INTRODUCTION
Duodenal obstruction is a late complication of pancreatic carcinomas and occurs in 10%-15% of cases[1-4]. Palliative surgical intervention for unresectable pancreatic malignancies with a gastrojejunostomy has been associated with increased morbidity and mortality[5]. Palliation with endoscopically or fluoroscopically placed duodenal self-expandable metal stents has been shown to be safe and cost-effective, and improves quality of life in patients with unresectable pancreatic carcinoma and gastric outlet obstruction. A meta-analysis comparing endoscopically placed enteral stents and gastroenterostomy for malignant gastric outlet obstruction showed that endoscopic stenting is associated with higher clinical success, decreased length of stay, shorter time from procedure to oral intake, decreased morbidity, and less delayed gastric emptying compared to the surgical group[6]. This procedure is considered by some as the procedure of choice for malignant gastric outlet obstruction[7] and has been used increasingly in the US. Currently, Wallstent® (Boston Scientific, Natick, MA), an uncovered duodenal stent, is the only stent approved by the Food and Drug Administration in the U.S. for palliation of malignant gastric outlet obstruction[8].
CASE REPORT
A 55-year-old female presented with a 2-wk history of a “viral illness” and a recent onset of painless jaundice with dark colored urine. Her past medical history was significant for colon cancer resected 30 years prior. Physical examination was remarkable only for scleral icterus and jaundice. Laboratory studies were significant for a conjugated hyperbilirubinemia. A computed tomography (CT) scan revealed a 1.5 cm mass in the head of the pancreas with biliary and pancreatic ductal dilatation. Endoscopic retrograde cholangiopancreatogram demonstrated a 2.5 cm stricture that was stented. Brushings revealed carcinoma. An endoscopic ultrasound, biopsy, and staging laparoscopy revealed an unresectable pancreatic carcinoma with encasement of the superior mesenteric vessels. Fifteen months after the initial presentation, the patient developed symptomatic gastric outlet obstruction and underwent endoscopic placement of two 20 mm × 60 mm Wallstent® (Boston Scientific, Natick, MA) stents across the duodenal narrowing.
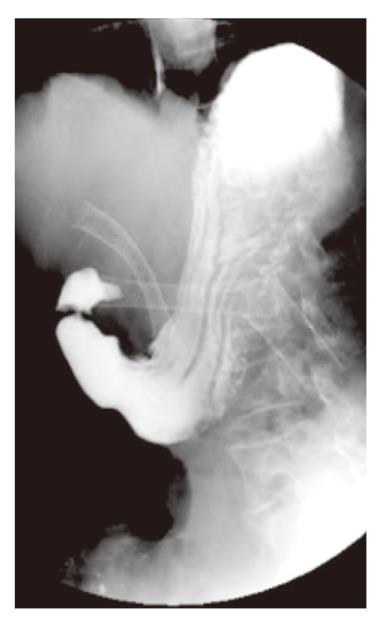
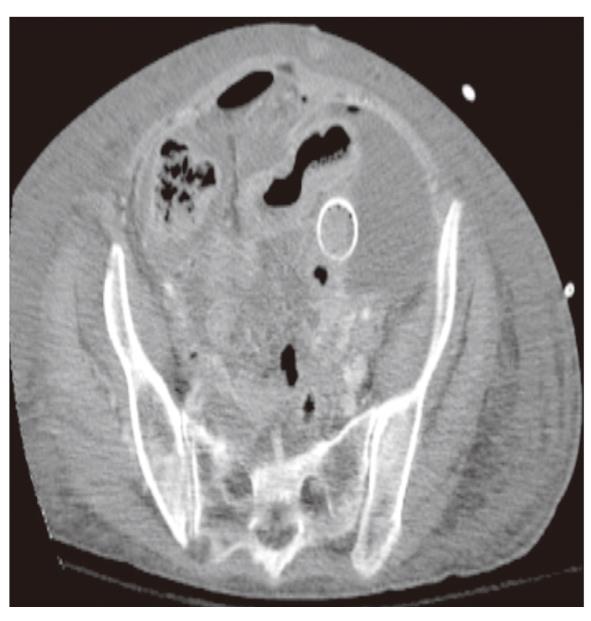
With failed resolution of her gastric outlet obstructive symptoms, a contrast study was obtained which demonstrated both the biliary stent and the two duodenal stents to be in proper position (Figure 1). Given the ongoing symptoms, a loop gastrojejunostomy was performed without incident. However, on postoperative day 5 the patient developed an acute onset of abdominal pain, acidosis, and leukocytosis. A CT scan revealed a large amount of free fluid in the abdomen, a small amount of free air, and a metallic stent in the distal small bowel (Figure 2). The patient was taken for an emergency exploratory laparotomy where one of the metallic stents was found 10 cm proximal to the ileocecal valve perforating the small bowel. The perforated segment of small bowel was resected along with the stent. However, the patient died 3 d later from multisystem organ failure secondary to overwhelming sepsis.
