Published online Dec 7, 2010. doi: 10.3748/wjg.v16.i45.5716
Revised: April 19, 2010
Accepted: April 26, 2010
Published online: December 7, 2010
AIM: To investigate morphological changes of the enteric nervous system (ENS) and the interstitial cells of Cajal (ICCs) in small bowel atresia.
METHODS: Resected small bowel specimens from affected patients (n = 7) were divided into three parts (proximal, atretic, distal). Standard histology and enzyme immunohistochemistry anti-S100, anti-protein gene product (PGP) 9.5, anti-neurofilament (NF), anti-c-kit-receptor (CD117) was carried out on conventional paraffin sections of the proximal and distal part.
RESULTS: The neuronal and glial markers (PGP 9.5, NF, S-100) were expressed in hypertrophied ganglia and nerve fibres within the myenteric and submucosal plexuses. Furthermore, the submucous plexus contained typical giant ganglia. The innervation pattern of the proximal bowel resembled intestinal neuronal dysplasia. The density of myenteric ICCs was clearly reduced in the proximal bowel, whereas a moderate number of muscular ICCs were found. The anti-CD117 immunoreaction revealed additional numerous mast cells. The distal bowel demonstrated normal morphology and density of the ENS, the ICCs and the mast cells.
CONCLUSION: The proximal and distal bowel in small bowel atresia revealed clear changes in morphology and density of the ENS and ICCs.
- Citation: Gfroerer S, Metzger R, Fiegel H, Ramachandran P, Rolle U. Differential changes in intrinsic innervation and interstitial cells of Cajal in small bowel atresia in newborns. World J Gastroenterol 2010; 16(45): 5716-5721
- URL: https://www.wjgnet.com/1007-9327/full/v16/i45/5716.htm
- DOI: https://dx.doi.org/10.3748/wjg.v16.i45.5716
Small bowel atresia is a congenital disorder that carries a substantial morbidity[1,2]. The etiology of bowel atresia remains unclear. One of two accepted theories of its pathogenesis is the concept of a lack of recanalization of the solid organ cord during the late stage of intestinal development[3]. Another concept is the occurrence of a late intrauterine mesenteric vascular accident[4]. The lack of revacuolization is the probable cause for most cases of duodenal atresia. Further studies have demonstrated that jejunoileal atresias occur as a result of intestinal volvulus, intussusception, internal hernia, or strangulation in a tight gastroschisis or omphalocele defect[5-11].
Newborns with small bowel atresia are operated on soon after birth. Owing to the severity of the dilatation of the proximal bowel and the hypoplasia of the distal bowel, various postoperative gastrointestinal motility problems may occur; such problems include prolonged adynamic ileus (11%) and the need for total parenteral nutrition (30%-70%)[12]. The underlying cause of this postoperative intestinal motility disorder is still unclear.
Basically, normal gastrointestinal motility depends on the coordinated function of the enteric nervous system (ENS), the intestinal smooth muscle and the interstitial cells of Cajal (ICCs). Previous studies revealed histological changes within the wall of the atretic and adjacent bowel in small bowel atresia. Hypertrophy of the bowel muscle proximal to the atresia was found in clinical and experimental studies on small bowel atresia. Various changes have been reported within the ENS in small bowel atresia[13]. Nevertheless, the relationship between the macroscopic and histological changes of the affected bowel and the postoperative motility disorder are still under investigation. Furthermore, the role of the ICCs in small bowel atresia needs to be elucidated further.
ICCs play a major role in gastrointestinal motility. ICCs express the tyrosine kinase receptor c-kit. Therefore specifically designed c-kit antibodies have been developed which stain ICCs but also other cell groups such as stem cells and mast cells. However, c-kit positive ICCs can be identified by clear morphological features.
The aim of this study was to investigate the morphology of the ENS and the ICCs in resection specimens of small bowel atresia.
Resected small bowel specimens (ileum) from affected newborn patients (n = 7) were included in the investigation after parental consent. The resected ileal specimens were divided into three parts (proximal, atretic, distal).
