Published online Nov 14, 2015. doi: 10.3748/wjg.v21.i42.12042
Peer-review started: April 18, 2015
First decision: May 18, 2015
Revised: May 28, 2015
Accepted: August 31, 2015
Article in press: August 31, 2015
Published online: November 14, 2015
Liver cancer is one of the world’s most common cancers and the second leading cause of cancer deaths. Hepatocellular carcinoma (HCC), a primary hepatic cancer, accounts for 90%-95% of liver cancer cases. The pathogenesis of HCC consists of a stepwise process of liver damage that extends over decades, due to hepatitis, fatty liver, fibrosis, and cirrhosis before developing fully into HCC. Multiple risk factors are highly correlated with HCC, including infection with the hepatitis B or C viruses, alcohol abuse, aflatoxin exposure, and metabolic diseases. Over the last decade, genetic alterations, which include the regulation of multiple oncogenes or tumor suppressor genes and the activation of tumorigenesis-related pathways, have also been identified as important factors in HCC. Recently, zebrafish have become an important living vertebrate model organism, especially for translational medical research. In studies focusing on the biology of cancer, carcinogen induced tumors in zebrafish were found to have many similarities to human tumors. Several zebrafish models have therefore been developed to provide insight into the pathogenesis of liver cancer and the related drug discovery and toxicology, and to enable the evaluation of novel small-molecule inhibitors. This review will focus on illustrative examples involving the application of zebrafish models to the study of human liver disease and HCC, through transgenesis, genome editing technology, xenografts, drug discovery, and drug-induced toxic liver injury.
Core tip: Hepatocellular carcinoma is one of the major cancers in the world and involves multiple mechanisms of tumor formation. Recently, the zebrafish has gained acceptance as a platform for developmental biology, drug toxicology, and translational medical research, offering innovative methods for studying disease and cancer formation. In this article, we summarize recent advances in the study of HCC based on the zebrafish as a model system through the use of transgenesis tools, genome editing technology, xenografts, drug hepatotoxicity, and novel drug discovery. Finally, we emphasize how each system works and how the technology was used in this cancer model.
- Citation: Lu JW, Ho YJ, Yang YJ, Liao HA, Ciou SC, Lin LI, Ou DL. Zebrafish as a disease model for studying human hepatocellular carcinoma. World J Gastroenterol 2015; 21(42): 12042-12058
- URL: https://www.wjgnet.com/1007-9327/full/v21/i42/12042.htm
- DOI: https://dx.doi.org/10.3748/wjg.v21.i42.12042
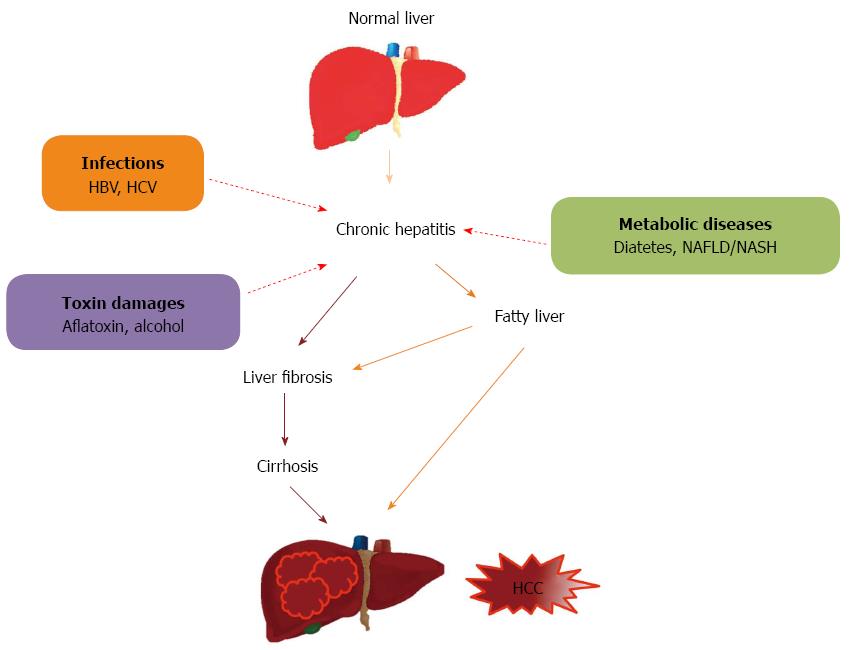
Liver cancer is one of the world’s most common cancers and the second leading cause of cancer deaths, with nearly 745000 deaths recorded in 2012[1]. The incidence of liver cancer is higher among men than women[2]. Hepatocytes are the main cells to constitute 70%-85% of the liver mass and are responsible for the metabolism of carbohydrates, amino acids, lipids, and chemical compounds as well as for the maintenance of the physiological environment[3-5]. Hepatocellular carcinoma (HCC), a primary hepatic cancer, accounts for 90%-95% of liver cancer cases. The pathogenesis of HCC consists of a stepwise process of liver damage that extends over decades, due to hepatitis, fatty liver, fibrosis, and cirrhosis before developing fully into HCC. Chronic liver damage induces genetic alterations of the hepatocytes, leading to cell death, cellular proliferation, dysplasia, and neoplasia. Multiple risk factors are highly correlated with HCC, including infection with hepatitis B virus (HBV) or hepatitis C virus (HCV), alcohol abuse, aflatoxin exposure[2,6], and metabolic diseases[7] (Figure 1). These factors play critical roles in regulating multiple oncogenes or tumor suppressor genes and activating tumorigenesis-related pathways.
Persistent viral infections are the critical cause of HCC formation. Statistically, 57% of cirrhosis cases and 78% of HCC cases result from HBV and HCV infection[8]. HBV infection causes chromosome instability or insertional mutagenesis[9]. In particular, the HBV X protein (HBx), a small peptide with a molecular mass of approximately 17 kDa, is vital in the pathogenesis of HCC and becomes a prognostic marker of HBV infection and HCC. HBV infection plays an important role in the development of the tumor microenvironment in HCC by regulating the accumulation and activation of both cellular components, such as immune cells and fibroblasts, and non-cellular components of the microenvironment, such as cytokines and growth factors. HBV thus significantly affects the progress of the disease and prognosis[10]. HBx is able to enhance HBV replication, interfere with host gene transcription, interrupt protein degradation, regulate signaling pathways, and deregulate the cell cycle to manipulate cell death[11]. Numerous studies[12,13] have confirmed that the overexpression of HBx causes HCC.
HCV infection is the main risk factor for HCC in developed countries, accounting for approximately one-third to half of all cases. HCV infection leads to activation of Notch and Toll-like receptor pathways in cirrhosis, deregulation of the Janus kinase (JAK)/signal transducer and activator of transcription (STAT) pathway in early carcinogenesis, and upregulation of DNA replication/repair genes and the cell cycle in the late cancerous stages[14]. HCV proteins such as the core protein and nonstructural protein 5A interact with host cells to regulate processes such as cell signaling, transcriptional modulation, apoptosis, and endoplasmic reticulum stress[15]. A large number of HCV-infected persons develop chronic HCV infection, which can lead to liver fibrosis, cirrhosis, and HCC[16].
Alcohol is a co-carcinogen and is synergistic with the above risk factors for liver cancer. Cirrhosis is observed to have a high correlation with alcohol-associated HCC. Alcohol activates the JAK/STAT and p38 mitogen-activated protein kinase (MAPK) pathways, which responds by producing cytokines, chemokines, and stress. These changes, in turn, affect cell differentiation and growth[17]. Acetaldehyde, a metabolite of alcohol, is even considered to be a carcinogen as it increases oxidative stress and damages DNA[18]. These effects may induce liver fibrosis and cause cirrhosis and HCC development. However, approximately 5%-30% of HCC patients lack any apparent identifiable risk factors for their cancer. Non-alcoholic fatty liver disease (NAFLD) is the hepatic component of metabolic syndromes such as insulin resistance, obesity, hypertension, and hyperlipidemia; it includes both simple steatosis and non-alcoholic steatohepatitis (NASH)[19]. NAFLD/NASH itself becomes a risk factor for HCC, even in the absence of cirrhosis, because insulin resistance and inflammation are involved in HCC carcinogenesis. Aflatoxin, especially Aflatoxin B1/AFB1, is a genotoxic hepatocarcinogen and a kind of co-carcinogen. AFB1 is metabolized by cytochrome-P450 enzymes to become less harmful metabolites. However, aflatoxin B1-8,9-epoxide (AFBO), the reactive intermediate chemical compound, is a highly reactive genotoxic compound. AFB1 and AFBO both bind to liver cell DNA and form DNA adducts, causing DNA strand breakage, DNA base damage, and oxidative damage[6,20]. AFB1 has been found to accelerate the development of HCC initiated by other risk factors.
The zebrafish has become a model organism exploited in life science fields including embryonic development, toxicity, cancer research, human diseases, and drug screening[21,22]. The genome of the zebrafish is comprised of 25 chromosomes, which contain the full set of genes homologous to other vertebrates. After the current zebrafish genome was fully sequenced, approximately 70% of its orthologous genes were found to be associated with human disease[23,24]. Zebrafish have the following advantages and disadvantages: a short life cycle, low maintenance costs, small space requirements for maintenance, a large number of offspring, immune system deficiencies in early zebrafish embryos, transparency and transgenic lines, lower numbers of cells required for xenotransplantation per animal, availability for high-throughput drug screening, small organs and blood vessels, low body temperature, and a lack of organs such as lungs, among others. Compared to the mouse model, zebrafish are inexpensive and can be easily used to rapidly create a transgenic animal model. Transgenes can be controlled by ubiquitous, inducible, or tissue-specific promoters. Furthermore, transparent zebrafish carry fluorescent proteins that allow the visualization of specific cells in real time. Such capabilities enable investigators to observe and trace specific cells and to produce a spatiotemporal analysis of gene expression. Therefore, the zebrafish is a suitable option for monitoring transgenic tumors from initiation, progression, and metastasis to transplantation. In addition, the zebrafish model can be used for large-scale genetic and high-throughput screening[25,26]. These attributes make the zebrafish a more flexible option among animal models amenable to liver disease studies.
The genes and pathways involved in hepatogenesis and liver cancer are largely conserved between zebrafish and humans[27]. Hepatocytes possess similar functions in zebrafish and mammals and demonstrate similar genesis for shared histopathological characteristics such as steatosis, cholestasis, and neoplasia[28]. Expression of HCV core protein in transgenic zebrafish treated with thioacetamide (TAA) was the first application of zebrafish in HCC studies.
Pathological features observed in this transgenic zebrafish model include steatohepatitis, fibrosis, cirrhosis and HCC. Progression to HCC is reduced to six weeks relative to TAA-treated wild type zebrafish and becomes a powerful preclinical platform for studying the mechanism of hepatocarcinogenesis in evaluating therapeutic strategies for HCC[29]. Today, genome editing technologies are rapidly advancing. Zinc-finger nucleases (ZFNs), transcription activator-like effector nucleases (TALENs), and clustered regularly interspaced short palindromic repeat (CRISPR)/CRISPR-associated (Cas) systems have been developed to rapidly induce targeted genetic modifications[30]. Such technologies promote the generation of transgenic animal models. This review focuses on the zebrafish model for HCC. We summarize liver development and the anatomy of the zebrafish. Subsequently, expression systems and genome editing technologies are presented to examine the current status of transgenic zebrafish development. Finally, the zebrafish models for liver disease and HCC are introduced for a better understanding of recent findings regarding mechanisms, drug screening, and drug-induced toxic liver injury.
The liver is a critical organ for vertebrates. Hepatocytes, the cell type which constitutes the majority of the liver, play a major role diverse biological functions, including digestion and metabolism through the regulation of many essential nutrients, the storage of vitamins, the decomposition of red blood cells, the synthesis of plasma proteins such as prothrombin, fibrinogen, and albumins, the production of hormones, and detoxification in mammals[31,32].
The zebrafish is effective as an animal model for studying liver development because of its experimental advantages, as has been demonstrated in numerous publications. However, some characteristics of the zebrafish liver differ from other vertebrates and mammals. For example, hepatocytes are not noticeably organized in cords or lobules, and the typical portal triads are not obvious in the zebrafish liver. The portal veins, hepatic arteries, and large biliary ducts of zebrafish are spread randomly within the hepatic parenchyma and are not grouped into portal tracts as in the mammalian system. Moreover, the hepatocytes are arranged as tubules that surround small bile ducts rather than as bilayered hepatocyte plates as in the mammalian system. The intrahepatic bile ducts are derived from the bile canaliculi. The bile ducts fuse and ultimately form the gallbladder. The bile is collected in the gallbladder via large ducts and an extrahepatic biliary system. Moreover, there are no Kupffer cells in the zebrafish liver[33,34]. The liver of zebrafish contains three lobes, one ventral and two lateral, which lie along the intestinal tract. The liver of teleosts is similar to the mammalian liver and plays a central role in metabolic homeostasis, including the processing of carbohydrates, proteins, lipids, and vitamins. In addition, it also plays an important role in detoxification and the synthesis of serum proteins, including albumin, fibrinogen, complement factors, and acute-phase proteins[34].
Similar to the process in the mammalian liver, hepatogenesis occurs in three major phases in zebrafish: hepatoblast specification, budding/differentiation, and hepatic outgrowth, accompanied by morphogenesis[28,35,36]. Cells in the anterior endodermal rod develop into hepatoblasts at 22 h post-fertilization (hpf) through the expression of hhex and prox1 during the hepatoblast specification phase. Hepatoblasts are located on the left side of the anterior gut tube, and the liver bud begins to form between 26 and 28 hpf. Some marker genes, such as ceruloplasmin (cp) and transferrin, are expressed in the liver bud at 32 hpf, with the clear emergence of the liver primordium at 48 hpf during the differentiation phase. The liver bud leaves the intestine at approximately 50 hpf. Due to proliferative acceleration, hepatic outgrowth begins between 60 and 72 hpf and continues until the liver attains its apposite size, and a rapid growth phase of the liver begins at 80-84 hpf[37]. During the end of the outgrowth phase (120 hpf), the liver relocates from the left side to the right side[28].
