Published online May 28, 2013. doi: 10.4329/wjr.v5.i5.226
Revised: April 1, 2011
Accepted: April 8, 2011
Published online: May 28, 2013
Intracranial arterial occlusion is rarely encountered in association with head injury. Only six cases of traumatic occlusion of the anterior cerebral artery (ACA) have previously been reported. In this paper, the authors describe a case of a posttraumatic occlusion of ACA. A 35-year-old male presented to the emergency room with severe head injury. Computed tomography (CT) scan displayed diffuse brain swelling with multiple skull fractures. Follow up CT scan showed extensive cerebral infarction in the territory of ACA. The patient underwent CT angiography that demonstrated occlusion of the ACA by a fracture of the anterior fossa. He died after 3 d. ACA traumatic occlusion is a rare condition, with poor prognosis. In this case, fracture was responsible for dissection and direct obstruction of the artery.
- Citation: Paiva WS, de Andrade AF, Soares MS, Amorim RL, Figueiredo EG, Teixeira MJ. Occlusion of the anterior cerebral artery after head trauma. World J Radiol 2013; 5(5): 226-228
- URL: https://www.wjgnet.com/1949-8470/full/v5/i5/226.htm
- DOI: https://dx.doi.org/10.4329/wjr.v5.i5.226
Intracranial arterial occlusion is rare associated with head injury[1,2]. The incidence of this condition with cerebral ischemia in the literature range from 0.2% to 1.6%[3,4]. Most injuries occur in the internal carotid artery, followed by the middle cerebral artery and the vertebrobasilar vessels[1,5]. Occlusion of the anterior cerebral artery (ACA) from head trauma is extremely uncommon. Six cases of traumatic occlusion of the ACA have been reported in literature[1-4,6,7]. In this paper the authors describe a case of severe head injury associated with traumatic occlusion of the ACA.
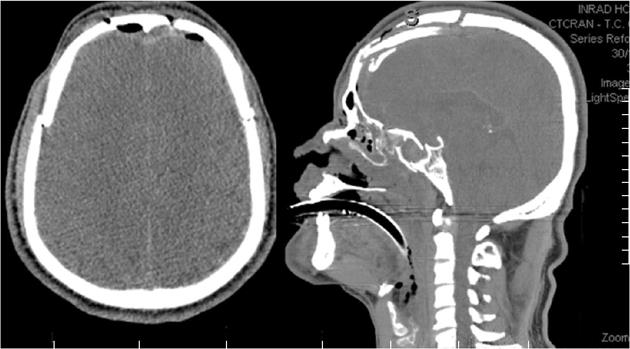
A 35-year-old male was admitted to the emergency room following a motorcycle accident. On admission his Glasgow Coma Score was 4, and he presented isochoric pupils, without systemic lesion. Immediate head multislice computed tomography (CT) scan was performed and showed diffuse brain swelling with multiple skull fractures, included one in the skull base (Figure 1).
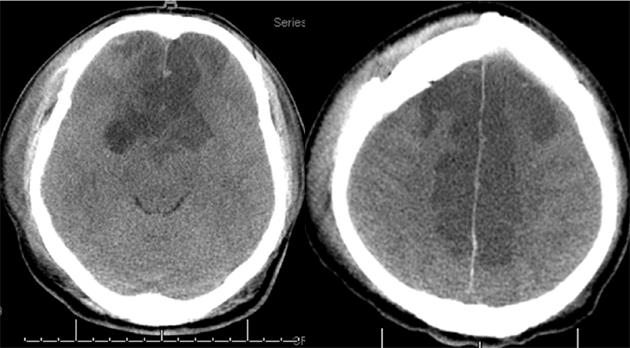
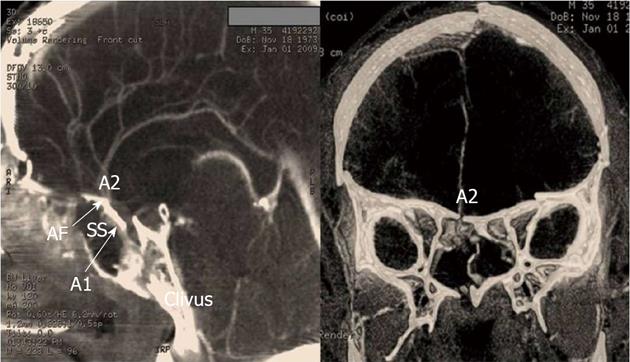
The patient developed mydriatic pupils after 24 h and an extensive cerebral infarction in the territory of ACA was found in the CT scan (Figure 2). Patient underwent CT angiography that demonstrated occlusion of the ACA caused by a fracture of the anterior fossa, with partial obstruction of the right and left branches, indicating a traumatic occlusion (Figure 3). Patient deceased after 3 d despite of medical management and intracranial pressure monitoring.
Fatal ACA infarct was encountered in half of the reported cases. Only one patient survived without neurological deficits. All patients except one sustained their injury in a road accident. In our patients a severe trauma following motorcycle accident indicates a high energy trauma mechanism.