The specimens were fixed in 4% paraformaldehyde and processed into paraffin blocks. Paraffin-embedded tissues were sectioned at 2-4 μm (Leica SM 2000 R) followed by drying at 37°C in an incubator overnight. Before immunohistochemical staining, the paraffin sections were dewaxed for 10 min in xylene, followed by 10 min in acetone and 10 min in acetone/Tris-buffered saline (TBS; 1:1). After this treatment, the slides were washed in TBS.
If heat antigen retrieval was required, dewaxed paraffin sections were placed in microwave-proof tubes containing target retrieval solution (Dako). The slides were treated in the tubes for 5 min at 600 W in a microwave (SS 566H; Bosch, Munich, Germany). The evaporated volume was replaced by distilled water, and the procedure was repeated twice. After microwave treatment, the slides were left to cool down, then were washed in TBS.
Standard histology [hematoxylin/eosin (HE)] was performed on the sections. For immunohistochemistry, an alkaline phosphatase-anti-alkaline phosphatase (APAAP) staining kit (Dako Real™ Detection System, APAAP, Mouse) using anti-S100, anti- protein gene product (PGP) 9.5, anti-neurofilament (NF) and anti-c-kit-receptor (CD117) antibodies was employed. A non-sense mAb (clone: MR 12/53) served as negative control by omitting the primary antibody. The final concentrations are given in Table 1.
| Antibody | Clone | Company | Dilution |
| S-100 | Polyclonal (Z0311) | Dako, Glostrup, Denmark | 1:500 |
| PGP-9.5 | Polyclonal (Z5116) | Dako, Glostrup, Denmark | 1:25 |
| Neurofilament | 2F11 (M0762) | Dako, Glostrup, Denmark | 1:50 |
| c-kit | Polyclonal (A4502) | Dako, Glostrup, Denmark | 1:50 |
The evaluation of the immunohistochemical staining results was focused on the proximal and distal parts of the resected ileum.
The sections were evaluated by two independent investigators using light microscopy (magnification, × 40). HE staining was used to determine the overall histology of the investigated specimen. The distribution and density of immunoreactive ganglion cells, glial cells, nerve fibers and c-kit positive cells (ICCs, mast cells) were studied in each part of the resected bowel (proximal, atretic, distal). Since quantitative analysis of immunohistochemical staining is not possible, semi-quantitative scoring was performed as follows; - no expression (no staining), + low expression (few neuronal fibers and cells/few ICCs), ++ moderate expression (numerous neuronal fibers and cells/numerous ICCs), +++ high expression (dense networks of neuronal fibers and cells/dense network of ICCs).
