Published online Mar 6, 2021. doi: 10.12998/wjcc.v9.i7.1734
Peer-review started: October 27, 2020
First decision: December 3, 2020
Revised: December 21, 2020
Accepted: January 6, 2021
Article in press: January 6, 2021
Published online: March 6, 2021
Reconstructive repair of huge full-thickness abdominal wall defects following debridement for abdominal electric burns remains a clinically challenging task. An ideal abdominal wall repair means a re-closure of the defected abdominal wall with pedicled neurovascular myofascial flaps, restoration of the abdominal wall integrity, and maintenance of the abdominal wall muscle tension to prevent the occurrence of abdominal wall hernia. When treating huge full-thickness defects, composite autologous tissue flaps are a good option for the repair.
This study reported the case of a 43-year-old male patient suffering from full-thickness abdominal wall defects complicated with necrosis of multiple bowel segments and duodenal leak following high-voltage burns involving the left upper limb and abdomen. After debridement for abdominal electric burns and end-to-end anastomosis for the necrotic bowels, reconstruction with acellular dermal matrix grafting and vacuum sealing drainage were performed for temporary abdominal closure. The remaining 18 cm × 15 cm full-thickness abdominal wall defect was repaired using a combined anterolateral thigh and tensor fascia lata free flap. The proposed method achieved the functional reconstruction of the abdominal wall.
This approach restored the abdominal wall integrity, maintained certain muscle tension, avoided abdominal hernia, reached satisfactory aesthetic effect, and resulted in no complications in the grafting regions.
Core Tip: The reconstruction of large full-thickness abdominal wall defects is still a challenging task clinically, and it is even more difficult if intestinal damage is combined. Before the intestinal wound healing, it is a great innovation to protect the intestinal tube with heterogeneous acellular dermal matrix and to drain the fluid with vacuum sealing drainage externally, thus avoiding the occurrence of serious infection. Autogenous compound tissue flap is a good choice to reconstruct the abdominal wall defect, restore the integrity of the abdominal wall, maintain the tension of the abdominal wall muscle, and prevent the occurrence of abdominal wall hernia. In this case, an anterolateral thigh flap with tensor fascia lata was used to reconstruct the abdominal wall defect, with good functional and aesthetic results.
- Citation: Wang J. Reconstructing abdominal wall defects with a free composite tissue flap: A case report. World J Clin Cases 2021; 9(7): 1734-1740
- URL: https://www.wjgnet.com/2307-8960/full/v9/i7/1734.htm
- DOI: https://dx.doi.org/10.12998/wjcc.v9.i7.1734
In severe abdominal burns due to contact with high-voltage electric circuits, the abdomen is usually the outlet of the current, and the injuries can be dichotomized into electrical burns of the abdominal wall and complicating abdominal organ damages. Such cases are rare in clinics, but special attention should be paid to them due to their hidden, complex, and rapid-progressing conditions. The repair of abdominal wall defects remains a huge challenge to surgeons due to abdominal organ damages and abdominal wall defects. The component separation technique was used for the repair of abdominal wall defects[1], but the range of repair was limited. A latissimus dorsi free flap was also used for the repair of abdominal wall defects[2], but patient position needed to be changed intraoperatively. Based on the perforators from the descending branch of the lateral circumflex femoral artery, an anterolateral thigh (ALT) free flap is increasingly used for reconstructions of various regions[3]; while some researchers[4-6] believe that a combined ALT and tensor fasciae lata (TFL) flap is the optimal flap for reconstructing abdominal wall defects.
In this study, a combined ALT and TFL flap was used for reconstructing the abdominal wall defect, achieving excellent functional and aesthetic outcomes.
A 43-year-old male patient was burned by 10 kV high voltage on the left upper limb and in the abdominal wall and was admitted to the Department of Burns and Skin Repair Surgery, Hainan General Hospital.