Signaling molecules and transcription factors are conserved in hepatogenesis between mammals and zebrafish. These pathways also regulate early liver development in zebrafish, though there are some differences. FGF, BMP, and WNT signaling pathways are crucial for hepatogenesis[38,39]. FGF signaling is critical for hepatic specification in zebrafish and mice. Overexpression of a dominant negative FGF-receptor in zebrafish embryos between 18 and 26 hpf decreases the later expression of hhex, prox1, gata4, gata6, and cp[40]. A previous study revealed that BMPs are vital for zebrafish hepatic specification: zebrafish mutations such as lost-a-fin or over-expression of a dominant negative BMP receptor led to reduced expression of some hepatic specification genes, such as hhex and prox1[40]. Induction of wnt expression led to a block in liver specification in early somitogenesis and created an enlarged liver after a few hours in zebrafish liver development[41].
Hepatogenesis is a complex process controlled by many transcription factors. The earliest conserved liver-specific transcription factors regulating hepatogenesis, such as hhex and prox1, are initially expressed and play crucial roles in the zebrafish hepatic bud at 24 hpf[40,42-44]. These hepatic nuclear factors also participate in liver development and differentiation in mammalian hepatogenesis[45]. Some transcription factors, including sox17, foxa1, foxa2, foxa3, and gata family members are required for both the generation of endoderm and the liver bud[35,46,47]. Recent research indicates that several genes, such as liver-enriched gene 1 (leg1), play important roles in the outgrowth stage in zebrafish[48]. Such research has also revealed that hypoxia-inducible transcription factors, such as hif2-alpha, directly regulate the hepatic outgrowth phase through binding to the promoter region of leg1 but do not directly regulate the liver specification phase in zebrafish embryos[49].
According to the latest data, there is evidence that epigenetic regulation of gene expression in zebrafish liver development also plays an important role. Histone acetylation (hdac) and DNA methylation (dnmtin) are two major mechanisms regulating gene expression. An analysis of mutations in hdac or dnmtin embryos demonstrated that epigenetic regulation controls both hepatic specification and outgrowth phases in zebrafish liver development. For example, hdac1 mutants develop small livers as a result of hepatic patterning defects[50]. Embryos treated with an hdac inhibitor at 24 hpf have also been shown to develop a small liver due to inhibition of hhex and prox1 gene expression. Furthermore, the knockdown of hdac1 and hdac3 results in multiple defects in embryos. Aberrant hdac3 is more specific for liver development as it regulates zebrafish liver growth by suppressing growth differentiation factor 11, a member of the TGF-β family of growth factors[51]. Ubiquitin-like with PHD and RING finger domains 1 (uhrf1) plays a role in DNA methylation by recruiting DNA methyltransferase 1 (dnmt1) to hemimethylated DNA. The uhrf1 mutants have defects in zebrafish hepatic outgrowth[52].
Over the past 25 years, the available zebrafish transgenic technology has advanced significantly[53,54]. Transgenesis is an essential technique as in other model organisms. A variety of transgenic expression systems exist for zebrafish, including constitutive and inducible systems. Initial transgenes were plasmid-based with ubiquitous promoters driving the expression of reporter genes and demonstrated that transgenic technology was a viable, reproducible strategy in zebrafish. In recent years, the use of transgenesis in zebrafish has become widespread. Researchers have used a mammalian promoter, promoters from other fish species, and tissue-specific promoters to drive gene expression[55]. In general, the design of most transgenic vectors thus far incorporates a single promoter to control when and where a transgene is expressed. The frequency of the development of germline founders is associated with the method of the introduction of the DNA. Supercoiled[53,56] or linear DNA[54] injection yields 1%-10% germline transgenic founders, while linearized ISce-I[57] meganuclease yield 20%-30%. The rate of transgenesis has recently seen a dramatic increase with the use of transposon-based systems: 30% with Sleeping Beauty[58] and Ac/Ds[59], and 50% with Tol2[60,61]. The Tol2 element is an active transposable element found in Medaka genomes, and subsequent production of some cloning vectors has facilitated the use of this element in zebrafish, allowing the generation of many transgenic fish lines[62]. The Tol2 element transposon can be efficiently excised and integrated into the zebrafish genome using coinjection with Tol2 mRNA and vector plasmid[60]. Cloning vectors from multiple sources, including mini inverted repeat transposons and Tol2 transposase transcription vectors, made use of multisite Gateway cloning vectors[63,64]. In particular, the Tol2-kit was established for the scientific community to allow the use of versatile vectors. Gateway cloning technology is a universal cloning method based on the att site-specific recombination properties of bacteriophage lambda and enables the rapid and highly efficient transfer of DNA sequences into multiple vector systems for protein expression and functional analysis[65]. The online Tol2-kit community (http://tol2kit.genetics.utah.edu/index.php/Main_Page) provides detailed information and has helped to make the Tol2 transposon system a routine genetic engineering tool. Widely useful entry clones were created by combining heat-shock protein 70 (hsp70), CMV/SP6, histone2A-X, β-actin, and upstream activating sequence (UAS) promoters, cytoplasmic, nuclear, membrane-localized fluorescent proteins and Gal4VP16, IRES-driven GFP cassettes, and two Tol2-based destination vectors, one with a Cmlc2/GFP transgenesis marker[64]. One of the most useful GFP transgenic fish lines was derived with a zebrafish liver fatty acid-binding protein (L-FABP) promoter[66,67]. A zebrafish model for hepatocarcinogenesis has been since developed through the expression of oncogenes under the control of the L-FABP promoter. Liver-specific expression of HBx, src, and endothelin 1 (edn1) established with Tol2 methodology triggered hepatocarcinogenesis in zebrafish[68,69].
While previous studies demonstrated the utility of constitutive expression systems, constitutive expression of oncogenes is often found to lead to gross tumor development which can result in embryonic lethality. Inducible systems can avoid these potentials deficiencies in constitutive systems as the duration and dosage of gene expression can be monitored, thus allowing for the spatiotemporal control of oncogene expression. Inducible systems currently being used include Heat-shock, Cre-loxP, GAL4-UAS, Tet-On, Tet-Off, and Mifepristone systems[70] (Table 1). Heat-shock proteins were originally identified in cells after exposure to environmental stress. Induced jumps in temperature have been used to achieve spatiotemporal control of transgene expression in zebrafish embryos. GFP linked to an hsp70 promoter has been used to establish the pattern of gene expression induced by heat shock. At a normal temperature, GFP expression in transgenic embryos was not detectable. However, single embryos heat-shocked by exposure to 38 °C for 30 min exhibited GFP expression in approximately 20%-90% of cells for more than 24 h after heat treatment in a variety of tissues types[71,72].
| Expression systems | Advantages | Disadvantages |
| Constitutive | Well established, commercially available; in vitro and in vivo, successful methodology for expression of transgene | Expression of oncogenes may cause advanced/highly aggressive tumors and early lethality |
| Heat-shock | Expression of transgene can be induced on a single cell level | Adverse effects that may arise from the heat shock |
| Cre-loxP | Well established; commercially available; in vivo, successful methodology for expression of transgene | Not all tissue specific promoters are perfectly specific; leaky gene expression; two plasmid system |
| GAL4/UAS | Well established; in vivo, successful methodology for expression of transgene | In vivo expression of GAL4 can have side effects, probably related to immune and stress responses; two plasmid system |
| Mifepristone | Well established; in vivo, successful methodology for expression of transgene | Opening and closing of the switch is slow (hours to days); cell permeability of the RU-486 can be restricted |
| Tet-on/off-inducible | Well established; commercially available; in vitro and in vivo, successful methodology for expression of transgene | Opening and closing of the switch is slow (hours to days); cell permeability of the doxycycline can be restricted; two plasmid system |
Multiple transgenic lines have been derived in zebrafish through the use of tissue-specific expression of Cre recombinase. Initially, a plasmid-based system was developed for detecting Cre expression in vivo[73]. A neural progenitor-specific (nestin) promoter was used to drive the expression of an mCherry gene, flanked by loxP sites, and upstream of a promoterless EGFP-fused to zebrafish kras-V12 oncogene, resulting in the exclusive expression of mCherry. Once this plasmid was exposed to Cre recombinase, the mCherry gene was excised, and the EGFP gene, fused to the oncogene, was controlled by the nestin promoter[74]. The GAL4-UAS system has also been successfully exploited in zebrafish to misexpress genes in a tissue-specific manner. The GAL4-UAS methodology requires two transgenic lines: the activator zebrafish line which expresses the yeast transcriptional activator GAL4 under the control of a specific promoter, and the effector zebrafish line which possesses the transgene of interest fused to the DNA-binding motif (UAS) of GAL4[75,76]. In 1999, an activator line was developed to express GAL4 under the control of the β-actin promoter. In these experiments, the transgene in the effector line encoded a myc-tagged protein adjacent to the UAS of GAL4[77]. This report demonstrated that the cross of the effector line with an activator line is necessary for gene expression. This strategy was used to develop an HCC model. In this model, walleye dermal sarcoma virus rv-cyclin gene (orf-A) fused to the UAS of GAL4 was expressed in the livers of zebrafish when crossed to animals harboring GAL4 under the control of L-FABP promoter[78].
Chemically inducible expression systems (Tet-On, Tet-Off, and Mifepristone) have also been used in zebrafish[79-82]. The Tet-On and Tet-Off systems are binary transgenic systems in which the expression of a transgene is dependent on the activity of an exogenous inducible transcriptional activator. In both the Tet-On and Tet-Off systems, expression of the transcriptional activator can be regulated both reversibly and quantitatively by exposing the transgenic animals to varying concentrations of tetracycline derivatives, such as doxycycline (Dox). The design of the Tet-On and Tet-Off systems allows tissue-specific promoters to drive the expression of the reverse Tet-controlled transcriptional activator (rtTA) and Tet-controlled transcriptional activator (tTA), resulting in tissue-specific expression of the regulated target transgene[55].
Several HCC models have been developed using such technology. Li et al[80,83] fused the xiphophorus xmark and mouse myc oncogenes to the rtTA responsive element, and placed the rtTA transgene was under the control of the 2.0-kb L-FABP promoter. Liu et al[81] fused the HBV and HCV oncogenes to the tTA responsive element, and placed the tTA transgene under the control of the 2.8-kb L-FABP promoter. In the mifepristone inducible LexPR system, the LexPR chimeric transactivator was fused to a 2.0-kb L-FABP promoter to produce the driving zebrafish line, and the effector zebrafish line contained EGFP-fused to zebrafish kras-V12 oncogene under the control of the LexA-binding site. Expression was induced by exposing animals to varying concentrations of mifepristone (RU-486)[81]. In these studies, dose-dependent, Dox, or mifepristone mediated activation of oncogene expression were detected in the liver of the transgenic zebrafish.
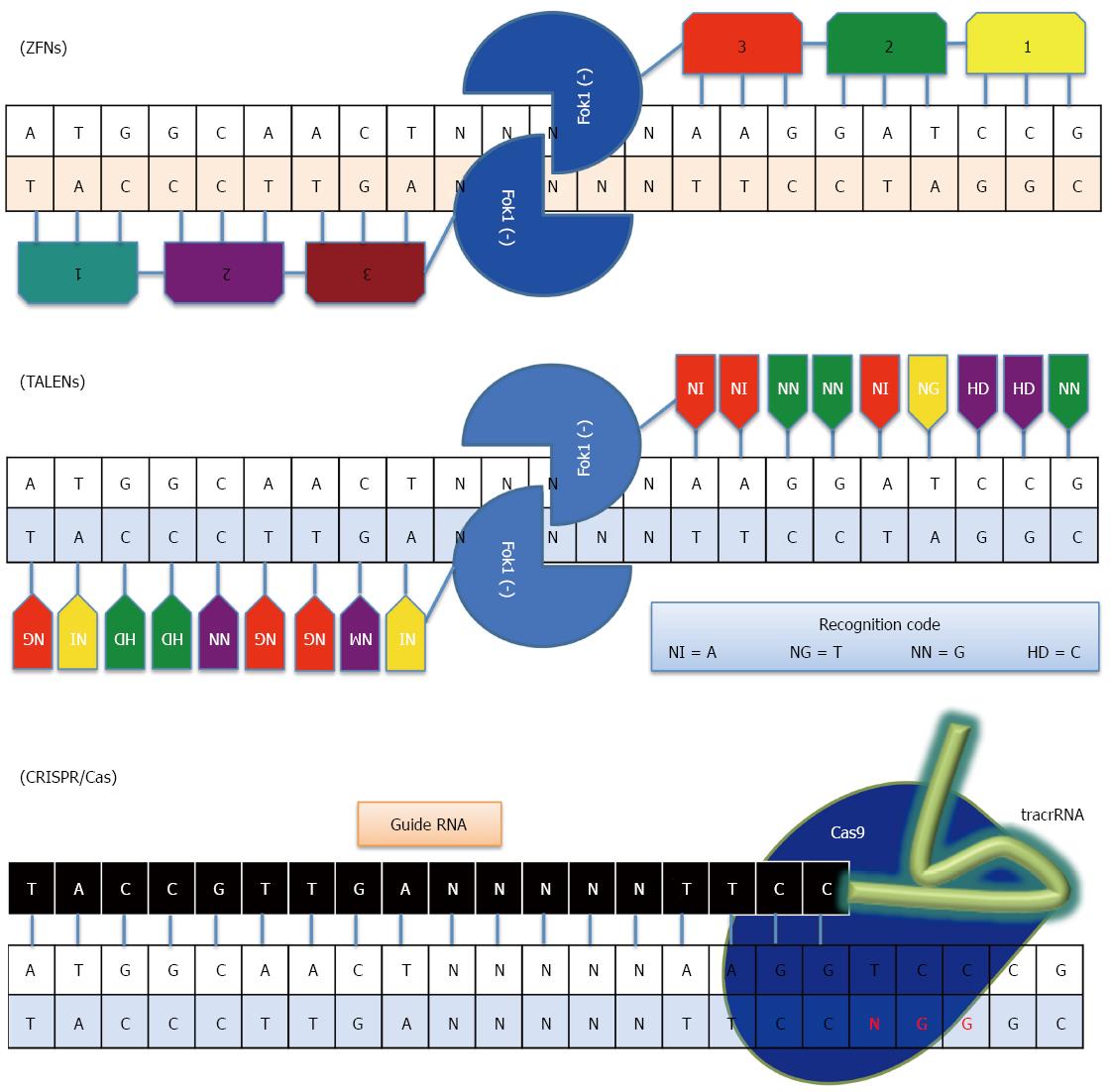
Over the past two decades, genetic engineers have made great strides in developing a reliable technique to examine genotypes. Gene knockdown using small interfering RNAs and microRNAs restore the function of dysfunctional genes, but the main disadvantages are off-target interactions and the temporary nature of inactivation achieved through these methods. Today, ZFNs, TALENs, and CRISPR/Cas have become well-established genome editing tools for customizing genomes in human, animal, and plant cells[83-85]. The characteristics and gene editing capabilities in complex genomes of ZFNs, TALENs, and CRISPR/Cas systems are summarized in Table 2 and Figure 2. RNA-programmable DNA nucleases have been adapted as a precise genetic scissors for correcting and editing genetic defects[86]. Site-specific nucleases induce DNA double strand breaks (DSBs) that stimulate non-homology end joining (NHEJ) and homology-directed repair (HDR) for targeted genomic loci[2].