The study included resected ileal segments from seven newborn patients (gestational age 38-40 wk). Six patients presented with type IIIa ileal atresia and one patient presented with multiple ileal atresia.
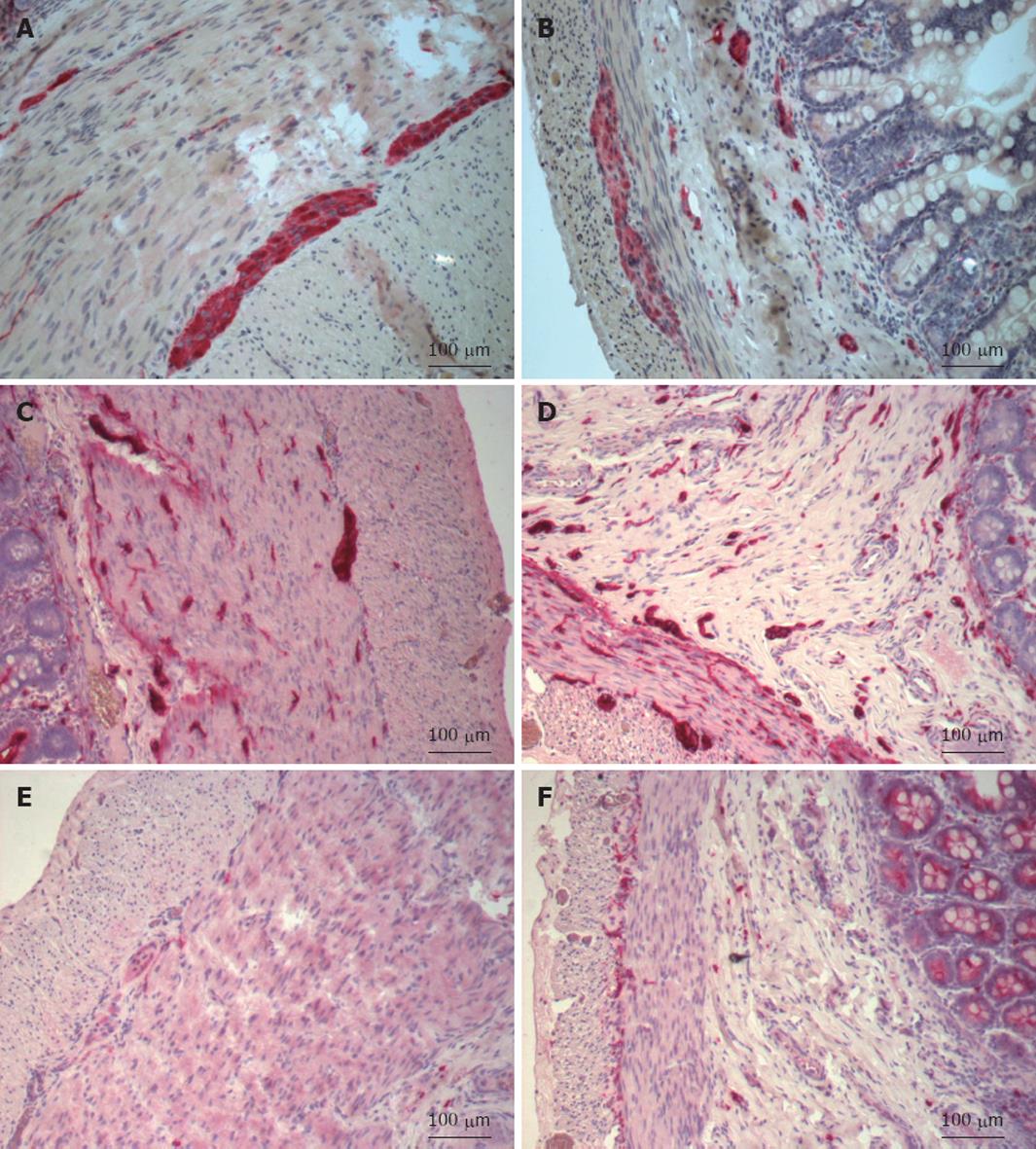
The neuronal markers PGP 9.5 and NF were strongly expressed within the ganglion cells and nerve fibers of the myenteric plexus (and submucosal plexus in the proximal ileum (Figure 1A). The submucosal plexus contained some giant ganglia (n > 10 ganglion cells) and numerous thick nerve fibers. The overall numbers of ganglia were not increased within the myenteric and submucosal plexuses (Table 2). The immunohistochemical staining revealed features of intestinal neuronal dysplasia (giant ganglia, hypertrophied nerve fibers).
| Proximal | Distal | |||||||
| SP | CM | MP | LM | SP | CM | MP | LM | |
| PGP 9.5 | ++ | + | ++ | + | ++ | + | ++ | + |
| S-100 | +++ | + | +++ | + | ++ | + | ++ | + |
| NF | ++ | + | ++ | + | ++ | + | ++ | + |
| c-Kit (ICCs) | - | -/+ | +/- | - | - | + | ++ | + |
The distal bowel had a normally expressed ENS within the submucosal and myenteric plexuses (Figure 1B).
Numerous S-100 immunoreactive glial cells were found in the two plexuses of the proximal ileum (Figure 1C). The expression of glial cells was increased within the proximal dilated bowel compared to the atretic and distal bowel (Table 2). Additional giant ganglia (> 10 ganglion cells/ganglion) were stained by S-100 within the submucosal plexus of the proximal bowel. Regular distribution and morphology of S-100 immunoreactive cells and fibers was found within the myenteric and submucosal plexuses of the distal ileum (Figure 1D).
The density of ICCs within the myenteric plexus was clearly reduced in the proximal bowel (Figure 1E), whereas some ICCs were found in the circular and longitudinal muscle layer (Table 2). The anti-CD117 immunoreaction revealed numerous mast cells within the proximal bowel. The distal bowel had a normal distribution of ICCs within the myenteric plexus and muscular layers and a normal number of mast cells (Figure 1F).