A 43-year-old male patient suffered from temporary unconsciousness after a 10-kV high-voltage electric shock on June 17, 2018. He had no history of falls from a height or incontinence. He was transferred to the local hospital for disinfection, wound dressing, and fluid transfusion. However, due to disease progression, he was transferred to the Department of Burns and Skin Repair Surgery, Hainan General Hospital, 8 h after the incident.
The patient had a free previous medical history.
The patient was born and brought up in the country of origin, and had no history of exposure to epidemic water and poisons. His living conditions were normal, and he denied any history of sexually transmitted diseases. He had no history of smoking or alcohol abuse. His family members were healthy, and he denied a family history of mental illness, genetic history, or tumor history.
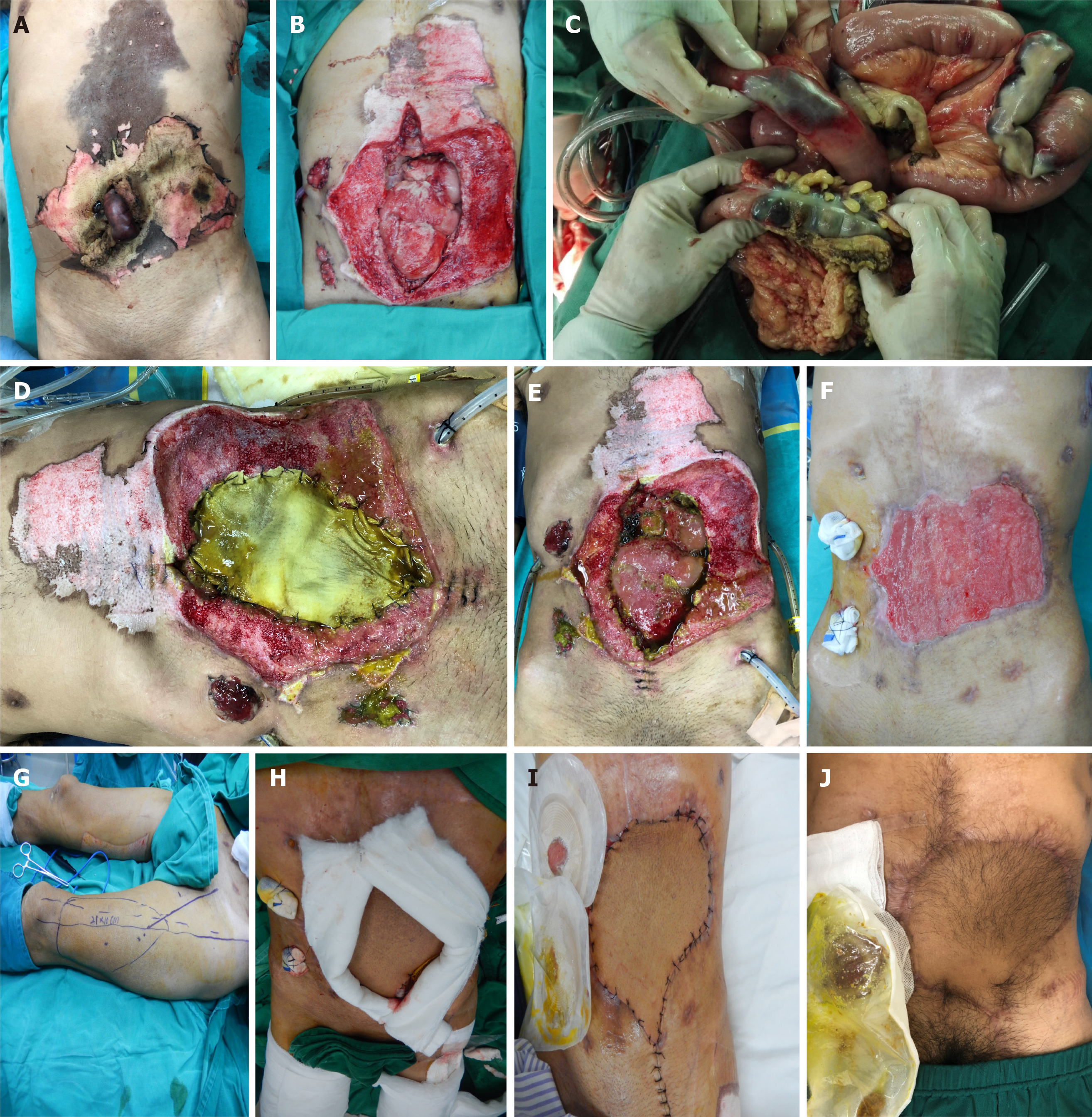
The physical examination at admission indicated a pulse of 69 beats/min and blood pressure of 134/99 mmHg. The patient had a pale face but was conscious and could answer simple questions. He had abdominal and rebound tenderness. The burned areas involved the middle abdomen and the left upper limb. The involved abdominal skin measured 18 cm × 15 cm. Full-thickness abdominal wall defects (5 cm × 2 cm, portrait) were noted 2 cm above the umbilicus, with carbonized marginal tissues and exposed blackened bowels (Figure 1A). Regarding the left upper limb injury, most skins were carbonized, the muscles were necrotic, arteries and veins were embolized, ulnar and radial arterial pulses disappeared, cyanosis was present, and the skin temperature significantly decreased.
Routine blood tests showed a white blood cell count of 26.20 × 109/L, a neutrophil percentage of 91.3%, a lymphocyte percentage of 2.5%, a monocyte percentage of 5.8 %, a red blood cell count of 4.26 × 1012/L, a hemoglobin level of 133 g/L, and a platelet count of 256 × 109/L.
Computerized tomography indicated subdiaphragmatic free air (suggesting pneumoperitoneum) and subcutaneous free air in the left upper limb and abdominal wall.
(1) High-voltage electrical burns involving the left upper limb and abdomen wall, with a total burn area of 15% (III); (2) osteofascial compartment syndrome of the left upper limb; and (3) gastrointestinal necrosis and perforation.
