Published online Oct 28, 2008. doi: 10.3748/wjg.14.6265
Revised: October 13, 2008
Accepted: October 20, 2008
Published online: October 28, 2008
Jejunal diverticulosis is a rare entity with variable clinical and anatomical presentations. Its reported incidence varies from 0.05% to 6%. Although there is no consensus on the management of asymptomatic jejunal diverticular disease, some complications are potentially life threatening and require early surgical treatment. We report a case of an 88-year-old man investigated for acute abdominal pain with a high biological inflammatory syndrome. Inflammation of multiple giant jejunal diverticulum was discovered at abdominal computed tomography (CT). As a result of the clinical and biological signs of early peritonitis, an emergency surgical exploration was performed. The first jejunal loop showed clear signs of jejunal diverticulitis. Primary segmental jejunum resection with end-to-end anastomosis was performed. Histopathology report confirmed an ulcerative jejunal diverticulitis with imminent perforation and acute local peritonitis. The patient made an excellent rapid postoperative recovery. Jejunal diverticulum is rare but may cause serious complications. It should be considered a possible etiology of acute abdomen, especially in elderly patients with unusual symptomatology. Abdominal CT is the diagnostic tool of choice. The best treatment is emergency surgical management.
- Citation: Staszewicz W, Christodoulou M, Proietti S, Demartines N. Acute ulcerative jejunal diverticulitis: Case report of an uncommon entity. World J Gastroenterol 2008; 14(40): 6265-6267
- URL: https://www.wjgnet.com/1007-9327/full/v14/i40/6265.htm
- DOI: https://dx.doi.org/10.3748/wjg.14.6265
The majority of jejunal diverticulosis cases are discovered incidentally during radiological investigations. Symptomatic presentations are rare and generally complicated. Jejunal and jejuno-ileal localization is nearly three times less frequent than duodenal, but about four times likely to develop complications[1]. Asymptomatic cases require neither medical nor surgical treatment. Rarity of mild or chronic presentations explains the absence of clear consensus on therapeutic strategy and conservative management[2]. Complicated presentations remain a diagnostic challenge because of non-specific and ambiguous symptomatology. Surgical exploration is the treatment of choice for almost all acute complicated cases[3].
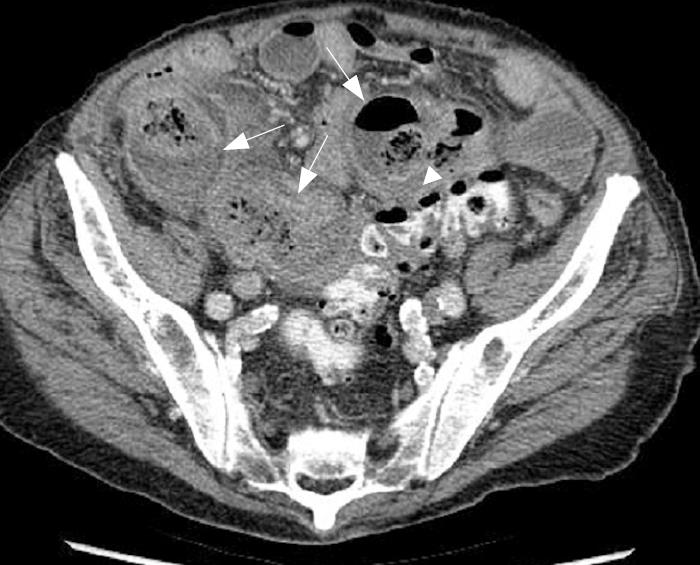
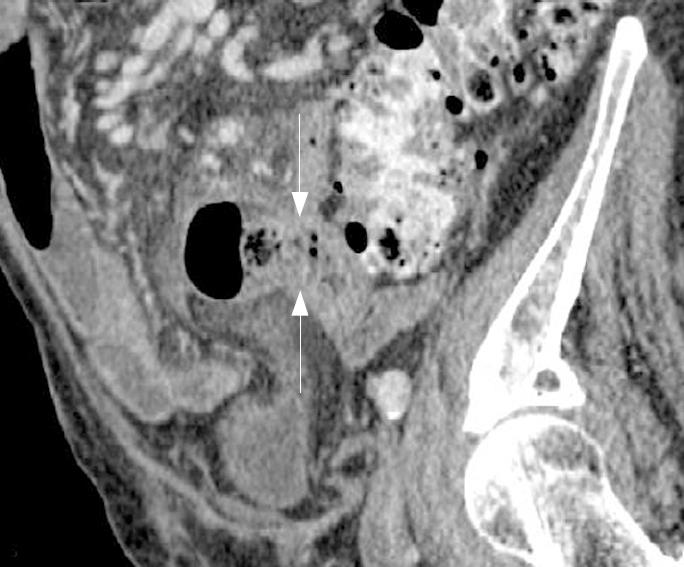
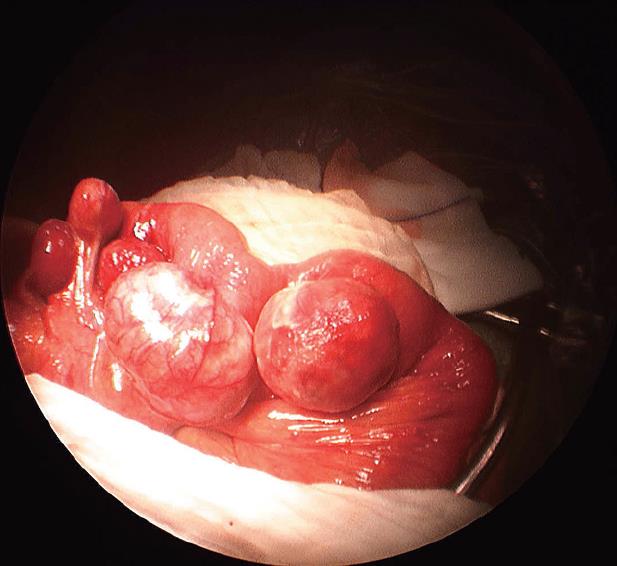
An 88-year-old male patient with a 6-year history of hypertensive terminal renal failure managed by hemodialysis was admitted for acute abdominal pain. Physical examination revealed right lower quadrant tenderness. C-reactive protein was 260 mg/L and white blood cell count was 19 g/L. There were no clinical or biological signs of bleeding. Abdominal computed tomography (CT) scan showed multiple small bowel giant diverticula, initially attributed to the ileum because of their localization in right iliac fossa. The diameters of these diverticula were between 3.5 cm and 6 cm and some showed clearly inflammatory infiltration (Figures 1 and 2). There was no pneumoperitoneum or intraperitoneal fluid. Emergency laparotomy confirmed the presence of inflamed diverticula on the proximal jejunal portion (Figure 3). Treatment was the resection of a 35-cm jeujunal segment, removing all visible diverticula. End-to-end anastomosis was performed. Histopathology report confirmed an ulcerative jejunal diverticulitis with some areas of perforation and acute local peritonitis. The patient made an excellent postoperative recovery with normalization of inflammatory parameters and rapid intestinal transit recovery. He was discharged on the 12th postoperative day.
