keeping the leg in an extended position. There was painful restriction of passive flexion beyond 90 degrees. Active movements showed a flexion of 70 degrees restricted by pain. There was no effusion, joint line tenderness or synovial thickening. Regional lymph nodes were not involved clinically and there was no distal neurovascular deficit. Routine hematological investigations were within normal limits. Radiographs showed multiple lytic and sclerotic lesions with ill-defined margins involving the anterior two-thirds of the patella (Figure 1). Computer tomography (CT) of the right knee joint showed destruction of patella with sclerotic and lytic lesions with intact posterior cortex. Magnetic resonance imaging showed the tumor mass involving the patella with an anterior soft tissue extension. There were no skip or satellite lesions. The possibility of either a primary malignancy of patella or metastatic lesion was considered. Clinical examination failed to reveal any primary for a metastatic lesion in the patella. CT of abdomen and chest were negative. As fine needle aspiration cytology gave inconclusive results, an incision biopsy was performed under lumbar subarachnoid block through anterior midline approach. Histopathology reports were suggestive of small round cell tumor possibly ES (Figure 2A). The tumour was classified as stage IIA as per the tumour staging by Enneking[10]. After four cycles of neoadjuvant chemotherapy with Vincristin, Adriamycin and Cyclophosphamide, wide excision of the tumor was done. Preoperative injection of 1 g cefazolin was given 30 min prior to surgery. Surgery was done under lumbar subarachnoid block. Patient was in supine position with a pillow underneath the right buttock. A longitudinal midline incision extending 15 cm above to 10 cm below the right patella was made and a wide excision of the tumor mass including the whole patella, anterior soft tissue mass, 5 cm of quadriceps tendon beyond tumor margin and patellar tendon was done.
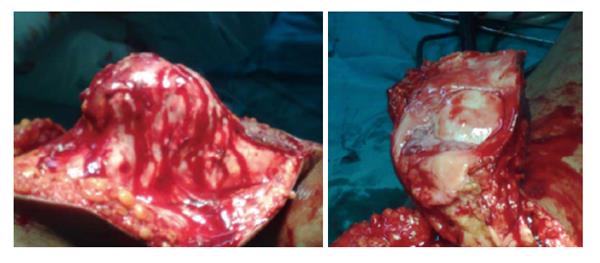
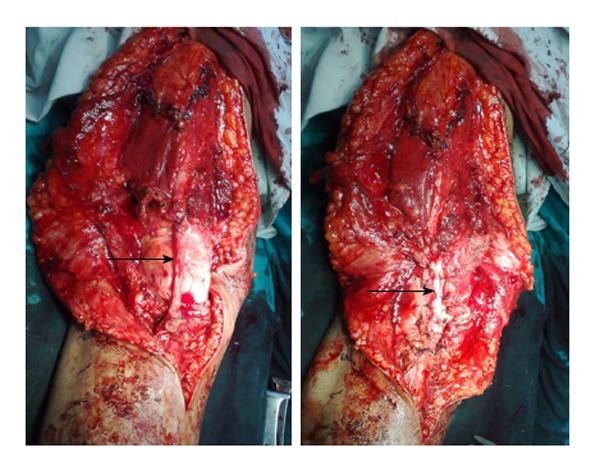
Intraoperatively, we found a 14 cm × 12 cm × 8 cm mass arising from the anterior aspect of right patella. The articular surface of the patella was grossly uninvolved (Figure 3). The whole patella appeared thickened with a soft tissue mass adherent to it. There was no involvement of the overlying skin. Intra operative frozen section showed that margins of resected specimen are free of tumor. This wide excision has created a 20 cm defect in the extensor mechanism of the knee. Then we opened the right tendoachilles tendon through a psterolateral 20 cm long incision. We took a 15 cm long lateral half of tendoachilles tendon as a graft. Extensor mechanism reconstruction was done with a V-Y quadriceps lengthening at musculo-tendinous junction and repair of defect using split graft taken from ipsilateral tendoachilles (Figure 4). The whole procedure took about two hours and a half and no tourniquet was used.
