Published online Aug 15, 2012. doi: 10.4239/wjd.v3.i8.142
Revised: July 30, 2012
Accepted: August 8, 2012
Published online: August 15, 2012
AIM: To monitor the course of continuous intraperitoneal insulin infusion (CIPII) and to gain more insight into possible complications.
METHODS: A retrospective, longitudinal observational cohort study in patients with type 1 diabetes mellitus (T1DM) was performed. Only patients with “brittle” T1DM who started CIPII between January 1, 2000 and June 1, 2011, and were treated in the only centre in The Netherlands providing CIPII treatment (Isala clinics, Zwolle) were eligible for inclusion. Outcomes were defined as operation-free period (OFP), rate and type of complications. Subanalyses were made between patients starting CIPII from 2000 to 2007 and from 2007 onwards in order to study possible changes over time in complications and/or OFP. The OFP was calculated as the time from initial implantation to the date of first documented re-operation. If patients had not experienced an operation, their data were recorded at the date of last follow up or death. Kaplan-Meier curves were constructed to visualize the OFP. A (two-sided) P value of less than 0.05 was considered statistically significant.
RESULTS: Fifty-seven patients were treated with CIPII, although one patient was excluded from analyses because of self-induced complications. In the remaining 56 patients, 70 complications occurred during 283 patient years. Catheter occlusion (32.9%), pump dysfunction (17.1%), pain at the pump site (15.7%) and infections (10.0%) were the most frequent complications. This resulted in a median OFP of 4.5 years (95% confidence interval 4.1-4.8 years) without any difference between the time periods. Fifty re-operations were performed because of complications, one per 5.6 patient years, with a decrease in pump dysfunction (P = 0.04) and pump explantations (P = 0.02) after 2007. In total, 9 episodes of ketoacidosis occurred during follow up and there were 69 hospital re-admissions, with a median duration of 6 d. CIPII was ceased in five patients due to recurrent infections (n = 2), pain (n = 1), inadequate glycaemic control (n = 1) or by own choice (n = 1). No CIPII related mortality was reported.
CONCLUSION: The OFP has been stable over the last decade. No CIPII related mortality was reported. A significant decrease in pump dysfunction and explantation was seen after 2007 compared to the period 2000-2007. CIPII remains a safe treatment modality for specific patient groups.
- Citation: Dijk PRV, Logtenberg SJ, Groenier KH, Haveman JW, Kleefstra N, Bilo HJ. Complications of continuous intraperitoneal insulin infusion with an implantable pump. World J Diabetes 2012; 3(8): 142-148
- URL: https://www.wjgnet.com/1948-9358/full/v3/i8/142.htm
- DOI: https://dx.doi.org/10.4239/wjd.v3.i8.142
Continuous intraperitoneal insulin infusion (CIPII) with an implantable pump has been a treatment option for patients with diabetes since the 1980s. Nowadays this treatment modality is mainly used in patients with so called “brittle diabetes”, i.e., failing to reach adequate glycaemic control despite intensive insulin therapy with multiple daily injections or continuous subcutaneous insulin infusion and/or having frequent hypoglycaemic episodes, or subcutaneous insulin resistance[1,2].
Although the long term feasibility and positive metabolic benefits of CIPII are established by several clinical studies, reports on the drawbacks of CIPII are relatively scarce[3,4]. Obviously, complications interfere with treatment outcome with respect to glycaemic control, costs and, most importantly, quality of life[5,6]. Furthermore, while technical problems prevented widespread use of CIPII in the past, modifications of both the catheter attached to the pump and the insulin have reduced the incidence of insulin aggregates blocking the insulin delivery, one of the major problems in earlier years[7].
Haveman et al[8] underlined this development by studying the complications of CIPII in patients who started with CIPII before 2007 in our hospital (Isala Clinics, Zwolle, The Netherlands). After introduction of a new battery and a change in insulin solution in 2000, the operation-free period (OFP) was estimated to increase from 21 to 78 mo. The incidence of complications such as pump site infections and catheter related problems decreased, in accordance with other studies on CIPII[5,6]. However, ongoing monitoring is necessary to observe the course of this decrease. Furthermore, following the changes in 2000 more accurate results are required on what the OFP really is as only a limited number of patients had reached a 78 mo follow-up at the time of the previous evaluation (follow-up until 2007). Thus it is essential to extend our former study to include the period from 2007 onwards.