Given the patient’s history and condition, osteofascial compartment syndrome of the left upper limb and abdominal wall defects complicated with bowel necrosis were preliminarily considered. After preoperative preparation for 1 h, an emergency surgery, combining the open amputation of the upper left upper limb, debridement for the abdominal burns, and exploratory laparotomy, was performed. The intraoperative findings showed full-thickness abdominal wall defects, measuring 18 cm × 15 cm (Figure 1B) after escharotomy. Large amounts of fecal water-like liquid and bowel fluid were found in the abdominal cavity. Partial necrosis of the transverse colon and necrosis of multiple bowel segments were also observed (Figure 1C). After resection of the necrotic bowels, end-to-end anastomosis was performed. The necrotic greater omentum was resected, and double-barrel terminal ileostomy was performed in the right lower abdomen. Normal saline and Anerdian III were used to thoroughly clean the abdominal cavity. Multiple silicone drainage tubes were placed in the pelvic floor, greater curvature of the stomach, anterior right subhepatic space, and left iliac fossa. The abdominal wall defects and bowels were covered with the acellular dermal matrix (ADM). Vacuum sealing drainage (VSD) was also used to cover the wound for temporary abdomen closure. After the surgery, measures such as anti-infective treatment, total parenteral nutrition (TPN), and continuous negative-pressure drainage of the wound were given, and the patient’s vital signs were stable. Five days after the exploratory laparotomy, the patient experienced abdominal pain; yellow-green fluids were drained out from the tube, and the negative-pressure materials were also dyed in yellow-green. Thus, another exploratory laparotomy was performed, revealing a duodenal leak, which was repaired. Two days after the leak repair, the oozing and leakage of the yellow-green duodenal fluids were still observed. The temporary closure was continued with ADM, VSD, and continuous negative-pressure drainage. The ADM and VSD materials were changed every 7-10 d (Figure 1D and E). Treatments such as gastrointestinal decompression, TPN, anti-infection, and symptomatic treatments were given while the duodenal fistula was healed 6 wk after the repair of the duodenal leak. Within this 6 wk period, dense granulation tissue grew on the serosal surface of the exposed bowel walls, forming a plate-like adhesive barrier that completely enclosed the abdominal cavity (Figure 1F). Hence, a left ALT flap measuring approximately 21 cm × 16 cm (Figure 1G) was designed for the repair. While harvesting, the TFL was included. The flap arteries and veins were anastomosed with the inferior epigastric artery and vein under a microscope to restore the abdominal wall integrity (Figure 1H and I). The patient was discharged 2 wk after the abdominal wall repair. He was followed every 2-3 mo for 1 year.