Postoperatively, right leg was immobilized in a long leg cast for six weeks followed by physiotherapy to regain the quadriceps power. She regained about 80 degrees of knee flexion and walked with support of a cane. She had 10 degrees of extension lag with no donor site morbidity. Postoperatively, adjuvant chemotherapy was started on with alternating regimen of vincristin, adriamycin, cyclophosphamide and ifosfamide, etoposide. After 12 mo she complained of recurrent backache. A Bone scan showed multiple metastatic lesions at different skeletal sites like cervical and thoracic vertebrae, scapula, pelvis and base of skull. Bone pain was treated symptomatically in consultation with the radiotherapy department. At two years follow-up, the patient is walking with cane support. There are no clinical or radiological evidences of local recurrence. CT thorax did not show any evidence of lung metastasis. Grossly, the resected specimen showed firm grey-white lesion arising from the patella with areas of hemorrhage and cystic degeneration. The extra osseous soft tissue component was soft and friable. Microscopy showed broad sheets and large nests of uniform, small, polygonal cells with scanty pale cytoplasm and indistinct cell borders (Figure 2A). There were also areas of rosette formation. The specimen margins were free of tumor tissue. Immunohistochemical examination of the specimen showed CD99 diffuse positivity that favored the diagnosis of ES (Figures 2B and 4).
Primary malignant tumors of patella are rare entity[12]. The fact that the patella is a sesamoid bone, developing from an endochondral centre with a relatively short period of growth plays a role in making patella a least preferred site for primary tumors[13,14]. Chondroblastomas and giant cell tumors form the most common tumors of the patella[12-14]. This is probably due to the similarity in the ossification of the patella with that of the epiphysis of long bones[11]. There are reports of tumors like osteoid osteoma, osteoblastoma, spindle cell sarcoma, osteitisfibrosacystica, aneurysmal bone cyst and myelomatous infiltration arising from the patella[15-20]. Osteosarcoma is the most frequent primary malignant tumor of patella[9]. Other reported primary malignant neoplasms are hemangioendothelioma, malignant fibrous histiocytoma and angiosarcoma[21]. Systemic lesions such as lymphoma and plasmacytoma may also involve patella[9]. There are several reports of metastasis to the patella from sites like kidney, lung, eye, prostate, breast and uterus[9,22-24]. However, documentation of ES of patella in the English medical literature is lacking. Chronic anterior knee pain is the most common presenting feature in patients with patellar tumors[11]. The prognosis for patellar tumors is good even though most of the cases appear late, as majority of the tumors are benign[11]. The outcome following a malignant tumor of the patella and the need of an immediate surgical intervention remain unanswered due to lack of adequate literature. ES is the third most common primary sarcoma of the bone after osteosarcoma and chondrosarcoma[25]. Approximately 80% of patients afflicted are younger than 20 years of age[26]. ES is now thought to be least differentiated of a group of small cell neoplasms with varying degrees of neuroectodermal differentiation. ES typically affects diaphysis of long bones. Epiphyseal ES is a rare entity[27]. Usual clinical features include pain and swelling associated with fever, anemia and leukocytosis. Radiological picture of ES consists of mixed sclerotic and lytic lesions. An ill-defined osteolytic lesion involving the diaphysis of a long bone or flat bone is the most common feature. ES is characterized by a recurrent (11:22) (q24:12) chromosomal translocation, which is detectable in 85% of cases[28]. ES has a strong potential to metastasize mostly to the lungs and bone. More than 10% of patients present with multiple bone metastases at initial