This study revealed distinct changes in the morphology of the ENS and ICCs in parts of the resected bowel proximal to small bowel atresia. In general, our findings are not unique since previous studies described changes within the ENS in small bowel atresia. Ozguner et al[14] reported that the proximal segment of the atretic intestine showed structural deficits. Abnormal ganglia cells and defects in the intestinal musculature were prominent, but the intestinal mucosa remained intact. They found abnormalities in both the antimesenteric side and mesenteric side. Their interpretation supported a vascular accident as a causative factor.
Di Nardo et al[15] presented an interesting case report of small bowel atresia that was initially diagnosed as hyper-ganglionosis and later changed to an enteric degenerative neuropathy. Watanabe et al[16] contributed an elegant study investigating the myenteric plexus in small bowel atresia using whole-mount preparations. This study showed mild hypoplasia of the ENS plexuses in the proximal segments[16].
In our study the expression of nerve fibers and glial cells appeared to be slightly increased, and some submucosal giant ganglia were found, which resembled intestinal neuronal dysplasia within the proximal dilated bowel. The expression of c-kit positive ICCs was clearly decreased in the dilated proximal bowel. The reduction of ICCs within the proximal dilated bowel has also been described before. In contrast to our study, some previous investigators have shown a reduction of the innervation density within the proximal bowel segments[13]. The innervation pattern and the expression of ICCs within the distal small bowel were normal in our study, similar to comparable investigations[13].
The crucial problem of investigating the developing ENS or pathological changes within the ENS in order to define hyper-ganglionosis or hypoganglionosis is the uncertainty in the normal numbers and distribution of enteric ganglia. The normal neuron density of the human myenteric plexus was investigated in several studies and resulted in a huge variation of more than 200-fold[17-20]. Schuffler et al[17] found 27.8 nerve cells per 100 mm of smooth muscle, Ikeda et al[19] described more than 30 nerve cells per 10 mm of smooth muscle as normal, whereas Smith[18] estimated 7 nerve cells per mm of smooth muscle. Finally Meier-Ruge et al[20] found 756 ganglion cells per 10 mm of smooth muscle. All these investigations were performed on conventional paraffin sections[17-20], which usually display only a two-dimensional image of the investigated structures. Since these profound differences have already been found within normal bowel specimens, conflicting results on numerical changes of ganglia and nerve fibers within the changed ENS in bowel atresia must be expected. Another major aspect is the widely accepted concept of ongoing postnatal plasticity of the ENS, which has to be taken into consideration.
A previous animal study which created a partial obstruction in dog ileum revealed that the ganglion cells increased in size and the smooth muscle of the dilated bowel became thicker[21]. The number of ganglion cells related to the muscle mass was decreased above the constriction. Although some ganglion cells increased in size, there was no evidence of any increase in number. Experimentally, a similar increase in ganglion size was observed proximal to a stenosis in another study[22]. In a chicken embryonic model of bowel obstruction, a marked reduction of the submucous plexus ganglia with intact muscular plexus ganglia was noted in the dilatated gut[23].
Our study also showed an increase in size of ganglia (hypertrophy). These hypertrophic myenteric and submucosal ganglia in the proximal resected bowel could be considered the result of adaptive phenomena to the long-lasting prenatal bowel obstruction. Several experimental models have been instrumental in supporting the concept that adaptive changes to the ENS occur proximal to the obstructed gut[24-31]. These studies revealed an increased density and size in both myenteric[26,28,29,31] and submucosal neurons[29-31], along with neurochemical[28,30] and cytoskeletal abnormalities of the myenteric neurons[31].
Ekblad et al[28] showed that, in the hypertrophic ileum, several neuronal populations showed changes in the expression of neuro-messengers. Myenteric neurons expressing vasoactive intestinal peptide (VIP), pituitary adenylate cyclase activating peptide, and galanin were notably increased in number. In submucosal ganglia, the number of VIP-immunoreactive neurons decreased, while those expressing VIP mRNA increased. NADPH diaphorase-positive submucosal neurons increased dramatically, while the number of neuronal-type nitric oxide synthase expressing neurons was unchanged. The number of ICCs decreased markedly in the hypertrophic ileum.
