Copyright
©The Author(s) 2025.
World J Hepatol. Aug 27, 2025; 17(8): 108845
Published online Aug 27, 2025. doi: 10.4254/wjh.v17.i8.108845
Published online Aug 27, 2025. doi: 10.4254/wjh.v17.i8.108845
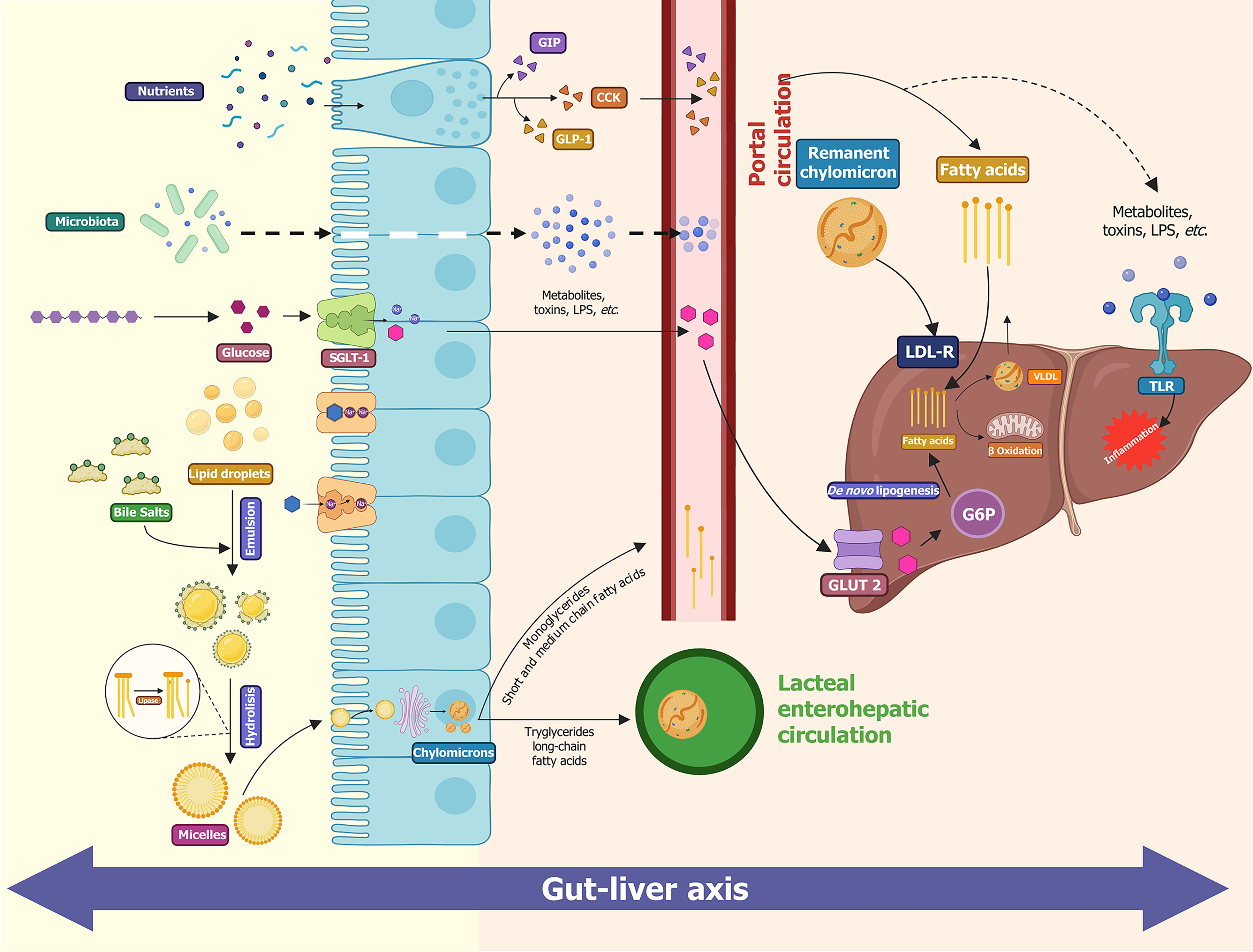
Figure 1 Duodenal lipid absorption and gut-derived signals involved in metabolic dysfunction-associated steatotic liver disease pathophysiology.
Lipid absorption in the duodenum begins with emulsification of dietary fats by bile salts, followed by enzymatic hydrolysis into monoglycerides and free fatty acids. These products are incorporated into micelles, absorbed by enterocytes, re-esterified and packaged into chylomicrons for transport through the lymphatic system. In parallel, luminal nutrients stimulate enteroendocrine cells to secrete hormones such as cholecystokinin, glucose-dependent insulinotropic polypeptide and glucagon-like peptide-1, which regulate insulin secretion, bile release and gastric motility. In the context of metabolic dysfunction-associated steatotic liver disease (MASLD), altered intestinal permeability and microbial dysbiosis may lead to increased translocation of microbial metabolites and toxins, such as lipopolysaccharides, into the portal circulation, contributing to hepatic inflammation and metabolic dysfunction. The dashed lines indicate pathological processes specifically associated with MASLD and do not reflect normal physiology. CCK: Cholecystokinin; GIP: Glucose-dependent insulinotropic polypeptide; GLP-1: Glucagon-like peptide-1; GLUT-2: Glucose transporter-5; LDL-R: Low-density lipoprotein receptor; LPS: Lipopolysaccharides; SGLT-1: Sodium-glucose cotransporter 1; TLR: Toll-like receptor; VLDL: Very low-density lipoproteins.
- Citation: Ramírez-Mejía MM, Méndez-Sánchez N. Duodenal mucosal ablation by irreversible electroporation: Modulating the gut-liver axis in metabolic steatotic liver disease. World J Hepatol 2025; 17(8): 108845
- URL: https://www.wjgnet.com/1948-5182/full/v17/i8/108845.htm
- DOI: https://dx.doi.org/10.4254/wjh.v17.i8.108845