diagnosis. While metastases in the lungs, bone, bone marrow, or a combination thereof are detectable in approximately 25% of patients, metastases to lymph nodes are rare[26]. Microscopically, classic ES consist of broad sheets and nests of uniform, small, polygonal cells with scanty pale cytoplasm and indistinct cell borders. About 10% of cases contain rosette-like structures that in reality represent necrotic cell “dropout” of a central mass. CD99 is one of the most sensitive markers for the diagnosis of ES[29,30]. It is expressed in almost all cases. They have also shown to express neural markers such as neuron specific enolase[8]. But these markers are less sensitive. The tumour can be staged according to the tumour staging by Enneking[31]. Extensive patellectomy with removal of the distal part of the quadriceps tendon, the proximal part of the patellar tendon, and the overlying patellar fascia is necessary in patients with Stage IIA tumors because these neoplasms might have satellites in the peripheral, reactive zone[9]. Surgical excision of the patellar tumor is justified in view of its location in an expendable bone[32]. Patella is an important part of the extensor mechanism. It seems logical to combine patellectomy with extensor mechanism reconstruction or reinforcements[33]. Whenever patellectomy is indicated. Several methods of extensor mechanism reconstruction like Z-plasty or cruciate plasty or fascia lata graft or vastusmedialisobliquus advancement have been described. Repair of the extensor mechanism using Achilles tendon allografts has produced good results[34,35]. We repaired the gap in the extensor mechanism following tumor excision using V-Y quadriceps plasty and ipsilateral split tendoachilles auto graft. Split tendoachilles auto graft is good option for reconstructing the extensor mechanism in places where allograft is not available. It has got advantages like ease of harvesting, free availability, good strength, low graft site morbidity and no issues related to disease transmission and graft rejection. Here we have a young lady with ES of the patella, which has not been reported earlier. The tumor being localized to the patella was excised along with a part of quadriceps and patellar tendon followed by extensor mechanism reconstruction using quadriceps lengthening and split tendoachilles auto graft after neoadjuvant chemotherapy. Two years after surgery, patient is able to carry out her activities of daily life. She is on regular follow up. There are only two cases of ES of patella reported previously of which one is a case associated with nail patella syndrome[36,37].
Primary malignant tumors of the patella are very rare. ES of the patella is a rare entity. Extensor mechanism reconstruction using split tendoachilles auto graft following excision of the patellar tumor is an effective technique. ES, though rare, should be included in the differential diagnosis of swellings arising from the patella.
A 26 years old woman presented with pain and swelling in the right knee for the past two months.
On examination there was a 19 cm × 16 cm × 10 cm warm tender swelling in the anterior aspect of the right knee.
Her radiograph and computer tomography showed multiple lytic and sclerotic lesions in the patella. Also, magnetic resonance imaging showed tumor in the patella with anterior soft tissue extension. Histopathology confirmed small round cell tumor - Ewings sarcoma with CD99 positivity in immunohistochemistry.
She was treated by a wide excision of tumor along with patella and resulted gap was repaired using tendoachilles auto graft taken from the ipsilateral side and a V-Y quadriceps lengthening.
This report is presented due to the rarity of patellar tumors and highlights the usefulness of tendoachilles auto graft in treating extensor mechanism defects of knee, especially after wide excision of tumors of patella.
The paper gives detail as to the biopsy results and method to treat plus basic follow up information.
