Published online Mar 20, 2024. doi: 10.5662/wjm.v14.i1.90127
Peer-review started: November 23, 2023
First decision: November 30, 2023
Revised: December 19, 2023
Accepted: January 16, 2024
Article in press: January 16, 2024
Published online: March 20, 2024
Processing time: 104 Days and 11.5 Hours
Systemic hypertension is an established risk factor for coronary artery disease and cerebrovascular accident and control of blood pressure reduces the risk of a major cardiovascular event. Both non-pharmacological and pharmacological treatment options are available to treat hypertension. Yoga, recently received more attention as a treatment modality for various lifestyle disorders, even though practiced in India since ancient times. In this review, we are analyzing the role of yoga in the treatment of systemic hypertension.
Core Tip: Lifestyle modification is a vital component in the management of hypertension in addition to pharmacotherapy. However, it is infrequently practiced in day-to-day life. Yoga practice helps in clinically relevant reduction in blood pressure in people with hypertension. However, there is a scarcity of the necessary information and awareness not only among the general population but also among healthcare professionals regarding the benefits of yoga in hypertension. Awareness of various yoga practices suitable for hypertension, their respective effects, and the necessary precautions when performing them helps in utilizing this in day-to-day life.
- Citation: Joshi AM, Raveendran AV, Arumugam M. Therapeutic role of yoga in hypertension. World J Methodol 2024; 14(1): 90127
- URL: https://www.wjgnet.com/2222-0682/full/v14/i1/90127.htm
- DOI: https://dx.doi.org/10.5662/wjm.v14.i1.90127
Systemic hypertension is a major public health issue and of the total hypertensives, only about 1 in 4 adults (24%) have well-controlled hypertension[1]. It is an established risk factor for coronary artery disease, cerebrovascular accident, cardiac failure, atrial fibrillation, chronic kidney disease, heart valve diseases, aortic syndromes, and dementia[2].
Hypertension accounts for 14% of deaths and control of hypertension is associated with a 35% to 40% reduction in the risk of cerebrovascular accident, a 50% reduction in the risk of heart failure, and a 20%-25% reduction in the risk of myocardial infarction[3,4]. Uncontrolled hypertension contributes to 49% of coronary artery disease and 62% of cerebrovascular disease[2]. On average, a 5 mm of Hg reduction in systolic blood pressure (BP) reduces the risk of a major cardiovascular event by about 10%[5].
Lifestyle modifications like reduced dietary sodium intake, increased intake of fruits and vegetables, and regular physical exercise help in the prevention and treatment of hypertension in addition to pharmacological agents. Yoga is becoming increasingly popular not only among the general population but also among healthcare professionals as a modality to tackle various lifestyle diseases like hypertension, diabetes, and dyslipidemia.
Yoga is an art, a science, and a philosophy of living a healthy lifestyle. Originating in India over 5000 years ago, yoga was primarily about spiritual progress. “Yoga” means union, and signifies the merging of Atman, the individual conscious
Yoga practices have the potential to influence somatic and psychological functions on different levels. Therefore, yoga interventions should be planned and performed accordingly. Apart from ‘doing’ yoga postures or breathing practices, the cultivation of the right values and attitudes towards day-to-day stressors and adopting a yogic lifestyle is vital in reducing stress and managing hypertension[6].
The classical yoga texts describe the concept of chitta prasadanam (happiness of mind) and ways to achieve it. The mental qualities of maitri, karuna, mudita, and upeksha are suggested to achieve a blissful state of mind. They provide a yogic way of approaching a wide variety of situations in everyday life.
Maitri is an attitude of friendliness toward the happiness of others. It is the ability to share another person’s happiness instead of being jealous. Having such a perspective makes it possible for us to celebrate the beauty of human experiences. We can learn, understand, and grow through the friendship of happy and positive people. Karuna means compassion for the sorrows of those suffering. This is essential for spiritual and personal growth. It means helping if someone is upset, and comforting them. Compassion teaches us to be less judgmental and accept others as they are. It also develops an emotional understanding and bond. Mudita is a joyfulness towards the good deeds of others. It is about appreciating the virtuous qualities of others and finding inspiration to cultivate them. Upeksha refers to indifference towards the negative behavior of others. It is the quality of developing equanimity or neutrality towards those who were unkind, or those who have hurt us. Taking the opposite view towards negative thoughts and actions (pratipaksha bhavanam) also gives important insights into the management of emotions.
Mindfulness qualities such as living in the present moment, acceptance, letting go, gratitude, and loving-kindness are also effective antidotes for stress and anxiety.
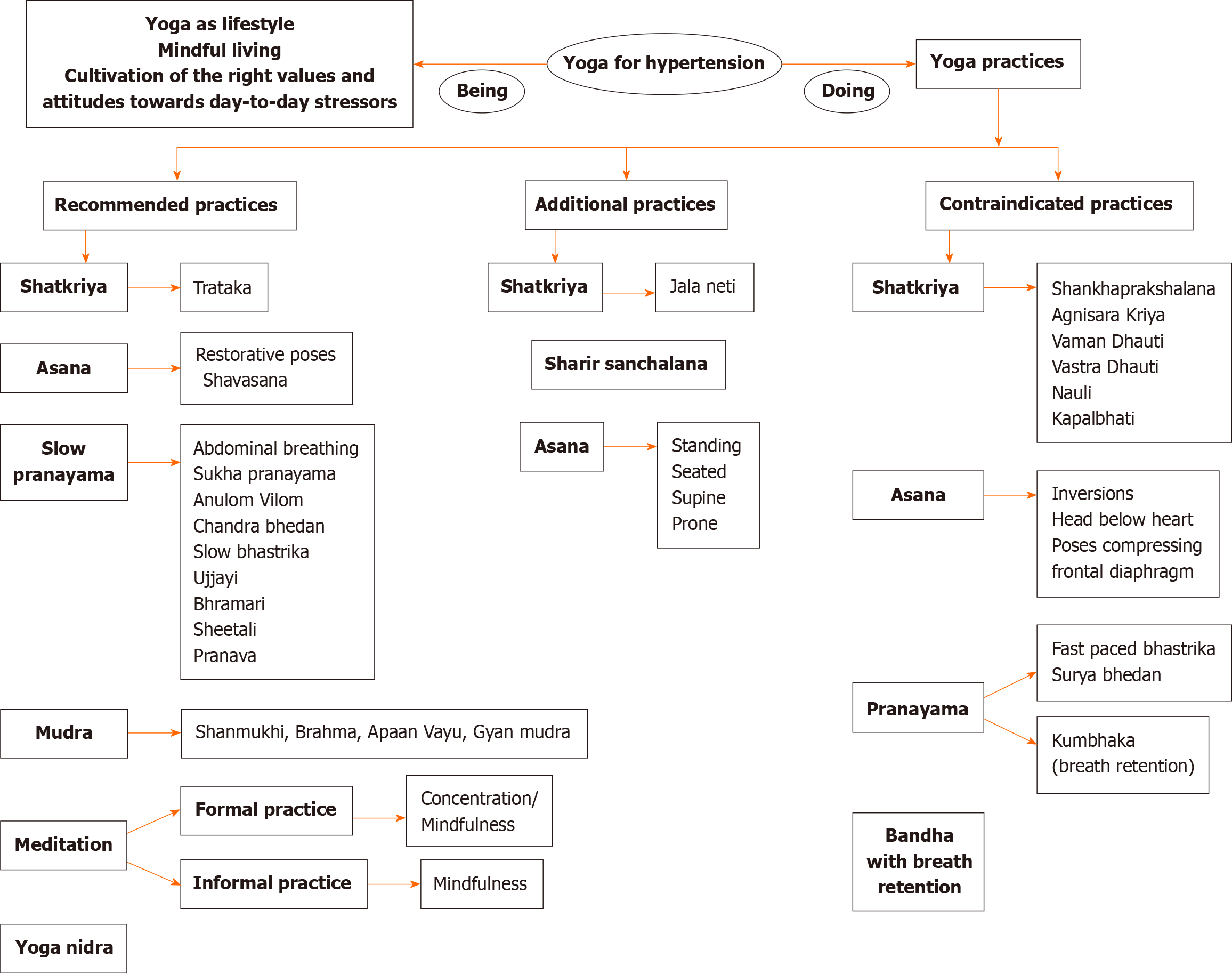
Sherman[7] proposed consideration of the domains such as style of yoga, the dose and delivery of yoga, components of the yoga intervention, specific class sequences, dealing with modifications, selection of instructors, facilitation of home practice and measurement of intervention fidelity over time while developing an appropriate yoga protocol. The yoga therapy prescription is based on the individual requirements of the patients. The following are some yoga practices recommended for hypertension (Table 1 and Figure 1). An additional file provides details of recommended yoga practices in hypertension with images (see Supplementary material).