Another observation is the delayed maturation of ENS within the distal bowel during fetal development in cases with small bowel atresia[32]. Distortion of the polygonal architecture of the myenteric plexus has been shown postnatally in atretic parts of ileal type IIIa atresia[33]. It could only be speculated that after the restoration of bowel continuity does maturation of the ENS occur.
A previous animal study using a partial small obstruction model in mice revealed that 2 wk following the onset of a partial obstruction, the bowel increased in diameter, and hypertrophy of the tunica muscularis was observed oral to the obstruction site[27]. Networks of ICCs were disrupted oral to the obstruction, and this disruption was accompanied by the loss of electrical slow waves and responses to enteric nerve stimulation. These defects were not observed aboral to the obstruction. Furthermore, it was shown that removal of the obstruction led to the redevelopment of ICC networks and the recovery of slow wave activity within 30 d. Neural responses were partially restored in 30 d[27]. Similar repair mechanisms may occur after surgical correction of small bowel atresia. It seems obvious that decreases in ICCs in small bowel atresia and their restoration after removal of the obstruction contributes to the regulation of gastrointestinal motility.
Masumoto et al[34] showed muscular alterations in both segments of IA cases, which further contributes to the postoperative motility disorder. Another case report recently revealed long lasting chronological changes within the ENS, muscle components and ICCs in small bowel atresia[35].
The ENS and ICCs are altered in the proximal and dilated bowel in small bowel atresia. The innervation pattern of the proximal bowel resembles intestinal neuronal dysplasia. These changes might be the result of long-lasting bowel obstruction and stasis of bowel contents. The presented histological features do not contribute to the search for the pathogenesis of small bowel atresia. Nevertheless, the confirmed innervation abnormalities and defective expression of CD117-positive cells of the proximal bowel may have an influence on the postoperative gastrointestinal motility of the affected patients.
Small bowel atresia is a congenital anomaly of unknown cause. Despite early corrective surgery, patients carry a substantial morbidity because of postoperative gastrointestinal motility problems. Normal gastrointestinal motility is generated by the complex interaction of the enteric nervous system (ENS), the intestinal smooth muscle and the interstitial cells of Cajal (ICCs). Alterations in the ENS and ICCs may contribute to the motility problems in patients with small bowel atresia after surgery.
Previous studies revealed histological changes within the wall of the atretic and adjacent bowel in small bowel atresia. Nevertheless the relationship between the macroscopic and histological changes of the affected bowel and the postoperative motility disorder are still under investigation. Furthermore, the role of the ICCs in small bowel atresia needs to be elucidated further.
This study showed that the ENS and ICCs are altered in the proximal and dilated bowel in small bowel atresia. The innervation pattern of the proximal bowel resembles intestinal neuronal dysplasia.
The changes within the ENS and the ICCs may be the result of a long-lasting bowel obstruction and stasis of bowel contents. The presented histological features do not contribute to the search for the pathogenesis of small bowel atresia. However, the confirmed innervation abnormalities and defective expression of CD117-positive cells of the proximal bowel may have an influence on postoperative gastrointestinal motility in the affected patients.
Bowel atresia is a congenital defect in the continuity of the bowel. The incidence of small bowel atresia is higher than that of large bowel atresia and varies between 1:300 to 1:3000.
The authors studied the ileum of seven patients with ileal atresia. They reported that the proximal dilated intestine had an increased expression of nerve fibers and glial cells, with a decrease in ICCs, and an increase in ganglia size, whereas the distal intestine displayed normal features. They conclude that these alterations may influence on postoperative intestinal motility. The authors performed a well designed study in a very uncommon congenital disease, which is very interesting for the readers.