The aim of the current study was to describe the complications of CIPII in patients with type 1 diabetes mellitus (T1DM) over the period from 2000 until 2011. We also studies in detail the origin and consequences of both pump- and/or catheter related problems and complications.
In the Netherlands, the following indications for CIPII have been formulated: subcutaneous insulin resistance, brittle diabetes, hypoglycaemia unawareness, delayed insulin absorption, allergies, lipohypertrophy and/or lipoatrophy, very lean subjects, needle phobia, severe skin scarring or chronic dermatological problems[9]. Patients were selected for CIPII after consultation with diabetes professionals well acquainted with CIPII with, as a minimum, the participation of an internist and a diabetes specialist nurse in the decision making. Implantation was always combined with intensive education and, when indicated, assessment by a psychologist.
All patients with T1DM who were treated with CIPII over the period from January 1, 2000 to June 1, 2011 were included in the current analysis. All of these patients were referred to and treated in the Isala Clinics in Zwolle, the only centre in The Netherlands providing this treatment. For all patients, detailed clinical data regarding surgical placement of the pump, short- and long-term complications and consequences were collected retrospectively by reviewing hospital charts, operation- and microbiology reports. Data were collected by use of standardized case record forms.
Insulin pump, implantation and post-operative treatment and refill procedures have been described previously[8]. In Brief, MiniMed MIP model 2007 CIPII devices (Medtronic-MiniMed, Northridge, CA, United States) were implanted in our clinic from 2000 onwards. This model has a reservoir which can contains 15 mL of a special solution of U400 insulin and has a battery with 7 years longevity.
An outpatient rinse procedure with NaOH was performed every 9 mo or in cases of insulin underdelivery. Insulin underdelivery is present when, after the pump reservoir is totally emptied, the ratio between programmed and actually infused volume of programmed insulin, calculated as % error, is higher than 20%. If the % error was higher than 20, or a clinically significant difference between the % error calculated at previous refill was found, a rinse procedure was performed. In addition, inspection of the patient-pump-communicator for hardware or electronic failure was performed. If these procedures failed to restore normal insulin infusion a catheter flushing and/or catheter X-ray investigation was also performed. In case of signs of intractable occlusion despite all of these actions, surgical examination of the catheter to discover possible blockages with a post-surgical rinse of the pump was deemed necessary.
Pump-site infection was defined as a culture-proven infection in the subcutaneous pocket of the insulin pump. Prolonged device-related pain was defined as pain at the pump site which lasted for more than 6 wk after surgery and necessitated use of analgesics. Cutaneous erosion of the skin was defined as redness with signs of (imminent) perforation of the overlying skin at the pump site. Post-operative haematoma was defined as a swelling at the pump site caused by bleeding. Pump dislocation was defined as migration or rotation of the pump relative to the initial place of implantation. Catheter occlusion was defined as blockage of the catheter by fibrin clots or an intrinsic catheter defect. Encapsulation in the peritoneal cavity was defined as encapsulation of the catheter tip, positioned in the peritoneal cavity, by the omentum as diagnosed by catheter X-ray investigation or during surgical inspection. Hardware problems were defined as demonstrated hardware failure of the pump. Premature battery end-of-life was defined as battery end-of-life within 3.5 years of implantation. Pump dysfunction was defined as acute or chronic dysfunction of the pump after excluding of other causes e.g., battery end-of-life or hardware failure.
All analyses were performed using SPSS version 18.0 (Inc., Chicago, IL, United States). Descriptive statistics include number (percentage), mean ± SD and median [interquartile range (IQR)]. Data were compared with the Fisher’s exact test in the case of categorical data. In the case of continuous data, Student’s t-test or Mann-Whitney U test were used if the data was distributed normally or skewed, respectively. Q-Q plots and histograms were used to determine if the tested variable had a normal distribution or not. The OFP was calculated as the time from initial implantation to the date of first documented re-operation. If patients had not experienced an operation, they data were recorded at the date of last follow up or time of death. Kaplan-Meier curves were constructed to visualize the OFP. In order to further analyze the course of the complications, subanalyses were made comparing patients starting CIPII from 2000 and 2007, the end of the previous study, and from 2007 onwards. Differences in time to the occurrence of complications and the OFP rates were assessed for statistical significance using the log-rank test. A Cox regression analysis was performed to study the influence of possible confounders (age, sex, body mass index, duration of diabetes) on the OFP. A (two-sided) P value of less than 0.05 was considered statistically significant.