| Yoga practice | Details of the yoga practice | Duration1 |
| Shatkriya (Yogic cleansing practices) | ||
| Shatkriya | Trataka (concentrated gazing) | 10 to 15 min |
| Jala neti (nasal cleansing with warm saline water) | 5 min (Once a week) | |
| Sharir sanchalana (Warm-up practices) | ||
| Sharir sanchalana (Warm-up practices) | Toe bending, ankle bending, knee bending, half butterfly, finger bending, wrist bending, elbow bending, shoulder rotation, and neck movements in a seated position with synchronization of breathing | 5 to 10 min |
| Surya namaskara (Sun salutations) | ||
| Surya namaskara (Sun salutations) | Series of dynamic yoga postures in a specific sequence with meditative awareness, practiced at slow-speed with breath synchronization | 3–7 rounds as per capacity; The postures can be held for a short period, without straining[6] |
| Asana (Yoga postures) for relaxation | ||
| Shavasana (Corpse pose) | Shavasana with slow, rhythmic diaphragmatic breathing, awareness of the sensation at the nostrils, the temperature of the inhaled and exhaled air, relaxing the muscles, and feeling the heaviness of different parts of the body | 5 to 30 min |
| Restorative Yoga (Conventional poses with props) | Supported and modified stretching to suit individual needs[11]; Shavasana (Corpse pose); Supta baddha konasana (Reclined bound angle pose); Upvistha konasana (Wide-angled seated forward bend); Balasana (Child's pose); Pashchimottanasana (Seated forward bend); Salamba kapotasana (Supported pigeon pose) | 15 min[11] |
| Other Asana (Additional practices) | ||
| Standing postures | Tadasana (Palm tree pose); Tiryak tadasana (Swaying palm tree pose); Katichakrasana (Standing spinal twist); Ardhachakrasana (Standing backward bend) | Synchronizing the movements with the breathing cycle; The postures can be held for a short period, without straining |
| Seated postures | Vakrasana (Seated spinal twist); Gomukhasana (Cow face Pose); Ardha Ushtrasana (Half camel pose); Pashchimottanasana (Seated forward bend); Marjarasana (Cat stretch) | |
| Prone postures | Bhujangasana (Cobra pose); Tiryak bhujangasana (Swaying cobra pose); Ardha Shalabhasana (Half locust pose) | |
| Supine postures | Pavanmuktasana (Wind releasing pose); Eka and Dwipada uttaanpadasana (straight single and both legs raising) | |
| Meditative Postures for Pranayama and Meditation | ||
| Meditative postures (Spine erect, shoulders relaxed, face softened) | Seated in a chair; Sukhasana (Comfort pose); Vajrasana (Thunderbolt pose); Ardha padmasana (Half lotus pose); Padmasana (Lotus pose) | During pranayama and meditation |
| Pranayama (Regulated breathing practices) | ||
| Deep abdominal breathing | Gentle deep inhalation and slow longer exhalation | 5 min |
| Sukha pranayama (Easy comfortable breathing) | Conscious, slow and deep breathing with equal duration for inhalation and exhalation) at the rate of 6 breaths/min | 5 min[16] |
| Anulom Vilom/Nadi shodhan pranayama (Alternate nostril breathing) | Gentle inhalation through the left nostril followed by exhalation through the right nostril. Next inhalation through the right nostril and exhalation through the left nostril | Upto 20 min[17] |
| Chandra nadi pranayama/Chandra bhedan pranayama (Left nostril breathing) | Unilateral left nostril breathing with inhalation and exhalation for an equal count of five; Variation: Inhalation through the left nostril followed by exhalation through the right nostril | 27 rounds of 6 breaths/min[19] |
| Slow bhastrika pranayama (Bellows breath) | Deep inhalation and slow exhalation (Respiratory rate 6/min), imagine the open blue sky while breathing[18] | 5 min[18] |
| Ujjayi pranayama (Ocean breath) | Slow inhalation and exhalation with a slight contraction around the glottis; Can be practiced in seated, supine, or standing position | 10 min[15] |
| Bhramari pranayama (Humming bee breath) | Slow deep inhalation followed by exhalation with a humming sound | 5 min[20] |
| Sheetali pranayama (Cooling breath) | Inhalation through curled tongue in the form of a tube, slow exhalation through the nose | 9 rounds each[9] |
| Pranava pranayama/ AUM chanting | Slow and deep inhalation with complete yogic breathing followed by the audible vibratory resonance of a prolonged AUM chant; Can be practiced in a supine position | 5 min[13] |
| Mudra (Subtle gestures) | ||
| Shanmukhi mudra (Closing the seven gates) | Closing the ears with the thumbs, placing the index fingers on the eyes, the middle fingers near the nostrils, the ring fingers, and the little fingers above and below the lips | Practiced during bhramari pranayama |
| Brahma mudra (Divine spiritual gesture) | Synchronizing neck movements with deep breathing and vibration sounds | 3 to 9 rounds of this practice at each sitting |
| Apan Vayu Mudra (Mudra of the heart) | Placing the tip of the index finger at the base of the thumb and joining the tips of the middle finger, ring finger, and thumb, the little finger extended | 15 min |
| Gyan mudra (Mudra of wisdom) | Joining the tips of the index finger and the thumb, other fingers extended | Practiced during pranayama and meditation; Up to 30 min a day |
| Meditation (Formal practice) | ||
| Concentration Meditation (Focus on a word, sound, prayer, mantra, or phrase) | Examples: AUM japa; Ajapa japa; Anahata (heart) chakra meditation with the mantra 'YAM' | 10-15 min |
| Mindfulness meditation (Open awareness of the present moment with kindness, acceptance, and curiosity) | Examples: Body scan meditation (Awareness of body parts); Mindful breathing meditation (Breath awareness); Loving-kindness meditation (having unconditional compassion towards ourselves and all other beings) | |
| Meditation (Informal/Integrated practice) | ||
| Mindfulness (Non-judgmental present-moment awareness during daily activities) | Examples: Mindful yoga (Yoga postures with awareness); Mindful Eating | Can be practiced anytime, anywhere in a day-to-day life |
| Yoga nidra (yogic sleep or effortless relaxation) | ||
| Yoga nidra | Relaxation practice that includes awareness of different body parts and breath, relaxation, auto-suggestions, and imagery | Up to 45 min[29] |
Shatkriya (Six cleansing practices): These are yogic cleansing techniques described in the Hatha Yoga texts. It is believed that regular internal cleansing enhances the functional capacity of the organs. There is limited scientific evidence on the efficacy of these practices in hypertension. Trataka (concentrated gazing) practice has been recommended for hypertension[8]. Jala neti (nasal cleansing with warm saline water) can be practiced once a week, however, other cleansing techniques are contraindicated[9].