Peer reviewers: Guida Portela-Gomes, MD, PhD, Professor, Faculty of Medicine, University of Lisbon, Rua Domingos Sequeira-128, Estoril 2765-525, Portugal; Damian Casadesus Rodriguez, MD, PhD, Calixto Garcia University Hospital, J and University, Vedado, Havana City, Cuba
S- Editor Wang JL L- Editor Cant MR E- Editor Zheng XM
| 1. | Stollman TH, de Blaauw I, Wijnen MH, van der Staak FH, Rieu PN, Draaisma JM, Wijnen RM. Decreased mortality but increased morbidity in neonates with jejunoileal atresia; a study of 114 cases over a 34-year period. J Pediatr Surg. 2009;44:217-221. [Cited in This Article: ] |
| 2. | Dalla Vecchia LK, Grosfeld JL, West KW, Rescorla FJ, Scherer LR, Engum SA. Intestinal atresia and stenosis: a 25-year experience with 277 cases. Arch Surg. 1998;133:490-496; discussion 496-497. [Cited in This Article: ] |
| 3. | Tandler J. Zur entwicklungsgeschichte des menschlichen duodenum in fruhen embryonalstadien. Morphol Jahrb. 1900;29:187-216. [Cited in This Article: ] |
| 4. | Louw JH, Barnard CN. Congenital intestinal atresia; observations on its origin. Lancet. 1955;269:1065-1067. [Cited in This Article: ] |
| 5. | Santulli TV, Blanc WA. Congenital atresia of the intestine: pathogenesis and treatment. Ann Surg. 1961;154:939-948. [Cited in This Article: ] |
| 6. | Nixon HH. Intestinal obstruction in the newborn. Arch Dis Child. 1955;30:13-22. [Cited in This Article: ] |
| 7. | DeLorimier AA, Fonkalsrud EW, Hays DM. Congenital atresia and stenosis of the jejunum and ileum. Surgery. 1969;65:819-827. [Cited in This Article: ] |
| 8. | Nixon HH, Tawes R. Etiology and treatment of small intestinal atresia: analysis of a series of 127 jejunoileal atresias and comparison with 62 duodenal atresias. Surgery. 1971;69:41-51. [Cited in This Article: ] |
| 9. | Grosfeld JL, Clatworthy HW Jr. The nature of ileal atresia due to intrauterine intussusception. Arch Surg. 1970;100:714-717. [Cited in This Article: ] |
| 10. | Todani T, Tabuchi K, Tanaka S. Intestinal atresia dur to intrauterine intussusception: analysis of 24 cases in Japan. J Pediatr Surg. 1975;10:445-451. [Cited in This Article: ] |
| 11. | Gornall P. Management of intestinal atresia complicating gastroschisis. J Pediatr Surg. 1989;24:522-524. [Cited in This Article: ] |
| 12. | Kumaran N, Shankar KR, Lloyd DA, Losty PD. Trends in the management and outcome of jejuno-ileal atresia. Eur J Pediatr Surg. 2002;12:163-167. [Cited in This Article: ] |
| 13. | Masumoto K, Suita S, Nada O, Taguchi T, Guo R. Abnormalities of enteric neurons, intestinal pacemaker cells, and smooth muscle in human intestinal atresia. J Pediatr Surg. 1999;34:1463-1468. [Cited in This Article: ] |
| 14. | Ozguner IF, Savas C, Ozguner M, Candir O. Intestinal atresia with segmental musculature and neural defect. J Pediatr Surg. 2005;40:1232-1237. [Cited in This Article: ] |
| 15. | Di Nardo G, Stanghellini V, Cucchiara S, Barbara G, Pasquinelli G, Santini D, Felicani C, Grazi G, Pinna AD, Cogliandro R. Enteric neuropathology of congenital intestinal obstruction: A case report. World J Gastroenterol. 2006;12:5229-5233. [Cited in This Article: ] |
| 16. | Watanabe Y, Ando H, Seo T, Katsuno S, Marui Y, Horisawa M. Two-dimensional alterations of myenteric plexus in jejunoileal atresia. J Pediatr Surg. 2001;36:474-478. [Cited in This Article: ] |
| 17. | Schuffler MD, Bird TD, Sumi SM, Cook A. A familial neuronal disease presenting as intestinal pseudoobstruction. Gastroenterology. 1978;75:889-898. [Cited in This Article: ] |
| 18. | Smith VV. Intestinal neuronal density in childhood: a baseline for the objective assessment of hypo- and hyperganglionosis. Pediatr Pathol. 1993;13:225-237. [Cited in This Article: ] |
