Published online May 15, 2012. doi: 10.4251/wjgo.v4.i5.103
Revised: January 19, 2012
Accepted: March 10, 2012
Published online: May 15, 2012
AIM: To study if HER-2 overexpression by locally advanced esophageal cancers increase the chance of brain metastasis following esophagectomy.
METHODS: We retrospectively reviewed the medical records of esophageal cancer patients who underwent esophagectomy at University of Iowa Hospitals and Clinics between 2000 and 2010. Data analyzed consisted of demographic and clinical variables. The brain metastasis tissue was assayed for HER-2 overexpression utilizing the FDA approved DAKO Hercept Test®.
RESULTS: One hundred and forty two patients were reviewed. Median age was 64 years (36-86 years). Eighty eight patients (62%) received neoadjuvant chemoradiotherapy. Pathological complete and partial responses were achieved in 17 (19%) and 71 (81%) patients. Cancer relapsed in 43/142 (30%) patients. The brain was the first site of relapse in 9/43 patients (21%, 95% CI: 10%-36%). HER-2 immunohistochemistry testing of the brain metastasis tissue showed that 5/9 (56%) cases overexpressed HER-2 (3+ staining).
CONCLUSION: HER-2 overexpression might be associated with increased risk of brain metastasis in esophageal cancer patients following esophagectomy. Further studies will be required to validate this observation.
- Citation: Abu Hejleh T, DeYoung BR, Engelman E, Deutsch JM, Zimmerman B, Halfdanarson TR, Berg DJ, Parekh KR, Lynch WR, Iannettoni MD, Bhatia S, Clamon G. Relationship between HER-2 overexpression and brain metastasis in esophageal cancer patients. World J Gastrointest Oncol 2012; 4(5): 103-108
- URL: https://www.wjgnet.com/1948-5204/full/v4/i5/103.htm
- DOI: https://dx.doi.org/10.4251/wjgo.v4.i5.103
Brain metastasis from locally advanced esophageal cancer as the first site of disease relapse following multimodality treatment that includes chemotherapy, radiation therapy and esophagectomy is rare[1,2]. The incidence rate of brain metastasis, thought to be around 1%-5%, is derived from case series and autopsy reports[3,4]. Although the treatment goal of locally advanced esophageal cancer is to cure the disease, there is a high rate of disease relapse, whether locally or as distant metastasis, with the majority of relapses occurring in the liver, abdomen, lungs and bone[1]. Urba et al[5], showed that 65% of patients treated with concurrent chemotherapy and radiation therapy then esophagectomy had distant metastases rather than local recurrence upon relapse.
Multiple clinical and pathological features have been identified as prognostic factors in patients who receive concurrent chemoradiotherapy and esophagectomy. Factors including pathological complete response (pCR) to neoadjuvant treatment[6,7], lower tumor grade and stage[8,9], and smaller tumor length[10] are associated with favorable outcomes. Other trials showed that larger tumors and perioperative chemotherapy or radiation therapy might be associated with a higher risk of subsequent brain metastases[11,12]. In breast cancer, other risk factors such as over expression of HER-2, a membrane bound tyrosine kinase, were shown to predispose to brain metastasis (hazard ratio: 4.23, P = 0.0007)[13,14].
HER-2 is over expressed in approximately 25% of esophageal cancers[15,16] and is associated with a worse prognosis[17]. HER-2 receptor status became more clinically relevant after the ToGA trial showed that targeting HER-2 positive gastric and gastroesophageal junction tumors with Trastuzumab (Herceptin), a recombinant humanized monoclonal antibody that inhibits HER-2 receptor, combined with chemotherapy improved survival in patients with metastatic disease[18]. To our knowledge, there has been no correlation identified between esophageal cancer HER-2 receptor positivity and risk of brain metastasis.
A request to review the electronic medical records of esophageal cancer patients who underwent esophagectomy at University of Iowa Hospitals and Clinics was submitted to the Institutional Review Board (IRB) and approved (IRB identification number: 201012764). The requirement for consent was waived by the IRB. We identified the patients who had esophagectomy for esophageal cancer through the pathology department database. A total of 142 electronic medical charts of patients with locally advanced esophageal cancer who underwent esophagectomy at UIHC between January 2000 and September 2010 were reviewed. Patients characteristics collected include age, sex, smoking history, esophagectomy date, cancer stage, location in the esophagus, histology and grade, administration and response to neoadjuvant chemotherapy and radiation therapy, resection margins status, number of total and positive lymph nodes removed, cancer relapse, date and location of relapse and survival data. HER-2 overexpression was assayed on the brain metastasis tissue utilizing the FDA approved DAKO Hercept Test® with exact following of the technique as outlined in the product insert. Semi-quantitative interpretation was done in accordance with the parameters outlined for gastro-intestinal malignancies in the ToGA trial[18].