| Nucleases | ZFN | TALEN | CRISPR/Cas |
| DNA binding domain | Multiple zinc finger peptides | Transcription-activator like effectors | CRISPR-derived RNA/Single-guide RNA |
| Endonuclease | Fok1 | Fok1 | Cas9 |
| Binding specificity of each repeat | 3 bp | 2 bp | 1 bp |
| Target site length | 18 to 36 bp | 30 to 40 bp | 23 bp |
| Off-target | High probability | Low probability | Variable |
| Libraries generation | No | Feasible, depend on technology | Yes, cloning 20 bp, oligos targeting each gene into a plasmid |
As one of the numerous DNA-binding motifs in eukaryotic genomes with the ability to recognize any sequence[87,88], ZFNs are being widely applied to anything in biological research, from the design of animal models to human gene therapies[89]. A ZFN is composed of two domains: a site-specific DNA-binding domain, which is derived from a zinc finger containing transcription factor, and a bacterial Fok1 restriction enzyme endonuclease domain. The zinc finger protein recognizes a 3-bp sequence of DNA on the major groove, with its tandem repeats potentially attaching to a stretch of nucleotides between 9 and 18 bp long[90].
To perform site-specific cleavage of DNA, two ZFN monomers are necessary for the process; one monomer recognizes the binding site on the forward strand while the other recognizes it on the reverse strand. The ZFN binding on both strands enables higher specificity targeting and dimerization of Fok1 in an adequate space[91], so that the pair of Fok1 nuclease domains can cleave the DNA generating a DSB. Cells then utilize either NHEJ or HDR to repair DSBs. The manner in which NHEJ introduces frameshifts into the coding region to knock out a gene, achieved for example through nonsense-mediated mRNA transcript disintegration, is not especially efficient. HDR, however, is used to generate a specific mutation by means of a repair template containing the desired mutation-paired oligonucleotide[92].
Zinc finger proteins with diverse binding specificities are designed using several methods. Modular assembly, which involves a preselected library comprising zinc finger domains for the recognition of 64 nucleotide triplets, is one way of generating customized zinc finger domains[93]. To identify the perfect combination, oligomerized pool engineering utilizes a zinc finger array, and through bacterial-based selection, identifies proteins that bind efficiently to the target site[94]. Other strategies also apply zinc finger modular assembly based on context-dependent DNA to produce ZFNs with endonuclease (endogenous) activities[95]. Although ZNFs offer convenience and are widely utilized, they still possess a high off-target effect[96], which may be improved by developing a heterodimer composed of ZFNs with different Fok1 domains to cleave target DNA[97-99].
TALENs contain a DNA-binding domain and a Fok1 catalytic domain, just like ZFNs, for genomic engineering. A DNA-binding domain is constructed with an N-terminal segment, a central repeat domain, and a half repeat. The central repeat domain is comprised of several monomers that are called transcription activator-like effectors (TALEs). TALEs are effector proteins that are secreted from the bacteria of the Xanthomonas genus. They were first found in plant cells, enhancing their susceptibility to pathogens[100]. TALEs are tandem repeats of a 34-amino-acid domain[101], and positions 12 and 13 are known as repeat-variable di-residue (RVD) domains used to determine the specificity of the TALEs. There are four RVD domains, NN, NI, HD, and NG, for the recognition of guanine, adenine, cytosine, and thymidine, respectively[102]. TALEs function as eukaryotic transcription factors via DNA binding to activate target gene expression. Fok1 is located in the C-terminal segment and generates a DSB in a spacer sequence. TALENs therefore can be used for targeted gene disruption[103]. It is challenging to construct TALE repeats because each TALE repeat unit has high similarity. Specific methods, such as the restriction enzyme and ligation method[104], Golden Gate cloning[105], and fast ligation-based automated solid-phase high-throughput system[106] have all been designed for the rapid assembly of specific TALENs, so that custom-designed TALENs are in fact a realistic possibility for genetic engineering.
CRISPR/Cas is a prokaryotic defense system against invasion of foreign DNA, utilizing an RNA-guided DNA cleavage system. Small fragments (protospacers) of foreign DNA are inserted at repeat sequences in their own genomes to form CRISPR[107]. The type II system consists of a trans-activating crRNA (tracrRNA) in addition to the primary CRISPR RNA transcript (pre-crRNA) transcribed from the protospacers, which is subsequently processed into short crRNAs[108]. To achieve direct sequence-specific DNA recognition and cleavage, CRISPR-associated protein 9 (Cas9) must be complexed with both the crRNA and the tracrRNA, with the crRNA providing the sequence required for target recognition through Cas9. The essential targeting component (5’-NGG-3’ protospacer adjacent motif sequence) is located upstream of the crRNA, which is recognized through the Cas9. Through this mechanism, CRISPR/Cas systems cleave the target DNA sequence of 23 bp. Compared to ZFNs and TALENs, the generation of a CRISPR/Cas target specific endonuclease is much easier with the methods of cloning and transcription[109]. Recently, a CRISPR/Cas9 construct was established for tissue-specific gene disruption in zebrafish, and this vector system may become a unique tool to spatially control targeted somatic mutations, gene knockout and loss of function studies in zebrafish[110].
The most studied oncogene associated with the development of HCC is the HBx antigen from HBV. HBx has been shown to induce HCC in mice and enhance colony formation in HCC cell lines[111-113]. Transgenic mouse models indicate that HCV is directly pathogenic and oncogenic[114,115]. AFB1 is one of the most prominent carcinogens associated with HCC[116], and it is known to induce formation of DNA adducts and p53 mutations in liver cell lines[117]. Mutational inactivation of p53 has been described as one of the key molecular mechanisms involved in the pathogenesis of HCC[118]. AFB1 is synergistic with other factors as AFB1 treatment induced significantly more liver tumors in HBx and HCV transgenic mice than in wild-type mice[114,115].
Models for liver disease and HCC have been generated in zebrafish through the tissue specific expression of such oncogenes regulated by the L-FABP promoter. In zebrafish, HBx overexpression causes hepatic fat accumulation and liver degeneration in a wild-type background[119]. Tumorigenesis however requires inactivation of the p53 tumor suppressor pathway, either through mutation of the gene itself or aberrant expression of a negative regulator, such as murine double minute 2 (mdm2) protein. Overexpression of mdm2 alone in the zebrafish liver leads to growth retardation and a fragile liver[120]. Another oncogene affecting the p53 pathways is gankyrin. This protein binds ubiquitin protein ligase mdm2 which promotes p53 degradation. The inhibition of p53 function through any of these mechanisms prevents the activation of p53-dependent apoptotic genes, which leads to cell survival, genomic instability, and oncogenic transformation[121]. Overexpression of gankyrin was found to induce hepatic steatosis and regulated miR-16, miR-27b, miR-122, and miR-126. The protein has also been shown to be involved in lipid metabolism[122].
UHRF1 is an important regulator of DNA methylation that is highly expressed in many cancers. UHRF1 overexpression destabilizes and delocalizes dnmt1, causing DNA hypomethylation, p53-mediated senescence, and hepatocarcinogenesis in zebrafish[123]. Cyclins are involved in tumor formation and cell death. rv-cyclin may also play a role in walleye dermal sarcoma tumor regression by inducing apoptosis[124,125]. Liver-specific expression of walleye dermal sarcoma virus rv-cyclin (orf-A) in zebrafish protects the fish liver from damage with treatment of 7,12-Dimethylbenz[a]anthracene and delays the onset of malignancy[78].
Edn1 has been identified as a gene that is significantly up-regulated in HBx-induced HCC in the mouse model[126]. Liver-specific induced expression of edn1 caused steatosis, bile duct dilation, hyperplasia, and HCC in zebrafish[68]. Expression of the transcription factor Yin Yang 1 (YY1) was also significantly up-regulated by HBV in a concentration-dependent manner[127]. A previous study has demonstrated through chromatin immunoprecipitation that HBx interacts with YY1[128]. CCAAT/enhancer-binding protein alpha which controls differentiation of hepatocytes was found to be a direct target down-regulated by YY1[129]. Overexpression of YY1 promoted zebrafish liver steatosis and lipotoxicity by inhibiting C/EBP homologous protein 10 expression[130].
Excessive food intake and increased weight gain to the point of obesity is one of the causes of steatosis. Activation of cannabinoid receptor 1 (CB1R) is a molecular mechanism underlying the regulation of food intake, weight gain, and obesity in mammals. Tet-Off conditional expression of the zebrafish CB1R ortholog gene promoted hepatic lipid accumulation and lipotoxicity through the induction of srebp-1c expression in zebrafish[131]. In vertebrates, apoptosis is a fundamental part of normal embryonic development and participates in sculpting organs and regulating cell populations. zfBLP1 and zfMcl-1a are functionally similar to members of the Bcl-2 family, which inhibit apoptosis. Overexpression of zfBLP1 or zfMcl-1a in zebrafish larval liver induced hyperplasia[132].
Combined treatment of zebrafish with HBx and AFB1 induced hepatitis, steatosis, and liver hyperplasia during the early stages of hepatocarcinogenesis[133]. HBx and src overexpression induced HCC in p53 mutant zebrafish and revealed a role for src in HCC progression[69]. TAA enhanced the development of steatohepatitis, cirrhosis, and HCC induced by the expression of the HCV core protein in transgenic zebrafish[29]. In vitro, the HCV core protein has been shown to directly activate the RAS-RAF-MEK-ERK pathway[134]. In human HCC, Ras proto-oncogenes are activated in as many as 50% of all HCC cases, which leads to activation of downstream signaling pathways including RAF-MEK-ERK and PI3K-AKT-mTOR. Approximately 7% of HCCs carry activating mutations in the K-RAS oncogene, which is higher than the percentage of cases carrying H-RAS and N-RAS mutations. A high level of kras-V12 expression induced through constitutive or inducible mechanisms initiated liver tumorigenesis in zebrafish[81,135]. The co-expression of HBx and the HCV core protein trigger intrahepatic cholangiocarcinoma in transgenic zebrafish[80]. However, transgenic zebrafish overexpressing HBx or HCV individually do not develop HCC.
Recently, expression of kras-GV12 and xmrk, the homolog of mammalian epidermal growth factor receptor oncogene, in zebrafish with Tet-On conditional methodology has been reported as an outstanding model for revealing new therapeutic targets involved in oncogene-regulated hepatocarcinogenesis[79,136]. RNA sequencing analysis of an xmrk transgenic HCC model revealed a potential role for immune responses in HCC progression and regression. This model may provide molecular insight into the targeted inhibition and significance of immune response in tumor regression[137].
The liver is one of the most important organs for the study of autophagy[138]. In fact, liver tumors are one of the main phenotypes in knockout mice of autophagy-related genes[139]. In zebrafish, the EGFP-Lc3 transgenic line crossed with the xmrk transgenic line yielded animals susceptible to HCC and thus, demonstrated that autophagy plays an important role in HCC development[140]. Cross-species analyses demonstrated that Tet-On conditional expression of myc in a zebrafish model paralleled findings in myc mouse models for HCC. Elevated myc expression in zebrafish caused liver hyperplasia, adenoma, and HCC. Myc-induced liver tumors in zebrafish also possessed molecular signatures that were similar to those from mouse and human HCC. This zebrafish model thus revealed a conserved role for myc in promoting hepatocarcinogenesis in all vertebrate species[82]. RNA expression profiling of liver tumors from the three different zebrafish models, xmrk, kras-G12V, and myc, showed however relatively little overlap in significantly deregulated genes and biological pathways. However, these three transgenic tumor signatures were found to be significantly correlated with advanced or late stage human HCC[141].