| 19. | Ikeda K, Goto S, Nagasaki A, Taguchi T. Hypogenesis of intestinal ganglion cells: a rare cause of intestinal obstruction simulating aganglionosis. Z Kinderchir. 1988;43:52-53. [Cited in This Article: ] |
| 20. | Meier-Ruge W, Morger R, Rehbein F. Hypoganglionic megacolon is associated with Hirschsprung’s disease. Z Kinderchir. 1970;8:254-264. [Cited in This Article: ] |
| 21. | Earlam RJ. Ganglion cell changes in experimental stenosis of the gut. Gut. 1971;12:393-398. [Cited in This Article: ] |
| 22. | Filogamo G, Vigliani F. [Experimental research on the correlation between the extent of innervation and the size and number of ganglion cells of the mesenteric plexus (Auerbach's plexus) in the dog.]. Riv Patol Nerv Ment. 1954;75:441-472. [Cited in This Article: ] |
| 23. | Fiegel HC, Schönberg RA, Roth B, Grasshoff S, Kluth D. Submucosal plexus of dilatated gut disappears after ligation in chicken embryos: preliminary results. Eur J Pediatr Surg. 2006;16:407-410. [Cited in This Article: ] |
| 24. | Kapur RP. Neuropathology of paediatric chronic intestinal pseudo-obstruction and related animal models. J Pathol. 2001;194:277-288. [Cited in This Article: ] |
| 25. | Barbosa AJ, Tafuri WL. Ganglion cell number in hypertrophic colon above experimental stenosis. Braz J Med Biol Res. 1983;16:165-169. [Cited in This Article: ] |
| 26. | Brehmer A, Göbel D, Frieser M, Graf M, Radespiel-Tröger M, Neuhuber W. Experimental hypertrophy of myenteric neurones in the pig: a morphometric study. Neurogastroenterol Motil. 2000;12:155-162. [Cited in This Article: ] |
| 27. | Chang IY, Glasgow NJ, Takayama I, Horiguchi K, Sanders KM, Ward SM. Loss of interstitial cells of Cajal and development of electrical dysfunction in murine small bowel obstruction. J Physiol. 2001;536:555-568. [Cited in This Article: ] |
| 28. | Ekblad E, Sjuve R, Arner A, Sundler F. Enteric neuronal plasticity and a reduced number of interstitial cells of Cajal in hypertrophic rat ileum. Gut. 1998;42:836-844. [Cited in This Article: ] |
| 29. | Gabella G. Size of neurons and glial cells in the intramural ganglia of the hypertrophic intestine of the guinea-pig. J Neurocytol. 1984;13:73-84. [Cited in This Article: ] |
| 30. | Gálvez Y, Skába R, Vajtrová R, Frantlová A, Herget J. Evidence of secondary neuronal intestinal dysplasia in a rat model of chronic intestinal obstruction. J Invest Surg. 2004;17:31-39. [Cited in This Article: ] |
| 31. | Jew JY, Williams TH, Gabella G, Zhang MQ. The intestine as a model for neuronal plasticity. Arch Histol Cytol. 1989;52 Suppl:167-180. [Cited in This Article: ] |
| 32. | Khen N, Jaubert F, Sauvat F, Fourcade L, Jan D, Martinovic J, Vekemans M, Landais P, Brousse N, Leborgne M. Fetal intestinal obstruction induces alteration of enteric nervous system development in human intestinal atresia. Pediatr Res. 2004;56:975-980. [Cited in This Article: ] |
| 33. | Ramachandran P, Vincent P, Ganesh S, Sridharan S. Morphological abnormalities in the innervation of the atretic segment of bowel in neonates with intestinal atresia. Pediatr Surg Int. 2007;23:1183-1186. [Cited in This Article: ] |
| 34. | Masumoto K, Suita S, Taguchi T. The occurrence of unusual smooth muscle bundles expressing alpha-smooth muscle actin in human intestinal atresia. J Pediatr Surg. 2003;38:161-166. [Cited in This Article: ] |
| 35. | Masumoto K, Akiyoshi J, Nagata K, Uesugi T, Taguchi S, Tajiri T, Taguchi T. Chronological change in intramural components in severe proximally dilated jejunal atresia: an immunohistochemical study. J Pediatr Gastroenterol Nutr. 2008;46:602-606. [Cited in This Article: ] |