Kaplan-Meier curves were constructed for overall survival. To compare survival distributions for the patients who had complete or partial tumor response to neoadjuvant treatment, a log-rank test was used. Statistical analyses were performed using SAS (version 9.2).
Demographics and clinical data are presented in Table 1. Median age at diagnosis was 64 years (36-86 years). There were 124 males (87%) and 18 females (13%). The number of patients who smoked more than 10 pack-years was 87 (61.3%). There were 118 (83%) adenocarcinomas, 22 (15.5%) squamous cell carcinomas, 1 (0.7 %) small cell carcinoma and 1 (0.7 %) gastrointestinal stromal tumor. Regarding staging, 47/142 (33%) patients had stage T3N1M0 (AJCC 6th edition). The frequency of T classification was: T1: 18 (12.7%), T2: 19 (13.4%), T3: 76 (53.5%), T4: 2 (1.4%). The frequency of nodal classification was: N0: 49 (34.5%), N1: 65 (45.8 %), N2: 3 (2.1%). Neoadjuvant chemoradiotherapy was delivered for 88 patients (62%). Out of those, 17 (19 %) patients had pCR and 71 (81%) patients had pathological partial response (pPR).
| Characteristics | n (%) |
| Age on diagnosis of esophageal cancer (yr) | |
| Median | 64 |
| Range | 36-86 |
| Sex | |
| Male | 124 (87.3) |
| Female | 18 (12.7) |
| Smoking | |
| < 100 cigs/life | 33 (23.2) |
| < 10 pack-year | 9 (6.3) |
| > 10 pack-year | 87 (61.3) |
| Unknown | 13 (9.2) |
| Esophageal cancer type (path report) | |
| Adenocarcinoma | 118 (83.1) |
| Squamous cell carcinoma | 22 (15.5) |
| Small cell carcinoma | 1 (0.7) |
| GIST | 1 (0.7) |
| T classification | |
| T1 | 18 (12.7) |
| T2 | 19 (13.4) |
| T3 | 76 (53.5) |
| T4 | 2 (1.4) |
| Unknown | 27 (19) |
| N classification | |
| N0 | 49 (34.5) |
| N1 | 65 (45.8) |