In human HCC, deregulation of MYC is frequently detected and correlated with poor prognosis. Two differentially expressed MYC orthologs exist in the zebrafish genome: myca and mycb. Overexpression of myca and mycb in the liver using a mifepristone-inducible system demonstrated that both myc genes were oncogenic. myca overexpression accelerated tumor progression and reduced apoptosis in p53 mutant zebrafish. Malignant hepatocytes were dependent on sustained myca expression; withdrawal of the mifepristone inducer resulted in a rapid regression of HCC, with liver tumor regression occurring even in a p53 mutant background[142].
RhoA is a member of the RHO small GTPase family, which is highly homologous to the RAS. These proteins are also involved in the regulation of cell cycle dynamics, and are key molecules for cell growth and tissue development of the switch. Expression levels and the overall activity of RhoA has been found to be elevated in HCC[143]. Tet-On conditional expression of kras-G12V, rhoA, constitutively active rhoA-G14V, dominant-negative rhoA-T19N, or kras-G12V plus one of the three rhoA genes, was also examined in zebrafish. Overexpression of kras-G12V during early development led to liver enlargement and hepatocyte proliferation. The increase in liver size was augmented by the dominant-negative rhoA-T19N, but abrogated by the constitutively active rhoA-G14V. This study revealed the existence of signaling crosstalk between kras-V12 and rhoA in regulating liver overgrowth and hepatocarcinogenesis[136]. Based on these results, the zebrafish emerges as a model system for elucidating the mechanisms of hepatocarcinogenesis and for screening drugs to inhibit the oncogenic effects of specific genes (Table 3).
| Transgene name | Expression system | Liver pathology | Ref. |
| cnr1 (Zebrafish) | Tet-off-inducible | Steatosis | [132] |
| edn1 (Zebrafish) | Constitutive | Steatosis, bile duct dilation, hyperplasia and HCC | [69] |
| gankyrin (Zebrafish) | Constitutive | Atrophy, hypoplasia and steatosis | [123] |
| HBx (Human) | Constitutive | Hypoplasia and steatosis | [120] |
| HBx + AFB1 (Human) | Constitutive | Hepatitis, steatosis and hyperplasia | [134] |
| HBx + HCV (Human) | Tet-off-inducible | Intrahepatic cholangiocarcinoma | [81] |
| HBx + p53M214 (Human) | Constitutive | Chronic inflammation, steatosis, bile duct dilation, dysplasia and HCC | [70] |
| HBx + src (Human/Zebrafish) | Constitutive | Chronic inflammation, steatosis, bile duct dilation, dysplasia and HCC | [70] |
| HCV (Human) | Constitutive | Steatosis | [29] |
| HCV + TAA (Human) | Constitutive | Steatosis and HCC | [29] |
| kras-G12V (Zebrafish) | Mifepristone | Hyperplasia and HCC | [82] |
| kras-G12V (Zebrafish) | Constitutive | Hyperplasia and hepatocellular adenoma | [82] |
| kras-G12V (Zebrafish) | Tet-on-inducible | Hyperplasia, hepatocellular adenoma and HCC | [137] |
| kras-G12V + p53M214 (Zebrafish) | Constitutive | Hyperplasia and hepatocellular adenoma | [82] |
| kras-G12V + RhoA (Zebrafish) | Tet-on-inducible | Hyperplasia, hepatocellular adenoma and HCC | [137] |
| kras-G12V + RhoAG14V (Zebrafish) | Tet-on-inducible | Hyperplasia, hepatocellular adenoma and HCC | [137] |
| kras-G12V + RhoAT19N (Zebrafish) | Tet-on-inducible | HCC | [137] |
| Lc3 (Rat) | Constitutive | Investigation of liver autophagy | [141] |
| mdm2 (Zebrafish) | Constitutive | Atrophy, contraction and hypoplasia | [121] |
| MYC (Mouse) | Tet-on-inducible | Hyperplasia and hepatocellular adenoma | [83] |
| myca (Zebrafish) | Mifepristone | Small, typical, hypervascular and ascites of liver tumor | [143] |
| myca + p53M214 (Zebrafish) | Mifepristone | Small, typical, hypervascular and ascites of liver tumor | [143] |
| mycb (Zebrafish) | Mifepristone | Small, typical, hypervascular and ascites of liver tumor | [143] |
| orf A (Human) | GAL4/UAS | Delayed onset of liver tumor | [79] |
| src (Zebrafish) | Constitutive | Chronic inflammation, steatosis, bile duct dilation, hyperplasia, dysplasia and HCC | [70] |
| src + p53M214 (Zebrafish) | Constitutive | Steatosis, hyperplasia, dysplasia and HCC | [70] |
| UHRF1 (Human) | Constitutive | Atypical cells, dysplastic foci and HCC | [124] |
| UHRF1 + p53M214 (Human) | Constitutive | Atypical cells, dysplastic foci and HCC | [124] |
| xmrk (Xiphophorus) | Tet-on-inducible | Hyperplasia, hepatocellular adenoma and HCC | [80] |
| yy1 (Zebrafish) | Constitutive | Steatosis | [131] |
| zfBLP1 (Zebrafish) | Constitutive | Hyperplasia | [133] |
| zfMcl-1α (Zebrafish) | Constitutive | Hyperplasia | [133] |
The United States Food and Drug Administration approves only a few new chemical entities for clinical usage each year because the investigation of new drugs is a lengthy and costly process. Drug-discovery generally proceeds first through in vitro assays, where cell proliferation, cytotoxicity, marker expression, motility, activation of specific signaling pathways, and changes in morphology are examined in response to treatment with small molecules[144], and second through in vivo screening where endpoints such as extended life span can be evaluated. The zebrafish has the advantage of combining both processes in a single model. It is a high-throughput and in vivo model simultaneously; therefore, the zebrafish might improve the success rate in the later stages of preclinical drug development while reducing the cost and the time necessary for the screening process[70].
The trend of using zebrafish embryos in screening for anti-cancer drugs continues to rise. The use of computational drug design and screening of zebrafish embryos has successfully uncovered a novel lead compound that displays selective inhibitory effects on CDK2 activity, cancer cell proliferation, and tumor progression in vivo[145].
Zebrafish/tumor xenograft models have been used to study angiogenesis, invasion, and metastasis. One advantage of zebrafish is that the embryos are transparent, allowing the observation of labeled tumor cells and the evaluation of response to candidate molecules in a high-throughput format in vivo[146]. In order to achieve maximum transparency, zebrafish embryos are incubated in an egg medium with 0.3% phenylthiourea to prevent the formation of pigments. (In the mouse system, the spatial resolution is limited in vivo due to normal opacification of the skin and subdermal structures). Tumor cells labeled with CM-Dil, a lipophilic fluorescent tracking dye, are injected into the perivitelline space or yolk of embryos at 48 hpf and are followed thereafter. fli1:gfp transgenic embryos and the whole-mount akaline phosphatase vessel staining assay allows for rapid and relatively easy investigation of tumor angiogenesis, cell dissemination, invasion, metastasis, and anti-vascular endothelial growth factor (VEGF) drugs for cancer therapy[68,147]. Transgenic zebrafish (vegfr2:grcfp) where GFP expression is restricted to blood vessels have been used to screen a compound library for antiangiogenic compounds. SU4312 and AG1478, two known anti-angiogenic compounds, were used as positive controls in the screen. Two new compounds with no previously described antiangiogenic activity, indirubin-3’-monoxime (IRO) and EM011 (9-bromonoscapine), were also identified[148,149]. Embryos of the transgenic flk:gfp zebrafish were also used in screening the compound library. One lead compound, rosuvastatin, was identified which could inhibit the growth of the zebrafish intersegmental vessels[150]. The zebrafish tumor xenograft model represents a new tool for investigating the neovascularization process and is exploitable for drug discovery as well as gene targeting in tumor angiogenesis.
In zebrafish HCC models, mifepristone-induced kras-V12 transgenic larvae treated with MEK1/2 inhibitor PD98059 resulted in the inhibition of hyperplastic liver growth in 49% of cases. Inhibition of PI3K-AKT-mTOR signaling by LY294002 or rapamycin restored the normal liver phenotype in 57% and 69% of kras-V12 transgenic larvae, respectively. Results furthermore demonstrated that blocking two pathways in kras-V12 transgenic larvae resulted in a more significant anti-tumor effect (78%-96%)[81]. Recently, liver tumors were induced in doxycycline regulated xmrk transgenic fish with 100% penetration in both juveniles and adults. Overexpression of xmrk activated downstream targets of MEK1/2 and STAT5, which led to increased cell proliferation during tumor progression and enhanced apoptosis during tumor regression. Juvenile fish were also exposed to MEK1/2 inhibitor PD98059 or STAT5 inhibitor nicotinohydrazide in combination with doxycycline. After three weeks of treatment, abdomens and livers in 100% of transgenic fish exposed to either inhibitor were reduced relative to untreated transgenics[79]. Transient expression of the HCV core protein under the control of a CMV promoter, human hepatic lipase promoter, and zebrafish L-FABP enhancer in zebrafish embryos was used as a possible model to examine HCV replication and treatment with drugs. The amplified sub-replicon was evidence of high expression of HCV core RNA and protein. This model was used to evaluate efficacy of four HCV clinical drugs: oxymatrine, ribavirin, IFNa-2b, and vitamin B12. Vitamin B12 inhibited HCV core mRNA and protein levels in a dose-dependent manner. Ribavirin and oxymatrine drugs also significantly inhibited replication of the HCV sub-replicon. Such models may provide a novel strategy for studying mechanisms of HCV replication as well as facilitate the discovery of new anti-HCV drugs[151-153].
Drug-induced liver injury (DILI) is a major problem in clinical pharmacology. Here, zebrafish is also promising as an animal model[25]. Zebrafish is a high-throughput in vivo model that can be potentially used to predict which therapeutic compounds will cause DILI in humans as well as present new markers and molecular mediators of DILI. One of the most important features of the model is that drug metabolization in zebrafish is mediated through similar pathways utilized in humans[154]. Different methods have been used in order to evaluate and quantify DILI in zebrafish. Although higher vertebrate organisms that are physiologically similar to humans have typically been used to assess DILI, the zebrafish has similar molecular and cellular processes that accurately simulate human physiology. Therefore, zebrafish provide a significant advantage for research purposes compared to higher vertebrate organisms (e.g., mice and rats). For example, the ability to assess liver damage with visually evaluable phenotypic endpoints enables the transparent larval zebrafish to be used in high-throughput screening[155,156]. In addition, DILI in embryonic or adult zebrafish exhibits histological changes, such as steatosis, apoptosis, and necrosis, that parallel human liver pathologies[157]. TAA has been shown to induce steatohepatitis in zebrafish, which is accompanied by the accumulation of fatty droplets and apoptosis[158]. AFB1 induced hepatitis and steatosis in zebrafish[133]. Zebrafish exposed to ethanol also exhibited histological changes such as steatosis, as found in alcoholic liver disease in humans[159]. Serum biochemical values, such as total bilirubin concentration and serum alanine transaminase (ALT) activity, have been determined in zebrafish[160]. Such values can be therefore used to evaluate liver function in response to drug treatment. ALT activity was found to be increased in zebrafish treated with paracetamol in a dose and time dependent fashion[157]. Furthermore, the circulating concentration of miR-122, a new experimental biomarker for liver toxicity, was increased in fish with paracetamol-induced liver injury[161].
Although many studies clearly illustrate the potential advantages of zebrafish as a model for liver toxicity, a number of challenges still exist. For example, zebrafish are exposed to a drug simply by introducing it into the water[162]. Immersion in the drug enables easy and fast administration, but the amount actually consumed by the fish is a variable even though the concentration is known and equal for all fish[163]. To overcome the problem of absorption, the quantity of the drug taken up by the fish can be determined by using a radio-labeled compound and liquid scintillation counting[154].
Before the zebrafish model can be more broadly applied, translatability of the model to humans must be confirmed. First, tests need to be conducted on established human hepatotoxic and nonhepatotoxic compounds, comparing dose responses between fish and humans. Second, translational biomarkers that bridge the gap between fish and humans must also be developed. Finally, immunological response in zebrafish must be evaluated in order to establish whether DILI develops similarly as in humans. The use of zebrafish as a model for liver injury shows promise and may enable better decision making in the early stages of drug discovery, before a compound is tested in higher mammals.
HCC is a primary malignant tumor of the liver. It is a complex disease that is accompanied by an overall poor prognosis. Although numerous oncogenes, tumor suppressor genes, and point mutations have associated with development of the disease over the past several decades, treatment options remain limited. One of the more intriguing approaches to the study of HCC and potential treatments, has been through the development of HCC disease models in zebrafish. Several zebrafish HCC models have been established through expression of various transgenes, including HBx, HCV, myc, kras-G12V, rhoA, xmrk, src, edn1, myca, mycb, or UHRF1. Zebrafish models have also been used for evaluation of DILI and tumor xenotransplantation. Recently, new genome editing technologies, including ZFNs, TALENs, and CRISPR/Cas systems, have been developed to facilitate targeted gene disruption in zebrafish. Together with transgenic technology, several inducible expression systems are also available for zebrafish, which will help to accelerate further development of fish models for HCC. Although establishment of liver disease and HCC models in zebrafish has led to further understanding of the molecular mechanisms and biology of these diseases, zebrafish perhaps more importantly serve as in vivo models with high throughput screening capabilities for the discovery of novel therapeutic agents. Novel inhibitors of angiogenesis, IRO and EM011, have been identified through such screening technology. As the utility of zebrafish for the study of HCC becomes more universally accepted, we will perhaps facilitate drug discovery and thus one day advance our treatment and the prognosis of HCC patients.