P- Reviewer: Cartmell S, Gokkus K, Ohishi T S- Editor: Ji FF L- Editor: A E- Editor: Liu SQ
| 1. | Ewing J. Diffuse endothelioma of bone. Proc NY Pathol Soc. 1921;21:17-24. [Cited in This Article: ] |
| 2. | Desai SS, Jambhekar NA. Pathology of Ewing’s sarcoma/PNET: Current opinion and emerging concepts. Indian J Orthop. 2010;44:363-368. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 62] [Cited by in F6Publishing: 68] [Article Influence: 4.9] [Reference Citation Analysis (0)] |
| 3. | Llombart-Bosch A, Lacombe MJ, Contesso G, Peydro-Olaya A. Small round blue cell sarcoma of bone mimicking atypical Ewing’s sarcoma with neuroectodermal features. An analysis of five cases with immunohistochemical and electron microscopic support. Cancer. 1987;60:1570-1582. [PubMed] [Cited in This Article: ] |
| 4. | Suvà ML, Riggi N, Stehle JC, Baumer K, Tercier S, Joseph JM, Suvà D, Clément V, Provero P, Cironi L. Identification of cancer stem cells in Ewing’s sarcoma. Cancer Res. 2009;69:1776-1781. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 231] [Cited by in F6Publishing: 224] [Article Influence: 14.9] [Reference Citation Analysis (0)] |
| 5. | Christensen FC. Bone tumors: analysis of one thousand cases with special reference to location, age and sex. Ann Surg. 1925;81:1074-1092. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 34] [Cited by in F6Publishing: 39] [Article Influence: 2.3] [Reference Citation Analysis (0)] |
| 6. | Goodwin MA. Primary Osteosarcoma of the patella. J Bone Joint Surg Br. 1961;43B:338-341. [Cited in This Article: ] |
| 7. | Saglik Y, Yildiz Y, Basarir K, Tezen E, Güner D. Tumours and tumour-like lesions of the patella: a report of eight cases. Acta Orthop Belg. 2008;74:391-396. [PubMed] [Cited in This Article: ] |
| 8. | Fletcher CDM, Krishnan Unn K, Mertens F. World Health Organisation Classification of Tumors. Pathology and genetics of tumors of soft tissue and bone.,vol. IARC Press: Lyon 2002; . [Cited in This Article: ] |
| 9. | Mercuri M, Casadei R. Patellar tumors. Clin Orthop Relat Res. 2001;35-46. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 51] [Cited by in F6Publishing: 55] [Article Influence: 2.4] [Reference Citation Analysis (0)] |
| 10. | O’Mara JW, Keeling J, Montgomery EA, Aaron AD. Primary lesions of the patella. Orthopedics. 2000;23:328, 348, 370, 376-377. [PubMed] [Cited in This Article: ] |
| 11. | Bhagat S, Sharma H, Bansal M, Reid R. Presentation and outcome of primary tumors of the patella. J Knee Surg. 2008;21:212-216. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 14] [Cited by in F6Publishing: 15] [Article Influence: 0.9] [Reference Citation Analysis (0)] |
| 12. | Mercuri M, Casadei R, Ferraro A, de Cristofaro R, Balladelli A, Picci P. Tumours of the patella. Int Orthop. 1991;15:115-120. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 20] [Cited by in F6Publishing: 23] [Article Influence: 0.7] [Reference Citation Analysis (0)] |
| 13. | Kransdorf MJ, Moser RP, Vinh TN, Aoki J, Callaghan JJ. Primary tumors of the patella. A review of 42 cases. Skeletal Radiol. 1989;18:365-371. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 51] [Cited by in F6Publishing: 51] [Article Influence: 1.5] [Reference Citation Analysis (0)] |
| 14. | Cole WH. Primary Tumors of the Patella. J Bone Joint Surg Am. 1925;7:637-654. [Cited in This Article: ] |
| 15. | Vallianatos PG, Tilentzoglou AC, Seitaridis SV, Mahera HJ. Osteoid osteoma of the patella: a case report. Knee Surg Sports Traumatol Arthrosc. 2006;14:161-164. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 9] [Cited by in F6Publishing: 12] [Article Influence: 0.7] [Reference Citation Analysis (0)] |
| 16. | Kelikian H, Clayton I. Giant-cell tumor of the patella. J Bone Joint Surg Am. 1957;39-A:414-420. [PubMed] [Cited in This Article: ] |
| 17. | Desnoyers V, Charissoux JL, Aribit F, Arnaud JP. [Aneurysmal bone cyst of the patella. A case report and literature review]. Rev Chir Orthop Reparatrice Appar Mot. 2000;86:616-620. [PubMed] [Cited in This Article: ] |