| N2 | 3 (2.1) |
| Unknown | 25 (17.6) |
| Neoadjuvant treatment | |
| Neoadjuvant treatment | 88 (62) |
| No neoadjuvant treatment | 52 (36.6) |
| Unknown | 2 (1.4) |
| Response to neoadjuvant treatment | |
| No residual tumor (complete response) | 17 (12) |
| Residual tumor present (partial response) | 71 (50) |
| No neoadjuvant treatment | 52 (36.6) |
| Unknown | 2 (1.4) |
| Tumor grade | |
| Well differentiated | 4 (2.8) |
| Moderately differentiated | 67 (47.2) |
| Poorly differentiated | 61 (43) |
| Unknown | 10 (7) |
| Disease relapse | |
| Yes | 43 (30.3) |
| No | 91 (64.1) |
| Unknown | 8 (5.6) |
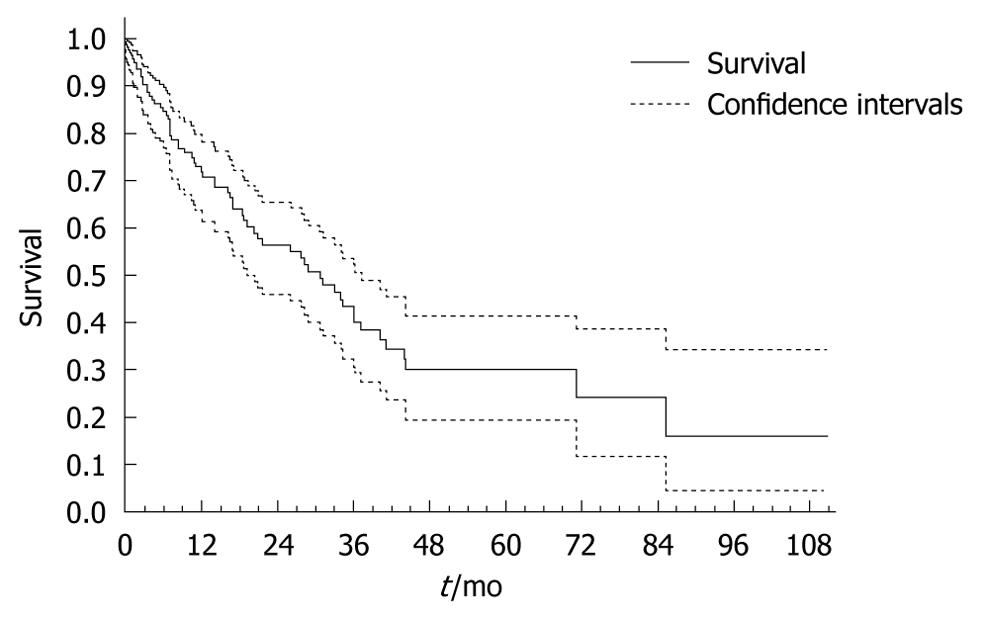
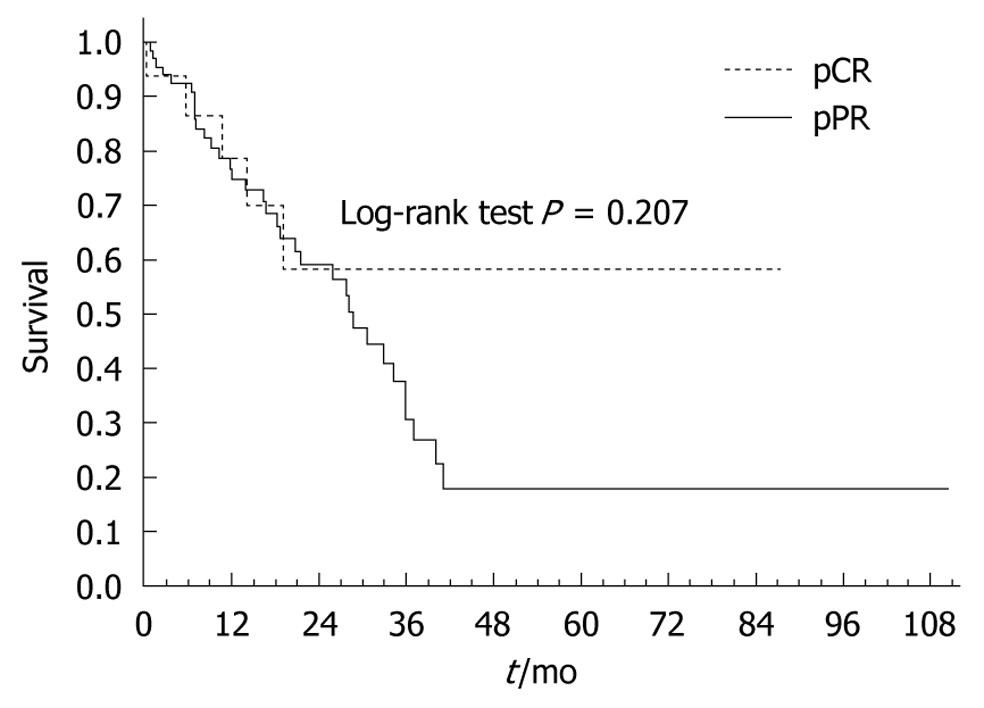
Regarding survival, 65/142 patients (45%) were deceased at the time of analysis. Overall survival for all patients is shown in Figure 1. Of the patients who reached pCR following neoadjuvant chemotherapy and radiation therapy, 58% were alive at 36 mo (median survival not reached). Median survival for the pPR patients was 28.8 mo (95% CI: 18.7-36.0). Although Figure 2 shows a survival difference for the patients who had pCR and pPR, this was not statistically significant (P = 0.207).
The total number of identified relapses was 43/142 (30.3%). Median follow up time was 11.8 mo (< 1-110 mo). Initial relapses occurred in the residual esophagus, para esophageal lymph nodes, mediastinum, liver, peritoneum, lungs, bone or brain. Frequencies of relapses at various sites are summarized in Table 2. There were 9/43 (21%) relapses in the brain (95% CI: 10%-36%) with the following characteristics: cancer stage T3N1M0 (7/9), neoadjuvant chemotherapy and radiation therapy (7/9), pCR (1/9), adenocarcinoma (7/9), squamous cell carcinoma (2/9).