P- Reviewer: Chintana PY, Wang DS S- Editor: Yu J L- Editor: A E- Editor: Ma S
| 1. | Stewart BW, Wild CP, editors . World cancer report 2014. Lyon: IARC Press 2014; . [Cited in This Article: ] |
| 2. | Bosch FX, Ribes J, Díaz M, Cléries R. Primary liver cancer: worldwide incidence and trends. Gastroenterology. 2004;127:S5-S16. [PubMed] [Cited in This Article: ] |
| 3. | Postic C, Dentin R, Girard J. Role of the liver in the control of carbohydrate and lipid homeostasis. Diabetes Metab. 2004;30:398-408. [PubMed] [Cited in This Article: ] |
| 4. | Hewitt NJ, Lechón MJ, Houston JB, Hallifax D, Brown HS, Maurel P, Kenna JG, Gustavsson L, Lohmann C, Skonberg C. Primary hepatocytes: current understanding of the regulation of metabolic enzymes and transporter proteins, and pharmaceutical practice for the use of hepatocytes in metabolism, enzyme induction, transporter, clearance, and hepatotoxicity studies. Drug Metab Rev. 2007;39:159-234. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 568] [Cited by in F6Publishing: 523] [Article Influence: 30.8] [Reference Citation Analysis (0)] |
| 5. | Häussinger D, Lamers WH, Moorman AF. Hepatocyte heterogeneity in the metabolism of amino acids and ammonia. Enzyme. 1992;46:72-93. [PubMed] [Cited in This Article: ] |
| 6. | Liu Y, Wu F. Global burden of aflatoxin-induced hepatocellular carcinoma: a risk assessment. Environ Health Perspect. 2010;118:818-824. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 698] [Cited by in F6Publishing: 623] [Article Influence: 44.5] [Reference Citation Analysis (0)] |
| 7. | Baffy G, Brunt EM, Caldwell SH. Hepatocellular carcinoma in non-alcoholic fatty liver disease: an emerging menace. J Hepatol. 2012;56:1384-1391. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 607] [Cited by in F6Publishing: 608] [Article Influence: 50.7] [Reference Citation Analysis (0)] |
| 8. | Perz JF, Armstrong GL, Farrington LA, Hutin YJ, Bell BP. The contributions of hepatitis B virus and hepatitis C virus infections to cirrhosis and primary liver cancer worldwide. J Hepatol. 2006;45:529-538. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 1764] [Cited by in F6Publishing: 1760] [Article Influence: 97.8] [Reference Citation Analysis (0)] |
| 9. | Laurent-Puig P, Zucman-Rossi J. Genetics of hepatocellular tumors. Oncogene. 2006;25:3778-3786. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 252] [Cited by in F6Publishing: 276] [Article Influence: 15.3] [Reference Citation Analysis (0)] |
| 10. | Yang P, Markowitz GJ, Wang XF. The hepatitis B virus-associated tumor microenvironment in hepatocellular carcinoma. Natl Sci Rev. 2014;1:396-412. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 48] [Cited by in F6Publishing: 64] [Article Influence: 6.4] [Reference Citation Analysis (0)] |
| 11. | Xie N, Chen X, Zhang T, Liu B, Huang C. Using proteomics to identify the HBx interactome in hepatitis B virus: how can this inform the clinic? Expert Rev Proteomics. 2014;11:59-74. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 17] [Cited by in F6Publishing: 17] [Article Influence: 1.5] [Reference Citation Analysis (0)] |
| 12. | Li CH, Xu F, Chow S, Feng L, Yin D, Ng TB, Chen Y. Hepatitis B virus X protein promotes hepatocellular carcinoma transformation through interleukin-6 activation of microRNA-21 expression. Eur J Cancer. 2014;50:2560-2569. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 48] [Cited by in F6Publishing: 57] [Article Influence: 5.7] [Reference Citation Analysis (0)] |
| 13. | Koike K, Moriya K, Iino S, Yotsuyanagi H, Endo Y, Miyamura T, Kurokawa K. High-level expression of hepatitis B virus HBx gene and hepatocarcinogenesis in transgenic mice. Hepatology. 1994;19:810-819. [PubMed] [Cited in This Article: ] |
| 14. | Wurmbach E, Chen YB, Khitrov G, Zhang W, Roayaie S, Schwartz M, Fiel I, Thung S, Mazzaferro V, Bruix J. Genome-wide molecular profiles of HCV-induced dysplasia and hepatocellular carcinoma. Hepatology. 2007;45:938-947. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 506] [Cited by in F6Publishing: 534] [Article Influence: 31.4] [Reference Citation Analysis (0)] |
| 15. | Levrero M. Viral hepatitis and liver cancer: the case of hepatitis C. Oncogene. 2006;25:3834-3847. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 287] [Cited by in F6Publishing: 314] [Article Influence: 17.4] [Reference Citation Analysis (0)] |
| 16. | Chen SL, Morgan TR. The natural history of hepatitis C virus (HCV) infection. Int J Med Sci. 2006;3:47-52. [PubMed] [Cited in This Article: ] |
| 17. | Plumlee CR, Lazaro CA, Fausto N, Polyak SJ. Effect of ethanol on innate antiviral pathways and HCV replication in human liver cells. Virol J. 2005;2:89. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 40] [Cited by in F6Publishing: 48] [Article Influence: 2.5] [Reference Citation Analysis (0)] |
| 18. | Voigt MD. Alcohol in hepatocellular cancer. Clin Liver Dis. 2005;9:151-169. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 53] [Cited by in F6Publishing: 54] [Article Influence: 2.8] [Reference Citation Analysis (0)] |
| 19. | Siegel AB, Zhu AX. Metabolic syndrome and hepatocellular carcinoma: two growing epidemics with a potential link. Cancer. 2009;115:5651-5661. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 296] [Cited by in F6Publishing: 277] [Article Influence: 18.5] [Reference Citation Analysis (0)] |
| 20. | Hamid AS, Tesfamariam IG, Zhang Y, Zhang ZG. Aflatoxin B1-induced hepatocellular carcinoma in developing countries: Geographical distribution, mechanism of action and prevention. Oncol Lett. 2013;5:1087-1092. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 169] [Cited by in F6Publishing: 173] [Article Influence: 15.7] [Reference Citation Analysis (0)] |
| 21. | Chakraborty C, Hsu CH, Wen ZH, Lin CS, Agoramoorthy G. Zebrafish: a complete animal model for in vivo drug discovery and development. Curr Drug Metab. 2009;10:116-124. [PubMed] [Cited in This Article: ] |
| 22. | McGrath P, Li CQ. Zebrafish: a predictive model for assessing drug-induced toxicity. Drug Discov Today. 2008;13:394-401. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 376] [Cited by in F6Publishing: 375] [Article Influence: 23.4] [Reference Citation Analysis (0)] |
| 23. | Dooley K, Zon LI. Zebrafish: a model system for the study of human disease. Curr Opin Genet Dev. 2000;10:252-256. [PubMed] [Cited in This Article: ] |
| 24. | Santoriello C, Zon LI. Hooked! Modeling human disease in zebrafish. J Clin Invest. 2012;122:2337-2343. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 319] [Cited by in F6Publishing: 333] [Article Influence: 27.8] [Reference Citation Analysis (0)] |
| 25. | Lieschke GJ, Currie PD. Animal models of human disease: zebrafish swim into view. Nat Rev Genet. 2007;8:353-367. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 1552] [Cited by in F6Publishing: 1449] [Article Influence: 85.2] [Reference Citation Analysis (0)] |
| 26. | Parng C, Seng WL, Semino C, McGrath P. Zebrafish: a preclinical model for drug screening. Assay Drug Dev Technol. 2002;1:41-48. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 292] [Cited by in F6Publishing: 274] [Article Influence: 13.7] [Reference Citation Analysis (0)] |
| 27. | Lu JW, Hsia Y, Tu HC, Hsiao YC, Yang WY, Wang HD, Yuh CH. Liver development and cancer formation in zebrafish. Birth Defects Res C Embryo Today. 2011;93:157-172. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 24] [Cited by in F6Publishing: 24] [Article Influence: 1.8] [Reference Citation Analysis (0)] |
| 28. | Chu J, Sadler KC. New school in liver development: lessons from zebrafish. Hepatology. 2009;50:1656-1663. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 152] [Cited by in F6Publishing: 152] [Article Influence: 10.1] [Reference Citation Analysis (0)] |
| 29. | Rekha RD, Amali AA, Her GM, Yeh YH, Gong HY, Hu SY, Lin GH, Wu JL. Thioacetamide accelerates steatohepatitis, cirrhosis and HCC by expressing HCV core protein in transgenic zebrafish Danio rerio. Toxicology. 2008;243:11-22. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 50] [Cited by in F6Publishing: 44] [Article Influence: 2.6] [Reference Citation Analysis (0)] |
| 30. | Gaj T, Gersbach CA, Barbas CF. ZFN, TALEN, and CRISPR/Cas-based methods for genome engineering. Trends Biotechnol. 2013;31:397-405. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 2477] [Cited by in F6Publishing: 2321] [Article Influence: 211.0] [Reference Citation Analysis (0)] |
| 31. | Herszényi L, Tulassay Z. Epidemiology of gastrointestinal and liver tumors. Eur Rev Med Pharmacol Sci. 2010;14:249-258. [PubMed] [Cited in This Article: ] |
| 32. | Lemaigre F, Zaret KS. Liver development update: new embryo models, cell lineage control, and morphogenesis. Curr Opin Genet Dev. 2004;14:582-590. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 210] [Cited by in F6Publishing: 192] [Article Influence: 10.1] [Reference Citation Analysis (0)] |
| 33. | Si-Tayeb K, Lemaigre FP, Duncan SA. Organogenesis and development of the liver. Dev Cell. 2010;18:175-189. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 520] [Cited by in F6Publishing: 500] [Article Influence: 35.7] [Reference Citation Analysis (0)] |
| 34. | Pack M, Solnica-Krezel L, Malicki J, Neuhauss SC, Schier AF, Stemple DL, Driever W, Fishman MC. Mutations affecting development of zebrafish digestive organs. Development. 1996;123:321-328. [PubMed] [Cited in This Article: ] |
| 35. | Menke AL, Spitsbergen JM, Wolterbeek AP, Woutersen RA. Normal anatomy and histology of the adult zebrafish. Toxicol Pathol. 2011;39:759-775. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 134] [Cited by in F6Publishing: 137] [Article Influence: 10.5] [Reference Citation Analysis (0)] |
| 36. | Field HA, Ober EA, Roeser T, Stainier DY. Formation of the digestive system in zebrafish. I. Liver morphogenesis. Dev Biol. 2003;253:279-290. [PubMed] [Cited in This Article: ] |
| 37. | Tao T, Peng J. Liver development in zebrafish (Danio rerio). J Genet Genomics. 2009;36:325-334. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 92] [Cited by in F6Publishing: 107] [Article Influence: 7.1] [Reference Citation Analysis (0)] |
| 38. | Korzh S, Pan X, Garcia-Lecea M, Winata CL, Pan X, Wohland T, Korzh V, Gong Z. Requirement of vasculogenesis and blood circulation in late stages of liver growth in zebrafish. BMC Dev Biol. 2008;8:84. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 121] [Cited by in F6Publishing: 128] [Article Influence: 8.0] [Reference Citation Analysis (0)] |
| 39. | Jung J, Zheng M, Goldfarb M, Zaret KS. Initiation of mammalian liver development from endoderm by fibroblast growth factors. Science. 1999;284:1998-2003. [PubMed] [Cited in This Article: ] |
| 40. | Niu X, Shi H, Peng J. The role of mesodermal signals during liver organogenesis in zebrafish. Sci China Life Sci. 2010;53:455-461. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 11] [Cited by in F6Publishing: 7] [Article Influence: 0.5] [Reference Citation Analysis (0)] |
| 41. | Shin D, Shin CH, Tucker J, Ober EA, Rentzsch F, Poss KD, Hammerschmidt M, Mullins MC, Stainier DY. Bmp and Fgf signaling are essential for liver specification in zebrafish. Development. 2007;134:2041-2050. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 153] [Cited by in F6Publishing: 154] [Article Influence: 9.6] [Reference Citation Analysis (0)] |
| 42. | Goessling W, North TE, Lord AM, Ceol C, Lee S, Weidinger G, Bourque C, Strijbosch R, Haramis AP, Puder M. APC mutant zebrafish uncover a changing temporal requirement for wnt signaling in liver development. Dev Biol. 2008;320:161-174. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 145] [Cited by in F6Publishing: 155] [Article Influence: 9.7] [Reference Citation Analysis (0)] |
| 43. | Wallace KN, Yusuff S, Sonntag JM, Chin AJ, Pack M. Zebrafish hhex regulates liver development and digestive organ chirality. Genesis. 2001;30:141-143. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 75] [Cited by in F6Publishing: 70] [Article Influence: 3.0] [Reference Citation Analysis (0)] |
| 44. | Ober EA, Field HA, Stainier DY. From endoderm formation to liver and pancreas development in zebrafish. Mech Dev. 2003;120:5-18. [PubMed] [Cited in This Article: ] |
| 45. | Liao W, Ho CY, Yan YL, Postlethwait J, Stainier DY. Hhex and scl function in parallel to regulate early endothelial and blood differentiation in zebrafish. Development. 2000;127:4303-4313. [PubMed] [Cited in This Article: ] |
| 46. | Cheng W, Guo L, Zhang Z, Soo HM, Wen C, Wu W, Peng J. HNF factors form a network to regulate liver-enriched genes in zebrafish. Dev Biol. 2006;294:482-496. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 66] [Cited by in F6Publishing: 62] [Article Influence: 3.4] [Reference Citation Analysis (0)] |