The patient was followed every 2-3 mo for 1 year. At the last follow-up in June 2019, the patient had no complications such as abdominal wall ulcer, abdominal wall hernia (Figure 1J), bowel obstruction, or bowel fistula.
Reconstructive repair of huge full-thickness abdominal wall defects following debridement due to abdominal electric burns remains a challenging task. A certain degree of tension is required for the abdominal wall integrity following the defect repair[4]. In the present case, the patient sustained severe electrical burns on the abdominal wall. A huge abdominal wall defect measuring 18 cm × 15 cm was present after the debridement. Repairing and reconstructing abdominal wall defects were challenging. Complications with necrosis of multiple bowel segments increased the therapeutic difficulty. The accidental and temporally unrepairable duodenal leak occurred 5 d after the first surgery, which extended into the abdominal cavity and severely contaminated the abdominal cavity and abdominal wall defects, further increasing the treatment difficulty. Maloney et al[1] believed that mesh repair was inappropriate for patients with huge defects, especially those with contaminated wounds because patients were more predisposed to mesh-related infections (incidence rate: 68.4%), fistula formation (incidence rate: 22%), and abdominal hernias. Karhof et al[7] thought that mesh repair used in traumatic abdominal wall defects could strengthen the abdominal wall and reduce the complication of abdominal hernias. However, the mesh would significantly increase the complication of wound infections in patients with contaminated wounds. The mesh was not chosen in the present case because the abdominal cavity and abdominal wall wound were heavily contaminated. Before healing of the fistula, temporary abdominal closure (TAC) with ADM grafting was applied to close the inner abdominal cavity. ADM had no immunogenicity, good tissue compatibility, and a certain degree of tension. Therefore, it temporarily served as an alternative to the peritoneum for bowel protection. Application of VSD as a closure layer for the outer abdominal cavity further strengthened the abdominal wall, avoided bulge of the abdominal organs, provided drainage for the duodenal leaks, and therefore effectively prevented severe infections of the abdominal cavity and the wounds. Maloney et al[1] believed that VSD-assisted delayed closure of the abdominal and subcutaneous wounds in patients with severely contaminated abdominal wall defects could avoid complications such as aggravation and spread of infections. After delaying the treatment for 6 wk using ADM- and VSD-assisted TAC, the duodenal leak was healed, the gastrointestinal functions were restored, and dense granulation tissues were formed on the bowel serosal surface, forming a plate-like adhesive barrier that completely enclosed the abdominal cavity. Thus, the conditions for wound repair were matched.
Justo et al[8] used allogeneic abdominal wall tissue grafting to treat huge abdominal wall defects. Despite some successful cases, risks of infectious diseases, immune rejection, and other problems, including lack of donors and ethics, remain. For the treatment of huge full-thickness abdominal wall defects, autologous flap repair has become a good choice[4-6]. Autologous flaps come from the same individual and match all the requirements of ideal repair material. Therefore, a combined ALT and TFL flap was used to repair the huge full-thickness abdominal wall defect in the present case. It turned out to be a good choice, resulting in excellent outcomes and avoiding problems such as infectious diseases, immune rejection, and lack of donors or ethics.