| Relapse site | n (%) |
| Brain | 9 (21) |
| Peritoneum | 3 (7) |
| Esophageal remnants, paraesophageal lymph nodes or mediastinum (locoregional relapse) | 13 (30) |
| Lungs | 8 (19) |
| Liver | 6 (14) |
| Bone | 4 (9) |
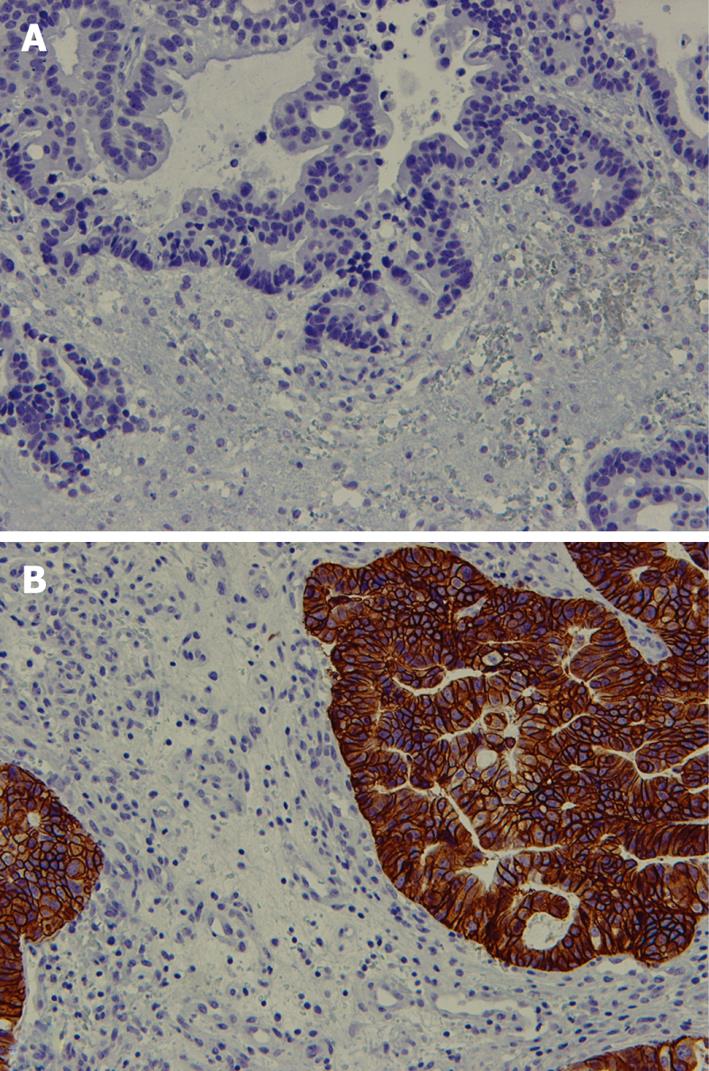
HER-2 immunohistochemistry staining of the brain metastasis specimens showed that 5/9 specimens (56%) overexpressed HER-2 (3+ staining). The rest of the specimens (4/9) did not stain for HER-2 (0 staining). Figure 3 shows brain metastasis specimens with 3+ and 0 staining.
Treatment of brain relapses included surgical resection (2 patients), stereotactic radiosurgery (SRS) (1 patient), surgical resection followed by SRS to the tumor bed (3 patients), and whole brain radiation (3 patients). Survival following diagnosis of brain relapse ranged from < 1-22 mo. Two patients who had brain surgery and SRS lived longer than others (18 and 22 mo).
Esophageal cancer is potentially a curable disease if diagnosed at an early stage but fatal when widely metastatic. The current standard of care of locally advanced esophageal cancer includes neoadjuvant concurrent chemotherapy and radiation therapy followed by esophagectomy[19,20]. Although significant advances have been made in achieving better quality of life and survival outcomes, it is estimated that only around 20% of the patients with local disease are alive 5 years following diagnosis[21,22].
Brain metastasis as the first site of disease relapse after esophagectomy for esophageal cancer is uncommon[3,4]. However, our study showed a higher frequency of brain relapses in locally advanced esophageal cancer patients who underwent esophagectomy compared to historical figures[1]. Recognizing the increased risk of brain metastasis in HER-2 positive breast cancer patients[13,14] and the known overexpression of HER-2 in esophageal cancers[23,24], we explored HER-2 expression status in the brain metastasis tissues obtained from esophageal cancer patients who underwent esophagectomy and relapsed in the brain. HER-2 was strongly positive in 56% of the cases which probably implies that HER-2 positivity in esophageal cancer predisposes to brain metastasis. Interestingly, in a phase I/II trial by Safran et al[25] testing Trastuzumab in HER-2 positive esophageal cancer patients, 3 out of the 10 relapses that occurred were in the central nervous systems (CNS).