Sharir Sanchalana (Warm-up practices): These are loosening exercises that relieve stiffness and prepare the body for the practice of asana. They ease tension accumulated in different body areas and improve blood circulation. For optimal pose performance and injury prevention, it is vital to perform sharir sanchalana before yoga practice.
Surya Namaskara (Sun salutation): It involves a series of dynamic yoga postures performed in a specific sequence. Slow-paced practice, according to the individual capacity, is advised for pre- and stage I hypertension[10]. Performing surya namaskara at a fast pace is comparable to aerobic exercise, resulting in increased strength and endurance. In contrast, slow-paced practice results in a decline in cardiovascular parameters to normal levels, similar to yoga training.
Asana (Yoga postures): Asana practiced with awareness is capable of bringing about the stability of body and mind. Asana practice improves the flow of vital energy through the body, resulting in a positive sense of well-being. It is a preparatory practice for meditation that fosters a quieting of the mind. The yoga postures should be modified to suit individual needs, considering other associated comorbidities.
Pandey et al[11] suggested the potential of gentle restorative yoga as a therapeutic option for hypertensive patients. In this practice, props are used to facilitate stretching, provide support, and induce relaxation in a yoga pose. Shavasana (corpse pose) is the most important posture described widely in the management of hypertension[12]. While relaxation poses and gentle restorative yoga postures are mostly effective in hypertension, other asanas may be performed as additional practices. An additional file provides details of additional yoga practices in hypertension with images (see Supplementary material).
Pranayama (Regulated breathing practices): Pranayama is a vital component of yoga and is associated with the regulation of breathing. Pranayama can be added as a supportive therapy with drugs in mild or moderate cases of hypertension[13]. Slow breathing practices are effective in reducing BP and are recommended as the first treatment for low-risk hypertensive and prehypertensive patients who are reluctant to start medication[14]. Ujjayi pranayama (ocean breath) without breath retention significantly decreases stress-induced changes in cardiorespiratory parameters and decreases BP[15]. Studies have shown immediate benefits of sukha pranayama (easy, comfortable breathing)[16], nadi shodhana (alternate nostril breathing)[17], slow-paced bhastrika (bellows breath)[18], chandra nadi (left unilateral forced nostril breathing)[19], bhramari (humming breath)[20], sheetali (cooling breath)[21], and pranava (Aum chanting)[13] pranayama practices in reduction of BP.
Pranayama and meditation can be practiced while sitting in a chair, sukhasana (comfort pose), ardha padmasana (half lotus pose), padmasana (lotus pose), or vajrasana (thunderbolt pose). In these meditative postures, the heart rate and the breath slow down, which lowers the BP.
Mudra (Subtle gestures): Mudra is a term meaning a ‘bodily position’ or ‘subtle gesture’. Mudra can be practiced independently or incorporated into yoga postures, pranayama, and meditation. The effects of yoga practices are enhanced with mudra, as they deepen awareness and concentration.
Dhyana (Meditation): There are two major types of meditation, concentration and open awareness. Concentration meditation involves a focus on a word, sound, prayer, or phrase. Expansive, open awareness or mindfulness meditations emphasize developing a passive attitude towards intruding thoughts, emotions, or body sensations, and a return to focus. Both types have a significant effect in reducing BP[22,23]. Mindfulness meditations can be practiced as formal, dedicated practice, or informal, integrated practice during the activities of daily life. While the formal practice deepens the meditation experience, the informal practice emphasizes meditation as a way of living.
Yoga Nidra (Yogic sleep or effortless relaxation): Yoga nidra is a comprehensive, profound relaxation technique for removing physical, mental, and emotional tensions. This practice includes awareness of different body parts, relaxation, breath awareness, auto-suggestions, and imagery. It reduces anxiety, and stress and improves autonomic functions in hypertensive patients[24].
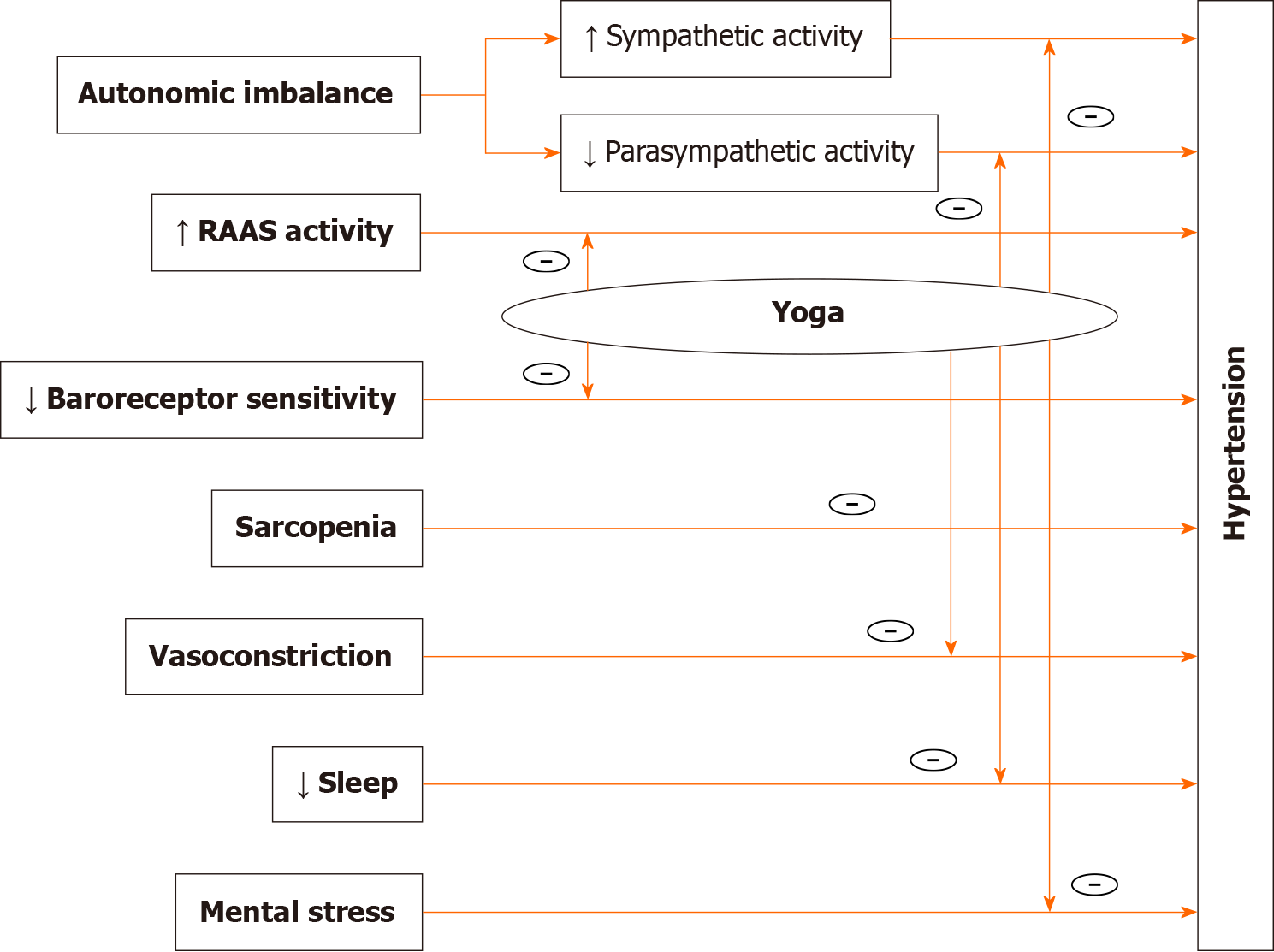
Various mechanisms (Figure 2) by which yoga practices reduce BP include:
Yoga, by reducing mental stress and autonomic imbalance, helps to prevent and control hypertension[24,25]. Mental stress and sympathetic overactivity contribute to the development of systemic hypertension and cardiovascular morbidity[26]. Yoga modulates the physiological response to stress via neurohumoral activation[27]. It optimally balances the sympatho-vagal stress response[27]. Yoga cultivates psychosomatic harmony, induces relaxation, and reduces stress. As a result, emotional stability occurs, the somatization symptoms are relieved, and the systolic and diastolic BP is reduced[23]. Chronic stress-induced sustained muscular contraction reduces the lumen/diameter of blood vessels in the muscles. This can lead to increased BP. Yoga induces relaxation and decreases arterial tone and peripheral resistance. Yoga is also helpful in various stress-induced psychological disorders like anxiety, depression, and insomnia[24].