A total of 57 patients with T1DM were treated with CIPII. One patient with self-induced complications was excluded from analysis; the remaining 56 patients are subject of this study. Patient characteristics are depicted in Table 1. Two hundred eighty three patient years of follow up were observed, with a median duration of 4.7 years. In total, 80 pumps were implanted; 20 (35.7%) patients had a second pump and 4 (7.1%) patients had a third pump implanted.
| All patients | Implantation date | ||
| 2000-2011 (n = 56) | 2000-2007 (n = 37) | 2007-2011 (n = 19) | |
| Age (mean ± SD, yr) | 37.6 ± 14.5 | 38.0 ± 14.4 | 36.6 ± 15.1 |
| Female sex | 38 (68) | 28 (76) | 10 (53) |
| Smokers | 12 (21.4) | 7 (18.9) | 5 (26.3) |
| Previous abdominal operation | 9 (16.1) | 7 (18.9) | 2 (10.5) |
| BMI (mean ± SD, kg/m2) | 25.4 ± 4.4 | 26.3 ± 4.2 | 23.7 ± 4.3 |
| Duration of diabetes (yr), median (IQR) | 16.7 (9.7-26.3) | 15.9 (9.8-26.8) | 19.1 (9.6-26.3) |
| Retinopathy | 13 (23.2) | 9 (24.3) | 4 (21.1) |
| Neuropathy | 17 (30.4) | 12 (32.4) | 5 (26.3) |
| Nephropathy | 4 (7.1) | 3 (8.0) | 1 (5.3) |
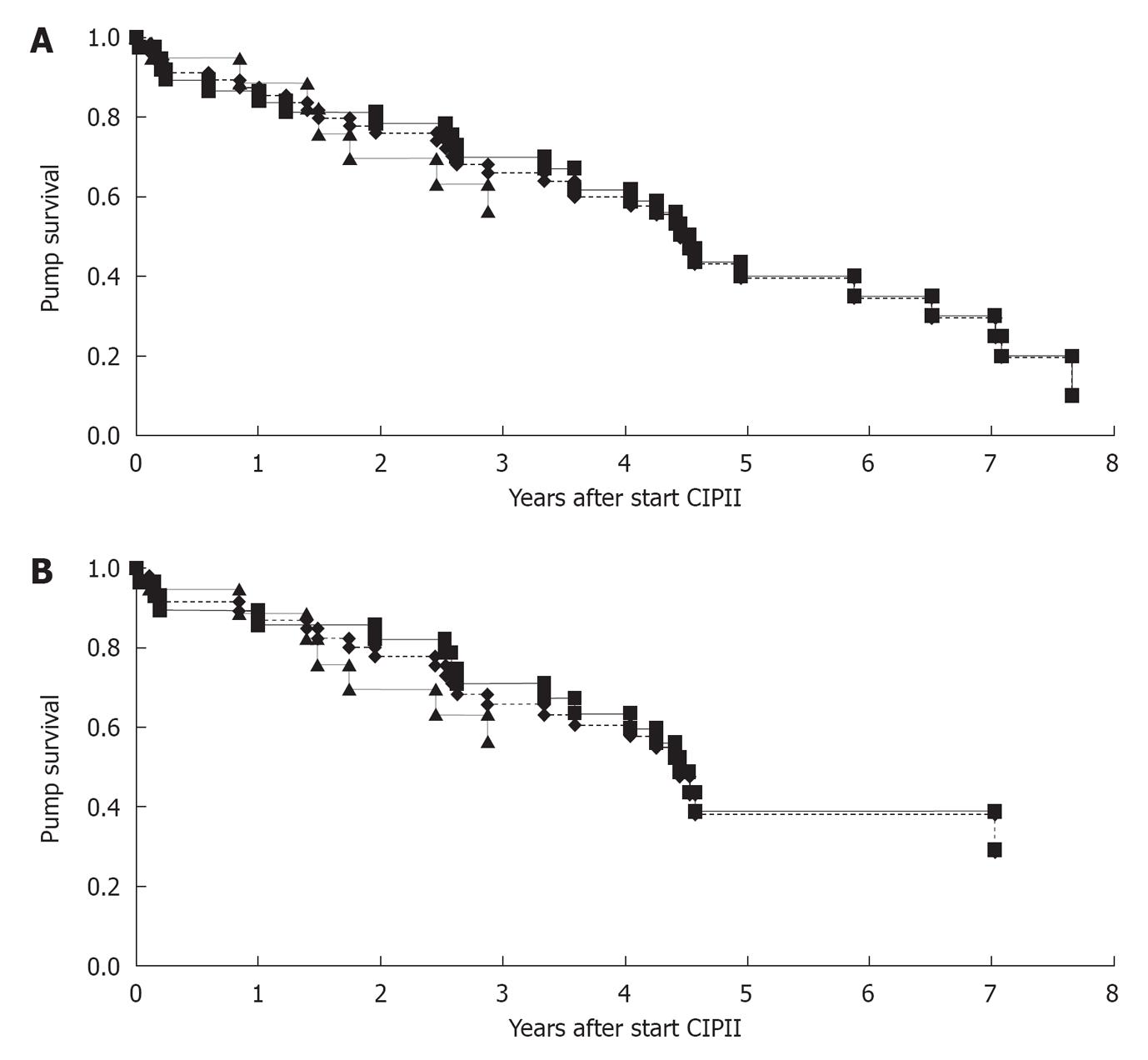
After starting CIPII, 33 patients underwent re-operation; 6 because of expected battery end-of-life, 24 because of complications and 3 for other reasons. As depicted in Figure 1, the median OFP between initial implantation and the first re-operation for all patients was 4.5 years [95% confidence interval (CI): 4.1-4.8 years]. After excluding operations for pump replacement for expected battery end-of-life or other reasons (n = 9) the median OFP was 4.5 years (95% CI: 3.9-5.0 years).
A total of 70 complications occurred during the follow-up (Table 2). Catheter occlusion (32.9%), pump dysfunction (17.1%) and pain at the pump site (15.7%) were the most frequent complications. Fifty-seven complications occurred with the first implanted pump in situ, 11 with the second and 2 with the third. 