Treatment of CNS metastasis, regardless of the primary cancer type, often includes surgery, radiation therapy or chemotherapy. Although surgical resection or SRS of a limited number of brain metastasis resulted in survival benefit in various cancers including esophageal cancer[26-28], chemotherapy treatment of CNS metastasis has been limited, primarily due to the blood brain barrier in addition to other factors[29,30]. Nevertheless, there have been recent advances in the chemotherapeutic management of CNS metastasis, whether parenchymal or leptomeningeal. Whereas Trastuzumab is known to be an effective treatment of metastatic HER-2 positive breast cancers, its CSF levels were reported to be low when administered intravenously[31]. Alternatively, intrathecal Trastuzumab showed encouraging results treating HER-2 positive breast cancer leptomeningeal metastasis[32,33]. Lapatinib, an oral HER-2 tyrosine kinase inhibitor that crosses the blood brain barrier, combined with Capecitabine resulted in partial and complete responses of brain metastasis from HER-2 positive breast cancers[34-37].
In summary, we noticed a high incidence of brain metastasis as the first site of cancer relapse in our series of locally advanced esophageal cancer patients who underwent esophagectomy. Additionally, we observed that HER-2 overexpression might be associated with increased risk of brain metastasis. The benefits of screening brain imaging in a selected population of HER-2 positive esophageal cancer patients before going through a major surgery such as esophagectomy and utilizing HER-2 directed therapy in case of brain relapse in that same subpopulation are potential considerations that deserve further exploration in future studies. Acknowledging the limitations of a retrospective study and the small sample size, our observations need to be replicated in a larger cohort.
The incidence of locoregional and advanced stage esophageal and gastroesophageal junction adenocarcinoma is rising in the western world. In spite of the treatment advances, recurrence rate of the locoregional disease is still high. Recently, there has been mounting evidence that the incidence of esophageal cancer relapse into the brain is rising, but no definite etiology has been identified so far to explain this observation.
HER-2 is a membrane tyrosine kinase that is over expressed in various cancers, including esophageal, breast and other cancers. It is well established that there is an association between HER-2 over expression and brain metastasis in breast cancer, but this correlation was not explored in esophageal cancer. In this study, the authors demonstrate that HER-2 over expressing locally advanced esophageal cancer patients might be prone to a higher incidence of brain relapse.
To our knowledge, this is the first study to suggest an association between esophageal cancer HER-2 status and the risk of brain metastasis. This finding is scientifically plausible given what we know about breast HER-2 over expression and brain metastasis. The test the authors used to examine the esophageal cancer HER-2 status (immunohistochemistry) is currently a standard and commonly used test in esophageal cancers as it has therapeutic implications. This broad application of HER-2 testing will definitely lead to identifying more patients who over express HER-2. Consequently, more robust studies with a larger sample size will be feasible to test the association between HER-2 over expression and brain relapse.
If subsequent larger studies support our observation of increasing risk of brain relapse from HER-2 overexpressing esophageal cancer, this will have various important implications. This subset of patients might benefit from screening brain imaging to rule our brain metastasis. This might decrease the number of futile esophagectomies which will be avoided if the patient is found to have brain metastasis before surgery. Additionally, there might be a role for biological agents, such as Trastuzumab or Lapatinib in the treatment of brain relapse from HER-2 overexpressing esophageal cancers.
HER-2 is a membrane tyrosine kinase involved in signal transduction pathways that regulate cellular proliferation. Overexpression of HER-2 was identified in various cancers, such as esophageal, gastric and breast cancers. It correlates with an aggressive disease and worse prognosis in breast cancer. Antibodies that target HER-2, such as Trastuzumab, are available for clinical use and commonly utilized in breast cancer. Trastuzumab was also found to prolong survival in advanced stage gastric and gastroesophageal cancers when administered with cytotoxic chemotherapies.
This paper presents an interesting topic about the relationship between HER-2 OVER expression and brain metastasis in esophageal cancer patients.