Yoga practices specifically affect cardiovascular autonomic regulation and tend to normalize it[28]. They control the autonomic nervous system and influence the brain’s electrical rhythms, heart rate, and systolic and diastolic BP[29]. Yoga relaxation[12], and slow-paced pranayama techniques[17,20,21] decrease sympathetic activity and enhance parasympathetic activity. These practices optimally balance sympatho-vagal stress response and enhance healthy cardiovascular functioning[16,27,30].
Various yogic practices also reduce chemoreceptor response and improve baroreceptor sensitivity, which restores BP to normal in patients with essential hypertension[25]. Baroreceptor sensitivity can be enhanced significantly by slow breathing practices of yoga[18]. Ujjayi pranayama (ocean breath) exerts gentle pressure on the carotid sinuses. Many baroreceptors in the carotid sinus serve as ‘sampling areas’ for homeostatic mechanisms that maintain BP. Improvement in baroreflex sensitivity results in the normalizing of autonomic cardiovascular rhythms[24].
Some yoga postures exert controlled pressure on the kidneys and the adrenals, regulating blood supply to them, which mainly regulates BP through secretions of hormones like renin, angiotensin, adrenalin, etc[31].
Yoga-based lifestyle intervention is an important treatment modality in the reduction of BP, as is found to be beneficial in various other cardiovascular risk factors like obesity, dyslipidemia, and diabetes mellitus[32,33].
Studies have shown an association between insomnia and elevated BP of stage 1 and 2 hypertension[34]. Yoga practices such as Om chanting and yoga nidra are beneficial in improving the sleep quality of chronic insomnia patients[24]. Yoga has been suggested as an adjuvant nonpharmacological option for making effective and sustainable changes in patients suffering from sleep disorders.
Sarcopenia, the age-related loss of muscle mass and muscle function, is associated with hypertension in older adults[35]. Yoga practice is beneficial to prevent and attenuate the age-related deterioration of physical health, muscular strength, and flexibility[36]. Holding yoga postures for a few seconds builds strength by using body weight for resistance, which in turn slows the onset of sarcopenia. They also strengthen the skeletal muscles and improve bone density. The effects of various yogic practices on managing hypertension and their mechanisms are mentioned in Table 2.
| Yoga Practice | Effect on hypertension | Mechanism of action |
| Shatkriya (Cleansing practices) | ||
| Trataka kriya | Significant reduction in BP and HR in patients with primary hypertension[8] | Induces calmness similar to a mental state during meditation[8] |
| Neti kriya | Clear up the head and neck region producing a sense of lightness[6]; Beneficial in reducing anxiety and depression | Reduce toxic accumulation in head and neck region |
| Sharir Sanchalana (Warm-up practices) | ||
| Sharir Sanchalana | Warm-up exercises prepare the body for the practice of asana | Removes stiffness in the muscles and joints; Improve blood circulation |
| Surya Namaskara (Sun salutations) | ||
| Slow practice of Surya Namaskara | Recommended for pre and stage I hypertension[10] | Produce psychosomatic harmony[6] |
| Asana (Yoga postures) | ||
| Asana practiced with awareness and breath synchronization | Prevent and attenuate the age-related deterioration of physical health, muscular strength, and flexibility[36]; Capable of bringing about the stability of body and mind; Improves the flow of vital energy through the body, resulting in a positive sense of well-being; Preparatory practice for meditation that fosters a quieting of the mind | Holding yoga postures for a few seconds build strength by using body weight for resistance, which in turn slows the onset of sarcopenia[36]; Mental relaxation and a state of “restful awareness”; Changes the long-held patterns of feelings and emotions; Exert controlled pressure on the kidneys and the adrenals, which regulates BP through secretions of hormones like renin, angiotensin, adrenaline, etc.[31] |
| Restorative Yoga | More effective with significantly greater reductions in BP and HR as compared to stretching[11] | Facilitates stretching, provides support, and induces relaxation. Releases habitual stress patterns that are stored in the body as areas of tension |
| Shavasana (corpse pose) with breath awareness | Effective in BP reduction[12] | Reduction in the load on the heart by blunting the sympathetic response along with an enhanced parasympathetic activity[12]; Allows the body and mind to integrate through mindful stillness |
| Forward bending poses | “Head-down” postures confer stress-reducing, calming, and mind-quietening benefits | Forward bends with head supported brings a sense of calm |
| Backward bending poses | Elevate low mood and have energizing effect | Chest opening poses that allow expansive inhalation; Stimulate the heart chakra associated with emotions and balance |
| Twisting postures | Release tension, and energize; Helps in de-stressing, relaxing, and unwinding | Relieve spinal stiffness and clear emotional blockages |
| Meditative postures | Maintain a steady comfortable position for a long time without conscious effort; Improve concentration and peace of mind | The heart rate and the breath slow down, which lowers the BP. Enhance feelings of being grounded, centred, and balanced |
| Pranayama (Regulated breathing practices) | ||
| Slow-paced pranayama | A modest reduction in BP[14] | Optimally balances sympathovagal stress response [27]; Baroreceptor sensitivity can be enhanced significantly by slow breathing[18] |
| Deep slow abdominal breathing | Effective in reduction of systolic BP | Improve vagal tone, increase parasympathetic dominance, and decrease sympathetic discharges[30] |
| Sukha pranayama (Easy, comfortable breathing) | A significant reduction in Heart rate, systolic pressure, pulse pressure, and mean arterial pressure[16] | Normalization of autonomic cardiovascular rhythms as a result of increased vagal modulation and/or decreased sympathetic activity and improved baroreflex sensitivity[16] |
| Immediate Effect of Nadi shodhana pranayama (Alternate nostril breathing) | Reduce the BP and HR[17] | Activating the parasympathetic nervous system and enhancing healthy cardiovascular functioning[17] |
| Slow pace (respiratory rate 6/min) bhastrika pranayama (Bellows breath) | Reduction in systolic and diastolic BP[18] | Enhanced parasympathetic activity[18] |
| Chandra nadi pranayama (Left unilateral forced nostril breathing) | An immediate decrease in cardiovascular parameters with the decrease in HR, systolic pressure, and pulse pressure[19] | Normalization of autonomic cardiovascular rhythms with increased vagal modulation and/or decreased sympathetic activity along with improvement in baroreflex sensitivity[19] |
| Bhramari pranayama (Humming breath) | Immediate positive effect on reducing the systolic BP[20] | Parasympathetic dominance[20] |