The present case shows an exemplary preoperative diagnosis and the surgical management of jejunal diverticula in its typical presentation.
The difficulty is that diverticular small bowel disease is an uncommon entity with an incidence between 0.05% and 6%. Jejuno-ileal diverticulosis remains asymptomatic in about 80% of cases, but chronic clinical manifestations may be under-or misdiagnosed with dyspepsia and irritable bowel syndrome. The mean age of symptomatic patients is up to 60 years in all reported studies. Only less than 10% of the affected individuals develop acute complications such as inflammation, perforation, hemorrhage and obstruction[4].
Complicated jejuno-ileal diverticulosis is generally present in elderly males with non-specific unexplained central abdominal pain, associated with clinical and biological septic syndrome. Some cases have a history of chronic symptoms such as vague abdominal discomfort, fullness, recurrent central and upper abdominal cramping pain caused by pseudo-obstruction or bacterial overgrowth. Yet the diagnostic accuracy of complicated acute jejunal diverticulosis based on simple clinical evaluation is still extremely poor[5,6].
Abdominal CT with double-oral and intravenous contrast may allow the diagnosis based on the following findings: focal area of out-pouching of the mesenteric side of the bowel filled or not filled with feces-like materials, focal asymmetric wall thickening, or inflammatory process adjacent to a loop of jejunum[7,8]. In some cases, use of coronal or sagittal reformatted images is helpful in identifying the bowel segment with diverticula (Figure 2). Today, multi-slice CT is very helpful in diagnosing jejunal diverticulosis and appears clearly superior to conventional enteroclysis for small intestine diseases[9].
Radiology-proven complicated presentations of jejuno-ileal diverticulosis require emergency surgical management. Emergency resection of perforated, inflamed, bleeding or obstructed bowel segment with primary anastomosis is safe and gives the best outcome.
Jejunal diverticulum is rare and generally discovered in complicated presentations only. Interpretation of abdominal CT findings is the key to its correct diagnosis. The treatment of choice is surgical excision of the affected jejunum segment with primary end-to-end anastomosis.
Peer reviewer: Amado Salvador Pena, Professor, Department of Pathology, VU University Medical Centre, De Bolelaan 117, Boelelaan 1117, Po Box 7057, Amsterdam 1007 MB, The Netherlands
S- Editor Tian L L- Editor Wang XL E- Editor Lin YP
| 1. | Miller RE, McCabe RE, Salomon PF, Knox WG. Surgical complications of small bowel diverticula exclusive of Meckel's. Ann Surg. 1970;171:202-210. [Cited in This Article: ] |
| 2. | Liu CY, Chang WH, Lin SC, Chu CH, Wang TE, Shih SC. Analysis of clinical manifestations of symptomatic acquired jejunoileal diverticular disease. World J Gastroenterol. 2005;11:5557-5560. [Cited in This Article: ] |
| 3. | Zager JS, Garbus JE, Shaw JP, Cohen MG, Garber SM. Jejunal diverticulosis: a rare entity with multiple presentations, a series of cases. Dig Surg. 2000;17:643-645. [Cited in This Article: ] |
| 4. | Akhrass R, Yaffe MB, Fischer C, Ponsky J, Shuck JM. Small-bowel diverticulosis: perceptions and reality. J Am Coll Surg. 1997;184:383-388. [Cited in This Article: ] |
| 5. | Lempinen M, Salmela K, Kemppainen E. Jejunal diverticulosis: a potentially dangerous entity. Scand J Gastroenterol. 2004;39:905-909. [Cited in This Article: ] |
| 6. | El-Haddawi F, Civil ID. Acquired jejuno-ileal diverticular disease: a diagnostic and management challenge. ANZ J Surg. 2003;73:584-589. [Cited in This Article: ] |
| 7. | Coulier B, Maldague P, Bourgeois A, Broze B. Diverticulitis of the small bowel: CT diagnosis. Abdom Imaging. 2007;32:228-233. [Cited in This Article: ] |
| 8. | Macari M, Faust M, Liang H, Pachter HL. CT of jejunal diverticulitis: imaging findings, differential diagnosis, and clinical management. Clin Radiol. 2007;62:73-77. [Cited in This Article: ] |