Peer reviewer: Dong Chang, MD, Department of Thoracic Surgery, Beijing Friendship Hospital, Capital Medical University, 95 YongAn Road, Beijing 100050, China
S- Editor Wang JL L- Editor Roemmele A E- Editor Zheng XM
| 1. | Meguid RA, Hooker CM, Taylor JT, Kleinberg LR, Cattaneo SM, Sussman MS, Yang SC, Heitmiller RF, Forastiere AA, Brock MV. Recurrence after neoadjuvant chemoradiation and surgery for esophageal cancer: does the pattern of recurrence differ for patients with complete response and those with partial or no response. J Thorac Cardiovasc Surg. 2009;138:1309-1317. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 79] [Cited by in F6Publishing: 74] [Article Influence: 4.9] [Reference Citation Analysis (0)] |
| 2. | Yoshida S. Brain metastasis in patients with esophageal carcinoma. Surg Neurol. 2007;67:288-290. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 37] [Cited by in F6Publishing: 45] [Article Influence: 2.5] [Reference Citation Analysis (0)] |
| 3. | Anderson LL, Lad TE. Autopsy findings in squamous-cell carcinoma of the esophagus. Cancer. 1982;50:1587-1590. [PubMed] [DOI] [Cited in This Article: ] [Cited by in F6Publishing: 1] [Reference Citation Analysis (0)] |
| 4. | Mandard AM, Chasle J, Marnay J, Villedieu B, Bianco C, Roussel A, Elie H, Vernhes JC. Autopsy findings in 111 cases of esophageal cancer. Cancer. 1981;48:329-335. [PubMed] [DOI] [Cited in This Article: ] [Cited by in F6Publishing: 1] [Reference Citation Analysis (0)] |
| 5. | Urba SG, Orringer MB, Turrisi A, Iannettoni M, Forastiere A, Strawderman M. Randomized trial of preoperative chemoradiation versus surgery alone in patients with locoregional esophageal carcinoma. J Clin Oncol. 2001;19:305-313. [PubMed] [Cited in This Article: ] |
| 6. | Hammoud ZT, Kesler KA, Ferguson MK, Battafarrano RJ, Bhogaraju A, Hanna N, Govindan R, Mauer AA, Yu M, Einhorn LH. Survival outcomes of resected patients who demonstrate a pathologic complete response after neoadjuvant chemoradiation therapy for locally advanced esophageal cancer. Dis Esophagus. 2006;19:69-72. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 35] [Cited by in F6Publishing: 39] [Article Influence: 2.2] [Reference Citation Analysis (0)] |
| 7. | Swisher SG, Hofstetter W, Komaki R, Correa AM, Erasmus J, Lee JH, Liao Z, Maru D, Mehran R, Patel S. Improved long-term outcome with chemoradiotherapy strategies in esophageal cancer. Ann Thorac Surg. 2010;90:892-898; discussion 898-899. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 41] [Cited by in F6Publishing: 44] [Article Influence: 3.1] [Reference Citation Analysis (0)] |
| 8. | Kim T, Grobmyer SR, Smith R, Ben-David K, Ang D, Vogel SB, Hochwald SN. Esophageal cancer--the five year survivors. J Surg Oncol. 2011;103:179-183. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 83] [Cited by in F6Publishing: 98] [Article Influence: 7.0] [Reference Citation Analysis (0)] |
| 9. | Yoon HH, Khan M, Shi Q, Cassivi SD, Wu TT, Quevedo JF, Burch PA, Sinicrope FA, Diasio RB. The prognostic value of clinical and pathologic factors in esophageal adenocarcinoma: a mayo cohort of 796 patients with extended follow-up after surgical resection. Mayo Clin Proc. 2010;85:1080-1089. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 33] [Cited by in F6Publishing: 36] [Article Influence: 2.6] [Reference Citation Analysis (0)] |
| 10. | Griffiths EA, Brummell Z, Gorthi G, Pritchard SA, Welch IM. Tumor length as a prognostic factor in esophageal malignancy: univariate and multivariate survival analyses. J Surg Oncol. 2006;93:258-267. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 52] [Cited by in F6Publishing: 58] [Article Influence: 3.2] [Reference Citation Analysis (0)] |
| 11. | Ogawa K, Toita T, Sueyama H, Fuwa N, Kakinohana Y, Kamata M, Adachi G, Saito A, Yoshii Y, Murayama S. Brain metastases from esophageal carcinoma: natural history, prognostic factors, and outcome. Cancer. 2002;94:759-764. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 81] [Cited by in F6Publishing: 90] [Article Influence: 4.1] [Reference Citation Analysis (0)] |
| 12. |
Rice TW, Khuntia D, Rybicki LA, Adelstein DJ, Vogelbaum MA, Mason DP, Murthy SC, Blackstone EH; Brain metastases from esophageal cancer: a phenomenon of adjuvant therapy |
| 13. | Tomasello G, Bedard PL, de Azambuja E, Lossignol D, Devriendt D, Piccart-Gebhart MJ. Brain metastases in HER2-positive breast cancer: the evolving role of lapatinib. Crit Rev Oncol Hematol. 2010;75:110-121. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 32] [Cited by in F6Publishing: 34] [Article Influence: 2.3] [Reference Citation Analysis (0)] |