| Ujjayi pranayama (Ocean breath) without breath retention or bandhas | Significantly decreases stress-induced changes in cardiorespiratory parameters and decreases BP[15] | Shift autonomic nervous control toward the parasympathetic side[15]; Exerts gentle pressure on the carotid sinuses that regulates BP through homeostatic mechanisms |
| Sheetali pranayama (Cooling breath) | The immediate effect: reduce the systolic and diastolic BP in hypertensive patients[21] | Decreasing the sympathetic activity[21] |
| Pranava pranayama/AUM chanting | Five min of AUM chanting reduces systolic and diastolic BP[13]; Reduces depression, anxiety, and stress[24]; Improves quality of sleep[24]; Promotes relaxation, and provides calmness | Improvement in baroreflex sensitivity resulting in the normalizing of autonomic cardiovascular rhythms[24] |
| Mudra (Subtle gestures) | ||
| Brahma mudra (Divine spiritual gesture) | Induces a sense of relaxation and reinvigoration in the head and neck region that reduces stress[6] | Cultivates psychosomatic harmony, induces relaxation, reduces stress |
| Apaan vayu mudra (Mudra of the heart) | Reduction in systolic and diastolic BP | The finger position sensitizes nerves in the palm and wrist area resulting in a systemic effect on the cardiovascular system |
| Shanmukhi mudra (Closing the 7 gates) | Produces a sense of inner calm[6] | This mudra encourages ‘pratyahara’, which means withdrawing the mind inwards by blocking some of the sensory distractions of the surroundings |
| Gyan mudra (Mudra of wisdom) | Reduces mental stress, indicated in hypertension | Deepens awareness; Enhances meditation experience; Regulates the fire and air elements in the body |
| Meditation | ||
| Formal meditation | ||
| Concentration meditation | Significant decrease in the HR and systolic and diastolic BP[22]; Reduces stress and anxiety; Induces relaxation | Modulates the physiological response to stress via neurohumoral activation[22]; Decreases the arterial tone and the peripheral resistance |
| Mindfulness Meditation (Non-judgmental awareness of the present moment with kindness, acceptance, and curiosity) | Significant effect on reducing systolic and diastolic BP in patients with hypertension[23] | Focus on the moment with “acceptance” and “non-criticism” helps in regulating the emotional state. Emotional stability relieves the somatization symptoms and the BP is reduced[23] |
| Informal meditation | ||
| Mindfulness | Helps to cope face day-to-day challenges and stressful situations | Serves as a ‘micro-meditation’ technique for quick stress relief |
| Yoga nidra (Yogic sleep or effortless relaxation) | ||
| Yoga nidra | Reduces systolic and diastolic BP[29]; Reduces depression, anxiety, and stress[24]; Improves quality of sleep[24] | Improve autonomic functions[24,29]; Influence the brain’s electrical rhythms[29] |
Population-based surveys and clinical trials suggest that yoga is a relatively safe intervention as compared to other forms of physical activity. However, the most commonly reported adverse effects of yoga are pain and soreness, muscle injuries, and fatigue[37]. To avoid the adverse effects, yoga should be learned under the guidance of a qualified yoga professional. Since the benefits of yoga are influenced by frequency, duration, and method of practice, the recommended yoga therapy protocol should be followed to gain optimum benefits[37].
Although yoga is an effective and promising approach to the management of hypertension, it should be used as a complementary therapy and not as a substitute for professional medical advice, diagnosis, and treatment of hypertension. It must be noted that yoga is not for medical emergencies.
Those who are having any health problems must get a medical opinion before proceeding with various yoga practices. Even if the BP is maintained at acceptable normal levels with medication, safety precautions should be followed.
The room where yoga is practiced should not be too hot as in ‘hot yoga,’ since it increases cardiovascular strain, raising BP.
The following is a brief description of precautions and contraindications of yoga practices in hypertension (Table 3).
| Yoga practice | Details of yoga practice | Precautions and contraindications |
| Shatkriya (Yoga cleansing practices) | ||
| Shatkriya (Yoga cleansing practices) | Shankhaprakshalana (Alimentary tract cleansing); Agnisara Kriya (Activating the digestive fire); Vaman dhauti (Regurgitative cleansing); Vastra dhauti (Cloth cleansing); Nauli kriya (Abdominal massaging); Basti kriya (Yogic enema); Kapalbhati (Skull shining breath) | Contraindicated in hypertension[9]; Kapalbhati increases diastolic BP suggesting sympathetic stimulation[41]; Laghu shankhaprakshalana, the simplified and shorter version of shankhaprakshalana is suggested in mild to moderate hypertension[42] |
| Asana (Yoga postures) | ||
| Inversions and head below the heart postures | Shirshasana (Headstand pose); Sarvangasana (Shoulderstand pose); Chakrasana (Wheel pose); Halasana (Plough pose); Adhomukh shvanasana (Downward facing dog pose); Prasarit Padottanasana (Wide-Legged standing forward bend) | Cause a significant rise in both the systolic and diastolic arterial pressures; Contraindicated in hypertension[9,38]; Increase intrathoracic pressure and strain the cardiovascular system; Pooling of the blood in the head and neck region resulting in the rise of BP |
| Other asanas | Mayurasana (peacock pose); Dhanurasana (bow pose) | Compress the front of the diaphragm, which can raise the BP |
| Pranayama (Regulated breathing practices) | ||
| Pranayama pace | Fast breathing | Rapid breath practices may be unsafe in patients with hypertension and cardiovascular disease |
| Pranayama type | Bhastrika pranayama (Bellows breath) with rapid forceful inhalation and exhalation | Increases HR and BP, producing vasoconstriction[39] |
| Pranayama type | Surya bhedan/surya nadi pranayama (Right nostril breathing) | Sympathetic stimulating effect[39] |
| Pranayama technique | Kumbhaka (breath retention) | Significant increase in systolic, diastolic BP, and mean arterial pressure[40] due to combined effect of increased level of HR and total peripheral resistance during kumbhaka |
| Bandha (lock) | ||
| Bandha (lock); Practiced with breath retention | Mula Bandha (Root lock, pulling the perineum inward); Uddiyan Bandha (Abdominal lock, lifting of the diaphragm); Jalandhar Bandha (Chin Lock, pressing the chin on the chest and contracting the throat) | Long retention of breath strains the heart and is not recommended for hypertension[9]; If the jalandhar bandha is not performed properly, the BP is raised |
Hypertensive practitioners have even higher BP during an exercise and in holding a static yoga posture, proportionate to the effort required to practice. Overstraining and excess muscular efforts stimulate the sympathetic nervous system, resulting in increased BP. Therefore, it is advised to refrain from the stronger forms of practices and holding static postures for long periods[38]. Relaxation in shavasana at the end of asana practice is beneficial.