| 47. | Alexander J, Stainier DY. A molecular pathway leading to endoderm formation in zebrafish. Curr Biol. 1999;9:1147-1157. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 258] [Cited by in F6Publishing: 265] [Article Influence: 10.6] [Reference Citation Analysis (0)] |
| 48. | Reiter JF, Kikuchi Y, Stainier DY. Multiple roles for Gata5 in zebrafish endoderm formation. Development. 2001;128:125-135. [PubMed] [Cited in This Article: ] |
| 49. | Chang C, Hu M, Zhu Z, Lo LJ, Chen J, Peng J. liver-enriched gene 1a and 1b encode novel secretory proteins essential for normal liver development in zebrafish. PLoS One. 2011;6:e22910. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 17] [Cited by in F6Publishing: 17] [Article Influence: 1.3] [Reference Citation Analysis (0)] |
| 50. | Lin TY, Chou CF, Chung HY, Chiang CY, Li CH, Wu JL, Lin HJ, Pai TW, Hu CH, Tzou WS. Hypoxia-inducible factor 2 alpha is essential for hepatic outgrowth and functions via the regulation of leg1 transcription in the zebrafish embryo. PLoS One. 2014;9:e101980. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 26] [Cited by in F6Publishing: 30] [Article Influence: 3.0] [Reference Citation Analysis (0)] |
| 51. | Noël ES, Casal-Sueiro A, Busch-Nentwich E, Verkade H, Dong PD, Stemple DL, Ober EA. Organ-specific requirements for Hdac1 in liver and pancreas formation. Dev Biol. 2008;322:237-250. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 60] [Cited by in F6Publishing: 64] [Article Influence: 4.0] [Reference Citation Analysis (0)] |
| 52. | Farooq M, Sulochana KN, Pan X, To J, Sheng D, Gong Z, Ge R. Histone deacetylase 3 (hdac3) is specifically required for liver development in zebrafish. Dev Biol. 2008;317:336-353. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 96] [Cited by in F6Publishing: 101] [Article Influence: 6.3] [Reference Citation Analysis (0)] |
| 53. | Sadler KC, Krahn KN, Gaur NA, Ukomadu C. Liver growth in the embryo and during liver regeneration in zebrafish requires the cell cycle regulator, uhrf1. Proc Natl Acad Sci USA. 2007;104:1570-1575. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 126] [Cited by in F6Publishing: 131] [Article Influence: 7.7] [Reference Citation Analysis (0)] |
| 54. | Culp P, Nüsslein-Volhard C, Hopkins N. High-frequency germ-line transmission of plasmid DNA sequences injected into fertilized zebrafish eggs. Proc Natl Acad Sci USA. 1991;88:7953-7957. [PubMed] [Cited in This Article: ] |
| 55. | Stuart GW, McMurray JV, Westerfield M. Replication, integration and stable germ-line transmission of foreign sequences injected into early zebrafish embryos. Development. 1988;103:403-412. [PubMed] [Cited in This Article: ] |
| 56. | Deiters A, Yoder JA. Conditional transgene and gene targeting methodologies in zebrafish. Zebrafish. 2006;3:415-429. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 19] [Cited by in F6Publishing: 19] [Article Influence: 1.2] [Reference Citation Analysis (0)] |
| 57. | Stuart GW, Vielkind JR, McMurray JV, Westerfield M. Stable lines of transgenic zebrafish exhibit reproducible patterns of transgene expression. Development. 1990;109:577-584. [PubMed] [Cited in This Article: ] |
| 58. | Thermes V, Grabher C, Ristoratore F, Bourrat F, Choulika A, Wittbrodt J, Joly JS. I-SceI meganuclease mediates highly efficient transgenesis in fish. Mech Dev. 2002;118:91-98. [PubMed] [Cited in This Article: ] |
| 59. | Ivics Z, Hackett PB, Plasterk RH, Izsvák Z. Molecular reconstruction of Sleeping Beauty, a Tc1-like transposon from fish, and its transposition in human cells. Cell. 1997;91:501-510. [PubMed] [Cited in This Article: ] |
| 60. | Emelyanov A, Gao Y, Naqvi NI, Parinov S. Trans-kingdom transposition of the maize dissociation element. Genetics. 2006;174:1095-1104. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 84] [Cited by in F6Publishing: 88] [Article Influence: 4.9] [Reference Citation Analysis (0)] |
| 61. | Kawakami K, Shima A, Kawakami N. Identification of a functional transposase of the Tol2 element, an Ac-like element from the Japanese medaka fish, and its transposition in the zebrafish germ lineage. Proc Natl Acad Sci USA. 2000;97:11403-11408. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 376] [Cited by in F6Publishing: 357] [Article Influence: 14.9] [Reference Citation Analysis (0)] |
| 62. | Kawakami K, Shima A. Identification of the Tol2 transposase of the medaka fish Oryzias latipes that catalyzes excision of a nonautonomous Tol2 element in zebrafish Danio rerio. Gene. 1999;240:239-244. [PubMed] [Cited in This Article: ] |
| 63. | Balciunas D, Wangensteen KJ, Wilber A, Bell J, Geurts A, Sivasubbu S, Wang X, Hackett PB, Largaespada DA, McIvor RS. Harnessing a high cargo-capacity transposon for genetic applications in vertebrates. PLoS Genet. 2006;2:e169. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 223] [Cited by in F6Publishing: 238] [Article Influence: 13.2] [Reference Citation Analysis (0)] |
| 64. | Villefranc JA, Amigo J, Lawson ND. Gateway compatible vectors for analysis of gene function in the zebrafish. Dev Dyn. 2007;236:3077-3087. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 263] [Cited by in F6Publishing: 250] [Article Influence: 15.6] [Reference Citation Analysis (0)] |
| 65. | Kwan KM, Fujimoto E, Grabher C, Mangum BD, Hardy ME, Campbell DS, Parant JM, Yost HJ, Kanki JP, Chien CB. The Tol2kit: a multisite gateway-based construction kit for Tol2 transposon transgenesis constructs. Dev Dyn. 2007;236:3088-3099. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 1507] [Cited by in F6Publishing: 1281] [Article Influence: 75.4] [Reference Citation Analysis (0)] |
| 66. | Walhout AJ, Temple GF, Brasch MA, Hartley JL, Lorson MA, van den Heuvel S, Vidal M. GATEWAY recombinational cloning: application to the cloning of large numbers of open reading frames or ORFeomes. Methods Enzymol. 2000;328:575-592. [PubMed] [Cited in This Article: ] |
| 67. | Her GM, Yeh YH, Wu JL. 435-bp liver regulatory sequence in the liver fatty acid binding protein (L-FABP) gene is sufficient to modulate liver regional expression in transgenic zebrafish. Dev Dyn. 2003;227:347-356. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 62] [Cited by in F6Publishing: 62] [Article Influence: 3.0] [Reference Citation Analysis (0)] |
| 68. | Her GM, Chiang CC, Chen WY, Wu JL. In vivo studies of liver-type fatty acid binding protein (L-FABP) gene expression in liver of transgenic zebrafish (Danio rerio). FEBS Lett. 2003;538:125-133. [PubMed] [Cited in This Article: ] |
| 69. | Lu JW, Liao CY, Yang WY, Lin YM, Jin SL, Wang HD, Yuh CH. Overexpression of endothelin 1 triggers hepatocarcinogenesis in zebrafish and promotes cell proliferation and migration through the AKT pathway. PLoS One. 2014;9:e85318. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 52] [Cited by in F6Publishing: 55] [Article Influence: 5.5] [Reference Citation Analysis (0)] |
| 70. | Lu JW, Yang WY, Tsai SM, Lin YM, Chang PH, Chen JR, Wang HD, Wu JL, Jin SL, Yuh CH. Liver-specific expressions of HBx and src in the p53 mutant trigger hepatocarcinogenesis in zebrafish. PLoS One. 2013;8:e76951. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 44] [Cited by in F6Publishing: 44] [Article Influence: 4.0] [Reference Citation Analysis (0)] |
| 71. | Huang X, Nguyen AT, Li Z, Emelyanov A, Parinov S, Gong Z. One step forward: the use of transgenic zebrafish tumor model in drug screens. Birth Defects Res C Embryo Today. 2011;93:173-181. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 14] [Cited by in F6Publishing: 14] [Article Influence: 1.1] [Reference Citation Analysis (0)] |
| 72. | Blechinger SR, Evans TG, Tang PT, Kuwada JY, Warren JT, Krone PH. The heat-inducible zebrafish hsp70 gene is expressed during normal lens development under non-stress conditions. Mech Dev. 2002;112:213-215. [PubMed] [Cited in This Article: ] |
| 73. | Shoji W, Sato-Maeda M. Application of heat shock promoter in transgenic zebrafish. Dev Growth Differ. 2008;50:401-406. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 49] [Cited by in F6Publishing: 54] [Article Influence: 3.4] [Reference Citation Analysis (0)] |
| 74. | Yang YS, Hughes TE. Cre stoplight: a red/green fluorescent reporter of Cre recombinase expression in living cells. Biotechniques. 2001;31:1036, 1038, 1040-1041. [PubMed] [Cited in This Article: ] |
| 75. | Seok SH, Na YR, Han JH, Kim TH, Jung H, Lee BH, Emelyanov A, Parinov S, Park JH. Cre/loxP-regulated transgenic zebrafish model for neural progenitor-specific oncogenic Kras expression. Cancer Sci. 2010;101:149-154. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 15] [Cited by in F6Publishing: 15] [Article Influence: 1.0] [Reference Citation Analysis (0)] |
| 76. | Fischer JA, Giniger E, Maniatis T, Ptashne M. GAL4 activates transcription in Drosophila. Nature. 1988;332:853-856. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 337] [Cited by in F6Publishing: 348] [Article Influence: 9.7] [Reference Citation Analysis (0)] |
| 77. | Brand AH, Perrimon N. Targeted gene expression as a means of altering cell fates and generating dominant phenotypes. Development. 1993;118:401-415. [PubMed] [Cited in This Article: ] |
| 78. | Scheer N, Campos-Ortega JA. Use of the Gal4-UAS technique for targeted gene expression in the zebrafish. Mech Dev. 1999;80:153-158. [PubMed] [Cited in This Article: ] |
| 79. | Zhan H, Spitsbergen JM, Qing W, Wu YL, Paul TA, Casey JW, Her GM, Gong Z. Transgenic expression of walleye dermal sarcoma virus rv-cyclin gene in zebrafish and its suppressive effect on liver tumor development after carcinogen treatment. Mar Biotechnol (NY). 2010;12:640-649. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 11] [Cited by in F6Publishing: 10] [Article Influence: 0.7] [Reference Citation Analysis (0)] |
| 80. | Li Z, Huang X, Zhan H, Zeng Z, Li C, Spitsbergen JM, Meierjohann S, Schartl M, Gong Z. Inducible and repressable oncogene-addicted hepatocellular carcinoma in Tet-on xmrk transgenic zebrafish. J Hepatol. 2012;56:419-425. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 90] [Cited by in F6Publishing: 92] [Article Influence: 7.7] [Reference Citation Analysis (0)] |
| 81. | Liu W, Chen JR, Hsu CH, Li YH, Chen YM, Lin CY, Huang SJ, Chang ZK, Chen YC, Lin CH. A zebrafish model of intrahepatic cholangiocarcinoma by dual expression of hepatitis B virus X and hepatitis C virus core protein in liver. Hepatology. 2012;56:2268-2276. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 52] [Cited by in F6Publishing: 56] [Article Influence: 4.7] [Reference Citation Analysis (0)] |
| 82. | Nguyen AT, Emelyanov A, Koh CH, Spitsbergen JM, Parinov S, Gong Z. An inducible kras(V12) transgenic zebrafish model for liver tumorigenesis and chemical drug screening. Dis Model Mech. 2012;5:63-72. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 119] [Cited by in F6Publishing: 125] [Article Influence: 9.6] [Reference Citation Analysis (0)] |
| 83. | Li Z, Zheng W, Wang Z, Zeng Z, Zhan H, Li C, Zhou L, Yan C, Spitsbergen JM, Gong Z. A transgenic zebrafish liver tumor model with inducible Myc expression reveals conserved Myc signatures with mammalian liver tumors. Dis Model Mech. 2013;6:414-423. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 59] [Cited by in F6Publishing: 63] [Article Influence: 5.3] [Reference Citation Analysis (0)] |
| 84. | Meng X, Noyes MB, Zhu LJ, Lawson ND, Wolfe SA. Targeted gene inactivation in zebrafish using engineered zinc-finger nucleases. Nat Biotechnol. 2008;26:695-701. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 602] [Cited by in F6Publishing: 568] [Article Influence: 35.5] [Reference Citation Analysis (0)] |
| 85. | Huang P, Xiao A, Zhou M, Zhu Z, Lin S, Zhang B. Heritable gene targeting in zebrafish using customized TALENs. Nat Biotechnol. 2011;29:699-700. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 538] [Cited by in F6Publishing: 564] [Article Influence: 43.4] [Reference Citation Analysis (0)] |
| 86. | Hwang WY, Fu Y, Reyon D, Maeder ML, Tsai SQ, Sander JD, Peterson RT, Yeh JR, Joung JK. Efficient genome editing in zebrafish using a CRISPR-Cas system. Nat Biotechnol. 2013;31:227-229. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 2349] [Cited by in F6Publishing: 2131] [Article Influence: 193.7] [Reference Citation Analysis (0)] |
| 87. | Kim H, Kim JS. A guide to genome engineering with programmable nucleases. Nat Rev Genet. 2014;15:321-334. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 839] [Cited by in F6Publishing: 780] [Article Influence: 78.0] [Reference Citation Analysis (0)] |
| 88. | Ul Ain Q, Chung JY, Kim YH. Current and future delivery systems for engineered nucleases: ZFN, TALEN and RGEN. J Control Release. 2015;205:120-127. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 77] [Cited by in F6Publishing: 81] [Article Influence: 8.1] [Reference Citation Analysis (0)] |