| 14. | Gabos Z, Sinha R, Hanson J, Chauhan N, Hugh J, Mackey JR, Abdulkarim B. Prognostic significance of human epidermal growth factor receptor positivity for the development of brain metastasis after newly diagnosed breast cancer. J Clin Oncol. 2006;24:5658-5663. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 229] [Cited by in F6Publishing: 241] [Article Influence: 13.4] [Reference Citation Analysis (0)] |
| 15. | Liang Z, Zeng X, Gao J, Wu S, Wang P, Shi X, Zhang J, Liu T. Analysis of EGFR, HER2, and TOP2A gene status and chromosomal polysomy in gastric adenocarcinoma from Chinese patients. BMC Cancer. 2008;8:363. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 44] [Cited by in F6Publishing: 54] [Article Influence: 3.4] [Reference Citation Analysis (0)] |
| 16. | Polkowski W, van Sandick JW, Offerhaus GJ, ten Kate FJ, Mulder J, Obertop H, van Lanschot JJ. Prognostic value of Laurén classification and c-erbB-2 oncogene overexpression in adenocarcinoma of the esophagus and gastroesophageal junction. Ann Surg Oncol. 1999;6:290-297. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 89] [Cited by in F6Publishing: 100] [Article Influence: 4.0] [Reference Citation Analysis (0)] |
| 17. | Brien TP, Odze RD, Sheehan CE, McKenna BJ, Ross JS. HER-2/neu gene amplification by FISH predicts poor survival in Barrett's esophagus-associated adenocarcinoma. Hum Pathol. 2000;31:35-39. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 113] [Cited by in F6Publishing: 120] [Article Influence: 5.0] [Reference Citation Analysis (0)] |
| 18. | Bang YJ, Van Cutsem E, Feyereislova A, Chung HC, Shen L, Sawaki A, Lordick F, Ohtsu A, Omuro Y, Satoh T. Trastuzumab in combination with chemotherapy versus chemotherapy alone for treatment of HER2-positive advanced gastric or gastro-oesophageal junction cancer (ToGA): a phase 3, open-label, randomised controlled trial. Lancet. 2010;376:687-697. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 4615] [Cited by in F6Publishing: 4839] [Article Influence: 345.6] [Reference Citation Analysis (1)] |
| 19. | Tepper J, Krasna MJ, Niedzwiecki D, Hollis D, Reed CE, Goldberg R, Kiel K, Willett C, Sugarbaker D, Mayer R. Phase III trial of trimodality therapy with cisplatin, fluorouracil, radiotherapy, and surgery compared with surgery alone for esophageal cancer: CALGB 9781. J Clin Oncol. 2008;26:1086-1092. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 941] [Cited by in F6Publishing: 1000] [Article Influence: 62.5] [Reference Citation Analysis (0)] |
| 20. | Walsh TN, Noonan N, Hollywood D, Kelly A, Keeling N, Hennessy TP. A comparison of multimodal therapy and surgery for esophageal adenocarcinoma. N Engl J Med. 1996;335:462-467. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 1513] [Cited by in F6Publishing: 1398] [Article Influence: 49.9] [Reference Citation Analysis (0)] |
| 21. | Kelsen DP, Ginsberg R, Pajak TF, Sheahan DG, Gunderson L, Mortimer J, Estes N, Haller DG, Ajani J, Kocha W. Chemotherapy followed by surgery compared with surgery alone for localized esophageal cancer. N Engl J Med. 1998;339:1979-1984. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 1025] [Cited by in F6Publishing: 937] [Article Influence: 36.0] [Reference Citation Analysis (0)] |
| 22. | Cooper JS, Guo MD, Herskovic A, Macdonald JS, Martenson JA, Al-Sarraf M, Byhardt R, Russell AH, Beitler JJ, Spencer S. Chemoradiotherapy of locally advanced esophageal cancer: long-term follow-up of a prospective randomized trial (RTOG 85-01). Radiation Therapy Oncology Group. JAMA. 1999;281:1623-1627. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 1261] [Cited by in F6Publishing: 1302] [Article Influence: 52.1] [Reference Citation Analysis (0)] |
| 23. | al-Kasspooles M, Moore JH, Orringer MB, Beer DG. Amplification and over-expression of the EGFR and erbB-2 genes in human esophageal adenocarcinomas. Int J Cancer. 1993;54:213-219. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 172] [Cited by in F6Publishing: 163] [Article Influence: 5.3] [Reference Citation Analysis (0)] |
| 24. | Hardwick RH, Shepherd NA, Moorghen M, Newcomb PV, Alderson D. c-erbB-2 overexpression in the dysplasia/carcinoma sequence of Barrett's oesophagus. J Clin Pathol. 1995;48:129-132. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 48] [Cited by in F6Publishing: 52] [Article Influence: 1.8] [Reference Citation Analysis (0)] |