21 patients did not experience any complication, 15 patients experienced 1 complication, 11 patients 2 complications, 7 patients 3 complications, 1 patient 4 complications, and 1 patient 8 complications. The latter patient had recurrent infections and peritonitis, after a catheter replacement procedure. The median time from implantation of the first pump to occurrence of the first complication (excluding battery end of life) was 3.6 years (95% CI: 2.2-5.0 years).
| All patients | Implantation date | |||||
| 2000-2011 (n = 56) | 2000-2007 (n = 37) | 2007-2011 (n = 19) | ||||
| n (%) | Per 100 PY | n (%) | Per 100 PY | n (%) | Per 100 PY | |
| Haematoma | 3 (4.3) | 1.1 | 2 (3.8) | 0.9 | 1 (5.9) | 1.8 |
| Infection | 7 (10.0) | 2.5 | 4 (7.5) | 1.8 | 3 (17.6) | 5.3 |
| Pain | 11 (15.7) | 3.9 | 8 (15.1) | 3.5 | 3 (17.6) | 5.3 |
| Cutaneous erosion | 2 (2.9) | 0.7 | 2 (3.8) | 0.9 | 0 (0.0) | 0.0 |
| Dislocation | 3 (4.3) | 1.1 | 2 (3.8) | 0.9 | 1 (5.9) | 1.8 |
| Hardware failure | 0 (0.0) | 0.0 | 0 (0.0) | 0.0 | 0 (0.0) | 0.0 |
| Premature battery end of life | 0 (0.0) | 0.0 | 0 (0.0) | 0.0 | 0 (0.0) | 0.0 |
| Insulin aggregate | 4 (5.7) | 1.4 | 4 (7.5) | 1.8 | 0 (0.0) | 0.0 |
| Catheter occlusion | 23 (32.9) | 8.1 | 16 (30.2) | 7.1 | 7 (41.2) | 12.3 |
| Encapsulation of the catheter tip | 3 (4.3) | 1.1 | 3 (5.7) | 1.3 | 0 (0.0) | 0.0 |
| Peritonitis | 1 (1.4) | 0.4 | 1 (1.9) | 0.4 | 0 (0.0) | 0.0 |
| Pump dysfunction | 12 (17.1) | 4.2 | 111 (20.8) | 4.9 | 11 (5.9) | 1.8 |
| Other | 1 (1.4) | 0.4 | 0 (0.0) | 0.0 | 1 (5.9) | 1.8 |
| All | 70 (100.0) | 24.8 | 53 (100.0) | 23.5 | 17 (100.0) | 29.9 |
Because of complications, 50 re-operations were performed: one per 5.6-year of follow up (Table 3). Explantation of the pump and catheter (34.0%, 6.0 per 100 patient years) and catheter replacement (26.0%, 4.6 per 100 patient years) were the most frequently performed re-operations. Nine episodes of ketoacidosis occurred during follow up, 8 due to pump dysfunction and 1 due to catheter occlusion. Sixty-nine hospital re-admissions were caused by complications. The median duration of admission was 6 d (IQR: 3.0-12.8 d).