Chou et al[3] believed that an ALT flap was increasingly popular because of its large harvest size, low donor site complications, versatile applications, and ease of harvest. During the surgery, two groups of surgeons could simultaneously perform ALT flap harvest and repair of the abdominal wall defect separately while the patient was placed in the supine position. This meant shorter operating time and no need to change patient position. Compared with the latissimus dorsi flap that required a change in the patient position[2], the ALT flap was superior in abdominal wall repair. In the present case, the surgeons designed a left-side ALT flap harvest with a size of 21 cm × 16 cm, including the TFL flap. The flap arteries and veins were anastomosed with the inferior epigastric artery and vein to restore the abdominal wall integrity, and skin graft repair was done after the wound size was reduced due to the shrunk donor area. Hence, not only the skin and fascia defects but also the muscular defects were repaired using TFL. Caliceti et al[9] believed that the harvest of an ALT flap with skin or muscle in a large size made the ALT flap an ideal flap for three-dimensional reconstruction. A combined ALT and TFL flap had an abundant blood supply and a strong anti-infective function, thus avoiding foreign body retention or severe infections related to mesh repair. The TFL flap had adequate strength and tension, enabling its functioning as muscles of the abdominal wall. This further strengthened the abdominal wall and avoided the occurrence of abdominal hernia postoperatively. During the 1-year follow-up of the patient, no abdominal hernia was found. Compared with pedicled flaps, a combined ALT and TFL free flap could repair any abdominal defects and avoid the restraints of space.
Delayed repair of abdominal wall defects due to electrical burns is reliable. This is because electrical burns of the abdomen not only involve skin necrosis but also damage the deep fascia, muscles, peritoneum, or even abdominal organs; the condition is often characterized by progressive necrosis. Therefore, temporary closure is required after early debridement. Also, the reconstruction of the abdominal wall should be performed only after necrosis goes away and stable gastrointestinal, liver, and kidney functions are achieved through proactive treatments. Maloney et al[1] suggested VSD-assisted delayed reconstruction for patients with severely contaminated abdominal wall defects, which was similar to the proposed method. Prior to the repair of abdominal defects, TAC with suitable material was required to avoid bulge of the bowel, bowel edema, abdominal infection, and other complications. ADM is a novel biomaterial with good tissue compatibility, no immunogenicity, and a certain degree of strength. Hence, it is a preferred material for TAC. Continuous VSD-assisted drainage helps control infection, promotes granulation tissue growth, and avoids retraction of the abdominal wall. This further enhances the repair of the abdominal wall and prevents the bulge of the bowels. However, VSD cannot be in direct contact with the abdominal organs. Greater omentum or an ADM layer is required to avoid organ damages. The combined use of ADM and VSD greatly protected the abdominal organs, effectively drained the bowel fluids, accelerated infection control, promoted granulation tissue growth, and fully prepared for the repair and reconstruction of the abdominal wall defects using the ALT flap.
Repair of huge abdominal wall defects following electrical burns using a combined ALT and TFL free flap effectively restored the integrity of the abdominal wall, maintained the tension and shape of the abdominal wall, and avoided complications such as abdominal wall ulcer, abdominal wall hernia, bowel obstruction, and bowel fistula in the long term. The present case might serve as a reference for the treatment of similar patients.
Satisfactory functional and aesthetic effects were achieved following the abdominal wall repair. However, severe bowel adhesions remained in the abdominal cavity, making intra-abdominal surgery impossible for the patient. Therefore, no closure of ileostomy was done for the patient, and he had to live with an ileostomy bag for a long time. More clinical studies should be performed in the future to provide solution to the aforementioned problem.