| 89. | Bitinaite J, Wah DA, Aggarwal AK, Schildkraut I. FokI dimerization is required for DNA cleavage. Proc Natl Acad Sci USA. 1998;95:10570-10575. [PubMed] [Cited in This Article: ] |
| 90. | Urnov FD, Rebar EJ, Holmes MC, Zhang HS, Gregory PD. Genome editing with engineered zinc finger nucleases. Nat Rev Genet. 2010;11:636-646. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 1482] [Cited by in F6Publishing: 1400] [Article Influence: 100.0] [Reference Citation Analysis (0)] |
| 91. | Miller J, McLachlan AD, Klug A. Repetitive zinc-binding domains in the protein transcription factor IIIA from Xenopus oocytes. EMBO J. 1985;4:1609-1614. [PubMed] [Cited in This Article: ] |
| 92. | Vanamee ES, Santagata S, Aggarwal AK. FokI requires two specific DNA sites for cleavage. J Mol Biol. 2001;309:69-78. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 129] [Cited by in F6Publishing: 144] [Article Influence: 6.3] [Reference Citation Analysis (0)] |
| 93. | Gupta RM, Musunuru K. Expanding the genetic editing tool kit: ZFNs, TALENs, and CRISPR-Cas9. J Clin Invest. 2014;124:4154-4161. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 278] [Cited by in F6Publishing: 270] [Article Influence: 27.0] [Reference Citation Analysis (0)] |
| 94. | Segal DJ, Beerli RR, Blancafort P, Dreier B, Effertz K, Huber A, Koksch B, Lund CV, Magnenat L, Valente D. Evaluation of a modular strategy for the construction of novel polydactyl zinc finger DNA-binding proteins. Biochemistry. 2003;42:2137-2148. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 127] [Cited by in F6Publishing: 116] [Article Influence: 5.5] [Reference Citation Analysis (0)] |
| 95. | Maeder ML, Thibodeau-Beganny S, Sander JD, Voytas DF, Joung JK. Oligomerized pool engineering (OPEN): an ‘open-source’ protocol for making customized zinc-finger arrays. Nat Protoc. 2009;4:1471-1501. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 171] [Cited by in F6Publishing: 160] [Article Influence: 10.7] [Reference Citation Analysis (0)] |
| 96. | Sander JD, Dahlborg EJ, Goodwin MJ, Cade L, Zhang F, Cifuentes D, Curtin SJ, Blackburn JS, Thibodeau-Beganny S, Qi Y. Selection-free zinc-finger-nuclease engineering by context-dependent assembly (CoDA). Nat Methods. 2011;8:67-69. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 422] [Cited by in F6Publishing: 359] [Article Influence: 27.6] [Reference Citation Analysis (0)] |
| 97. | Hockemeyer D, Soldner F, Beard C, Gao Q, Mitalipova M, DeKelver RC, Katibah GE, Amora R, Boydston EA, Zeitler B. Efficient targeting of expressed and silent genes in human ESCs and iPSCs using zinc-finger nucleases. Nat Biotechnol. 2009;27:851-857. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 878] [Cited by in F6Publishing: 792] [Article Influence: 52.8] [Reference Citation Analysis (0)] |
| 98. | Miller JC, Holmes MC, Wang J, Guschin DY, Lee YL, Rupniewski I, Beausejour CM, Waite AJ, Wang NS, Kim KA. An improved zinc-finger nuclease architecture for highly specific genome editing. Nat Biotechnol. 2007;25:778-785. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 809] [Cited by in F6Publishing: 751] [Article Influence: 44.2] [Reference Citation Analysis (0)] |
| 99. | Szczepek M, Brondani V, Büchel J, Serrano L, Segal DJ, Cathomen T. Structure-based redesign of the dimerization interface reduces the toxicity of zinc-finger nucleases. Nat Biotechnol. 2007;25:786-793. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 415] [Cited by in F6Publishing: 428] [Article Influence: 25.2] [Reference Citation Analysis (0)] |
| 100. | Doyon Y, Vo TD, Mendel MC, Greenberg SG, Wang J, Xia DF, Miller JC, Urnov FD, Gregory PD, Holmes MC. Enhancing zinc-finger-nuclease activity with improved obligate heterodimeric architectures. Nat Methods. 2011;8:74-79. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 318] [Cited by in F6Publishing: 304] [Article Influence: 21.7] [Reference Citation Analysis (0)] |
| 101. | Li T, Liu B, Spalding MH, Weeks DP, Yang B. High-efficiency TALEN-based gene editing produces disease-resistant rice. Nat Biotechnol. 2012;30:390-392. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 772] [Cited by in F6Publishing: 595] [Article Influence: 49.6] [Reference Citation Analysis (0)] |
| 102. | Joung JK, Sander JD. TALENs: a widely applicable technology for targeted genome editing. Nat Rev Mol Cell Biol. 2013;14:49-55. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 1038] [Cited by in F6Publishing: 995] [Article Influence: 82.9] [Reference Citation Analysis (0)] |
| 103. | Deng D, Yan C, Pan X, Mahfouz M, Wang J, Zhu JK, Shi Y, Yan N. Structural basis for sequence-specific recognition of DNA by TAL effectors. Science. 2012;335:720-723. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 476] [Cited by in F6Publishing: 436] [Article Influence: 36.3] [Reference Citation Analysis (0)] |
| 104. | Bedell VM, Wang Y, Campbell JM, Poshusta TL, Starker CG, Krug RG, Tan W, Penheiter SG, Ma AC, Leung AY. In vivo genome editing using a high-efficiency TALEN system. Nature. 2012;491:114-118. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 727] [Cited by in F6Publishing: 702] [Article Influence: 58.5] [Reference Citation Analysis (0)] |
| 105. | Reyon D, Khayter C, Regan MR, Joung JK, Sander JD. Engineering designer transcription activator-like effector nucleases (TALENs) by REAL or REAL-Fast assembly. Curr Protoc Mol Biol. 2012;Chapter 12:Unit 12.15. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 48] [Cited by in F6Publishing: 64] [Article Influence: 5.8] [Reference Citation Analysis (0)] |
| 106. | Weber E, Gruetzner R, Werner S, Engler C, Marillonnet S. Assembly of designer TAL effectors by Golden Gate cloning. PLoS One. 2011;6:e19722. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 177] [Cited by in F6Publishing: 169] [Article Influence: 13.0] [Reference Citation Analysis (0)] |
| 107. | Reyon D, Tsai SQ, Khayter C, Foden JA, Sander JD, Joung JK. FLASH assembly of TALENs for high-throughput genome editing. Nat Biotechnol. 2012;30:460-465. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 835] [Cited by in F6Publishing: 862] [Article Influence: 71.8] [Reference Citation Analysis (0)] |
| 108. | Wiedenheft B, Sternberg SH, Doudna JA. RNA-guided genetic silencing systems in bacteria and archaea. Nature. 2012;482:331-338. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 1269] [Cited by in F6Publishing: 1305] [Article Influence: 108.8] [Reference Citation Analysis (0)] |
| 109. | Deltcheva E, Chylinski K, Sharma CM, Gonzales K, Chao Y, Pirzada ZA, Eckert MR, Vogel J, Charpentier E. CRISPR RNA maturation by trans-encoded small RNA and host factor RNase III. Nature. 2011;471:602-607. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 1870] [Cited by in F6Publishing: 1630] [Article Influence: 125.4] [Reference Citation Analysis (0)] |
| 110. | Ding Q, Regan SN, Xia Y, Oostrom LA, Cowan CA, Musunuru K. Enhanced efficiency of human pluripotent stem cell genome editing through replacing TALENs with CRISPRs. Cell Stem Cell. 2013;12:393-394. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 365] [Cited by in F6Publishing: 382] [Article Influence: 34.7] [Reference Citation Analysis (0)] |
| 111. | Ablain J, Durand EM, Yang S, Zhou Y, Zon LI. A CRISPR/Cas9 vector system for tissue-specific gene disruption in zebrafish. Dev Cell. 2015;32:756-764. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 298] [Cited by in F6Publishing: 275] [Article Influence: 30.6] [Reference Citation Analysis (0)] |
| 112. | Kim CM, Koike K, Saito I, Miyamura T, Jay G. HBx gene of hepatitis B virus induces liver cancer in transgenic mice. Nature. 1991;351:317-320. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 880] [Cited by in F6Publishing: 855] [Article Influence: 25.9] [Reference Citation Analysis (0)] |
| 113. | Seifer M, Höhne M, Schaefer S, Gerlich WH. In vitro tumorigenicity of hepatitis B virus DNA and HBx protein. J Hepatol. 1991;13 Suppl 4:S61-S65. [PubMed] [Cited in This Article: ] |
| 114. | Wu BK, Li CC, Chen HJ, Chang JL, Jeng KS, Chou CK, Hsu MT, Tsai TF. Blocking of G1/S transition and cell death in the regenerating liver of Hepatitis B virus X protein transgenic mice. Biochem Biophys Res Commun. 2006;340:916-928. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 92] [Cited by in F6Publishing: 99] [Article Influence: 5.2] [Reference Citation Analysis (0)] |
| 115. | Jeannot E, Boorman GA, Kosyk O, Bradford BU, Shymoniak S, Tumurbaatar B, Weinman SA, Melnyk SB, Tryndyak V, Pogribny IP. Increased incidence of aflatoxin B1-induced liver tumors in hepatitis virus C transgenic mice. Int J Cancer. 2012;130:1347-1356. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 26] [Cited by in F6Publishing: 27] [Article Influence: 2.1] [Reference Citation Analysis (0)] |
| 116. | Lian M, Liu Y, Yu SZ, Qian GS, Wan SG, Dixon KR. Hepatitis B virus x gene and cyanobacterial toxins promote aflatoxin B1-induced hepatotumorigenesis in mice. World J Gastroenterol. 2006;12:3065-3072. [PubMed] [Cited in This Article: ] |
| 117. | Akriviadis EA, Llovet JM, Efremidis SC, Shouval D, Canelo R, Ringe B, Meyers WC. Hepatocellular carcinoma. Br J Surg. 1998;85:1319-1331. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 119] [Cited by in F6Publishing: 122] [Article Influence: 4.7] [Reference Citation Analysis (0)] |
| 118. | Aguilar F, Harris CC, Sun T, Hollstein M, Cerutti P. Geographic variation of p53 mutational profile in nonmalignant human liver. Science. 1994;264:1317-1319. [PubMed] [Cited in This Article: ] |
| 119. | Pang R, Tse E, Poon RT. Molecular pathways in hepatocellular carcinoma. Cancer Lett. 2006;240:157-169. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 62] [Cited by in F6Publishing: 69] [Article Influence: 3.6] [Reference Citation Analysis (0)] |
| 120. | Shieh YS, Chang YS, Hong JR, Chen LJ, Jou LK, Hsu CC, Her GM. Increase of hepatic fat accumulation by liver specific expression of Hepatitis B virus X protein in zebrafish. Biochim Biophys Acta. 2010;1801:721-730. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 53] [Cited by in F6Publishing: 60] [Article Influence: 4.3] [Reference Citation Analysis (0)] |
| 121. | Chen LJ, Hsu CC, Hong JR, Jou LK, Tseng HC, Wu JL, Liou YC, Her GM. Liver-specific expression of p53-negative regulator mdm2 leads to growth retardation and fragile liver in zebrafish. Dev Dyn. 2008;237:1070-1081. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 13] [Cited by in F6Publishing: 13] [Article Influence: 0.8] [Reference Citation Analysis (0)] |
| 122. | Higashitsuji H, Higashitsuji H, Itoh K, Sakurai T, Nagao T, Sumitomo Y, Masuda T, Dawson S, Shimada Y, Mayer RJ. The oncoprotein gankyrin binds to MDM2/HDM2, enhancing ubiquitylation and degradation of p53. Cancer Cell. 2005;8:75-87. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 165] [Cited by in F6Publishing: 176] [Article Influence: 9.3] [Reference Citation Analysis (0)] |
| 123. | Her GM, Hsu CC, Hong JR, Lai CY, Hsu MC, Pang HW, Chan SK, Pai WY. Overexpression of gankyrin induces liver steatosis in zebrafish (Danio rerio). Biochim Biophys Acta. 2011;1811:536-548. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 52] [Cited by in F6Publishing: 50] [Article Influence: 3.8] [Reference Citation Analysis (0)] |
| 124. | Mudbhary R, Hoshida Y, Chernyavskaya Y, Jacob V, Villanueva A, Fiel MI, Chen X, Kojima K, Thung S, Bronson RT. UHRF1 overexpression drives DNA hypomethylation and hepatocellular carcinoma. Cancer Cell. 2014;25:196-209. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 212] [Cited by in F6Publishing: 238] [Article Influence: 23.8] [Reference Citation Analysis (0)] |
| 125. | LaPierre LA, Casey JW, Holzschu DL. Walleye retroviruses associated with skin tumors and hyperplasias encode cyclin D homologs. J Virol. 1998;72:8765-8771. [PubMed] [Cited in This Article: ] |
| 126. | Quackenbush SL, Holzschu DL, Bowser PR, Casey JW. Transcriptional analysis of walleye dermal sarcoma virus (WDSV). Virology. 1997;237:107-112. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 35] [Cited by in F6Publishing: 36] [Article Influence: 1.3] [Reference Citation Analysis (0)] |
| 127. | Lu JW, Hsia Y, Yang WY, Lin YI, Li CC, Tsai TF, Chang KW, Shieh GS, Tsai SF, Wang HD. Identification of the common regulators for hepatocellular carcinoma induced by hepatitis B virus X antigen in a mouse model. Carcinogenesis. 2012;33:209-219. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 45] [Cited by in F6Publishing: 48] [Article Influence: 3.7] [Reference Citation Analysis (0)] |