Aggressive and sudden changes in yoga postures such as standing up quickly from a lying down position should be avoided as they may be stressful. Care should be taken while practicing backbends, especially in a standing position. Breath should not be held during a yoga posture. Strenuous practice should also be avoided in the elderly or people with high ocular pressure disorders. During yoga practice, if the breath is rapid, and the person feels agitated, flushed, dizzy, or uncomfortable, it is advised to come out of the pose and rest in shavasana. Supported and modified stretching using blankets, bolsters, or a chair for support is also recommended.
Although inversions and head-below-heart postures improve health and reduce anxiety and stress, they are not recommended for people suffering from high BP[9,38]. They can cause a significant rise in both systolic and diastolic arterial pressures. In inverted yoga poses, the intra-thoracic pressure is increased. Pumping against gravity increases the cardiovascular strain, resulting in increased BP. Modifications in some of these yoga poses are recommended. For example, in balasana (child’s pose), or adho mukha shvanasana (downward facing dog pose), the head can be supported with folded blankets or pillows, so that it is at the level of the heart. In viparita karni (yoga inversion pose), supported legs up the wall position can give inversion benefits of lymphatic drainage and improved venous return from the lower extremities without adding the risk of increased BP. Other asanas such as mayurasana (peacock pose), and dhanurasana (bow pose) compress the front of the diaphragm, which can raise BP.
Pranayama is a safe practice suitable for all age groups. However, if practiced in the wrong way, it may cause harm or complications. Judicious practice under expert guidance is a must. Caution is required, especially for vulnerable patients and those having health concerns. Gentle, soothing, and relaxing pranayama practices are effective in the management of hypertension. No violent or fast breathing should be practiced. Overstraining is not recommended. The ratio of the inhalation and exhalation should not be forced.
Hyperventilation practices such as fast-paced bhastrika pranayama (bellows breath) may be unsafe in patients with hypertension and cardiovascular disease, as they cause vasoconstriction and increase BP[39]. Suryabhedan pranayama (right nostril breathing) has a sympathetic stimulating effect and should be avoided[10]. Practicing kumbhaka (breath retention) during pranayama can result in a significant increase in systolic, diastolic, and mean arterial pressure[40]. It may be due to the combined effect of an increased level of heart rate and total peripheral resistance during kumbhaka. It is contraindicated in hypertension, heart disease, and individuals recovering from an illness, surgery, or injury.
Bandha, which means to lock, close off, or stop, are yoga practices that redirect the flow of blood and lymph to other parts of the body. They consist of neuro-muscular locks and involve changes in internal pressure to a very high degree. The practice of bandha with long retention of breath strains the heart and is not recommended for hypertension[9]. Bandha practices during pranayama should also be avoided.
Kapalbhati (Skull shining breath), a popular breathing technique that consists of forceful exhalations followed by passive inhalations, increases diastolic BP, suggesting sympathetic stimulation[41]. Shankha prakshalana (alimentary tract cleansing) involves repeating rounds of drinking salt water, performing a set of asanas, and evacuating the bowels. This kriya (set of practices) can be risky for individuals with hypertension because water intake may lead to a rise in blood volume and, thus, cardiac output. The physical exertion involved in the procedure may further increase the heart rate. A short and simplified version of this kriya, known as laghu shankha prakshālana, requires a lesser physical strain. Preliminary evidence suggests its safety in patients with mild to moderate essential hypertension[42]. An additional file provides a brief description of contraindicated yoga practices in hypertension with images (see Supplementary material).
A meta-analysis showed that yoga had a modest and significant effect on BP control (systolic 4.17 and diastolic 3.26 mm of Hg)[43]. It was also observed that yoga had a significant effect on BP when compared to those not taking any treatment but had no effect in comparison with the exercise group. Subgroup analysis showed that maximum benefit was seen in those who were practicing postures, meditation, and breathing. Studies incorporating yoga postures, meditation, and breathing resulted in higher BP reduction (systolic 8.17 and diastolic 6.14 mm of Hg)[43]. However, according to some studies, the suggested key components of yoga intervention for hypertensive patients are breathing and meditation rather than physical activity[44]. In a meta-analysis, different yoga interventions were compared, and it was observed that only the studies that included breathing and/or meditation techniques without postures had significant effects on hypertension[45]. BP reduction with yoga is compatible with other non-pharmacological interventions like exercise, and salt restriction[46]. Even this small reduction in BP in people with hypertension reduces the risk of cardiovascular events[47].
Yoga reduces BP significantly (systolic 7.96 and diastolic 5.52 mm of Hg) as compared to the no-treatment group and is comparable to exercise and other non-pharmacological treatment groups. Exercise and other non-pharmacological treatments reduce BP in the range of 3-9 mm of Hg as compared to the no-treatment group[43].
The average BP reduction with a single antihypertensive agent is about 10/5 mm of Hg and the addition of the second drug results in lower BP reduction[48]. Considering these facts, the amount of BP reduction achieved by yoga is significant and clinically relevant. Yoga practices combined with antihypertensive drugs have been shown to reduce BP and pulse rate during resting conditions, during stimulus-induced conditions, and in mild-to-moderate hypertension. In most hypertensive patients, it reduces the dose of antihypertensive drugs required[28].
There are studies showing no beneficial effect of yoga on BP. There are a lot of limitations in published studies, including small sample size, the absence of uniform yoga practices, the absence of adequate controls, and the absence of blinding and non-uniform research methodologies, making it difficult to compare various research protocols. Yoga practices, the duration of recommended practices, the techniques, and in some cases, even the names of yoga practices differ with different schools of yoga.
Standardized yoga therapy protocols for specific conditions are a debatable topic. A uniform set of practices cannot be recommended to every patient, as it requires a customized, tailor-made approach.
Yoga is sometimes termed as 'a laborious way to well-being' because of the time, effort, and motivation required for the practice. Yoga requires the person's willingness and cooperation for the practice. Patients' participation determines the treatment outcome in yoga therapy. Finally, it must be emphasized, that yoga is not a substitute for standard medical care and it is not for medical emergencies.
Yoga is an effective, time-honored, and promising approach to the management of hypertension. It is a safe intervention if practiced according to prescribed safety guidelines. Yoga practices influence various somatic and psychological functions and help to bring a state of physiological and psychological balance. This helps in clinically relevant reduction in BP in hypertension with a reduction in the dose of antihypertensive drugs required. Yoga postures, breathing practices, and meditation are the three most important components in the effective management of hypertension. Yoga therapy is not just about performing yoga, but also about the cultivation of the right values and attitudes towards day-to-day stressors. Yoga needs to be incorporated as a way of living a yogic lifestyle.
Provenance and peer review: Invited article; Externally peer reviewed.