Manuscript source: Unsolicited manuscript
Specialty type: Medicine, research and experimental
Country/Territory of origin: China
Peer-review report’s scientific quality classification
Grade A (Excellent): 0
Grade B (Very good): B
Grade C (Good): 0
Grade D (Fair): 0
Grade E (Poor): 0
P-Reviewer: Ramesh B S-Editor: Fan JR L-Editor: Wang TQ P-Editor: Li JH
| 1. | Maloney SR, Augenstein VA, Oma E, Schlosser KA, Prasad T, Kercher KW, Sing RF, Colavita PD, Heniford BT. The use of component separation during abdominal wall reconstruction in contaminated fields: A case-control analysis. Am J Surg. 2019;218:1096-1101. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 5] [Cited by in F6Publishing: 7] [Article Influence: 1.4] [Reference Citation Analysis (0)] |
| 2. | Kadoch V, Bodin F, Himy S, Bollecker V, Wilk A, Bruant-Rodier C. Latissimus dorsi free flap for reconstruction of extensive full-thickness abdominal wall defect. A case of desmoid tumor. J Visc Surg. 2010;147:e45-e48. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 20] [Cited by in F6Publishing: 20] [Article Influence: 1.4] [Reference Citation Analysis (0)] |
| 3. | Chou PY, Kao D, Denadai R, Huang CY, Lin CH, Lin CH. Anterolateral thigh free flaps for the reconstruction of scalp angiosarcoma - 18-year experience in Chang Gung memorial hospital. J Plast Reconstr Aesthet Surg. 2019;72:1900-1908. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 8] [Cited by in F6Publishing: 8] [Article Influence: 1.6] [Reference Citation Analysis (0)] |
| 4. | Shih PK. Feasibility of pedicled anterolateral thigh flap with tensor fascia lata and vastus lateralis for difficult abdominal wall closure. Hernia. 2019;23:749-755. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 14] [Cited by in F6Publishing: 14] [Article Influence: 2.3] [Reference Citation Analysis (0)] |
| 5. | Kagaya Y, Arikawa M, Kobayashi E, Kawai A, Miyamoto S. Successful Pregnancy and Delivery after Autologous Abdominal Wall Reconstruction using Anterolateral-Thigh and Iliotibial-Tract Flap. Plast Reconstr Surg Glob Open. 2018;6:e1819. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 2] [Cited by in F6Publishing: 2] [Article Influence: 0.3] [Reference Citation Analysis (0)] |
| 6. | Kagaya Y, Arikawa M, Higashino T, Miyamoto S. Autologous abdominal wall reconstruction using anterolateral thigh and iliotibial tract flap after extensive tumor resection: A case series study of 50 consecutive cases. J Plast Reconstr Aesthet Surg. 2020;73:638-650. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 5] [Cited by in F6Publishing: 4] [Article Influence: 0.8] [Reference Citation Analysis (0)] |
| 7. | Karhof S, Hietbrink F, Boot R, van Wessem KJP, Leenen LPH, Simmermacher RKJ. Management strategies and outcome of blunt traumatic abdominal wall defects: a single centre experience. Injury. 2019;50:1516-1521. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 3] [Cited by in F6Publishing: 3] [Article Influence: 0.6] [Reference Citation Analysis (0)] |
| 8. | Justo I, Manrique A, Calvo J, Marcacuzco A, Caso Ó, García-Sesma Á, Nutu A, García-Conde M, Cambra F, Loinaz C, Jiménez-Romero C. Abdominal wall transplantation in organ transplantation: Our experience. Cir Esp. 2019;97:247-253. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 2] [Cited by in F6Publishing: 2] [Article Influence: 0.4] [Reference Citation Analysis (0)] |
| 9. | Caliceti U, Sgarzani R, Cipriani R, Cantore S, Contedini F, Pinto V, Gelati C, Piccin O. Single stage reconstruction of complex head and neck defects involving the skin with a single ALT flap: A ten year review. JPRAS Open. 2019;22:55-64. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 3] [Cited by in F6Publishing: 3] [Article Influence: 0.6] [Reference Citation Analysis (0)] |