Published online Feb 14, 2006. doi: 10.3748/wjg.v12.i6.977
Revised: April 1, 2005
Accepted: July 28, 2005
Published online: February 14, 2006
Crohn’s disease is well known to affect any part of the gastrointestinal tract including the oral cavity and anus. Various extraintestinal complications have been reported in Crohn’s disease, but extraintestinal involvement characterized by granulomatous lesions is uncommon. Here, we have reported a case about the involvement of the gallbladder in Crohn’s disease. A 33-year-old woman was diagnosed having panperitonitis due to intestinal perforation and cholecystitis. The patient was moved to the surgical service for an emergency operation. On the resected specimen, there was a broad longitudinal ulcer at the mesenteric side. The mucosa of the gallbladder was nodular and granular, and the wall was thickened. The surface epithelium of the gallbladder was partially eroded and pyloric gland metaplasia was observed focally. Rokitansky-Aschoff sinuses were also present. From the lamina propria to the subserosal layer, there were several well-formed epithelioid cell granulomas, which were the non-caseating sarcoidal type different from the foreign-body and xanthomatous granulomas. Periodic-acid Schiff and acid fast stains revealed no organism within the granulomas. Lymphoid aggregates were present throughout the gallbladder wall. Sections from the resected ileum showed typical features of the Crohn’s disease. When cholecystectomy is performed in a patient with Crohn’s disease, the possibility of gallbladder involvement should be carefully examined by histopathological tests.
- Citation: Andoh A, Endo Y, Kushima R, Hata K, Tsujikawa T, Sasaki M, Mekata E, Tani T, Fujiyama Y. A case of Crohn’s disease involving the gallbladder. World J Gastroenterol 2006; 12(6): 977-978
- URL: https://www.wjgnet.com/1007-9327/full/v12/i6/977.htm
- DOI: https://dx.doi.org/10.3748/wjg.v12.i6.977
Crohn’s disease is well known to affect any part of the gastrointestinal tract including the oral cavity and anus. Various extraintestinal complications have been reported in Crohn’s disease, but extraintestinal involvement characterized by granulomatous lesions is uncommon. Here, we report a case of the involvement of the gallbladder in Crohn’s disease.
The patient was a 33-year-old woman who was admitted to the Shiga University of Medical Science Hospital with complaints of nausea, vomiting, and severe abdominal pain, which had lasted for a couple of hours. Her past history included Crohn’s disease (ileocolonic type) and gallbladder stone, which had been diagnosed 2 years ago. She was well controlled with medications (2 250 mg/d 5-aminosalicilate and 2 000 kcal/d elemental diet) in these 2 years. She did not feel any symptoms of gallbladder stone.
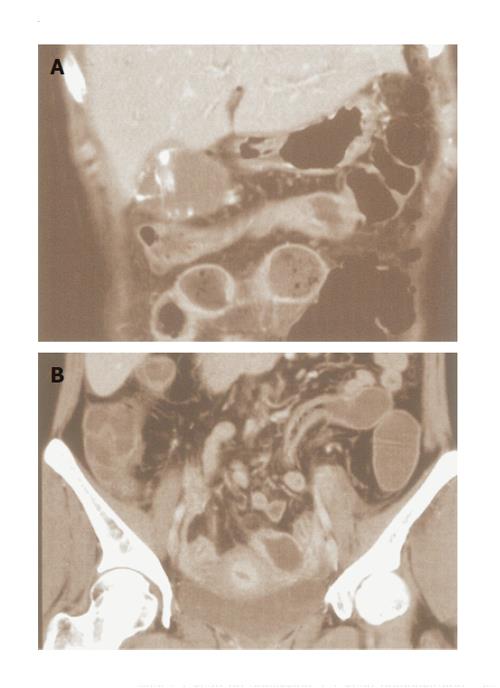
At the time of admission, her vital signs were as follows: body temperature 37.4 °C, blood pressure 92/60 Pa, and pulse 98 beats/min. The laboratory data included a white blood count of 13.1 (×103/mL), and C-reactive protein of 13.6 mg/dL. The values for biochemistry were within the normal range. An abdominal CT scan demonstrated a free-air space located in the dorsal side of the abdomen, ascites, strong contrast enhancement of a thickened ileum, fluid collection in the small intestine, and gallbladder swelling with calcifications (Figure 1). The intra- and extrahepatic bile ducts appeared normal. These findings were suggestive of panperitonitis due to intestinal (ileal) perforation and cholecystitis.