| All patients | Implantation date | |||||
| 2000-2011 (n = 56) | 2000-2007 (n = 37) | 2007-2011 (n = 19) | ||||
| n (%) | Per 100 PY | n (%) | Per 100 PY | n (%) | Per 100 PY | |
| Catheter inspection | 2 (4.0) | 0.7 | 2 (5.3) | 0.9 | 0 (0.0) | 0.0 |
| Catheter replacement | 13 (26.0) | 4.6 | 8 (21.1) | 3.5 | 5 (41.7) | 8.8 |
| Explantation of pump and catheter | 17 (34.0) | 6.0 | 151 (39.5) | 6.6 | 21 (16.7) | 3.5 |
| Repositioning of pump | 2 (4.0) | 0.7 | 2 (5.3) | 0.9 | 0 (0.0) | 0.0 |
| Fixation of pump | 2 (4.0) | 0.7 | 1 (2.6) | 0.4 | 1 (8.3) | 1.8 |
| Cutaneous problem | 0 (0.0) | 0.0 | 0 (0.0) | 0.0 | 0 (0.0) | 0.0 |
| Intra-abdominal problem | 1 (2.0) | 0.4 | 1 (2.6) | 0.4 | 0 (0.0) | 0.0 |
| Remove clot at tip of catheter/flush catheter | 7 (14.0) | 2.5 | 4 (10.5) | 1.8 | 3 (25.0) | 5.3 |
| Haematoma | 1 (2.0) | 0.4 | 1 (2.6) | 0.4 | 0 (0.0) | 0.0 |
| Reposition of catheter | 3 (6.0) | 1.1 | 3 (7.9) | 1.3 | 0 (0.0) | 0.0 |
| Infection | 2 (4.0) | 0.7 | 1 (2.6) | 1.2 | 1 (8.3) | 1.8 |
| All | 50 (100.0) | 17.7 | 38 (100.0) | 44.3 | 12 (100.0) | 21.1 |
Between 2000 and 2007, 37 (median follow up 5.3 years) patients received a pump and 19 (median follow up 3.7 years) patients received a pump between 2007 and 2011. The clinical characteristics of patients in the two different timeframes were comparable. Median OFP period for patients initially implanted between 2000 and 2007 was 4.5 years (95% CI: 4.1-5.0 years). Only seven patients implanted after 2007 had a re-operation, therefore the median OFP could not be calculated. There were no significant differences in median OFP (log rank: P = 0.80) between the two timeframes, even when excluding operations for expected battery end-of-life and reasons other than complications (log rank: P = 0.72) (Figure 1A and B).
The number of pump dysfunctions among patients who started CIPII after 2007 was significantly lower than in the group of patients who started CIPII before 2007 (P = 0.04) (Table 2). As depicted in Table 3, from 2007 onwards there were significantly less re-operations for pump and catheter explantation following complications (P = 0.02). The Cox regression analysis showed a non-significant hazard ratio of 1.12 (95% CI: 0.46-2.75, P = 0.52) for patients implanted after 2007 compared to those who were implanted between 2000 and 2007. None of the confounders had a significant relation with time to first re-intervention.
During the follow up period, one patient died due to heart failure whilst being treated with CIPII. In 5 patients, CIPII was stopped and the pump removed. In two patients the pump was removed because of recurrent infections and in the other cases because of pain (n = 1), inadequate glycaemic control (n = 1) or by own choice (n = 1). The remaining 50 patients are still being treated with CIPII.