| 25. | Safran H, Dipetrillo T, Akerman P, Ng T, Evans D, Steinhoff M, Benton D, Purviance J, Goldstein L, Tantravahi U. Phase I/II study of trastuzumab, paclitaxel, cisplatin and radiation for locally advanced, HER2 overexpressing, esophageal adenocarcinoma. Int J Radiat Oncol Biol Phys. 2007;67:405-409. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 91] [Cited by in F6Publishing: 103] [Article Influence: 5.7] [Reference Citation Analysis (0)] |
| 26. | Flannery TW, Suntharalingam M, Regine WF, Chin LS, Krasna MJ, Shehata MK, Edelman MJ, Kremer M, Patchell RA, Kwok Y. Long-term survival in patients with synchronous, solitary brain metastasis from non-small-cell lung cancer treated with radiosurgery. Int J Radiat Oncol Biol Phys. 2008;72:19-23. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 81] [Cited by in F6Publishing: 88] [Article Influence: 5.5] [Reference Citation Analysis (0)] |
| 27. | Muacevic A, Kreth FW, Horstmann GA, Schmid-Elsaesser R, Wowra B, Steiger HJ, Reulen HJ. Surgery and radiotherapy compared with gamma knife radiosurgery in the treatment of solitary cerebral metastases of small diameter. J Neurosurg. 1999;91:35-43. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 207] [Cited by in F6Publishing: 221] [Article Influence: 8.8] [Reference Citation Analysis (0)] |
| 28. | Weinberg JS, Suki D, Hanbali F, Cohen ZR, Lenzi R, Sawaya R. Metastasis of esophageal carcinoma to the brain. Cancer. 2003;98:1925-1933. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 80] [Cited by in F6Publishing: 82] [Article Influence: 3.9] [Reference Citation Analysis (0)] |
| 29. | Bart J, Groen HJ, Hendrikse NH, van der Graaf WT, Vaalburg W, de Vries EG. The blood-brain barrier and oncology: new insights into function and modulation. Cancer Treat Rev. 2000;26:449-462. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 144] [Cited by in F6Publishing: 150] [Article Influence: 6.3] [Reference Citation Analysis (0)] |
| 30. | Cordon-Cardo C, O'Brien JP, Casals D, Rittman-Grauer L, Biedler JL, Melamed MR, Bertino JR. Multidrug-resistance gene (P-glycoprotein) is expressed by endothelial cells at blood-brain barrier sites. Proc Natl Acad Sci USA. 1989;86:695-698. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 1184] [Cited by in F6Publishing: 1163] [Article Influence: 33.2] [Reference Citation Analysis (0)] |
| 31. | Pestalozzi BC, Brignoli S. Trastuzumab in CSF. J Clin Oncol. 2000;18:2349-2351. [PubMed] [Cited in This Article: ] |
| 32. | Oliveira M, Braga S, Passos-Coelho JL, Fonseca R, Oliveira J. Complete response in HER2+ leptomeningeal carcinomatosis from breast cancer with intrathecal trastuzumab. Breast Cancer Res Treat. 2011;127:841-844. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 50] [Cited by in F6Publishing: 51] [Article Influence: 3.9] [Reference Citation Analysis (0)] |
| 33. | Platini C, Long J, Walter S. Meningeal carcinomatosis from breast cancer treated with intrathecal trastuzumab. Lancet Oncol. 2006;7:778-780. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 69] [Cited by in F6Publishing: 64] [Article Influence: 3.6] [Reference Citation Analysis (0)] |
| 34. | Metro G, Foglietta J, Russillo M, Stocchi L, Vidiri A, Giannarelli D, Crinò L, Papaldo P, Mottolese M, Cognetti F. Clinical outcome of patients with brain metastases from HER2-positive breast cancer treated with lapatinib and capecitabine. Ann Oncol. 2011;22:625-630. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 113] [Cited by in F6Publishing: 121] [Article Influence: 8.6] [Reference Citation Analysis (0)] |
| 35. | Glück S, Castrellon A. Lapatinib plus capecitabine resolved human epidermal growth factor receptor 2-positive brain metastases. Am J Ther. 2009;16:585-590. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 14] [Cited by in F6Publishing: 18] [Article Influence: 1.3] [Reference Citation Analysis (0)] |
| 36. | Ekenel M, Hormigo AM, Peak S, Deangelis LM, Abrey LE. Capecitabine therapy of central nervous system metastases from breast cancer. J Neurooncol. 2007;85:223-227. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 115] [Cited by in F6Publishing: 109] [Article Influence: 6.4] [Reference Citation Analysis (0)] |
| 37. | Lin NU, Diéras V, Paul D, Lossignol D, Christodoulou C, Stemmler HJ, Roché H, Liu MC, Greil R, Ciruelos E. Multicenter phase II study of lapatinib in patients with brain metastases from HER2-positive breast cancer. Clin Cancer Res. 2009;15:1452-1459. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 481] [Cited by in F6Publishing: 476] [Article Influence: 31.7] [Reference Citation Analysis (0)] |