Peer-review model: Single blind
Corresponding Author's Membership in Professional Societies: Association of Physicians of India, L-16571.
Specialty type: Medicine, general and internal
Country/Territory of origin: India
Peer-review report’s scientific quality classification
Grade A (Excellent): 0
Grade B (Very good): 0
Grade C (Good): C
Grade D (Fair): 0
Grade E (Poor): 0
P-Reviewer: Wang KJ, China S-Editor: Liu JH L-Editor: A P-Editor: Zhao YQ
| 1. | Centers for Disease Control and Prevention, National Center for Health Statistics. High blood pressure. Accessed December 30, 2022. Available from: https://www.cdc.gov/bloodpressure/facts.htm. |
| 2. | Fuchs FD, Whelton PK. High Blood Pressure and Cardiovascular Disease. Hypertension. 2020;75:285-292. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 912] [Cited by in RCA: 1004] [Article Influence: 200.8] [Reference Citation Analysis (37)] |
| 3. | Mills KT, Stefanescu A, He J. The global epidemiology of hypertension. Nat Rev Nephrol. 2020;16:223-237. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1423] [Cited by in RCA: 1952] [Article Influence: 390.4] [Reference Citation Analysis (3)] |
| 4. | Antonakoudis G, Poulimenos L, Kifnidis K, Zouras C, Antonakoudis H. Blood pressure control and cardiovascular risk reduction. Hippokratia. 2007;11:114-119. [PubMed] |
| 5. | Blood Pressure Lowering Treatment Trialists' Collaboration. Pharmacological blood pressure lowering for primary and secondary prevention of cardiovascular disease across different levels of blood pressure: an individual participant-level data meta-analysis. Lancet. 2021;397:1625-1636. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 374] [Cited by in RCA: 601] [Article Influence: 150.3] [Reference Citation Analysis (1)] |
| 6. | Bhavanani YD. Normalization of the blood pressure with Yoga. In Proceedings of the International Interdisciplinary Scientific Conference "Yoga in Science-Future and Perspectives" organised by the Yoga Federation of Serbia, Belgrade Sept 2010; 23-24. |
| 7. | Sherman KJ. Guidelines for developing yoga interventions for randomized trials. Evid Based Complement Alternat Med. 2012;2012:143271. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 104] [Cited by in RCA: 102] [Article Influence: 7.8] [Reference Citation Analysis (0)] |
| 8. | Kusuma AS, Nandeesh NS, Shetty S, Shetty P. Immediate effect of trataka on blood pressure indices in individuals with primary hypertension-a randomized controlled trial. Arterial Hypertension. 2021;25:82-87. [RCA] [DOI] [Full Text] [Reference Citation Analysis (4)] |
| 9. | Saraswati SS. In: Asana, pranayama, mudra bandha. Bihar: Yoga Publications Trust; 2012. |
| 10. | Karpagam S, Gaur GS, Trakroo M, Kumar SS. Comparative Study of effect of Slow and Fast Suryanamaskar on Work Load of Heart in Normal Human Subjects. International Journal of Physiology. 2013;1: 166-169. [DOI] [Full Text] |
| 11. | Pandey A, Huq N. Acute and sub-acute hemodynamic effects of restorative yoga. JACC. 2017;69:1735. [RCA] [DOI] [Full Text] [Reference Citation Analysis (1)] |
| 12. | Madanmohan, Udupa K, Bhavanani AB, Krishnamurthy N, Pal GK. Modulation of cold pressor-induced stress by shavasan in normal adult volunteers. Indian J Physiol Pharmacol. 2002;46:307-312. [PubMed] |
| 13. | Arora J, Dubey N. Immediate benefits of" Om" chanting on blood pressure and pulse rate in uncomplicated moderate hypertensive subjects. Natl J Physiol Pharm Pharmacol. 2018;8:1162-1165. [DOI] [Full Text] |
| 14. | Chaddha A, Modaff D, Hooper-Lane C, Feldstein DA. Device and non-device-guided slow breathing to reduce blood pressure: A systematic review and meta-analysis. Complement Ther Med. 2019;45:179-184. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 15] [Cited by in RCA: 8] [Article Influence: 1.3] [Reference Citation Analysis (1)] |
| 15. | Mahour J, Verma P. Effect of ujjayi pranayama on cardiovascular autonomic function tests. Natl J Physiol Pharm Pharmacol. 7:391. [DOI] [Full Text] |
| 16. | Bhavanani AB, Sanjay Z, Madanmohan. Immediate effect of sukha pranayama on cardiovascular variables in patients of hypertension. Int J Yoga Therap. 2011:73-76. [PubMed] |
| 17. | Tripathy M, Sahu B. Immediate Effect of Nadi Shodhana Pranayama on Blood Glucose, Heart Rate and Blood Pressure. Am J Sci. 2019;15:65-70. [DOI] [Full Text] |
| 18. | Pramanik T, Sharma HO, Mishra S, Mishra A, Prajapati R, Singh S. Immediate effect of slow pace bhastrika pranayama on blood pressure and heart rate. J Altern Complement Med. 2009;15:293-295. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 85] [Cited by in RCA: 93] [Article Influence: 5.8] [Reference Citation Analysis (0)] |
| 19. | Bhavanani AB, Madanmohan, Sanjay Z. Immediate effect of chandra nadi pranayama (left unilateral forced nostril breathing) on cardiovascular parameters in hypertensive patients. Int J Yoga. 2012;5:108-111. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 24] [Cited by in RCA: 27] [Article Influence: 2.1] [Reference Citation Analysis (0)] |
| 20. | Sathe S, Thodge K, Rajandekar T, Agrawal A. To find out immediate effect of bhramari pranayama on blood pressure, heart rate and oxygen saturation in hypertensive patients. IJCRR. 2020;12:193-197. [DOI] [Full Text] |
| 21. | Kumar N, Thanalakshmi J, Kannan R, Kumar M, Allu AR, Vijayalakshmi B. The immediate effect of Sheethali and Sheethkari Pranayama on blood pressure and cardiovascular changes among hypertensive patients. IJRPS. 2018;9:1249-1252. [DOI] [Full Text] |
| 22. | Sinha SS, Jain AK, Tyagi S, Mahajan AS. Effect of meditation on heart rate, blood pressure and exercise performance in coronary artery disease patients. Indian J Physiol Pharmacol. 2018;62:209-216. |
| 23. | Liu Y, Liu JQ, Li X, Zhong ZB. Research Progress of the Intervention Effect of Mindfulness Therapy on Patients with Hypertension. In2020 4th International Seminar on Education, Management and Social Sciences (ISEMSS 2020) 2020 Aug 28 (pp. 1109-1112). Atlantis Press. Accessed December 30, 2022. [DOI] [Full Text] |
| 24. | Rajagopalan A, Krishna A, Mukkadan JK. Effect of Om chanting and Yoga Nidra on depression anxiety stress, sleep quality and autonomic functions of hypertensive subjects - a randomized controlled trial. J Basic Clin Physiol Pharmacol. 2023;34:69-75. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1] [Cited by in RCA: 1] [Article Influence: 0.5] [Reference Citation Analysis (2)] |
| 25. | Tyagi A, Cohen M. Yoga and hypertension: a systematic review. Altern Ther Health Med. 2014;20:32-59. [PubMed] |
| 26. | Manolis AJ, Poulimenos LE, Kallistratos MS, Gavras I, Gavras H. Sympathetic overactivity in hypertension and cardiovascular disease. Curr Vasc Pharmacol. 2014;12:4-15. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 58] [Cited by in RCA: 75] [Article Influence: 6.8] [Reference Citation Analysis (0)] |