| 128. | Zhang L, Cai X, Chen K, Wang Z, Wang L, Ren M, Huang A, Tang H. Hepatitis B virus protein up-regulated HLJ1 expression via the transcription factor YY1 in human hepatocarcinoma cells. Virus Res. 2011;157:76-81. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 21] [Cited by in F6Publishing: 22] [Article Influence: 1.7] [Reference Citation Analysis (0)] |
| 129. | Sung WK, Lu Y, Lee CW, Zhang D, Ronaghi M, Lee CG. Deregulated direct targets of the hepatitis B virus (HBV) protein, HBx, identified through chromatin immunoprecipitation and expression microarray profiling. J Biol Chem. 2009;284:21941-21954. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 37] [Cited by in F6Publishing: 38] [Article Influence: 2.5] [Reference Citation Analysis (0)] |
| 130. | Zhang S, Jiang T, Feng L, Sun J, Lu H, Wang Q, Pan M, Huang D, Wang X, Wang L. Yin Yang-1 suppresses differentiation of hepatocellular carcinoma cells through the downregulation of CCAAT/enhancer-binding protein alpha. J Mol Med (Berl). 2012;90:1069-1077. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 28] [Cited by in F6Publishing: 24] [Article Influence: 2.0] [Reference Citation Analysis (0)] |
| 131. | Her GM, Pai WY, Lai CY, Hsieh YW, Pang HW. Ubiquitous transcription factor YY1 promotes zebrafish liver steatosis and lipotoxicity by inhibiting CHOP-10 expression. Biochim Biophys Acta. 2013;1831:1037-1051. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 28] [Cited by in F6Publishing: 29] [Article Influence: 2.6] [Reference Citation Analysis (0)] |
| 132. | Pai WY, Hsu CC, Lai CY, Chang TZ, Tsai YL, Her GM. Cannabinoid receptor 1 promotes hepatic lipid accumulation and lipotoxicity through the induction of SREBP-1c expression in zebrafish. Transgenic Res. 2013;22:823-838. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 31] [Cited by in F6Publishing: 27] [Article Influence: 2.5] [Reference Citation Analysis (0)] |
| 133. | Her GM, Cheng CH, Hong JR, Sundaram GS, Wu JL. Imbalance in liver homeostasis leading to hyperplasia by overexpressing either one of the Bcl-2-related genes, zfBLP1 and zfMcl-1a. Dev Dyn. 2006;235:515-523. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 18] [Cited by in F6Publishing: 18] [Article Influence: 1.0] [Reference Citation Analysis (0)] |
| 134. | Lu JW, Yang WY, Lin YM, Jin SL, Yuh CH. Hepatitis B virus X antigen and aflatoxin B1 synergistically cause hepatitis, steatosis and liver hyperplasia in transgenic zebrafish. Acta Histochem. 2013;115:728-739. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 28] [Cited by in F6Publishing: 33] [Article Influence: 3.0] [Reference Citation Analysis (0)] |
| 135. | Hayashi J, Aoki H, Kajino K, Moriyama M, Arakawa Y, Hino O. Hepatitis C virus core protein activates the MAPK/ERK cascade synergistically with tumor promoter TPA, but not with epidermal growth factor or transforming growth factor alpha. Hepatology. 2000;32:958-961. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 114] [Cited by in F6Publishing: 116] [Article Influence: 4.8] [Reference Citation Analysis (0)] |
| 136. | Nguyen AT, Emelyanov A, Koh CH, Spitsbergen JM, Lam SH, Mathavan S, Parinov S, Gong Z. A high level of liver-specific expression of oncogenic Kras(V12) drives robust liver tumorigenesis in transgenic zebrafish. Dis Model Mech. 2011;4:801-813. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 77] [Cited by in F6Publishing: 81] [Article Influence: 6.2] [Reference Citation Analysis (0)] |
| 137. | Chew TW, Liu XJ, Liu L, Spitsbergen JM, Gong Z, Low BC. Crosstalk of Ras and Rho: activation of RhoA abates Kras-induced liver tumorigenesis in transgenic zebrafish models. Oncogene. 2014;33:2717-2727. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 69] [Cited by in F6Publishing: 74] [Article Influence: 6.7] [Reference Citation Analysis (0)] |
| 138. | Li Z, Luo H, Li C, Huo X, Yan C, Huang X, Al-Haddawi M, Mathavan S, Gong Z. Transcriptomic analysis of a transgenic zebrafish hepatocellular carcinoma model reveals a prominent role of immune responses in tumour progression and regression. Int J Cancer. 2014;135:1564-1573. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 18] [Cited by in F6Publishing: 18] [Article Influence: 1.8] [Reference Citation Analysis (0)] |
| 139. | Rautou PE, Mansouri A, Lebrec D, Durand F, Valla D, Moreau R. Autophagy in liver diseases. J Hepatol. 2010;53:1123-1134. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 302] [Cited by in F6Publishing: 315] [Article Influence: 22.5] [Reference Citation Analysis (0)] |
| 140. | Takamura A, Komatsu M, Hara T, Sakamoto A, Kishi C, Waguri S, Eishi Y, Hino O, Tanaka K, Mizushima N. Autophagy-deficient mice develop multiple liver tumors. Genes Dev. 2011;25:795-800. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 923] [Cited by in F6Publishing: 961] [Article Influence: 73.9] [Reference Citation Analysis (0)] |
| 141. | Cui J, Sim TH, Gong Z, Shen HM. Generation of transgenic zebrafish with liver-specific expression of EGFP-Lc3: a new in vivo model for investigation of liver autophagy. Biochem Biophys Res Commun. 2012;422:268-273. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 24] [Cited by in F6Publishing: 22] [Article Influence: 1.8] [Reference Citation Analysis (0)] |
| 142. | Zheng W, Li Z, Nguyen AT, Li C, Emelyanov A, Gong Z. Xmrk, kras and myc transgenic zebrafish liver cancer models share molecular signatures with subsets of human hepatocellular carcinoma. PLoS One. 2014;9:e91179. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 46] [Cited by in F6Publishing: 51] [Article Influence: 5.1] [Reference Citation Analysis (0)] |
| 143. | Sun L, Nguyen AT, Spitsbergen JM, Gong Z. Myc-induced liver tumors in transgenic zebrafish can regress in tp53 null mutation. PLoS One. 2015;10:e0117249. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 21] [Cited by in F6Publishing: 25] [Article Influence: 2.8] [Reference Citation Analysis (0)] |
| 144. | Gómez del Pulgar T, Benitah SA, Valerón PF, Espina C, Lacal JC. Rho GTPase expression in tumourigenesis: evidence for a significant link. Bioessays. 2005;27:602-613. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 170] [Cited by in F6Publishing: 178] [Article Influence: 9.4] [Reference Citation Analysis (0)] |
| 145. | Michelini E, Cevenini L, Mezzanotte L, Coppa A, Roda A. Cell-based assays: fuelling drug discovery. Anal Bioanal Chem. 2010;398:227-238. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 137] [Cited by in F6Publishing: 144] [Article Influence: 10.3] [Reference Citation Analysis (0)] |
| 146. | Xiang J, Yang H, Che C, Zou H, Yang H, Wei Y, Quan J, Zhang H, Yang Z, Lin S. Identifying tumor cell growth inhibitors by combinatorial chemistry and zebrafish assays. PLoS One. 2009;4:e4361. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 25] [Cited by in F6Publishing: 25] [Article Influence: 1.7] [Reference Citation Analysis (0)] |
| 147. | Konantz M, Balci TB, Hartwig UF, Dellaire G, André MC, Berman JN, Lengerke C. Zebrafish xenografts as a tool for in vivo studies on human cancer. Ann N Y Acad Sci. 2012;1266:124-137. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 161] [Cited by in F6Publishing: 165] [Article Influence: 13.8] [Reference Citation Analysis (0)] |
| 148. | Lee SL, Rouhi P, Dahl Jensen L, Zhang D, Ji H, Hauptmann G, Ingham P, Cao Y. Hypoxia-induced pathological angiogenesis mediates tumor cell dissemination, invasion, and metastasis in a zebrafish tumor model. Proc Natl Acad Sci USA. 2009;106:19485-19490. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 190] [Cited by in F6Publishing: 193] [Article Influence: 12.9] [Reference Citation Analysis (0)] |
| 149. | Karna P, Rida PC, Turaga RC, Gao J, Gupta M, Fritz A, Werner E, Yates C, Zhou J, Aneja R. A novel microtubule-modulating agent EM011 inhibits angiogenesis by repressing the HIF-1α axis and disrupting cell polarity and migration. Carcinogenesis. 2012;33:1769-1781. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 13] [Cited by in F6Publishing: 14] [Article Influence: 1.2] [Reference Citation Analysis (0)] |
| 150. | Tran TC, Sneed B, Haider J, Blavo D, White A, Aiyejorun T, Baranowski TC, Rubinstein AL, Doan TN, Dingledine R. Automated, quantitative screening assay for antiangiogenic compounds using transgenic zebrafish. Cancer Res. 2007;67:11386-11392. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 185] [Cited by in F6Publishing: 171] [Article Influence: 10.7] [Reference Citation Analysis (0)] |
| 151. | Wang C, Tao W, Wang Y, Bikow J, Lu B, Keating A, Verma S, Parker TG, Han R, Wen XY. Rosuvastatin, identified from a zebrafish chemical genetic screen for antiangiogenic compounds, suppresses the growth of prostate cancer. Eur Urol. 2010;58:418-426. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 97] [Cited by in F6Publishing: 100] [Article Influence: 7.1] [Reference Citation Analysis (0)] |
| 152. | Ding CB, Zhao Y, Zhang JP, Peng ZG, Song DQ, Jiang JD. A zebrafish model for subgenomic hepatitis C virus replication. Int J Mol Med. 2015;35:791-797. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 20] [Cited by in F6Publishing: 20] [Article Influence: 2.2] [Reference Citation Analysis (0)] |
| 153. | Zhao Y, Qin W, Zhang JP, Hu ZY, Tong JW, Ding CB, Peng ZG, Zhao LX, Song DQ, Jiang JD. HCV IRES-mediated core expression in zebrafish. PLoS One. 2013;8:e56985. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 9] [Cited by in F6Publishing: 9] [Article Influence: 0.8] [Reference Citation Analysis (0)] |
| 154. | Ding CB, Zhang JP, Zhao Y, Peng ZG, Song DQ, Jiang JD. Zebrafish as a potential model organism for drug test against hepatitis C virus. PLoS One. 2011;6:e22921. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 38] [Cited by in F6Publishing: 37] [Article Influence: 2.8] [Reference Citation Analysis (0)] |
| 155. | Vliegenthart AD, Tucker CS, Del Pozo J, Dear JW. Zebrafish as model organisms for studying drug-induced liver injury. Br J Clin Pharmacol. 2014;78:1217-1227. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 111] [Cited by in F6Publishing: 120] [Article Influence: 13.3] [Reference Citation Analysis (0)] |
| 156. | He JH, Guo SY, Zhu F, Zhu JJ, Chen YX, Huang CJ, Gao JM, Dong QX, Xuan YX, Li CQ. A zebrafish phenotypic assay for assessing drug-induced hepatotoxicity. J Pharmacol Toxicol Methods. 2013;67:25-32. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 133] [Cited by in F6Publishing: 135] [Article Influence: 11.3] [Reference Citation Analysis (0)] |
| 157. | Hill A, Mesens N, Steemans M, Xu JJ, Aleo MD. Comparisons between in vitro whole cell imaging and in vivo zebrafish-based approaches for identifying potential human hepatotoxicants earlier in pharmaceutical development. Drug Metab Rev. 2012;44:127-140. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 82] [Cited by in F6Publishing: 73] [Article Influence: 6.1] [Reference Citation Analysis (0)] |
| 158. | North TE, Babu IR, Vedder LM, Lord AM, Wishnok JS, Tannenbaum SR, Zon LI, Goessling W. PGE2-regulated wnt signaling and N-acetylcysteine are synergistically hepatoprotective in zebrafish acetaminophen injury. Proc Natl Acad Sci USA. 2010;107:17315-17320. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 112] [Cited by in F6Publishing: 116] [Article Influence: 8.3] [Reference Citation Analysis (0)] |
| 159. | Amali AA, Rekha RD, Lin CJ, Wang WL, Gong HY, Her GM, Wu JL. Thioacetamide induced liver damage in zebrafish embryo as a disease model for steatohepatitis. J Biomed Sci. 2006;13:225-232. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 65] [Cited by in F6Publishing: 59] [Article Influence: 3.3] [Reference Citation Analysis (0)] |
| 160. | Passeri MJ, Cinaroglu A, Gao C, Sadler KC. Hepatic steatosis in response to acute alcohol exposure in zebrafish requires sterol regulatory element binding protein activation. Hepatology. 2009;49:443-452. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 148] [Cited by in F6Publishing: 150] [Article Influence: 10.0] [Reference Citation Analysis (0)] |
| 161. | Murtha JM, Qi W, Keller ET. Hematologic and serum biochemical values for zebrafish (Danio rerio). Comp Med. 2003;53:37-41. [PubMed] [Cited in This Article: ] |
| 162. | Vliegenthart AD, Starkey Lewis P, Tucker CS, Del Pozo J, Rider S, Antoine DJ, Dubost V, Westphal M, Moulin P, Bailey MA. Retro-orbital blood acquisition facilitates circulating microRNA measurement in zebrafish with paracetamol hepatotoxicity. Zebrafish. 2014;11:219-226. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 30] [Cited by in F6Publishing: 30] [Article Influence: 3.0] [Reference Citation Analysis (0)] |
| 163. | Burns CG, Milan DJ, Grande EJ, Rottbauer W, MacRae CA, Fishman MC. High-throughput assay for small molecules that modulate zebrafish embryonic heart rate. Nat Chem Biol. 2005;1:263-264. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 264] [Cited by in F6Publishing: 254] [Article Influence: 13.4] [Reference Citation Analysis (0)] |