Figure 1 Contrast study prior to the gastrojejunostomy reveals a gastric outlet obstruction with two duodenal stents and a biliary stent in proper position.
Figure 2 Computed tomography scan reveals a stent in the small bowel protruding intra-peritoneally with pneumoperitoneum.
DISCUSSION
Malignant gastric outlet obstruction is most commonly seen with pancreatic cancer[9]. Traditional palliation with gastroenteric bypass has been shown to be associated with a significant degree of morbidity and mortality[3,5,10]. In recent years, enteral stents placed under endoscopic or fluoroscopic guidance has emerged as an effective, less morbid alternative to surgical intervention. In the US, the enteral Wallstent® (Boston Scientific, Natick, MA) has been approved for duodenal placement for palliation of gastric outlet obstruction[7]. While these stents have many advantages when compared with gastrojejunostomy, including improved oral nutrition[9,11-13], increased cost-effectiveness[9,14], and decreased morbidity and hospital stay, there is no improvement in 30-d mortality[6]. Despite these advantages, enteral stents are associated with a 17% complication rate including migration, duodenal perforation, biliary enteric fistulas, and reobstruction due to tumor growth and stent fracture[9,11,13].
Although the incidence of clinically significant stent migration is rare, they can cause significant morbidity or mortality when they occur. To our knowledge, there is only one other known report of a palliative duodenal stent migrating to the distal small bowel causing perforation. Reported by Moxey et al[15], it occurred 1 mo after a self-expandable stent was placed for presumed pancreatic carcinoma, and was thought to have migrated after the patient’s pancreatic inflammation had resolved. The patient underwent a surgical small bowel resection but later expired due to bacterial endocarditis. Other reported stent-related complications described in the literature include stent collapse, bleeding, large-bowel obstruction[16], reobstruction, tumor overgrowth, jaundice, food impaction, and late duodenal perforation[17]. The migration rate of uncovered stents has been reported to be in the range of 0%-11%[11,18,19], compared to 21%-26% for covered stents[20,21].
Given that the stents were confirmed to be in the duodenum prior to the gastrojejunostomy, the migrated stent found during the second exploration must have migrated past the gastrojejunostomy anastomosis to the distal ileum, soon after surgery, leading to the bowel perforation. We presume that the migrated stent may have been dislodged, at least partially, from manipulation during the gastrojejunostomy. The time between the endoscopic placement of the stents and the subsequent gastrojejunostomy was too short to allow for any stabilization of the stents by tumor in-growth or scarring[22].
The enteral Wallstent® has an open mesh and has been associated with insertion difficulties around acute angles as well as damage to tissues and endoscopes by the exposed proximal and distal wires[23]. Sometimes more than one stent is necessary when the first stent is not deployed into the ideal location. The forward force generated by the expanding stent may sometimes lead to undesired forward displacement of the stent, particularly at the site of strictures[22].
In conclusion, we report a rare complication of a duodenal Wallstent® placed for malignant gastric outlet obstruction secondary to pancreatic cancer that migrated to the distal ileum resulting in small bowel perforation. Although uncommon, it is important to be aware of the potential risk of duodenal stent migration, particularly after any manipulation of the stomach or the duodenum during surgery, and especially if the time between stent placement and surgery has been short.