The current study describes the incidence of complications in 56 patients treated with CIPII with an implanted insulin pump during the last decade. During 282.6 patient years of follow up, 70 complications occurred, i.e., one complication per 4.0 patient years. Catheter occlusion (32.9%), pump dysfunction (17.1%), pain (15.7%) and infections (10.0%) were the most frequent complications. A significant decrease in pump dysfunction and the need of premature explantation of the pump was seen in the period since 2007, compared to the period before 2007. There was a non-significant but potentially relevant increase in infections, catheter related complications and re-operations since 2007, although this did not affect the OFP during the last decade.
In the present study we report an OFP of 4.5 years (95% CI: 4.1-4.8 years) among patients who started CIPII between 2000 and 2007. This OFP differs from the OFP of 6.5 years (95% CI: 2.2-10.8 years) found by Haveman et al[8] among a subset of the same patients in the same period due to differences in follow up period. The current study had a longer follow up period for these patients and thus gives a more accurate estimate of the OFP.
The incidence of infections in the present study, 2.5 per 100 patient years, is comparable to previous studies on CIPII and other implanted devices[5,6,8,10-13]. Apparently, this rate has increased in patients operated on after 2007 to 5.3 infections per 100 patient years. However, all infections appeared in one patient. Due to combined improvements in pump technology, insulin stability and frequent rinse procedures, the previously high incidence of catheter blockage (between 7.8 and 57.3 per 100 patient years) has been substantially reduced[4,14-19]. In 2003, Gin et al[6] reported an incidence of 3.7 catheter obstructions needing surgical intervention, per 100 patient years. Although we found no difference in the course of treatment, compared to the limited recent literature on this topic, the incidence of catheter occlusions and re-operation for catheter replacement (14.5 respectively 8.8 per 100 patient years) since 2007 are rather high compared to the findings of Gin et al[6].
Besides the number of re-operations, the impact of complications is illustrated by the number of ketoacidosis occurrences (n = 9) and the hospital re-admissions (median duration of 6 d) following complications. DeVries et al[1] showed that initiation of CIPII diminishes the median duration hospital stay for patients with poorly regulated diabetes from 45 d in the year before implantation to 13 d in the year after implantation, the latter mostly due to implantation of the pump. As far as we know, the present study is the first to report on the number of hospital re-admissions due to complications. This number would strengthen future analysis of cost-effectiveness and health-related quality of life of CIPII.
This study has some limitations. First, since the follow up of the study performed by Haveman et al[8] ended at January 1, 2007 we decided to use this arbitrary point as cut-off for our subanalyses for the time course of the complications. Although this date is arbitrary and the numbers of patients are small, it can may give insight into changes in complications, positively and negatively, specific for a timeframe, that would need attention for the present care of these patients. Second, the exact cause of catheter or pump dysfunction could not always be determined and therefore the rate of factors such as insulin aggregates that may have led to pump dysfunction may be underestimated.
In conclusion, the median OFP for patients treated by CIPII with an implantable pump has been stable at 4.5 years over the last decade. Catheter occlusion (32.9%), pump dysfunction (17.1%), pain at the pump site (15.7%) and infections (10.0%) were the most frequent complications. There was a significant decrease in the number of pump dysfunctions and pump explantations and no significant alterations in the course of complications when comparing the period from 2000 until 2007 and that from 2007 onwards. However, the former group had a longer follow up period. This may mask a transition or possible future increase in complications and re-operations, thus suggesting a relatively stable OFP among patients. This will require ongoing investigation and thorough monitoring over the coming years.
Furthermore, since a new intraperitoneal insulin formulation had to be introduced in June 2011 since there are no batches of the original insulin formulation left, the findings of the present study should be taken into account when evaluating the effects associated with the use of the new insulin formulation. No CIPII related mortality was reported. CIPII remains a safe treatment modality for specific patient groups.
Intraperitoneal (IP) insulin infusion with an implantable insulin pump has been a treatment option for patients with diabetes since the 1980s. Nowadays this treatment is mainly used in patients who fail to reach adequate glycaemic control despite intensive insulin treatment with multiple daily injections or continuous subcutaneous insulin infusion. The aim of the current study was to monitor the course and to gain more insight into the surgical aspects and complications of continuous intraperitoneal insulin infusion (CIPII) using an implantable pump.
CIPII using an implantable pump improves glycaemic regulation in selected patients, compared to subcutaneous insulin infusion. In addition, if IP delivery could be linked to a kind of permanent sensor, and with a logarithm between this sensor and pump, a closed loop system could be created in the future. However, the complications and surgical experience with CIPII are important factors in the clinical use of CIPII.