After the admission, the patient was moved to the surgical service for an emergency operation. A perforating hole (diameter 5 mm) was located at the ileum 20 cm oral side from Bauhin’s valve, and thus segmental ileotomy (25 cm resection) was performed. On the resected specimen, there was a broad longitudinal ulcer at the mesenteric side. Following an ileotomy, the patient also received a cholecystectomy. The serosal surface of the gallbladder adhered tightly to the greater omentum and duodenal bulbus.
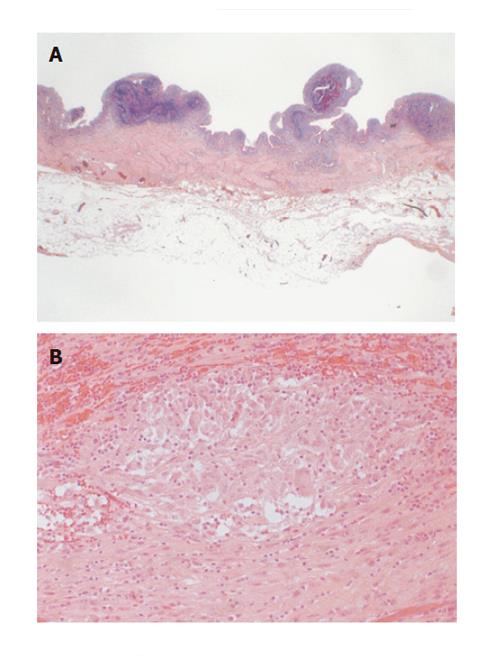
The mucosa was nodular and granular, and the wall was thickened. Erosion and submucosal bleeding were also observed, but there were no obvious ulcers (Figure 2A). The surface epithelium of the gallbladder was partially eroded and pyloric gland metaplasia was observed focally. The lamina propria showed discontinuous chronic active inflammation. The muscular layer was hypertrophied and the subserosal layer was thickened with marked fibrosis. Rokitansky-Aschoff sinuses were also present. From the lamina propria to the subserosal layer, there were several well-formed epithelioid cell granulomas, which were the non-caseating sarcoidal type, different from the foreign-body and xanthomatous granulomas (Figure 2B). Periodic-acid Schiff and acid fast stains revealed no organism within the granulomas. Lymphoid aggregates were present throughout the gallbladder wall. Sections from the resected ileum showed typical features of Crohn’s disease.
Her clinical course was good, and she was discharged from the hospital 1 mo after the operation.
A high prevalence of gallstones in Crohn’s disease has been reported[1], but gallbladder involvement in Crohn’s disease is very rare. Based on our MEDLINE search of the literature, only three case reports were found[2-4]. In all cases including our patient, the pathological examination of the gallbladder revealed transmural inflammation, granulomatous change and lymphoid aggregation, all of which were similar to those seen in the bowel lesions. Duodenal Crohn’s disease has been reported to occasionally involve the surrounding organs[2,3], but our case did not present any duodenal lesions, indicating that the gallbladder lesion might not be a consequence of spread by contiguity. When cholecystectomy is performed in a patient with Crohn’s disease, the possibility of gallbladder involvement should be carefully examined by histopathological examinations.
S- Editor Xu XQ and Guo SY L- Editor Elsevier HK E- Editor Bi L
| 1. | Lapidus A, Bångstad M, Aström M, Muhrbeck O. The prevalence of gallstone disease in a defined cohort of patients with Crohn's disease. Am J Gastroenterol. 1999;94:1261-1266. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 68] [Cited by in F6Publishing: 72] [Article Influence: 2.9] [Reference Citation Analysis (0)] |
| 2. | McClure J, Banerjee SS, Schofield PS. Crohn's disease of the gall bladder. J Clin Pathol. 1984;37:516-518. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 11] [Cited by in F6Publishing: 13] [Article Influence: 0.3] [Reference Citation Analysis (0)] |
| 3. | Post AB, van Stolk R, Broughan TA, Tuthill RJ. Crohn's disease of the gallbladder. J Clin Gastroenterol. 1993;16:139-142. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 9] [Cited by in F6Publishing: 10] [Article Influence: 0.3] [Reference Citation Analysis (0)] |
| 4. | Rettally CA, Treviño HH, Molina K, Kane SV. Crohn's disease involving the gallbladder. case report and review of the literature. Am J Gastroenterol. 2003;98:509-511. [PubMed] [Cited in This Article: ] |