The initial diagnosis is often delayed because of the low incidence of traumatic ACA occlusion[1]. Lucid intervals are common in patients with traumatic arterial obstruction[3,6]. However in this case, the authors believe that axonal diffuse injury associated with arterial lesion were responsible for the coma, with no lucid interval.
Outcome is generally poor. Three patients died, and one remained in persistent vegetative state. Mechanisms such as direct injury, dissecting aneurysm, thrombosis, and embolism have been reported as cause for intracranial vessel occlusion in association with head injury[1,3]. In this case, occlusion probably was caused by dissection and direct obstruction of artery by fracture. We believe that the extensive line of fracture at the base of the anterior fossa and sella resulted in partial traumatic occlusion by clamping of both anterior cerebral arteries in A1 and A2 segment. The ACA and the terminal branch of internal carotid artery, its first segment, designated A1 presents length ranging from 10 to 20 mm, an average of 15 mm[8]. This segment goes on the optic chiasm in 17% and on the nerve in 83%, while the A2 segment goes hand in hand in 26%[8], as we believe occurred in our patient, which allowed bilateral compression with elevation of bone the fracture and thus clamping these vessels.
Vasospasm is another factor in the pathogenesis of intracranial artery occlusion[9]. Spasm following traumatic subarachnoid hemorrhage is most common in the distal portion of the internal carotid artery and the proximal portion of the middle cerebral artery and ACA[10,11]. The reported incidence of intracranial arterial spasm following moderate to severe head injury range from 5% to 10%[10]. In this patient, presence of early hypodensity on CT skull do not favor spasm as the primary mechanism, nonetheless one may not totally exclude it, mainly in the terminal branches of the anterior cerebral arteries.
P- Reviewer Luo CB S- Editor Cheng JX L- Editor A E- Editor Xiong L
| 1. | Amagasa M, Sato S, Shimizu Y, Otabe K, Onuma T. [Post-traumatic occlusion of the anterior cerebral artery]. No Shinkei Geka. 1988;16:103-107. [PubMed] [Cited in This Article: ] |
| 2. | Dratz HM, Woodhall B. Traumatic dissecting aneurysm of left internal carotid, anterior cerebral and middle cerebral arteries. J Neuropathol Exp Neurol. 1947;6:286-291. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 56] [Cited by in F6Publishing: 48] [Article Influence: 3.4] [Reference Citation Analysis (0)] |
| 3. | Ishibashi A, Kubota Y, Yokokura Y, Soejima Y, Hiratsuka T. Traumatic occlusion of the anterior cerebral artery: case report. Neurol Med Chir (Tokyo). 1995;35:882-885. [DOI] [Cited in This Article: ] [Cited by in Crossref: 13] [Cited by in F6Publishing: 15] [Article Influence: 0.5] [Reference Citation Analysis (0)] |
| 4. | Iwamoto Y, Fujimoto M, Nakagawa Y, Yamamoto K. Study of the traumatic cerebral infarcti on. Kyoto Furitsu Ikadaigaku Zasshi. 1993;102:965-971. [Cited in This Article: ] |
| 5. | De Araujo JC, De Moraes GP. [Traumatic occlusion of the middle cerebral artery: report of a case]. Arq Neuropsiquiatr. 1984;42:50-54. [PubMed] [Cited in This Article: ] |
| 6. | Levin W. Vascular lesions in head injuries. Brit J Surg. 1968;55:321-331. [DOI] [Cited in This Article: ] [Cited by in Crossref: 18] [Cited by in F6Publishing: 19] [Article Influence: 0.3] [Reference Citation Analysis (0)] |
| 7. | Nelson JW. Dissecting subintimal hematomas of the intracranial arteries: report of a case. J Am Osteopath Assoc. 1968;67:512-527. [PubMed] [Cited in This Article: ] |
| 8. | Perlmutter D, Rhoton AL. Microsurgical anatomy of the anterior cerebral-anterior communicating-recurrent artery complex. J Neurosurg. 1976;45:259-272. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 310] [Cited by in F6Publishing: 248] [Article Influence: 5.2] [Reference Citation Analysis (0)] |
| 9. | Mobbs RJ, Chandran KN. Traumatic middle cerebral artery occlusion: case report and review of pathogenesis. Neurol India. 2001;49:158-161. [PubMed] [Cited in This Article: ] |
| 10. | Yamada K, Harada M, Hasegawa S, Ushio Y. Delayed posttraumatic middle cerebral artery vasospasm demonstrated by magnetic resonance angiography: case report. Neurosurgery. 1998;43:153-156. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 9] [Cited by in F6Publishing: 10] [Article Influence: 0.4] [Reference Citation Analysis (0)] |
| 11. | Suwanwela C, Suwanwela N. Intracranial arterial narrowing and spasm in acute head injury. J Neurosurg. 1972;36:314-323. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 110] [Cited by in F6Publishing: 110] [Article Influence: 2.1] [Reference Citation Analysis (0)] |