| 18. | Trebse R, Rotter A, Pisot V. Chondroblastoma of the patella associated with an aneurysmal bone cyst. Acta Orthop Belg. 2001;67:290-296. [PubMed] [Cited in This Article: ] |
| 19. | Marudanayagam A, Gnanadoss JJ. Secondary aneurysmal bone cyst of the patella: a case report. Iowa Orthop J. 2006;26:144-146. [PubMed] [Cited in This Article: ] |
| 20. | Linscheid RL, Dahlin DC. Unusual lesions of the patella. J Bone Joint Surg Am. 1966;48:1359-1366. [PubMed] [Cited in This Article: ] |
| 21. | Ferguson PC, Griffin AM, Bell RS. Primary patellar tumors. Clin Orthop Relat Res. 1997;199-204. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 40] [Cited by in F6Publishing: 43] [Article Influence: 1.6] [Reference Citation Analysis (0)] |
| 22. | Lim CT, Wong AS, Chuah BY, Putti TC, Stanley AJ, Nathan SS. The patella as an unusual site of renal cell carcinoma metastasis. Singapore Med J. 2007;48:e314-e319. [PubMed] [Cited in This Article: ] |
| 23. | Jaeger HJ, Kreugener GH. Solitary metastasis of the patella as the first manifestation of lung cancer. Int Orthop. 1991;15:179. [PubMed] [Cited in This Article: ] |
| 24. | George MK, Venkitaraman R, Chandra A, Sagar TG. Late solitary skeletal metastasis to the patella from retinoblastoma. J Indian Med Assoc. 2008;106:313-314. [PubMed] [Cited in This Article: ] |
| 25. | Committee JMT. The Incidence of BoneTumors in Japan. Tokyo: Japan 2003; . [Cited in This Article: ] |
| 26. | Iwamoto Y. Diagnosis and treatment of Ewing’s sarcoma. Jpn J Clin Oncol. 2007;37:79-89. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 137] [Cited by in F6Publishing: 148] [Article Influence: 8.7] [Reference Citation Analysis (0)] |
| 27. | Fechner RE, Mills SE. Tumors ofbones and joints. Atlas of Tumor Pathology. 3rd Series, Fasc 8 ed. Washington, DC: AFIP 1993; . [Cited in This Article: ] |
| 28. | Aurias A, Rimbaut C, Buffe D, Dubousset J, Mazabraud A. [Translocation of chromosome 22 in Ewing’s sarcoma]. C R Seances Acad Sci III. 1983;1105-2547. [Cited in This Article: ] |
| 29. | Collins BT, Cramer HM, Frain BE, Davis MM. Fine-needle aspiration biopsy of metastatic Ewing’s sarcoma with MIC2 (CD99) immunocytochemistry. Diagn Cytopathol. 1998;19:382-384. [PubMed] [Cited in This Article: ] |
| 30. | Enneking WF. A system of staging musculoskeletal neoplasms. Instr Course Lect. 1988;37:3-10. [PubMed] [Cited in This Article: ] |
| 31. | de Alava E. Diagnosis of small round cell tumors of bone. Curr Diagn Pathol. 2001;7:251-261. [DOI] [Cited in This Article: ] [Cited by in Crossref: 1] [Cited by in F6Publishing: 1] [Article Influence: 0.0] [Reference Citation Analysis (0)] |
| 32. | Link MPGH, Donaldson SS. Sarcomas of bone. Clinical Pediatric oncology. 4th 261 edn. St. Louis, Missouri: Mosby Year Book 1991; 559-576. [Cited in This Article: ] |
| 33. | Günal I, Karatosun V. Patellectomy: an overview with reconstructive procedures. Clin Orthop Relat Res. 2001;74-78. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 32] [Cited by in F6Publishing: 32] [Article Influence: 1.4] [Reference Citation Analysis (0)] |
| 34. | Lewis PB, Rue JP, Bach BR. Chronic patellar tendon rupture: surgical reconstruction technique using 2 Achilles tendon allografts. J Knee Surg. 2008;21:130-135. [PubMed] [Cited in This Article: ] |
| 35. | Falconiero RP, Pallis MP. Chronic rupture of a patellar tendon: a technique for reconstruction with Achilles allograft. Arthroscopy. 1996;12:623-626. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 67] [Cited by in F6Publishing: 68] [Article Influence: 2.4] [Reference Citation Analysis (0)] |
| 36. | Gorelik N, Dickson BC, Wunder JS, Bleakney R. Ewing’s sarcoma of the patella. Skeletal Radiol. 2013;42:729-733. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 4] [Cited by in F6Publishing: 5] [Article Influence: 0.5] [Reference Citation Analysis (0)] |