The median operation-free period (OFP) for patients treated by CIPII with an implantable pump has been stable at 4.5 years over the last decade. Catheter occlusion (32.9%), pump dysfunction (17.1%), pain at the pump site (15.7%) and infections (10.0%) were the most frequent complications. Fifty re-operations were performed due to complications, one per 5.6 patient years. No CIPII related mortality was reported. CIPII remains a safe treatment modality for specific patient groups.
Knowledge of the complications of CIPII adds to patient counseling and clinical care. Since a new intraperitoneal insulin formulation had to be introduced in June 2011 as there were no batches of the original insulin formulation left, the findings of the present study should be taken into account when evaluating the effects associated with the use of the new insulin formulation.
Insulin delivered into the peritoneal space using an implantable pump. Insulin which is delivered into the peritoneal space is, to a large extent, absorbed directly (detectable within 1 h after administration) into the portal system, thereby mimicking the physiological route of insulin delivery from the pancreas. The time period between the initial operation and the first re-operation or, if patients have not experienced a re-operation, date of last follow up or death.
The manuscript by van Dijk et al reports on the complications of CIPII in type 1 diabetes. This study is an important addition to the literature, as it enumerates the complications of CIPII with a follow-up period of up to 12 years. In addition to providing data for the entire patient group, they also perform a subanalysis comparing patients starting CIPII between 2000-2007 and those starting from 2007 onward. The current study provides longer follow-up of the patients who began CIPII in 2000 or later. This is most relevant to current care, as a pump battery with a longer life was introduced in 2000, as was a change in the insulin formulation used in the pump.
Peer reviewer: Dr. Teresa DiLorenzo, PhD, Albert Einstein College of Medicine, 1300 Morris Park Ave, Bronx, NY 10461, United States
S- Editor Wu X L- Editor Hughes D E- Editor Zheng XM
| 1. | DeVries JH, Eskes SA, Snoek FJ, Pouwer F, Van Ballegooie E, Spijker AJ, Kostense PJ, Seubert M, Heine RJ. Continuous intraperitoneal insulin infusion in patients with 'brittle' diabetes: favourable effects on glycaemic control and hospital stay. Diabet Med. 2002;19:496-501. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 34] [Cited by in F6Publishing: 35] [Article Influence: 1.6] [Reference Citation Analysis (0)] |
| 2. | Renard E, Schaepelynck-Bélicar P. Implantable insulin pumps. A position statement about their clinical use. Diabetes Metab. 2007;33:158-166. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 54] [Cited by in F6Publishing: 54] [Article Influence: 3.2] [Reference Citation Analysis (0)] |
| 3. | Logtenberg SJ, van Ballegooie E, Israêl-Bultman H, van Linde A, Bilo HJ. Glycaemic control, health status and treatment satisfaction with continuous intraperitoneal insulin infusion. Neth J Med. 2007;65:65-70. [PubMed] [Cited in This Article: ] |
| 4. | Broussolle C, Jeandidier N, Hanaire-Broutin H. French multicentre experience of implantable insulin pumps. The EVADIAC Study Group. Evaluation of Active Implants in Diabetes Society. Lancet. 1994;343:514-515. [PubMed] [Cited in This Article: ] |
| 5. | Renard E, Bouteleau S, Jacques-Apostol D, Lauton D, Gibert-Boulet F, Costalat G, Bringer J, Jaffiol C. Insulin underdelivery from implanted pumps using peritoneal route. Determinant role of insulin pump compatibility. Diabetes Care. 1996;19:812-817. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 36] [Cited by in F6Publishing: 36] [Article Influence: 1.3] [Reference Citation Analysis (0)] |
| 6. | Gin H, Renard E, Melki V, Boivin S, Schaepelynck-Bélicar P, Guerci B, Selam JL, Brun JM, Riveline JP, Estour B. Combined improvements in implantable pump technology and insulin stability allow safe and effective long term intraperitoneal insulin delivery in type 1 diabetic patients: the EVADIAC experience. Diabetes Metab. 2003;29:602-607. [PubMed] [Cited in This Article: ] |