| 27. | Pal GK. Effects of pranayama on cardiovascular health. Int J Clin Exp Physiol. 2016;3:57-58. [DOI] [Full Text] |
| 28. | Jain PK, Malhotra V, Goel N, Gupta S. Effects of 40 days of pranayama training in hypertensive subjects. Int J Psychophysiol. 2019;7. [DOI] [Full Text] |
| 29. | Devraj JP, Santosh Kumar B, Raja Sriswan M, Jagdish B, Priya BS, Neelu SB, Desai Rao V, Kumar M, Geddam JJB, Hemalatha R. Effect of Yoganidra on Blood Pressure, Hs-CRP, and Lipid Profile of Hypertensive Subjects: A Pilot Study. Evid Based Complement Alternat Med. 2021;2021:2858235. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 4] [Reference Citation Analysis (1)] |
| 30. | Jerath R, Edry JW, Barnes VA, Jerath V. Physiology of long pranayamic breathing: neural respiratory elements may provide a mechanism that explains how slow deep breathing shifts the autonomic nervous system. Med Hypotheses. 2006;67:566-571. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 198] [Cited by in RCA: 219] [Article Influence: 11.5] [Reference Citation Analysis (0)] |
| 31. | Mittal K, Sirohi P, Mathur KC, Agrawal RP, Agrawal V. Effect of mind body therapy (yoga, meditation & music) on elderly hypertensive people. JCHM. 2016;3:108-112. [DOI] [Full Text] |
| 32. | Raveendran AV, Deshpandae A, Joshi SR. Therapeutic Role of Yoga in Type 2 Diabetes. Endocrinol Metab (Seoul). 2018;33:307-317. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 42] [Cited by in RCA: 65] [Article Influence: 9.3] [Reference Citation Analysis (1)] |
| 33. | Haider T, Sharma M, Branscum P. Yoga as an Alternative and Complimentary Therapy for Cardiovascular Disease: A Systematic Review. J Evid Based Complementary Altern Med. 2017;22:310-316. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 14] [Cited by in RCA: 15] [Article Influence: 1.7] [Reference Citation Analysis (0)] |
| 34. | Bathgate CJ, Fernandez-Mendoza J. Insomnia, Short Sleep Duration, and High Blood Pressure: Recent Evidence and Future Directions for the Prevention and Management of Hypertension. Curr Hypertens Rep. 2018;20:52. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 38] [Cited by in RCA: 59] [Article Influence: 8.4] [Reference Citation Analysis (0)] |
| 35. | Bai T, Fang F, Li F, Ren Y, Hu J, Cao J. Sarcopenia is associated with hypertension in older adults: a systematic review and meta-analysis. BMC Geriatr. 2020;20:279. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 25] [Cited by in RCA: 87] [Article Influence: 17.4] [Reference Citation Analysis (1)] |
| 36. | Halder K, Chatterjee A, Pal R, Tomer OS, Saha M. Age related differences of selected Hatha yoga practices on anthropometric characteristics, muscular strength and flexibility of healthy individuals. Int J Yoga. 2015;8:37-46. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 19] [Cited by in RCA: 12] [Article Influence: 1.2] [Reference Citation Analysis (0)] |
| 37. | Telles S, Sharma SK, Chetry D, Balkrishna A. Benefits and adverse effects associated with yoga practice: A cross-sectional survey from India. Complement Ther Med. 2021;57:102644. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 5] [Cited by in RCA: 13] [Article Influence: 2.6] [Reference Citation Analysis (1)] |
| 38. | Cramer H, Quinker D, Schumann D, Wardle J, Dobos G, Lauche R. Adverse effects of yoga: a national cross-sectional survey. BMC Complement Altern Med. 2019;19:190. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 29] [Cited by in RCA: 41] [Article Influence: 6.8] [Reference Citation Analysis (1)] |
| 39. | Nivethitha L, Mooventhan A, Manjunath NK. Effects of Various Prāṇāyāma on Cardiovascular and Autonomic Variables. Anc Sci Life. 2016;36:72-77. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 49] [Cited by in RCA: 41] [Article Influence: 4.6] [Reference Citation Analysis (0)] |
| 40. | Nivethitha L, Mooventhan A, Manjunath NK. A pilot study on evaluating cardiovascular functions during the practice of Bahir Kumbhaka (external breath retention). Adv Integr Med. 2017;4:7-9. [RCA] [DOI] [Full Text] [Cited by in Crossref: 4] [Cited by in RCA: 4] [Article Influence: 0.5] [Reference Citation Analysis (0)] |
| 41. | Gokhale V, Lakshmeesha DR, Shetty V, Rani V, Naresh Kumar M. Influence of kapalabhati pranayama on oxygen saturation and blood pressure. International Journal of Medical and Health Research. 2018;4:113-117. |
| 42. | Mashyal P, Bhargav H, Raghuram N. Safety and usefulness of Laghu shankha prakshalana in patients with essential hypertension: A self controlled clinical study. J Ayurveda Integr Med. 2014;5:227-235. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 11] [Cited by in RCA: 10] [Article Influence: 0.9] [Reference Citation Analysis (0)] |
| 43. | Hagins M, States R, Selfe T, Innes K. Effectiveness of yoga for hypertension: systematic review and meta-analysis. Evid Based Complement Alternat Med. 2013;2013:649836. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 63] [Cited by in RCA: 101] [Article Influence: 8.4] [Reference Citation Analysis (0)] |
| 44. | Cramer H. The Efficacy and Safety of Yoga in Managing Hypertension. Exp Clin Endocrinol Diabetes. 2016;124:65-70. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 11] [Cited by in RCA: 17] [Article Influence: 1.7] [Reference Citation Analysis (0)] |
| 45. | Cramer H, Haller H, Lauche R, Steckhan N, Michalsen A, Dobos G. A systematic review and meta-analysis of yoga for hypertension. Am J Hypertens. 2014;27:1146-1151. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 60] [Cited by in RCA: 60] [Article Influence: 5.5] [Reference Citation Analysis (0)] |
| 46. | Subramanian H, Soudarssanane MB, Jayalakshmy R, Thiruselvakumar D, Navasakthi D, Sahai A, Saptharishi L. Non-pharmacological Interventions in Hypertension: A Community-based Cross-over Randomized Controlled Trial. Indian J Community Med. 2011;36:191-196. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 28] [Cited by in RCA: 36] [Article Influence: 2.6] [Reference Citation Analysis (0)] |
| 47. | Hegde SV, Adhikari P, Kotian S, Pinto VJ, D'Souza S, D'Souza V. Effect of 3-month yoga on oxidative stress in type 2 diabetes with or without complications: a controlled clinical trial. Diabetes Care. 2011;34:2208-2210. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 90] [Cited by in RCA: 77] [Article Influence: 5.5] [Reference Citation Analysis (0)] |
| 48. | Swedish Council on Technology Assessment in Health Care. Moderately Elevated BloodPressure. 2013, Accessed December 30, 2022. (Published October 2004). Available from: http://www.sbu.se/upload/Publikationer/Content0/1/Blodtryck_2004/Hypertoni_vol2.pdf. |