| 7. | Gin H, Melki V, Guerci B, Catargi B. Clinical evaluation of a newly designed compliant side port catheter for an insulin implantable pump: the EVADIAC experience. Evaluation dans le Diabete du Traitement par Implants Actifs. Diabetes Care. 2001;24:175. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 15] [Cited by in F6Publishing: 16] [Article Influence: 0.7] [Reference Citation Analysis (0)] |
| 8. | Haveman JW, Logtenberg SJ, Kleefstra N, Groenier KH, Bilo HJ, Blomme AM. Surgical aspects and complications of continuous intraperitoneal insulin infusion with an implantable pump. Langenbecks Arch Surg. 2010;395:65-71. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 25] [Cited by in F6Publishing: 22] [Article Influence: 1.4] [Reference Citation Analysis (0)] |
| 9. | Nederlandse Internisten Vereniging: Statement regarding indications for continuous intraperitoneal insulin infusion. 2007;. [Cited in This Article: ] |
| 10. | Bélicar P, Lassmann-Vague V. Local adverse events associated with long-term treatment by implantable insulin pumps. The French EVADIAC Study Group experience. Evaluation dans le Diabète du Traitement par Implants Actifs. Diabetes Care. 1998;21:325-326. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 19] [Cited by in F6Publishing: 19] [Article Influence: 0.7] [Reference Citation Analysis (0)] |
| 11. | Renard E, Rostane T, Carriere C, Marchandin H, Jacques-Apostol D, Lauton D, Gibert-Boulet F, Bringer J. Implantable insulin pumps: infections most likely due to seeding from skin flora determine severe outcomes of pump-pocket seromas. Diabetes Metab. 2001;27:62-65. [PubMed] [Cited in This Article: ] |
| 12. | Udelsman R, Chen H, Loman K, Pitt HA, Saudek CD. Implanted programmable insulin pumps: one hundred fifty-three patient years of surgical experience. Surgery. 1997;122:1005-1011. [PubMed] [Cited in This Article: ] |
| 13. | Darouiche RO. Treatment of infections associated with surgical implants. N Engl J Med. 2004;350:1422-1429. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 1677] [Cited by in F6Publishing: 1498] [Article Influence: 74.9] [Reference Citation Analysis (0)] |
| 14. | One-year trial of a remote-controlled implantable insulin infusion system in type I diabetic patients. Point Study Group. Lancet. 1988;2:866-869. [PubMed] [Cited in This Article: ] |
| 15. | Saudek CD, Selam JL, Pitt HA, Waxman K, Rubio M, Jeandidier N, Turner D, Fischell RE, Charles MA. A preliminary trial of the programmable implantable medication system for insulin delivery. N Engl J Med. 1989;321:574-579. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 92] [Cited by in F6Publishing: 94] [Article Influence: 2.7] [Reference Citation Analysis (0)] |
| 16. | Selam JL, Micossi P, Dunn FL, Nathan DM. Clinical trial of programmable implantable insulin pump for type I diabetes. Diabetes Care. 1992;15:877-885. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 67] [Cited by in F6Publishing: 53] [Article Influence: 1.7] [Reference Citation Analysis (0)] |
| 17. | Hanaire-Broutin H, Broussolle C, Jeandidier N, Renard E, Guerci B, Haardt MJ, Lassmann-Vague V. Feasibility of intraperitoneal insulin therapy with programmable implantable pumps in IDDM. A multicenter study. The EVADIAC Study Group. Evaluation dans le Diabète du Traitement par Implants Actifs. Diabetes Care. 1995;18:388-392. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 68] [Cited by in F6Publishing: 68] [Article Influence: 2.3] [Reference Citation Analysis (0)] |
| 18. | Scavini M, Galli L, Reich S, Eaton RP, Charles MA, Dunn FL. Catheter survival during long-term insulin therapy with an implanted programmable pump. The Implantable Insulin Pump Trial Study Group. Diabetes Care. 1997;20:610-613. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 18] [Cited by in F6Publishing: 18] [Article Influence: 0.7] [Reference Citation Analysis (0)] |
| 19. | Renard E, Baldet P, Picot MC, Jacques-Apostol D, Lauton D, Costalat G, Bringer J, Jaffiol C. Catheter complications associated with implantable systems for peritoneal insulin delivery. An analysis of frequency, predisposing factors, and obstructing materials. Diabetes Care. 1995;18:300-306. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 35] [Cited by in F6Publishing: 35] [Article Influence: 1.2] [Reference Citation Analysis (0)] |